Mitral valve stenosis (MS) is attributed mainly to rheumatic fever and may remain unrecognised for several years. Early diagnosis of this lesion is important in order to implement the necessary management when either severe or complicated by atrial fibrillation. However, its incidence in a multi-ethnic community has not yet been recognised. We retrospectively studied 2,099 consecutive subjects for the presence of MS. All the patients were newly referred by general practitioners to a community general cardiology clinic and hypertension clinic in a district of London because of different cardiac symptoms, significant cardiac history or because of uncontrolled hypertension. All the patients underwent echocardiography routinely. Classical clinical signs of MS were present in four patients. Echocardiography showed MS in eight patients, in four of whom the MS was mild, moderate in three and severe in one patient. None of the patients had symptoms related to the MS and all were in sinus rhythm both clinically and during Holter monitoring. Only one patient was Caucasian, two were of Caribbean origin and five were of Indo-Asian origin. Subsequent cardiac catheterisation and mitral valve replacement were successfully carried out in two patients. It is concluded that rheumatic MS is still prevalent in the UK population and is more common in subjects of Indo-Asian origin than either Caucasian or Afro-Caribbean subjects. MS was not recognised by the general practitioners: its diagnosis was only made possible by echocardiography.
Introduction
Rheumatic fever is the leading cause of acquired heart disease in children and young adults in the world.1,2 The relationship between rheumatic fever and streptococcal infection has been well documented.3,4 Stenosis of the mitral valve, either alone or in combination with other valvular diseases, is caused almost exclusively by rheumatic fever.3 Involvement of the mitral valve represents the most common of all sites affected by the rheumatic process.5 However, as many as half of the population with mitral stenosis give no history of rheumatic fever.5 On the other hand, the majority of patients with mitral stenosis remain asymptomatic for a significant time. Although in some studies a lapse of two to eight years has been reported,5 it has been demonstrated in one study that nearly two-thirds of children with a history of acute rheumatic fever did not show the disease after 10 years of follow-up.6 In another study, an average latent period of 19 years before the disease becomes clinical was reported with an average mean age for the attack of carditis being 12 years and the age of the appearance of symptoms 31 years.7 Five years after onset of rheumatic fever, there is less ability to diagnose mitral valve disease when compared with the period during the rheumatic fever episode.8
Doppler ultrasound and echocardiography have improved the detection of subclinical rheumatic carditis. It has been reported that subclinical mitral stenosis can persist even after five years of follow-up, thus emphasising the importance of echocardiography in the diagnosis of subclinical mitral stenosis.8 With better detection and early treatment of rheumatic fever there has been a significant drop in the prevalence of mitral valve stenosis in Europe. However, London is a multi-ethnic city with a population of about nine million. Brent is a borough with a population of 263,464 (in 2001) with its ethnic distribution demonstrated in figure 1.9
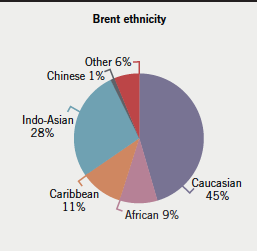
The prevalence of subclinical mitral stenosis in a community cardiology clinic serving a multi-ethnic population has not recently been studied. In this study, we assess the prevalence of subclinical mitral stenosis in community cardiology and hypertension clinics set up in a multi-ethnic community in London using Doppler ultrasound and echocardiography in its detection.
Patients and methods
During a period of 24 months (August 2006 to July 2008) the clinical records of a total of 2,099 newly referred patients who were seen in our community general cardiology clinic, and cardiovascular risks and hypertension clinic, were retrospectively reviewed. The ethnic distribution of those subjects was: Caucasian (n=545, 26%), African (n=160, 8%), Caribbean (n=318, 15%), Indo-Asian (n=1071, 51%) and Chinese (n=5, 0%).
