Unwanted clots – the pathology of thrombosis
We have seen how blood clots to stop bleeding in response to injury. This is haemostasis – its physiological role. In health, it is tightly regulated to restrict clots to where they are needed. If this regulation fails, or is overwhelmed, clots can form excessively or in the wrong places. When an unwanted clot blocks an artery or vein it is called a thrombosis. Although both platelets and the clotting cascade are involved in the development of all clots, the main driver in thromboses of arteries and veins is thought to be different, because of the different shear stresses involved:
- in arterial thrombosis, platelets take a lead role;
- in venous thrombosis, coagulation factors seem to be more important.
This has crucial implications for management and prevention.
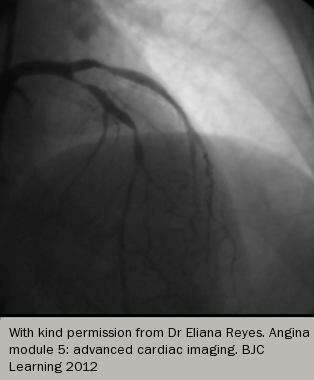
Arterial thrombosis
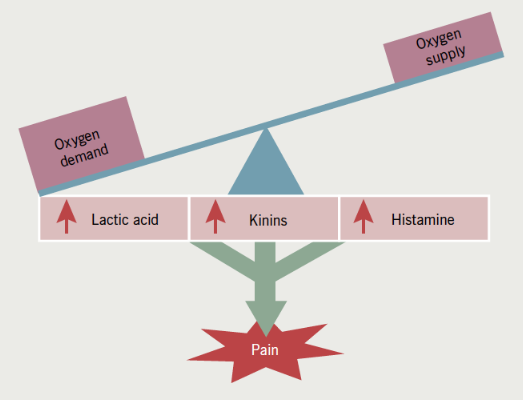
Atherosclerosis is a chronic lipid-driven inflammatory disease of the arterial wall, which is promoted by the well-known cardiovascular risk factors (diabetes, smoking, hypertension and dyslipidaemia). It leads to the formation of plaques of lipids and other material at several key anatomical points, especially the coronary arteries, carotid arteries, cerebral circulation, and the aorta, iliac and femoral arteries. These plaques lead to gradual stenosis of these arteries (see figure 8) which restricts blood flow and can lead to tissue hypoxia at times of high oxygen demand. In such conditions, the tissues are forced to respire anaerobically, leading to the accumulation of lactic acid and the development of pain symptoms (see figure 9) – the syndromes of angina and intermittent claudication.
Atherosclerotic plaques also promote thrombus formation, which, when it occurs acutely and occludes the vessel, leads to acute ischaemia in the supplied organ – myocardial infarction or stroke (see figure 10). The thrombogenicity of atherosclerotic plaques is thought to be multifactorial: plaque rupture exposes sub-endothelial collagen and tissue factor, but there is also evidence that the endothelium overlying plaques loses its anticoagulant function and becomes pro-thrombotic.7 Under the conditions of high shear stress in arteries, platelet tethering via von Willebrand factor is thought to be the predominant initiating mechanism for thrombus formation, leading to the formation of a platelet-rich thrombus.7 However, activation of the clotting cascade and generation of cross-linked fibrin is also important.

The central role of platelets in initiating arterial thrombus formation explains the essential role of antiplatelet agents (aspirin, clopidogrel, dipyridamole) in prevention of cardiovascular disease. Antiplatelet agents are also essential for the treatment of acute thrombotic events, but anticoagulants and fibrinolytics are also used. Antiplatelet and anticoagulant therapy will be discussed in more detail in modules 2 and 3.
