Dextrocardia is a rare anomaly with an estimated prevalence of about one in 10,000. The incidence of coronary artery disease is the same as in the general population. We report two cases of successful percutaneous treatment of coronary stenoses and aim to highlight some of the additional technical challenges that such patients present to the Interventional Cardiologist.
Case report 1
A 51-year-old man with known dextrocardia presented with a 12-month history of angina and an early positive exercise electrocardiogram (ECG). His risk factors were hypertension, hyperlipidaemia and cigarette smoking. Physical examination revealed a right-sided apex beat and chest radiography confirmed the presence of dextrocardia.
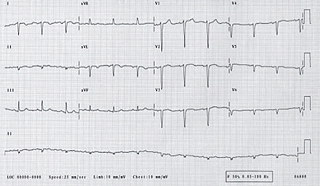
A 12-lead ECG (figure 1) showed sinus rhythm with a reduction in the R-wave voltage in the standard chest leads and a corresponding increase in the right-sided leads.
Coronary angiography of the left coronary system (right sided) revealed minor non-flow limiting disease. The morphologic right coronary artery (left sided) however, revealed a severe discrete stenosis (figure 2A) in the mid-vessel. Following a review of the coronary anatomy, percutaneous intervention was planned for a subsequent sitting.
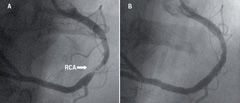
The procedure was performed using a 6 French AL-2 guide catheter and a high-torque, extra support guidewire. The lesion was directly stented with a 3.5 x 18 mm Zeta stent (Guidant). An excellent angiographic result was obtained (figure 2B) and there were no complications.
Case report 2
An 84-year-old woman with known dextrocardia was transferred from one of our referring hospitals with early post infarct unstable angina following an anterior ST elevation myocardial infarction for which she had received thrombolytic therapy.
Her risk factors were hypertension, hyperlipidaemia and previous smoking habit. Physical examination revealed findings consistent with situs inversus. A 12-lead ECG with leads reversed appropriately for dextrocardia, revealed well-controlled atrial fibrillation with widespread T wave inversion in the anterior chest leads. Chest radiography showed dextrocardia with a right-sided aortic knuckle as well as a right-sided gastric air bubble. Echocardiography confirmed a normal cardiac structure with impairment of left ventricular systolic function and evidence of hypokinesia in the antero-septal left ventricular territory.
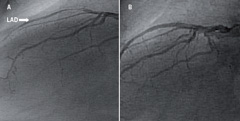
Coronary angiography of the morphologic left coronary system (right sided) revealed a subtotally occluded proximal left anterior descending artery (figure 3A) and a left circumflex artery that was free of disease. The anatomical right coronary artery (left sided) revealed a moderate stenosis in a small-calibre distal posterior descending artery.
A decision was made to proceed to percutaneous revascularisation of the left anterior descending artery at the same sitting. The procedure was performed using a 6 French JL 3.5 guide catheter and Galeo medium guidewire. The subtotally occluded proximal left anterior descending artery was sequentially pre-dilated using 1.5 and 2.0 mm balloon catheters prior to deployment of a 2.5 x 20 mm paclitaxel-coated Taxus stent (Boston Scientific). This resulted in an excellent angiographic appearance (figure 3B) and there were no complications.
Discussion
The first cardiac catheterisation in dextrocardia was reported in 1973,1 the first coronary artery bypass surgery in 19802 and the first percutaneous intervention in dextrocardia was performed in 1987.3 There have since been a few reports of percutaneous treatment of coronary stenoses in dextrocardia patients.
Performing percutaneous coronary intervention in patients with dextrocardia presents several challenges to the interventional cardiologist. These include selection of appropriate diagnostic and interventional catheters, acquisition of modified interventional views and in some cases mirror image visualisation using image reversal software.
Conflict of interest
None declared.
References
- Ettinger PO, Brancato R, Penn D. Dextrocardia, anteroseptal infarction and fascicular block. Chest 1975;68:229–30.
- Irvin RG, Ballenger JF. Coronary artery bypass surgery in a patient with situs inversus. Chest 1982;81:380–1.
- Moreyra AE, Saviano GJ, Kostis JB. Percutaneous transluminal coronary angioplasty in situs inversus. Cathet Cardiovasc Diagn 1987;13:114–16.

