Cardiac tamponade and myocardial infarction (MI) are rare as the initial presentation of a malignancy. ST-elevation myocardial infarction (STEMI) and cardiac tamponade have been described to present together in the setting of a type-A aortic dissection causing coronary malperfusion. We describe a case with an atypical presentation of an MI due to a thrombus in the right coronary artery occurring simultaneously with a pericardial effusion causing tamponade physiology, related to malignancy. We present this unique case of MI and cardiac tamponade as it was not caused by a type-A aortic dissection. We suggest that malignancy be considered in the differential diagnosis when these findings present together.
Introduction
Cardiac tamponade and myocardial infarction (MI) are rare as the initial presentation of a malignancy. Lung cancer is among the most common sites from which cardiac metastases arise.1,2 The majority of cases of neoplastic pericardial disease are not detected or diagnosed antemortem due to the usual lack of clinical symptoms.3 Cardiac metastases most commonly occur between ages 50 and 70 years, notably via lymphatic and haematogenous dissemination.4,5 Tumour cells also have the ability to activate the coagulation system causing a prothrombic or hypercoagulable state to develop throughout the course of malignancy.6
Case
A 57-year-old man with a past medical history of hypertension, hyperlipidaemia, tobacco abuse of over 45 years, anaemia, infra-renal abdominal aortic aneurysm with a chronic mural thrombus, and a skin lesion on his nose presented with shortness of breath of two months’ duration, productive cough with clear-white sputum, and recent 20-pound weight loss.

His electrocardiogram (ECG) showed an acute inferior ST-elevation myocardial infarction (STEMI) with possible right ventricular (RV) involvement (III>II), and although troponins were initially trending downward, they began to trend upward. His echocardiogram showed that he had a large pericardial effusion with tamponade physiology (figure 1). After diagnosis of the STEMI with cardiac tamponade, the patient underwent computed tomography angiography (CTA) to rule out aortic dissection prior to pericardiocentesis and catheterisation.
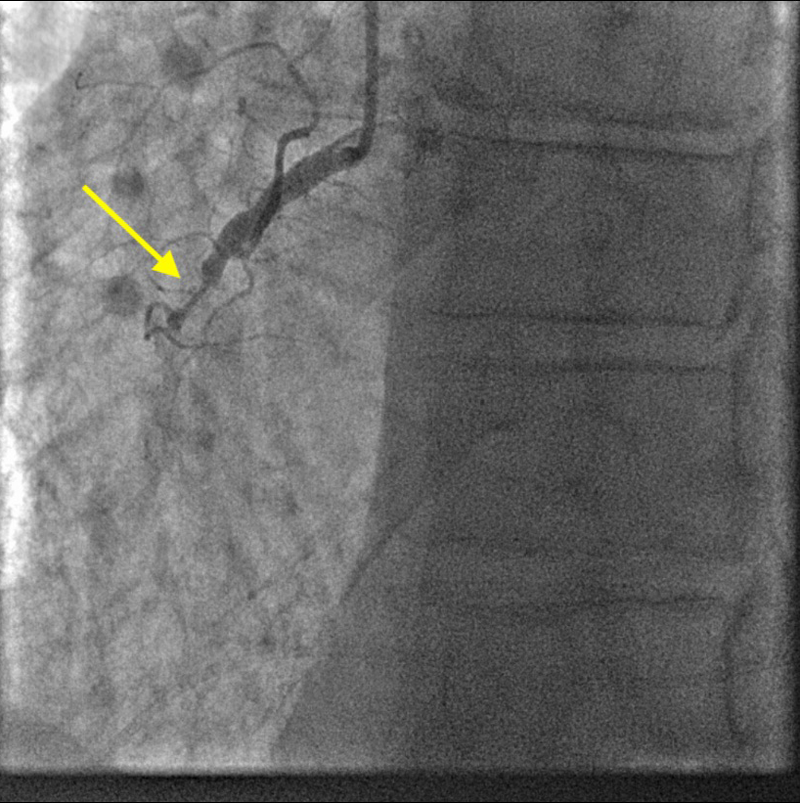
The CTA came back negative for aortic dissection, but showed that he had a medial right upper lobe spiculated lung nodule measuring 1.2 × 1.4 × 1.2 cm. Pulmonology and Oncology colleagues were consulted, and he was sent to the catheterisation lab where he underwent pericardiocentesis and placement of a drainage tube that drained 1,190 ml of sanguineous fluid at the time of the puncture. Immediately following the pericardiocentesis, percutaneous coronary intervention (PCI) was performed and a drug-eluting stent was placed in the mid-right coronary artery, which was found to be 100% occluded (figure 2). The patient remained hypotensive, had RV hypokinesis, and had fluid re-accumulation in the pericardium. Cardiothoracic surgery then placed a pericardial window and chest tube for continued drainage of fluid.
