Clinical articles

October 2015 Br J Cardiol 2015;22:147–54 doi :10.5837/bjc.2015.034 Online First
Treatment patterns and lipid levels among patients with high-risk atherosclerotic CVD in the UK
Beth L Nordstrom, Jenna M Collins, Robert Donaldson, William A Engelman, Antje Tockhorn, Yajun Zhu, Zhenxiang Zhao
| Full text
October 2015 Br J Cardiol 2015;22:157 doi :10.5837/bjc.2015.035 Online First
Pre-alert calls for primary PCI: a single-centre experience
Jennifer A Rossington, Stephen F Cole, Yasmin Zaidy, Michael S Cunnington, Richard M Oliver
| Full text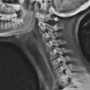
October 2015 Br J Cardiol 2015;22:159 doi :10.5837/bjc.2015.036 Online First
Atypical chest pain in young adult patients: dropped shoulder syndrome as a cause
Ali Abdul-Latif, Adnan Shakir
| Full text
October 2015 Br J Cardiol 2015;22:160 doi :10.5837/bjc.2015.037
Coenzyme Q10 and cardiovascular disease: an overview
David Mantle
| Full textAugust 2015 Br J Cardiol 2015;22:101–4 doi :10.5837/bjc.2015.029
Inflammation is associated with myocardial ischaemia
Kushal Pujara, Ashan Gunarathne, Anthony H Gershlick
| Full textAugust 2015 Br J Cardiol 2015;22:105–9 doi :10.5837/bjc.2015.030
Oral anticoagulation in hospitalised patients with newly diagnosed AF: a story of too little, too late
Shohreh Honarbakhsh, Leigh-Ann Wakefield, Neha Sekhri, Kulasegaram Ranjadayalan, Roshan Weerackody, Mehul Dhinoja, R Andrew Archbold
| Full textAugust 2015 Br J Cardiol 2015;22:118 doi :10.5837/bjc.2015.031
UK experience of conversion of radial to femoral access in coronary interventions
Shana Tehrani, David Hackett
| Full text
July 2015 Br J Cardiol 2015;22:(3) doi :10.5837/bjc.2015.023 Online First
FY1 in heart failure: the good, the bad and the ugly! Reflections by the FY1 doctors in heart failure and their supervisor on the first year of a new post
Laura Styles, Sarah Soar, Philippe Wheeler, Abdallah Al-Mohammad
| Full text
July 2015 Br J Cardiol 2015;22:(3) doi :10.5837/bjc.2015.024
The use of EKOS-catheter-directed thrombolysis in the management of extensive thromboembolism
Lisa Leung, Aerakondal B Gopalamurugan
| Full text
July 2015 Br J Cardiol 2015;22:(3) doi :10.5837/bjc.2015.025 Online First
Calling the cardioverted: an audit of long-term anticoagulation in patients attending for DCCV
Philippa Howlett, Michael Hickman, Edward Leatham
| Full text
