A clinical audit of ezetimibe in the treatment of refractory hyperlipidaemia was conducted in 100 high-risk patients who failed to achieve desirable levels of total and low-density lipoprotein (LDL)-cholesterol on statins. Of these, 59 had familial hypercholesterolaemia (FH), the remainder had other aetiologies (non-FH). The percentage of patients achieving the total and LDL-cholesterol targets of the International Panel on the Management of FH or the Second Joint British Societies’ guidelines in non-FH patients was determined.
Ezetimibe significantly decreased mean LDL-cholesterol when used as an adjunct to statins or as monotherapy, from 3.9 to 3.1 mmol/L in FH, from 3.4 to 2.4 mmol/L in non-FH and from 6.0 to 4.4 mmol/L in statin-intolerant patients. The decrease in LDL-cholesterol on statins was inversely correlated with the decrement after adding ezetimibe (r= -0.67, p<0.0001) but 15% of patients showed no further decrease. The percentage of patients achieving target levels of LDL-cholesterol was 27% on statins and 63% on statins plus ezetimibe (p<0.007). None of the non-FH patients achieved target levels on statins but 33% did so when ezetimibe was added (p<0.001).
Ezetimibe is an effective adjunct to statins for lowering LDL-cholesterol in refractory hyperlipidaemia, except in a minority of patients, and is a useful substitute in statin-intolerant subjects.
Introduction
About 10 million deaths in the world are caused each year by coronary heart disease (CHD) and stroke.1 Comparative statistics in Britain2 are on a smaller scale but in relative terms, similar. Total mortality in the UK is approximately 600,000 annually, 36% of which is due to cardiovascular disease. Half of the latter is from CHD, a quarter from stroke and it is the main cause of premature mortality in both men and women. Recently it was estimated that the major modifiable risk factor, raised serum cholesterol, accounted for 45% of all myocardial infarcts in Western Europe.3
The introduction of statins 20 years ago has revolutionised the management of hypercholesterolaemia and the prevention of cardiovascular disease. In the Cholesterol Treatment Trialists’ Collaborators’ meta-analysis the mean reduction in low-density lipoprotein (LDL)-cholesterol in subjects on statins was 29%, which was associated with a 21% decrease in coronary mortality.4 It was suggested that decreasing LDL-cholesterol by 50%, achievable with high doses of atorvastatin and rosuvastatin, could reduce the risk of coronary disease by 40% but this would still leave the majority of those on treatment vulnerable.
The recent introduction of the cholesterol absorption inhibitor, ezetimibe, offers an alternative to statin monotherapy.5 Combining ezetimibe with a statin augments the latter’s LDL-lowering efficacy by an additional 15–20% and theoretically should achieve a reduction in CHD risk of similar magnitude, additional to that from statin alone. The effects of ezetimibe on cardiovascular disease remain to be determined but its use to treat hypercholesterolaemic patients who are intolerant of, or refractory to, statins has recently been endorsed by the National Institute for Health and Clinical Excellence (NICE).6 Here we describe a clinical audit of the role of ezetimibe in the management of such patients undergoing routine out-patient care in a hospital setting.
Subjects and methods
Subjects
One hundred patients with primary hypercholesterolaemia and CHD or at high risk of developing the latter who were attending the Lipid Clinic at Hammersmith Hospital participated in the audit. They were selected serially on the basis of failing to achieve, what were considered at the time to be, desirable lipid levels7 (total cholesterol [TC] <5 mmol/L, LDL-cholesterol <3 mmol/L) on maximally tolerated doses of statins, therefore being eligible for ezetimibe. Of these, 92 patients received ezetimibe 10 mg daily in addition to a statin, commonly atorvastatin 40–80 mg daily, while eight statin-intolerant patients took ezetimibe 10 mg daily alone. All patients received lifestyle advice, including the dietary use of plant stanols and sterols, and all were on ezetimibe for at least three months before analysis of serum lipids and safety parameters.
Fifty-nine patients had familial hypercholesterolaemia (FH), the diagnosis being made on Simon Broome criteria.8 A genetic defect was identified in 49 of these patients, 26 of whom were LDL-receptor negative, 16 were LDL-receptor defective and seven had familial defective apolipoprotein B (FDB). None carried the PCSK9 mutation. The remaining 41 patients had diagnoses of familial combined hyperlipidaemia or polygenic types IIa and IIb hyperlipidaemia. None of the statin-intolerant patients had FH.
