May 2019 Br J Cardiol 2019;26:59–62 doi:10.5837/bjc.2019.018
Sally Youssef, Mariam Ali, Kim Heathcote, Alistair Mackay, Chris Isles

Introduction Most patients presenting as an emergency with chest pain do not have myocardial infarction (MI),1 which must, nevertheless, be ruled out in order to reassure and discharge from hospital. High-sensitivity cardiac troponin T (hs-TnT) and troponin I (hs-TnI) have streamlined the assessment and management of chest pain, as a rapid rule out of MI is now possible, particularly if hs-TnT or hs-TnI are undetectable at presentation.2-8 Undetectable troponin cannot, however, be used to exclude unstable angina, which by definition is not associated with a troponin rise.9 It is for this reason that physicians and cardiologists may be reluct
May 2019 Br J Cardiol 2019;26:50
Gerald Chi, Syed Hassan Abbas Kazmi, C. Michael Gibson

ACC.19 was held in New Orleans, US PARTNER 3 and Evolut Low Risk add to evidence base for TAVR Prior literature suggests that transcatheter aortic-valve replacement (TAVR) is non-inferior or even superior to standard surgical aortic-valve replacement (SAVR) among high and intermediate surgical risk patients with aortic stenosis (AS). Two pivotal studies have now addressed the efficacy and safety of TAVR in AS patients at low mortality risk from surgery. PARTNER 3 (ClinicalTrials.gov: NCT02675114) was an open-label trial that randomised 1,000 subjects with severe AS at low mortality risk from surgery into either TAVR with a third-generation ba
October 2018 Br J Cardiol 2018;25:143–6 doi:10.5837/bjc.2018.028
Debjit Chatterjee, Priya Philip, Kay Teck Ling

Introduction We published three cases with electrocardiogram (ECG) manifestation of new-onset giant T-wave inversion and QT prolongation associated with significant left main/left anterior descending artery disease in 2015.1 Since this publication we prospectively looked for patients in coronary care and the cardiology ward in our hospital who were admitted with, or developed during hospital stay, the above ECG changes. We found 10 patients with similar ECG features between March 2016 and February 2018. Four cases were associated with significant left main stem and/or left anterior descending coronary artery disease. Two cases were due to Tak
January 2018 doi:10.5837/bjc.2018.004 Online First
Ruan Vlok, Joshua Wall, Hannah Kempton, Thomas Melhuish, Astin Lee, Leigh White

Figure 1. ST-elevation in aVR Introduction The variety of electrocardiogram (ECG) changes that occur following acute myocardial infarction (AMI), occur in concordance with coronary circulation anatomy. ST-segment elevation in lead aVR can indicate an anterior wall AMI.1,2 However, lead aVR is commonly neglected by clinicians,3 and as such, this may be a potential source of adverse patient outcomes. The aim of this single-centre study is to investigate how proficiently AMIs presenting with aVR ST-elevation are recognised, using ‘door-to-balloon times’ as an outcome measure in patients having primary percutaneous coronary intervention (PCI)
November 2017 Br J Cardiol 2017;24:129
BJC Staff

The COMBO™ dual therapy stent REDUCE (Short-term Dual Anti Platelet Therapy in Patients with ACS Treated with the COMBO Dual-therapy Stent), a physician-initiated, prospective, multi-centre, randomised study, was conducted in 36 hospitals in Europe and Asia, enrolling a total of 1,496 ACS patients. The study was designed to demonstrate non-inferiority of a strategy of short-term (three months) dual antiplatelet therapy (DAPT) compared to standard 12-month DAPT in patients with ACS treated with a dual-therapy stent. The stent used in the study COMBO™ (OrbusNeich) is a sirolimus-eluting stent with an abluminal biodegradable polymer matrix,

September 2017 Br J Cardiol 2017;24(suppl 1):S3–S9 doi:10.5837/bjc.2017.s01
Chris P Gale

Definition of ACS Acute coronary syndromes (ACS) include unstable angina and acute myocardial infarction (AMI). AMI is classified according to those patients with electrocardiographic ST-segment elevation, ST-elevation myocardial infarction (STEMI) and those without electrocardiographic ST-segment elevation, non-ST-elevation myocardial infarction (NSTEMI).1 The requirement for a diagnosis of AMI in the universal definition is the detection of troponin release from injured cardiac myocytes with at least one value >99th centile of the upper reference limit.1 Diagnosis is confirmed only if this is associated with at least one of: symptoms of
April 2016 Br J Cardiol 2016;23:78 doi:10.5837/bjc.2016.017 Online First
Luciano Candilio, Juliana Duku, Alexander W Y Chen

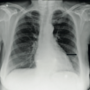
Figure 1. Patient chest X-ray showing a ‘full metal jacket’ Her physical examination and vital signs were unremarkable. Routine blood tests had been requested. Resting 12-lead electrocardiogram (ECG) showed left bundle branch block; no previous ECGs were available for comparison. A chest X-ray was performed, which gave another clue to the diagnosis… The chest radiograph (figure 1) shows clear lung fields, normal cardiac contour and, more importantly, a radio-opaque structure across the anterior surface of her heart. This is sometimes termed a ‘full metal jacket’, implying extensive stenting of a coronary artery in its entirety f
June 2015 Br J Cardiol 2015;22:79 doi:10.5837/bjc.2015.022
Faheem A Ahmad, Stephen Dobbin, Allister D Hargreaves

Introduction Current evidence suggests there has been a marked proliferation of troponin testing within medical units as the troponin assay has become the cornerstone biomarker in the diagnosis of an acute myocardial infarction (AMI).1,2 Both troponin T (TnT) and troponin I (TnI) are cardio-specific structural subunits and highly sensitive and specific markers of myocardial injury.3,4 Newer generation high-sensitivity troponin (hs-Tn) assays can detect increasingly lower troponin concentrations within an earlier time window of up to three hours.5 Early implementation of first-generation assays were accompanied with poor patient selection; ava
December 2014 Br J Cardiol 2014;21:147–52 doi:10.5837/bjc.2014.035
Anna Kate Barton, Stephanie H Rich, Keith A A Fox

Introduction For patients with acute coronary syndrome (ACS) who survive to reach hospital, the majority of mortality and morbidity over the following five years occurs after discharge.1 Of all complications, development of acute heart failure (AHF) and left ventricular systolic dysfunction (LVSD) are key determinants of adverse outcome. Approximately half of patients with ACS are readmitted to hospital, constituting a profound burden on healthcare resources.1 In several healthcare systems there are financial penalties when ACS patients are readmitted within 30 days.2 Prediction of the development of AHF and hospital readmission following ACS

October 2014 Br J Cardiol 2014;21:153–7 doi:10.5837/bjc.2014.033 Online First
Simon W Dubrey, Sarah Ghonim, Molly Teoh

Introduction Approximately 4.2 million people (7.5% of population), whose racial origins are from South Asia, live in the UK. High rates of coronary disease in Asians,1-4 seem likely to be influenced by genetic factors.5 We have previously reported differences in the presentation of coronary syndromes between British South Asians, as a whole, and white Europeans.6 The term ‘South Asian’ describes around 1.5 billion people (22.5% of the world’s population), occupying regions as diverse as Sri Lanka to Nepal. A wide variety of genotypes, cultures, diets, belief systems, educational attainment, socioeconomic status and risk factors are enc

You need to be a member to print this page.
Find out more about our membership benefits

You need to be a member to download PDF's.
Find out more about our membership benefits