Anticoagulation

As so many of the common problems in clinical practice today relate to arterial and venous thrombosis, it is important that all healthcare professionals have a clear understanding of the basics of thrombosis/haemostasis and coagulation/anticoagulation pathways. The underlying final pathophysiological process in myocardial infarction and ischaemic stroke is thrombus formation (thrombogenesis). Other common cardiovascular disorders, such as atrial fibrillation (AF), heart failure, peripheral arterial disease and venous thromboembolism, are also associated with thrombogenesis.
In this updated and revised modular programme, we will first be introduced to antithrombotic therapy by examining the mechanism of coagulation and how this relates to the development of arterial and venous thrombosis. Module two will discuss how and why antiplatelet therapy is important, and module three will look at the value of anticoagulant therapy. Later modules consider the clinical aspects of anticoagulation, including the use of anticoagulants in acute coronary syndromes, non-valvular AF, cardioversion, peripheral arterial disease and venous thromboembolism. The role of the pharmacist is also considered.
Each module will have a series of multiple-choice questions. Its five and a half hours of learning leads to five and a half continuing professional development (CPD) credits.
This latest 2021 revision and earlier revisions of the anticoagulation modular programme have been funded by educational grants from Bayer. Bayer had no role in the writing of the modules and had no editorial control over the content. The original programme was made available with an educational grant from Bristol Myers Squibb (BMS) and Pfizer UK Limited. It has been independently written by leading UK physicians and pharmacists, and has been endorsed by the Atrial Fibrillation Association and Arrhythmia Alliance – the Heart Rhythm Charity.
Original modular programme written by:
Dr Andrew Blann, Consultant Clinical Scientist, City Hospital, Birmingham
Dr Louise Tillyer (retired)
Mr Sotiris Antoniou, Consultant Pharmacist, Barts Health NHS Trust and North East London Cardiovascular & Stroke Network, London
2016 revisions by:
Dr Matthew Rogers, Locum Consultant Haematologist, Royal Surrey County Hospital, Guildford; and
Mr Sotiris Antoniou, Consultant Pharmacist, Barts Health NHS Trust and North East London Cardiovascular & Stroke Network, London
2019 revisions (and module 6) by:
Dr Zara Sayar, Haematology Registrar (ST7), University College London Hospitals NHS Foundation Trust
2019 revision of module 5 by:
Mr Sotiris Antoniou, Consultant Pharmacist, Barts Health NHS Trust and North East London Cardiovascular & Stroke Network, London
2021 revisions by:
Dr Prabal Mittal, Haematology Clinical Research Fellow, University College London Hospitals NHS Foundation Trust, in association with Dr Zara Sayar
2021 revision of module 5 by:
Mrs Sana Harrison, Lead Pharmacist Anticoagulation and Haemostasis, St George’s University Hospitals NHS Trust, London
Anticoagulation module 1: Introduction to antithrombotic therapy
Released 27 October 2021 Programme: Anticoagulation 1 CPD/CME credit
- Understand the role of Virchow’s triad
- Discuss the coagulation cascade
- Recognise key aspects of platelet function
- Appreciate the consequences of loss of haemostasis
- Appreciate the importance of antiplatelet drugs in treating arterial thrombosis
- Explain the role of anticoagulants in treating venous thrombosis
Anticoagulation module 2: Antiplatelet therapy
Released 27 October 2021 Programme: Anticoagulation 1 CPD/CME credit
 Upon completing this module, participants should be better able to:
Upon completing this module, participants should be better able to:
- Understand the importance of platelets in pathology
- Be able to discuss the physiology of the platelet
- Recognise three major routes for suppressing platelet function
- Be aware of the mode of action of metabolic inhibitors
- Appreciate the value of ADP-receptor blockers
- Explain the uses of GpIIb/IIIa receptor blockers
- Be prepared for the consequences of mis-management of antiplatelet therapy: haemorrhage
Anticoagulation module 3: Anticoagulant therapy
Released 27 October 2021 Programme: Anticoagulation 1.5 CPD/CME credits

- Understand key aspects of the coagulation pathway
- Discuss the action of heparin, low molecular weight heparin, fondaparinux and vitamin K antagonists such as warfarin
- Recognise the mode of action of direct oral anticoagulants
- Appreciate the uses of anticoagulants in acute coronary syndromes and atrial fibrillation
- Prepare for the consequences of mis-managed anticoagulation, including haemorrhage.
Anticoagulation module 4: Clinical aspects of anticoagulation
Released 27 October 2021 Programme: Anticoagulation 1 CPD/CME credit

- How to initiate anticoagulation with vitamin K antagonists (VKA)
- Practical issues around VKAs and monitoring
- When and how to use direct oral anticoagulants (DOACs)
- Influence of DOACs on laboratory coagulation tests
- Anticoagulation management around invasive procedures
Anticoagulation module 5: The role of the pharmacist
Released 27 October 2021 Programme: Anticoagulation 0.5 CPD/CME credits

- Discuss the role of the hospital and community pharmacist in the provision of anticoagulant services
- Understand the initiation of anticoagulants, and patient counselling
- Provide pragmatic advice on use of warfarin and direct oral anticoagulants
Anticoagulation module 6: Peripheral arterial disease, cancer, thrombosis and anticoagulation requirements
Released 27 October 2021 Programme: Anticoagulation 0.5 CPD/CME credits
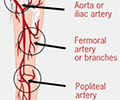
- Identify peripheral arterial disease and its management
- Understand the risk factors for venous thromboembolism (VTE) and the management options with direct oral anticoagulants
- Know about the prevalence of undiagnosed cancer in patients with an unprovoked VTE and the management of cancer-associated thrombosis

