This study examined the effect of a community-based intervention on the natural rise with age of the Framingham 10-year risk score. Patients in the 45–64-year-old age group from 10 general practices were sent an invite card including five self-screening questions. Those with any of the prescribed risk factors were invited to arrange an appointment to assess their risk of heart disease, where a Framingham risk score was calculated and advice given, and then invited for re-assessment around 18 months later.
Of 6,704 individuals contacted, 2,017 individuals (30.1%) arranged a health check, 982 followed up, and risk scores were calculated on 727. A significant reduction in the geometric mean Framingham risk was observed (from 10.65% to 10.34%), largely attributable to improvements in systolic blood pressure, high-density lipoprotein (HDL), reduced smoking and, perhaps, increased fruit and vegetable consumption. Although participants were 1.5 years older at follow-up, their risk profile corresponded to being 0.55 years younger, and, arguably, progression of risk was wound back by just over two years. Some self-selection bias was apparent, as those followed up had higher mean anxiety/depression scores at baseline.
In conclusion, community interventions can reduce cardiovascular risk even in deprived communities, although further analysis is required to establish cost-effectiveness.
Introduction
Cardiovascular disease (CVD) is a major cause of morbidity and mortality, particularly in deprived communities.1 Community or primary care based vascular risk assessment programmes are being introduced in England,2 Scotland and Wales, and are becoming central to USA health reform plans.3 However, the evidence base for these programmes is still emerging.4 The World Health Organization (WHO) estimate that better use of existing preventative measures could reduce the global burden of disease by as much as 70%5 based on some evidence from CVD prevention interventions that target risk factor management.6-8 However, the most effective methods for delivering these interventions are unclear. This study describes one approach, tailored toward the needs of a deprived community in a Welsh valley, with one of the highest standardised mortality rates for CVD in Wales.9,10 There is evidence that screening is particularly challenging in deprived communities as engagement rates are lower.11,12
This study utilised the Framingham Heart Study risk score, which estimates the 10-year risk of CVD. This scoring system combines seven risk factors: gender, age, cholesterol, high-density lipoprotein (HDL), systolic and diastolic blood pressure (BP), smoking status and family history. Although this calculation has been criticised,13 and there are alternatives such as the QRISK score,14 there is still debate on the best tool,15-17 and the Framingham score is still widely recommended and used in clinical practice and in research.18
Although primary prevention, aimed at altering lifestyle factors, has a relatively small impact on mortality,19 there is scope to examine the relative contribution of the components of the Framingham risk score that are impacted on most by primary prevention in high-risk populations. Some risk factors such as age, gender and family history cannot be modified. Taking into account changes to the Framingham risk score between initial assessment and follow-up is challenging, as risk scores will have increased simply because the average age in the study group will have increased. One of the aims of this paper was, therefore, to develop and test the concept that primary prevention of CVD could ‘wind back the clock’ in comparison to the expected rise in the Framingham risk score due to the progression of time alone.
