This year’s 9th Annual Scientific Meeting of the Cardiorenal Forum looked at glucose, gender, rhythm and risks. Experts in the fields of cardiology, diabetes and renal medicine presented the latest developments in their fields. The meeting was held at the Royal College of Obstetricians and Gynaecologists in London and endorsed by The Renal Association and the British Society for Heart Failure. Dr Legate Philip reports on its highlights.
Managing risk factors – the old offenders
Diet
An update on diet and cardiovascular disease was given by Professor Kay Tee Khaw (University of Cambridge). A surprise recent finding has been that increased body mass index (BMI) trends do not directly correlate with cardiovascular mortality, particularly in Mediterranean countries (figure 1).
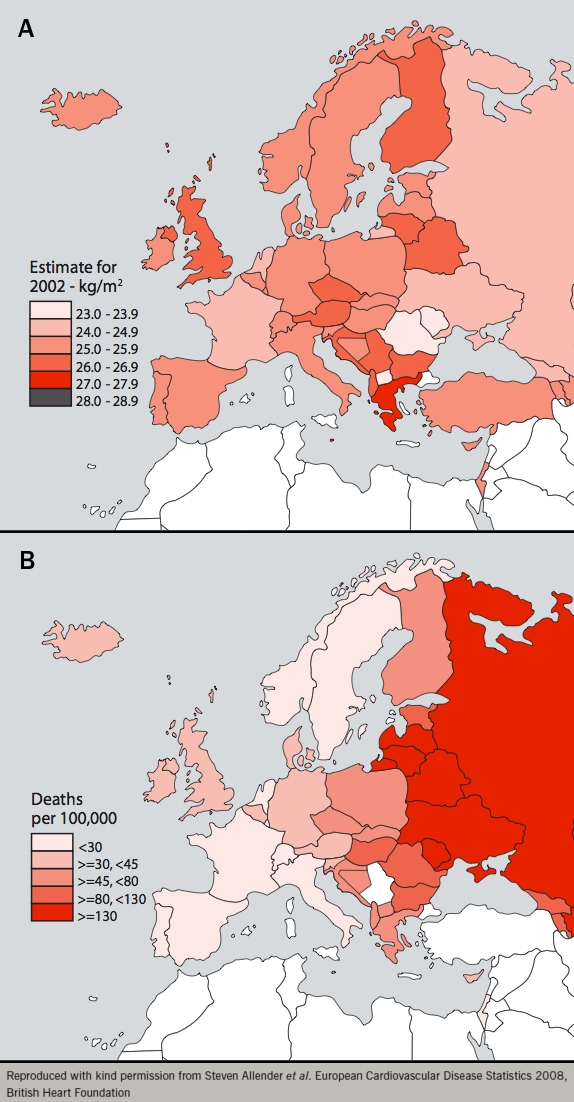
This gives rise to the question: is diet a key moderating factor in the relationship between BMI and cardiovascular mortality? The PREDIMED (Effects of the Mediterranean Diet on the Primary Prevention of Cardiovascular Disease) study compared the intervention of three diets; a Mediterranean diet plus 1 litre/week of extra virgin olive oil; a Mediterranean diet plus 30 g/day of mixed nuts; and a control group with an advised low-fat diet. People on either Mediterranean diet did significantly better than the control group: cardiovascular mortality, incidence of diabetes, acute myocardial infarction (MI) and stroke were significantly lower in the extra virgin olive oil and mixed nuts diet groups. This study reinforces the need for future interventional trials in different populations with different dietary patterns. Could the future of cardiovascular diet in the UK be fish and chips fried in extra virgin olive oil?
Diabetes
Diabetes management is an area that is constantly developing. With many new drugs being discovered and marketed, Professor Cliff Bailey (Aston University, Birmingham) took us back to basics, recapping on the mechanisms of action and evidence behind current antidiabetic medications and newer ones.
A comprehensive overview of the various pathways that are being targeted and the respective medications that are currently being used and developed in diabetes is shown in figure 2.
