Clinical articles

2026, Volume 33, Issue 1, pages 1–40
Editorials Clinical articles News and viewsTopics include:-
- Now is the time to take syncope seriously
- Modern angina assessment
- SGLT2 inhibitors in frailty
- BJCA prize-winning essay
Editorials
Back to topJanuary 2024 Br J Cardiol 2024;31:4–6 doi:10.5837/bjc.2024.001
Dishing out the meds
David Mulcahy, Palwasha Khan

Twenty years ago, Wald and Law1 hypothesised that, if a combination pill could be made including aspirin, folic acid, a statin, and a low-dose diuretic, beta blocker and angiotensin-converting enzyme (ACE) inhibitor (thus, allowing for the simultaneous modification of four different risk factors: low-density lipoprotein [LDL]-cholesterol, blood pressure, homocysteine, and platelet function), and administered to everyone with existing cardiovascular disease and everyone over 55 years old, there would be an 88% reduction in ischaemic heart disease events, and an 80% reduction in stroke. One third of people over the age of 55 years would benefit by gaining an average of 11 years free from a cardiac event or stroke (subsequently termed the vaccination approach). They called this pill the ‘Polypill’, and concluded that treatment would be acceptably safe and, with widespread use, would have a greater impact on the prevention of disease in the Western world than any other single intervention. They noted that, while such a preventative strategy was radical, if such a formulation existed that prevented cancer and was safe, it would be widely used. “It is time to discard the view that risk factors need to be measured and treated individually if found to be abnormal. There is much to gain and little to lose by the widespread use of these drugs.” While subsequent works have shown that folic acid is not prognostically beneficial in preventing cardiovascular disease,2 and that aspirin may not be beneficial overall in primary prevention settings,3 the concept of the combination pill was awakened in the public eye.

December 2014 Br J Cardiol 2014;21:128–30 doi:10.5837/bjc.2014.031
Hypoglycaemia: patient inconvenience or serious cardiovascular risk?
Vidya Srinivas, Kashif Kazmi, Ketan Dhatariya

Hypoglycaemia is defined as a lower than normal level of blood glucose, and in patients on glucose-lowering therapy, defined as glucose levels less than 4 mmol/L. In the UK, it is usually classified as ‘mild’, if the episode is self-treated, or ‘severe’, if the individual requires third-party assistance. However, the American Diabetes Association definition of hypoglycaemia is different.1 They classify hypoglycaemia into five categories. These are shown in table 1.
Clinical articles
Back to topMarch 2026 Br J Cardiol 2026;33:19–22 doi:10.5837/bjc.2026.010
Exercise and competitive sport in those with genetic heart disease: what we know and what we don’t know. Part 1
Liam Fitzpatrick, Valerie Hayes, Habitha Sulaiman, Deirdre Ward, David Mulcahy

Historically, young people with genetic heart diseases were discouraged from active sport due to concerns about the increased risk of sudden cardiac death during competitive or intensive exercise. The shock resulting from the sudden death of a young athlete, an event often highly publicised, tends to generate concern in the general population, and fear of litigation in a low-evidence area: both influence decision-making by the medical profession when discussing ‘restrictions’, especially in patients with genetic heart diseases, who by definition, are at increased risk of sudden cardiac death. In recent years, however, we have moved to a point where many athletes with certain genetic heart diseases can, with optimal medical therapy, be considered for involvement in various sporting and athletic pursuits. We are cautiously moving away from the assumption that exercise is contraindicated; we are factoring in the wishes of the patient-athlete (shared decision-making), and we are encouraging optimal protection for these athletes during their sporting endeavours (easily available automated external defibrillators [AEDs], and club personnel trained in basic life support [BLS]), while ensuring regular medical assessment to identify alterations in risk status. With dedicated follow-up of all such patient-athletes, we can refine our understanding of how best to advise (and protect) them in terms of exercise for enhanced quality of life.
March 2026 Br J Cardiol 2026;33:40 doi:10.5837/bjc.2026.011
Mapping the patient pathway for ICI cardiac toxicities: a single-centre case series with clinical practice insights
Yu-Hsuen Yang,* Shayan Datta,* Oluwabukola Thomas-Orogan, Susan Ellery, Anna Olsson-Brown

Immune checkpoint inhibitors (ICIs) have revolutionised cancer care, but can cause serious cardiac immune-related adverse events (irAEs), particularly myocarditis, which carries up to 50% mortality. This study explores patient pathways to improve early recognition and management of ICI myocarditis in acute settings.
This was a retrospective, single-centre case series from a UK tertiary hospital with a specialist cardio-oncology multi-disciplinary team (MDT). Ten patients referred to the cardio-oncology MDT between March and August 2024 were included if diagnosed with myocarditis, pericarditis, or arrhythmias linked to ICI treatment. Clinical pathways were described using structured vignettes.
Seven patients had myocarditis, two pericarditis, and one bradyarrhythmia. Fatigue (57%) was the most common presenting symptom in myocarditis. Echocardiography was unremarkable in 86% of cases, while cardiac magnetic resonance imaging (MRI) confirmed myocarditis in 57%. N-terminal pro-B-type natriuretic protein (NT-proBNP) rose 17-fold from baseline compared with a four-fold rise in troponin T. Early MDT referral facilitated prompt diagnosis and treatment, while delayed recognition was associated with worse outcomes.
This case series highlights the importance of early MDT involvement, and the utility of additional cardiac biomarkers, such as NT-proBNP. It provides practical guidance to improve the acute care pathway for patients developing ICI-associated cardiac toxicities.
March 2026 Br J Cardiol 2026;33:36–9 doi:10.5837/bjc.2026.013
User experience of a combined 2-in-1 home ECG and blood pressure monitor: a qualitative study
Ven Gee Lim, Cleo White, Lucy Gilbert, Faizel Osman

We evaluated the usability of a novel 2-in-1 blood pressure (BP) and electrocardiogram (ECG) monitor (developed to facilitate earlier detection of hypertension and atrial fibrillation). Arrhythmia clinic patients and public volunteers were recruited. Key themes were generated from semi-structured interviews.
Patients (n=12) found the experience of measuring ECG and BP equally positive. Public volunteers (n=11) found BP measurement a more positive experience compared with ECG recording. Several key themes were generated: patient empowerment, investment in health, technical know-how, user requirements and ergonomics.
In conclusion, the 2-in-1 BP and ECG monitor received overall positive reviews, showcasing the device’s potential to enhance patient care in the management of hypertension and atrial fibrillation.
February 2026 Br J Cardiol 2026;33:9–12 doi:10.5837/bjc.2026.006
Now is the time to take syncope seriously
Richard Sutton, Frederik de Lange

Syncope, as a symptom, remains poorly understood and handled in the UK. Personal involvement stemmed from successful abolition of syncope by cardiac pacing, initially in atrioventricular block then other bradycardias; UK facilities were sparse in the late 1970s. The aim was to broaden distribution and encourage understanding. To achieve this required abandoning the typical cardiology mindset and re-engaging with internal medicine. Syncope is poorly taught in medical schools, which implies that few physicians understand it and, therefore, cannot practise it to benefit patients. Syncope patients presenting in emergency departments (>1% of all) are frequently admitted to hospital to undergo numerous non-diagnostic tests, then discharged without diagnosis. Syncope has life-threatening causes in >1% of patients; given its prevalence, this represents a large number. Treatment is now possible.
Syncope science has notably advanced, offering valuable diagnostic and therapeutic strategies. Ubiquitous delivery in the UK requires a new approach, which has been applied in the Netherlands. Now, more than ever, is the time to take syncope seriously, with action now to address this critical situation.
February 2026 Br J Cardiol 2026;33:23–5 doi:10.5837/bjc.2026.008
Green at heart: can cardiology become more environmentally sustainable without compromising patient care?
Isabel Carter

This article won first prize in the recent British Junior Cardiologists’ Association (BJCA) essay competition.
January 2026 Br J Cardiol 2026;33:13–8 doi:10.5837/bjc.2026.002
SGLT2 inhibitors in frailty: a review of current evidence, and clinical recommendations
Milo Simpson,* Shayan Datta,* Jonathan Golding, Gaurav Gulsin, Sergio Kaiser, Amar Puttanna

There is a high prevalence of frailty in people with heart failure, chronic kidney disease, type 2 diabetes, and multiple long-term conditions. These groups are eligible for treatment with sodium-glucose cotransporter 2 inhibitors (SGLT2i), with numerous large-scale trials demonstrating favourable clinical outcomes spanning disease states. There are now increasing data that the benefits of these agents are consistent across all frailty severities and are well tolerated. However, real-world data suggest a hesitancy in SGLT2i use in those with frailty. As a result, SGLT2i are either not initiated or discontinued inappropriately in people with frailty who are likely to derive benefit from these agents. This review critically evaluates current evidence and clinical guidelines for SGLT2i use in people with frailty, addressing safety concerns and offering practical recommendations for clinical practice.
January 2026 Br J Cardiol 2026;33:31–5 doi:10.5837/bjc.2026.003
Does severe pulmonary hypertension affect long-term survival after TAVI for severe aortic stenosis?
Hasan Mohiaddin, Kevin Mohee, Robert Ambrogetti, Sanjay S Bhandari, Jan Kovac, Elved Roberts

Pulmonary hypertension (PH) is common in patients with severe aortic stenosis (AS). Severe PH has been associated with mortality up to two years following transcatheter aortic valve implantation (TAVI). Data on longer-term outcomes in TAVI patients with severe PH are limited. We aimed to compare all-cause mortality at five years post-TAVI in patients with and without severe PH and to identify any patient factors associated with reduced long-term survival.
TAVI patients meeting our inclusion criteria between January 2013 and October 2017 at a specialist cardiac centre in the UK were retrospectively analysed. Severe PH was defined as a systolic pulmonary arterial pressure >40 mmHg, estimated on transthoracic echocardiography. Data on patient demographics, comorbidities and mortality were obtained from routinely collected registry data. Kaplan-Meier and Cox-proportional hazards analyses were performed.
The median ages of the patients were 84 and 83 years in the group without severe PH and the group with severe PH, respectively. Severe PH was present in 95 out of 219 patients (43%). Patients with severe PH had higher levels of disability, left ventricular impairment and serum creatinine. On multi-variate analysis, the presence of severe PH was not associated with an increased mortality (adjusted hazard ratio [HR]=1.23, p=0.29). Peripheral vascular disease (PVD) was associated with a significantly increased risk of death at five years’ follow-up (adjusted HR=2.24, p=0.002). A lower body mass index (BMI) was also independently associated with reduced survival (adjusted HR=0.96, for an increase of 1 kg/m2, p=0.038).
In conclusion, our data show that severe PH in patients with AS did not affect five-year survival post-TAVI. Reduced BMI and PVD were significantly associated with long-term all-cause mortality in patients undergoing TAVI.
January 2026 Br J Cardiol 2026;33:26–30 doi:10.5837/bjc.2026.004
Risks of bleeding vs. thromboembolism in patients with mechanical valves anticoagulated with warfarin
Hannah Glatzel, Heba Nashat, Dalia Khan, Lucy Wood, Claire Harris, Victoria McDonnell, Gurpreet Bahra, Elizabeth Orchard

Anticoagulation with vitamin K antagonists is recommended for prevention of thromboembolism in patients with mechanical heart valves. However, this treatment carries a notable risk of bleeding. We performed a retrospective analysis of patients with mechanical heart valves who were anticoagulated with warfarin, extracting the number and type of mechanical heart valves and their time in therapeutic range (TTR) for various recommended international normalised ratio (INR) ranges. Following this, we carried out a prospective study, over two separate six-month periods, identifying those with mechanical heart valves who sustained a bleeding or thromboembolic event.
We identified 409 patients with mechanical heart valves with an overall TTR of 68%. Over 12 months, we recorded 32 possible bleeding incidents in 22 patients. There was one thromboembolic event during this period, specifically a cerebrovascular event.
In conclusion, while our data indicate an elevated risk of bleeding, additional larger studies are needed to better understand bleeding risks across different demographic groups.
January 2026 Br J Cardiol 2026;33(1) doi:10.5837/bjc.2026.005
Ipilimumab/nivolumab-induced severe triple M syndrome in a patient with metastatic renal cancer
Oghenevwede Okuma, Oladipo Olatunji, Ehiosa Charles Okuofo, Chizoba Nwankwo, Alison Humphreys

A 78-year-old man presented to the cancer assessment bay with a history of progressive fatigue, generalised muscle pain, and bilateral ptosis after completing two cycles of nivolumab/ipilimumab for metastatic renal cancer. Physical examination revealed mild bilateral ptosis (right > left), worsening with upward gaze, binocular diplopia, and fatigable weakness in the right shoulder. Electrocardiogram (ECG) showed a new right-bundle branch block (RBBB), with left-axis deviation, and left ventricular hypertrophy. Blood analyses showed elevated troponin I, brain natriuretic peptide, and creatine kinase with values of 221 ng/L, 114 ng/L, and 1,109 U/L, respectively. He was managed as immune checkpoint inhibitor-related severe myocarditis, myositis, and myasthenia gravis overlap (triple M) syndrome with high-dose steroids and pyridostigmine, resulting in clinical and biochemical improvement. However, immunotherapy was permanently discontinued, and follow-up imaging after three months showed evidence of disease progression. This case explores the importance of a multi-disciplinary approach in the effective management of a rare and severe immune-related toxicity and the impact of toxicities on treatment options and cancer progression.
December 2025 Br J Cardiol 2025;32:148–51 doi:10.5837/bjc.2025.052
Cardiology without ejection fraction
Peter L M Kerkhof, Rienzi A Diaz-Navarro, Neal Handly

Ejection fraction (EF) offers a remarkable approach to assess ventricular and atrial pumping capacity. Its value can easily be calculated, and it seems to reflect performance. However, EF is a non-preferred candidate from a conceptual point of view. To fully understand the weakness of the EF metric, it is necessary to appreciate that its numerical value (by its definition) solely depends on end-systolic volume (ESV) and end-diastolic volume (EDV). This tight mathematical connection can best be graphically represented in the ventricular volume domain while relating ESV to EDV, leading to straight conclusions about EF.
No previous paper has addressed the curious tradition of applying EF in cardiology in terms of the indirect reasons for its popularity, as well as the intrinsic shortcomings, alongside the statistical irregularities involved. This review highlights the misleading attractiveness of EF, while also offering logical alternatives without invoking the need for relying on additional data beyond standard measurements.
December 2025 Br J Cardiol 2025;32:152–7 doi:10.5837/bjc.2025.053
Using nanotechnology for the diagnosis and treatment of coronary artery disease: a narrative review
Reina Ibrahim,* Lea Nohra,* Waleed Inayat Mohamed, Kristina Nasr, Laurentia Fidella Averina Setia Santoso, Peter Raffoul, Abdallah Alkhaldi

Cardiovascular disease incidence is increasing worldwide, rendering it the most common cause of death worldwide. As such, nanomedicine has emerged in the context of overcoming these biological barriers. In this review, novel technologies are illustrated on two levels: molecular imaging and nanotechnology in atherosclerosis and therapeutic options in atherosclerosis. The former includes many diagnostic techniques, such as fluorescence imaging, computed tomography angiography (CTA), magnetic resonance imaging (MRI), photoacoustic imaging, contrast-enhanced ultrasound (CEUS), and multi-modality imaging. The latter is divided into two main subgroups: the first group includes inflammation-targeted therapies involving the endothelial cells and macrophages, and the second group includes nanoparticle transporters, like liposomes, micelles, dendrimers, polymeric nanoparticles (NPs), gel-like NPs, carbon nanotube, magnetic NPs, iron oxide NPs and gold NPs, and nanocoating (stent polymeric coatings to nanotextured ceramic coatings). In conclusion, nanoparticles show promise in enhancing the early diagnosis and targeted treatment of coronary artery disease. While several imaging and therapeutic techniques have demonstrated efficacy in preclinical models, only a few have progressed to human trials or clinical use.
December 2025 Br J Cardiol 2025;32(4) doi:10.5837/bjc.2025.054
Multi-systemic diseases with cardiac involvement: insights from two clinical cases
Simão Carvalho, Diana Carvalho, Inês Cruz, Tiago Aguiar, Carlos Costa, Raquel Ferreira, Andreia Fernandes, Ana Briosa Neves

Systemic inflammatory diseases (SIDs) can present with a wide range of cardiac manifestations, which, although uncommon, are frequently associated with significant morbidity and poor prognosis. Behçet’s disease and antiphospholipid syndrome (APS) are two distinct immune-mediated disorders encompassed within this spectrum, both capable of causing intracardiac thrombi and systemic embolisation, which causes diagnostic and therapeutic challenges. While Behçet’s disease is a classic systemic inflammatory vasculitis, APS primarily represents a prothrombotic autoimmune disorder with variable inflammatory features. This case series highlights two patients with cardiac involvement in SIDs, emphasising the importance of early recognition, individualised treatment strategies, and a multi-disciplinary approach to optimise outcomes in these complex clinical scenarios.
December 2025 Br J Cardiol 2025;32(4) doi:10.5837/bjc.2025.055
Multiple coronary artery fistulae unmasked by myopericarditis
Gregory Offiah, Caroline Daly, Ross T Murphy

A coronary artery fistula (CAF) is an abnormal connection between a coronary artery and another structure. This rare condition has an incidence in the general population of 0.002%. A 57-year-old woman presented with angina, a normal electrocardiogram (ECG) and a peak troponin I of 0.22 µg/L (normal <0.04 µg/L). She was treated with a standard medical regimen for non-ST-elevation myocardial infarction. Coronary angiography revealed non-obstructed coronary arteries, with fistulae arising from the left anterior descending, left circumflex and right coronary arteries, all terminating in the pulmonary artery. Cardiac magnetic resonance (CMR) imaging was performed to investigate coronary steal syndrome. This confirmed there was no significant shunt or evidence of infarction. There was a small concentric pericardial effusion with a focal region of inferolateral epicardial fibrosis, suggesting a diagnosis of myopericarditis. The patient was treated with colchicine for three months.
CAF can cause patients to present with a variety of symptoms or potentially life-threatening complications, including fistula rupture and myocardial infarction. Early recognition, characterisation and shunt analysis are imperative to facilitate management. Although left/right heart catheterisation is considered the gold standard, CMR proved to be a useful diagnostic tool in our case, ruling out significant shunting and helping to identify a differential diagnosis.
December 2025 Br J Cardiol 2025;32(4) doi:10.5837/bjc.2025.056
Refractory ventricular tachycardia: clinical challenges and management strategies
Mohamed Elhadi, Mohamed Daoub, Kanarath P Balachandran

This case report highlights the clinical course of a young patient with a history of ischaemic cardiomyopathy and severely impaired left ventricular (LV) systolic function following a delayed anterior myocardial infarction, which was further complicated by the presence of large LV thrombus. The patient subsequently presented with persistent ventricular tachycardia (VT) refractory to multiple anti-arrhythmic medications and antitachycardia pacing (ATP). VT ablation was contraindicated due to the LV thrombus, and the failure of conventional medical therapy. Heart transplantation was considered as the final viable management strategy. This case highlights the complexity of managing patients with advanced heart failure and ventricular arrhythmias, emphasising the importance of timely consideration of advanced therapeutic options in refractory scenarios.
November 2025 Br J Cardiol 2025;32:130–4 doi:10.5837/bjc.2025.048
Cardiac screening in athletes: benefits and potential challenges
Pranav Ramesh, Harshil Dhutia

Sudden cardiac death (SCD) in young athletes is a rare but devastating event, most often caused by structural or electrical abnormalities of the heart. Although athletes are generally among the healthiest individuals, the occurrence of SCD in this group attracts significant public attention, particularly as exercise may trigger fatal events in those with underlying disease. This has driven debate around the role of pre-participation screening (PPS) as a strategy to identify at-risk individuals before they compete. Several international sporting and scientific organisations have issued recommendations, but screening protocols vary, and the balance between benefit, feasibility, cost, and potential harm remains controversial. While evidence suggests that screening may detect otherwise silent cardiovascular disease, limitations include false-positives, false-negatives, interpretation challenges, and the ethical implications of disqualification. This review explores the benefits and potential challenges of cardiac screening in athletes, and the implications for protecting athlete health and ensuring safe participation in sport.
November 2025 Br J Cardiol 2025;32:145–7 doi:10.5837/bjc.2025.051
Demystifying AI for early AF detection: enhancing diagnostic transparency across modalities
Justin Lee Mifsud, Mark Adrian Sammut, Claire Galea

This article explores using artificial intelligence (AI) to detect atrial fibrillation (AF) early, highlighting its potential to revolutionise cardiology. It reviews numerous studies demonstrating AI’s superior accuracy to traditional methods, particularly in leveraging electrocardiography data from various sources like smart devices and chest radiographs. A key concern addressed is the ‘black box’ nature of some AI algorithms, emphasising the critical need for transparency to build clinician confidence and ensure ethical patient care. It concludes by advocating for policy changes and further research to enhance AI algorithm transparency and integration into clinical practice.
October 2025 Br J Cardiol 2025;32:139–44 doi:10.5837/bjc.2025.044
Comparative efficacy of drug-coated balloons versus drug-eluting stents in treating de novo CAD in ACS
Sushant Saluja, Fahmida Mannan, Maaham Saleem, Magdi El-Omar, Amjad Khanfar, Anusha Singh, Freidoon Keshavarzi, Mohammed Alawami

Drug-eluting stents (DES) are a common treatment for acute coronary syndrome (ACS) but pose risks like bleeding, re-stenosis, stent thrombosis, and neo-atherosclerosis. Drug-coated balloons (DCB) may mitigate these risks. This study compares DCB therapy’s effectiveness with DES in ACS patients with de novo lesions.
A retrospective observational study was conducted on ACS patients undergoing percutaneous coronary intervention (PCI) with either DES or DCB from May 2019 to August 2022 at a single tertiary centre. Patients with left central trunk lesions were excluded. The primary end point was a composite of major adverse cardiovascular events (MACE), cardiac death, myocardial infarction, and target lesion revascularisation, evaluated 12 months post-intervention. Statistical analysis was performed using R software with significance set at a two-tailed p value <0.05.
Of 168 patients, 101 received DES and 67 received DCB. The DCB group had a mean age of 61.9 years, while the DES group averaged 63 years. The DCB group had more prior PCIs and myocardial infarctions. Baseline characteristics, including target and number of lesions, were comparable. MACE occurred in eight (11.9%) DCB patients and 11 (10.9%) DES patients, showing no significant difference (p=0.64).
In conclusion, this study suggests that DCB therapy may be an effective alternative to DES for ACS. However, limitations, including a single-centre setting and short follow-up, warrant the need for more extensive, randomised trials to validate these findings.
October 2025 Br J Cardiol 2025;32:135–8 doi:10.5837/bjc.2025.045
Interpretation of echocardiography reports by oncologists: a regional survey
Muhammad Hamza Riaz, Adrian Ionescu, Rupali Nayar, Mark Davies

Cardiotoxicity, including left ventricular (LV) dysfunction, is a dreaded side-effect of selected drugs that are widely used in oncology. Guidelines recommend the assessment of LV systolic function, primarily by echocardiography, before and during exposure to cardiotoxic medications. However, apart from LV ejection fraction (LVEF), echocardiography reports include dozens of numerical data points and other detailed information familiar to cardiologists, but which may not be familiar to other specialties.
With a rising need for echo in oncology patients, and with no cardio-oncology service within our hospital, we assessed what is understood by oncologists regarding the information provided within an echocardiographic report, and what action they take subsequent to the report. Morriston Cardiac Centre provides tertiary care to a population of 1.2 million and conducts 12,000 transthoracic echocardiograms (TTE) annually.
We ran a survey of all consultant clinical oncologists in Wales, using a set of multiple-choice questions via Google Forms. We presented the responders to our questionnaire with a set of hypothetical echocardiographic findings, drawn from common clinical scenarios, and asked what they would do if they received a report containing such a finding. Our questionnaire was completed by 14 of 19 (74%) oncology consultants.
Only a little better than half reported low-to-moderate confidence in interpreting the findings that echo reported. Oncologists varied in their level of confidence and understanding of what TTE findings meant, and the responses to commonly reported echocardiographic findings (e.g. actions they would take if echo report stated low-normal ejection fraction) had inhomogeneity.
Our work supports the utility of a dedicated cardio-oncology clinical pathway or service, which would assist with these queries, and may even obviate them, by providing the echo report directly to a cardio-oncologist.
October 2025 Br J Cardiol 2025;32:159 doi:10.5837/bjc.2025.046
Thromboprophylaxis strategies for patients with a Fontan palliation: practice in the NHS
Elen Hanna Hughes, Sadaf Raza, Sarah Moharem-Elgamal, Vasileios Papaioannou, Jaspal Dua, Petra Jenkins, Damien Cullington, Reza Ashrafi, Robert Johnson, Julia Jones

Adults with Fontan palliation face variable risks of thrombosis and bleeding. The optimal thromboprophylaxis strategy remains unclear. There is a balance between the risk of thromboembolism and bleeding with thromboprophylaxis. Recent studies suggest direct oral anticoagulants (DOACs) may provide effective thromboembolism prevention, but concerns regarding bleeding risk, hepatic impairment, and lack of robust data persist. This study investigates thromboprophylaxis practices among UK adult congenital heart disease (ACHD) specialists, focusing on the use of DOACs in Fontan patients.
An electronic survey was distributed to UK National ACHD Consultant Group members from February to March 2023. Based on hypothetical clinical scenarios, the survey collected demographic data, familiarity with DOACs, and preferred thromboprophylaxis strategies. Responses were analysed using descriptive statistics to identify patterns in practice.
There was a maximum response rate of 42%, with 32 respondents participating, primarily consultants from level 1 ACHD centres. Thromboprophylaxis strategies varied significantly: DOACs, warfarin, and aspirin were used with varying frequency, depending on clinical factors, such as arrhythmias, thrombosis history, and patient-specific challenges. While 35% of respondents were comfortable prescribing DOACs, 42% expressed reservations, citing limited evidence and concerns about risks.
This study highlights wide variability in thromboprophylaxis strategies for Fontan patients in the NHS, underscoring significant gaps in evidence. Hepatic considerations, patient-specific challenges, and the lack of DOAC licensing for certain scenarios contribute to the complexity of clinical decision-making. Prospective studies are essential to guide practice, and patient involvement in shared decision-making is critical in the interim.
October 2025 Br J Cardiol 2025;32:160 doi:10.5837/bjc.2025.047
Optimising the management of temporary epicardial atrial pacing to combat postoperative atrial fibrillation
Daniel St. Ange-Meese, Christopher Monkhouse, Julian O M Ormerod

Temporary epicardial pacing is a cornerstone of postoperative cardiac care, but improper management, particularly of atrial pacing, may contribute to the onset of postoperative atrial fibrillation (POAF). In this article we review the challenges involved in identifying atrial lead malfunction and the associated arrhythmogenic risk. As well as implementing strategies to reduce risk, the development of advanced technology capable of detecting and correcting atrial pacing dysfunction in real time should be a priority.
September 2025 Br J Cardiol 2025;32:115 doi:10.5837/bjc.2025.039
A follow-up analysis of PCSK9 inhibition therapy in real-world practice: evaluating the efficacy of inclisiran
Prashasthi Devaiah, Jacob George

Reduction in low-density lipoprotein-cholesterol (LDL-C) in patients with hypercholesterolaemia is associated with a lower risk of cardiovascular (CV) events. Proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibiting therapy is approved by the National Institute for Health and Care Excellence (NICE) and the Scottish Medicines Consortium (SMC) for use in high-risk patients who are unable to achieve the LDL-C target levels, despite other maximum tolerated lipid-lowering therapies. Our prior publication analysed the records of patients in a large Scottish health board with familial hypercholesterolaemia and high CV risk and confirmed the real-world efficacy of PCSK9 inhibiting monoclonal antibodies (mAbs) in routine clinical care.
In this follow-up study, we examined the comparative efficacy of inclisiran, a small-interfering ribonucleic acid (siRNA) therapeutic, in a similar patient cohort to provide real-world data that can guide clinicians in optimising lipid-lowering strategies.
September 2025 Br J Cardiol 2025;32(3) doi:10.5837/bjc.2025.040
The convergence of diversity: an ECG sign of high lateral coronary occlusion
Maroua Dali, Zaki Akhtar, Richard G Bogle

A 44-year-old man presented with chest pain and an unusual pattern of ST-elevation in leads aVL and V2, and ST-depression in leads II, III and aVF on electrocardiogram (ECG). Artificial intelligence (AI)-augmented ECG interpretation reported the abnormality as indicative of occlusive myocardial infarction (OMI) and highlighted the abnormal leads in the pattern that was recognised to be that of the South African flag. This previously reported pattern is associated with acute occlusion of the intermediate or high diagonal coronary arteries, which was then confirmed on coronary angiography, but only when an extreme left anterior oblique (LAO) caudal view was used. The intermediate artery was successfully treated with percutaneous coronary intervention (PCI). It is our experience, like that of Louis Pasteur, that chance appears to favour the prepared mind. This case highlights the importance of being prepared by recognising non-typical ECG patterns associated with acute coronary occlusion, and being aware of which vessel is likely to be occluded. This demonstrates the utility that AI-augmented ECG interpretation can bring to cardiologists to refine patient management.
September 2025 Br J Cardiol 2025;32(3) doi:10.5837/bjc.2025.041
Balloon-uncrossable SVG lesion managed with recanalisation of CTO using rotational atherectomy
Nawaz Z Safdar, Syed Y Naqvi, Ali M Bhatty, Muhammad Usman Shah, Angela Hoye

Saphenous vein grafts (SVGs) are frequently used for coronary artery bypass grafting (CABG) of severe coronary artery disease; however, re-stenosis is common. Restoration of blood flow to the SVG is uncommonly achieved via revascularisation of the native vessel. A man in his 70s with previous CABGs presented with prolonged chest pain at rest. The left anterior descending (LAD) and left circumflex arteries had chronic total occlusions (CTO), and the SVG and left internal mammary artery, previously used to bypass the LAD, were severely diseased with sluggish flow and an inability to pass a balloon or microcatheter. Rotational atherectomy was successfully performed to cross the LAD CTO, with good flow post-stenting. He remained asymptomatic one year later. Where management of calcified venous grafts precludes passage with balloon or microcatheter, rotational atherectomy of the native coronary may represent an alternative method of restoring blood flow.
August 2025 Br J Cardiol 2025;32:87–90 doi:10.5837/bjc.2025.035
Atrial fibrillation and physical activity
Cai Lloyd Davies, Anvesha Singh, G André Ng, Gerry P McCann, Susil Pallikadavath

Habitual physical activity improves cardiovascular health but there is a higher risk of atrial fibrillation (AF) in endurance athletes. The physiological processes underlying this observation are not fully understood, but adaptations to exercise, such as bradycardia and atrial dilatation, may contribute to arrhythmia susceptibility. Further data on long-term implications and individualised management strategies in athletes with AF are required.
August 2025 Br J Cardiol 2025;32(3) doi:10.5837/bjc.2025.037
Platypnea-orthodeoxia syndrome – a rare presentation and diagnostic challenge
Miriam Jassam Walker, Gowri Sri Paranthaman, Haqeel Jamil

Platypnea-orthodeoxia syndrome (POS) is a rare condition which presents with positional dyspnoea and deoxygenation on an orthopneic position which resolves when supine. We present a rare presentation of POS in a 75-year-old man, who initially presented with mixed symptomology including dyspnoea on exertion and syncope. He was found to have intermittent symptomatic hypoxia and initial investigations ruled out infection, pulmonary embolism and interstitial lung disease. Pulse oximetry confirmed positional variations in oxygenation. A transthoracic echocardiogram and a transoesophageal bubble echocardiogram with positional manoeuvres confirmed the presence of a large patent foramen ovale (PFO) with shunting. The patient was referred to the tertiary centre for PFO closure which resulted in resolution of his symptoms. This case report highlights the importance of recognising POS as a rare differential in causes of unexplained dyspnoea and utilising multiple imaging techniques to confirm the diagnosis.
August 2025 Br J Cardiol 2025;32:118–20 doi:10.5837/bjc.2025.038
Heartbeats interrupted – unveiling cardiac sarcoidosis
Sriya Prakash Nair, Michael Benedict Connolly

Cardiac sarcoidosis is a rare but potentially deadly complication of systemic sarcoidosis, in which the heart is affected by immune dysregulation and granulomatous infiltration. We present a case of a 65-year-old woman who presented with worsening breathlessness and bradycardia secondary to complete heart block. Workup with cardiovascular magnetic resonance imaging showed an increased signal on late gadolinium enhancement sequences in the anteroseptum and inferoseptum consistent with active infiltration from cardiac sarcoidosis. High-resolution computed tomography of the chest showed multifocal ground-glass opacities with a peribronchovascular distribution in keeping with sarcoidosis. A dedicated CT scan of the chest showed bilateral hilar lymphadenopathy. A further positive emission tomography scan confirmed the diagnosis of cardiac sarcoidosis in the left ventricle. The findings were discussed in the cardiology multidisciplinary team meeting and it was decided the patient needed an implantable cardioverter defibrillator with further follow-up with the respiratory and cardiology team.
July 2025 Br J Cardiol 2025;32:91–9 doi:10.5837/bjc.2025.030
Differential diagnosis between ‘athlete’s heart’ and cardiomyopathies
Alessio Petrone, Tiziana Cristina Minopoli, Michael Papadakis, Sanjay Sharma, Gherardo Finocchiaro