Materials and methods
Participants aged 45–64 years from 10 general practices in the most deprived area in the north of Caerphilly Borough,20 who were not registered on GP disease registers as having CVD, hypertension, hyperlipidaemia, diabetes or terminal illness, were invited to attend an appointment with a nurse in the community for a ‘Healthy Heart’ check. The invitation was in the form of a brief self-screening card with questions on risk factors, a measured piece of string, 80 cm long for women and 94 cm long for men, was included to measure whether their central obesity exceeded accepted thresholds.21 A reminder letter was sent two weeks after the first invitation. A follow-up invitation was sent to attendees around 18 months later, to re-assess the risk of heart disease. All participants completed health locus of control22 and Hospital Anxiety and Depression23 questionnaires. Fasting lipids and blood glucose were measured, BP recorded, and body mass index (BMI) calculated, prior to being seen by a CVD specialist nurse for a discussion on lifestyles, risk factors and assessment of the Framingham risk score. Participants who were identified as being at high risk of CVD (above 20%), or with fasting glucose over 6 mmol/L, or an irregular pulse, were referred back to their GP. The assessment process is described in a previous paper based on a smaller data set.10
Study data were analysed using SPSS. Where data were skewed, log transformation (100 x natural log) was undertaken. Chi-square test, t-test, Wilcoxon test and U/mn index were used to compare groups, as appropriate. The U/mn statistic and its 95% confidence intervals (CI) were useful when comparing ordinal and quantitative variables. The statistic takes the value of 0.5 when the two samples are identical, and 1 or 0 if they do not overlap. It is not affected when a variable is log transformed.24 BMI was calculated using height at baseline. The risk score based on the Framingham longitudinal study was calculated using the algorithm presented in table 6 of Wilson et al.,13 the formula being multiplied by 1.5 in the event of positive family history. This figure was chosen as reasonably representative of the impact of family history in the available literature.13,25-27
The Framingham score has an inbuilt dependence on age; furthermore, most of the other variables included in the formula are prone to change systematically with ageing. To calculate the effect of ageing by 18 months, changes observed at follow-up for quantitative variables were adjusted. The adjustment was based on the regression coefficient b, representing the rate of change of the variable in question per year of age in a cross-sectional analysis of the baseline data. For consistency, only those individuals with follow-up as well as baseline data for the variable in question were used in this regression model. The adjusted mean change was, therefore, given by Δ -b×t where Δ denoted the unadjusted mean change and t represents the mean interval to follow-up in years, restricted to the same subjects. The standard errors for Δ and b were used to construct a standard error and, hence, a hypothesis test and 95% CI for the adjusted mean change.
Three additional analyses using the Framingham formula were undertaken to address this issue using a range of methods.
- Scores at baseline and follow-up were calculated, except that a constant age of 55 years was used in both baseline and follow-up scores.
- The score at baseline was calculated using the standard formula and the score at follow-up using the subject’s age at baseline.
- The score at baseline was calculated using the standard formula and the score at follow-up using the subject’s age at follow-up, but other data as at the baseline visit.
The analyses were designed to give insight into several different facets of the input of age into the score.
Ethical approval for the study was obtained from the Gwent Research Ethics Committee (Ref. No. RD/294/04).
Results
Between September 2004 and May 2007, 6,704 individuals were contacted and invited to self-assess their eligibility to attend an appointment to assess their risk of heart disease, of whom 2,017 individuals (30.1%) presented themselves for a health check. Of these, 982 attended an 18-month follow-up appointment. Framingham scores were calculated on 727 subjects, although data were available for most fields for 738 individuals. This was because of problems in calculating a Framingham score for individuals with very high lipid levels. The exact number of records, for whom data were available for each variable, is indicated in tables 1 and 2. Figure 1 briefly summarises the data used in the study.
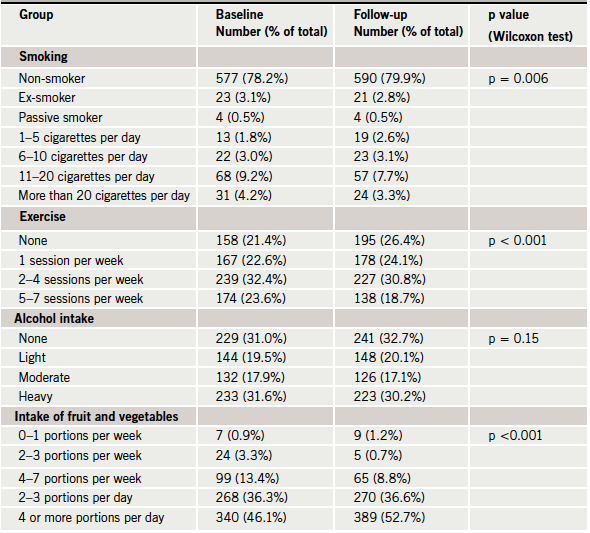
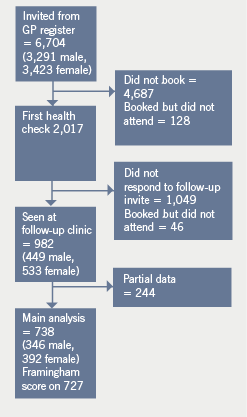
Comparing the data of those who were and were not followed up, the proportion of participants who smoked was statistically significantly lower among those who were followed up (70.5%), compared with those who were not (78.2%). There was also a small (0.12 mmol/L) but significantly higher fasting glucose level in those who presented for follow-up. Participants, who were followed up, were on average more than a year older at entry than those who were not, had higher levels of anxiety and depression, and had slightly lower blood pressure levels, than those who did not come for follow-up.