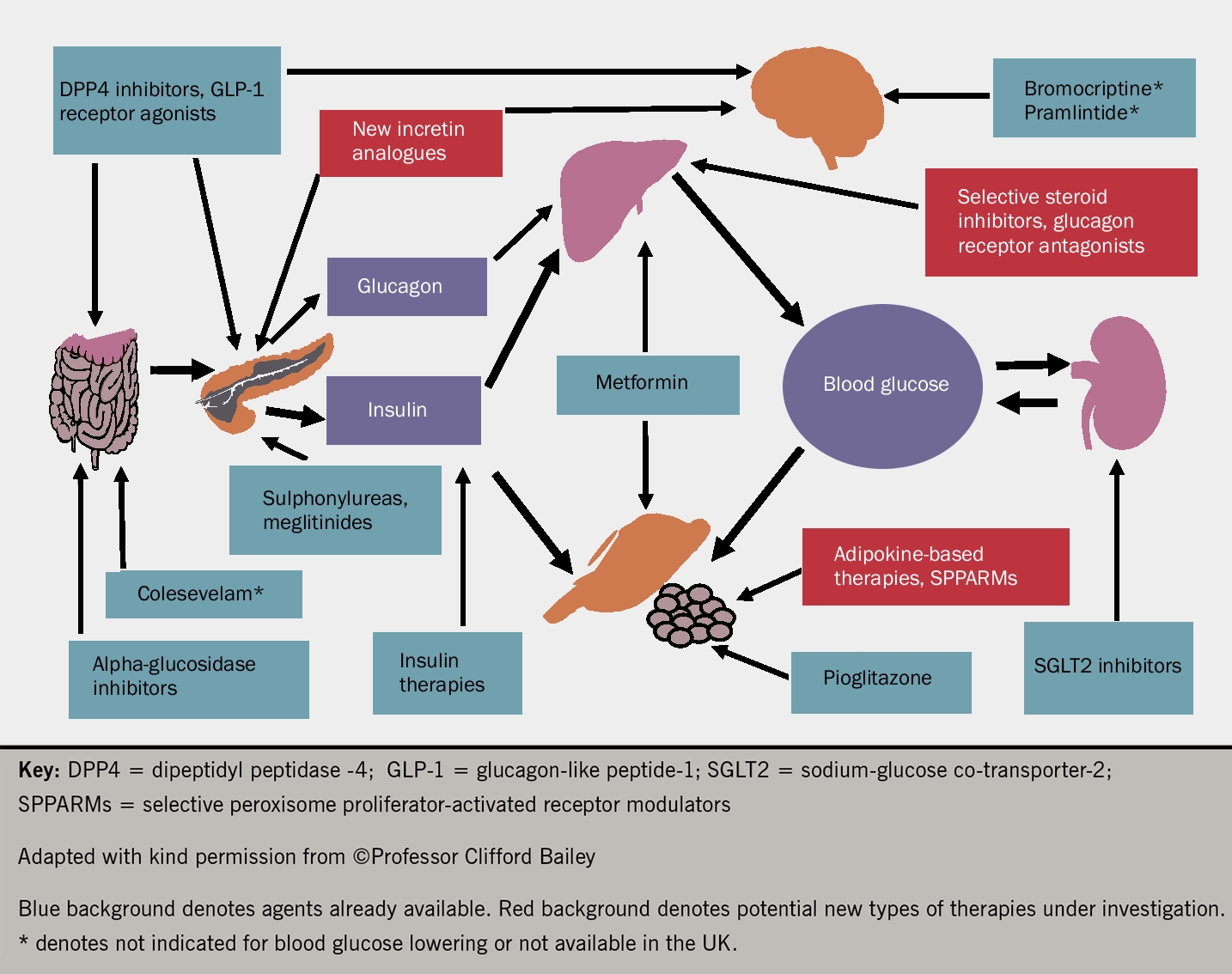
Exciting developments in this field include inhaled insulin and a once a month preparation of insulin. One could easily speculate about the convenience this would bring, but cost may be an issue.