Physiological adaptation to exercise results in a series of electrical, structural, and functional cardiac changes, broadly named ‘athlete’s heart’. Symmetrical enlargement of all cardiac chambers and mild increase in wall thickness are common findings in highly trained athletes. Typical electrocardiogram (ECG) features include sinus bradycardia, first-degree atrioventricular (AV) block, isolated voltage criteria for right and left ventricular hypertrophy and early repolarisation. Cardiac remodelling may be marked in some athletes, and it may be challenging to distinguish physiological adaptation from cardiac conditions at risk of sudden cardiac death (SCD), such as cardiomyopathies. Differential diagnosis often requires a comprehensive assessment starting from a detailed personal and family history to baseline tests, such as ECG and echocardiogram. In some cases, second-line tests, such as prolonged ambulatory ECG monitoring, exercise tolerance test and cardiovascular magnetic resonance are required.
In this narrative review, we will explore the key features of physiological cardiac adaptation to exercise, and we will focus on differential diagnosis between ‘athlete’s heart’ and cardiomyopathies.
July 2025 Br J Cardiol 2025;32:105–11 doi:10.5837/bjc.2025.032
Different cardiac phenotypes of sickle cell disease revealed using cardiac magnetic resonance imaging
Candice Park, Payal Desai, Subha Raman, Regina Crawford, Yuchi Han

Sickle cell disease (SCD) is an inherited haematologic disorder with cardiac-related complications. Cardiac magnetic resonance (CMR) imaging allows us to assess the cardiac morphology and function of this population. Our aim was to better characterise phenotypic variations among SCD patients utilising CMR data.
This retrospective study included 72 patients with SCD who underwent CMR between May 2013 and July 2023. We recorded baseline characteristics, medical history, and indication and setting of CMR. CMR parameters relating to morphology and function were collected. Patients were placed into the following groups based on cardiac parameters on CMR: high output, pulmonary hypertension (PH; defined by mean pulmonary artery pressure >20 mmHg on right heart catheterisation or elevated tricuspid regurgitation velocity >3.4 m/s on echocardiogram), left ventricular (LV) dysfunction, or normal size and function. Between- and within-group comparisons were performed.
Demographic data were similar among groups. The PH group was more likely to have a history of smoking, chronic hypoxia, lower baseline haemoglobin, and need for blood transfusion (p<0.05 for all). There were significant between-group differences in CMR structural and function parameters.
In conclusion, sickle cell patients present with different cardiac phenotypes. Patients with PH are associated with significantly higher morbidities.
July 2025 Br J Cardiol 2025;32:100–4 doi:10.5837/bjc.2025.033
Auditing CV risk assessment of inpatients with acute high-risk chest pain: room for improvement?
Sasha T Gold, Muhammad H Riaz, Fraser C Goldie, Adrian J B Brady

Low-density lipoprotein-cholesterol (LDL-C) is accepted as a causal risk factor for development of atherosclerotic cardiovascular disease (CVD) and acute coronary syndromes (ACS). In individuals aged 40–75 years, reducing LDL-C constitutes a main treatment target for prevention of atherosclerotic CVD in all international guidelines. Furthermore, diabetes mellitus (DM) confers a two-fold excess risk of vascular outcomes (coronary heart disease, ischaemic stroke, and vascular deaths), independent of other risk factors. Our audit project identified a deficit in current standards following an audit of adherence to lipid profile and glycated haemoglobin (HbA1c) testing in the high-risk chest pain population in our city hospital setting. We found only 49% of patients had LDL-C checked during their inpatient stay, and only 45% had HbA1c checked, of our targeted 100% of patients. This allowed the introduction of a planned intervention to improve admission testing and re-auditing demonstrated an improvement in testing, mainly driven by improved LDL-C testing. Despite this, a deficit still exists and more work is needed to meet our target of 100% compliance.
July 2025 Br J Cardiol 2025;32(3) doi:10.5837/bjc.2025.034
A concealed arrhythmia: Brugada phenocopy as a cardiac manifestation of hyperkalaemia in diabetic ketoacidosis
Attia Mustafa, Rajaa Jadulmawlay, Waleed El-Mabrouk

A 32-year-old man presented to the emergency department with shortness of breath and altered mental status. He reported a two-day history of epigastric pain, nausea, and vomiting. His past medical and family history were unremarkable. He was haemodynamically unstable, and his initial electrocardiogram (ECG) revealed a Brugada type 1 ECG pattern. The initial diagnostic assessment revealed significant metabolic derangements consistent with diabetic ketoacidosis, accompanied by hyperkalaemia. Notably, the prompt and effective management of hyperkalaemia resolved the Brugada type 1 ECG pattern, confirming the diagnosis of Brugada phenocopy.
June 2025 Br J Cardiol 2025;32:58–62 doi:10.5837/bjc.2025.025
CR in HF: impact of frailty and mobility on proportion of inpatients eligible for CR referral at the point of discharge
Hannah Waterhouse, Iain Squire, Sally Singh

Cardiac rehabilitation (ExCR) is an essential, evidence-based part of the management of people with chronic heart failure (CHF), but research indicates it is underused. This retrospective audit explores the eligibility of heart failure inpatients for ExCR, according to the European Society of Cardiology (ESC) consensus statement, and the impact of frailty on referral rates.
The first 100 patients admitted with a diagnosis of CHF from 1 February 2020 within one hospital trust were included in the audit. Only 54% of patients were eligible for ExCR at discharge and, of them, 43% were referred. Most patients (69%) admitted to cardiology wards were eligible for ExCR compared with 14% of those admitted to non-specialist care. Frail patients were less likely to be admitted to cardiology wards (43%) than their non-frail counterparts (93%).
Not all patients admitted to hospital with heart failure are eligible for ExCR, and assessing eligibility is important in identifying the true referral rate to allow national benchmarking. Interventions to improve referral are still important, but focus also needs to be directed to developing interventions for those individuals currently not eligible for standard ExCR programmes.
June 2025 Br J Cardiol 2025;32:72–6 doi:10.5837/bjc.2025.026
ACE inhibitors reduce the risk of myocardial fibrosis post-cardiac injury: a systematic review
Ahmed Ali Kayyale, Peter Timms, Han B Xiao

Myocardial fibrosis is a common pathological process associated with various cardiovascular diseases, contributing to adverse cardiac remodelling and increased morbidity. Angiotensin-converting enzyme inhibitors (ACEi) have been widely used for myocardial protection in high-risk patients. However, there are no clear recommendations for their use for the prevention of fibrosis after myocardial injury. On the other hand, procollagen type III amino-terminal propeptide (PIIIP) and procollagen type I propeptide (PIP) have been identified as effective biomarkers for predicting fibrotic change in the myocardium. It is important to evaluate the effects of ACEi by PIIIP and PIP levels to provide insights into the potential antifibrotic effects of ACEi.
We assessed the effects of ACEi on the process of fibrosis in the myocardium through serum levels of PIIIP and PIP. Four databases were searched to identify relevant studies investigating the association between the use of ACEi and myocardial fibrosis marked by PIIIP and PIP levels. Animal and non-original research articles were excluded.
Six studies with a total of 706 participants met the inclusion criteria. Three studies assessed the change of PIIIP and PIP levels in patients with hypertension, while the other three were in patients with heart failure, myocardial infarction and congenital heart diseases. The included studies demonstrated a significant reduction in PIIIP and PIP serum levels with ACEi therapy (p<0.05), except in patients with post-myocardial infarction. The mean reduction in serum PIIIP levels in all patients treated by ACEi was 20.8%.
These results suggest that ACEi can effectively inhibit collagen synthesis and deposition in the myocardium, potentially preventing, or even reversing, the progression of myocardial fibrosis. This supports the idea that ACEi have potent antifibrotic effects and can contribute to improved clinical outcomes in cardiac conditions that are not currently indicated, including myocarditis.
June 2025 Br J Cardiol 2025;32(2) doi:10.5837/bjc.2025.027
Acute myocardial infarction in a young patient with diabetes and ulcerative colitis
Chukwuemeka Lekwa, Jomith Jose, Saad Ahmad, Sunita Avinash

This case report describes a young man in his early thirties with insulin-dependent diabetes mellitus and ulcerative colitis, who developed acute myocardial infarction (AMI) during an acute flare-up of ulcerative colitis. The case highlights the diagnostic and therapeutic challenges involved in managing AMI in patients with systemic inflammatory diseases and metabolic conditions. The patient was successfully treated with a combination of thrombectomy and a drug-eluting balloon procedure for coronary occlusion, along with pharmacotherapy consisting of intravenous steroids, intravenous glycoprotein IIb/IIIa inhibitor and the involvement of a multi-disciplinary team of cardiologists and gastroenterology specialists. This case underscores the need for an integrated care approach, aggressive cardiovascular risk management, and interdisciplinary collaboration to optimise outcomes in complex clinical scenarios where systemic inflammation intersects with cardiovascular events.
June 2025 Br J Cardiol 2025;32(2) doi:10.5837/bjc.2025.028
Percutaneous valve intervention for severe mitral regurgitation complicated by lung sepsis
Farah Greiw, Shkaar Affandi, Will Wallis

Severe mitral regurgitation (MR), when complicated by a co-existing lung abscess, is a management challenge, as both conventional cardiac and thoracic surgical interventions may be contraindicated. In the case described below, transcatheter edge-to-edge mitral valve repair (TEER) was utilised to achieve haemodynamic stability, permitting subsequent thoracic surgical lung abscess resection.
We report the case of a 60-year-old man with torrential MR secondary to chordal rupture presenting with recurrent pulmonary oedema, complicated by lung sepsis and abscess formation resistant to antibiotic therapy and precluding open valvular repair. The presence of a lung abscess contraindicated open mitral valve repair, and the severity of MR precluded thoracic surgical treatment of the lung abscess, precluding any form of surgical intervention.
A successful TEER procedure resulted in a reduction of MR from severe to no more than mild-to-moderate, enabling haemodynamic stabilisation and permitting subsequent thoracic surgical treatment of the lung abscess.
Our case demonstrates the possibility of treating severe MR with TEER in the presence of a lung sepsis and abscess, when both conventional cardiac and thoracic surgical interventions were considered contraindicated. This later enabled thoracic surgery and treatment of the lung abscess.
June 2025 Br J Cardiol 2025;32(2) doi:10.5837/bjc.2025.029
Vascular terror: the strange nightmare of a knotted guidewire during central venous catheterisation
José Darío Valencia González, Eduardo Sánchez Cortes, Armando Espinosa Eugenio, Cristian Baltazar Jiménez, Raúl Cruz Palomera, Marco Antonio Morales González, Alejandro Carcaño Cuevas, Juan Guzmán Olea

A 79-year-old woman presents to the hospital with dyspnoea, fever, and hypotension, and is diagnosed with community-acquired pneumonia and septic shock. Resuscitation is initiated with fluids and vasopressors, and a central venous catheter is placed. However, during the procedure, the guide experiences resistance and cannot be removed, becoming trapped. This is confirmed with tomography and reconstruction, demonstrating intravascular position. The patient is then sent to interventional cardiology for extraction, which is successfully performed using the EN Snare (Merit Medical). The significance of this case lies in the complications of not guiding procedures with ultrasound and how to resolve them, such as the guide being trapped in this patient.
May 2025 Br J Cardiol 2025;32:49–52 doi:10.5837/bjc.2025.019
Epidemiology and aetiology of sudden cardiac death in athletes
Joseph Westaby, Mary N Sheppard

Sudden cardiac death (SCD) is a devastating and tragic occurrence that may affect individuals of all ages. It is defined as an unexpected death occurring within one hour of the onset of symptoms, if witnessed, or within 24 hours of last being seen alive and well, if unwitnessed. Athletes are considered to be the healthiest of all the population, and exercise is known to reduce the risk of atherosclerotic coronary artery disease. However, both amateur and highly trained athletes do die suddenly and unexpectedly, and this gets widespread media attention as it is so shocking and unexpected. This brings SCD, its frequency and causes into the spotlight. This review focuses on the epidemiology and aetiology of SCD in athletes from a pathological perspective.
May 2025 Br J Cardiol 2025;32:68–70 doi:10.5837/bjc.2025.021
Proton-pump inhibitors: use and effectiveness in ACS patients receiving dual antiplatelet therapy
Faisal Shehzad, Sundip Patel, Khurram Shahzad, Obi Ikechukwu

We performed a cross-sectional study to determine the frequency of use of proton-pump inhibitors (PPIs) in acute coronary syndrome (ACS) patients on dual antiplatelet therapy (DAPT) within 24 hours of hospital admission, and their effectiveness in reducing bleeding complications.
This cross-sectional study included a total of 83 patients admitted via the medical take to Queen Elizabeth Hospital, Lewisham and Greenwich Trust (LGT), London, with ACS from May 2022 to June 2022. The data of these patients were analysed to see whether ACS patients on DAPT were given PPIs within 24 hours of their hospital admission. These patients were further assessed for any bleeding event during their hospital admission and its association with the prescription of PPIs.
A significant number of ACS patients (26, 32.1%) were not prescribed PPIs within 24 hours of hospital admission. However, 55 (67.9%) patients were prescribed PPIs within 24 hours of their hospital admission. Of the 26 ACS patients not given PPIs within 24 hours of their hospital admission, three patients developed bleeding complications during their admission. Two out of the three patients developed gastrointestinal (GI) bleeding (melena) with a significant drop in their haemoglobin levels, while one patient developed haematuria.
In conclusion, a large number of patients admitted with ACS and started on DAPT did not receive a concomitant PPI within 24 hours of admission to the hospital in accordance with European Society of Cardiology (ESC) and American Heart Association (AHA) guidelines, and, as such, were at significant risk of bleeding events.
May 2025 Br J Cardiol 2025;32:63–7 doi:10.5837/bjc.2025.022
Delay to ICA for patients with NSTEMI admitted to hospitals without cardiac catheterisation facilities in SE Scotland
Man Hei Marcus Kam, Reagan Lee, Brayden Zheng Lin Ng, David Gringras, Joseph Coong, Brian Moosa, Lynn Wood, Sara Bamford, Nicholas L M Cruden, Rong Bing, Peter A Henriksen

National Institute for Health and Care Excellence (NICE) guidance recommends routine early inpatient invasive coronary angiography (ICA) for patients presenting with non-ST-elevation acute myocardial infarction acute coronary syndrome (NSTEMI-ACS) within 72 hours of hospital admission. For patients admitted to hospitals without invasive cardiac facilities, completing interhospital transfer and investigation within this timeframe is challenging. This retrospective cohort study evaluated factors influencing time to ICA, diagnosis and treatment allocation decisions in 4,087 NSTEMI-ACS patients referred from five district general hospitals to the Royal Infirmary of Edinburgh over four years. The mean time from admission to coronary angiography was 5.0 ± 3.0 days, with the majority waiting longer than the 72-hour NICE target. Admission towards the end of the week, defined as Wednesday to Saturday, was associated with longer delay. Coronary revascularisation was not required in 34% of patients. The presence of obstructive coronary disease and use of coronary revascularisation varied with age and sex, with younger female patients more likely to have normal coronary arteries or mild non-obstructive plaque disease. Use of percutaneous coronary intervention (PCI) varied with supervising consultant operator. These findings highlight disparity between clinical practice and NICE guideline recommendations for NSTEMI-ACS patients admitted to hospitals without invasive cardiac facilities, and highlight the need for the development of treatment pathways that reduce delay and better identify patients who will benefit from coronary revascularisation.
May 2025 Br J Cardiol 2025;32(2) doi:10.5837/bjc.2025.023
Devastating impact of performance-enhancing drugs: a case of severe heart failure in a young bodybuilder with body dysmorphic disorder
Ismail Sooltan, Sudantha Bulugahapitiya

A 24-year-old male bodybuilder presented with cardiac symptoms following long-term performance-enhancing drug (PED) use. He was diagnosed with heart failure with reduced ejection fraction and body dysmorphic disorder. Treatment included cardiac medical therapy and psychiatric support. After PED discontinuation and ongoing psychological care, symptoms improved and relapse was prevented. This case highlights the potential severe cardiovascular consequences of PED abuse in young, healthy individuals. It emphasises the importance of early recognition, multidisciplinary intervention addressing both physical and psychological aspects, and increased awareness about PED risks, particularly among those with body image disorders.
April 2025 Br J Cardiol 2025;32:77–80 doi:10.5837/bjc.2025.017
Effect of hyperbaric oxygen therapy on LV function in CAD patients after reperfusion based on echo: a meta-analysis
Ketut Angga Aditya Putra Pramana, Ni Gusti Ayu Made Sintya Dwi Cahyani, Yusra Pintaningrum

Hyperbaric oxygen therapy (HBOT) is successfully implemented for the treatment of several disorders. HBOT is a promising treatment modality for coronary artery disease (CAD), where outcomes are frequently poor despite early revascularisation. The aim of this study is to investigate the effect of HBOT on the left ventricular function of patients with CAD after reperfusion.
Electronic journal searching was performed in PubMed, ScienceDirect, and Cochrane to find studies that investigate the effect of HBOT on the myocardial function of patients with CAD. The primary outcomes were left ventricular end-diastolic volume (LVEDV), left ventricular end-systolic volume (LVESV), and left ventricular ejection fraction (LVEF). Meta-analyses were performed on included studies and mean differences (MD) and 95% confidence intervals (CI) were estimated using Review Manager v5.4.
A total of three observational studies enrolling 195 participants were included in our analysis. HBOT significantly increased LVEF by 4.16% in patients with CAD after revascularisation compared with non-HBOT (MD=4.16, 95%CI 0.97 to 7.34, p=0.01). There was no statistical significance observed in the HBOT versus non-HBOT comparison on LVEDV (MD=–1.63, 95%CI –6.52 to 3.26, p=0.51) and LVESV (MD=–1.58, 95%CI –4.06 to 0.90, p=0.21).
In general, this meta-analysis shows HBOT significantly increased LVEF in patients with CAD after revascularisation compared with non-HBOT. There were no significant changes in LVEDV and LVESV in the HBOT group and non-HBOT group.
April 2025 Br J Cardiol 2025;32:53–7 doi:10.5837/bjc.2025.018
Heart failure services from the community perspective in the UK: a cross-sectional survey
Jayne Masters, Chun Shing Kwok, Simon Duckett, Susan E Piper, Christi Deaton

Heart failure (HF) is a highly prevalent long-term condition, with variation in services and resources across the UK. This report provides findings from a cross-sectional survey of community HF services in the UK between September 2021 and February 2022.
Eighty-five responses describing community HF services were received. Community services were primarily led by a HF specialist nurse (HFSN), with a median of 1.25 cardiology consultants with HF training, and a variety of other nurses and support workers. All services reviewed patients with HF with reduced ejection fraction (HFrEF), only 58% reviewed patients with HF with preserved ejection fraction (HFpEF). Median wait time was 20 days, with substantially longer waits in many areas. All services accepted referrals from multiple sources. Most services provided admission avoidance (96.5%), post-discharge checks (87%), pharmacological optimisation (99%), ongoing monitoring (82%) and palliative care (87%).
In conclusion, UK community-based HF teams provide many services, however, there is significant geographical variation. Studies are needed to determine if they are adequately resourced to meet population needs and improve patient outcomes.
March 2025 Br J Cardiol 2025;32:7–11 doi:10.5837/bjc.2025.011
Diagnosis and management of ACS in patients with ESRD on haemodialysis: a comprehensive review
Muhammad Anis Haider, Muhammad Usman Shah, Xenophon Kassianides, Adil Hazara, Noman Ali, Dmitriy N Feldman

Acute coronary syndromes (ACS) are common in patients with end-stage renal disease (ESRD). Diagnosis may be challenging given diverse symptomatology, absence of classical symptoms on presentation, and difficulties in the interpretation of biomarkers. Morbidity and mortality in this patient population remain high compared with patients with normal renal function, partly due to a lack of evidence for optimal management. This review presents a summary of the diagnostic features and early management of ACS in patients with ESRD on haemodialysis.
March 2025 Br J Cardiol 2025;32:37–40 doi:10.5837/bjc.2025.013
Screening for atrial fibrillation: a narrative review
Ali Wahab, Ramesh Nadarajah, Chris P Gale

This review provides information about the current evidence-base for screening for atrial fibrillation (AF). The current burden of AF and recommendations related to AF screening are discussed, and randomised-controlled trial evidence for AF detection, clinical outcomes, harms and cost-effectiveness of population-based AF screening are reviewed. Finally, novel methods to refine the population to whom AF screening should be offered, which may improve clinical and cost-effectiveness, are considered.
March 2025 Br J Cardiol 2025;32(1) doi:10.5837/bjc.2025.014
Recurrent polymorphic ventricular tachycardia without chest pain: an unusual presentation of focal coronary artery spasm
Vikram Singh, Roger Clark, Sergey Barsamyan

Coronary artery spasm (CAS), or Prinzmetal angina, is a recognised cause of myocardial ischaemia in non-obstructed coronary arteries which typically presents with anginal chest pain. This case report describes an atypical presentation of CAS in a 68-year-old white British male with cardiovascular risk factors. The patient presented with recurrent palpitations and pre-syncope, with no chest pain. Ambulatory electrocardiography (ECG) monitoring revealed recurrent polymorphic ventricular tachycardia (PMVT). Coronary angiography identified moderate stenosis of the right coronary artery (RCA), without significant flow restriction by invasive pressure wire interrogation.
Inpatient monitoring revealed episodes of recurrent PMVT coinciding with transient inferior ST elevation and a distinct ‘shark fin’ waveform, indicating dynamic RCA occlusion. The arrhythmias persisted despite initial medical management, including calcium channel blockers and intravenous glyceryl trinitrate. Percutaneous coronary intervention to the moderate RCA lesion was performed, which definitively treated the arrhythmias.
This case emphasises the importance of recognising plaque-associated CAS as a potential trigger for life-threatening arrhythmias, even in the absence of chest pain. While medical therapy remains first-line treatment, life-threatening presentations may necessitate invasive interventions to stabilise the patient and prevent recurrence.
March 2025 Br J Cardiol 2025;32(1) doi:10.5837/bjc.2025.015
Pericardial cyst: an unexpected diagnosis in a patient presenting with breathlessness
Henry HL Wu, Omar Elboraey, Joseph Zacharias, Danielle Bury, Chee Kheng Liew, Irfan Ahmed

Pericardial cyst is a rare diagnosis, mainly considered a congenital condition. Most patients with pericardial cysts present without symptoms. Symptomatic presentation often relates to the size and location of the pericardial cyst. We report a case of a 49-year-old man who presented with subacute breathlessness in which the diagnosis of a pericardial cyst was made following various investigations – from transthoracic echocardiography and computed tomography scan to video-assisted thoracoscopic surgery biopsy, upon which a histological diagnosis was made. This case report reviews and discusses the available literature on the epidemiology and potential presenting features of a pericardial cyst, and the current recommended assessment and management strategies thereof. This case highlights the importance of effective multidisciplinary communication and joint input towards clinical decision-making, particularly in complex scenarios, to achieve optimal patient outcomes.
February 2025 Br J Cardiol 2025;32:12–3 doi:10.5837/bjc.2025.005
Turning the tide: how will novel diabetes drugs change the future management of cardiovascular disease?
Tobias MacCarthy

This article won first prize in the recent British Junior Cardiologists’ Association (BJCA) essay competition.
February 2025 Br J Cardiol 2025;32(1) doi:10.5837/bjc.2025.006
Acute type A aortic dissection with cerebral malperfusion: diagnosis and repair using a novel technique
Marina Elias, Abubakar Ibn Sidik, Sergey Garmanov, Vladimir Mironenko, Aliu Moomin

Though a rare condition, acute type A aortic dissection (ATAAD) is associated with high morbidity and mortality; hence, timely diagnosis and surgery are important to reduce the risk of mortality. If the dissection extends into the aortic arch branches, ensuring adequate cerebral perfusion during surgery is crucial to preventing stroke.
A 50-year-old man presented to the emergency department with symptoms of acute chest pain, dizziness, and headache. His blood pressure was 180/110 mmHg and heart rate was 100 bpm. He had a high blood pressure and heart rate and was initially treated with glyceryl trinitrate. Initial investigations ruled out acute coronary syndrome. Further investigations revealed ATAAD with the involvement of arch branches, an incomplete (open) circle of Willis and cerebral malperfusion. He was prepared for a branch-first total aortic arch replacement. Due to the high risk of stroke in this patient, off-pump axillo-axillary bypass (adaptive perfusion technique) was used to ensure bihemispheric cerebral perfusion throughout the surgery. The surgery was uneventful, and the patient was discharged 12 days later. Postoperative follow-up at six months was normal.
In conclusion, ATAAD is a surgical emergency that can mimic other acute thoracic conditions, such as pulmonary embolism and acute coronary syndrome; therefore, a judicious approach should be applied in the diagnosis and early management of symptoms. The reconstruction technique should be tailored to the patient’s needs; as this patient had a poorly functioning circle of Willis and cerebral hypoperfusion, continuous bilateral cerebral perfusion was essential to prevent irreversible cerebral ischaemic insult. The adaptive technique is easy to learn for surgeons who are already proficient in aortic dissection procedures, it is reproducible and requires only minor changes to the surgical setup without any substantial increase in operative time. Adoption of this technique in other surgical centres could be beneficial in increasing the success rate for the treatment of ATAAD.
February 2025 Br J Cardiol 2025;32:23–5 doi:10.5837/bjc.2025.007
Low prevalence of CRT upgrade in patients with significant RV pacing: 10-year real-world data in a UK DGH
Thet Y Hnin, Paresh A Mehta

In heart failure patients with reduced ejection fraction (HFrEF) requiring a pacemaker, biventricular cardiac resynchronisation therapy (CRT) is preferred to right ventricular (RV) pacing. Moreover, HFrEF patients who already have a conventional pacemaker in situ should be considered for CRT ‘upgrade’ in the presence of worsening symptoms and a significant proportion of RV pacing. While international guidelines are clearly defined, the ‘real-world’ prevalence of upgrading to CRT in patients with a significant proportion of RV pacing remains unclear. We aim to report the prevalence and characteristics of CRT upgrades in a UK district general hospital over a 10-year period.
We performed a retrospective univariate analysis of consecutive adult patients who underwent pacemaker implantation for Mobitz type 2 and complete atrioventricular (AV) block from January 2009 to December 2018. Over the study period, 34 patients were upgraded to CRT (prevalence 4.6%). Male patients were more likely to receive CRT upgrade (p=0.027). There was no statistically significant difference in RV-pacing burden or RV-paced QRS duration between CRT upgrade and non-upgrade groups. Patients who received CRT had lower baseline left ventricular (LV) ejection fraction than the non-upgrade group (50% vs. 60%, p=0.049).
In conclusion, this real-world study supports the notion that patients with impaired LV function and likely high requirements for RV pacing should be informed of the possible future need for device CRT upgrade. CRT should be considered upfront in selected patients with lower baseline LV systolic function.
February 2025 Br J Cardiol 2025;32:19–22 doi:10.5837/bjc.2025.008
The eye as a window to CVD: case series and literature review of retinal ischaemic perivascular lesion (RIPL)
Vanessa Yeo, Rubia Akhtar, Sobha Joseph, Yousuf Ansari

Retinal ischaemic perivascular lesions (RIPL) are characterised on spectral domain optical coherence tomography (SD-OCT) as focal thinning of the inner nuclear layer (INL) associated with outer nuclear layer (ONL) upward expansion. We present a small case series of 11 patients and reviewed all relevant original research on RIPL and its association with cardiovascular diseases (CVD). All 11 patients had RIPL incidentally identified on SD-OCT by two consultant ophthalmologists during a routine medical retina clinic. We obtained a thorough medical history to identify risk factors and CVD. The most common risk factor was type 2 diabetes mellitus (90.9%), followed by hypertension (81.9%). A diagnosis of arrhythmia was determined in 36.4% patients, coronary artery disease in 27.3%, cerebrovascular events in 36.4%, peripheral vascular disease in 27.3% and carotid artery stenosis in 8.3%. A literature search was conducted using PubMed, Google Scholar and Scopus, using all relevant key words. Seven pieces of original research were described in the literature. Six of these described a RIPL prevalence ranging from 34.62% to 91%. One paper described a case series with an incidence of 72.7% new diagnosis of CVD in their cohort who were identified to have RIPLs. The ophthalmologists’ role in detecting RIPLs could be used to assess cardiovascular risk status, supporting a multi-disciplinary approach in managing CVD.
February 2025 Br J Cardiol 2025;32(1) doi:10.5837/bjc.2025.009
Successful medical management of Wellens’ syndrome type B in an elderly patient with high procedural risk
Aqib Khan, Ismail Sooltan, Sudantha Bulugahapitiya

Wellens’ syndrome, characterised by specific T-wave changes on electrocardiogram (ECG), indicates critical proximal left anterior descending (LAD) stenosis and high acute myocardial infarction risk. While revascularisation is the standard treatment, it may be unsuitable for elderly patients with comorbidities. We present a case of successful medical management of Wellens’ syndrome type B in a 94-year-old woman deemed unfit for invasive interventions. The patient was treated with dual antiplatelet therapy, high-intensity statin, and anti-anginal medications. Symptom control was achieved, and serial ECGs and cardiac biomarkers remained stable. This case demonstrates that aggressive medical management can be a viable alternative in elderly patients with Wellens’ syndrome type B, unsuitable for invasive procedures.
January 2025 Br J Cardiol 2025;32:14–8 doi:10.5837/bjc.2025.001
Heart failure services from the hospital perspective in the UK: a cross-sectional survey
Chun Shing Kwok, Susan E Piper, Christi Deaton, Jayne Masters, Simon Duckett

Heart failure (HF) is a significant problem in the UK with variation in services across the country. Here we describe the findings from a cross-sectional survey of HF services in the UK performed between September 2021 and February 2022.
Seventy-nine responses describing hospital-based HF services from all devolved countries were received. The clinical lead in 82% of hospitals was a cardiologist with specialist interest in HF. Just over half of HF hospital services had a one-stop diagnostic clinic with a median of two clinics per week. A two-week pathway and six-week pathway were present in 78.5% and 75%, respectively. Only 4% of services met referral waiting time targets 100%, and 15% never met targets. The majority of inpatient HF services reviewed patients with primary (96%) or secondary (89%) admission for HF with reduced ejection fraction (HFrEF), corresponding percentages for HF with preserved ejection fraction (HFpEF) were 68% and 51%, respectively. HF services reported a median of two HF consultant cardiologists, five non-HF consultant cardiologists, one palliative care consultant, two band seven and one band six HF specialist nurses.
In conclusion, considerable variation in hospital-based HF services across the UK exist, which may not meet the needs of patients.
January 2025 Br J Cardiol 2025;32:36 doi:10.5837/bjc.2025.002
Patient and public perspectives of involvement in CV research in Scotland: heart engagement and research talks
Sheona McHale, Alice Pearsons, Coral Hanson, Mary McAuley, Maggie Simpson, Carol Porteous, Val Irvine, Roisin Houston, Paula Henderson, Lis Neubeck

Cardiovascular disease (CVD) is a leading cause of global mortality, necessitating extensive research efforts. In Scotland, the NHS Research Scotland (NRS) Cardiovascular Network plays a pivotal role in coordinating cardiovascular research. Patient and public involvement (PPI) is crucial for shaping meaningful research strategies, yet barriers to such engagement persist.
We organised a hybrid PPI event, bringing together patients, researchers, and stakeholders. Interactive sessions explored barriers and enablers of PPI. Qualitative and quantitative data were collected, focusing on communication, commitment, and value as key themes.
Participants highlighted communication challenges, emphasising the need for clear, accessible information about research involvement. Commitment barriers included costs, travel, and time constraints. Feeling valued as research participants was essential, emphasising recognition of diverse experiences. Running the event as a hybrid facilitated broader participation, employing professional notetakers, British sign language (BSL) interpreters, and moderators.
In conclusion, holding this event emphasised the importance of PPI in cardiovascular research, outlining communication, commitment, and value as key facets. Hybrid events enhance inclusivity but demand careful planning. Meaningful PPI, as exemplified in this study, informs and enhances research quality, underscoring the need for continued investment in patient involvement initiatives.
January 2025 Br J Cardiol 2025;32:31–5 doi:10.5837/bjc.2025.003
Predictors of requirement for urgent versus elective TAVI and comparison of short and medium outcomes
Elliott J Carande, Keiron Morgan, Chayanee Leenachunangkool, Joy Shome, Ahmed Hailan, Ayush Khurana, Dave Smith, Alexander Chase, Daniel R Obaid

Previous studies have shown mixed results comparing short-term mortality in patients undergoing urgent transcatheter aortic valve implantation (Urg-TAVI) compared with elective procedures (El-TAVI) for severe aortic stenosis (AS). This study aimed to explore the predictors of requirement for Urg-TAVI versus El-TAVI, as well as compare differences in short- and intermediate-term mortality.
This single-centre, retrospective cohort study investigated 358 patients over three years. Baseline demographic data were collected for patients undergoing elective and urgent procedures, and mortality outcomes at one-month, one-year and three-year follow-up were compared.
Urg-TAVI was required in 131 (36.6%) patients. Patients undergoing Urg-TAVI were significantly more likely to be female, have poor left ventricular (LV) function, with higher baseline creatinine and higher clinical frailty score (CFS). Higher rates of vascular complications were independently associated with increased mortality at one month. Mortality at one year was associated with higher creatinine level (odds ratio [OR] 1.01, 95% confidence interval [CI] 1.00 to 1.01, p=0.0013) and an urgent procedure (OR 2.25, 95%CI 1.28 to 3.97, p=0.0048). There remained a higher mortality in the urgent patients at three-year follow-up.
In conclusion, undergoing TAVI urgently did not have a statistically significant effect on 30-day mortality. However, over long-term follow-up of one year, it was associated with worse mortality than elective TAVI, and this persisted out to three years.
January 2025 Br J Cardiol 2025;32:26–30 doi:10.5837/bjc.2025.004
Finding Fabry: a survey on missed opportunities for detection and diagnosis of Fabry disease in patients with LVH
Hibba Kurdi, Henry Procter, Matthew Aldred, Katie Linden, Angela Langton, Akriti Naraen, Kathryn Abernethy, Sabrina Nordin, Ashwin Roy, Ben Leach, James Moon, Derralynn Hughes