Waist circumference at or above the 94 cm threshold for men was present in 53.7% of men; similarly, 63.3% of women were over the female waist circumference threshold of 80 cm.
Changes at follow-up
These analyses relate to 738 of the 2,017 participants who were followed up on average 1.488 years (range 0.844 to 2.162 years) from the initial visit. A positive family history was reported at baseline in 215 of these 738 participants; however, an additional eight of them reported a positive family history by the time of follow-up.
Table 1 summarises changes in the categorical variables. At follow-up there were modest, nevertheless statistically significant, improvements in fruit and vegetable intake, reduction in smoking, and a slight suggestion of a decrease in alcohol consumption. Conversely, there was a statistically significant decrease in exercise, which was not explicable in terms of seasonal differences.
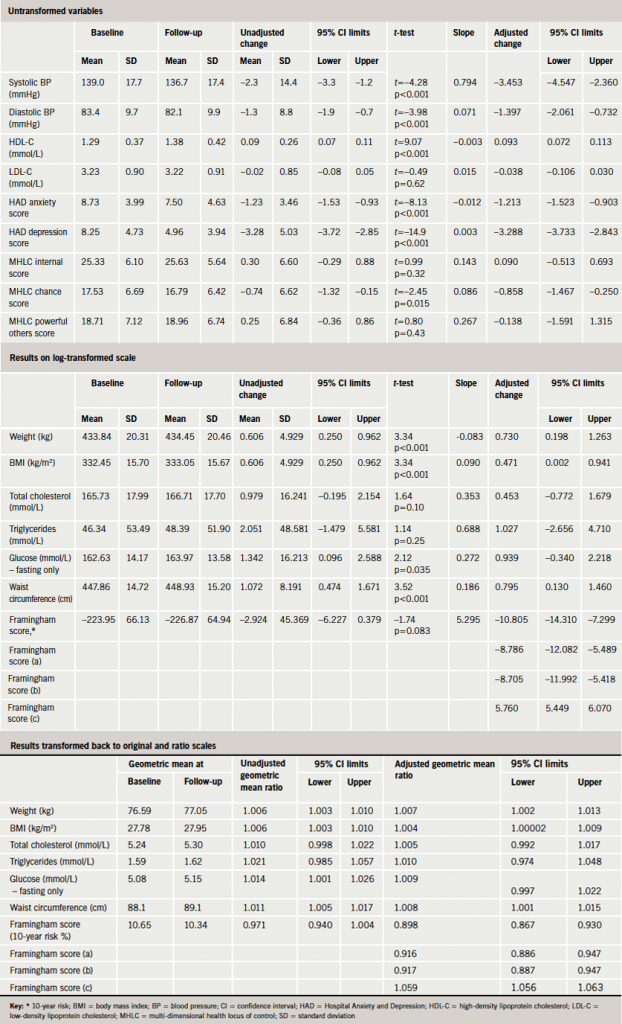
Table 2 summarises changes in the quantitative variables. The depression and anxiety scores, HDL cholesterol levels, and systolic and diastolic BP show very clear evidence of improvement at follow-up. There was a small, although statistically significant, increase in the ‘internal locus of control’. Mean height decreased by 0.5 cm over the 18 months of the study.
