Despite the major role of primary care in the management of people with, or at risk of developing, cardiovascular disease, little is known about the availability and state of readiness of cardiovascular diagnostic and monitoring equipment in general practice premises. We surveyed 170 general practices in one cardiac network. Our findings suggest that both provision of cardiac equipment, and training of staff in its use, is variable.
Background
Cardiovascular diseases are the most common cause of premature death in developed countries. The National Service Framework for Coronary Heart Disease (NSF CHD)1 sets out national standards for the prevention, diagnosis and treatment of CHD including explicit recognition of the role of primary care teams. A further NSF chapter ‘Arrhythmias and sudden cardiac death’ was published in 2005,2 emphasising that patients with long-term conditions may be managed in primary care. It also highlighted better access to effective management of arrhythmias in all areas, including primary care.
Cardiovascular diagnostic and monitoring equipment is therefore required in the primary care setting. There has been significant investment in cardiac services since the introduction of the NSF CHD, enabling primary care teams to receive funding for equipment, although tracking of expenditure on equipment has proven difficult and it is unclear what cardiac equipment is currently available in primary care.
Once equipment has been purchased and installed there is a need for appropriate maintenance and training to ensure optimal use and patient safety. However, with the exception of resuscitation equipment, no national guidelines or standards regarding equipment maintenance and training within primary care premises were identified in a literature search.
Guidelines on recommended equipment for resuscitation in primary care have been published by the Resuscitation Council (UK).3 These suggest that each primary care organisation (PCO) should designate a named person responsible for co-ordinating resuscitation services at both PCO and practice level. Training should be undertaken “…to a level appropriate to the individual’s expected role”.2
We found few peer-reviewed or authoritative recommendations for the extent of provision of cardiac equipment such as 12-lead electrocardiogram (ECG) machines, Holter monitors or blood pressure (BP) monitors (static or ambulatory) in primary care, nor were we able to identify local guidance from primary care trusts (PCTs) on provision of resuscitation equipment. While an informal ‘Google’ search yielded examples of internal PCT reports, there were no peer-reviewed reports of audit of cardiac equipment and training in primary care. With practice-based commissioning (PBC) in development at the time of the survey, the extent to which PBC ‘clusters’ were facilitating direct access to these investigations in local hospitals across the network was unknown.
In order to obtain baseline information to inform future requirements and planning, together with development of appropriate care pathways, Coventry and Warwickshire Cardiac Network commissioned a survey on behalf of local PCTs on the provision of cardiac equipment, including maintenance and training arrangements, available in general practice premises.
Aims
To assess the availability and state of readiness of 12-lead ECG machines, ambulatory ECG (Holter) monitors, static and ambulatory BP monitors and defibrillators in general practice premises, with a view to making recommendations for future provision, maintenance and training.
Methods
A structured questionnaire was mailed to each of 170 practices identified by the Cardiac Network, which serves a population of 840,000 people across two PCTs established in Spring 2006. Within the network, Coventry and North Warwickshire are spearhead areas, being in the lower quintile nationally for deprivation and premature death from heart disease in males aged 75 and under. Over the next 15 years the population in the age groups with the highest prevalence of cardiovascular disease is expected to increase by around 25%. Where GPs work from multiple premises, all were sent a questionnaire. Consent to participate was assumed via return of the completed questionnaire and ethical approval was not required on the advice of a local PCT research department. To increase return rate, a generic reminder was issued two weeks after initial distribution, and a further final reminder issued after four weeks. Data were analysed using SPSS version 12.0 (SPSS Inc., Chicago, USA).
Results
Seventy-five (44%) completed responses were returned for analysis. An additional six invalid responses were received and excluded. Of the questionnaires returned 43 (57%) were completed by practice nurses, 19 (25%) by practice managers and 13 (17%) by general practitioners (GPs). Of responding practices, 61 (82%) were multiple partner and 13 (18%) single partner.