Fabry disease (FD), resulting from alpha-galactosidase A enzyme deficiency, remains underdiagnosed despite readily available methods for diagnosis. This multi-centre prospective survey across six tertiary centres aimed to determine the level of consideration of FD in patients presenting with left ventricular hypertrophy (LVH). LVH was defined according to the guidelines of the European Society of Cardiology (ESC) and the American College of Cardiology/American Heart Association (ACC/AHA) for the management of cardiomyopathies, where LVH is diagnosed if the left ventricular wall thickness exceeds 15 mm in any segment or exceeds 13 mm in the presence of a known diagnosis in a first-degree relative. Of 143 patients surveyed, only three with LVH underwent diagnostic testing for FD, all testing negative. Moreover, 44% of patients with LVH had an ambiguous aetiology, highlighting possible missed FD diagnostic opportunities. A discrepancy was observed between electrocardiogram (ECG) results and echocardiography or cardiac magnetic resonance (CMR) in diagnosing LVH, emphasising the need for comprehensive cardiac imaging. This project highlights the urgent requirement to amplify FD awareness, especially in patients with LVH, to ensure early intervention and better patient outcomes.
December 2024 Br J Cardiol 2024;31:136–8 doi:10.5837/bjc.2024.052
A UK-wide prospective assessment of donor heart echocardiography pathway
Waqas Akhtar, Ashok Padukone, Rachel Rowson, Helen Buglass, Thomas Billyard, Reinout Mildner, Marcus Peck, Marian Ryan, Christopher Gough, Fernando Riesgo Gil, Marius Berman, Antonio Rubino

This study aimed to understand the national echocardiography assessment pathway in heart donation. We carried out a prospective national specialist nurses in organ donation (SNOD) audit of UK donor offers between 20 August and 31 November 2022, and a prospective national recipient transplant centre audit of all donor offers between 22 September and 19 December 2022.
The SNOD audit identified median time delay between requesting and performing an echocardiogram of 17.9 hours (interquartile range [IQR] 13.9–33.2). The staff group performing the echo were a cardiac physiologist in 57% (17/30) of cases and a medical doctor in 43% (13/30) of cases. Only 30% (9/30) of providers held comprehensive accreditation, 13% (4/30) were focused accredited, 33% (10/30) had no accreditation, and 23% (7/30) were unknown. Only 50% (15/30) of images were transferred for review to the transplant centre. Images were transferred via email (10/15, 67%), WhatsApp (4/15, 27%) and a standard picture archiving system (PACS) (1/15, 3%).
The transplant centre audit revealed that in 21% of donors, the transplant team felt that the echo performed at the referring centre contained inadequate information, and in 11% of donors, no echo was performed at all. Only 52% of potential donors had echo images available for direct review by the transplant centre. In 17% of cases, the transplant team felt that if good quality echo data and imaging had been available, the decision regarding mobilising the retrieval team may have been altered.
In conclusion, to improve donor heart utilisation rates we believe there is a need to recognise the contribution of focused echo and improve guidance for echo image acquisition. There is also a need for a robust system for image transfer to transplant centres.
December 2024 Br J Cardiol 2024;31:144–9 doi:10.5837/bjc.2024.053
Evaluating real-world mortality risk after defibrillator implantation
Lisa W M Leung, Zaki Akhtar, Oswaldo Valencia, Genevieve Shouls, Rabia Warraich, Jennifer Vara, Sue Jones, Pamala Kanagasabapathy, Mark M Gallagher, Nesan Shanmugam

Protection against the increased risk of sudden cardiac death (SCD) due to ventricular arrhythmias is offered by the implantation of cardiac defibrillators. A life-expectancy of less than one year is usually a contraindication to the implantation of these devices. We evaluated the outcomes of all those who received defibrillator implantation for any clinical indication at our centre in the same year that early (<12 months) death notifications occurred.
This is a single-centre retrospective study on the outcomes of all patients who had a transvenous defibrillator implant in 2015. All transvenous defibrillator devices implanted for both primary and secondary prevention of SCD were included. Patient demographic data and device data were studied.
Data from 235 patients were analysed. In a follow-up period of 66.2 ± 3.8 months, 77 (32.8%) of the study cohort died; 20 (8.5%) of these patients died less than 12 months post-implant. None of the deaths were directly arrhythmia related. Factors that were significant in predicting mortality included age and ejection fraction <35% (p<0.01). From a pre-procedure biomarker perspective, an increased red cell distribution width (RDW) was strongly associated with early mortality risk on univariate and multi-variate analysis (p<0.001). Receiver operator characteristics (ROC) curve analysis found that the optimal cut-off for RDW was 14.75% (area under curve 0.75; sensitivity 0.69; specificity 0.77; p<0.001).
In conclusion, there are limitations in fully assessing patient prognosis despite current guidance. Universal clinical frailty scores that incorporate biomarkers may be helpful in enhancing this pre-assessment process to improve the evaluation of the risk of early non-arrhythmic-related death for implantable cardioverter defibrillator candidates.
December 2024 Br J Cardiol 2024;31:160 doi:10.5837/bjc.2024.054
AV nodal ablation, where are we now? Insight from real-world Northern Irish multi-centre registry data
James Mannion, Niall Leahy, Kathryn Hong, Sean Esmonde

Atrioventricular nodal (AVN) ablation with permanent pacemaker implantation – ‘pace and ablate’ – may be considered for patients with symptomatic atrial fibrillation (AF) for whom rhythm control has been unsuccessful. This creates concerns about inducing pacemaker dependence and potential pacemaker-induced cardiomyopathy (PICM). Conduction-system pacing mitigates PICM, so we expect a greater uptake of AVN ablation going forward.
We conducted a retrospective multi-centre review of our patients who underwent AVN ablation over a one-year period. AVN ablation was successful with durable lesions at one year. Radiofrequency energy was utilised in all patients, with a median application time of 2.67 minutes. Median procedure time was found to be 55.5 minutes and fluoroscopy median of 3.5 minutes. Median radiation dose was 11 mGy. We found no acute or subacute complications up to three months.
In conclusion, our right-sided approach for ablation, staged post-device insertion demonstrated results in keeping with other centres in the UK and Europe. We expect our current practice to become more widespread, given the increased risk of lead-related complications or failures associated with physiological pacing compared with standard pacing methods.
December 2024 Br J Cardiol 2024;31(4) doi:10.5837/bjc.2024.055
A case of myocarditis and associated atrioventricular heart block: a diagnostic conundrum
Louis Graham-Hart, Wai Nyunt Thinn, Kaushik Guha

The combination of atrioventricular (AV) block – specifically high-grade AV block– within the setting of myocarditis, is a rarely encountered clinical phenomenon. It is commonly encountered in infiltrative cardiomyopathies but may be associated with myocarditis.
Beyond conventional investigation and consideration of endomyocardial biopsy, there is a paucity of data to guide clinicians with regards to the issue of heart rhythm disorder. Options include a ‘watch-and-wait’ policy, anti-arrhythmic drugs, consideration of a permanent pacemaker or, alternatively, a wearable or implantable cardioverter-defibrillator (ICD).
The case encapsulates the difficulties facing clinicians with such pathology and the need to further investigate and risk stratify such patients.
December 2024 Br J Cardiol 2024;31(4) doi:10.5837/bjc.2024.056
A rare case of hypereosinophilic endomyocardial fibrosis due to PCM1-JAK2
Hannah Cooke, Amy Burchell

Endomyocardial fibrosis is a common cause of restrictive cardiomyopathy worldwide, but rarely occurs in patients living outside tropical regions.1 Herein is the first published case report of a 48-year-old woman with endomyocardial fibrosis due to hypereosinophilia secondary to a rare chromosome 8 and 9 PCM1-JAK2 translocation.
December 2024 Br J Cardiol 2024;31(4) doi:10.5837/bjc.2024.057
A tale of two hearts
Amar Ahmed, Waqas Akhtar, Tarun Mittal, David Jones, Fernando Riesgo Gil, Andrew Morley-Smith, Owais Dar

A 74-year-old man with a heterotopic heart transplant experienced alternating episodes of sustained native heart ventricular tachycardia and prolonged asystole. These were managed with cardioversion, drug therapy and pacemaker insertion. The unique physiology in such patients lends itself to numerous clinical considerations that would otherwise be routine management for most.
November 2024 Br J Cardiol 2024;31:150–4 doi:10.5837/bjc.2024.046
SGLT2 inhibitors: between the zeal of the clinical studies and the challenges of the day-to-day practice
Mohamed ElRefai, Mohamed Abouelasaad, Alice Zheng, Chitsa Seyani, Amy Greenwood, Hari Johal, Jake Hudson, Claire O’Dowling, Chris Young, Paul Haydock

Sodium-glucose cotransporter type 2 inhibitors (SGLT2i) have demonstrated efficacy in reducing cardiovascular deaths and hospitalisations associated with heart failure patients. Despite well-established benefits observed in clinical trials, their real-world application remains underexplored. The purpose of this quality improvement project was to investigate and address the gap between evidence-based guidelines and the practical application of SGLT2i therapy in patients with heart failure with reduced ejection fraction (HFrEF).
The medical records were assessed in retrospect for HFrEF-related admissions at our cardiac centre. The main target of assessment was the dapagliflozin prescriptions in eligible patients. After the first cycle of data collection and analysis, several interventions, in the form of targeted teaching, empowering pharmacists, and utilising digital tools, were employed to improve compliance with prescriptions. After the implementation of our measures, a further cycle of data collection and analysis was carried out.
In the first cycle, 31% of 225 HFrEF patients, aged 74 ± 15 years, received dapagliflozin or had plans for its initiation. Prescription rates were influenced by age (mean 69 vs. 76 years, p<0.001) and admission under cardiology (70% vs. other specialties, p<0.001), while gender and diabetes had no impact. In the second cycle, 52% of 172 HFrEF, aged 74 ± 14 years, received dapagliflozin or had plans for its initiation. Prescription rates correlated with age (71 vs. 79 years, p<0.001) and admission under cardiology (59% vs. other specialties, p=0.002), with male patients more likely to be initiated on dapagliflozin (p=0.005).
Our quality improvement project sheds light on the challenges and opportunities in implementing dapagliflozin therapy for patients with HFrEF in a real-world clinical setting. The interventions introduced led to a substantial improvement in prescription rates, indicating the potential for positive change. There is a need for ongoing efforts to bridge the gap between evidence-based guidelines and clinical practice.
November 2024 Br J Cardiol 2024;31:139–43 doi:10.5837/bjc.2024.047
Devising and delivering the UK’s first nurse-led cardiac catheter laboratory radial access programme
Dorota Wojcik, Rithik Mohan Singh Sindhi, Mahmood Ahmad, Tim Lockie, Roby Rakhit, John Gerry Coghlan

Traditionally, radial artery access (RAA) has been an exclusively ‘physician-delivered’ service, but with adequate training, nurse-led arterial cannulation can become widely adopted. In this clinical audit, senior nursing practitioners with at least two years of catheter lab experience, were offered RAA training. In phase 1 of training, two nurses were initially familiarised with a well-structured training protocol. Each of the two nurses carried out the first 50 RAA procedures under supervision on elective patients. In phase 2, candidates independently performed 100 procedures. The success and complication rates of these procedures were evaluated prior to their sign-off as competent. The procedural efficacy of nurses was compared with medical registrars of the department to assess the measures of patient satisfaction and time elapsed prior to the insertion of sheath.
During the first 100 directly observed RAA procedures, nurse 1 and nurse 2 achieved success rates of 84% (42/50 procedures) and 86% (43/50 procedures), respectively. During the second phase, nurse 1 achieved a success rate of 82% (82/100 procedures), whereas nurse 2 achieved a success rate of 97% (97/100 procedures). Overall, a success rate of 88% was achieved in the first 300 patients. No significant complications were noted. In contrast to medical registrars, nurse-led cannulation was associated with a greater extent of patient satisfaction, reduced pain intensity (p<0.001), and decreased patient-on-table to sheath insertion intervals (p<0.001). During embedding of the programme, the two nursing practitioners trained additional nurses. Of the five nurses that subsequently entered into training, two have successfully completed both training phases while a further three have completed phase 1. To date, an overall success rate of 91.1% (1,307/1,435 procedures) has been documented.
In conclusion, a nurse-led RAA program is feasible, with satisfactory success rates, no significant complications, and improved rates of patient satisfaction.
November 2024 Br J Cardiol 2024;31(4) doi:10.5837/bjc.2024.049
Tricuspid valve endocarditis presenting as multifocal cavitating pneumonia
Arun Kumar Baral, Michael Connolly

A young man with multifocal cavitating pneumonia presented with early abscess formation secondary to Staphylococcus aureus bacteraemia treated with intravenous (IV) flucloxacillin. Further workup with transthoracic echocardiography revealed a large vegetation on the tricuspid valve with at least moderate tricuspid regurgitation; however, there were no peripheral stigmata of infective endocarditis. There was no history of intravenous drug use, but he had a history of administering frequent intramuscular recreational steroid injections. He also had a recent history of a loose tooth. In addition, there were multiple skin excoriations from scratching related to anxiety. Transoesophageal echocardiography confirmed two vegetations on the tricuspid valve, the largest measuring 21 mm with evidence of severe tricuspid regurgitation. The findings were discussed in the cardiac surgery multidisciplinary meeting and the consensus was for initial sterilisation with IV antibiotics followed by surgery.
November 2024 Br J Cardiol 2024;31(4) doi:10.5837/bjc.2024.050
Transient T-wave oversensing as a result of COVID-19: a case report
Zeyad Khalil, Dixon Ward, Cristiana Ribiero, Antony French

This case report explores the effects of myocarditis induced by coronavirus disease 2019 (COVID-19) on a cardiac implanted electronic device (CIED) and its ability to differentiate depolarisation and repolarisation. Through the modification of the device settings, inappropriate CIED discharges were prevented for the duration of the illness in this 76-year-old male patient. This provides supporting evidence to consider episodes of acute COVID-19 as a cause for T-wave oversensing (TWOS).
October 2024 Br J Cardiol 2024;31:129–35 doi:10.5837/bjc.2024.041
Cardiorenal effects of therapies for type 2 diabetes and obesity
Clifford J Bailey, Caroline Day

Sodium-glucose cotransporter type 2 (SGLT2) inhibitors and glucagon-like peptide-1 (GLP-1) receptor agonists are established glucose-lowering and weight-lowering agents used in the management of type 2 diabetes mellitus and obesity. Several recent clinical trials have provided evidence that these agents can decrease the risk of, and slow progression of, cardiovascular and renal diseases independently of their glucose-lowering and weight-lowering effects. In clinical trials and ‘real-world’ observational studies in people with and without diabetes, SGLT2 inhibitors have offered protection against heart failure and chronic kidney disease, while GLP-1 receptor agonists have been associated with reductions in atherosclerotic cardiovascular events and albuminuria. Based on this evidence, SGLT2 inhibitors and GLP-1 receptor agonists can now be considered for use beyond diabetes and obesity as new treatment options in the management of cardiorenal disease.
October 2024 Br J Cardiol 2024;31:155–9 doi:10.5837/bjc.2024.043
Long-term blood pressure variability: an emerging cardiovascular risk factor
Allis Lai, Lawrence Lam, Akshita Raminemi, Akhil Sonecha, Peter Sever

Clinical trials and observational studies have demonstrated that long-term systolic blood pressure variability derived from repeated measurements of visit-to-visit clinic blood pressure is an important predictor of cardiovascular outcomes, independent of average levels of systolic pressure. Even in patients with well-controlled blood pressure (<140/90 mmHg), high systolic blood pressure variability confers an increased risk of cardiovascular events. Systolic blood pressure variability is currently derived from several measurements of visit-to-visit clinic blood pressure and expressed as the standard deviation of systolic pressure. Values in excess of 12 are indicative of high systolic blood pressure variability. Ongoing studies aim to determine whether home blood pressure monitoring may be an alternative way of measuring blood pressure variability. Evidence from several clinical trials shows that long-acting calcium-channel blockers, such as amlodipine, and thiazide-like diuretics are the only antihypertensive drugs that reduce long-term systolic blood pressure variability, and should be used preferentially in patients with high variability.
October 2024 Br J Cardiol 2024;31(4) doi:10.5837/bjc.2024.044
Subclavian venoplasty for device implantation in a district general hospital: a case series
Muhammad Usman Shah, Kelvin Lee, Hira Yousuf, David Morgan, Juan Fernandez

Subclavian venoplasty is commonly performed for subclavian vein stenosis in patients with long-term dialysis lines or fistulae. Such stenosis may also occur in patients with previously implanted intra-cardiac devices. It poses a problem if a further device upgrade or implantation is planned as the stenosis restricts the advancement of leads. Venoplasty before device implantation may provide a feasible alternative to lead tunnelling or extraction, which have their limitations. Four cases of varying complexities and devices that were implanted in patients with subclavian stenosis are presented herein. These were done in a district general hospital within the cardiology team. Venoplasty was performed using peripheral angioplasty balloons after which the device was implanted. All cases were performed successfully without any immediate complications with the patients discharged home the same day. These cases show the utility of subclavian venoplasty in facilitating device implantation without the need to utilise contralateral venous access, hence preserving venous access for the future. Additionally, they illustrate that this may be performed locally in a district general hospital setting, where appropriate expertise is available, with a high success rate and without the need to refer patients to an alternate tertiary care institute which may be associated with additional difficulties for the patient. To the best of our knowledge, this is the first instance where several cases of this procedure were performed successfully in a secondary care setting.
October 2024 Br J Cardiol 2024;31(4) doi:10.5837/bjc.2024.045
Sudden cardiac death associated with a pathogenic genetic variant in HCN4
Gokul Parameswaran, Edward Blair, Hugh C Watkins, Julian OM Ormerod

Pathogenic genetic variants in the HCN4 (hyperpolarisation-activated and cyclic nucleotide-gated channel) gene can cause sinus node dysfunction, disrupting the function of the pacemaker region of the heart. Patients with such variants can present with a wide spectrum of arrhythmias but sudden death is generally considered rare. We report two cases from the same family with different outcomes to highlight a potential high-risk phenotype in HCN4-related disease.
September 2024 Br J Cardiol 2024;31:106–110 doi:10.5837/bjc.2024.037
Lessons learnt from HF coding in primary care. What might best practice look like?
Amanda Crundall, Mary Crawshaw-Ralli, Ahmet Fuat, Jaya Authunuri, Kavita Oberoi, Jo Crossan, Sharon Jones

Heart failure (HF) is a prevalent and complex condition that demands precise and efficient management. This paper delves into a critical, yet often under-recognised, challenge in HF care – the accurate coding of patients on HF registers. We explore how discrepancies in coding, including missing patients and incorrect HF type classifications, can significantly impact patient management. The experiences of our healthcare system’s staff are examined to shed light on the real-world implications of these issues.
Clinicians and administrative staff in primary care can play a pivotal role in identifying, monitoring, and ensuring the accuracy of patient coding. By sharing their insights, we uncover the intricacies of addressing coding discrepancies and strategies suggested to optimise patient management. Furthermore, we investigate the technology and systems in place to aid staff in this endeavour.
This paper aims to contribute to the broader healthcare community’s understanding of the challenges related to coding accuracy in HF registers and to offer insights into potential solutions. By rectifying these coding discrepancies, we can enhance patient care, minimise potential oversights, and ultimately improve outcomes for individuals living with HF. Our findings underscore the significance of ensuring that no HF patient is missed or misclassified, emphasising the need for continued improvement in this vital aspect of HF care.
September 2024 Br J Cardiol 2024;31:111–4 doi:10.5837/bjc.2024.038
Navigating the research landscape in cardiology. Part 4: beyond the finish line
Hibba Kurdi, William Fowkes, C Fielder Camm

In this four-part editorial series, we have looked at the significance of research within cardiology training in the UK. The first three instalments explored the impact of research on a career in cardiology, identified the diverse research avenues, and provided guidance on navigating the application process. In the final part of this series, our focus shifts to post-higher degree opportunities within the field, and discuss the skills developed in research that can be applied to clinical practice.
August 2024 Br J Cardiol 2024;31:92–7 doi:10.5837/bjc.2024.031
Artificial intelligence in heart valve disease: diagnosis, innovation and treatment. A state-of-the-art review
Paul Bamford, Amr Abdelrahman, Christopher J Malkin, Michael S Cunnington, Daniel J Blackman, Noman Ali

In recent years, artificial intelligence (AI) has been used to improve the precision of valvular heart disease diagnosis and treatment. It has the ability to identify and risk stratify patients with valvular heart disease and holds promise in improving the innovation of new treatments through shorter, safer and more effective clinical trials. AI can help to guide the treatment of patients with valvular heart disease, by aiding in optimal device selection for transcatheter valvular interventions and, potentially, predicting the risk of specific complications. This review article explores the various potential applications of AI in the diagnosis and treatment of valvular heart disease in more detail.
August 2024 Br J Cardiol 2024;31:101–5 doi:10.5837/bjc.2024.032
Rehospitalisation rates of heart failure patients treated with SGLT2 inhibitors as an inpatient versus post-discharge
Roy Bo Wang, Michelle Che Ting Yick, Martin Thomas, Simon Woldman, Ceri Davies, Sveeta Badiani, Debashish Das, Paul Wright, Sotiris Antoniou, Christopher Primus, Francesco Papalia, Angela Gallagher, Shanti Velmurugan

Sodium-glucose cotransporter-2 inhibitors (SGLT2i) have been shown to reduce cardiovascular rehospitalisation in heart failure with reduced ejection fraction (HFrEF) patients. However, it is unknown whether initiating SGLT2i during an inpatient stay for a HFrEF exacerbation results in better outcomes versus initiation post-discharge in a cohort of diabetic and non-diabetic patients. This study compares cardiovascular rehospitalisation, heart failure specific rehospitalisation, cardiovascular death, and all-cause death between patients initiated on SGLT2i as an inpatient versus post-discharge.
A retrospective study of four hospitals in England involving 184 patients with HFrEF exacerbations between March 2021 and June 2022 was performed. Cardiovascular rehospitalisation, heart failure specific rehospitalisation, cardiovascular death, and all-cause death were compared between the two groups using Cox regression. A Cox proportional-hazards model was fitted to determine predictors of cardiovascular rehospitalisation.
There were 148 (80.4%) individuals who received SGLT2i as an inpatient, while 36 (19.6%) individuals received SGLT2i post-discharge. Median follow-up was 6.5 months for inpatients and 7.5 months for post-discharge patients (p=0.522). SGLT2i inpatients had significantly reduced cardiovascular rehospitalisations (22.3%) versus post-discharge patients (44.4%) (p=0.005), and significantly reduced heart failure specific rehospitalisations (10.1%) versus post-discharge patients (27.8%) (p=0.018). There was no significant difference in all-cause death (p=0.743) and cardiovascular death (p=0.816) between the two groups. Initiating SGLT2i post-discharge was an independent predictor of cardiovascular rehospitalisation (hazard ratio 2.40, 95% confidence interval 1.31 to 4.41, p=0.005).
In conclusion, inpatient SGLT2i initiation for HFrEF exacerbations may reduce cardiovascular and heart failure specific rehospitalisation versus initiation post-discharge. In the absence of contraindications, clinicians should consider initiating SGLT2i once patients are clinically stable during inpatient HFrEF admissions.
August 2024 Br J Cardiol 2024;31:98–100 doi:10.5837/bjc.2024.033
Randomised trial of app-led motivational support for patients with AF to promote weight loss (MOTIVATE-AF)
Thomas A Slater, Evelyn Manford, Lucy Leese, Michael Wilkinson, Muzahir H Tayebjee

Atrial fibrillation (AF) is responsible for significant patient morbidity, and obesity is a major contributor to AF incidence and symptom burden. Weight loss has been shown to positively modify AF symptoms, but weight loss in a real-world population is often only temporary. This randomised study set out to examine if smartphone-based app technology could increase weight loss in a patient population with obesity and AF.
Individuals were screened following outpatient referral to Leeds Teaching Hospitals NHS Trust for symptomatic AF. Block randomisation was performed to allocate the treatment groups to either clinical follow-up or app-based follow-up, with weight loss updates planned fortnightly. Patients randomised to clinical follow-up received nurse-led telephone calls every two weeks, while those in the app arm received automated reminder messages every two weeks. Final follow-up at six months included clinical and weight data and a quality-of-life questionnaire.
Sixty-four patients underwent randomisation. No significant difference in weight loss was seen between the groups. Patient engagement was far more consistent in the telephone follow-up group.
In conclusion, no significant difference in weight loss was seen between the two groups, despite patient education on the value of weight loss to improve their AF symptoms.
August 2024 Br J Cardiol 2024;31:115 doi:10.5837/bjc.2024.035
Impact of obesity on echocardiographic parameters in individuals free of CVD using anthropometric measurements
Leila Bigdelu, Seyed Mahdi Majidi Talab, Muhammad Usman Shah, Parisa Niknafs, Majid Khadem Rezaiyan, Syed Yaseen Naqvi

Obesity is a global pandemic and is a recognised risk factor for cardiovascular diseases. However, its impact on cardiac structure and function using echocardiography, as well as its association with anthropometric parameters in otherwise healthy individuals, requires further investigation. Therefore, we conducted an observational study with a cohort of 196 participants, comparing various echocardiographic parameters in normal weight individuals and those who were overweight or obese but had no other risk factors. Our findings revealed that obese participants had significant changes in echocardiographic measurements of the structure and functions of the left ventricle, left ventricular global longitudinal strain, left atrium, right ventricle and right ventricular global longitudinal strain compared with the control group. Body surface area and body mass index were important anthropometric features that correlated with the above echocardiographic changes, and should be routinely evaluated to assess cardiovascular risk in patients. Further larger studies are necessary to determine the clinical significance of the echocardiographic changes observed in obese individuals and their impact on health.
July 2024 Br J Cardiol 2024;31:116–9 doi:10.5837/bjc.2024.028
Correlation between simplified treadmill score, significantly stenosed blood vessels and SYNTAX score in CAD
Yusra Pintaningrum, Jeffrey D Adipranoto, Ketut Angga Aditya Putra Pramana

The purpose of this study was to determine the correlation between the simplified treadmill score (STS) and both the number of blood vessels with significant stenosis and the severity of the SYNTAX score in patients with coronary artery disease (CAD). This was an observational, cross-sectional study conducted at Dr. Soetomo General Hospital and Premier Surabaya Hospital in Indonesia from January 2011 to February 2012.
The results of the analysis using the Spearman correlation showed that there was a strong positive relationship between STS and the number of blood vessels with significant stenosis (rs=0.616 and p<0.001). Similarly, the relationship between STS and SYNTAX score obtained (rs=0.500 and p<0.001) indicates a fairly strong positive relationship.
In conclusion, there is a significant correlation between the STS as a clinical reference for estimating the probability of CAD through a weight-training test with the number of blood vessels experiencing significant stenosis.
July 2024 Br J Cardiol 2024;31(3) doi:10.5837/bjc.2024.029
Simultaneous Takotsubo syndrome and spontaneous coronary artery dissection: a case report
Carla Oliveira Ferreira, Cátia Costa Oliveira, Carlos Galvão Braga, Jorge Marques

A 59-year-old woman presented to the emergency room with sudden onset of retrosternal thoracic pain following emotional stress. The electrocardiogram (ECG) revealed T-wave inversions on precordial leads. Her blood analyses demonstrated elevation of myocardial necrosis markers (peak of troponin I of 3.4 ng/ml). Transthoracic echocardiogram (TTE) findings were consistent with Takotsubo syndrome, accompanied by mild left ventricular dysfunction. The patient underwent invasive coronary angiography revealing a spontaneous coronary artery dissection in the left anterior descending artery and left main artery. A repeat TTE one week later showed complete resolution of the segmental contractility with a full recovery of left ventricular function. Cardiac magnetic resonance imaging revealed no abnormalities. The patient was discharged on dual-antiplatelet therapy. A follow-up coronary angiography performed one month later confirmed complete resolution of the dissection. Takotsubo syndrome and spontaneous coronary artery dissection predominantly affect women and share common triggers. This case highlights the often misdiagnosed association and emphasises the specific diagnosis and treatment nuances associated with it.
July 2024 Br J Cardiol 2024;31(3) doi:10.5837/bjc.2024.030
Shortness of breath caused by a right ventricular metastasis: a case report
Muhammad Qasim Shahid, Suat Loo

Cardiac metastases normally reflect diffuse metastatic spread of the primary tumour and are rarely found in isolation. We present a case of a 71-year-old man with a history of completely resected high-grade spindle cell sarcoma of the left thigh, who presented with shortness of breath, and was found to have a large right ventricular mass, subsequently diagnosed as a metastasis of the prior sarcoma. It was deemed inoperable and incurable, and the patient was offered palliative chemotherapy. Unfortunately, the patient died within four months of his original presentation.
June 2024 Br J Cardiol 2024;31:58–60 doi:10.5837/bjc.2024.022
Reducing heart failure deaths by 25% in 25 years: the ‘25in25’ heart failure summit
Lucy Beishon, Rebecca Jayasinghe, Carys Barton, Shahbaz Roshan-Zamir

Heart failure (HF) is a major cause of morbidity and mortality in older people, and 80% of people with HF are aged over 60 years. HF is the end point for almost all common cardiovascular diseases, as well as many non-cardiovascular diseases. Despite this, HF remains underdetected and undertreated. Detection and treatment of HF has improved significantly in recent years, with several novel treatments developed in the last decade improving outcomes for patients. Therefore, earlier detection and improved treatment of HF has the potential to reduce morbidity and mortality for older people, particularly given the shift in ageing demographics anticipated over the coming decades. The British Geriatrics Society Cardiovascular Specialist Interest Group recently participated in the British Society for Heart Failure (BSH) ‘25in25’ Heart Failure Summit, which aims to reduce deaths due to HF by 25% in the next 25 years. The 2023 summit comprised experts from over 45 top health organisations across Europe, Canada and the US. The summit brought together cross-disciplinary expertise to support the implementation of strategies to improve outcomes for people living with HF, and, in this commentary, we reflect upon the priorities identified. We discuss the current barriers to the early detection and management of HF, and the particular challenges and complexity of managing HF in older people. Finally, we discuss the role of patient empowerment and how this can lead to improved care for older people living with HF.
June 2024 Br J Cardiol 2024;31:65–8 doi:10.5837/bjc.2024.023
The 2023 ESC heart failure guideline update and its implications for clinical practice
Ameer Rashed, Mohammad Wasef, Paul R Kalra

In this article we focus on areas of the European Society for Cardiology (ESC) heart failure guideline 2023 update that will be most relevant in the day-to-day management of patients with heart failure. These include an expanded indication for sodium-glucose cotransporter 2 (SGLT2) inhibitors and intravenous iron, together with rapid optimisation of foundation therapies. With important outcomes for patients, there will undoubtedly need to be modifications to service delivery to ensure that they are widely available for patient benefit.
June 2024 Br J Cardiol 2024;31:80 doi:10.5837/bjc.2024.024
Emergency pacemaker implantation in nonagenarians with CHB: single- versus dual-chamber pacing
Edd Maclean, Karishma Mahtani, Maurizio Parker, Rohan Vyas, Roy Bo Wang, Marina Roelas, Nikhil Ahluwalia, Vijayabharathy Kanthasamy, Antonio Creta, Malcolm Finlay, Ross J Hunter, Syed Ahsan, Mark J Earley, Pier D Lambiase, James Elliott, Filip Zemrak, Amal Muthumala, Philip Moore, Simon Sporton, Anthony Chow, Christopher Monkhouse

In ambulatory patients with complete heart block (CHB), dual-chamber (DDD) pacing confers physiological benefits versus single-chamber (VVI) pacing, however, the impact on mortality is disputed. Nonagenarians constitute an expanding proportion of pacemaker recipients, yet data on device selection and outcomes are limited, especially in emergency situations.
In nonagenarians with emergent CHB, we compared the clinical characteristics and outcomes of patients receiving VVI versus DDD pacemakers. Cox proportional-hazards analysis examined all-cause mortality and death from congestive cardiac failure (CCF).
There were 168 consecutive patients followed-up for 30.6 ± 15.5 months. Of these, 22 patients (13.1%) received VVI pacemakers; when compared with DDD recipients, these patients had similar median age (93 vs. 91 years, p=0.15) and left ventricular (LV) systolic function (LV ejection fraction [EF] 49.2% ± 9.7 vs. 50.7% ± 10.1, p=0.71), but were more frail (Rockwood scale 5.2 ± 1.8 vs. 4.3 ± 1.1, p=0.004) and more likely to have dementia (27.3% vs. 8.9%, p=0.011). Post-implant, device interrogation demonstrated that VVI recipients had higher respiratory rates (21.3 ± 2.4 vs. 17.5 ± 2.6 breaths per minute, p=0.002), lower mean heart rates (65.5 ± 10.1 vs. 71.9 ± 8.6 bpm, p=0.002), and lower daily activity levels (0.57 ± 0.3 vs. 1.5 ± 1.1 hours of activity, p=0.016) than DDD recipients. Adjusting for age, frailty and dementia, VVI pacing was associated with an increased risk of all-cause mortality (adjusted hazard ratio [HR] 2.1, 95% confidence interval [CI] 1.08 to 4.1, p=0.03) and death from CCF (adjusted HR 7.1, 95%CI 2.5 to 20.6, p<0.001).
In conclusion, in nonagenarians with emergent CHB, dual-chamber pacing was associated with improved symptomatic and prognostic outcomes versus single-chamber pacing.
June 2024 Br J Cardiol 2024;31:68–72 doi:10.5837/bjc.2024.025
Navigating the research landscape in cardiology. Part 3: the application process
Benjamin Dowsing, C Fielder Camm, Hibba Kurdi

