Although peak TRV cannot be measured in every patient, the success in locating the jet is related to taking multiple views to find it. The following points should be remembered when calculating the sPAP.
- Doppler ultrasound can easily underestimate peak velocity if the ultrasound beam is not correctly aligned with the jet, which is often eccentric in pulmonary hypertension. It will not overestimate it.
- Right atrial pressure is estimated from the diameter of the inferior vena cava and its response to sharp inspiration or sniff (table).
- The estimated systolic PAP at echocardiography cannot be directly translated to mean PAP at cardiac catheterisation. This is because of the noise of the echocardiographic measurement and the lack of a reliable relationship between systolic and mean PAP. For this reason, there is no absolute cutoff level of peak velocity or estimated sPAP, which indicates PH.
- For guidance only, the ESC 2009 guidelines2 suggest that pulmonary hypertension is considered likely if the TRV is >3.4 m/s and PA systolic pressure > 50 mmHg, with or without additional echocardiographic variables that suggest this diagnosis. Diagnosis of PH is possible if TRV <=2.8 m/s, SAP <=36 mmHg but in the presence of other variables suggestive of PH; or with TRV 2.9-3.4 m/s and SAP 37-50 mmHg with or without additional echocardiographic variables (figure 6).
Other findings on echocardiography that suggest PH include:
- dilatation of right atrium and right ventricle
- increased right ventricular wall thickness
- flattening of the interventricular septum and compression of the left ventricle
- a dilated main pulmonary artery and mid-systolic closure of the pulmonary valve.
- functional tricuspid regurgitation may accompany right ventricular dilatation
- pericardial effusion may be observed in severe PH. This is a consequence of the pericardial space draining to the right atrium. In the presence of high right atrial pressure, pericardial effusion may form. CTD may also be associated with pericardial effusion.
- tissue Doppler imaging may also suggest PH.
- severe tricuspid regurgitation may result in the underestimation of peak tricuspid regurgitation velocity.
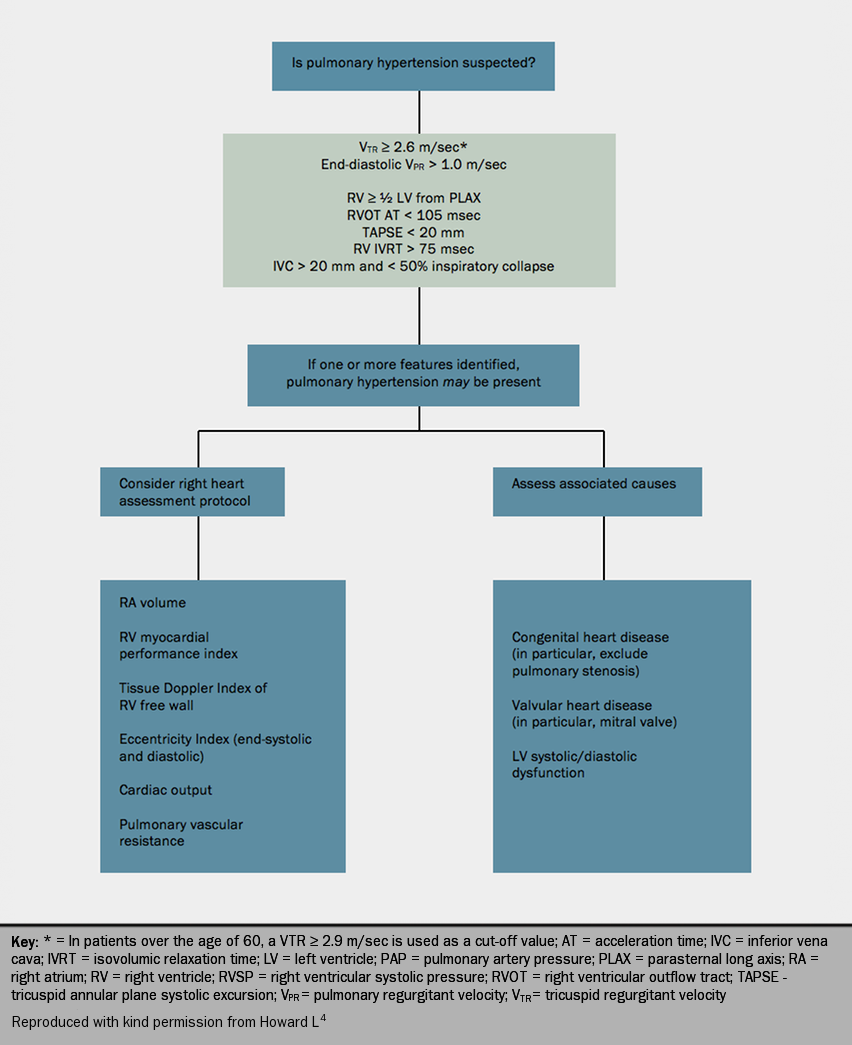
A protocol for the investigation of pulmonary hypertension using transthoracic echocardiography is shown in figure 7.4
Identification of conditions that predispose to PH
Echocardiography may identify the following conditions that predispose to PH:
- Valve disease such as mitral stenosis or mitral regurgitation
- Left ventricular systolic dysfunction
- Left ventricular diastolic function. For both systolic and diastolic dysfunction, always look carefully at left atrial size provided the patient is in sinus rhythm. A dilated left atrium in this situation indicates likely left ventricular or valve disease. Remember that the commonest cause of right ventricular failure is left ventricular failure.
- Congenital heart disease e.g. atrial septal defect (ASD), patent ductus arteriosus, ventricular septal defect. ASD is one of the most common conditions that is misdiagnosed as pulmonary hypertension. Echocardiography in suspected PH should always include detailed examination of the interatrial septum as well as a search for a sinus venosus defect. In some patients it may be necessary to use contrast echocardiography to confirm the diagnosis. A secundum ASD should be distinguished from a patent foramen ovale, which may become stretched in the presence of PH.


