Tag Archives: chronic heart failure
January 2017 Br J Cardiol 2017;24:14 Online First
News from the BSH 19th Annual Autumn Meeting
Dr Matthew Kahn

Systems of heart failure delivery Best practice tariff There is now a ‘best practice tariff’ (BPT) programme for heart failure (and for many other conditions). Professor Iain Squire (University of Leicester) reviewed the implications of this and discussed National Institute for Health and Care Excellence (NICE) quality standards for chronic heart failure (CHF). The first year of the BPT (April 2015–March 2016) was voluntary but it has been compulsory since the beginning of the 2016–2017 financial year. For the financial year 2016–2017, the tariff is worth a 5% uplift in the amount a trust is paid for each and every admission. It is

September 2013 Br J Cardiol 2013;20:116
Audit of communication with GPs regarding renal monitoring in CHF patients: a comment from primary care
Dr John B Pittard

The Sheffield audit of heart failure discharge advice given to GPs by Kanaan, Bashforth and Al-Mohammed (see pages 113–16) illustrates perfectly the imperfections of implementing research findings and guidelines into every day clinical practice. The paper rightly points out the selective nature of the entry criteria of patients to RALES (Randomised Aldactone Evaulation Study).1 Most research trial patients are more scrupulously managed and monitored than in real world circumstances. The traditional way of organising discharge summaries usually defaults to the least experienced junior staff. The perception is often that a career in account
June 2013 Br J Cardiol 2013;20:45–6 doi:10.5837/bjc.2013.14
Reducing the cost of heart failure while improving quality of life
Richard Brown, Andrew L Clark

In the USA, in 2008 the total inflation-adjusted cost of heart failure admissions was US$10.7 billion, compared with US$6.9 billion in 1997.2 So heart failure admissions are expensive and there is considerable interest in how we might reduce admissions, thereby reducing costs and leading to an improved quality of life (QoL) for patients with heart failure.3 One solution might be the Observation Unit (OU) proposed by Collins et al.4 as an alternative to hospital admission for patients needing a brief period (under 24 hours) of intravenous diuretic therapy. Observation, by definition, is the use of appropriate monitoring, diagnostic testing,

April 2013 Br J Cardiol 2013;20:(2) Online First
BSH 5th annual heart failure day for training and revalidation

A new treatment for acute heart failure? The recently published RELAX-AHF (Efficacy and Safety of Relaxin for the Treatment of Acute Heart Failure) study was a prospective, randomised, double-blind, placebo-controlled trial carried out in a targeted population of patients with acute HF.1 Relaxin is a physiological hormone that regulates maternal adaptations to pregnancy, increasing cardiac output, renal blood flow, and arterial compliance, alongside decreased peripheral vascular resistance.2,3 Serelaxin is a recombinant human relaxin-2 shown to have beneficial effects on symptoms and outcomes in early studies.4 The primary end points in thi

May 2012 Br J Cardiol 2012;19:85–9 doi:10.5837/bjc.2012.017
Drugs for diabetes: part 9 prescribing for patients with cardiac disease
Anna White, Gerard A McKay, Miles Fisher

(more…)
March 2012 Br J Cardiol 2012;19:15
Correspondence: Anaemia in CHF
Mohammed Shamim Rahman, Matthew Pavitt, TP Chua

Anaemia in chronic heart failure: what constitutes optimal investigation and treatment? Dear Sirs, We read with interest the recent supplement on anaemia in heart failure patients.1 Since the publication by Bolger et al.2 on the benefits of intravenous iron therapy in chronic heart failure (CHF), we have been screening for anaemia and iron deficiency in this cohort. We actively treat these patients based on the criteria of a haemoglobin level less than 12 g/dL, already on optimal conventional heart failure therapy, New York Heart Association (NYHA) class II symptoms or worse, and a ferritin of less than 100 μg/L. We were previously using an

March 2012 Br J Cardiol 2012; 19 :30–3 doi:10.5837/bjc.2012.006
Low pulse pressure does not reduce the efficacy of a heart failure exercise programme
Rosalind Leslie, John P Buckley

(more…)

September 2010 Br J Cardiol 2010;17:231–4
Drugs for diabetes: part 1 metformin
James G Boyle, Gerard A McKay, Miles Fisher

(more…)
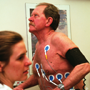
May 2010 Br J Cardiol 2010;17:133-7
Exercise heart rate guidelines overestimate recommended intensity for chronic heart failure patients
Louisa Beale, Helen Carter, Jo Doust, Gary Brickley, John Silberbauer, Guy Lloyd

(more…)
July 2009 Br J Cardiol 2009;16:194–6
Achieving preferred place of death – is it possible for patients with chronic heart failure?
Miriam J Johnson, Sharon Parsons, Janet Raw, Anne Williams, Andrew Daley

Introduction End-of-life care is now a Department of Health (DoH) priority. Primary care trusts have been charged with ensuring provision of high-quality end-of-life care, utilising enhanced central funding.1 While most people would prefer not to die in hospital, many still do.2 In order to change this situation, clinicians need to establish individual patient’s preferences regarding place of death (PPD) and then work proactively towards their achievement. The DoH is promoting the use of tools to help with this, such as the Gold Standards Framework (GSF), Liverpool Care Pathway (LCP) and Preferred Place of Care Plan, all of which are applic