This editorial series explores research in UK cardiology and acts as a practical guide to trainees interested in pursuing early career research. Two earlier entries in the series have explored the rationale for pursuing research and how to identify a project and supervisor. We now take a closer look at navigating the application processes, including funding opportunities and regulatory approvals, to get your research off the ground.
June 2024 Br J Cardiol 2024;31:79 doi:10.5837/bjc.2024.026
Cardiovascular disease development in COVID-19 patients admitted to a tertiary medical centre in Iran
Erfan Kazemi, Salman Daliri, Reza Chaman, Marzieh Rohani-Rasaf, Ehsan Binesh, Hossein Sheibani

Cardiovascular diseases (CVDs) have been reported to occur in a significant number of patients diagnosed with coronavirus disease 2019 (COVID-19). We report our experience regarding the occurrence of symptomatic and asymptomatic CVDs in COVID-19 patients. In this cross-sectional study, 690 COVID-19 patients were included. Cardiovascular consultation had been requested for all of the patients based on their primary clinical examination, vital signs, and electrocardiogram (ECG). Additionally, 2D transthoracic echocardiography (TTE), and myocardial injury serum biomarkers assays (creatine phosphokinase-MB [CPK-MB] and cardiac troponins [cTn]) were measured once. Manifestations of CVDs, such as chest pain, abnormal serum markers, unstable angina, myocardial infarction (MI), myocarditis, and new-onset hypertension, were documented. The most common symptom was left hemithorax and interscapular pain (317 patients, 46%). New-onset high systolic and diastolic blood pressures were seen in 67 patients (10%). Unstable angina, MI, and myocarditis were, respectively, diagnosed in 20 (2.8%), five (0.7%), and 12 (1.7%) patients. On TTE, pericardial effusion was diagnosed in 139 patients (31.1%). The most common abnormal ECG changes seen were regarding the T-wave, including flat T-wave (148 cases, 21.4%) and inverted T-wave (141 cases, 20.4%). Serum cTn levels were positive or weekly positive in 17 cases (7.4%). The incidence rate of cardiovascular involvements was high in COVID-19 patients.
May 2024 Br J Cardiol 2024;31:49–54 doi:10.5837/bjc.2024.018
Factor XI and XIa inhibition: a new approach to anticoagulant therapy
Mark Anthony Sammut, Nadir Elamin, Robert F Storey

Factor (F) XI or XIa inhibition has attracted interest due to the protection from thrombotic events and minimal bleeding tendency observed in FXI-deficient individuals. The prospect of uncoupling the management of thrombosis from the bleeding risk inadvertently associated with current therapy inspired the development of agents directed towards this step in the coagulation process. This review describes the physiological rationale behind FXI/FXIa inhibition and the pharmacological properties of existing FXI/FXIa inhibitors. It also explores the potential clinical use of these agents in various thromboembolic pathologies, predominantly through the phase II clinical trials conducted so far comparing them to current anticoagulant therapy or placebo.
May 2024 Br J Cardiol 2024;31:65–7 doi:10.5837/bjc.2024.020
A retrospective observational study of certain interactions with simvastatin 40 mg in an acute hospital in England
Danita Boamah, Liam Bastian, Michael Wilcock

The use of simvastatin 40 mg with various interacting medicines may lead to an increased risk of myopathy. We examined the extent to which hospital inpatients were prescribed simvastatin 40 mg with amiodarone, amlodipine, diltiazem, or verapamil, and assessed if any action was taken by prescribers or the pharmacy team to avoid this interaction. We found 56 patients on a combination of interest during their stay. Of the 20 (36%) patients not discharged on the combination, in six instances this was due to pharmacy intervention, while the remaining instances when simvastatin 40 mg or the interacting drug was amended or ceased were due to other clinical reasons. There is a need among clinicians and pharmacy teams within the hospital for recognition and management of these particular interactions.
April 2024 Br J Cardiol 2024;31:76 doi:10.5837/bjc.2024.014
Cardioversion versus ablation versus ‘pace and ablate’ for persistent atrial fibrillation in older patients
William Eysenck, Neil Sulke, Nick Freemantle, Neil Bodagh, Nikhil Patel, Stephen Furniss, Rick Veasey

Our objective was to compare the efficacy of atrial fibrillation (AF) ablation versus permanent pacemaker (PPM) with atrioventricular node ablation (AVNA) versus direct current cardioversion (DCCV) for persistent AF in patients ≥65 years old.
Seventy-seven patients (aged 66–86, mean 75.4 years) with persistent AF were randomised (1:1:1) to AF ablation + amiodarone (± DCCV), PPM with AVNA (+DCCV) or DCCV + amiodarone. The primary end point was persistent AF recurrence, measured with an implanted cardiac monitor or PPM. Cardiopulmonary exercise testing (CPET) was performed at baseline and six months. Symptom questionnaires were completed monthly. Follow-up was 12 months.
The primary end point occurred in fewer patients following AF ablation + amiodarone than DCCV + amiodarone (seven patients, 28% vs. 15 patients, 60%; hazard ratio [HR] 0.559, 95% confidence interval [CI] 0.293 to 1.065, p=0.073) with no differences between DCCV + amiodarone and PPM with AVNA (HR 0.990, 95%CI 0.539 to 1.818, p=0.973). AF ablation + amiodarone resulted in a lower AF burden at 12 months compared with DCCV + amiodarone (17.0 ± 37.9% vs. 61.7 ± 48.6%, p<0.0001). Modified European Heart Rhythm Association (EHRA) symptom class improved in all patients (baseline 2.4 ± 0.495 vs. 12-month follow-up 1.84 ± 0.081, p=0.00001). Six-month CPET demonstrated a higher VO2 peak in sinus rhythm (SR) compared with baseline in AF (12.1 ± 4.2 ml/kg/min at baseline to 15.3 ± 4.2 ml/kg/min at six months, p=0.013).
In conclusion, in older patients with persistent AF, ablation + amiodarone resulted in a lower AF burden at 12 months than DCCV + amiodarone. There was a non-significant trend toward reduced recurrence of device-detected persistent AF episodes. All therapies improved symptoms despite DCCV restoring SR in <50% of patients at 12 months. CPET demonstrated improved VO2 peak with SR restoration.
April 2024 Br J Cardiol 2024;31:55–7 doi:10.5837/bjc.2024.015
Heartificial intelligence: in what ways will artificial intelligence lead to changes in cardiology over the next 10 years
Sam Brown

Artificial intelligence (AI) will revolutionise cardiology practices over the next decade, from optimising diagnostics to individualising treatment strategies. Moreover, it can play an important role in combating gender inequalities in cardiovascular disease outcomes. There is growing evidence that AI algorithms can match humans at echocardiography analysis, while also being able to extract subtle differences that the human eye cannot detect. Similar promise is evident in the analysis of electrocardiograms, creating a new layer of interpretation. From big data, AI can produce algorithms that individualise cardiac risk factors and prevent perpetuating gender biases in diagnosis. Nonetheless, AI implementation requires caution. To avoid worsening health inequalities, it must be trained across diverse populations, and when errors arise, a robust regulatory framework must be in place to ensure safety and accountability. AI is perfectly positioned to capitalise on the growth of big data, but to proceed we require a generation of physicians who understand its fundamentals.
April 2024 Br J Cardiol 2024;31:77 doi:10.5837/bjc.2024.016
Outcomes of PCI of all comers: the experience of a Kuwaiti independent healthcare institution
Telal Mudawi, Waleed Alenezi, Ahmed Amin, Dalia Besada, Asmaa Aly, Assem Fathi, Darar Al-Khdair, Muath Al-Anbaei

We present the cumulative percutaneous coronary intervention (PCI) data of all comers (stable angina and acute coronary syndromes [ACS]) who presented to Hadi Clinic between January 2018 and December 2020. As a low-volume PCI centre in the Middle East, we wanted to find out if the outcomes of our PCI procedures are different from those of high-volume PCI centres in the UK and the Western world.
Prospectively collected data of all comers for PCI (urgent and elective) were retrospectively analysed. Pre-procedural data included patients’ baseline characteristics (age, gender, clinical presentation and comorbidities). Intra-procedural data included access route, coronary anatomy, lesion complexity, number of stents deployed, door-to-balloon time for primary PCI, and any intra-procedural complications. Post-procedural data included average length of in-hospital stay, intra-hospital morbidity and mortality, and mortality or admission with ACS 12–36 months after the index procedure.
A total of 567 patients underwent coronary catheterisation for the three-year period between January 2018 and December 2020. Mean age was 60.9 ± 9.4 years, and 459/567 (81.0%) were male. Comorbidities included dyslipidaemia 515/567 (90.9%), hypertension 460/567 (81.2%), diabetes 346/567 (61%), known prior coronary disease 250/567 (44.2%), and smoking 188/567 (33.1%). Clinical presentation was stable angina 130/567 (22.9%), non-ST-elevation acute coronary syndrome (NSTEACS) 312/567 (55%), ST-elevation myocardial infarction (STEMI) 125/567 (22.0%), and STEMI with cardiogenic shock 13/125 (10.4%). The radial approach was used in 544/567 (95.94%), the average SYNTAX score was 34.8 ± 9.6, and the average number of stents 2.6. The total number of PCI was 367 (122.3 annually) with PCI procedural complete success in 349/367 (95.1%), partial success 5/367 (1.36%), PCI procedural complications 3/367 (0.82%), PCI in-hospital mortality 1/367 (0.27%), door-to-balloon time for primary PCI 31.8 ± 12.2 minutes, subsequent admission with ACS after 12–36 months 2/367 (0.54%), and post-discharge mortality after 12–36 months 1/367 (0.27%).
In conclusion, our patient population have more comorbidities and more complex coronary disease in comparison to their western counterparts. Our annual PCI numbers have been significantly lower than the recommended 400 minimum cut-off figure, yet we have achieved comparable outcomes to those of larger institutions of the western world.
April 2024 Br J Cardiol 2024;31:78 doi:10.5837/bjc.2024.017
Safety outcomes of suspected cardiac pathology assessed in an ambulatory rapid-access cardiology clinic
Pok-Tin Tang, Benjamin Bussmann, Asad Shabbir, Andrew Elkington, William Orr

Cardiac pathology contributes to a significant proportion of emergency department (ED) attendances. Many could be managed as urgent outpatients and avoid hospital admission. We evaluated a novel rapid-access general cardiology clinic to achieve this, implemented during the COVID-19 pandemic.
We performed a retrospective review of baseline characteristics, investigations, final diagnoses, and 90-day safety (readmission, major adverse cardiovascular events [MACE], mortality) from electronic records and conducted a patient experience survey.
There were 216 ED referrals made between 1 June and 30 October 2020. The median time to review was two days (interquartile range 1–5). At 90 days, there were three (1.4%) re-presentations requiring admission, two (0.9%) MACE, and no deaths. There were 205 (95%) successfully managed without hospital admission. Among surveyed patients, 96% felt they had concerns adequately addressed in a timely manner.
In conclusion, our rapid-access cardiology clinic is a safe model for outpatient management of a range of cardiovascular presentations to the ED.
March 2024 Br J Cardiol 2024;31:36 doi:10.5837/bjc.2024.009
The prevalence of coronary artery disease in patients presenting with ‘non-anginal chest pain’
William Chick, Anita Macnab

The National Institute for Health and Care Excellence (NICE) advise against routine testing for coronary artery disease (CAD) in patients with non-anginal chest pain (NACP). This clinical audit sought to establish the prevalence of significant CAD in this cohort using computed tomography angiography (CTCA) and evaluate differences in the prevalence of cardiovascular risk factors between those with and without obstructive coronary disease.
Over 23 months, 866 patients with NACP underwent CTCA. Patients were separated into three groups for analysis depending on the degree of CAD on CTCA using the CAD-RADS (Coronary Artery Disease Reporting and Data System) scoring system; no evidence of CAD (group 1), a degree of CAD requiring medical therapy only (group 2), significant CAD defined as a CAD-RADS score 4A/B or 5 (group 3). Cardiovascular risk factors were compared between the groups.
We found 11.5% had significant CAD (group 3), 58.3% required medical therapy (group 2) and 30.1% had no CAD (group 1). There were 32 patients who required coronary revascularisation. Patients in group 2 and 3 were more likely to be male (p<0.001) and older (p<0.001) when compared to patients in group 1. Patients in group 3 were more likely to be hypertensive (p=0.008) and have higher Qrisk2 scores (p<0.001) when compared with those in group 1.
In conclusion, NICE guidelines for NACP may result in a significant proportion of patients with CAD being underdiagnosed, including some with severe disease requiring revascularisation. This analysis suggests age, male gender, Qrisk2 score and hypertension are predictors of CAD in this cohort.
March 2024 Br J Cardiol 2024;31:27 doi:10.5837/bjc.2024.010
Comparison between early and late dapagliflozin administration for decompensated heart failure
Takahiro Tokuda, Yoriyasu Suzuki, Ai Kagase, Hiroaki Matsuda, Akira Murata, Tatsuya Ito

Sodium-glucose cotransporter 2 inhibitors have demonstrated positive effects in heart failure (HF) patients. However, the effects of dapagliflozin in patients with decompensated HF remain unclear. This study aimed to compare the efficacy and safety of early and late dapagliflozin administration for decompensated HF. Data regarding dapagliflozin administration from 70 patients diagnosed with HF between December 2020 and November 2021 at a Japanese heart centre were analysed retrospectively. Propensity score matching was performed to compare the clinical outcomes of early and late dapagliflozin administration for decompensated HF. The primary end point was HF admission one year after dapagliflozin administration. The secondary end points were evaluated based on 24-hour urine volume, cardiac death, changes in ejection fraction (EF), blood pressure, glomerular filtration rate (GFR), haemoglobin and N-terminal pro-B-type natriuretic peptide (NT-proBNP) levels, and side effects within one year of treatment. Fifteen matched pairs of patients were analysed. Admission rate within one year was significantly lower in the early administration group than in the late administration group (0 vs. 20%, p=0.03). Secondary end points were not significantly different between the two groups. In conclusion, early dapagliflozin administration significantly reduced HF admission within one year of treatment, although no differences were observed in 24-hour urine volume, cardiac death, EF, GFR, haemoglobin and NT-proBNP levels, and side effects.
March 2024 Br J Cardiol 2024;31:32–5 doi:10.5837/bjc.2024.011
Navigating the research landscape in cardiology. Part 2: finding the right research
Hibba Kurdi, Jessica Artico, Freya Lodge, C Fielder Camm

This editorial series provides an in-depth exploration of research avenues in UK cardiology. It underscores the pivotal role of research in cardiology training and addresses the challenges faced by trainees in identifying apt research opportunities. This second article categorises available research roles, weighing their pros and cons, and outlines various supervisory styles to guide trainees in finding the optimal fit. It also summarises the primary research degrees, namely MPhil, MSc, MD, and PhD, tailored to diverse research goals.
March 2024 Br J Cardiol 2024;31:31 doi:10.5837/bjc.2024.012
Mitral valvular surgery outcomes in a centre with a dedicated mitral multi-disciplinary team
Ishtiaq Rahman, Cristina Ruiz Segria, Jason Trevis, Sharareh Vahabi, Richard Graham, Jeet Thambyrajah, Ralph White, Andrew Goodwin, Simon Kendall, Enoch Akowuah

International guidelines recommend ‘heart teams’ as the preferred method for decision-making. Heart team processes, mandatory attendees and investigations vary significantly between hospitals. We assessed outcomes following mitral valvular surgery in a tertiary referral centre with a dedicated mitral multi-disciplinary team (MDT).
This was a single-centre retrospective review of prospectively collected data within the ‘mitral database’ of mitral valvular disease patients. The ‘mitral MDT’ meeting involved pre-operative imaging and clinical data review, including mandatory transoesophageal echocardiography; recommendation for planned procedure, as well as an appropriate surgeon; and review of echocardiography images and clinical outcomes after surgery had been performed.
Between 2016 and 2020, 395 patients with mitral valvular disease were discussed at MDT. Of these, 310 patients underwent surgery. During the same time interval, 75 patients had surgery without MDT discussion: 84% of patients not discussed were urgent or emergent procedures and, in these, the most common pathology was degenerative mitral regurgitation (DMR, 46%) followed by infective endocarditis (30%). Of those discussed at MDT the pathology was: DMR 65%; mitral stenosis 14%; functional mitral regurgitation (MR) 5%; rheumatic MR 4%; endocarditis 4%; ischaemic MR 4%; and other pathologies 4%. For patients with DMR having elective surgery, the repair rate was 93% with mortality 2% and median (IQR) length of stay 5 (4–6) days. Postoperative transthoracic echocardiography demonstrated 99% of elective DMR patients had ≤2+ MR and <1% severe (3+) MR.
In conclusion, a dedicated ‘mitral MDT’ can enhance the safe delivery of care with consistently high repair rates for DMR patients with excellent outcomes.
February 2024 Br J Cardiol 2024;31:13–6 doi:10.5837/bjc.2024.006
A retrospective single-centre study on determinants of high-risk coronary artery calcium (CAC) score in women
Saskia D Handari, Naesilla, Annisya Dinda Paramitha

One of the assessments for coronary atherosclerosis during cardiac computed tomography (CT) is coronary artery calcium (CAC) scoring. We conducted analysis on the determinants of high-risk coronary calcification, represented by CAC score, among women as a step to improve their outcomes and prognosis. This study involved a total of 1,129 female patients from a single centre. There were 127 patients (11.2%) classified as high risk (CAC ≥400). We found that a history of hypertension and diabetes are independent determinants of having a high-risk CAC score. Furthermore, this study demonstrated protective effects associated with physical activity and diastolic blood pressure. In conclusion, a history of hypertension, diabetes, and high uncontrolled systolic blood pressure might be used as cues for physicians to prioritise CAC assessment in women, despite the absence of chest pain or atypical symptoms.
February 2024 Br J Cardiol 2024;31:28–30 doi:10.5837/bjc.2024.007
Transcatheter versus surgical valve replacement in patients with bicuspid aortic valves: an updated meta-analysis
Peter S Giannaris, Viren S Sehgal, Branden Tejada, Kenzy H Ismail, Roshan Pandey, Eamon Vega, Kathryn Varghese, Ahmed K Awad, Adham Ahmed, Irbaz Hameed

Patients with bicuspid aortic valves (BAV) are predisposed to the development of aortic stenosis. We performed a pairwise meta-analysis, comparing the efficacy of transcatheter aortic valve replacement (TAVR) versus surgical aortic valve replacement (SAVR) in patients with BAV.
Medical databases were queried to pool comparative studies of interest. Single-arm studies, conference presentations, animal studies, and studies that involved patients with tricuspid aortic morphology were excluded. Outcomes were pooled as risk ratios (RRs) with their 95% confidence intervals (CI) using the random effects model in R.
There were 60,858 patients with BAV (7,565 TAVR, 53,293 SAVR) included. Compared with SAVR, TAVR was associated with a significantly lower risk of 30-day major bleeding (RR 0.29, 95%CI 0.13 to 0.63, p=0.01) but a higher risk of new permanent pacemaker placement (RR 2.17, 95%CI 1.03 to 4.58, p=0.04). No significant differences were seen with other explored outcomes, including 30-day/mid-term mortality, stroke, acute kidney injury, major vascular complications, paravalvular leak, and conduction abnormalities.
In conclusion, in patients with BAV, TAVR is associated with a lower risk of 30-day major bleeding but has an increased risk for permanent pacemaker implantation when compared with SAVR. Future large-scale randomised trials comparing both the short- and long-term outcomes of SAVR and TAVR in patients with BAV are needed to assess the efficacy of each modality in a controlled population across long follow-up durations.
February 2024 Br J Cardiol 2024;31:40 doi:10.5837/bjc.2024.008
Solving problems at the cath lab
Rita Caldeira da Rocha, Alejandro Diego Nieto, Jesus Garibi, Ignacio Cruz-Gonzalez

We describe a case of aortic rupture following transcatheter aortic valve implantation that was managed percutaneously.
January 2024 Br J Cardiol 2024;31:4–6 doi:10.5837/bjc.2024.001
Dishing out the meds
David Mulcahy, Palwasha Khan

Twenty years ago, Wald and Law1 hypothesised that, if a combination pill could be made including aspirin, folic acid, a statin, and a low-dose diuretic, beta blocker and angiotensin-converting enzyme (ACE) inhibitor (thus, allowing for the simultaneous modification of four different risk factors: low-density lipoprotein [LDL]-cholesterol, blood pressure, homocysteine, and platelet function), and administered to everyone with existing cardiovascular disease and everyone over 55 years old, there would be an 88% reduction in ischaemic heart disease events, and an 80% reduction in stroke. One third of people over the age of 55 years would benefit by gaining an average of 11 years free from a cardiac event or stroke (subsequently termed the vaccination approach). They called this pill the ‘Polypill’, and concluded that treatment would be acceptably safe and, with widespread use, would have a greater impact on the prevention of disease in the Western world than any other single intervention. They noted that, while such a preventative strategy was radical, if such a formulation existed that prevented cancer and was safe, it would be widely used. “It is time to discard the view that risk factors need to be measured and treated individually if found to be abnormal. There is much to gain and little to lose by the widespread use of these drugs.” While subsequent works have shown that folic acid is not prognostically beneficial in preventing cardiovascular disease,2 and that aspirin may not be beneficial overall in primary prevention settings,3 the concept of the combination pill was awakened in the public eye.
January 2024 Br J Cardiol 2024;31:17–22 doi:10.5837/bjc.2024.002
Assessment of the diagnostic value of NT-proBNP in heart failure with preserved ejection fraction
Hayley Birrell, Omar Fersia, Mohamed Anwar, Catherine Mondoa, Angus McFadyen, Christopher Isles

Heart failure with preserved ejection fraction (HFpEF) is a common concern in the medical field due to its prevalence in an ageing western population. HFpEF is associated with significant morbidity and mortality not dissimilar to heart failure (HF) with reduced ejection fraction. N-terminal pro-B-type natriuretic peptide (NT-proBNP) levels and echocardiography are the guideline diagnostic indicators of HF and their use is being examined in this study, with the aim to consider NT-proBNP thresholds performance as a rule-out test.
The current National Institute for Health and Care Excellence (NICE) and European guidelines recommend a single NT-proBNP threshold of >400 ng/L and >125 ng/L, respectively, to trigger echocardiographic assessment of HF in the outpatient setting. NT-proBNP levels are known to increase with age and worsening renal function. Unsurprisingly, a single threshold significantly increases demand for echocardiography. NT-proBNP measurements and echocardiograms performed within six months of each other were included for 469 patients with suspected HF.
A significant relationship between NT-proBNP levels and diastolic dysfunction was established. NT-proBNP levels and age are significant predictors of diastolic dysfunction in uni-variant (odds ratio 1.251, 95% confidence interval [CI], p<0.001) and multi-variant analysis (odds ratio 1.174, 95%CI, p=0.002). High negative-predictive values (NPVs) were obtained in severe diastolic impairment with the NPV being 95% at the European NT-proBNP cut-off of 125 ng/L, 95% at the NICE cut-off of 400 ng/L, 93% at 1,000 ng/L and 92% at 2,000 ng/L.
There is a significant association between NT-proBNP and diastolic dysfunction. NT-proBNP and age can predict diastolic dysfunction, and age can predict NT-proBNP levels, thus, these variables should be considered when considering referral for an echocardiogram. Most importantly, at higher NT-proBNP cut-offs the NPVs remain above 90% suggesting that different thresholds for subpopulations could yield a more effective strategy and mitigate the increased demand for echocardiography.
January 2024 Br J Cardiol 2024;31:23–6 doi:10.5837/bjc.2024.003
Inpatient initiation of sodium-glucose cotransporter-2 inhibitors: the prescribing learning curve
Charlotte Gross, Hiba Hammad, Thomas A Slater, Sam Straw, Thomas Anderton, Caroline Coyle, Melanie McGinlay, John Gierula, V Kate Gatenby, Vikrant Nayar, Jiv N Gosai, Klaus K Witte

We aimed to describe the safety and tolerability of initiation of sodium-glucose cotransporter 2 inhibitors (SGLT2i) during hospitalisation with heart failure, and the frequency of, and reasons for, subsequent discontinuation.
In total, 934 patients who were not already prescribed a SGLT2i were hospitalised with heart failure, 77 (8%) were initiated on a SGLT2i a median of five (3–8.5) days after admission and two (0.5–5) days prior to discharge. During a median follow-up of 182 (124–250) days, SGLT2i were discontinued for 10 (13%) patients, most frequently due to deteriorating renal function. We observed reductions in body weight (mean difference 2.0 ± 0.48 kg, p<0.001), systolic blood pressure (mean difference 9.5 ± 1.9 kg, p<0.001) and small, non-significant reductions in estimated glomerular filtration rate (eGFR mean difference 2.0 ± 1.5 ml/min/1.73 m2, p=0.19) prior to initiation, with further modest reductions in weight (mean difference 1.2 ± 0.4 kg, p=0.006) but not systolic blood pressure (2.4 ± 1.5 mmHg, p=0.13) or eGFR following initiation of SGLT2i. At discharge the proportion prescribed a beta blocker (44% to 92%), angiotensin-receptor/neprilysin inhibitor (6% to 44%) and mineralocorticoid-receptor antagonist (35% to 85%) had increased.
In conclusion, inpatient initiation of SGLT2i was safe and well tolerated in a real-world cohort of patients hospitalised with worsening HF. We observed a 13% frequency of discontinuation or serious side effects.
January 2024 Br J Cardiol 2024;31:37–9 doi:10.5837/bjc.2024.004
Pulmonary hypertension secondary to arteriovenous fistula: a case report
Karla Alejandra Pupiales-Dávila, David Jacobo Sánchez-Amaya, Rodrigo Zebadúa-Torres, Julio César López-Reyes, Nayeli Guadalupe Zayas-Hernández

Pulmonary hypertension is a rare disease, associated with a significant deterioration in quality of life, usually not curable and with an ominous prognosis. It is classified into five groups according to similar pathophysiological, clinical, haemodynamic, and treatment options in each of them. However, group 5 is the least common, encompassing different types of aetiological, semiological, and management conditions. We present the case of a patient diagnosed with precapillary component pulmonary hypertension, with the finding of an arteriovenous fistula at the peripheral level. Interventional exclusion was performed, achieving remission of her disease.
November 2023 Br J Cardiol 2023;30:139–43 doi:10.5837/bjc.2023.040
Drug therapies for stroke prevention
Nimisha Shaji, Robert F Storey, William A E Parker

Stroke is a major cause of mortality, morbidity and economic burden. Strokes can be thrombotic, embolic or haemorrhagic. The key risk factor for cardioembolic stroke is atrial fibrillation or flutter, and oral anticoagulation (OAC) is recommended in all but the lowest-risk patients with evidence of these arrhythmias. Risk factors for thrombotic stroke overlap strongly with those for other atherosclerotic cardiovascular diseases (ASCVDs). Antiplatelet therapy (APT) should be considered in patients with established ASCVD to reduce risk of cardiovascular events, including stroke. Intensification from single to dual APT or a combination of APT with low-dose OAC can reduce ischaemic stroke risk further, but increases bleeding risk. Blood pressure and lipid profile should be controlled appropriately to guideline targets. In patients with diabetes, good glycaemic control can reduce stroke risk. Inflammation is another emerging target for stroke prevention. Overall, comprehensive assessment and pharmacological modification of risk factors are central to stroke prevention.
November 2023 Br J Cardiol 2023;30:150 doi:10.5837/bjc.2023.041
CMR is vital in the management of cardiology inpatients: a tertiary centre experience
Rumneek Hampal, Kristopher D Knott, Aristides Plastiras, Nicholas H Bunce

To review the utility of cardiovascular magnetic resonance (CMR) in the management of hospital inpatients, we performed a retrospective review of all inpatient CMR scans performed over a six-month period at a tertiary referral cardiology centre. Patient demographics, indication for CMR imaging, results of the CMR scans and whether the results changed patient management were recorded. Change in management included medication changes, subsequent invasive procedures, or avoidance of such, and hospital discharge.
Overall, 169 patients were included in the study cohort, 66% were male, mean age was 57.1 years. The most common indication for inpatient CMR was to investigate for cardiomyopathy (53% of patients). The most prevalent diagnosis post-CMR in our cohort was ischaemic heart disease, including ischaemic cardiomyopathy and coronary artery disease. There was a complete change in diagnosis or additional diagnosis found in 29% of patients following CMR. Overall, inpatient CMR led to a change in management in 77% of patients; the most common being changes to medication regimen. CMR was well tolerated in 99% of patients and image quality was diagnostic in 93% of cine scans performed.
In conclusion, CMR is vital for the management of cardiology inpatients, having an impact that is at least as significant as in the management of outpatients.
November 2023 Br J Cardiol 2023;30:144–7 doi:10.5837/bjc.2023.042
Myocardial revascularisation in complex patients: does it happen as prescribed by the heart team?
Montasir Ali, Abdul R A Bakhsh, Omer Elsayegh, Hussain Al-Sadi, Adrian Ionescu

Guidelines recommend decision-making using the heart team (HT) in complex patients considered for myocardial revascularisation, but there are little data on how this approach works in practice. We data-mined our electronic HT database and selected patients in whom the clinical question referred to revascularisation, and documented HT recommendations and their implementation.
We identified 154 patients (117 male), mean age 68.9 ± 11.4 years, discussed between February 2019 and December 2020. The clinical questions were coronary artery bypass graft (CABG) versus percutaneous coronary intervention (PCI) (141 cases, 91%), and medical treatment versus revascularisation by PCI (eight cases, 6%) or by CABG (five cases, 3%).
HT recommended CABG in 55 cases (35%), PCI in 43 (28%), medical treatment in 15 (10%), and equipoise in seven (5%) and further investigations in 34 (22%): non-invasive imaging for ischaemia in 11 (32%), invasive coronary physiology studies in eight (24%), further clinical assessment in seven (20%), structural imaging for five (15%), invasive coronary angiography in two (6%), and an electrophysiology opinion in one case (3%).
Decisions were implemented in 135 cases (89%). The average time between the HT and the implementation of its decision was 80.5 ± 129.3 days. There were 17 deaths: 10 cardiac, six non-cardiac and one of unknown cause. Patients who survived were younger (68.6 ± 11.3 years) than those who died (73.8 ± 10.0 years, p = 0.03).
In conclusion, almost 90% of the decisions of the HT on myocardial revascularisation are implemented, while ischaemia testing is the main investigation required for decision-making. Recent data on the futility of such an approach have not yet permeated clinical practice.
November 2023 Br J Cardiol 2023;30:148 doi:10.5837/bjc.2023.043
Improvement in LV end-diastolic pressure after primary PCI and its impact on patients’ recovery
Usman Hanif Bhatti, Khalid Naseeb, Muhammad Nauman Khan, Vashu Mal, Muhammad Asad Baqai, Musa Karim, Muhammad Ashar Khan, Tahir Saghir

In this study, we evaluated the change in left ventricular end-diastolic pressure (LVEDP) after primary percutaneous coronary intervention (PCI) and its impact on in-hospital outcomes and 30-day and three-month quality of life (SAQ-7), ejection fraction (EF), and major adverse cardiovascular events (MACE). LVEDP ≥19 mmHg was taken as elevated LVEDP. In a sample of 318 patients, 18.9% (n=60) were females and mean age was 55.7 ± 10.52 years. Post-procedure elevated LVEDP was observed in 20.8% (n=66) with a mean reduction of 1.65 ± 4.35 mmHg. LVEDP declined in 39% (n=124) and increased in 10.7% (n=34). In-hospital mortality rate (9.1% vs. 2.4%, p=0.011), 30-day MACE (9.1% vs. 4.0%), and three-month MACE (21.2% vs. 5.6%) were found to be significantly higher among patients with elevated LVEDP, respectively. Elevated LVEDP was found to be associated with a reduced SAQ-7 score (89.84 ± 8.09 vs. 92.29 ± 3.03, p<0.001) and reduced (25–40%) EF (55.6% vs. 22.6%) at three-month follow-up. LVEDP declined acutely in a significant number of patients after primary PCI. Post-procedure elevated LVEDP was found to be associated with poor quality of life and an increased risk of immediate and short-term MACE.
November 2023 Br J Cardiol 2023;30:153–6 doi:10.5837/bjc.2023.044
Efficacy and tolerability of PCSK9 inhibitors in real-world clinical practice
Prashasthi Devaiah, Sava Handjiev, Jacob George

Despite widespread use of statins and other lipid-lowering therapies for hypercholesterolaemia, cardiovascular (CV) mortality and morbidity remains high. The proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors, alirocumab and evolocumab, have been approved for use in patients with familial hypercholesterolaemia and high CV risk in the UK. We reviewed the records of patients at a large health board in Scotland, who were prescribed these agents, to determine their real-world efficacy and tolerability in routine clinical care.
November 2023 Br J Cardiol 2023;30:158–60 doi:10.5837/bjc.2023.045
Brachial artery approach for managing retroperitoneal bleed following coronary intervention for STEMI
Muhammad Usman Shah, Krishna Poudyal, Ramy Goubran, Adnan Ahmed, Syed Yaseen Naqvi