Managing risk factors – the new kids on the block
Lipids
An update on the latest developments in the field of hyperlipidaemia was given by Professor Anthony Wierzbicki (Guy’s and St.Thomas’ Hospital, London). PCSK9 (proprotein convertase subtilisin/kexin type 9)inhibitors are a new class of drugs that lower low-density lipoprotein (LDL) cholesterol. The postulated mechanism of action is that LDL cholesterol is removed from the blood when it binds to a low-density lipoprotein receptor (LDLR) on the surface of liver cells, and is taken inside the cells. When PCSK9 binds to an LDLR, the receptor is destroyed along with the LDL particle. But if PCSK9 does not bind, the receptor can return to the surface of the cell and remove more cholesterol. Early studies are promising and there is widespread excitement about the potential clinical applicability of this class of drugs.
The other new promising class of drugs, the CETP (cholesterylester transfer protein) inhibitors inhibit CETP, which normally transfers cholesterol from high-density lipoprotein (HDL) to very low-density or low-density lipoprotein (VLDL or LDL). Thus they have a dual mechanism of action by both raising HDL cholesterol and lowering LDL cholesterol. With some patients not being able to tolerate statins and the need for novel therapies in high-risk groups (e.g. diabetes, chronic kidney disease) becoming clear, this continues to be an area of innovative drug development.
Phosphates
Is phosphate the new cholesterol of renal medicine? Professor David Goldsmith (Guy’s and St.Thomas’ Hospital, London) gave us a tantalising taster of what is being considered as a new major risk factor in cardiovascular disease. Both in vitro and in vivo studies have shown that increased phosphate levels are associated with increased vascular calcification and endothelial dysfunction, thus possibly explaining its association with increased cardiovascular mortality in patients with chronic kidney disease.
The DCOR (Dialysis Clinical Outcomes Revisited) trial was a large, multi-centre, randomised, open label trial that compared the effects of sevelamer with calcium-based phosphate binders on mortality and hospitalisation in haemodialysis patients. Sevalamer is a polymeric phosphate binder that decreases serum phosphate without changing calcium, aluminium or bicarbonate concentrations. Results of the study showed there was no significant difference in all-cause mortality between the two groups but there was a benefit seen in terms of reduced hospitalisation favouring sevelamer.
A further study, RIND (Renagel® [sevelamer hydrochloride] in New Dialysis Patients), randomly assigned patients to either sevelamer or calcium-based phosphate binders. Relatively less progression of coronary artery calcification was seen in the sevelamer group and there was also a difference seen in mortality favouring sevelamer.1 A point to note is that regulatory hormones have also been implicated in increasing vascular calcification.
Sleep disordered breathing
Sleep disordered breathing and its association with cardiorenal disease was discussed by Professor Mike Polkey (Royal Brompton Hospital, London). A key point is the distinction between central and obstructive sleep apnoea. Central sleep apnoea (CSA) is a disorder of the central drive for respiration (e.g. Cheyne Stokes in association with heart failure) while obstructive sleep apnoea (OSA) is a mechanical obstruction affecting respiratory effort. In real life an overlap of these conditions may be seen clinically. Studies have shown that impaired renal function is associated with an increase in the prevalence of both obstructive and central sleep apnoea.
Why is this important? OSA has been associated with hypertension, congestive heart failure and cerebrovascular events. It is also associated with an increased propensity for arrhythmias; OSA has been shown to be more common in patients with atrial fibrillation.2 The risk is greatest if the apnoea/hypopnoea index (AHI) is greater than 30. Should we then be asking about a history of sleep disturbances or snoring during routine consultations? In terms of management, although data does not yet support continuing positive airway pressure (CPAP) therapy for the purpose of preserving renal function, there is evidence of benefit in treating OSA in heart failure patients. Further data from a large interventional study in patients with heart failure and CSA will be presented in 2015.