Study design
The main objective of this clinical audit was to compare, in the three groups of patients, the results of the initial pre-treatment lipid profile carried out at the time of referral with the results obtained either on statin or ezetimibe monotherapy and also, except for statin-intolerant patients, with those obtained on statin/ezetimibe combination therapy. The percentage of patients achieving target levels of total and LDL-cholesterol after the addition or substitution of ezetimibe was then calculated. Target values for primary and secondary prevention were those recommended by Civeira et al.9 for FH patients and those stipulated in the second Joint British Societies’ guidelines (JBS-2)10 for non-FH patients. Cardiovascular risk was calculated in FH and non-FH patients without clinical evidence of cardiovascular disease according to the appropriate guidelines.
Analytical methods
Serum TC and triglycerides (TG) were measured enzymatically using cholesterol esterase and glycerolphosphate oxidase, respectively. High-density lipoprotein (HDL)-cholesterol was measured in serum after addition of surfactants and detergents followed by cholesterol oxidase. LDL-C was calculated in patients with serum TG <4.5 mmol/L using the Friedewald equation. Liver and renal function were assessed by measurement of serum alanine transferase (ALT) and serum creatinine, respectively.
Mutations in the LDL-receptor were identified by performing sequence analysis of all 18 exons of the LDL-receptor gene, as reported elsewhere.11 Functionality has been confirmed for all mutations. The A3500G mutation of FDB was identified by sequencing of the apolipoprotein B100 gene.
Statistical methods
Changes in absolute levels of serum lipids were compared using a paired t-test. The effectiveness of statin and ezetimibe treatment was determined by the percentage changes in LDL-cholesterol compared with pre-treatment levels at presentation. Stepwise multi-variate regression was performed to determine the relationship between the effectiveness of statin treatment with the subsequent effectiveness of adding ezetimibe, using age, gender, body mass index and FH status as co-variates. A two-tailed McNemar’s test with the exact binomial probability was used to assess whether ezetimibe increased the number of patients achieving the appropriate targets. The null hypothesis was rejected at a two-tailed p<0.05.
Results
Clinical characteristics of subjects
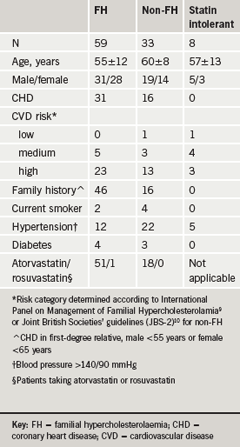
The majority of patients had heterozygous FH, as shown in table 1. More than half of these had CHD and most of the remainder were classified as being at high risk of cardiovascular disease. Most FH patients were receiving atorvastatin 40–80 mg daily. Non-FH patients were older than those with FH and just under half had CHD. Most of the remainder were in the high-risk category, many of whom had hypertension, diabetes and/or a family history of CHD. Slightly more than half of these non-FH patients were on atorvastatin. None of the statin-intolerant patients (all non-FH) had CHD but most were at medium or high risk of cardiovascular disease. All told, only two patients were in the low-risk category, one with a serum cholesterol of >9 mmol/L, the other with a raised lipoprotein (a).
Serum lipids
Table 2 shows baseline values of serum lipids and changes on treatment in FH and non-FH patients. As would be expected, FH patients had higher pre-treatment levels of total and LDL-cholesterol and higher total:HDL-cholesterol ratios. The mean percentage reduction in LDL-cholesterol on statins was greater in FH than in non-FH patients (50.3% vs. 35.6%) probably reflecting the fact that a higher proportion of the former were on high doses of atorvastatin or rosuvastatin.
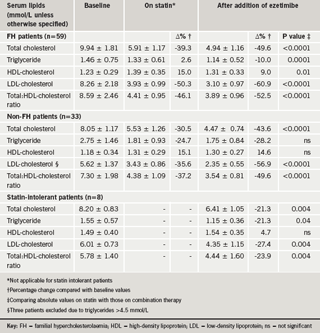
The addition of ezetimibe to statin therapy in FH patients caused significant decreases in total and LDL-cholesterol, TG and the total:HDL-cholesterol ratio compared with statins alone and reduced LDL-cholesterol by over 60% from baseline. No significant differences were seen between receptor-negative, receptor-defective and FDB subjects, respectively, in the decrease in LDL-cholesterol on statins (49.6%, 53.3% and 52.8%) or on statins plus ezetimibe (60.4%, 62.6% and 61.5%).