Primary percutaneous coronary intervention (PPCI) remains the gold-standard treatment for ST-elevation myocardial infarction (STEMI). Femoral arterial access for the procedure may be an ideal option in patients who are haemodynamically unwell. However, it is associated with rare, but life-threatening, complications such as perforation, leading to retroperitoneal haemorrhage. We present the case of a man in his 50s, admitted with cardiac arrest secondary to inferolateral STEMI. Successful PPCI was performed via right femoral artery, with access gained under ultrasound guidance. However, the patient deteriorated and was diagnosed to have a retroperitoneal haematoma secondary to femoral artery perforation. Additional arterial access via left brachial artery was obtained, and a covered stent was deployed successfully in the right femoral artery with satisfactory haemostasis. The patient recovered successfully and was discharged two weeks later. Early recognition of such complications is imperative to adequate management and percutaneous treatment is a viable option for such situations, in comparison with open surgical repair.
November 2023 Br J Cardiol 2023;30:128–31 doi:10.5837/bjc.2023.035
Personal recording devices for arrhythmia detection
Gabriele Volucke, Guy A Haywood

Persistent cardiac arrhythmias are readily amenable to detection by performing a standard electrocardiogram (ECG), but detection of transient (paroxysmal) arrhythmias has long been a significant cause of frustration to both doctors and patients. Often a significantly symptomatic arrhythmia is experienced by the patient but terminates before an ECG can be recorded to allow diagnosis. Prognostically important treatment is often delayed, and recurrent symptomatic attacks represent a high morbidity in patients’ lives and result in a burden on emergency services, who often arrive after the arrhythmia has terminated with no resultant progress in making a diagnosis.
Another area of concern has been the presence of asymptomatic, but clinically important, arrhythmias that can go unnoticed by people experiencing them and may result in permanent harm; asymptomatic paroxysmal atrial fibrillation in patients with high CHA2DS2-VASc scores being the most common example.
Both these issues are now being importantly addressed by the widespread availability of portable ECG recording devices, which patients can either manually activate themselves or program to automatically detect abnormal arrhythmias. Information on the range of devices available and their strengths and weaknesses is limited. This article aims to provide a helpful overview for patients and doctors advising them.
November 2023 Br J Cardiol 2023;30:149 doi:10.5837/bjc.2023.037
Stent, balloon and hybrid in de novo PCI: could the whole be greater than the sum of its parts?
Pitt O Lim

Andreas Grüntzig, an ardent angiologist crafted an indeflatable sausage-shaped dual-lumen balloon-catheter, designed its delivery to the heart, launched minimally invasive coronary intervention and taught by beaming live demonstration. Subsequent advances are just incremental tweaks and tinkers around this fully formed framework from 1978. The near-immediate or instant feedback learning process by which the heart responds to any new invasive procedural variation facilitates each new change; be it drug-eluting stent, drug-coated balloon, or both in different combinations and permutations. Now with Grüntzig’s balloon armed with an antiproliferative drug, it could dominate the field once more, as he originally envisaged.
October 2023 Br J Cardiol 2023;30:152 doi:10.5837/bjc.2023.030
Type of thrombus, no reflow and outcomes of coronary intervention in ACS patients: OCT-guided study
Mostafa Abdelmonaem, Mohamed Farouk, Ahmed Reda

Thrombus is the main finding in most patients with acute coronary syndrome (ACS), the type of which potentially impacts the end result of the interventional procedure in terms of no reflow and edge dissection. Optical coherence tomography (OCT) is considered a precise intra-vascular tool to image thrombi and characterise its properties. We aimed to study the impact of thrombus type, as defined by OCT, on procedural outcome in ACS patients. In this retrospective study we enrolled 100 patients who were treated by percutaneous coronary intervention (PCI) with the guidance of OCT. We recorded demographic and clinical data of the whole studied cohort. Angiographic details and procedural data were noted. Baseline OCT study was performed before intervention and repeated post-intervention. Plaque characterisation was identified, and thrombi were defined as red or white thrombi. Acute angiographic outcome was defined with special emphasis on no reflow.
Male patients and ST-elevation myocardial infarction (STEMI) patients more often had white thrombi (58.1% and 71.2%, respectively). Cases with red thrombi had longer pain duration, which was statistically significant. Edge dissection was more frequent with red thrombus, 44.7% versus 32.1% with white thrombus, but the difference is not statistically significant, while 17% of patients with white thrombi were complicated by no-reflow phenomenon versus only 4.3% in patients with red thrombi, and this difference was statistically significant.
In conculsion, OCT-guided PCI is feasible and safe in ACS settings. OCT-guided intra-procedural differentiation of thrombus type is potentially beneficial in predicting acute procedural outcome.
October 2023 Br J Cardiol 2023;30:151 doi:10.5837/bjc.2023.031
A survey of digital access, digital confidence and rehabilitation delivery preferences of patients referred for CR
Helen Alexander, Andrew D’Silva, Christopher Tack, Aynsley Cowie

Remote delivery of cardiovascular rehabilitation (CR) has been vital during the COVID pandemic when restrictions have been placed on face-to-face services. In the future, CR services are likely to offer alternatives to centre-based CR, including digital options. However, little is known about the digital access and confidence of CR service users, or their CR delivery preferences.
A telephone survey was conducted of those referred for CR in the London boroughs of Lambeth and Southwark (n=60) in which questions were asked about digital access and confidence, as well as current and future delivery preferences for their CR.
Between March and July 2021, 60 service-users met the inclusion criteria and were recruited for a telephone survey (mean age 60 ± 11.2 years). Of those, 82% had regular access to a smartphone, 60% to a computer or laptop and 43% to a tablet device. A high proportion of service users perceived themselves to be ‘extremely’ or ‘somewhat’ confident to use their devices. Thirty-nine (65%) service users would currently prefer a face-to-face assessment, rising to 82% once the perceived COVID-19 threat and restrictions are less. Preferences for accessing exercise were equally split between face-to-face and remotely supported independent exercise, with low interest in digital options. Delivery preferences for education, relaxation and peer support were more heterogeneous with interest in all delivery options.
In conclusion, digital access and confidence in CR service users was good. Redesigning CR services to offer more rehabilitation delivery options, aligned with patient choice may increase uptake and further trials are needed to assess the impact.
October 2023 Br J Cardiol 2023;30:157 doi:10.5837/bjc.2023.032
Investigating infective endocarditis: teaching hospitals to choose wisely
Jake Williams, Megan Rawcliffe, Mark T Mills, David R Warriner

Transthoracic echocardiography (TTE) is used to assess for evidence of infective endocarditis (IE). Inappropriate patient selection leads to significant burden on healthcare services. We aimed to assess effectiveness of cardiology consultant vetting of TTE requests for suspected IE in reduction of unnecessary scans. All inpatient TTE requests querying IE over a six-month period were vetted. Clinical information and pathology results were reviewed, and requests were either accepted, deferred, or rejected. A total of 103 patients had TTE requested: 39 (38%) were accepted for scan; four cases of IE were confirmed on TTE. There were 62% of patient requests rejected and not scanned, and no cases of IE subsequently diagnosed. Thus, consultant vetting of TTE requests for suspected IE is an effective way to safely reduce unnecessary scans and enables cost-effective streamlining of echocardiography services.
October 2023 Br J Cardiol 2023;30:138 doi:10.5837/bjc.2023.033
Share The Pressure
Michaela Nuttall, Mark Cobain, Shaantanu Donde, Joanne Haws

This paper summarises ‘Share The Pressure’, a project that developed and piloted a scalable model for engaging patients on the benefits of risk factor control for healthy ageing; training healthcare professionals (HCPs) in cardiovascular disease (CVD) risk communication; and improving the shared decision-making process between nurses, pharmacists and patients. The study features the use of a CVD risk tool called Heart Age, which has been shown to effectively motivate risk factor reduction in individuals.
The study team engaged virtually with patients and HCPs through established relationships within the community, third sector, charities, and social media. In addition, patients living with high blood pressure (hypertension) participated via online focus groups and surveys, which provided insight into patients’ preferences for conveying CVD risk, quantification of intervention benefits, side effects and processes to facilitate shared decision-making.
This insight gained from the focus group and survey data informed adaptations made to the Heart Age tool to provide ‘years off’ – or lowering of heart age – benefits for different aspects of blood pressure lowering, focusing on the independent and joint benefits of medication management and lifestyle.
The study piloted a training programme for nurses and pharmacists to support them in communicating and framing risk and intervention benefits.
The study trained 1,148 HCPs from 37 countries over 17 sessions. Post-training survey results of HCPs indicated an increase in self-rated knowledge and a strong likelihood of applying information learned to their clinical practice. In addition, the Heart Age users found the personalised report and Heart Age test results very motivating for patients with high blood pressure.
October 2023 Br J Cardiol 2023;30:132–7 doi:10.5837/bjc.2023.034
Mitral valve TEER in the UK: what you need to know as TEER becomes routinely available in the NHS
Daniel J Blackman, Sam Dawkins, Robert Smith, Jonathan Byrne, Dominik Schlosshan, Philip A MacCarthy

Transcatheter edge-to-edge repair (TEER) was first performed in 2003, and is now established across the developed world as an effective, minimally invasive treatment option for patients with mitral regurgitation (MR). Multiple large registries have established the efficacy of mitral TEER in patients with primary or degenerative MR in whom surgery is considered prohibitive or high risk, while ongoing randomised-controlled trials will determine its role in younger and lower-risk patients. In patients with secondary or functional MR, in whom mitral valve surgery is not routinely recommended, the pivotal COAPT trial showed a profound reduction in both mortality and heart failure hospitalisation in carefully selected patients.
NHS England approved the routine commissioning of mitral TEER in 2019, and following a substantial delay, due in large part to the COVID pandemic, the procedure is now widely available across the UK. This review article describes the TEER procedure, currently available devices, the underlying evidence base, and the key facts needed for clinicians to understand who, how, and where to refer patients for consideration of mitral TEER. The emerging role of TEER in patients with severe symptomatic tricuspid regurgitation is also considered.
September 2023 Br J Cardiol 2023;30:95–8 doi:10.5837/bjc.2023.025
Screening for the vulnerable aorta: targeting high-risk groups in the population
Riccardo Proietti, Mark Field, Victoria McKay, Gregory Y H Lip, Manoj Kuduvalli, on behalf of UK Aortic Society

Thoracic aortic aneurysms are often asymptomatic until patients present with a life-threatening acute aortic syndrome. The vulnerability of an aorta to an acute aortic syndrome is determined by cross-sectional diameter and underlying aetiological factors, such as genotype or acquired disease. Screening the general population for thoracic aneurysms presents multiple resource issues including the availability of imaging modalities. Targeted screening of high-risk groups provides the only currently pragmatic solution. Opportunistic imaging through lung cancer screening programmes could pick up a proportion. Until we have a comprehensive screening programme it is incumbent on all healthcare professionals to have a low threshold for considering acute aortic pathologies when reviewing patients presenting with chest pain.
September 2023 Br J Cardiol 2023;30:105 doi:10.5837/bjc.2023.026
Where are we getting it wrong? Prevalence and causes of unplanned SAVR in a UK regional cardiac centre
Montasir H Ali, Amir Mushtaq, Abdul R A Bakhsh, Ahmed Salem, Kawan Abdulwahid, Adrian Ionescu

Surgical aortic valve replacement (SAVR) prolongs life and improves its quality in patients with severe aortic stenosis (AS). Unplanned SAVR is a failure of AS screening and follow-up programmes. We identified all elective, first, isolated SAVRs performed between 1 January and 31 December 2019 in a Welsh tertiary cardiac centre, and documented the clinical and echocardiographic variables, and reasons for unplanned SAVR.
Of 140 isolated SAVR, 37 (26%) were unplanned (16 female, mean age 72.3 ± 8.4 years). Twenty had been on the SAVR waiting list and had expedited operations because of concerns about the severity of the AS (12 patients), or because of acute (four patients) or chronic (four patients) left ventricular failure (LVF). Of the 17 not on the waiting list, AS was known in seven: three had acute pulmonary oedema while under follow-up with ‘moderate AS’, one had been referred but developed pulmonary oedema while waiting for a surgical outpatient appointment, one refused SAVR but was subsequently admitted with acute pulmonary oedema and accepted SAVR, one was admitted directly from home because concerns about worsening AS, and one had infective endocarditis with severe aortic regurgitation. Of 10 patients with a new diagnosis of AS, five presented with LVF, four with angina and in three there was a history of syncope (p=0.003 vs. known AS; multiple symptoms). Survival, age, Canadian Cardiovascular Society (CCS) and New York Heart Association (NYHA) class, number of risk factors, peak and mean aortic valve (AV) gradients, AV area, and stroke volume index were not different between patients who had planned versus unplanned SAVR, or with known or new AS. Patients with a new diagnosis of AS had longer pre-operative wait (22.3 ± 9.3 vs. 6.0 ± 10.3 days, p<0.001).
In conclusion, a quarter of SAVRs are unplanned and half are in patients without a prior diagnosis of AS. Unplanned SAVR is associated with prolonged length of hospital stay and with a history of syncope, but other conventional clinical and echocardiographic parameters do not differ between patients undergoing planned versus unplanned SAVR.
September 2023 Br J Cardiol 2023;30:91–4 doi:10.5837/bjc.2023.027
Navigating the research landscape in cardiology. Part 1: research – career necessity or bonus?
Hibba Kurdi, Aderonke Abiodun, Mark Westwood, C Fielder Camm

Undertaking a period of research in cardiology is considered a vital part of training. This has many advantages including enhancing skills that better equip the clinician for patient care. However, in modern cardiology training, the feasibility and necessity of undertaking a period of formal research during training should be considered on an individual basis. The first of this four-part editorial series will explore the benefits of and obstacles to pursuing research in cardiology, with the aim of equipping the reader with an understanding of the options around research during cardiology training in the UK.
September 2023 Br J Cardiol 2023;30:106–7 doi:10.5837/bjc.2023.028
NICE guidelines in the Sunderland RACPC cohort study: one size does not fit all
Kerrick Hesse, Zaw Htet, Mickey Jachuck, Nicholas Jenkins

At least 5% of GP and accident and emergency (A&E) attendances are undifferentiated chest pain. Rapid access chest pain clinics (RACPC) offer urgent guideline-directed management of suspected cardiac chest pain. The National Institute for Health and Care Excellence (NICE) recommends computed tomography coronary angiography (CTCA) as a first-line investigation. We evaluated the effectiveness and efficiency of a local RACPC.
Retrospective analysis of unselected referrals to a RACPC in the Northeast of England was conducted for 2021. Baseline demographics and major adverse cardiovascular events (MACE) were compared between typical, atypical and non-angina. Anatomical and functional imaging results were recorded. Backward stepwise binary logistic regression modelled obstructive coronary artery disease (CAD) incidence.
There were 373/401 (93.0%) patients with chest pain; 139 (37.3%) typical angina, 122 (32.8%) atypical angina and 112 (30.0%) non-angina. Typical angina patients were older (p<0.001) with more cardiovascular risk factors (p<0.001) and increased risk of obstructive CAD (adjusted odds ratio [OR] 6.27, 95% confidence interval [CI] 2.93 to 13.38) and MACE (9.4%, p=0.029). In total, 164 (44.0%) had invasive coronary angiography (ICA) within 7.4 ± 4.8 weeks; 19.5% had normal coronary arteries, 26.2% had obstructive CAD and 22.6% proceeded to invasive haemodynamic assessment ± PCI without major procedural complications. There were 39 (10.5%) who had CTCA within 34.6 ± 18.1 weeks; 25.6% needed ICA to clarify diagnosis.
In conclusion, typical angina patients were at heightened risk of cardiovascular events. In the absence of adequate CTCA capacity, greater reliance on ICA still facilitated accurate diagnosis with options for immediate revascularisation, timely and safely, in the right patients. Better risk stratification and expansion of non-invasive imaging can improve local RACPC service delivery in the wider Northeast cardiology network.
September 2023 Br J Cardiol 2023;30:119–20 doi:10.5837/bjc.2023.029
Large fusiform aneurysm of the superior vena cava: CT findings
Nihal M Batouty, Donia M Sobh, Hoda M Sobh, Ahmed M Tawfik

A 62-year-old man presented complaining of atrial fibrillation. Plain chest radiography and contrast-enhanced computed tomography (CT) revealed a large fusiform aneurysmal dilatation of the upper segment of the superior vena cava (SVC) without evidence of rupture, thrombosis, or pulmonary embolism. It was decided to treat the patient conservatively with follow-up imaging recommended.
August 2023 Br J Cardiol 2023;30:117–8 doi:10.5837/bjc.2023.024
Mechanical life support algorithm for the emergency management of patients with left-sided Impella
Waqas Akhtar, Kristine Kiff, Agnieszka Wypych-Zych, Sofia Pinto, Audrey K H Cheng, Winston Banya, Alexander Rosenberg, Christopher T Bowles, John Dunning, Vasileios Panoulas

We sought to remedy the limited guidance that is available to support the resuscitation of patients with the Impella Cardiac Power (CP) and 5.0 devices during episodes of cardiac arrest or life-threatening events that can result in haemodynamic decompensation.
In a specialist tertiary referral centre we developed, by iteration, a novel resuscitation algorithm for Impella emergencies, which we validated through simulation and assessment by our multi-disciplinary team. A mechanical life support course was established to provide theoretical and practical education, combined with simulation to consolidate knowledge and confidence in algorithm use. We assessed these measures using confidence scoring, a key performance indicator (the time taken to resolve a suction event) and a multiple-choice question (MCQ) examination.
Following this intervention, median confidence score increased from 2 (interquartile range [IQR] 2 to 3) to 4 (IQR 4 to 4) out of a maximum of 5 (n=53, p<0.0001). Theoretical knowledge of the Impella, as assessed by median MCQ score, increased from 12 (IQR 10 to 13) to 13 (12 to 14) out of a maximum of 17 (p<0.0001).
The use of a bespoke Impella resuscitation algorithm reduced the mean time taken to identify and resolve a suction event by 53 seconds (95% confidence interval 36 to 99, p=0.0003).
In conclusion, we present an evidence-based resuscitation algorithm that provides both technical and medical guidance to clinicians responding to life-threatening events in Impella recipients.
July 2023 Br J Cardiol 2023;30:113–6 doi:10.5837/bjc.2023.020
The usefulness of initial serum ferritin level as a predictor of in-hospital mortality in STEMI
Mahmoud Abdelnabi, Abdallah Almaghraby, Juthipong Benjanuwattra, Yehia Saleh, Rawan Ghazi, Ahmed Abd El Azeem

Several studies have shown that elevated serum ferritin level is associated with a higher risk of coronary artery disease. Recently, it has been shown that high serum ferritin levels in men are independently correlated with an increased risk of cardiovascular mortality. This study aimed to investigate the possible correlation between the initial serum ferritin level and in-hospital mortality in patients presenting with ST-elevation myocardial infarction (STEMI).
This retrospective cohort study included 890 patients who presented with acute STEMI and underwent successful primary percutaneous coronary intervention (PPCI) according to the standard techniques during the period from 1 May 2020 to 1 May 2021. At the time of admission, an initial serum ferritin level was measured in all patients. Comparison between initial ferritin levels was made between two groups: died and survived. Propensity matching was performed to exclude confounding factors effect.
Forty-one patients had in-hospital mortality. There was no significant difference between both groups regarding baseline clinical characteristics. Initial serum ferritin levels were higher in deceased patients, even after propensity matching.
In conclusion, even after propensity matching, initial ferritin levels were significantly higher in patients who died after being admitted for STEMI.
July 2023 Br J Cardiol 2023;30:99–103 doi:10.5837/bjc.2023.021
Cardiac catheterisation: avoiding common pitfalls with transradial vascular access
Matthew Sadler, Clive Lawson

Cardiac catheterisation is a common invasive procedure. Transradial vascular access is the default approach due to a reduced risk of vascular and bleeding complications. Although transradial vascular access complications are infrequent it is important to identify, mitigate and manage them appropriately when they arise. Several techniques have been identified to try to reduce their occurrence pre- and post-procedurally, as well as manage any complication sequalae. This review article summarises the incidence, type, prevention and management of complications encountered in transradial vascular access.
July 2023 Br J Cardiol 2023;30:108–12 doi:10.5837/bjc.2023.022
The effect of icosapent ethyl on left atrial and left ventricular morphology
Spencer S Kitchin, Suvasini Lakshmanan, April Kinninger, Song S Mao, Mark G Rabbat, Deepak L Bhatt, Matthew J Budoff

Atrial fibrillation (AF) is a common arrhythmia associated with poor outcomes. N-3 fatty acids have been shown to provide significant cardiovascular risk reduction, but they may exacerbate the risk of AF. The pathway by which N-3 fatty acids may be arrhythmogenic is unknown. One possible mechanism involves cardiac chamber morphology alteration. The purpose of this study was to investigate the effect of icosapent ethyl (IPE) on left atrial (LA) size and left ventricular (LV) mass.
This study used coronary computed tomographic angiography images gathered from the Effect of Icosapent Ethyl on Progression of Coronary Atherosclerosis (EVAPORATE) trial. EVAPORATE was a randomised, double-blind, placebo-controlled study finding a significant reduction in coronary atherosclerosis progression in patients with residually elevated triglycerides despite statin therapy on 4 g IPE daily versus 4 g placebo daily. Computed tomography images were used to measure LA size and LV mass at 0 and 18 months.
Of 80 enrolled patients, 68 were included in the final analysis. Baseline demographics and risk factors were similar between IPE and placebo cohorts. LA anterior-posterior diameter measured on axial (p=0.51) and sagittal (p=0.52) orientations were not different over time. Also, there was no difference between groups in the change in LA volume (p=0.84). Change in LV mass was similar between groups (p=0.13).
In conclusion, this study did not detect differences in LA size or LV mass over 18 months between patients on 4 g daily IPE versus placebo.
June 2023 Br J Cardiol 2023;30:56–61 doi:10.5837/bjc.2023.016
Evaluating the impact of the COVID-19 pandemic on the delivery and efficiency of cardiac rehabilitation
Natalie Kilner, Sharlene Greenwood, Janet Cable, Iain Waite

The SARS-CoV-2 (COVID-19) pandemic brought disruption to cardiac rehabilitation (CR) services in the UK, requiring innovation and use of remote interventions. This retrospective longitudinal study compares single-centre CR service data across three time periods: ‘pre’ (June 2019 to December 2019), ‘during’ (January 2020 to May 2020) and ‘post’ (June 2020 to December 2020), evaluating adaptations in programme delivery and subsequent effect on efficiency.
There were 614 patients (72.7% male) identified between June 2019 and December 2020. Eligible CR referrals reduced 30.3% and encountered >50% decrease in engagement ‘during’ the pandemic, compared with ‘pre’ pandemic. The ‘post’ pandemic hybrid redesign led to a significant reduction in hospital discharge to CR contact (mean 5.39 days, p=0.001), and time spent in CR (41.33 days, p=0.001) when compared with ‘pre’ and ‘during’ figures. CR engagement significantly increased ‘post’ pandemic for ST-elevation myocardial infarction (STEMI)/non-STEMI (NSTEMI)/acute coronary syndrome (ACS) (56%, p=0.02) and ‘post’ cardiac surgery (76%, p=0.015). Referrals to cardiac psychology increased >50% ‘post’ pandemic (7.8%, p=0.038).
A ‘post’ pandemic hybrid CR programme is effective at reducing wait times, increasing engagement and reducing time to completion of CR, compared with ‘pre’ and ‘during’ pandemic figures. A significant increase in cardiac psychology referrals ‘post’ pandemic highlights the importance of psychology support within CR.
June 2023 Br J Cardiol 2023;30:70–3 doi:10.5837/bjc.2023.017
Metabolic syndrome components determine the presence of subclinical atherosclerosis in obese and overweight
Gustavo A Giunta, Pablo D Cutine, María F Aguiló Iztueta, Daniel Pirola, Nahuel Messina, Lorena Helman, María I Rodríguez Acuña, Ariel Kraselnik, Laura Brandani, Juan J Badimon

Metabolic syndrome (MS) is frequently associated with an increased body mass index (BMI), and related to an adverse cardiovascular prognosis. The purpose of this study is to evaluate the prevalence and association between MS, obesity and subclinical atherosclerosis (SA).
This cross-sectional study included healthy adults, allocated to normal weight (NW) when BMI <25 kg/m2, overweight (OW) BMI ≥25 and <30 kg/m2, or obese (OB) BMI ≥30 kg/m2 groups. Presence of MS was defined according to National Cholesterol Education Program (NCEP) criteria. SA was evidenced with vascular ultrasound. Association between SA, obesity and MS, was evaluated by logistic regression models.
There were 3,716 patients studied (female 66.7%, mean age 47 ± 17.5 years). According to BMI, NW represented 28.2%, OW 39.4% and OB 32.4%. MS showed a strong correspondence with BMI (NW 4.9%, OW 21.4%, OB 49.7%; p<0.001). SA was more prevalent in each group when MS was present: NW (25.4% vs. 45.1%, p<0.005), OW (43.2% vs. 58.9%, p<0.0001) and OB (44.2% vs. 57.8%, p<0.0001). Logistic-regression models showed an independent association of SA with MS criteria (arterial hypertension p<0.001; high-density lipoprotein [HDL] p<0.05; and triglycerides p<0.005) adjusted by gender, age and BMI.
In conclusion, overweight and obesity are frequent and strongly linked with MS and SA. Prevalence of SA is high, and is independently associated with MS components. However, BMI could not retain statistical significance in the multi-variate analyses.
June 2023 Br J Cardiol 2023;30:74 doi:10.5837/bjc.2023.018
Diabetic cardiomyopathy: an educational review
Su-Lee Xiao, Emilia Bober, Xenophon Kassianides, Francesco Medici, Han B Xiao

This educational review provides information about the epidemiology of diabetes and heart failure (diabetic cardiomyopathy) and the challenges in diagnosis and screening. Details on how to investigate patients with imaging and other modalities are discussed, as well as an update regarding the efficacy and safety of novel agents for treatment of diabetic cardiomyopathy.
May 2023 Br J Cardiol 2023;30:51–5 doi:10.5837/bjc.2023.013
Reasons and resolutions for gender inequality among cardiologists and cardiology trainees
Clara Portwood

Women represented 29% of cardiology trainees and 16% of consultants in the UK in 2021. While the numbers of women in cardiology have increased over the last 20 years, these proportions remain among the lowest in comparison with other medical specialties. This essay aims to explore the contributing factors behind, and plans to reduce, gender disparity in cardiology.
PubMed was searched using keywords such as ‘gender’, ‘inequality’, ‘women’, ‘training’ and ‘cardiology’. Retrieved studies were screened for themes contributing towards, and strategies to overcome, gender inequality within cardiology.
Reasons for gender inequality included poor perceptions of cardiology as a female-friendly specialty, experiences of gender-based discrimination, inflexible working hours, poor work–life balance, and lack of female role models. Recommended resolutions should target these themes; increase opportunities for flexible working hours, enforce a discrimination-free workplace culture, and encourage mentoring relationships between female senior and junior doctors. Improving the experience of the existing female workforce in cardiology will have a knock-on effect on the perceptions of trainees rotating through departments, in addition to initiatives promoting cardiology as a female-friendly specialty.
In conclusion, promoting gender equality within cardiology remains an ongoing challenge. Nationwide efforts to increase retention and improve perceptions should target issues highlighted by the voices of women.
May 2023 Br J Cardiol 2023;30:69 doi:10.5837/bjc.2023.014
Assessing opinion on lower LDL-cholesterol lowering, and the role of newer lipid-reducing treatment options
Derek L Connolly, Azfar Zaman, Nigel E Capps, Steve C Bain, Kevin Fernando

While statins are the gold standard for lipid-lowering therapies, newer therapies, such as PCSK9 inhibitors, have also demonstrated low-density lipoprotein cholesterol (LDL-C) reduction, but with a similar or better safety profile. Conflicting guidance has contributed to a low uptake. More up-to-date, evidence-led guidance supports greater use of newer therapies, particularly in combination with statins, to reduce LDL-C to levels shown to be effective in trials. The aim of this study was to determine how such guidance can be implemented more effectively in the UK.
Using a modified Delphi approach, a panel of healthcare professionals with an interest in the management of dyslipidaemia developed 27 statements across four key themes. These were used to form an online survey that was distributed to healthcare professionals working in cardiovascular care across the UK. Stopping criteria included 100 responses received, a seven-month window for response (September 2021 to March 2022), and 90% of statements passing the predefined consensus threshold of 75%.
A total of 109 responses were analysed with 23 statements achieving consensus (four statements <75%). Variance was observed across respondent role, and by UK region. From the high degree of consensus, seven recommendations were established as to how evidence-based guidance can be delivered, including a call for personalised therapy strategies and simplification of LDL-C goals, which should be achieved within as short a time as possible.
May 2023 Br J Cardiol 2023;30:79–80 doi:10.5837/bjc.2023.015
Concurrent left ventricular and left anterior coronary artery thrombus: is COVID-19 an innocent bystander?
Vincenzo Somma, Anthony Brennan, Francis Ha, Adam Trytell, Khoa Phan, Kegan Moneghetti

We present the angiographic findings of a case of myocardial infarction associated with COVID-19 with a heavy burden of thrombus, despite only minor obstructive coronary disease.
April 2023 Br J Cardiol 2023;30:75–6 doi:10.5837/bjc.2023.011
The role of vitamin D/calmodulin/calcium signalling/ACE2 pathway in COVID-19
Artemio García-Escobar, Silvio Vera-Vera, Daniel Tébar-Márquez, Alfonso Jurado-Román, Santiago Jiménez-Valero, Guillermo Galeote, José Ángel Cabrera, Raul Moreno

There has been suggestion that vitamin D may play a role in protection against severe infection with COVID-19. In this article a potential mechanism involving angiotensin-converting enzyme 2 (ACE2) is proposed.
April 2023 Br J Cardiol 2023;30:62–8 doi:10.5837/bjc.2023.012
Diagnosis and acute management of type A aortic dissection
Metesh Acharya, Giovanni Mariscalco

Acute type A aortic dissection is a devastating aortic disease associated with significant morbidity and mortality. Clinicians should maintain a high degree of suspicion in patients presenting with sudden-onset chest pain, although the diagnosis may be confounded by the broad spectrum of attendant symptoms and signs. Accurate and timely identification of the acute dissection is of paramount importance to ensure suitable patients are referred promptly for definitive surgical management. This review focuses on the diagnosis of acute type A aortic dissection and discusses the haematological tests, and electrocardiographic, echocardiographic and radiological investigations necessary to confirm the diagnosis and assess for associated complications. The acute medical management of patients with acute type A dissection is also reviewed.
March 2023 Br J Cardiol 2023;30:16–20 doi:10.5837/bjc.2023.009
Acute aortic dissection (AAD) – a lethal disease: the epidemiology, pathophysiology and natural history
Karen Booth (on behalf of UK-AS, the UK Aortic Society)

Aortic dissection is a life-threatening condition that is often under-recognised. In the first in a series of articles about the condition, the epidemiology, pathology, classification and clinical presentation of aortic dissection are discussed.
February 2023 Br J Cardiol 2023;30:26–30 doi:10.5837/bjc.2023.006
Antibiotic prophylaxis for patients at risk of infective endocarditis: an increasing evidence base?
Mark J Dayer, Martin Thornhill, Larry M Baddour

Around 100 years ago, the first link between infective endocarditis (IE) and dental procedures was hypothesised; shortly after, physicians began to use antibiotics in an effort to reduce the risk of developing IE. Whether invasive dental procedures are linked to the development of IE, and antibiotic prophylaxis (AP) is effective, have since remained topics of controversy. This controversy, in large part, has been due to the lack of prospective randomised clinical trial data. From this suboptimal position, guideline committees representing different societies and countries have struggled to reach an optimal position on whether AP use is needed for invasive dental procedures (or other procedures) and in whom. We present the findings from an investigation involving a large US patient database, published earlier this year, by Thornhill and colleagues. The work featured the use of both a cohort and case-crossover design and demonstrated there was a significant temporal association between invasive dental procedures and development of IE in high-IE-risk patients. Furthermore, the study showed that AP use was associated with a reduced risk of IE. Additional data, also published this year, from a separate study using nationwide hospital admissions data from England by Thornhill’s group, showed that certain dental and non-dental procedures were significantly associated with the subsequent development of IE. Two other investigations have reported similar concerns for non-dental invasive procedures and risk of IE. Collectively, the results of this work support a re-evaluation of the current position taken by the National Institute for Health and Care Excellence (NICE) and other organisations that are responsible for publishing practice guidelines.
February 2023 Br J Cardiol 2023;30:35–8 doi:10.5837/bjc.2023.007
Cardiac sarcoidosis: the role of cardiac MRI and 18F-FDG-PET/CT in the diagnosis and treatment follow-up
Muntasir Abo Al Hayja, Sobhan Vinjamuri

Sarcoidosis is a multi-factorial inflammatory disease characterised by the formation of non-caseating granulomas in the affected organs. Cardiac involvement can be the first, and occasionally the only, manifestation of sarcoidosis. The prevalence of cardiac sarcoidosis (CS) is higher than previously suspected. CS is associated with increased morbidity and mortality. Thus, early diagnosis is critical to introducing immunosuppressive therapy that could prevent an adverse outcome. Endomyocardial biopsy (EMB) has limited utility in the diagnostic pathway of patients with suspected CS. As a result, advanced imaging modalities, i.e. cardiac magnetic resonance imaging (MRI) and positron emission tomography with 18F-Fluorodeoxyglucose/computed tomography scan (18F-FDG-PET/CT), have emerged as alternative tools for diagnosing CS and might be considered the new ‘gold standard’. This focused review will discuss the epidemiology and pathology of CS, when to suspect and evaluate CS, highlight the complementary roles of cardiac MRI and 18F-FDG-PET/CT, and their diagnostic and prognostic values in CS, in the current content of guidelines for the diagnostic workflow of CS.
January 2023 Br J Cardiol 2023;30:21–5 doi:10.5837/bjc.2023.002
Evaluating initiation and real-world tolerability of dapagliflozin for the management of HFrEF
Alyson Hui Ling Tee, Gayle Campbell, Andrew D’Silva