Thirty-four (45%) indicated that they currently had defibrillators. Of these, 18 (53%) had been purchased within the previous five years, eight (24%) were purchased more than five years ago and eight (24%) practices did not specify. In 28 (82%) practices there was a person identified as responsible for the state of readiness of the defibrillator, which in 22 (65%) cases was the practice nurse. Of 34 defibrillators, six (18%) were reported as having been used in a clinical emergency.
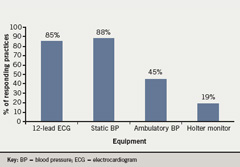
Some form of cardiac equipment was present in all 75 responding practices (figure 1).
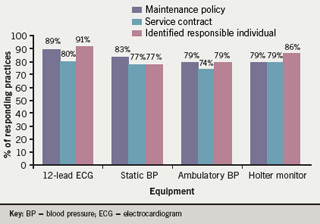
Practices were asked whether they had a service contract, maintenance contract and an identified responsible individual for the specified equipment (figure 2). Service contract providers included local hospitals and equipment suppliers.
Respondents indicated that in the majority of practices, practice nurses are the group of staff that are most likely to be responsible for the equipment on a day-to-day basis.
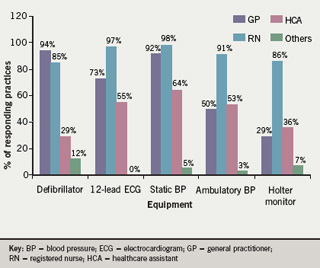
Staff trained in equipment use are shown in figure 3. Training updates were not provided for defibrillators in six practices (18%), 12-lead ECG in 20 practices (31%), static BP in 26 practices (39%), ambulatory BP in 21 practices (62%) and Holter monitors in 10 practices (71%). Responding practices indicated that staff require additional training in the following equipment: defibrillator 18 (53%), 12-lead ECG 17 (27%), static BP 3 (5%), ambulatory BP 11 (32%), and Holter monitor 8 (57%).
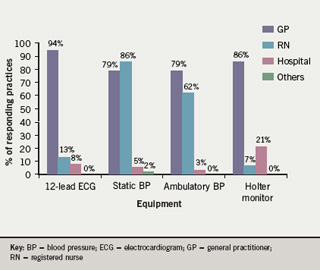
Respondents were asked which practice members were responsible for diagnostic interpretation (figure 4).
Discussion
Our findings demonstrate heterogeneity in provision of cardiac equipment and associated training and service arrangements in primary care. We did not obtain information on practices that did not respond to the survey and therefore are unable to determine how they might differ from those that did participate.
Defibrillators
Defibrillators are the only cardiac equipment for which authoritative guidance on use in primary care is available. Although there is no statutory legal requirement under English or Welsh law to provide a defibrillator, there are implications under common law if adequate safeguards are not provided to protect the public within a facility. Automated external defibrillators (AEDs) may be appropriate in the primary care environment due to ease of use, but installing them in every practice carries cost implications.
Where practices reported having a defibrillator, 10 (29%) had healthcare assistants (HCAs) trained in their use and four (12%) acknowledged another category such as receptionists and pharmacists. Over half (18, 53%) reported no training updates for any staff. Poor skill retention following resuscitation training for nursing and medical staff is well documented.4 Initial training improves performance of skills but regular updates are required to retain proficiency.5 A training needs assessment is required to determine deficits in use and diagnostic interpretation of cardiac equipment. Communication regarding equipment maintenance and training should occur via the practice nurse/practice manager based on the results of the survey, which indicated that these were the practice members most likely to be responsible for the equipment’s state of readiness.
12-lead ECGs
Most responding practices (64, 85%) had 12-lead ECG machines and 58 (91%) used these on a weekly or more frequent basis. Eighty per cent of these machines had a service contract and an identified responsible individual within the practice to oversee this role.
