Management of high INR and bleeding
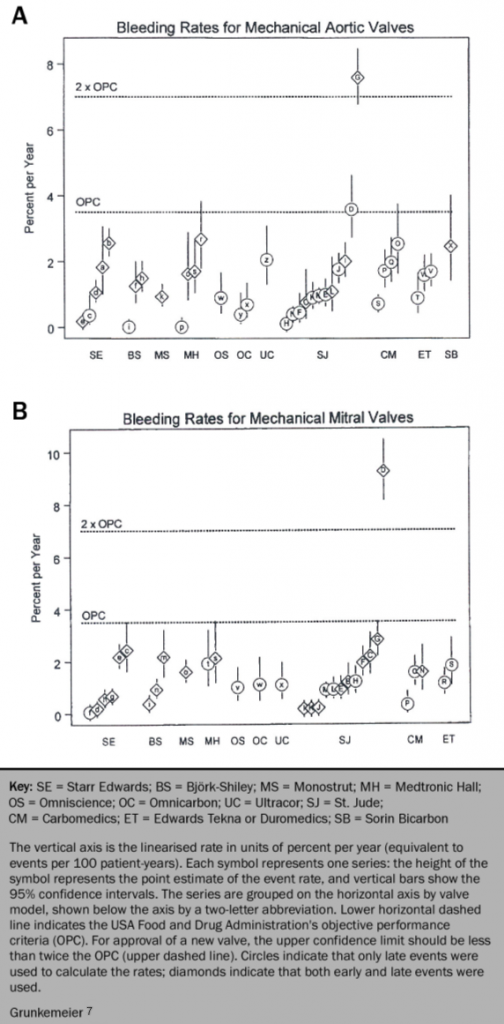
The rate of significant bleeding for mechanical valves is approximately 1–3% per year (see figure 4).7 The risk of bleeding increases exponentially above INR 6.0 and the vitamin K antagonist should be withdrawn. If the INR is greater than 10 and the patient is not bleeding, oral vitamin K in aliquots of 1–2 mg should be given. When the INR falls to a safe level, VKA therapy can be restarted with the dose adjusted to maintain adequate anticoagulation. High-dose vitamin K should not be given as it can result in a prolonged hypocoagulable state.
If there is active bleeding which cannot be controlled by compression, e.g. intracranial or gastrointestinal, anticoagulation should be reversed rapidly. Use intravenous prothrombin complex concentrate (which should be stocked by all hospitals in the UK providing emergency care of patients on anticoagulants), plus 5 mg intravenous vitamin K.
Management of thromboembolism
Thromboembolism occurs partly as a result of the thrombogenicity of the replacement valve but partly as a result of non-prosthetic factors including the heart rhythm, atrial volume and left ventricular (LV) systolic function. Thromboembolism may also occur from extracardiac sources including carotid disease and more peripheral cerebrovascular atheroma. Thorough investigation of each episode of thromboembolism is essential.
If the INR is low and the transient ischaemic attack (TIA) is distant, it is reasonable to check that prosthetic valve function is normal on echocardiography, then ensure that the INR returns to the therapeutic range.
A new TIA and low INR require admission for cardiac imaging to detect non-obstructive thrombosis and for treatment with intravenous heparin.
If the INR is in the therapeutic range or there are recurrent TIAs, full investigation including brain imaging and ultrasound scanning of the head and neck vessels is indicated. The INR control should be optimised rather than increasing the target. If TIAs continue, consider the addition of low-dose aspirin.