Untreated heart failure with reduced ejection fraction (HFrEF) has a one-year mortality rate of 40%. The DAPA-HF trial found that dapagliflozin reduces mortality and heart failure (HF) hospitalisation by 17% and 30%, respectively. We describe the initiation and real-world tolerability of dapagliflozin for the management of HFrEF at a large university teaching hospital in central London.
We reviewed 118 HFrEF patients initiated on dapagliflozin from January to August 2021 in both inpatient and outpatient settings using the Trust’s electronic records. A total of 69 (58.4%) patients were on optimised HF pharmacological therapy upon initiation of dapagliflozin. Dapagliflozin was discontinued in 12 (13.0%) patients. Twenty-three (42.6%) patients either discontinued or had a dose reduction in loop diuretics post-initiation of dapagliflozin.
In clinical practice, early initiation of dapagliflozin is safe, well-tolerated and resulted in earlier discontinuation or dose reduction in loop diuretics, providing opportunities to further optimise other HF medicines. This retrospective observational study supports the safety of the updated European Society of Cardiology (ESC) guidelines to initiate all four key HF medicines to minimise delays in HF treatment optimisation, which could translate to reduced National Health Service healthcare costs through fewer HF hospitalisations.
January 2023 Br J Cardiol 2023;30:39–40 doi:10.5837/bjc.2023.004
Pectus excavatum with right ventricular compression-induced ventricular arrhythmias
Lisa Ferraz, Diana Carvalho, Simão Carvalho, Adriana Pacheco, Ana Faustino, Ana Neves

A 33-year-old woman, with palpitations since the age of 15, was referred to a cardiology consultation due to very frequent ventricular extrasystoles with morphology of left bundle branch block, inferior frontal axis, late precordial transition, rS in V1, R in V6 and rS in DI. She had pectus excavatum. The cardiac magnetic resonance showed severe pectus excavatum associated with exaggerated cardiac levoposition, compression and deformation of the right cardiac chambers. However, the patient became pregnant, and follow-up was delayed.
January 2023 Br J Cardiol 2023;30:31–4 doi:10.5837/bjc.2023.005
The prognostic impact of HDL-C level in patients presenting with ST-elevation myocardial infarction
Ahmed Mahmoud El Amrawy, Abdallah Almaghraby, Mahmoud Hassan Abdelnabi

Low high-density lipoprotein-cholesterol (HDL-C) concentration is among the strongest independent risk factors for cardiovascular disease, however, studies to assess the cardioprotective effect of normal or high HDL-C level are lacking.
To determine the prognostic impact of initial serum HDL-C level on in-hospital major adverse cardiovascular and cerebrovascular events (MACCE) and the one-year all-cause mortality in patients presenting with ST-elevation myocardial infarction (STEMI) we performed a retrospective analysis of the data from 1,415 patients presenting with STEMI in a tertiary-care centre equipped with a 24-hour-ready catheterisation laboratory. The period from June 2014 to June 2017 was reviewed with a follow-up as regards one-year all-cause mortality. Patients were divided into two groups according to HDL-C level. HDL-C <40 mg/dL (2.22 mmol/L) was considered low, while HDL-C ≥40 mg/dL was considered normal.
There were 1,109 patients with low HDL-C, while 306 had normal HDL-C levels, which was statistically significant (p<0.001). Total MACCE and all-cause mortality were significantly lower in patients with normal HDL-C (p=0.03 and p=0.01, respectively).
In conclusion, this retrospective study to assess the prognostic effect of HDL-C in patients presenting with STEMI, found normal HDL-C level was associated with lower in-hospital MACCE and all-cause mortality at one-year follow-up.
November 2022 Br J Cardiol 2022;29:141–4 doi:10.5837/bjc.2022.037
Outpatient-based acute HF care calls for development of clinical psychology service for whole-person care provision
Abdullah Abdullah, Suzanne Y S Wong, Robbie Jones, Kenneth Y K Wong

Acute heart failure (AHF) is associated with 9.3% mortality. Depression and hopelessness are prevalent. We conducted an online survey using Survey Monkey, via the UK Heart Failure (HF) Investigators Research Network of 309 cardiologists, in 2021, to determine: what proportion of UK centres offer outpatient-based management (OPM) for AHF including the use of parenteral diuretics; and what proportion of HF services have clinical psychology support.
There were 51 services that responded, and an estimated 25,135 patients with AHF receive inpatient care per year (median 600 per site). There are 2,631 patients (median 50 per site) treated per year with OPM (9.7% of the population of AHF patients). While 65% of centres provided access to OPM, only 20% have a clinical psychology service.
In conclusion, nearly 10% of patients with AHF receive outpatient-based intravenous diuretic therapy. Only 20% of hospitals have a clinical psychology service for patients who suffer from HF.
November 2022 Br J Cardiol 2022;29:145–9 doi:10.5837/bjc.2022.038
Should we be screening people with diabetes for atrial fibrillation? Exploring patients’ views
Angela Hall, Andrew Robert John Mitchell, Lisa Ashmore, Carol Holland

Atrial fibrillation (AF) and diabetes are increasingly prevalent worldwide, both increasing stroke risk. AF can be detected by patient-led electrocardiogram (ECG) screening applications. Understanding patients’ views around AF screening is important when considering recommendations, and this study explores these views where there is an existing diagnosis of diabetes.
Nine semi-structured qualitative interviews were conducted with participants from a previous screening study (using a mobile ECG device), who were identified with AF. Thematic analysis was completed using NVivo 12 Plus software and themes were identified within each research question for clarity.
Themes were identified in four groups:
In conclusion, eliciting patients’ views has demonstrated the need for clear and concise information around the delivery of an AF diagnosis. Screening initiatives should factor in location, convenience, personnel, and cost, all of which were important for promoting screening inclusion.
November 2022 Br J Cardiol 2022;29:150–3 doi:10.5837/bjc.2022.039
Patient satisfaction with telephone consultations in cardiology outpatients during the COVID-19 pandemic
Jack William Goodall, Ravish Katira

The COVID-19 pandemic required a radical change in healthcare delivery methods, including the remote delivery of many outpatient services. We aimed to understand patient satisfaction with telephone consultations.
Patients who had undergone a cardiology telephone consultation between 24 February and 19 July 2021 were asked to complete a survey. The survey assessed their satisfaction with the consultation and their preference between remote and face-to-face consultation. The 56 responses demonstrated high levels of satisfaction with 56% agreeing they were “completely satisfied” with the consultation compared with 5% who disagreed. However, 63% would have preferred a face-to-face appointment compared with 22% preferring a telephone consultation.
No patterns were observed that might help to guide who should be offered the different modalities of consultation; to maximise patient satisfaction a flexible and individualised approach is likely to be required.
November 2022 Br J Cardiol 2022;29:137–40 doi:10.5837/bjc.2022.034
Evaluation of a lipid management pathway within a local cardiac rehabilitation service
Claire Jones

Elevated cholesterol/lipid levels, especially low-density lipoprotein cholesterol (LDL-C) are known to contribute to the development of atherosclerotic cardiovascular disease (ASCVD). The attainment of lipid targets is known to be suboptimal both globally and locally. This study aimed to evaluate the effectiveness of a lipid management pathway (LMP) in supporting attainment of lipid targets following an acute coronary syndrome (ACS) in a local cohort of cardiac rehabilitation (CR) patients.
Quantitative data were retrospectively collected from 54 CR patient records. Local lipid target attainment was benchmarked against national guidelines and pre-pathway implementation audit results.
The number of admission lipid profiles increased by 24.8% to 79.6% following implementation of the LMP. There was a 31% improvement in the number of patients achieving either a 50% reduction in LDL-C or an LDL-C level of <1.4 mmol/L. In conclusion, the LMP had a significant positive impact upon the attainment of lipid goals.
November 2022 Br J Cardiol 2022;29:155–7 doi:10.5837/bjc.2022.036
COVID-19 related myopericarditis and cardiac tamponade: a diagnostic conundrum
Nirmol Amin Meah, Hon-Ting Wai, Kalyan Ram Bhamidipati, Sukumaran Binukrishnan

We report the case of a 45-year-old man presenting with worsening shortness of breath and chest tightness on a background of type 2 diabetes mellitus, hypertension and stable angina. He felt generally unwell and had a productive cough two weeks prior to presentation. Initial examination found quiet heart sounds and reduced air entry bi-basally on auscultation. Electrocardiography (ECG) demonstrating lateral T-wave flattening and ongoing chest tightness directed management towards an acute coronary syndrome (ACS). However, negative troponin I and positive D-dimer prompted investigation with computed tomography pulmonary angiogram (CTPA) identifying a 3.5 cm thickness pericardial effusion and no pulmonary embolism. Initial COVID-19 nasopharyngeal swabs were negative for SARS-CoV-2. Echocardiography identified features consistent with cardiac tamponade prompting pericardiocentesis. Over 1,000 ml of straw-coloured aspirate was drained with significant clinical improvement, and the patient was discharged with plans for urgent outpatient cardiac magnetic resonance imaging (MRI). Interestingly, despite multiple negative nasopharyngeal swabs for COVID-19, serum antibodies to SARS-CoV-2 were detected.
October 2022 Br J Cardiol 2022;29:154 doi:10.5837/bjc.2022.032
A retrospective observational study of the use of gastroprotection for patients on dual antiplatelet therapy
Ee Woon Wong, Liam Bastian, Mike Wilcock

Dual antiplatelet therapy is recommended for secondary prevention of ischaemic events in coronary artery disease. Some patients, who may be at high bleed risk if other factors are present, should be considered for gastroprotection. In our survey, we assessed whether gastroprotection was prescribed for hospital inpatients, especially high-risk patients, who were receiving dual antiplatelet therapy at discharge, and the type of gastroprotection prescribed. We found that over 13 months, a total of 1,693 patient episodes were prescribed dual antiplatelet therapy at discharge, of which 71% also received gastroprotection. Of the patient episodes who were not prescribed gastroprotection, 46% (223/483) met the criterion of age as a risk factor for gastroprotection. A further 30 episodes met other risk criteria of certain concomitant drugs or prior comorbidity. There is a need among clinicians and pharmacy teams within the hospital for recognition and management of this opportunity to improve the care of these patients.
October 2022 Br J Cardiol 2022;29:158–60 doi:10.5837/bjc.2022.033
Echocardiography in new-onset heart failure: a mid-ventricular Takotsubo case report
Milaras Nikias, Boli Aikaterini, Beneki Eirini, Nevras Vasilios, Zachos Panagiotis, Tsatiris Konstantinos

We report the case of an elderly woman with recent hip replacement surgery that presented with cardiogenic shock. The initial echocardiogram was suggestive of mid-ventricular Takotsubo cardiomyopathy, which was later confirmed due to absence of severe coronary artery disease and complete resolution of the patient’s cardiac systolic dysfunction. Fluid and inotrope administration in the acute phase, and guideline-directed medical therapy for heart failure, thereafter, led to full recovery.
August 2022 Br J Cardiol 2022;29:106–8 doi:10.5837/bjc.2022.027
It’s time to ‘Build Back Fairer’: what can we do to reduce health inequalities in cardiology?
Cong Ying Hey

Disparities in cardiovascular morbidity and mortality are among the leading health and social care concerns in the UK. The disruption of the COVID-19 pandemic to health services has further placed cardiovascular care and the respective patient communities at the sharp end, not least in exacerbating existing health inequalities across service interfaces and patients’ health outcomes. While the pandemic engenders unprecedented constraints within established cardiology services, it conduces to a unique opportunity to embrace novel transformative approaches within the way we deliver patient care in maintaining best practices during and beyond the crisis. As the first step in navigating toward the ‘new norm’, a clear recognition of the challenges inherent in cardiovascular health inequalities is critical, primarily in preventing the widening of extant inequalities as cardiology workforces continue to build back fairer. We may consider the challenges through the lens of health services’ diverse facets, including the aspects of universality, interconnectivity, adaptability, sustainability, and preventability. This article explores the pertinent challenges and provides a focused narration concerning potential measures to foster equitable and resilient cardiology services that are patient centred in the post-pandemic landscape.
August 2022 Br J Cardiol 2022;29:109–11 doi:10.5837/bjc.2022.029
An audit comparing management of patients with HFrEF at a DGH before and during the COVID-19 pandemic
Olivia Morey, Rebecca Day, Yuk-ki Wong

This audit compared the management of patients with heart failure with reduced ejection fraction (HFrEF) admitted to a district general hospital (DGH) during comparative eight month periods before and during the COVID-19 pandemic. The periods studied were from 1 February 2019 to 30 September 2019 and between the same dates in 2020. We investigated differences in mortality and patient characteristics (age, gender and new or prior diagnosis). For patients who survived to discharge and who were not referred to palliative care, we also investigated whether there were differences in rates of echocardiography and prescription of angiotensin-converting enzyme (ACE) inhibitors, angiotensin II receptor antagonists and beta blockers.
We found that the number of cases was lower during the pandemic and there was a lower mortality rate that was not statistically significant. There was a higher proportion of new cases (odds ratio [OR] 2.21, 95% confidence interval [CI] 1.24 to 3.94, p=0.008) and of female patients (OR 2.03, 95%CI 1.14 to 3.61, p=0.019). For survivors, there was a non-significant decrease in prescription rates for ACE inhibitors and angiotensin II receptor antagonists (81.6% vs. 71.4%, p=0.137) that was not seen for beta blockers. The length of stay was increased and there was also an increase in the interval between admission and echocardiography in patients who were newly diagnosed. Regardless of time period, the time before echocardiography was significantly associated with length of stay.
August 2022 Br J Cardiol 2022;29:119–20 doi:10.5837/bjc.2022.030
SARS-CoV-2 dilated cardiomyopathy
Manuel Felipe Cáceres-Acosta, Bairon Díaz Idrobo, Diana Carolina Urbano Albán

SARS-CoV-2 is an emerging cause of viral myocarditis that generates multiple complications, such as dilated cardiomyopathy. We describe a young, obese male patient with severe myocardial involvement by the SARS-CoV-2 virus, who presented with chest pain, elevated cardiac enzymes, non-specific electrocardiographic findings, echocardiogram with evidence of dilated heart disease with reduced ejection fraction, and subsequent verification using magnetic resonance imaging (MRI). The results of the cardiac MRI were typical of viral myocarditis. The patient did not respond to a short course of systemic steroids and the standard management for heart failure, had multiple re-admissions, and, unfortunately, died.
July 2022 Br J Cardiol 2022;29:89–94 doi:10.5837/bjc.2022.023
Age and the power of zero CAC in cardiac risk assessment: overview of the literature and a cautionary case
John P Sheppard, Suvasini Lakshmanan, Seth J Lichtenstein, Matthew J Budoff, Sion K Roy

The coronary artery calcium (CAC) score is a marker of advanced coronary atherosclerosis. Numerous prospective cohorts have validated CAC as an independent marker that improves prognostication in atherosclerotic cardiovascular disease (ASCVD) beyond traditional risk factors. Accordingly, CAC is now incorporated into international cardiovascular guidelines as a tool to inform medical decision-making. Particular interest concerns the significance of zero CAC score (CAC=0). While many studies report CAC=0 to virtually exclude obstructive coronary artery disease (CAD), non-negligible rates of obstructive CAD despite CAC=0 are reported in certain populations. Overall, the current literature supports the power of zero CAC as a strong downward risk classifier in older patients, whose CAD burden predominantly involves calcified plaque. However, with their higher burden of non-calcified plaque, CAC=0 does not reliably exclude obstructive CAD in patients under 40 years. Illustrating this point, we present a cautionary case of a 31-year-old patient found to have severe two-vessel CAD despite CAC=0. We highlight the value of coronary computed tomography angiography (CCTA) as the gold-standard non-invasive imaging modality when the diagnosis of obstructive CAD is in question.
July 2022 Br J Cardiol 2022;29:102–5 doi:10.5837/bjc.2022.024
Pain after pacemaker/ICD implants
Selwyn Brendon Goldthorpe

A retrospective study of 322 patient experiences of post-operative pain, short term and long term, following a cardiac implantable electronic device (CIED) procedure. Pain from pacemaker and ICD (implantable cardioverter-defibrillator) implant surgery remains a problem both in terms of severity and longevity. There is a subset of patients receiving implants that have severe pain that may be of a long duration. Patient advice needs to be appropriate to these findings.
This study illustrates a need for better pain management by physicians, support, and realistic communication with their patients.
July 2022 Br J Cardiol 2022;29:112–6 doi:10.5837/bjc.2022.025
Infective endocarditis: acne to zoonoses on the valve, an A to Z perspective
Mark Boyle, Charlene Tennyson, Achyut Guleri, Antony Walker

Cutibacterium acnes (C. acnes), previously known as Propionibacterium acnes, is a rare cause of infective endocarditis (IE). We provide a review of the literature and describe two recent cases from a single centre to provide insight into the various clinical presentations, progression and management of patients with this infection.
The primary objective of our review is to highlight the difficulty in the initial assessment of these patients with an aim to improve the time and accuracy of diagnosis and expedite subsequent treatment. There are currently no guidelines in the literature specific to the management of IE caused by C. acnes. Our secondary objectives are to disseminate information about the indolent course of the disease and add to the growing body of evidence around this rare, yet complex, cause of IE.
July 2022 Br J Cardiol 2022;29:117–8 doi:10.5837/bjc.2022.026
High-output heart failure due to arteriovenous malformation treated by endovascular embolisation
Federico Liberman, Roberto Cooke, María J Cabrera, Santiago Vigo, Guillermo Allende, Luciana Auad, Juan P Ricarte-Bratti

High-output heart failure (HF) is an uncommon condition. This occurs when HF syndrome patients have a cardiac output higher than eight litres per minute. Shunts, such as fistulas and arteriovenous malformations are an important reversible cause. We present the case of a 30-year-old man who presented to the emergency department due to decompensated HF. Echocardiogram showed dilated myocardiopathy with high cardiac output (19.5 L/min calculated on long-axis view). He was diagnosed with arteriovenous malformation by computed tomography (CT) and subsequent angiography, and a multi-disciplinary team decided to perform endovascular embolisation with ethylene vinyl alcohol/dimethyl sulfoxide at different times. The transthoracic echocardiogram showed a significant decrease in cardiac output (9.8 L/min) and his general condition improved significantly.
June 2022 Br J Cardiol 2022;29:95–101 doi:10.5837/bjc.2022.021
Evolution of a circulatory support system with full implantability: personal perspectives on a long journey
Stephen Westaby

Implantable mechanical circulatory support systems have evolved dramatically over the last 50 years. The objective has been to replace or support the failing left ventricle with a device that pumps six litres of blood each minute, a massive 8,640 litres per day. Noisy cumbersome pulsatile devices have been replaced by smaller silent rotary blood pumps that are much more patient friendly. Nonetheless, the tethering to external components, together with the risks of power line infection, pump thrombosis and stroke, must be addressed before widespread acceptance. Infection predisposes to thromboembolism, so elimination of the percutaneous electric cable has the capacity to transform outcomes, reduce costs and improve quality of life.
Developed in the UK, the Calon miniVAD is powered by an innovative coplanar energy transfer system. As such, we consider it can achieve those ambitious objectives.
May 2022 Br J Cardiol 2022;29:46–51 doi:10.5837/bjc.2022.015
Clinical and health economic evaluation of a post-stroke arrhythmia monitoring service
David Muggeridge, Kara Callum, Lynsey Macpherson, Nick Howard, Claudia Graune, Ian Megson, Adam Giangreco, Susan Gallacher, Linda Campbell, Gethin Williams, Ashish Macaden, Stephen J Leslie

Atrial fibrillation (AF) is a major cause of recurrent stroke and transient ischaemic attack (TIA) in the UK. As many patients can have asymptomatic paroxysmal AF, prolonged arrhythmia monitoring is advised in selected patients following a stroke or TIA. This service evaluation assessed the clinical and potential health economic impact of prolonged arrhythmia monitoring post-stroke using R-TEST monitoring devices.
This was a prospective, case-controlled, service evaluation in a single health board in the North of Scotland. Patients were included if they had a recent stroke or TIA, were in sinus rhythm, and did not have another indication for, or contraindication to, oral anticoagulation. A health economic model was developed to estimate the clinical and economic value delivered by the R-TEST monitoring. Approval to use anonymised patient data in this service evaluation was obtained.
During the evaluation period, 100 consecutive patients were included. The average age was 70 ± 11 years, 46% were female. Stroke was the presenting complaint in 83% of patients with the other 17% having had a TIA. AF was detected in seven of 83 (8.4%) patients who had had a stroke and one of 17 (5.9%) patients with a TIA. Health economic modelling predicted that adoption of R-TEST monitoring has a high probability of demonstrating both clinical and economic benefits.
In conclusion, developing a post-stroke arrhythmia monitoring service using R-TEST devices is feasible, effective at detecting AF, and represents a probable clinical and economic benefit
May 2022 Br J Cardiol 2022;29:60–3 doi:10.5837/bjc.2022.017
Total ischaemic time in STEMI: factors influencing systemic delay
Cormac T O’Connor, Abdallah Ibrahim, Anthony Buckley, Caoimhe Maguire, Rajesh Kumar, Jatinder Kumar, Samer Arnous, Thomas J Kiernan

Total ischaemic time in ST-elevation myocardial infarction (STEMI) has been shown to be a predictor of mortality. The aim of this study was to assess the total ischaemic time of STEMIs in an Irish primary percutaneous coronary intervention (pPCI) centre. A single-centre prospective observational study was conducted of all STEMIs referred for pPCI from October 2017 until January 2019.
There were 213 patients with a mean age 63.9 years (range 29–96 years). The mean ischaemic time was 387 ± 451.7 mins. The mean time before call for help (patient delay) was 207.02 ± 396.8 mins, comprising the majority of total ischaemic time. Following diagnostic electrocardiogram (ECG), 46.5% of patients had ECG-to-wire cross under 90 mins as per guidelines; 73.9% were within 120 mins and 93.4% were within 180 mins. Increasing age correlated with longer patient delay (Pearson’s r=0.2181, p=0.0066). Women exhibited longer ischaemic time compared with men (508.96 vs. 363.33 mins, respectively, p=0.03515), driven by a longer time from first medical contact (FMC) to ECG (104 vs. 34 mins, p=0.0021).
The majority of total ischaemic time is due to patient delay, and this increases as age increases. Women had longer ischaemic time compared with men and longer wait from FMC until diagnostic ECG. This study suggests that improved awareness for patients and healthcare staff will be paramount in reducing ischaemic time.
May 2022 Br J Cardiol 2022;29:64–6 doi:10.5837/bjc.2022.018
Evaluation of the prognostic value of the admission ECG in COVID-19 patients: a meta-analysis
Mateusz Wawrzeńczyk, Marcin D Grabowski

The assessment of the prognostic value of the admission electrocardiography (ECG) (specifically of the duration of the PR and QTc intervals, the QRS complex and the heart rate [HR]) in COVID-19 patients on the basis of nine observational studies (n=1,424) indicates that relatively long duration of the QTc interval and QRS complex, as well as higher HR, are linked to a severe course of COVID-19, which may be of use in risk stratification. Since there are important differences in suggested indicators of adverse prognosis between observational studies, further research is necessary to clarify high-risk criteria.
May 2022 Br J Cardiol 2022;29:73–6 doi:10.5837/bjc.2022.019
The use of PYP scan for evaluation of ATTR cardiac amyloidosis at a tertiary medical centre
Joshua Dower, Danai Dima, Mumtu Lalla, Ayan R Patel, Raymond L Comenzo, Cindy Varga

Cardiac transthyretin amyloidosis (ATTR) is an often underdiagnosed disease that can lead to significant morbidity and mortality for patients. In recent years, technetium-99m pyrophosphate scintigraphy (PYP) imaging has become a standard of care diagnostic tool to help clinicians identify this disease. With newly emerging therapies for ATTR cardiomyopathy, it is critical to identify patients who are eligible for therapy as early as possible. At our institution, we sought to describe the frequency of PYP scanning and how it has impacted the management of a patient suspected to have amyloid cardiomyopathy.
Between 1 January 2017 and 31 December 2020, we identified 273 patients who completed PYP scanning for evaluation of cardiac amyloidosis at Tufts Medical Center, a tertiary care centre. We reviewed pertinent clinical data for all study subjects. A PYP scan was considered positive when the heart to contralateral lung ratio was greater than or equal to 1.5, with a visual grade of 2 or 3, and confirmation with single-photon emission computerised tomography (SPECT) imaging.
In total there were 55 positive, 202 negative, and 16 equivocal PYP scans. Endomyocardial biopsies were rarely performed following PYP results. Of the seven patients with a positive PYP scan who underwent biopsy, five were positive for ATTR amyloid; of the patients with a negative scan who were biopsied, none were positive for ATTR amyloidosis and two were positive for amyloid light-chain (AL) amyloidosis. The biomarkers troponin I, B-type naturietic peptide (BNP), and N-terminal pro-BNP (NT-proBNP), as well as the interventricular septal end-diastolic thickness (IVSd) seen on echocardiogram, were all found to be statistically higher in the PYP positive cohort than in the PYP negative cohort using Mann-Whitney U statistical analysis. In total, 27 out of the 55 patients with a positive PYP scan underwent therapy specific for cardiac amyloid.
In conclusion, this study reinforces the clinical significance of the PYP scan in the diagnosis and management of cardiac amyloidosis. A positive scan allowed physicians to implement early amyloid-directed treatment while a negative scan encouraged physicians to pursue an alternative diagnosis.
May 2022 Br J Cardiol 2022;29:79–80 doi:10.5837/bjc.2022.020
Angina pain associated with isolated R-IIP modified Lipton classification coronary artery anomaly
Nicholas Coffey, Alexis Smith, Rich Pham, Mohammed Kazimuddin, Aniruddha Singh

We report a case of a patient that presented with typical angina pain and associated risk factors for coronary artery disease (CAD). Subsequent cardiac catheterisation led to the discovery of an isolated R-IIP modified Lipton classification coronary artery anomaly with follow-up coronary computed tomography angiography (CCTA) confirmation. This case report includes images of the CCTA and left heart catheterisation results, along with a discussion of the potential for increased risk of atherosclerosis in our patient, and a proposed explanation of his presentation with prototypical angina pain, despite lack of apparent atherosclerosis.
April 2022 Br J Cardiol 2022;29:55–9 doi:10.5837/bjc.2022.011
Marijuana: cardiovascular effects and legal considerations. A clinical case-based review
Saad Ahmad, Shwe Win Hlaing, Muhammad Haris, Nadeem Attar

Though coronary artery disease primarily occurs in those over the age of 40 years, younger individuals who use recreational drugs may be afflicted with coronary events. Cannabis is one such perilous agent that can cause myocardial infarction (MI) and is one of the most common psychoactive drugs used worldwide. Cannabis (also known as marijuana, weed, pot, dope or grass) is the most widely used illegal drug in the UK. The desired euphoric effects are immediate, as are life-threatening hazardous ones.
In this article, we briefly describe a case series of two unique but similar cases of cannabis-induced ST-elevation MI witnessed at our hospital in quick succession. We will analyse the composite pathophysiology in acute coronary syndromes provoked by cannabis and discuss the evolving legality around the use of the drug.
April 2022 Br J Cardiol 2022;29:52–4 doi:10.5837/bjc.2022.012
Drive-by collection and self-fitting of ambulatory electrocardiogram monitoring
Mark T Mills, Sarah Ritzmann, Maisie Danson, Gillian E Payne, David R Warriner

Ambulatory electrocardiogram (AECG) monitoring is a common cardiovascular investigation. Traditionally, this requires a face-to-face appointment. In order to reduce contact during the COVID-19 pandemic, we investigated whether drive-by collection and self-fitting of the device by the patient represents an acceptable alternative.
A prospective, observational study of consecutive patients requiring AECG monitoring over a period of one month at three hospitals was performed. Half underwent standard (face-to-face) fitting, and half attended a drive-by service to collect their monitor, fitting their device at home. Outcome measures were quality of the recordings (determined as good, acceptable or poor), and patient satisfaction.
A total of 375 patients were included (192 face-to-face, 183 drive-by). Mean patient age was similar between the two groups. The quality of the AECG recordings was similar in both groups (52.6% good in face-to-face vs. 53.0% in drive-by; 34.9% acceptable in face-to-face vs. 32.2% in drive-by; 12.5% poor in face-to-face vs. 14.8% in drive-by; Chi-square statistic 0.55, p=0.76). Patient satisfaction rates were high, with all patients in both groups satisfied with the care they received.
In conclusion, drive-by collection and self-fitting of AECG monitoring yields similar AECG quality to conventional face-to-face fitting, with high levels of patient satisfaction.
April 2022 Br J Cardiol 2022;29:67–72 doi:10.5837/bjc.2022.013
Angina with coronary microvascular dysfunction and its physiological assessment: a review with cases
Pitt O Lim

Imagine that it is possible to know, the actual coronary blood flow. Would this not remove any doubt, if a chest pain is the heart’s fault?
April 2022 Br J Cardiol 2022;29:77–8 doi:10.5837/bjc.2022.014
Iatrogenic aortic dissection of the descending aorta after percutaneous coronary intervention
Kristen Westenfield, Shannon Mackey-Bojack, Yale L Wang, Kevin M Harris

Aortic dissection is a rare and potentially fatal complication of coronary angiography. We report a case of a woman in her late 80s who underwent a left femoral approach coronary angiogram for evaluation of a transcatheter aortic valve replacement (TAVR). Following the procedure, she had a cardiac arrest and was found to have a descending aortic dissection on transoesophageal echocardiogram. Autopsy showed an acute intimal tear of the descending aorta, most likely related to catheter manipulation. Patients undergoing evaluation for TAVR, who tend to be elderly with concomitant atherosclerosis, are at risk for complications following cardiac catheterisation including aortic dissection.
March 2022 Br J Cardiol 2022;29:21–5 doi:10.5837/bjc.2022.008
Atrial fibrillation prevalence and predictors in patients with diabetes: a cross-sectional screening study
Angela Hall, Andrew Robert John Mitchell, Lisa Ashmore, Carol Holland

Prevalence of atrial fibrillation (AF) and diabetes is increasing worldwide. Diabetes is a risk factor for AF and both increase stroke risk. Previous AF screening studies have recruited high-risk patient groups, but not with diabetes as the target group. This study aims to determine whether people with diabetes have a higher prevalence of AF than the general population and investigate whether determinants, such as diabetes duration or diabetes control, add to AF risk.
In a cross-sectional screening study, patients with diabetes were recruited via their GP surgeries or a diabetes centre. A 30-second single-lead electrocardiogram (ECG) was recorded using the Kardia® device, along with physiological measurements and details relating to risk factor variables.
There were 300 participants recruited and 16 patients identified with AF (5.3% prevalence). This demonstrated a significantly greater likelihood of AF than the background population (p=0.043). People with diabetes and AF were significantly older than those who only had diabetes. More people with type 2 diabetes had AF than people with type 1. Prediction of AF diagnosis by age, sex, diabetes type, diabetes duration and level of control revealed only age as a significant predictor.
In conclusion, these findings add to existing data around the association of these chronic conditions, supporting AF screening in this high-risk group, particularly in those of older age. This can contribute to appropriate management of both conditions in combination, not least with regards to stroke prevention.
March 2022 Br J Cardiol 2022;29:31–5 doi:10.5837/bjc.2022.009
Dermatological manifestations of cardiac conditions
Arnav Katira, Ravish Katira

Various cardiac disorders seen in general and acute medicine have dermatological manifestations that may provide critical clues to the underlying disease. This review will discuss the important dermatological signs seen in cardiac conditions. We believe greater interdisciplinary liaison will improve our understanding of the link between the dermatological and cardiovascular systems and the underlying disease processes.
January 2022 Br J Cardiol 2022;29:16–20 doi:10.5837/bjc.2022.003
Observational case series of postural tachycardia syndrome (PoTS) in post-COVID-19 patients
Nicholas P Gall, Stephen James, Lesley Kavi

There is emerging evidence that a proportion of patients who develop long (post)-COVID-19 have abnormalities in the regulation of their autonomic nervous system manifesting as postural tachycardia syndrome (PoTS). We report a series of 14 patients who developed symptoms and signs compatible with PoTS following clinically diagnosed COVID-19 infection. Their symptoms and clinical findings were consistent with those of patients with non-COVID-related PoTS. The authors recommend an active stand test for patients who present after COVID-19 infection with cardiovascular symptoms including chest pain, palpitations, light-headedness and breathlessness that are worse with the upright posture. They further recommend training of clinicians and investment in health services to provide for the anticipated significant increase in patients presenting with PoTS and other forms of autonomic dysfunction due to the COVID-19 pandemic.
January 2022 Br J Cardiol 2022;29:36–40 doi:10.5837/bjc.2022.004
Effect of the COVID-19 pandemic on ST-elevation myocardial infarction presentation and survival
Sachintha Perera, Sudhir Rathore, Joanne Shannon, Peter Clarkson, Matthew Faircloth, Vinod Achan