The Framingham score decreased, from a geometric mean of 10.65 to 10.34, representing a reduction in 10-year risk of CVD from 10.65% to 10.34%. The change in the geometric mean (0.971) represents a relative decrease in the Framingham risk score of 2.9%. A 95% CI for this change is from a 6.0% decrease to a 0.4% increase.
Compensating for the effect of ageing on CVD risk
Table 2 also incorporates an adjustment for the fact that, on average, 18 months had elapsed from entry to follow-up. The effect of adjustment for ageing is to enhance substantially the benefit for systolic BP reduction. Taking elapsed time into account enhances the mean systolic BP decrease from 2.27 mmHg to 3.45 mmHg. In effect, winding back of the clock enhances the effect of the intervention on systolic BP by around 50%.
Diastolic BP, HDL cholesterol, anxiety and depression scales alter little on adjustment for ageing. Adjustment for ageing partly explains the deterioration in cholesterol, triglycerides, waist circumference and blood glucose. Only blood glucose was no longer statistically significant after adjustment.
The first Framingham analysis presented in table 2 indicates a reduction of 2.9 (in log-scale units) in the log-transformed Framingham risk score, at follow-up. This reduction in the Framingham risk score may be regarded as the consequence of two separate effects: an increase of 5.8 units, due purely to the age component of the score being increased by 1.5 years, and a decrease of 8.7 or 8.8 units, due to the other risk factors included in the Framingham score having improved at follow-up. Some of the health gain in ‘winding back’ CVD risk, as a result of the intervention, is masked by the effect of ageing on the Framingham risk calculation.
Additional analyses are presented in table 2, which address the issue of adjusting for ageing in different ways. The separate estimates (a, b, and regression adjustment) of age-adjusted benefit of 8.8, 8.7 and 10.8, are reasonably similar, considering that they are derived in quite different ways, and demonstrate that when age is taken into account, the improvements this intervention has demonstrated are significantly enhanced. Even in those individuals where the Framingham risk score has not decreased, there has been some ‘winding back of the clock’ in relation to CVD risk, as the risk would have been expected to rise with age.
Based on the cross-sectional analysis of the baseline scores, the adjusted analysis showed that the risk score at follow-up was 8–10% lower than would have been expected as a result of the cohort ageing by 1.49 years. Indeed, it could be said that the effect of intervention on the Framingham score was to ‘wind back the clock’ by approximately 0.55 years (2.924/5.295). These participants were actually 1.49 years older than at entry, but their risk profile corresponded to being 0.55 years younger, so it could be argued that at follow-up their risk was equivalent to retarding the progression of risk by just over two years.
Discussion
A significant reduction in the mean Framingham risk was demonstrated in this study for those who attended the follow-up appointment around 18 months later. This effect was largely dependent on improvements in systolic BP, HDL and a reduction in the proportion who smoked. Fruit and vegetable consumption was also increased and this may have played a part. The small change in internal locus of control may indicate that the intervention has had some effect in the direction of empowering participants. This study supports the proposal that nurse-led CVD screening in a deprived population has a reasonable uptake, is feasible, and is of benefit in reducing mean CVD risk. This study did not elicit data on changes to drug prescribing. Part of the benefit observed in this study may have resulted from screened individuals then being prescribed blood pressure and cholesterol lowering medications by their GPs.
The study also explored the concept of adjustment for the passage of time. Using a variety of approaches, it has been demonstrated that when the Framingham risk score does not rise to the extent that would be expected solely on the basis of the passage of time, the intervention has ‘wound back the clock’ in that some health gain is achieved in those individuals. A concept similar to winding back the clock has previously been described.28 The authors of this paper used the concept of ‘heart age’ and compared this against ‘chronological age’. Both concepts may be useful in communicating risk to individuals and communicating something of the benefit that has been gained by changes in the individual’s Framingham risk score.
It is possible that the small increase in internal locus of control may represent increased empowerment of participants, which may have mediated some of the health gain achieved. The project emphasised the importance of motivational interviewing and sought to empower participants to take responsibility for their own wellbeing.