Interestingly, respondents indicate that a higher proportion of registered nurses (RNs) (64, 97%) had received formal training in the use of ECG machines compared with GPs (47, 73%), although interpretation of ECG recordings is predominantly undertaken by GPs (60, 94%) rather than RNs (8, 13%). While there have been earlier consensus-based recommendations on ECG interpretation, substantive evidence on the training required to obtain and sustain competence in ECG interpretation is not available.6 Seventeen (27%) respondents reported that their practice members require additional training in 12-lead ECG use.
Static BP, ambulatory BP and Holter monitors
Sixty-six (88%) practices had static BP machines with a high proportion of practice staff trained in their use. BP recording is one of the most common measurements carried out in primary care, but it is often measured incorrectly. Health professionals taking BP measurements need adequate initial training and periodic review of their performance.7 A significant minority of staff (26, 39%) were not offered training updates, with only three (5%) practices considering this necessary. We did not seek to distinguish between mercury or other types of static BP equipment.8
Thirty-four practices (45%) possessed ambulatory BP machines, with 31 (91%) having RNs that were trained in their use. This finding is unexpected given National Institute of Health and Clinical Excellence (NICE) guidelines which state that routine use of automated ambulatory BP monitoring or home monitoring devices in primary care is not recommended because their value has not been adequately established.7 This raises the possibility that there may have been some confusion about the terminology used in the questionnaire. It is possible that respondents may have interpreted ‘ambulatory’ as ‘portable’. Surprisingly, 14 practices (19%) indicated that they possessed Holter monitors, with 12 (86%) of these practices indicating that RNs were responsible for interpretation of data. This is a specialist role usually undertaken in the hospital setting. These findings should therefore be treated with caution.
Conclusion
Provision of cardiac equipment in general practice premises is variable. Where equipment is available, service and maintenance provision is provided through a variety of sources and training policies appear inconsistent.
Acknowledgements
We thank Molly Gilchrist, Principal Lecturer at Coventry University, for her statistical support and Rachael Rowe, Director of the Coventry & Warwickshire Cardiac Network.
Conflict of interest
Funding for the study was provided by the Coventry and Warwickshire Cardiac Care Network and Coventry University via a Knowledge Transfer Enterprise Grant.
Key messages
- In the absence of national guidelines on provision of cardiac equipment in primary care, there is a need to develop guidelines (taking into account population characteristics, list size and availability of resources)
- Since management of cardiac equipment is nearly always undertaken in the majority of practices by non-medical staff, it would seem appropriate for communication to be via practice nurses/practice managers
- Training needs analysis is required in resuscitation and 12-lead ECG interpretation. Auditing of diagnostic interpretation and related findings should be performed
References
- Department of Health. National Service Framework for coronary heart disease. London: Department of Health, 2000.
- Department of Health. National Service Framework for coronary heart disease. Chapter 8: arrhythmias and sudden cardiac death. London: Department of Health, 2005.
- Resuscitation Council (UK). Guidance for clinical practice and training in primary care. London: Resuscitation Council (UK), 2001.
- Hamilton R. Nurses’ knowledge and skill retention following cardiopulmonary resuscitation training: a review of the literature. J Adv Nurs 2005;51:288–97.
- Woollard M, Whitfield R, Smith A et al. Skill acquisition and retention in automated external defibrillator (AED) use and CPR by lay responders: a prospective study. Resuscitation2004;60:17–28.
- Salerno SM, Alguire PC, Waxman HS. Training and competency evaluation for interpretation of 12 lead electrocardiograms: recommendations from the American College of Physicians.Ann Intern Med 2003;139:747–50.
- National Institute for Health and Clinical Excellence. Hypertension. Management of hypertension of adults in primary care. London: NICE, 2006.
- Report of the Independent Advisory Group on blood pressure monitoring in clinical practice. June 2005. Available from: www.mhra.gov.uk [accessed 18/07/07].

