Primary mitral regurgitation
This causes dilatation and hyperactivity of the left ventricle which in the long-term induces myocardial fibrosis with a consequent deterioration in contractile function. However, because the left ventricle empties partly into the left atrium which is at a lower pressure than the aorta, the LV ejection fraction or fractional shortening is normal until the terminal stages.71
An average time of 24 years from detection of murmur to presentation with symptoms has been shown72 and presentation with symptoms is more common in middle aged than younger patients. In a USA study of mitral valve prolapse, 10 year mortality was not significantly higher than in the general population: 91% were free of cardiovascular mortality at 10 years, with mortality predicted by LV ejection fraction <50%, and MR of moderate or greater severity.73 However the grade of regurgitation is worse with ruptured chordae leading to flail or partially flail leaflet segments. In these the mean 10 year survival without heart failure is only 37%.74
Left atrial enlargement secondary to the mitral regurgitation (see figure 10) is associated with paroxysmal or sustained atrial arrhythmias and if these are present there is an increased risk of thromboembolism for which anticoagulation with warfarin is indicated. The mean 10-year risk of atrial fibrillation is 30% with severe regurgitation as a result of a flail or partially flail leaflet.74 There is a 1-2.5% risk of sudden death.75
Infective endocarditis: Chronic mitral regurgitation is the underlying substrate in between 20 and 30% of cases of infective endocarditis.26
There is no convincing association between mitral valve prolapse and stroke76 in the absence of associated atrial fibrillation.77 Myxomatous valves could cause platelet aggregation or possibly thrombus formation78 although this remains uncertain.
Symptoms
Chronic MR may present with dyspnoea, palpitations and fatigue. The inability to increase cardiac output on exertion leads to shortness of breath, but overt cardiac failure may also occur. Atrial arrhythmias may themselves be symptomatic, or be unmasked by associated thrombo-embolic complications. In the later stages of the disease, pulmonary hypertension may lead to symptoms of right heart failure.
Signs
Murmur
There is a pansystolic murmur at the apex usually radiating to the axilla. However in mitral prolapse, anteriorly directed jets may be loudest at the base of the heart and posteriorly directed jets may be loudest in the back.
The amplitude is approximately related to the grade of regurgitation.45 If the regurgitation is mild and caused by prolapse, there may be a late systolic murmur sometimes preceded by a systolic click. Papillary muscle dysfunction can also result in a murmur late in systole. A musical or ‘seagull’ quality to the murmur occurs if there is a perforation or fluttering of a flail leaflet segment.
Diastolic sound
The diastolic sound is composed of a third heart sound sometimes succeeded by a mid-diastolic murmur caused by functional MS as a result of high flow in the presence of rheumatic disease.
Wide splitting of the second sound in severe mitral regurgitation is caused by early cessation of systole leading to an early aortic closure sound.
Other signs
The radial pulse is usually normal, although in severe chronic regurgitation there may be atrial fibrillation. There may be a parasternal impulse as a result of left atrial enlargement78 and in severe regurgitation the apex is displaced laterally.
Mitral regurgitation
Acute mitral regurgitation
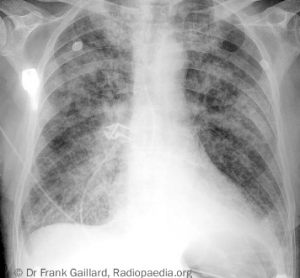
The adaptation to regurgitation does not have time to occur in acute MR, resulting in more fulminant symptoms. This is the case even in cases of pre-existing MR, such as with a flail segment resulting from chordal rupture in degenerative mitral valve disease.
Patients with acute severe MR present with sudden onset pulmonary oedema (see figure 11), and may be in cardiogenic shock. The cause may be clear, such as in papillary muscle rupture following myocardial infarction (MI), but when valve destruction results from IE, aetiology may be less evident. Symptoms of malaise, fevers and weight loss, and peripheral signs of IE may be discovered with appropriate clinical suspicion. When there is a known background of chronic MR, this should also prompt rapid assessment for acute deterioration in valve function.