Presentation and outcomes of patients with ST-elevation myocardial infarction (STEMI) may change during viral pandemics. We compared symptom-to-call (STC), call-to-balloon (CTB), door-to-balloon (DTB) times; high-sensitivity troponin (hs-cTnI) levels; and survival of patients (n=39) during the first wave of the COVID-19 pandemic (defined as a ‘COVID period’ starting four weeks before lockdown) to historical controls from a ‘pre-COVID period’ (n=45).
STEMI admissions fell one week before lockdown by 29%. Median STC times began to rise one month before lockdown (54 vs. 25 min, p=0.06), with peak increases between 9 March and 5 April (166 vs. 59 min, p=0.04). Median CTB and DTB times were unchanged. Mean peak hs-cTnI increased during COVID-19 (15,225 vs. 8,852 ng/ml, p=0.004). Six-month survival following all STEMI reduced (82.1% vs. 95.6%, p<0.05).
STC times are the earliest indicator that STEMI-patient behaviour changed four weeks before lockdown, correlating with higher troponin levels and reduced survival. These early signals could guide public health interventions during future pandemics.
January 2022 Br J Cardiol 2022;29:9–11 doi:10.5837/bjc.2022.005
Heart failure care pathways: the power of collaboration and marginal gains
Carys Barton, Simon Gordon, Afsana Safa, Carla M Plymen

Heart failure (HF) is increasingly common and incurs a substantial cost, both in terms of quality and length of life, but also in terms of societal and economic impact. While significant gains are being made in the therapeutic management of HF, we continue to diagnose most patients when they are acutely unwell in hospital, often with advanced disease.
This article presents our experience in working collaboratively with primary care colleagues to redesign our HF pathway with the aim of facilitating earlier, community, diagnosis of HF. In so doing, and, thus, starting prognostic therapy much earlier in the course of the disease, we seek to avoid both the cost of emergency hospitalisation and the cost of poorer outcomes.
January 2022 Br J Cardiol 2022;29:26–30 doi:10.5837/bjc.2022.001
New agents for DOAC reversal: a practical management review
Katie White, Uzma Faruqi, Alexander (Ander) T Cohen

Bleeding is the commonest and most concerning adverse event associated with anticoagulants. Bleeding, depending on the severity, is managed in various ways, and for severe or life-threatening bleeding, specific antidotes are indicated and recommended. This review provides guidance relating to specific direct oral anticoagulant (DOAC) reversal agents, the antidotes. We discuss their indications for use, dosing, and potential side effects.
January 2022 Br J Cardiol 2022;29:12–15 doi:10.5837/bjc.2022.002
Foundational drugs for HFrEF: the growing evidence for a rapid sequencing strategy
Kieran F Docherty, John J V McMurray

In randomised, placebo- or active-controlled trials in patients with heart failure with reduced ejection fraction (HFrEF), each of the combination of a neprilysin inhibitor and an angiotensin-receptor blocker (i.e. sacubitril/valsartan), a beta blocker, a mineralocorticoid-receptor antagonist and a sodium-glucose co-transporter 2 (SGLT2) inhibitor have been shown to reduce morbidity and mortality, firmly establishing the role of these five agents, prescribed as four pills, as foundational therapy for HFrEF. Traditionally, the guideline-advocated strategy for the initiation of these therapies was based on the historical order in which the landmark clinical trials were performed, and the requirement to up-titrate each individual drug to the target dose (or maximally tolerated dose below this) prior to initiation of another therapy. This process could take six months or more to complete, during which time patients would not be taking one or more of these life-saving drugs. Recently an alternative, evidence-based, rapid three-step sequencing strategy has been proposed with the aim of establishing HFrEF patients on low-doses of all four foundational treatments within four weeks. This strategy is based on the premise that the benefits of each of these therapies are independent and additive to the others, the benefits are apparent at low doses early following initiation, and a specific ordering of therapies may increase likelihood of tolerance of others. This article will outline this novel rapid-sequencing strategy and provide an evidence-based framework to support its adoption into clinical practice.
November 2021 Br J Cardiol 2021;28:155–62 doi:10.5837/bjc.2021.051
Transcatheter mitral valve intervention
Rea Ganatra, Robert Smith

Mitral regurgitation is a common valvular heart disorder increasing with age. Many patients are ineligible for mitral valve surgery due to their age and other comorbidities. Left untreated, patients develop severe disease with a poor prognosis. The development of lower risk percutaneous mitral valve interventions has helped meet the needs of this previously untreated patient group. This review explores the recent and more established developments that have expanded the armamentarium for transcatheter mitral valve intervention.
November 2021 Br J Cardiol 2021;28:134–38 doi:10.5837/bjc.2021.048
Real-world evaluation of follow-up strategies after ICD therapies in patients with VT (REFINE-VT)
Patrick Tran, Leeann Marshall, Ian Patchett, Handi Salim, Shamil Yusuf, Sandeep Panikker, Michael Kuehl, Faizel Osman, Prithwish Banerjee, Harpal Randeva, Tarvinder Dhanjal

Implantable cardiac defibrillators (ICDs) can prevent sudden cardiac death, but the risk of recurrent ventricular arrhythmia (VA) and ICD shocks persist. Strategies to minimise such risks include medication optimisation, device programming and ventricular tachycardia (VT) ablation. Whether the choice of these interventions at follow-up are influenced by factors such as the type of arrhythmia or ICD therapy remains unclear. To investigate this, we evaluated ICD follow-up strategies in a real-world population with primary and secondary prevention ICDs.
REFINE-VT (Real-world Evaluation of Follow-up strategies after Implantable cardiac-defibrillator therapies in patients with Ventricular Tachycardia) is an observational study of 514 ICD recipients recruited between 2018 and 2019. We found that 77 patients (15%) suffered significant VA and/or ICD therapies, of whom 26% experienced a second event; 31% received no intervention. We observed an inconsistent approach to the choice of strategies across different types of arrhythmias and ICD therapies. Odds of intervening were significantly higher if ICD shock was detected compared with anti-tachycardia pacing (odds ratio [OR] 8.4, 95% confidence interval [CI] 1.7 to 39.6, p=0.007). Even in patients with two events, the rate of escalation of anti-arrhythmics or referral for VT ablation were as low as patients with single events.
This is the first contemporary study evaluating how strategies that reduce the risk of recurrent ICD events are executed in a real-world population. Significant inconsistencies in the choice of interventions exist, supporting the need for a multi-disciplinary approach to provide evidence-based care to this population.
November 2021 Br J Cardiol 2021;28:144–7 doi:10.5837/bjc.2021.049
Statin prescription and CV risk assessment in adult psychiatric outpatients with intellectual disability
Jamie Sin Ying Ho, George Collins, Vikram Rohra, Laura Korb, Bhathika Perera

We performed a single-centre study to assess the risk of cardiovascular disease (CVD) in psychiatry outpatients with intellectual disability (ID) using the QRISK-3 score.
There were 143 patients known to the ID psychiatry clinic enrolled. Of these, 28 (19.6%) had elevated CVD risk – defined as 10-year risk of heart attack or stroke of ≥10%. Of these, 57.1% were not prescribed statin therapy, which – after lifestyle measures – is recommended by National Institute for Health and Care Excellence (NICE) guidelines. The mean QRISK-3 score was 6.31% (95% confidence interval [CI] 4.84 to 7.78), with a relative risk of 3.50 (95%CI 2.34 to 4.67) compared with matched controls.
The high CVD risk identified in this study supports routine CVD risk assessment and management in adult outpatients with ID. Appropriate lifestyle measures and statin therapy could help reduce the excess CVD-related morbidity and mortality in ID patients.
November 2021 Br J Cardiol 2021;28:148–52 doi:10.5837/bjc.2021.050
Piloting structured focused TTE in outpatients during the COVID-19 pandemic: ‘old habits die hard’
Kay Dowling, Amanda Colling, Harriet Walters, Badrinathan Chandrasekaran, Helen Rimington

Transthoracic echocardiography presents a risk of COVID-19 transmission between an echocardiographer and the patient. Reducing the scanning time is likely to mitigate this risk for them both. British Society of Echocardiography (BSE) level 1 echocardiography offers a potential framework for focused scanning in an outpatient setting. There were 116 outpatients scheduled for a level 1 scan supplemented with additional pre-defined views, if required. Unexpectedly, a fifth of the scans were performed as an unintended full scan for a variety of reasons. Our results showed that focused scans were performed more quickly than full scans and below the NHS Test and Trace exposure cut-off of 15 minutes. However, if more than three sets of additional measurements were required then a full scan could be performed more quickly. Seniority of the echocardiographer and scan time had an inverse relationship. By examining the patients’ clinical records we were confident that all of the scans, whether focused or full, had answered the requestor’s clinical question. Although the COVID-19 vaccination programme should reduce the necessity of minimising exposure time during a scan there could still be a role for level 1 scanning during the COVID-19 recovery programme to tackle the vast lists of patients waiting for an echocardiogram.
October 2021 Br J Cardiol 2021;28:139–43 doi:10.5837/bjc.2021.042
Quality of life among people with atrial fibrillation with and without diabetes: a comparison study
Angela Hall, Andrew Robert John Mitchell, Lisa Ashmore, Carol Holland

Quality of life (QoL) is an essential consideration when managing the wellbeing of patients and assists in interpretation of symptoms, functional status and perceptions. Atrial fibrillation (AF) and diabetes demand significant healthcare resources. Existing data demonstrate a negative impact on QoL as individual conditions, but there is less evidence relating to the impact of these disease groups in combination. This study therefore explores QoL in patients with AF and diabetes.
This cross-sectional, observational study required participants to complete the short form (SF)-36 survey via an online platform and was offered to people affected by AF alone and people with AF and diabetes in combination. The SF-36 provides a prevalidated tool with eight domains relating to physical and psychological health.
A total of 306 surveys were completed (231 AF group, 75 AF and diabetes group). The mean and standard deviation (SD) were calculated for each QoL domain, after re-coding in accordance with SF-36 guidance. Multi-variate analysis of variance (MANOVA) demonstrated an overall significant difference between the groups when considered jointly across all domains. There were significant differences between AF and AF with diabetes QoL responses in physical functioning, energy fatigue, emotional wellbeing, social functioning and pain. In these domains, the mean was highest in the AF group. There were no significant differences in the role physical, role emotional and general health domains.
In conclusion, this study demonstrates that diabetes and AF has a more detrimental effect on QoL than AF alone, in the majority of domains. Further research into the general AF population and where chronic conditions co-exist is important to comprehend the true impact this disease combination has on QoL.
October 2021 Br J Cardiol 2021;28:128–133 doi:10.5837/bjc.2021.043
Pain during cardiac implantable electronic device implantation
David G Wilson, Nicki Brewster, Robin J Taylor, Amelia Trevelyan, Michail Apostolakis, Deepak Goyal, Will Foster, Elaine Walklet, Eleanor Bradley

In order to evaluate the extent and causes of pain during cardiac implantable electronic device (CIED) implantation in our hospital, a prospective audit over a 23-month period using a patient self-reporting questionnaire was undertaken.
In total, 599 procedures were reported, 52.9% for de novo pacemaker implantation and 23.4% for high-energy devices (cardiac resynchronisation therapy defibrillator [CRT-D], implantable cardiac defibrillator [ICD], subcutaneous ICD). Overall, the median pain score was 2/10 (interquartile range 2–4). In total, 61.6% (367/599) reported no pain or mild pain (pain scores 0–3/10), 27.7% (165/599) reported moderate pain (pain score of 4–6/10) and 10.7% (64/599) reported severe pain (pain score of 7–10/10) during the procedure. Significant pre-implant worry (odds ratio [OR] 2.13, 95% confidence interval [CI] 1.22 to 3.73) and higher lidocaine doses (OR 1.06, 95%CI 1.00 to 1.11) were associated with severe patient-reported pain.
In conclusion, most patients underwent CIED implantation with minimum stress and maximum comfort. An important minority reported severe pain during the procedure. Optimising surgical technique and interventions targeted at reducing pre- and peri-implant worry, particularly in women, and especially in those receiving ICDs, warrants further investigation to reduce patient-reported pain during CIED implantation.
October 2021 Br J Cardiol 2021;28:153–4 doi:10.5837/bjc.2021.044
Analysis of the trend in community prescribing of RAAS inhibitors during the COVID-19 pandemic
Layla Guscoth, Sam Hodgson

The coronavirus disease 2019 (COVID-19) pandemic has sparked novel research and insights, but also concerns and anxiety regarding established practices. Early into the pandemic, public and scientific concern was raised regarding the role of renin–angiotensin–aldosterone system (RAAS) inhibitors on the susceptibility to COVID-19 given their effect on angiotensin-converting enzyme 2 (ACE-2), the host receptor for the virus. This gathered media attention globally, despite several health boards encouraging the ongoing use of these medications. We aimed to investigate whether, despite advice supporting continued use of these medications, there was a change in prescribing practices for RAAS inhibitors in general practice. Data were collated from the NHS digital platform, which provides monthly practice-level prescribing information for all primary care practices in England. We performed an interrupted time-series analysis on national-level prescribing data comparing time-series coefficients pre- and post-March 2020 with metformin used as a control. We find that from March to December 2020, prescribing rates of RAAS inhibitors were reduced relative to the previous time-series trend. This finding persisted after adjustment for rates of metformin prescription. This suggests that there was a change in prescribing behaviour during the COVID-19 pandemic, which may be linked to the public and scientific concerns during this time.
October 2021 Br J Cardiol 2021;28:163–5 doi:10.5837/bjc.2021.046
Loperamide-induced ventricular tachycardia storm
Mohamed Daoub, Philippa Cawley, Jonathan Sahu

Loperamide is an over-the-counter, peripherally-acting, µ-opioid receptor agonist commonly used in the treatment of diarrhoea. It has increasingly been recognised as a potential drug of misuse, having previously been thought to have low potential for abuse owing to its low bioavailability and poor penetration of the central nervous system. High doses can result in life-threatening cardiac-toxicity.
We present a case of a young woman who had been self-treating her depression with high doses of loperamide for one year, who then presented to hospital with syncope secondary to ventricular tachycardia (VT). While in the emergency department (ED) the patient had monomorphic pulseless VT requiring electrical cardioversion multiple times. Transfer to a tertiary cardiac centre was immediately arranged after she was stabilised and intubated. This complicated the diagnostic process as a thorough history could not be obtained on arrival to the tertiary centre, which meant the loperamide misuse only came to light multiple days into admission, after the patient was extubated. The final diagnosis of loperamide-induced secondary long-QT syndrome was made and the patient made a full recovery.
September 2021 Br J Cardiol 2021;28:89–94 doi:10.5837/bjc.2021.037
Real-life outcomes and readmissions after a TAVI procedure in a Glasgow population
Joanna Osmanska, David Murdoch

Transcatheter aortic valve implantation (TAVI) is a routine procedure for patients with symptomatic severe aortic stenosis who are deemed inoperable or high-risk surgical candidates. The aim of this study was to examine real-world data on death and readmission rates in patients following the procedure.
Electronic health records for patients who underwent TAVI between April 2015 and November 2018 were reviewed. Details of the procedure, complications, length of initial hospital stay and outcomes of interest (subsequent admissions and mortality) were recorded.
In our cohort of 124 patients, the mean age was 80.8 years and 43% were male. Cardiac comorbidities were common, more than 30% had myocardial infarction (MI) and 15% had a previous coronary artery bypass graft (CABG). One in five suffered from chronic obstructive pulmonary disease (COPD), with similar prevalence of diabetes mellitus and cerebrovascular accident (CVA). In-hospital mortality was low at 3.3%, however, 30-day readmission rates were high at 14.6%; 44.4% were readmitted to hospital within one year.
TAVI is a successful procedure in Scotland with good outcome data. The potential benefit of the procedure in many patients is limited by comorbidities, which shorten life-expectancy and lead to hospital readmission. These data highlight the importance of effective multi-disciplinary discussion in a time of realistic medicine.
September 2021 Br J Cardiol 2021;28:98–101 doi:10.5837/bjc.2021.038
Outpatient parenteral antimicrobial therapy (OPAT) service is associated with inpatient-bed cost savings
Chun Shing Kwok, Joanna J Whittaker, Caroline Malbon, Barbara White, Jonathan Snape, Vikki Lloyd, Farah Yazdani, Timothy Kemp, Simon Duckett

In a cardiology department, there are some patients that require long-term antibiotics, such as those with infective endocarditis or infected prosthetic devices. We describe our experience with intravenous antibiotic therapy for patients with cardiology diagnoses who require a period of antibiotics in our outpatient service during the period of the COVID-19 pandemic. A total of 15 patients were selected to have outpatient antibiotic therapy (age range 36 to 97 years, 60% male). A total of nine patients had infective endocarditis, four patients had infected valve prosthesis or transcatheter aortic valve implantation (TAVI) endocarditis, one patient had infected pericardial effusion while another had infected pericarditis. For these 15 patients there was a total of 333 hospital bed-days, on average 22 days per patient. These patients also had a total of 312 days of outpatient antibiotic therapy, which was an average of 21 days per patient. The total cost, if patients were admitted for those days, assuming a night cost £400, was £124,800, which was on average £8,320 per patient. Three patients were readmitted within 30 days. One had ongoing endocarditis that was managed medically and another had pulmonary embolism. The last patient had a side effect related to daptomycin use. In conclusion, outpatient antibiotic therapy in selected patients with native or prosthetic infective endocarditis appears to be safe for a selected group of patients with associated cost savings.
September 2021 Br J Cardiol 2021;28:109–11 doi:10.5837/bjc.2021.039
Heparin-free distal radial artery approach to cardiac catheterisation and the small radial recurrent artery
Pitt O Lim, Ziyad Elghamry

Radial artery access has transformed cardiac catheterisation, allowing it to be performed in a daycase setting, saving both hospital beds, and nursing care costs. However, there are two common and seemingly diametrically opposite complications. These are radial artery occlusion and forearm haematoma; the former could be reduced by heparin, but at the expense of precipitating the latter. These complications increase proportionally to the size of radial artery sheath used. Interestingly, by cannulating the radial artery more distally beyond its bifurcation in the hand, the distal radial approach appears to be the ‘one stone, two birds’ or the synchronous Chinese idiom, ‘yīshí’èrniǎo’s’ solution, reducing both complications at the same time. Extending this further and downsizing to a 4Fr catheter system, heparin use could be spared altogether, without complications, and haemostasis achieved with short manual pressure at the puncture site. Hence, further cost savings by foregoing commercial compression bands, and abolishing access site care for nurses. We illustrate the above strategy in a patient with challenging radial anatomy, made simple and easy.
September 2021 Br J Cardiol 2021;28:117–8 doi:10.5837/bjc.2021.040
Severe orthostatic hypotension and weight loss associated with cancer therapy
Peter Sever

Two cases of orthostatic hypotension associated with weight loss following cancer treatment are described. Conventional treatments for orthostatic hypotension proved ineffective. A hypothesis of association with skeletal muscle wasting is discussed.
September 2021 Br J Cardiol 2021;28:166–8 doi:10.5837/bjc.2021.041
Post-stenting angiographically silent coronary dissection: OCT comes to the rescue
Roopali Khanna, Anindya Ghosh, Ankit Kumar Sahu, Pravin K Goel

Stent edge dissection is one of the procedural complications concerning percutaneous coronary intervention (PCI). We present a clinical case of multi-vessel PCI where the patient had to return with recurring symptoms within two weeks of a seemingly successful PCI, only to teach us a valuable lesson in the more frequent and judicious use of intracoronary imaging.
July 2021 Br J Cardiol 2021;28:102–4 doi:10.5837/bjc.2021.031
The ePortfolio in UK cardiology training: time for a new digital platform?
Ahmed Elamin, Mohammed Obeidat, Gershan Davis

The UK cardiology specialist training programme utilises the National Health Service (NHS) e-Portfolio to ensure adequate progression is being made during a trainees’ career. The NHS e-portfolio has been used for 15 years, but many questions remain regarding its perceived learning value and usefulness for trainees and trainers. This qualitative study in the recent pre-COVID era explored the perceived benefits of the NHS e-Portfolio with cardiology trainees and trainers in two UK training deaneries. Questionnaires were sent to 66 trainees and to 50 trainers. 50% of trainees felt that their development had benefited from use of the ePortfolio. 61% of trainees found it an effective educational tool, and 25% of trainees and 39% of trainers found the ePortfolio useful for highlighting their strengths and weaknesses. 75% of trainees viewed workplace based assessments as a means to passing the ARCP. The results show that the NHS ePortfolio and workplace based assessments were perceived negatively by some trainees and trainers alike, with many feeling that significant improvements need to be made. In light of the progress and acceptance of digital technology and communication in the current COVID-19 era, it is likely to be the time for the development of a new optimal digital training platform for cardiology trainees and trainers. The specialist societies could help develop a more speciality specific learning and development tool.
July 2021 Br J Cardiol 2021;28:105–8 doi:10.5837/bjc.2021.032
Real-world experience of selexipag titration in pulmonary arterial hypertension
Sarah Cullivan, Anandan Natarajan, Niamh Boyle, Ciara McCormack, Sean Gaine, Brian McCullagh

Selexipag is an oral selective prostacyclin-receptor agonist that was approved for use in patients with World Health Organisation (WHO) functional class II–III pulmonary arterial hypertension (PAH). Treatment with individualised doses of selexipag resulted in significant reductions in the composite end point of death or a complication related to PAH in the phase III GRIPHON (Prostacyclin [PGI2] Receptor Agonist In Pulmonary Arterial Hypertension) study. In order to better understand the real-world approach to selexipag titration and to establish the individualised maintenance regimens used in our centre, we performed this retrospective study of the first 20 patients prescribed selexipag. Baseline characteristics differed from the GRIPHON study, with more combination therapy and comorbidities at drug initiation. Maintenance doses were stratified as low-dose in 10% (n=2), medium-dose in 70% (n=14) and high-dose in 20% (n=4). This study highlights that selexipag can be safely initiated, titrated and transitioned in an outpatient setting to achieve an individualised dosing regimen.
July 2021 Br J Cardiol 2021;28:115–6 doi:10.5837/bjc.2021.033
Acute Takotsubo cardiomyopathy as a complication of transoesophageal echocardiogram
Fraser J Graham, Shona M M Jenkins

A 52-year-old woman, referred for transoesophageal echocardiography, developed acute Takotsubo cardiomyopathy during the examination as a result of emotional distress beforehand. Asymptomatic left ventricular apical ballooning with severe systolic dysfunction within minutes of the emotional trigger was the first sign of any abnormality.
July 2021 Br J Cardiol 2021;28:119–20 doi:10.5837/bjc.2021.034
A broad complex tachycardia in a patient on flecainide
Debjit Chatterjee

This is an interesting case of wide complex tachycardia in a patient on flecainide for paroxysmal atrial fibrillation. Diagnostic possibilities were discussed, actual diagnosis revealed, and explanation provided.
June 2021 Br J Cardiol 2021;28:55 doi:10.5837/bjc.2021.024
ECG changes in hospitalised patients with COVID-19 infection
Mengshi Yuan, Zafraan Zathar, Frantisek Nihaj, Stavros Apostolakis, Fairoz Abdul, Derek Connolly, Chetan Varma, Vinoda Sharma

The coronavirus disease 2019 (COVID-19) commonly involves the respiratory system but increasingly cardiovascular involvement is recognised. We assessed electrocardiogram (ECG) abnormalities in patients with COVID-19.
We performed retrospective analysis of the hospital’s COVID-19 database from April to May 2020. Any ECG abnormality was defined as: 1) new sinus bradycardia; 2) new/worsening bundle-branch block; 3) new/worsening heart block; 4) new ventricular or atrial bigeminy/trigeminy; 5) new-onset atrial fibrillation (AF)/atrial flutter or ventricular tachycardia (VT); and 6) new-onset ischaemic changes. Patients with and without any ECG change were compared.
There were 455 patients included of whom 59 patients (12.8%) met criteria for any ECG abnormality. Patients were older (any ECG abnormality 77.8 ± 12 years vs. no ECG abnormality 67.4 ± 18.2 years, p<0.001) and more likely to die in-hospital (any ECG abnormality 44.1% vs. no ECG abnormality 27.8%, p=0.011). Cox-proportional hazard analysis demonstrated any ECG abnormality (hazard ratio [HR] 1.97, 95% confidence interval [CI] 1.12 to 3.47, p=0.019), age (HR 1.03, 95%CI 1.01 to 1.05, p=0.0009), raised high sensitivity troponin I (HR 2.22, 95%CI 1.27 to 3.90, p=0.006) and low estimated glomerular filtration rate (eGFR) (HR 1.73, 95%CI 1.04 to 2.88, p=0.036) were independent predictors of in-hospital mortality.
In conclusion, any new ECG abnormality is a significant predictor of in-hospital mortality.
June 2021 Br J Cardiol 2021;28:67–9 doi:10.5837/bjc.2021.026
Reducing antithrombotic-related bleeding risk in urgent and emergency cardiac surgery
Amer Harky, Abdul Badran

This review focuses on the role of CytoSorb® (CytoSorbents Corporation, Monmouth Junction, New Jersey, USA), a technology for purifying extracorporeal blood. The technology is designed for several indications to prevent bleeding complications during on-pump cardiac surgery, including removal of the antiplatelet agent, ticagrelor, and the oral anticoagulant, rivaroxaban, from the blood. Recent clinical studies are briefly reviewed.
June 2021 Br J Cardiol 2021;28:73–6 doi:10.5837/bjc.2021.027
The effect of a standardised protocol for CIED insertion on complications and infection rates in a DGH
Eliza Foster, Guy Furniss, Mark Dayer

Cardiac implantable electronic device (CIED)-related complications and infections typically lead to prolonged hospital stays and, very occasionally, death. A new CIED insertion protocol was implemented in a district general hospital. The primary objective of this study was to determine whether a significant reduction in complication and infection rates occurred after implementation of the new protocol. Medical records were reviewed for patients who had a CIED inserted in the two years pre- and post-protocol implementation, and any complications were identified in a one-year follow-up period.
An increase in the complexity of the devices implanted after introduction of the protocol was observed. The number of complications was significantly reduced from 6.86% to 3.95% (p<0.0001). In the two years prior to protocol implementation, 14 of 871 (1.6%) patients suffered a CIED-related infection. In contrast, four of 683 (0.44%) patients suffered a CIED-related infection in the two years post-implementation. This was not statistically significant (p=0.093).
In conclusion, implementing a standardised protocol for CIED insertion significantly reduced the rate of complications, and also reduced the rate of infection, but this was not statistically significant.
June 2021 Br J Cardiol 2021;28:112–4 doi:10.5837/bjc.2021.029
Liver function monitoring in Fontan-procedure patients: audit of current practice across South Wales
Elliott J Carande, Gergely Szantho

The Fontan procedure provides a palliative surgical repair for complex congenital heart disease, but it is associated with many long-term problems, including liver cirrhosis, and hepatocellular carcinoma. The current suggestion from international guidance is that end-organ surveillance should be carried out, with a particular focus on regular blood tests and imaging for liver function.
In this study, retrospective analysis was performed on adult patients who had previously had a Fontan operation performed to determine the regularity of end-organ surveillance in regards to their liver function covering the three calendar years from 2016 to 2018, and the first six months of 2019.
Eighty-six patients were identified in South Wales monitored by the adult congenital heart disease unit. We found that the number of investigations performed in the first six months of 2019 was comparable to other calendar years in their entirety. Liver function tests had been performed in 57% of patients throughout 2018, with only 8% having had an alpha-fetoprotein taken, and only 9% having had imaging of the liver performed. Over the course of their lifetime, 97% of patients had had a liver function blood test performed at some point, with 17% having had an alpha-fetoprotein taken, and 49% having their liver imaged.
In conclusion, end-organ surveillance is an important follow-up for patients with a Fontan circulation, with guidelines proposing yearly blood test and imaging investigations. This study shows the opportunities to improve surveillance in this group of patients to highlight the development of liver cirrhosis, and/or hepatocellular carcinoma.
June 2021 Br J Cardiol 2021;28:95–7 doi:10.5837/bjc.2021.030
Can too much exercise be dangerous: what can we learn from the athlete’s heart?
Fang Qin Goh

Exercise prevents and aids treatment of coronary heart disease, hypertension, heart failure, diabetes mellitus, obesity and depression, reduces cardiac events and improves survival. However, evidence suggests that the relationship between exercise and mortality may be curvilinear, with modest additional benefit at higher levels. Intensive exercise has also been associated with increased atrial fibrillation risk, although its clinical implications are not well understood. Other proposed adverse effects of exercise on the heart, including reduced right ventricular function, elevated cardiac biomarkers, myocardial fibrosis and coronary artery calcification, are less substantiated. Current evidence cannot affirm that extreme exercise is dangerous and future studies should combine large cohorts to obtain a statistically reliable limit. Associations between features of the athlete’s heart and cardiovascular morbidity and mortality should also be explored.
April 2021 Br J Cardiol 2021;28:62–6 doi:10.5837/bjc.2021.017
Management of hyperlipidaemia following acute coronary syndrome: a retrospective audit
Handi Yuwono Salim, Kaung Lwin, Chee Khoo, David Wilson

Control of hypercholesterolaemia is an effective way of reducing cardiovascular events in patients at elevated risk of cardiovascular disease. Repeat cholesterol measurement is a good practice, but is rarely performed, with clinicians often adopting a ‘fire and forget’ policy.
A retrospective audit at two cardiac centres in the West Midlands was performed to evaluate performance in lipid measurement following initiation of lipid therapy, and to evaluate whether all patients with an indication for a proprotein convertase subtisilin/kexin 9 inhibitor (PCSK9i) following acute coronary syndrome (ACS) were identified according to National Institute for Health and Care Excellence (NICE) recommendations.
We identified 167/7,048 patients with a total cholesterol of ≥7.2 mmol/L, of which 33 patients had previous vascular disease affecting more than one territory (polyvascular disease). Total cholesterol threshold ≥7.2 mmol/L was chosen in order to achieve a sufficient number of samples for the audit to be completed successfully. Low-density lipoprotein (LDL) level was performed in 93 patients on admission and repeated within three months in 20 patients (13%). Overall, 48 patients (30%) had any repeat LDL recorded. Of this group, 10 patients met the NICE criteria for PCSK9i.
Failure to repeat LDL levels in patients following hospital discharge with a diagnosis of ACS, is likely to explain the small number of patients identified as being eligible for PCSK9i. Underreporting of comorbid vascular disease also prevents the identification of patients at very high risk. We advocate re-establishing the practice of routine repeat fasting lipids measurement following discharge from hospital in order to correctly identify patients who may be eligible for optimal lipid-lowering therapy.
April 2021 Br J Cardiol 2021;28:56–61 doi:10.5837/bjc.2021.018
Eligibility for dapagliflozin in unselected patients hospitalised with decompensated heart failure
Hibba Kurdi, Parin Shah, Simon Barker, Daniel Harris, Benjamin Dicken, Carey Edwards, Geraint Jenkins

Patients with heart failure with reduced ejection fraction (HFrEF) who received the sodium-glucose co-transport 2 inhibitor, dapagliflozin, in the DAPA-HF (Dapagliflozin and Prevention of Adverse Outcomes in Heart Failure) study have a significant reduction in worsening heart failure (HF) and cardiovascular death. It is uncertain what proportion of patients admitted to a large regional cardiac centre with decompensated heart failure would be eligible for dapagliflozin post-discharge based on their characteristics at discharge.
The DAPA-HF study criteria were retrospectively applied to a cohort of 521 consecutive patients referred to the inpatient HF service in a tertiary cardiac centre in South West Wales between April 2017 and April 2018. Inclusion criteria: left ventricular ejection fraction (LVEF) <40%, New York Heart Association (NYHA) class II–IV symptoms and an elevated N-terminal pro-B-type naturietic peptide (NT-proBNP). Exclusion criteria: systolic blood pressure (SBP) <95 mmHg, estimated glomerular filtration rate (eGFR) <30 ml/min/1.73 m2 or type 1 diabetes mellitus. We did not have complete NT-proBNP data for the cohort, as it was not routinely measured at the time in our institute.
There were 478 patients, mean age 78 ± 13 years, 57% male and 91% NYHA class II–IV symptoms, were included in the analysis. Of these, 247 patients had HFrEF, 219 (46%) patients met the inclusion criteria, 231 (48%) were excluded as LVEF was >40%, and 48 (10%) were excluded with NYHA class I symptoms. Of the 219 patients who met the inclusion criteria, 13 (5.9%) had a SBP <95 mmHg, 48 (22%) had eGFR <30 ml/min/1.73 m2, leaving 136 (28.5% of total and 55% of those with HFrEF) who met DAPA-HF study criteria.
In our study, 28.5% of all heart failure admissions and 55% of patients with HFrEF would be eligible for dapagliflozin post-discharge according to the DAPA–HF study entry criteria.
April 2021 Br J Cardiol 2021;28:77–8 doi:10.5837/bjc.2021.019
When Blades broke my heart
Nadir Elamin, Izhar Hashmi, Martin Tilney, Ever Grech

Takotsubo cardiomyopathy (TCM) was first described about 30 years ago. It has been attributed to the sudden catecholamine surge in relation to severe stress, which can cause multi-vessel coronary spasms and myocardial apical ballooning. Football supporters are prone to develop severe stress due to sudden changes in match results. This case presents a football supporter of Sheffield United (the Blades) who was admitted to the hospital with cardiac sounding chest pain following a last minute goal by the opposing team. The necessary investigations were carried out including coronary angiogram and echocardiogram. He was diagnosed with TCM following a left ventricular angiogram demonstrating the typical appearance of the octopus pot.
April 2021 Br J Cardiol 2021;28:70–2 doi:10.5837/bjc.2021.020
Minimising permanent pacemaker implantation (PPI) after TAVI
Philip MacCarthy, Azfar Zaman, Neal Uren, James Cockburn, Stephen Dorman, Iqbal Malik, Douglas Muir, Muhiddin (Mick) Ozkor, David Smith, Sarah Shield

Increased demand for transcatheter aortic valve implantation (TAVI) procedures for patients with severe aortic stenosis has not been matched with a proportional increase in available resources in recent years. This article highlights the importance of developing integrated care pathways for TAVI, which incorporate standardised protocols for permanent pacemaker implantation (PPI) to ensure best practice, increase service efficiency and reduce rates of PPI post-TAVI.
April 2021 Br J Cardiol 2021;28:54 doi:10.5837/bjc.2021.021
The primary prevention implantable cardioverter-defibrillator (ICD) during the COVID-19 pandemic
Christopher J Cassidy, Khalid Abozguia, Michael J Brack, Angelic Goode, Grahame K Goode, Alison Seed

During the recent ‘first wave’ of the COVID-19 pandemic, the National Health Service (NHS) has triaged planned services to create surge capacity. The primary prevention implantable cardioverter-defibrillator (ICD) was in a grey area of triage guidance, but it was suggested as a procedure that could be reasonably stopped. Recent reports have highlighted deaths of patients awaiting ICDs who may have been deferred during the pandemic. In our trust we reorganised our device service and continued to implant primary prevention ICDs during the ‘first wave’ and, here, report that most patients wished to proceed and underwent uncomplicated implantations. One patient later died from COVID-19, although the transmission site cannot be definitively concluded. With strict adherence to public health guidance and infection prevention strategies, we believe that ICD implantation can be performed safely during the pandemic, and this should be standard practice during subsequent surges.
April 2021 Br J Cardiol 2021;28:79–80 doi:10.5837/bjc.2021.023
TAVR for severe aortic stenosis and papillary fibroelastoma in a high-risk setting
Ishtiaq Rahman, Ammar Alibrahim, Mohammad Zahrani, Joji Ito, Kim Connelly, Chris Buller, Mark Peterson, David Latter

Papillary fibroelastomas (PFE) are rare benign cardiac tumours mainly originating on aortic and mitral valvular surfaces. Management is individualised, but most recommend surgical excision due to thromboembolic risk. We report a 75-year-old man with symptomatic severe aortic stenosis compounded by PFE. Redo sternotomy aortic valve replacement was deferred in favour of the trans-apical (TAVR) approach. This report highlights, for the first time, the application of TAVR as a strategy for aortic valve stenosis and PFE to mitigate risk posed by injury to patent internal mammary arterial graft in close proximity to the manubrium, and complications due to the patient’s multiple comorbidities.