Referral of the patients was made by their general practitioners for the investigation and management of various cardiac symptoms, or if there was either of the following: the presence of a significant cardiac history of myocardial infarction, coronary bypass surgery or percutaneous interventional procedures, cardiomegaly on a routine chest X-ray, uncontrolled raised blood pressure, suspicion of white-coat hypertension, atrial fibrillation, or abnormal resting electrocardiogram (ECG) indicating arrhythmia, conduction defects, ischaemic changes or abnormal repolarisation. Full history was obtained followed by a full cardiovascular clinical examination. Each patient underwent a resting ECG and a resting transthoracic echocardiogram using Vivid I (manufactured by General Electric, GEMS ultrasound, Tirat Carmel, Israel).
Patients with mitral stenosis alone were enrolled into the study (n=8, mean age 46 years, standard deviation [SD] 3.76). The mitral valve area was derived from averaging that derived from the pressure half-time and that derived from planimetry. Grading of mitral stenosis was made in accordance with the British Society of Echocardiography guidelines.10 In order to elucidate the presence or absence of paroxysmal atrial fibrillation, Holter monitoring was carried out in the seven subjects who had dilated left atrium. Subsequent cardiac catheterisation was carried out in two patients because of the echocardiographic findings of mixed aortic valve disease beside the severe mitral valve stenosis in one patient and the other due to her subsequent admission with pulmonary oedema.
The ethnic distribution of the patients referred to our clinics is demonstrated in figure 2.
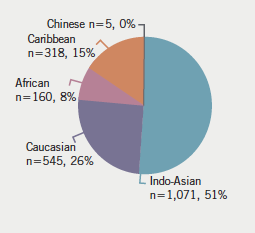
Results
The main results on the eight patients diagnosed by echocardiography to have mitral valve stenosis are summarised in table 1. Rheumatic echocardiographic features were present in all the patients. Typical clinical signs of mitral stenosis were present in three patients only. One patient also had prolapse of the anterior leaflet of the mitral valve. All the eight patients had mitral valve regurgitation. Two patients had an elevated clinic blood pressure >140/90 mmHg and four subjects had left ventricular hypertrophy (two of whom were referred because of uncontrolled raised blood pressure). Although none of the patients gave a history of rheumatic fever, six subjects had typical rheumatic changes on the mitral valve. All patients were in sinus rhythm clinically and during 24-hour ambulatory ECG monitoring. The left atrium was dilated in seven patients. One patient (RC) also had severe aortic valve disease. The latter patient underwent an elective cardiac catheterisation, which confirmed severe mitral and aortic valve disease. One of the subjects (SB), who was referred because of dyspnoea on exertion, while waiting for cardiac catheterisation was admitted to the Accident and Emergency Unit of our Hospital with acute dyspnoea and was found to be in pulmonary oedema. Both these patients (SB and RC) underwent mitral valve replacement successfully.
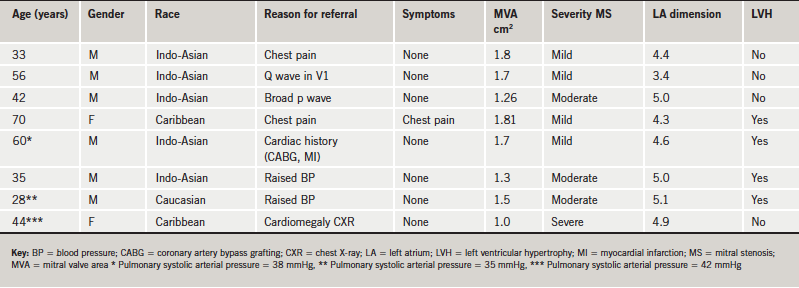
Discussion
In this report, we have demonstrated that subclinical mitral stenosis is still in existence, though with a low prevalence, in patients of different ethnic backgrounds referred for various cardiac causes to a community cardiology service in a district of London. The highest prevalence was among the Indo-Asian community, which constituted the largest of the ethnic groups referred to our clinics. Only three of the eight patients had clinical signs of mitral stenosis, although not detected by their general practitioners. Our findings are in support of a previous report8 that echocardiography and Doppler ultrasound are very useful tools to detect clinically unrecognised carditis. The value of echocardiography was also previously demonstrated in the diagnosis of rheumatic valvular insufficiency.11-13 Seven of our patients were symptom free when seen in the clinic. Early diagnosis of mitral valve stenosis using echocardiography is the only way to identify cases of rheumatic mitral valve disease at an early stage and allow the appropriate management, irrespective of patient’s ethnicity.