In non-FH patients addition of ezetimibe to statin therapy significantly decreased total and LDL-cholesterol and the total:HDL-cholesterol ratio compared with statins alone and decreased LDL-cholesterol by almost 57% from its baseline value.
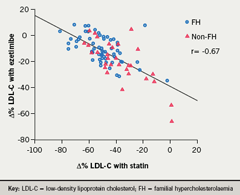
As shown in figure 1 there was a highly significant inverse correlation between percentage reductions in LDL-cholesterol on statin and the percentage changes resulting from the addition of ezetimibe. On multi-variate analysis, this relationship was independent of age, gender, body mass index and the presence of FH (data not shown).
The effect of ezetimibe monotherapy in the eight statin-intolerant patients, as shown in table 1, was to cause significant decreases in total and LDL-cholesterol, TG and the total:HDL-cholesterol ratio, with the decrease in LDL-cholesterol averaging 27%.
Attainment of LDL targets
The number of FH patients achieving the International Panel on the Management of FH targets for LDL-cholesterol (<3.4 mmol/L or 50% reduction if at moderate risk, <2.6 mmol/L or 60% reduction if at high risk) on statin monotherapy was 16 (27%) compared with 37 (63%) on statin plus ezetimibe (p=0.007). None of the non-FH patients achieved JBS-2 targets for cholesterol (TC <4 mmol/L and LDL-cholesterol <2 mmol/L or >25% reduction in TC and >30% reduction in LDL-cholesterol) on statin alone but nine (30%) did so when ezetimibe was added (p=0.001). None of the statin-intolerant patients achieved JBS-2 targets on ezetimibe.
Hepatic and renal function
Addition of ezetimibe to ongoing statin treatment resulted in a mean increase in serum ALT from 30.9 to 34.5 IU/L (p<0.01). All patients remained asymptomatic and none had an elevation of ALT greater than three times the upper limit of normal. No significant changes in serum creatinine occurred.
Discussion
Ezetimibe, a cholesterol absorption inhibitor, and statins, which reduce cholesterol synthesis, have additive effects in lowering serum cholesterol, as was reviewed recently.12 In published studies involving patients with FH the combination of ezetimibe and statin therapy resulted in overall reductions in LDL-cholesterol of 56%13 and 57%,14 respectively, similar to the 60% decrease which we observed. In another, larger trial where more than half the subjects had FH and the remainder had CHD or were at high risk, as was the case in this audit, the percentage of patients who achieved an LDL-cholesterol ≤2.6 mmol/L after the addition of ezetimibe to atorvastatin was threefold greater than after doubling the dose of statin.15 A similar increase in the proportion of FH and non-FH patients who reached their LDL target when ezetimibe was added to ongoing statin therapy was evident in our audit. In addition the 27% decrease in LDL-cholesterol and 21% decrease in TG that we observed in eight statin-intolerant patients treated with ezetimibe alone were remarkably similar to the 30% and 20% decreases in LDL-cholesterol and TG, respectively, reported previously in 50 statin-intolerant patients.14 The fact that our results were so closely comparable with those obtained by others under clinical trial conditions suggests that despite the uncontrolled nature of the audit, drug compliance was similar.
As first reported by Pisciotta et al.14 in FH patients, we found an inverse correlation between the magnitude of the decrease in LDL-cholesterol on statins and the decrement in LDL-cholesterol attributable to the addition of ezetimibe. The lesser the response to statins, the better the response to ezetimibe and vice versa. This relationship was apparent both in FH and non-FH patients and suggests that ezetimibe was most effective in subjects who had <40% reduction in LDL-cholesterol on a statin, but much less effective in those who achieved a >60% decrease. In 15% of patients the addition of ezetimibe either had no effect or diminished the LDL-lowering effect of statins. These findings indicate that ezetimibe is most effective in patients who respond poorly to statin monotherapy and suggest that its impact on LDL-cholesterol should be checked within three months of starting the drug. Like Pisciotta et al.14 we observed no difference between the response of LDL-receptor negative and defective patients to combination therapy and we confirmed their observation that ezetimibe monotherapy decreased LDL-cholesterol by approximately 30% and TG by 20% in statin-intolerant subjects.