Attendance for health checks in socioeconomically deprived populations is widely recognised as being lower than that of the wider population.11,12 Given the deprived nature of this community, and the fact that community interventions usually have great difficulty in recruiting men, an encouraging proportion of those who attended were men (44.8%). It may be possible to improve this figure further by the introduction of ‘out of hours’ appointments.
A significant proportion of participants did not attend for follow-up. Differences in the characteristics of those who are followed up can introduce bias as they are a self-selected population. Examining the baseline data, there were differences between those who were followed up and those who were not. The differences may indicate that those who believed they had made significant changes to their risk profile were more ready to return to a follow-up appointment.
In this study, those who attended for follow-up had significantly higher mean anxiety and depression scores (p<0.001), which would support the concept that those who participate in ongoing health check ups have some characteristics associated with poorer mental health. However, the intervention does not appear to have increased anxiety in those who did return when anxiety levels at baseline and follow-up are compared.
This study was not a randomised-controlled trial and the results should, therefore, be considered as ‘hypothesis raising’. A randomised trial might be the next step forward. However, the resources required to undertake one would be very much greater than those incurred in the present study, for two reasons. A trial randomised at individual level requires at least four times as many subjects as a before-and-after study in order to be powered to detect a difference of any specified size. Moreover, the increase in sample size required would be very much larger still, in that only a cluster randomised trial, randomised at practice level, is likely to provide a robust form of randomisation. However, cluster randomised trials have successfully been undertaken for a range of other behavioural interventions, for example smoking cessation, and funding should be sought to test cardiovascular risk reduction in a cluster randomised trial.
It was evident that there were no improvements in waist circumference, exercise levels and total cholesterol. There is, therefore, a need to further examine ways in which the effectiveness of the intervention can be increased.
The slight reduction in average height, an average of 0.5 cm over 18 months, was an interesting incidental finding. This rate is consistent with the average loss of height of several centimetres that occurs in middle age.29
There are a number of ways in which this work can be taken forward in the future. Vascular risk assessment could be provided in a wider variety of community contexts, particularly in community pharmacies. There is also scope to compare the use of the Framingham risk score against the QRISK score in community settings. Finally, there is also a need for further work to examine the cost-effectiveness of vascular screening in different community settings and to compare this with the National Institute for Health and Clinical Excellence (NICE) cost-effectiveness threshold of £30,000 per quality-adjusted life year (QALY).
Acknowledgements
We want to express our thanks to the GP practices
that helped identify patients from their registers, and to staff that have worked on this project including Tracey Deacon, Sue Scrozynska, Monica Harries, Lyn Stallard and David Simpson. This project was funded by Caerphilly Teaching Local Health Board which now forms part of Aneurin Bevan Health Board. REH was employed by this organisation.
Conflict of interest
None declared.
Key messages
- Community-based interventions can reduce Framingham cardiovascular risk scores, even in deprived communities
- The effect of this intervention was to ‘wind back the clock’ on the Framingham score by approximately 0.55 years, and arguably, progression of risk was wound back by just over two years
- This study supports the increased development of vascular risk reduction measures, although further health economic assessment of the potential benefits is required
References
- World Health Organization. Prevention of Cardiovascular Disease. Guidelines for assessment and management of total cardiovascular risk. Geneva: WHO, 2007.
- Department of Health. Putting prevention first – NHS health check: vascular risk assessment and management. Best practice guidance. London: DoH, 2008.
- Obama B. Modern health care for all Americans. N Engl J Med 2008;359:1537.
- Robson J, Boomla K, Hart B, Feder G. Estimating cardiovascular risk for primary prevention: outstanding questions for primary care. BMJ 2000;320:702–04.
- Chan M. The world health report 2008: Primary health care now more than ever. Geneva: WHO, 2008.
- Cupples ME, Smith SM, Murphy AW. How effective is prevention in coronary heart disease? Heart 2008;94:1370–1.
- Hobbs FD. Primary prevention of cardiovascular disease: managing hypertension and hyperlipidaemia. Heart 2004;90(suppl 4):iv22–iv25.