The pathology of the biopsy of the pericardium reported positive for scant adenocarcinoma with lymphovascular invasion. The pericardial fluid was thyroid transcription factor 1 (TTF1) positive, favouring pulmonary origin.
The patient progressed and the chest tube was discontinued. A repeat echocardiogram did not show any significant effusion. He desaturated enough to require home oxygen. He was discharged with a strong recommendation for outpatient follow-up with concern for malignancy and continued work-up of such.
Discussion
It is curious that the patient had both an MI and pericardial effusion with tamponade physiology at the same time. Metastases to the heart are rare, as are MI and cardiac tamponade in the setting of metastatic cancer as the initial presentation.1,2,7 Usually this presentation is consistent with a type-A aortic dissection affecting the coronary artery by causing coronary malperfusion along with pericardial effusion and tamponade.8 This was considered and ruled out in this patient, making this a very unusual presentation. To our knowledge, this is the first reported case of a STEMI due to thrombus formation with pericardial effusion causing tamponade physiology related to malignancy.
Conclusion
It is hypothesised that the patient likely had undiagnosed lung cancer leading to metastatic spread to the heart causing pericardial effusion and tamponade. It is suspected that the patient had an MI due to the prothrombotic nature of his lung malignancy. We present this unique case of MI and cardiac tamponade as this was not caused by a type-A aortic dissection. We suggest that malignancy be considered in the differential diagnosis when these findings present together.
Key messages
- This is a rare case of malignancy initially presenting as concurrent ST-elevation myocardial infarction (STEMI) and cardiac tamponade
- This presentation is typically associated with type-A aortic dissections
Conflicts of interest
None declared.
Funding
None.
Consent
The authors have received written patient consent to publish this case report.
References
1. Ben-Horin S, Bank I, Guetta V, Livneh A. Large symptomatic pericardial effusion as the presentation of unrecognized cancer: a study in 173 consecutive patients undergoing pericardiocentesis. Medicine (Baltim.) 2006;85:49–53. https://doi.org/10.1097/01.md.0000199556.69588.8e
2. Navi BB, Reiner AS, Kamel H et al. Arterial thromboembolic events preceding the diagnosis of cancer in older persons. Blood 2008;133:781–9. https://doi.org/10.1182/blood-2018-06-860874
3. Letonja M, Debeljak A. Cardiac tamponade as the initial manifestation of pulmonary adenocarcinoma. Radiol Oncol 2007;41:161–5. https://doi.org/10.2478/v10019-007-0025-6
4. Reynen K, Kockeritz U, Strasser RH. Metastases to the heart. Ann Oncol 2004;15:375–81. https://doi.org/10.1093/annonc/mdh086
5. Chiles C, Woodard PK, Gutierrez FR, Link KM. Metastatic involvement of the heart and pericardium: CT and MR imaging. Radiographics 2001;21:439–49. https://doi.org/10.1148/radiographics.21.2.g01mr15439
6. Caine GJ, Stonelake PS, Lip GY, Kehoe ST. The hypercoagulable state of malignancy: pathogenesis and current debate. Neoplasia 2002;4:465–73. https://doi.org/10.1038/sj.neo.7900263
7. Abraham KP, Reddy V, Gattuso P. Neoplasms metastatic to the heart: review of 3314 consecutive autopsies. Am J Cardiovasc Pathol 1990;3:195–8.
8. Erbel R, Alfonso F, Boileau C et al. Task Force on Aortic Dissection, European Society of Cardiology. Diagnosis and management of aortic dissection. Eur Heart J 2001;22:1642–81. https://doi.org/10.1053/euhj.2001.2782