Similar to other previous reports,8,11,12 our findings have confirmed the value of echocardiography and Doppler ultrasound in identifying rheumatic carditis in the absence of clinical signs and/or symptoms. In one study, the number of patients with rheumatic carditis detected by echocardiography was reported to be four times higher than the number of patients detected clinically.14
Atrial fibrillation, which first appears in its paroxysmal form then becomes persistent, constitutes the most common complication of mitral valve stenosis.5 It affects 40% of cases of mitral stenosis.7 Atrial fibrillation is related to left atrial dilatation and left atrial hypertension.3 Although all of our patients except one had left atrial dilatation, all were in sinus rhythm. The majority of our subjects are liable to develop atrial fibrillation, which is the most common clinical entity that causes the development of symptoms in a previously asymptomatic subject. It is, therefore, important that the clinician and the general practitioner are made aware of this possibility. A proper follow-up of these patients is necessary in order to spot the appearance of atrial fibrillation at an early stage and implement the use of the appropriate medication and anticoagulation therapy. Furthermore, implementing the appropriate steps, as set up in the current guidelines, is necessary in the follow-up of those subjects.15 Accordingly, in our study, the six subjects who did not undergo invasive management because they were asymptomatic, with pulmonary artery systolic pressure estimated at <50 mmHg and mild-to-moderate mitral stenosis, should be followed up annually.
Though rheumatic fever is the leading cause of mitral valve stenosis,1,2 none of our patients reported a history of rheumatic fever, although rheumatic changes were noticed on the mitral valves in all eight of the patients in our study. This confirms a previous report that as many as half of the population with mitral stenosis give no history of rheumatic fever, which may be because such patients may have suffered from subclinical rheumatic fever, especially if it was not associated with polyarthritis.5 The absence of a history of rheumatic fever in a subject does not preclude the presence of rheumatic heart disease.
The cohort studied does not represent the ethnic distribution of the Brent population. The majority (51%) of the subjects referred to our clinic were of Indo-Asian origin (figure 2) as compared with 28% of the general Brent population (figure 1). This, therefore, may be one of the reasons why the highest prevalence of rheumatic mitral valve stenosis appeared to be among subjects of Indo-Asian origin. There have been few reports on the ethnic distribution of mitral valve stenosis, mostly reporting on regional incidence of symptomatic cases in individual countries. To our knowledge, there have been no reports on the incidence of asymptomatic cases of mitral stenosis in individual ethnic groups. It has been reported that the prevalence of symptomatic mitral stenosis in central Europe is two per 1,000.16 Although there are only a few population surveys in India for the prevalence of rheumatic heart disease, the few available community surveys indicate that until 1994 there were more than one million patients with rheumatic heart disease with at least 50,000 new episodes occurring every year.17 Despite that, rheumatic heart disease in India is most frequent among school children,17 in a report from a medical centre in Chennai in India, mitral stenosis was shown as the most dominant lesion of rheumatic heart disease at an incidence of 29.4% of people aged 18 years or over.18
The Indo-Asian subjects in our current study, who were immigrants from the Indian subcontinent, ranged in age between 33 and 60 years and represented a small sample of the 28% of the Brent population in London. This may suggest that further studies are needed to investigate the prevalence of mitral valve disease in such a population, and equally in the rest of the Indo-Asian population in the UK.
One of the important factors that has been implicated in causing high prevalence of rheumatic carditis is a low social class and living standards.19 This, rather than racial factors, has been blamed for the high prevalence of rheumatic carditis among the aboriginal people of Northern Australia, where rheumatic fever develops in 0.2–0.5% of school-age children annually, and where more than 2% of people of all ages have rheumatic heart disease.20 We do not believe that this factor is implicated in the causes leading to rheumatic carditis in our subjects while they were residing in the UK.