It has recently become apparent that genetic factors regulating cholesterol absorption play an important role in determining inter-individual variability in the response to ezetimibe and, indirectly, to statins. Niemann-Pick C1-like 1 (NPC1L1) encodes the intestinal sterol transporter, which mediates cholesterol absorption and is inhibited by ezetimibe. Several studies14,16,17 have shown that genetic polymorphism of NPC1L1 influences the extent to which LDL-cholesterol is decreased by ezetimibe; subjects with DNA sequence variants associated with efficient cholesterol absorption exhibit the best response. In contrast, such individuals respond poorly to statins, probably because efficient cholesterol absorption results in down-regulation of hepatic hydroxymethylglutaryl coenzyme A (HMG CoA) reductase, the target of statins. In this context we have previously shown that FH patients with a high rate of cholesterol synthesis, reflecting up-regulation of HMG CoA reductase, respond better to statins than those with a low rate of cholesterol synthesis.18 Hence, the efficiency with which cholesterol is absorbed plays a key role in determining not only the response of individuals to ezetimibe but also, by regulating hepatic HMG CoA reductase activity, their responsiveness to statins.
It has not been established whether the greater reduction in LDL-cholesterol resulting from combining ezetimibe with statins will result in increased clinical benefit. At present the only evidence relating to this issue comes from the Effect of Ezetimibe Plus Simvastatin Versus Simvastatin Alone on Atherosclerosis in the Carotid Artery (ENHANCE) trial, which used a surrogate marker of atherosclerosis to determine outcome. This double-blind, multi-centre study compared the anti-atherosclerotic effects of simvastatin 80 mg and simvastatin 80 mg plus ezetimibe 10 mg daily in over 600 patients with heterozygous FH. The primary end point was change in carotid intima-medial thickness (IMT) after two years, as measured by ultrasound.19 The suitability of using changes in carotid IMT as an index of progression of atherosclerosis in ENHANCE has been discussed in detail by Brown et al.,20 who pointed out that baseline values of carotid IMT were surprisingly normal for patients with FH. This probably reflects the fact that 80% had been on intensive long-term lipid-lowering therapy prior to the study, which would tend to reverse any previous accumulation of cholesterol in the vessel wall and make it harder to ascertain the effects of subsequent treatment.
The results showed that LDL-cholesterol was reduced by 41% by simvastatin versus 58% by simvastatin plus ezetimibe. Corresponding changes in IMT were increases of 0.0058 mm and 0.0111 mm, respectively; the difference between the treatment groups was not significant. The question has been raised of whether the apparent lack of benefit from ezetimibe in ENHANCE was due to the fact that it lowers LDL by a different mechanism from statins and therefore lacks their pleiotropic effects. The latter include improved endothelial function and anti-inflammatory properties. However, it is debatable whether these actions are genuinely independent of the LDL-lowering effect of statins and, if so, whether they make any additional contribution to the reduction in clinical events.21 A meta-analysis, which compared trials conducted in the pre-statin era, using diet, bile acid sequestrants and partial ileal bypass, with trials using statins, showed that in both instances the reduction in cardiovascular risk was directly proportional to the extent of reduction of LDL-cholesterol.22 In other words, the pleiotropic effects of statins did not appear to contribute any additional benefit. Bile acid sequestrants and ezetimibe both up-regulate HMG CoA reductase, so neither can exert the LDL-independent pleiotropic effects attributed to statins, which reflect inhibition of HMG CoA reductase. Hence, the argument that the negative outcome of ENHANCE was due to the absence of these pleiotropic effects lacks credibility. So too do calls to withdraw or withhold ezetimibe from patients on the basis of this result, especially since there was no increase in adverse events when it was combined with simvastatin. Clearly, the results of a large clinical outcome trial now underway (Improved Reduction of Outcomes: Vytorin Efficacy International Trial [IMPROVE-IT]) are needed before this controversial issue can be resolved but that will not be until 2011.23Until then achieving current LDL-cholesterol targets remains a valid strategy in which ezetimibe can play an important role when other approaches have failed.
Acknowledgements
We greatly appreciate assistance and support from Professors Tim Aitman and Anne Soutar, and also Isabella Tosi.
Conflict of Interest
MS has received a travel grant from Merck, Sharp and Dohme to attend a scientific meeting. RS, CN, SW, YT, GRT, RPN: none declared.
Key messages
- Ezetimibe is an effective therapeutic adjunct in hyperlipidaemic patients who do not achieve sufficient low-density lipoprotein (LDL)-cholesterol reduction on statins and a useful substitute in those who are statin-intolerant
- Subjects who respond least well to statins respond best to ezetimibe in terms of further LDL-reduction and vice versa
- The controversy surrounding the results of the ENHANCE trial should not be allowed to constrain the continuing use of ezetimibe as a means of achieving LDL targets in high-risk patients
References
- Murray CJ, Lopez AD. Mortality by cause for eight regions of the world: Global Burden of Disease Study. Lancet 1997;349:1269–76.
