Tag Archives: diagnosis

October 2014 Br J Cardiol 2014;21:159 doi:10.5837/bjc.2014.034 Online First
The utilisation of ECG in the Emergency Department
Simiao Liu, Boyang Liu, Han B Xiao

Introduction Electrocardiogram (ECG) is a common investigation carried out in the Emergency Department (ED) and provides important information for both diagnosis and prognosis. In the pre-primary coronary intervention era, ECG had been the key investigation for the prompt diagnosis and management of patients with acute myocardial infarction, particularly those with ST elevation.1-5 Since primary coronary angioplasty became widely available in the UK, patients with typical ST-elevation myocardial infarction are filtered directly to specialist centres by the ambulance service. Acute coronary syndrome (ACS) patients without typical ST elevation

June 2014 Br J Cardiol 2014;21:75 doi:10.5837/bjc.2014.017
Do NICE tables overestimate the prevalence of significant CAD?
Jaffar M Khan, Rowena Harrison, Clare Schnaar, Christopher Dugan, Vuyyuru Ramabala, Edward Langford

Introduction There is no universal definition for stable angina, as there is for acute coronary syndrome.1 The diagnosis may be based on clinical history alone or on clinical history supplemented by functional testing, or angiography, or both. Angina pectoris is most often due to obstruction to flow in the epicardial coronary arteries, and the ‘gold-standard’ investigation, to date, to detect this, has been invasive coronary angiography.2 A small proportion of patients may have angina with unobstructed coronary arteries secondary to either microvascular coronary disease or coronary spasm.3 Functional ischaemia is not routinely tested for

June 2014 Br J Cardiol 2014;21:49–50 doi:10.5837/bjc.2014.014
Where has the jugular venous pressure gone?
David E Ward

(more…)
October 2011 Br J Cardiol 2011;18:219–22 doi:10.5837/bjc.2011.002
Patent foramen ovale: diagnosis, indications for closure and complications
Sudhakar George, David Hildick-Smith

(more…)
July 2010 Br J Cardiol 2010;17:195-200
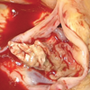
The role of nucleic acid amplification techniques (NAATs) in the diagnosis of infective endocarditis
Gillian Rodger, Stephen Morris-Jones, Jim Huggett, John Yap, Clare Green, Alimuddin Zumla

Introduction Figure 1. A large vegetation on the aortic valve from a patient with infective endocarditis Untreated infective endocarditis (IE) is fatal; even with appropriate treatment, IE is associated with high rates of morbidity and mortality worldwide.1 The annual incidence of IE over the past two decades has remained relatively constant, ranging between 1.7 and 6.2 cases/100,000 population. Neither advances in healthcare nor revisions made to the current diagnostic criteria have substantially altered this.1-3 The current definition for IE now incorporates infections of prosthetic heart valves (both bioprosthetic and mechanical), implante
March 2010 Br J Cardiol 2010;17:94–6
Brady/tachyarrhythmia preceding the diagnosis of cardiac sarcoid
Henry Oluwasefunmi Savage, Sheel Patel, Jonathan Lyne, Tom Wong

Case report A 51-year-old Asian woman presented with intermittent presyncope and profound breathlessness. She had no significant past medical history of note and was not receiving any regular medication. A resting 12-lead electrocardiogram (ECG) revealed a second-degree atrioventricular block. She subsequently underwent insertion of a dual-chamber permanent pacemaker. Further investigations at that time revealed unobstructed coronary arteries on angiography and normal ventricular function on transthoracic echocardiography. Figure 1. 12-lead electrocardiogram (ECG) demonstrates ventricular tachycardia of varying morphology Her symptoms initial
September 2008 Br J Cardiol 2008;15:269-70
Occlusion of left main coronary artery diagnosed by computed tomography of the chest
Scot Garg, Christos Bourantas, Simon Thackray, Farqad Alamgir

Figure 1. Computed tomography (CT) scan of the chest showing normal contrast filling of the right coronary artery (panel A), and absence of contrast within the left main coronary artery (panels B and C) A computed tomography (CT) scan of the chest excluded a pulmonary embolism and aortic dissection, and, although not a dedicated cardiac CT, suggested an occlusion of the left main coronary artery (LMCA) (figure 1). Echocardiography showed impaired left ventricular function with an akinetic anterior, inferior and lateral wall. An intra-aortic balloon pump (IABP) was inserted and coronary angiography was performed, which confirmed an occlusion o
July 2008 Br J Cardiol 2008;15:199-204–6
Cost-consequences analysis of natriuretic peptide assays to refute symptomatic heart failure in primary care
Michael A Scott, Christopher P Price, Martin R Cowie, Martin J Buxton

Introduction Heart failure is a serious syndrome accounting for around 4% of UK general practitioner (GP) consultations in patients over 45 years.1 Diagnosis is complex with frequent co-existing symptoms; misdiagnosis may lead to inappropriate treatment and inefficient use of scarce healthcare resources.2 The National Institute for Health and Clinical Excellence (NICE) guidelines for chronic heart failure state that the 12-lead electrocardiogram (ECG) and/or natriuretic peptides tests (where available) may be used to help exclude heart failure.3 Abnormal ECGs are usually observed in heart failure cases, although in one study, around 20% of pa
March 2008 Br J Cardiol 2008;15:79–81
Familial hypercholesterolaemia: recognising the unrecognised
Jonathan Morrell

(more…)