Clinical implications
Rheumatic mitral valve stenosis still exists and provides a challenge to medical practice when it is clinically unrecognised. The majority of the patients with this lesion in our study were of Indo-Asian origin. It was only possible to diagnose these cases of mitral valve stenosis with echocardiography, although, in retrospect, three patients had typical clinical signs. Regular follow-up of such patients is necessary in order to assess the progress of the mitral stenosis and to diagnose atrial fibrillation early.
Acknowledgement
We thank Ms Dinta Tailor from Physiological Measurements for her technical assistance.
Conflict of interest
None declared.
Key messages
- Rheumatic mitral valve stenosis still exists in the UK and healthcare professionals should be aware
- In most cases echocardiography is the key diagnostic tool
- Regular follow-up of such patients is necessary to assess the progress of
the lesion
References
- Nordet P; WHO/ISFC. Global programme for the prevention and control of RF/RHD. J Int FedCardiol 1993;3:4–5.
- Eisenberg MJ. Rheumatic heart disease in the developing world: prevalence, prevention and control. Eur Heart J 1993;14:122–8.
- Rick AR, Gregory JE. Experimental evidence that lesions with the basic characteristics of rheumatic carditis can result from anaphylactic hypersensitivity. Bull Johns Hopkins Hosp 1943;73:239.
- Murphy GE, Swift HF. The induction of rheumatic-like cardiac lesions in rabbits by repeated focal infections with group A streptococci; comparison with the cardiac lesions of serum disease. J Exper Med 1949;89:687.
- Selzer A, Cohn KE. Natural history of mitral stenosis: a review. Circulation 1972;45:878–90.
- Bland EF, Jones TD. Rheumatic fever and rheumatic heart disease, a twenty-year report on 1000 patients followed since childhood. Circulation 1961;24:836.
- Wood P. An appreciation of mitral stenosis. BMJ 1954;1(4871):1113–24.
- Figueroa FE, Fernandez MS, Valdes P et al. Prospective comparison of clinical and echocardiographic diagnosis of rheumatic carditis: long term follow up of patients with subclinical disease. Heart 2001;85:407–10.
- Office for National Statistics. Census 2001. Brent. Available from : www.statistics.gov.uk/census2001/profiles/00ae.asp
- British Society of Echocardiography. BSE echocardiogram report: recommendations for standard adult transthoracic echocardiography. Available from: http://bsecho.org/index.php option=com_content&task=view&id=205&Itemid=96
- Folger GM, Hajar R, Robida A, Hajar HA. Occurrence of valvular heart disease in acute rheumatic fever without evident carditis: colour-flow Doppler identification. Br Heart J 1992;67:434–8.
- Abernethy M, Bass N, Sharpe N et al. Doppler echocardiography and the early diagnosis of carditis in acute rheumatic fever. Aust N Z Med 1994;24:530–5.
- Wilson NJ, Neutze JM. Echocardiographic diagnosis of subclinical carditis in acute rheumatic fever. Int J Cardiol 1995;50:1–6.
- Marijon E, Ou P, Celemajer DS et al. Prevalence of rheumatic heart disease detected by electrocardiographic screening. N Engl J Med 2007;357:470–6.
- Bonow RO, Carabello BA, Chatterjee K et al. 2008 focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association task force on practice guidelines (writing committee to revise the 1998 guidelines for the management of patients with valvular heart disease) endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol 2008;53:1–142.
- Horstkotte D, Niehues R, Strauer BE. Pathological aspects, aetiology and natural history of acquired mitral stenosis. Eur Heart J 1991;12(suppl B):55–60.
- Vijaykumar M, Narula J, Reddy S, Kaplan EL. Incidence of rheumatic fever and prevalence of rheumatic heart disease in India. Int J Cardiol 1994;43:221–8.
- Chockalingam A, Gananavelu G, Elangovan S, Chockalingam V. Clinical spectrum of chronic rheumatic heart disease in India. J Heart Valve Dis 2003;12:577–81.
- Carapetis JR, Steer AC, Mulholland EK, Weber M. The global burden of group A streptococcal diseases. Lancet Infect Dis 2005;5:685–94.
- Carapetis JR. Rheumatic heart disease in developing countries. N Engl J Med 2007;357:439–41.