- Coronary heart disease statistics, 2007 edition. British Heart Foundation Statistics Database. Available from: www.heartstats.org
- Yusuf S, Hawken S, Ounpuu S et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet2004;364:937–52.
- Cholesterol Treatment Trialists’ (CTT) Collaborators. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90056 participants in 14 randomised trials of statins. Lancet 2005;366:1267–78.
- Knopp RH, Gitter H, Truitt T et al. Effects of ezetimibe, a new cholesterol absorption inhibitor, on plasma lipids in patients with primary hypercholesterolemia. Eur Heart J 2003;24:729–41.
- National Institute of Health and Clinical Excellence. Ezetimibe for the treatment of primary (heterozygous-familial and non-familial) hypercholesterolaemia. London: NICE, 2007. Available from: http://www.nice.org.uk/guidance/TA132
- Department of Health. National Service Framework for coronary heart disease. Preventing coronary heart disease in high risk patients. London: Department of Health, 2000.
- Scientific Steering Committee on behalf of the Simon Broome Register Group. Risk of fatal coronary heart disease in familial hypercholesterolaemia. BMJ 1991;303:893–6.
- Civeira F. International panel on management of familial hypercholesterolemia. Guidelines for the diagnosis and management of heterozygous familial hypercholesterolaemia. Atherosclerosis2004;173:55–68.
- Joint British Societies. JBS2: Joint British Societies’ guidelines on prevention of cardiovascular disease in clinical practice. Heart 2005;91:1–52.
- Tosi I, Toledo-Leiva P, Neuwirth C et al. Genetic defects causing familial hypercholesterolaemia: identification of deletions and duplications in the LDL-receptor gene and summary of all mutations found in the Hammersmith Hospital Lipid Clinic. Atherosclerosis 2007;194:102–11.
- Mikhailidis DP, Wierzbicki AS, Daskslopoulou SS et al. The use of ezetimibe in achieving low density lipoprotein lowering goals in clinical practice: position statement of a United Kingdom consensus panel. Curr Med Res Opin 2005;21:959–69.
- Pitsavos C, Skoumas I, Tousoulis D et al. The impact of ezetimibe and high-dose statin treatment on LDL levels in patients with heterozygous familial hypercholesterolemia. Int J Cardiol2008. doi:10.1016/j.ijcard.2007.12.065.
- Pisciotta L, Fasano T, Bellocchio A et al. Effect of ezetimibe coadministered with statins in genotype-confirmed heterozygous FH patients. Atherosclerosis 2007;194:e116–e122.
- Stein E, Stender S, Mata P et al. Achieving lipoprotein goals in patients at high risk with severe hypercholesterolaemia: efficacy and safety of ezetimibe coadministered with atorvastatin. Am Heart J 2004;148:447–55.
- Simon JS, Karnoub MC, Devlin DJ et al. Sequence variation in NPC1L1 and association with improved LDL-cholesterol lowering in response to ezetimibe treatment. Genomics2005;86:648–56.
- Hegele AH, Guy J, Ban MR, Wang J. NPC1L1 haplotype is associated with inter-individual variation in plasma low-density lipoprotein response to ezetimibe. Lipids Health Dis 2005;4:16–21.
- Naoumova RP, Marais AD, Mountney J et al. Plasma mevalonic acid, an index of cholesterol synthesis in vivo, and responsiveness to HMG CoA reductase inhibitors in familial hypercholesterolaemia. Atherosclerosis 1996;119:203–13.
- Kastelein JJP, Akdim F, Stroes ESG et al. Simvastatin with or without ezetimibe in familial hypercholesterolemia. N Engl J Med 2008;358:1431–43.
- Brown BG, Taylor AJ. Does ENHANCE diminish confidence in lowering LDL or ezetimibe? N Engl J Med 2008;358:1504–07.
- Futterman LG, Lemberg L. Statin pleiotropy: fact or fiction? Am J Crit Care 2004;13:244–9.
- Robinson JG, Smith B, Maheshwari N, Schrott H. Pleiotropic effects of statins: benefit beyond cholesterol reduction? A meta-regression analysis. J Am Coll Cardiol 2005;46:1855–62.
- Drazen JM, Jarcho JA, Morrissey S, Curfman GD. Cholesterol lowering and ezetimibe. N Engl J Med 2008;358:1507–08.

