Clinical articles
November 2019 Br J Cardiol 2019;26:141–4 doi :10.5837/bjc.2019.041
Lipid testing and treatment after acute myocardial infarction: no flags for the flagship
Louise Aubiniere-Robb, Jonathan E Dickerson, Adrian J B Brady
| Full textNovember 2019 Br J Cardiol 2019;26:153–6 doi :10.5837/bjc.2019.042
The permanent decline of temporary pacing
Richard Baker, David Wilson
| Full textOctober 2019 Br J Cardiol 2019;26:149–52 doi :10.5837/bjc.2019.033
Transcatheter aortic valve replacement in patients with systolic heart failure
Tariq Enezate, Jad Omran, Obai Abdullah, Ehtisham Mahmud
| Full textOctober 2019 Br J Cardiol 2019;26:157–8 doi :10.5837/bjc.2019.034
The effect of ageing on the frontal QRS-T angle on the 12-lead ECG
Sadia Chaudhry, Jagan Muthurajah, Keoni Lau, Han B Xiao
| Full textOctober 2019 Br J Cardiol 2019;26:145–8 doi :10.5837/bjc.2019.035
Clinical CMR: one-year case mix, outcomes and stress-testing accuracy from a regional tertiary centre
Protik Chaudhury, Min Aung, Rossella Barbagallo, Edward Barden, Swamy Gedela, Stuart J Harris, Henry O Savage, Jason N Dungu
| Full textOctober 2019 Br J Cardiol 2019;26:137–40 doi :10.5837/bjc.2019.036
PCSK9 inhibitors in familial hypercholesterolaemia: a real-world experience and a meta-analysis
Harshal Deshmukh, Deepa Narayanan, Maria Papageorgiou, Yvonne Holloway, Sadaf Ali, Thozhukat Sathyapalan
| Full textOctober 2019 Br J Cardiol 2019;26:159–60 doi :10.5837/bjc.2019.037
Atypical presentation of STEMI with pericardial effusion causing cardiac tamponade related to malignancy
Matthew J Johnson, Rohan Penmetcha
| Full textSeptember 2019 Br J Cardiol 2019;26:99–100 doi :10.5837/bjc.2019.028
My 60-year relationship with aortic stenosis
Anthony P C Bacon, Harry Rosen, Neil Ruparelia
| Full text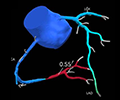
September 2019 Br J Cardiol 2019;26:105–9 doi :10.5837/bjc.2019.029
CT coronary angiography with HeartFlow®: a user’s perspective
Paul Brady, Andrew Kelion, Tom Hyde, Edward Barnes, Hazim Rahbi, Andy Beale, Steve Ramcharitar
| Full textSeptember 2019 Br J Cardiol 2019;26:114–8 doi :10.5837/bjc.2019.030
Coronary artery bypass angiography: the exception to the radial access rule?
Amir Orlev, Amna Abdel-Gadir, Graeme Tait, Jonathan P Bestwick, David S Wald
| Full text