Heart failure update
An update on key trials in heart failure over the last year, was given by Professor Iain Squire (University of Leicester). He selected the ROSE AHF (Renal Optimisation Strategies Evaluation in Acute Heart Failure) and PARADIGM-HF studies
ROSE AHF was a double blind, randomised, placebo controlled, multi-centre clinical trial looking into the critical issue of worsening renal function during the treatment of acute heart failure. Patients were randomised to receive low-dose dopamine, low-dose nesiritide or placebo, in addition to intravenous loop diuretics. Primary end points were change in renal function (serum cystatin C) and decongestion (cumulative urine volume). There was no significant change in either outcome when the drugs were compared to placebo and thus the results do not support the routine use of either dopamine or nesiritide in patients with acute heart failure.
Neutral endopeptidase (NEP) inhibitors are an exciting group of drugs since some peptides have beneficial compensatory effects in heart failure (e.g. natriuretic peptides). Neutral endopeptidase is an enzyme that breaks down many of these compensatory peptides. The Overture trial compared omapatrilat (a combination of angioconverting-enzyme [ACE] inhibitor and a NEP inhibitor) to the ACE inhibitor enalapril. Omapatrilat was not found to be superior to enalapril in the treatment of heart failure. Furthermore it was associated with an increased risk of serious angioedema. This led to the development of an angiotensin receptor blocker ARB and NEP inhibitor (ARNI). The PARADIGM-HF study compared the effects of the ARNI, LCZ696 (valsartan and a NEP inhibitor) to enalapril in a large, multi-centre, randomised, double-blind trial. The other strength of this trial was that the drug was compared to a dose of enalapril that was proven to be efficacious from previous trials. The trial was stopped early due to LCZ696 showing a significantly lower incidence of primary outcome (cardiovascular death or heart failure hospitalisation) and death from any cause when compared to enalapril. The scene seems set for ACE inhibitors, the cornerstone of modern heart failure treatment to be replaced with this new class of drug.
Renal medicine update
Key messages from recent trials in renal medicine were given by Dr William Herrington (Clinical Trial Service Unit, John Radcliffe Hospital, Oxford). Renal denervation is a novel therapy for the treatment of resistant hypertension that was reported at the last Cardiorenal Forum meeting.3 It is an endovascular catheter-based procedure which uses radiofrequency ablation to target the sympathetic nerves in the adventitia of the renal arteries thereby decreasing activation of the renin-angiotensin-system (RAS). It had showed promising results in the SIMPLICITY I and II trials but some pitfalls in these studies were highlighted by Dr Herrington.
In SIMPLICITY HTN I, 153 patients with resistant hypertension underwent renal denervation and change in office blood pressure (BP) was measured but there was no comparison arm. In SIMPLICITY HTN 2, renal denervation was compared to a control arm but there was no blinding done. While there was a significant change in office BP, there was no significant change in 24-hour ambulatory BP. Could the significant change in office BP have been observer bias? SIMPLICITY HTN 3 was a prospective, single-blind, randomised, sham-controlled trial that randomly assigned patients with resistant hypertension to either renal denervation or a sham procedure. This trial failed to show a significant reduction in systolic BP at six months. This latter study was also the strongest in terms of methodology as it had the most participants, a control arm and both patients and BP assessors were blinded.4 Thus renal denervation has not been proven to be a significant contender in hypertension management.
Legate Philip
CT2
Queen Alexandra Hospital, Portsmouth
Diary date
The next meeting of the Cardiorenal Forum will take place on 2nd October 2015 at the Royal College of Obstetricians and Gynaecologists, London.
References
1. Spaia S. Phosphate binders: sevelamer in the prevention and treatment of hyperphosphataemia in chronic renal failure. Hippokratia 2011;15(Suppl 1):22–26.
2. Gami AS, Pressman G, Caples SM et al. Association of atrial fibrillation and obstructive sleep apnoea. Circulation 2004;110:364−7. http://dx.doi.org/10.1161/01.CIR.0000136587.68725.8E
3. What’s hot in cardiorenal medicine. A report of the 8th Annual Scientific Meeting of the Cardiorenal Forum. Br J Cardiol 2013:20:134−6.
4. Bhatt DL, Kandzari DE, O’Neill WW et al. A controlled trial of renal denervation for resistant hypertension. N Engl J Med 2014;370:1393−1401. http://dx.doi.org/10.1056/NEJMoa1402670