- Redberg RF, Benjamin EJ, Bittner V et al. ACCF/AHA 2009 performance measures for primary prevention of cardiovascular disease in adults. Circulation 2009;120:1296–336.
- Davies G, Price T. Health Needs Assessment 2006 – Health Status and Key Determinants. Cardiff: National Public Health Service for Wales, 2007.
- Richardson G, van Woerden HC, Morgan L et al. Healthy Hearts – a community-based primary prevention programme to reduce coronary heart disease. BMC Cardiovasc Disord 2008;8.
- Thorogood M, Coulter A, Jones L, Yudkin P, Muir J, Mant D. Factors affecting response to an invitation to attend for a health check. BMJ 1993;47:224–8.
- Waller D, Agass M, Mant D et al. Health checks in general practice: another example of inverse care? BMJ 1990;300:1115–18.
- Wilson PWF, D’Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB. Prediction of coronary heart disease using risk factor categories. Circulation 1998;97:1837–47.
- Hippisley-Cox J, Coupland C, Vinogradova Y, Robson J, May M, Brindle P. Derivation and validation of QRISK, a new cardiovascular disease risk score for the United Kingdom: prospective open cohort study. BMJ 2007;335:136–41.
- Collins GS, Altman DG. An independent external validation and evaluation of QRISK cardiovascular risk prediction: a prospective open cohort study. BMJ 2009;339:b2584.
- Liew SM, Glasziou P. QRISK validation and evaluation QRISK may be less useful. BMJ 2009;339:b3485.
- Tunstall-Pedoe H, Woodward M, Watt G. QRISK validation and evaluation ASSIGN, QRISK, and validation. BMJ 2009;339:b3514.
- Wood D, Wray R, Poulter N et al. JBS 2: Joint British Societies’ guidelines on prevention of cardiovascular disease in clinical practice. Heart 2005;91(suppl 5):v1–v52.
- Ebrahim S, Beswick A, Burke M, Smith GD. Multiple risk factor interventions for primary prevention of coronary heart disease. Cochrane Database Syst Rev 2006;(4):CD001561.
- Caerphilly County Borough. A partnership strategy for health, social care and well-being in Caerphilly County Borough 2005–2008. Ystrad Mynach: Caerphilly County Borough, 2005.
- Dobbelsteyn CJ, Joffres MR, MacLean DR, Flowerdew G. A comparative evaluation of waist circumference, waist-to-hip ratio and body mass index as indicators of cardiovascular risk factors. The Canadian Heart Health Surveys. Int J Obes Relat Metab Disord 2001;25:652–61.
- Wallston KA, Wallston S. Development of the multidimensional health locus of control (MHLC) scales. Health Educ Monogr 1978;6:160–70.
- Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand 1983;67:361–70.
- Newcombe RG. Confidence intervals for an effect size measure based on the Mann-Whitney statistic. Part 2: Asymptotic methods and evaluation. Stat Med 2006;25: 559–73.
- Roncaglioni MC, Santoro L, D’Avanzo B et al. Role of family history in patients with myocardial infarction. An Italian case-control study. GISSI-EFRIM Investigators. Circulation 1992;85:2065–72.
- Cooper JA, Miller GJ,
Humphries SE. A comparison of the PROCAM and Framingham point-scoring systems for estimation of individual risk of coronary heart disease in the Second Northwick Park Heart Study. Atherosclerosis 2005;181:93–100. - Philips B, de Lemos JA, Patel MJ, McGuire DK, Khera A. Relation of family history of myocardial infarction and the presence of coronary arterial calcium in various age and risk factor groups. Am J Cardiol 2007;99:825–9.
- D’Agostino RB, Vasan RS, Pencina MJ et al. General cardiovascular risk profile for
use in primary care: The Framingham heart study. Circulation 2008;118:E86. - Sorkin JD, Muller DC, Andres R. Longitudinal change in height of men and women: implications for interpretation of the body mass index: the Baltimore Longitudinal Study of Aging. Am J Epidemiol 1999;150:969–77.