April 2021 doi:10.5837/bjc.2021.015
Amyloid heart disease module 1: diagnosis
Joseph M Krepp, Richard Katz, Rachel Volke, Angela Ryan, Gurusher Panjrath

![]() This article is available as a 'Standalone BJC Learning module' CPD activity
This article is available as a 'Standalone BJC Learning module' CPD activity
Background
Cardiac amyloidosis (CA) is a disorder of protein misfolding with resultant accumulation within the myocardium ultimately leading to clinical heart failure. It is subcategorised, according to the type of misfolded protein, into primary light-chain amyloidosis (AL) and transthyretin amyloidosis (ATTR). AL-CA is the result of cardiac infiltration of misfolded light-chain proteins; whereas ATTR-CA is caused by cardiac deposition of the misfolded thyroid hormone transport protein, transthyretin. ATTR-CA can be further subcategorised into hereditary (hATTR) versus wild-type (wtATTR).1,2 Although the exact prevalence of ATTR-CA is unknown, it has become increasingly accepted as a common cause of heart failure, particularly in the elderly. Despite this knowledge, ATTR-CA remains a widely underdiagnosed cause of heart failure, and there are frequently delays to achieving the accurate diagnosis. Prompt recognition and early diagnosis of ATTR-CA is critical to decreasing morbidity and mortality, particularly as disease-modifying therapies emerge in the treatment of ATTR-CA. We present a case of ATTR-CA that remained undiagnosed until later disease stages and we will subsequently review the diagnostic evaluation of patients with suspected ATTR-CA.

April 2021 doi:10.5837/bjc.2021.016
Amyloid heart disease module 2: management
Tamer Rezk, Julian D Gillmore

![]() This article is available as a 'Standalone BJC Learning module' CPD activity
This article is available as a 'Standalone BJC Learning module' CPD activity
Transthyretin amyloidosis (ATTR) is a progressive, fatal disease in which deposition of amyloid derived from either mutant or wild-type transthyretin (wtATTR) causes progressive and severe organ dysfunction. The two key clinical phenotypes are transthyretin amyloid cardiomyopathy (ATTR-CM) or transthyretin amyloid polyneuropathy (ATTR-PN), which both carry significant morbidity and mortality. Hereditary ATTR amyloidosis frequently presents with a mixed phenotype (ATTR-mixed).
ATTR-CM is an infiltrative, restrictive cardiomyopathy characterised by congestive cardiac failure, often with preserved left ventricular ejection fraction, and significant risk of conduction disease.
Treatment focuses on supportive care, reduction and ideally elimination of transthyretin (TTR) from the plasma, stabilisation of the tetramic structure of TTR and dissolution of the existing ATTR amyloid matrix.
Liver transplantation, to remove variant TTR production remains a treatment option for a select cohort of patients with hereditary ATTR-PN, although it is likely to be replaced by novel RNA-targeting therapies aimed at reducing TTR production. TTR stabilisers, such as tafamidis and acoramidis, may offer disease-modifying therapy to the majority of elderly patients with wild-type ATTR-CM. The rapidly evolving landscape of treatment options for ATTR amyloidosis, particularly among older patients with wtATTR, validates improved efforts to diagnose ATTR-CM.

April 2021 doi:10.5837/bjc.2021.014
Novel potassium binders: a clinical update
Hon-Ting Wai, Nirmol Meah, Ravish Katira

Introduction
Hyperkalaemia (HK) in heart failure and chronic kidney disease patients limits the use of renin–angiotension–aldosterone system (RAAS) inhibitors, and successful intervention may allow patients to remain on optimal RAAS therapy. The management of HK is an established practice, but the increasing popularity of novel potassium binders may represent an effective and better-tolerated alternative compared with conventional therapy, such as sodium polystyrene sulfonate.1
This article reviews the efficacy, and safety profile of patiromer and sodium zirconium cyclosilicate (SZC), and summarises the National Institute for Health and Care Excellence (NICE) guidance for both agents.2,3
March 2021 Br J Cardiol 2021;28:7–10 doi:10.5837/bjc.2021.007
COVID-19: treatments and the potential for cardiotoxicity
Sarah Maria Birkhoelzer, Elena Cowan, Kaushik Guha

A wide range of medications including antimalarial preparations (chloroquine, hydroxychloroquine), macrolide antibiotics (azithromycin) and the interleukin-6 inhibitor (tocilizumab) may be effective in treating patients with coronavirus disease 2019 (COVID-19). Such agents may be associated with cardiotoxicity, and the purpose of this brief review is to draw attention to potential areas of pharmacovigilance. These include prolongation of the QT-interval and the development of occult cardiomyopathy. Alternatively, some of the agents seem to have minimal impact on the cardiovascular system. The review highlights the need for an ongoing evaluation of such agents within carefully constructed clinical trials with embedded attention to cardiovascular safety.
The reason to be cautious when evaluating curative or symptomatic treatments is the fact that SARS-CoV-2 has affected large segments of the population, with disproportionate mortality rates within certain subgroups. Some of the enhanced mortality may reflect inherent cardiovascular disease risk factors related to acute COVID-19 infection.
It is hoped that the review will stimulate a greater awareness of potential cardiovascular side effects and encourage reporting of those in future trials.
March 2021 Br J Cardiol 2021;28:19–21 doi:10.5837/bjc.2021.009
Driving after cardiac intervention: are we doing enough?
Inderjeet Bharaj, Jaskaran Sethi, Sohaib Bukhari, Harmandeep Singh

Around 7.4 million people in the UK have heart and cardiovascular disease, coronary artery disease (CAD) being the most common type. The Driving and Vehicle Licensing Agency (DVLA) has guidance for medical professionals to aid assessment of cardiac patients with respect to driving. The guidance is different for personal, Public Carriage Office (PCO) and goods vehicles. It remains the doctors’ responsibility to advise patients of any driving restrictions, as certain cardiac conditions can limit patients’ ability to drive. This gains importance especially after certain procedures. A retrospective review of discharge summaries from electronic medical records was undertaken for a period of three months to review the number of patients getting appropriate advice. It was noted that frequently no written driving advice was recorded on discharge, neglecting an important element of patient safety. Steps were taken to counteract the lack of proper driving advice and documentation, which were effective on second review. Therefore, measures similar to ones outlined here should be put in place to ensure safe discharge and knowledge of the clinicians in accordance with the DVLA guidance.
March 2021 Br J Cardiol 2021;28:14–18 doi:10.5837/bjc.2021.010
Study of patients with iron deficiency and HF in Ireland: prevalence and treatment budget impact
Bethany Wong, Sandra Redmond, Ciara Blaine, Carol-Ann Nugent, Lavanya Saiva, John Buckley, Jim O’Neill

This study aims to present the screening, prevalence and treatment of heart failure (HF) patients with iron deficiency in an Irish hospital and use an economic model to estimate the budget impact of treating eligible patients with intravenous ferric carboxymaltose (IV FCM).
Retrospective data were collected on 151 HF patients over a one-year period from all newly referred HF patients to a secondary care hospital. This included 36 patients with preserved ejection fraction (HFpEF) and 115 with reduced ejection fraction (HPrEF). An existing budget impact model was adapted to incorporate Irish unit cost and resource use data to estimate the annual budget impact of treating patients with IV FCM.
The total number of HFrEF patients who met criteria for iron replacement was 44 (38% of total HFrEF patients); of this, only nine (20%) were treated. The budget impact model estimates that treating all eligible patients with IV FCM in this single centre would save 40 bed-days and over €7,600/year.
To improve the quality of life and reduce hospitalisation, further identification and treatment of iron deficient patients should be implemented. Expanding the use of IV iron nationally would be cost and bed saving.
March 2021 Br J Cardiol 2021;28:30–4 doi:10.5837/bjc.2021.011
Takotsubo syndrome: the broken-heart syndrome
Rienzi Díaz-Navarro

Takotsubo syndrome – also known as broken-heart syndrome, Takotsubo cardiomyopathy, and stress-induced cardiomyopathy – is a recently discovered acute cardiac disease first described in Japan in 1991. This review aims to update understanding on the epidemiology, pathophysiology, clinical presentation, diagnosis, and treatment of Takotsubo syndrome, highlighting aspects of interest to cardiologists and general practitioners.
March 2021 Br J Cardiol 2021;28:37–8 doi:10.5837/bjc.2021.012
Takotsubo syndrome: a predominantly female CV disorder, from the perspective of primary care
Melissa Matthews, Terry McCormack

We describe two cases of Takotsubo syndrome and discuss the issues relating to diagnosis and patient communication that they raise.
March 2021 Br J Cardiol 2021;28:29–32 doi:10.5837/bjc.2021.013
ECG changes during ISWTs in adult patients commencing CR: a retrospective case note review
Alexandra Palma, Charlotte Pereira, Heather Probert, Harriet Shannon

The incremental shuttle walk test (ISWT) is a valid, reliable submaximal exercise test used in the assessment of patients prior to cardiac rehabilitation (CR). Simultaneous electrocardiogram (ECG) measurements would provide important information on the safety of the test, and adequacy of subsequent cardiac risk stratification. Risk stratification is recommended to assess patients’ suitability for cardiac rehabilitation. For example, ST-segment depression >2 mm from baseline during testing would place a person in a high-risk category. However, such ECG measurements are rarely undertaken in clinical practice. The aim of the study was to investigate the incidence of ECG changes during an ISWT, and report on the possible impact of these findings on subsequent cardiac risk stratification.
A retrospective case note review was undertaken for the year 2017. Baseline clinical characteristics from eligible patients were gathered including those with ischaemic heart disease, heart failure, transplant and valve replacement, along with ECG measurements during the ISWT. The impact of ECG findings on cardiac risk stratification was calculated, based on risk stratification developed by the American Association of Cardiovascular and Pulmonary Rehabilitation. The safety of the ISWT was measured by the absence of major ECG changes.
Data were gathered for 295 patients. Minor ECG changes were identified during the ISWT in 189 patients (64.1%), with no major changes. The presence of silent myocardial ischaemia (ST-segment depression) had an impact on cardiac risk stratification in 27 patients. There was a statistically significant positive association between ST-segment depression with cardiac risk stratification (p<0.001).
In conclusion, the ISWT is safe in terms of ECG changes. The impact of ECG findings on cardiac risk stratification is significant and worthy of further consideration.
January 2021 Br J Cardiol 2021;28:22–5 doi:10.5837/bjc.2021.001
The impact of COVID-19 on cardiology training
Samuel Conway, Ali Kirresh, Alex Stevenson, Mahmood Ahmad

The coronavirus disease 2019 (COVID-19) pandemic has produced a dramatic shift in how we practise medicine, with changes in working patterns, clinical commitments and training. Cardiology trainees in the UK have experienced a significant loss in training opportunities due to the loss of specialist outpatient clinics and reduction in procedural work, with those on subspecialty fellowships perhaps losing out the most. Training days, courses and conferences have also been cancelled or postponed. Many trainees have been redeployed during the crisis, and routes of career progression have been greatly affected, prompting concerns about extensions in training time, along with effects on mental health.
With the pandemic ongoing and its effects on training likely long-lasting, we examine areas for improvement and opportunities for change in preparation for the ‘new normal’, including how other specialties have adapted. The increasingly routine use of video conferencing and online education has been a rare positive of the pandemic, and simulation will play a larger role. A more coordinated, national approach will need to be introduced to ensure curriculum components are covered and trainees around the country have equal access to ensure cardiology training in the UK remains world class.
January 2021 Br J Cardiol 2021;28:35–6 doi:10.5837/bjc.2021.002
Lockdown cardiomyopathy: from a COVID-19 pandemic to a loneliness pandemic
Baskar Sekar, Hibba Kurdi, David Smith

Social distancing/isolation is vital for infection control but can adversely impact on mental health. As the spread of COVID-19 is contained, mental health issues will surface with particular concerns for elderly, isolated populations. We present a case of Takotsubo cardiomyopathy related to lockdown anxiety.
January 2021 Br J Cardiol 2021;28:39 doi:10.5837/bjc.2021.003
Pneumopericardium in a patient with trisomy 21 and COVID-19 following emergency pericardiocentesis
Apurva H Bharucha, Ritesh Kanyal, James W Aylward, Parthipan Sivakumar, Ian Webb

We describe a case of pneumopericardium following emergency pericardiocentesis in a patient with coronavirus disease 2019 (COVID-19).
January 2021 Br J Cardiol 2021;28:11–3 doi:10.5837/bjc.2021.005
Evaluating the use of a mobile device for detection of atrial fibrillation in primary care
Patrick J Highton, Amit Mistri, Andre Ng, Karen Glover, Kamlesh Khunti, Samuel Seidu

Atrial fibrillation (AF) increases cardio-embolic stroke risk, yet AF diagnosis and subsequent prophylactic anticoagulant prescription rates are suboptimal globally. This project aimed to increase AF diagnosis and subsequent anticoagulation prescription rates in East Midlands Clinical Commissioning Groups (CCGs).
This service improvement evaluation of the East Midlands AF Advance programme investigated the implementation of mobile AF detection devices (Kardia, AliveCor) into primary-care practices within East Midlands CCGs, along with audit tools and clinician upskilling workshops designed to increase AF diagnosis and anticoagulation prescription rates. AF prevalence and prescription data were collected quarterly from July to September (Q3) 2017/18 to April to June/July to September (Q2/3) 2018/19.
AF prevalence increased from 1.9% (22,975 diagnoses) in Q3 2017/18 to 2.4% (24,246 diagnoses) in Q2 2018/19 (p=0.026), while the percentage of high-risk AF patients receiving anticoagulants increased from 80.5% in Q3 2017/18 to 86.9% in Q3 2018/19 (p=0.57), surpassing the Public Health England 2019 target of 85%.
The East Midlands AF Advance programme increased AF diagnosis and anticoagulation rates, which is expected to be of significant clinical benefit. The mobile AF detection devices provide a more practical alternative to traditional 12-lead electrocardiograms (ECGs) and should be incorporated into routine clinical practice for opportunistic AF detection, in combination with medication reviews to increase anticoagulant prescription.
December 2020 Br J Cardiol 2020;27:115–8 doi:10.5837/bjc.2020.035
Clinical application of physical-activity monitoring in patients with CIEDs
Kara Callum, David J Muggeridge, Oonagh M Giggins, Daniel R Crabtree, Trish Gorely, Stephen J Leslie

Regular physical activity for secondary prevention in cardiovascular disease has many well-recognised benefits, with declines in physical activity being associated with worsening cardiovascular disease, suboptimal treatment or worsening comorbidities that might be rectified by early intervention. Most cardiovascular implantable electronic devices (CIED) now have the ability to detect, analyse and interpret physical activity data through an inbuilt accelerometer. Currently, these data are not being utilised to their full potential. We present three cases that demonstrate some of the possible uses of CIED-collected physical-activity data. These data have the potential to detect a deteriorating patient, to monitor the effects of an intervention, and/or provide motivational feedback to a patient. However, for the data to be used in this manner in the future, greater transparency from manufacturers and robust validation studies will be needed.
December 2020 Br J Cardiol 2020;27:124–5 doi:10.5837/bjc.2020.036
DOACs for stroke prevention in patients with AF and cancer
Dipal Mehta, Avirup Guha, Peter K MacCallum, Amitava Banerjee, Charlotte Manisty, Thomas Crake, Mark Westwood, Daniel M Jones, Arjun K Ghosh

Stroke prophylaxis in atrial fibrillation is an important consideration in patients with cancer. However, there is little consensus on the choice of anticoagulation, due to the numerous difficulties associated with active cancer. Direct oral anticoagulants (DOACs) have been shown to be a promising option. Here, we conduct a simple cross-sectional analysis of 29 cancer patients receiving DOACs for stroke prophylaxis in atrial fibrillation at a tertiary-care institution in London. Our study demonstrates an encouraging efficacy and safety profile of DOACs used in this setting. We conclude by suggesting that, while DOACs may be useful, anticoagulation in cancer patients should continue to be individualised.
December 2020 Br J Cardiol 2020;27:126–8 doi:10.5837/bjc.2020.037
Timely discharge of low-risk STEMI patients admitted for primary PCI in an Essex cardiothoracic centre
Izza Arif, Rajender Singh

Data for low-risk ST-elevation myocardial infarction (STEMI) patients in the Essex cardiothoracic centre (CTC) during a three-month period were evaluated and the average duration of admission was calculated to be 67.2 hours. The data were sifted by applying Second Primary Angioplasty in Myocardial Infarction (PAMI-II) criteria for low-risk STEMI patients who could be safely discharged after 48 hours. After application of a proforma as a quality improvement intervention tool, data were re-assessed and the average time of admission observed for a similar cohort of patients dropped down to an average of 55.2 hours. Overall, there was a 13% average increase in rate of early discharge for low-risk STEMI patients.
December 2020 Br J Cardiol 2020;27:129–31 doi:10.5837/bjc.2020.038
Is there a need to measure pre- and post-capillary blood glucose following a cardiac exercise class?
Tim P Grove, Neil E Hill

Exercise training is associated with positive health outcomes in people with cardiovascular disease (CVD) and type 2 diabetes mellitus (T2DM). However, fear of hypoglycaemia is a potential barrier to participants attending a cardiac exercise class. Therefore, we assessed the capillary blood glucose (CBG) responses to the Imperial NHS Trust cardiac exercise class.
Forty patients (median age 66 years, interquartile range [IQR] 57–74 years) with CVD and T2DM treated with insulin and/or sulfonylureas completed a cardiac exercise class. CBG was measured immediately before and after the exercise class. Subgroup analysis assessed CBG levels in patients who had consumed food <2 and ≥2 hours and had taken their insulin and/or sulfonylureas <4 and ≥4 hours before the exercise class.
Overall, post-exercise CBG had significantly decreased (–3.0 mmol/L, p≤0.0001). Subgroup analyses demonstrated significant reductions in CBG in both food consumption groups (<2 hours –2.9 mmol/L, p≤0.0001, and ≥2 hours –3.1 mmol/L, p≤0.0001) and medication groups (<4 hours –3.4 mmol/L, p≤0.0002, and ≥4 hours –2.7 mmol/L, p≤0.0001). However, there were no significant differences in CBG between the food consumption groups and the medication groups, respectively (p=0.7 and p=0.3).
Cardiac exercise classes resulted in significant reductions in CBG levels. However, the timing of food consumption or medication intake did not influence the magnitude of CBG decline after the cardiac exercise class.
December 2020 Br J Cardiol 2020;27:141–2 doi:10.5837/bjc.2020.039
C-reactive protein: a prognostic indicator for sudden cardiac death post-myocardial infarction
Jordan Faulkner, Francis A Kalu

The inflammatory component of ischaemic heart disease (IHD) is well recognised. An elderly male, following primary percutaneous coronary intervention (pPCI) for ST-elevation myocardial infarction (STEMI), had, otherwise unexplained, severely elevated C-reactive protein (CRP) prior to sudden cardiac death (SCD). Post-mortem showed only old infarct, no re-stenosis, and no evidence of inflammation elsewhere. The levels of CRP in this case are much higher than those documented previously in IHD. Current guidelines advocate for implantable cardioverter defibrillator (ICD) implantation after acute coronary syndrome (ACS) only in the context of left ventricular ejection fraction <35%, therefore, this patient would not qualify. Multiple risk-stratification tools have been developed to widen ICD prescription after ACS, but have not yet been integrated into the National Institute for Health and Care Excellence (NICE) guidelines. This case is a poignant reminder that we must widen ICD prescription, and CRP should be considered as a likely predictor.
December 2020 Br J Cardiol 2020;27:143–4 doi:10.5837/bjc.2020.040
Quadricuspid aortic valve: a case report and review of the literature
Nicholas Cereceda-Monteoliva, Massimo Capoccia, Kwabena Mensah, Ruediger Stenz, Mario Petrou

Quadricuspid aortic valve (QAV) is a rare congenital anomaly that can present as aortic insufficiency later in life. We report a case of aortic regurgitation associated with a QAV, treated by aortic valve replacement. The patient presented with breathlessness, lethargy and peripheral oedema. Echocardiography and cardiac magnetic resonance revealed abnormal aortic valve morphology and coronary angiography was normal. The presence of a quadricuspid aortic valve was confirmed intra-operatively. This was excised and replaced with a bioprosthetic valve and the patient recovered well postoperatively. Importantly, the literature indicates that specific QAV morphology and associated structural abnormalities can lead to complications. Hence, early detection and diagnosis of QAV allows effective treatment. Aortic valve surgery is the definitive treatment strategy in patients with aortic valve regurgitation secondary to QAV. However, the long-term effects and complications of treatment of this condition remain largely unknown.
October 2020 Br J Cardiol 2020;27:119–23 doi:10.5837/bjc.2020.030
Women not in cardiology: where are we going wrong? A survey of the perceptions and barriers to training
Hibba Kurdi, Holly Morgan, Claire Williams

In the UK, there is a difference between the medical specialties and cardiology in recruitment of women. Research, thus far, has concentrated on women already in cardiology. Although invaluable in understanding barriers to training, these studies fail to provide insight into why other trainees chose an alternative. Therefore, we designed a survey aimed at medical personnel, evaluating why higher trainees in other specialties overlooked cardiology.
An online survey was distributed via email to non-cardiology higher trainees in Wales. Questions covered previous clinical experiences of cardiology, interactions with cardiologists, and tried to identify deterrent factors.
There were 227 responses received over six weeks: 61.7% (n=137) female respondents, 23.5% (n=52) less than full-time. Of these, 49% completed a cardiology placement previously. Bullying was witnessed and experienced equally among genders, females witnessed and experienced sexism, 24% (n=24) and 13% (n=13), respectively. In contrast, male trainees witnessed and experienced sexism 14% (n=7) and 0%. There were 62% (n=133) who felt cardiologists and registrars were unapproachable. Work-life balance ranked first (40%), as the most important factor influencing career choice. The negative attitudes of cardiologists and registrars was ranked top 3 for not pursuing cardiology.
In conclusion, many barriers exist to cardiology training including poor work-life balance, sexism and lack of less than full-time opportunities. However, this survey highlights that the behaviour of cardiologists and registrars has the potential to impact negatively on trainees. It is, therefore, our responsibility to be aware of this and encourage change.
October 2020 Br J Cardiol 2020;27:138–40 doi:10.5837/bjc.2020.032
Clinical cases illustrating the efficacy of intra-coronary lithotripsy
Paula Finnegan, John Jefferies, Ronan Margey, Barry Hennigan

We provide the details of three cases utilising intravascular lithotripsy, a novel approach to percutaneous coronary intervention (PCI).
October 2020 Br J Cardiol 2020;27:132–7 doi:10.5837/bjc.2020.034
FFR-CT strengthens multi-disciplinary reporting of CT coronary angiography
Iain T Parsons, Michael Hickman, Mark Ingram, Edward W Leatham

The utility of computed tomography (CT) coronary angiography (CTCA) is underpinned by its excellent sensitivity and negative-predictive value for coronary artery disease (CAD), although it lacks specificity. Invasive coronary angiography (ICA) and invasive fractional flow reserve (FFR), are gold-standard investigations for coronary artery disease, however, they are resource intensive and associated with a small risk of serious complications. FFR-CT has been shown to have comparable performance to FFR measurements and has the potential to reduce unnecessary ICAs. The aim of this study is to briefly review FFR-CT, as an investigational modality for stable angina, and to share ‘real-world’ UK data, in consecutive patients, following the initial adoption of FFR-CT in our district general hospital in 2016.
A retrospective analysis was performed of a previously published consecutive series of 157 patients referred for CTCA by our group in a single, non-interventional, district general hospital. Our multi-disciplinary team (MDT) recorded the likely definitive outcome following CTCA, namely intervention or optimised medical management. FFR-CT analysis was performed on 24 consecutive patients where the MDT recommendation was for ICA. The CTCA + MDT findings, FFR-CT and ICA ± FFR were correlated along with the definitive outcome.
In comparing CTCA + MDT, FFR-CT and definitive outcome, in terms of whether a percutaneous coronary intervention was performed, FFR-CT was significantly correlated with definitive outcome (r=0.471, p=0.036) as opposed to CTCA + MDT (r=0.378, p=0.07). In five cases (21%, 5/24), FFR-CT could have altered the management plan by reclassification of coronary stenosis. FFR-CT of 60 coronary artery vessels (83%, 60/72) (mean FFR-CT ratio 0.82 ± 0.10) compared well with FFR performed on 18 coronary vessels (mean 0.80 ± 0.11) (r=0.758, p=0.0013).
In conclusion, FFR-CT potentially adds value to MDT outcome of CTCA, increasing the specificity and predictive accuracy of CTCA. FFR-CT may be best utilised to investigate CTCAs where there is potentially prognostically significant moderate disease or severe disease to maximise cost-effectiveness. These data could be used by other NHS trusts to best incorporate FFR-CT into their diagnostic pathways for the investigation of stable chest pain.
September 2020 Br J Cardiol 2020;27:80–2 doi:10.5837/bjc.2020.026
Cardio-nephrology MDT meetings play an important role in the management of cardiorenal syndrome
Rajiv Sankaranarayanan, Homeyra Douglas, Christopher Wong

Cardiorenal syndrome is a complex condition associated with significant morbidity in the form of symptoms secondary to fluid overload, leading to hospitalisations, and portends increased mortality. Both the diagnosis and management of the conditions are complicated by the fact that there is dysfunction of the heart as well as the kidney, usually with uncertainty with regards to the timing of the first insult. Management in primary care, or in the emergency setting, tends to be predominantly focused on short-term improvement in function of one organ, leading to deleterious effects on the other. A consensus multi-disciplinary approach involving both cardiologists and nephrologists has been advocated in order to devise a unified management plan. Our report presents findings of monthly cardio-nephrology multi-disciplinary team meetings and illustrates that this can be an efficacious approach both in terms of avoiding unnecessary outpatient clinic visits, as well as consensus decision-making.
September 2020 Br J Cardiol 2020;27:100–1 doi:10.5837/bjc.2020.027
Twisting interval in complete heart block, cannot be overlooked: a challenging ECG dilemma
Mohsin Gondal, Ali Hussain

Ventriculophasic arrhythmia (VPA) is an intriguing electrocardiogram (ECG) phenomenon, often seen in patients with complete heart block, and could sometimes pose a challenging diagnostic dilemma for physicians. By definition, in VPA, the P–P intervals that contain a QRS complex are shorter than the P–P intervals that do not have a QRS complex. VPA is often a tell-tale ECG finding of complete heart block. We describe a case in which paroxysmal VPA led us to diagnose complete heart block.
September 2020 Br J Cardiol 2020;27:102–4 doi:10.5837/bjc.2020.028
New cardiac manifestation of IgG4-related disease: a case report
Marina Pourafkari, Prodipto Pal, Adriana Luk, Daniel Ennis, Mini Pakkal, Patrik Rogalla

Immunoglobulin G4-related disease (IgG4-RD) is a systemic fibro-inflammatory immune-mediated disease, which has been defined in the past few years. IgG4-RD affects various organs and leads to a variety of clinical manifestations. As it is a relatively newly defined entity, new manifestations are now being recognised and reported. We describe a case involving the cardiovascular system.
July 2020 Br J Cardiol 2020;27:83–6 doi:10.5837/bjc.2020.021
Coronary lithotripsy: a novel approach to intra-coronary calcification with ‘cracking’ results?
Paula Finnegan, John Jefferies, Ronan Margey, Barry Hennigan

![]() This article is available as a BJC Learning CPD activity
This article is available as a BJC Learning CPD activity
Coronary lithotripsy is a novel approach to percutaneous coronary intervention (PCI). It is based on well-established technology dating back to 1980 when lithotripsy was first used to treat renal calculi. Its application in cardiovascular medicine is a more recent development that involves using a low-pressure lithotripsy balloon to deliver unfocused acoustic pulse waves in a circumferential mechanical energy distribution. This causes fracturing of calcification within the surrounding vasculature, facilitating optimal stent deployment.
This article aims to review recent clinical experience and the published data regarding intravascular lithotripsy (IVL). All relevant articles were identified via PubMed using keywords including “intravascular lithotripsy”, “shockwave” and “coronary”. All studies that contained published datasets regarding IVL with patient numbers >50 were included for review. There were 116 results found. After reviewing all the publications, articles were then tabulated and 17 were found to be relevant, including only four clinical studies.
In this review we found that intracoronary lithotripsy for heavily calcified arteries appears to be a safe, effective, easy-to-use method of dealing with an otherwise technically-challenging and high-risk scenario. It appears to carry low risk, uses low pressures, and exerts its effects on both superficial and deep intravascular calcium. Further prospective data with long-term follow-up will be required to explore both the off-label uses of IVL (such as post-stent dilatation), and the long-term patency of these vessels.
July 2020 Br J Cardiol 2020;27:87–92 doi:10.5837/bjc.2020.022
Personalised external aortic root support (PEARS) to stabilise an aortic root aneurysm
John Pepper, Tal J Golesworthy, Cemil Izgi, Johanna J M Takkenberg, Tom Treasure

Patients with congenitally determined aortic root aneurysms are at risk of aortic valve regurgitation, aortic dissection, rupture and death. Personalised external aortic root support (PEARS) may provide an alternative to aortic root replacement.
This was a multi-centre, prospective cohort of all consecutive patients who received ExoVasc mesh implants for a dilated aortic root between 2004 and 2017. Baseline and peri-operative characteristics, as well as early postoperative outcomes are described, and time-related survival and re-operation free survival are estimated using the Kaplan-Meier method.
From 2004 through 2017, 117 consecutive patients have received ExoVasc mesh implants for aortic root aneurysm. The inclusion criteria were an aortic root/sinus of Valsalva and ascending aorta with asymptomatic dilatation of between 40 and 50 mm in diameter in patients aged 16 years or more. Patients with more than mild aortic regurgitation were excluded. There was one early death. The length of stay was within seven days in 75% of patients.
In conclusion, the operation achieves the objectives of valve-sparing root replacement. PEARS may be seen as a low-risk conservative operation, which can be applied earlier on in the disease process, and which is complementary to more invasive procedures, such as valve-sparing root replacement or total root replacement.
July 2020 Br J Cardiol 2020;27:93–6 doi:10.5837/bjc.2020.023
Shared decision-making for ICDs: a regional collaborative initiative
Honey Thomas, Mark Lambert, Chris Plummer, Craig Runnett, Richard Thomson, Anne Marie Troy-Smith, Andrew J Turley

The National Institute for Health and Care Excellence (NICE) and NHS England have shown a commitment to embedding shared decision-making (SDM) in clinical practice and developing decision aids based on clinical guidelines. Healthcare policy makers are keen to enhance the engagement of patients in SDM in the belief that it improves the benefits accrued from healthcare interventions. This may be important for interventions such as implantable cardioverter-defibrillator (ICD) implantation, where cost-effectiveness is under scrutiny. NHS England invited the ICD implanters in the north of England to participate in a regional commissioning quality incentive (CQUIN) project to improve decision-making around a primary prevention ICD implant. A collaborative project included the development of a specific SDM tool, the first of its kind in the UK, followed by training and education of the clinical teams. The project illustrates that this approach is practical and deliverable and could be applied and used in other regions, and considered in additional clinical areas.
July 2020 Br J Cardiol 2020;27:97–9 doi:10.5837/bjc.2020.024
Computed tomography artefact finding of pacing lead perforation
Holly Morgan, Christopher Williams, Robert A Bleasdale

Computed tomography (CT) is a widely available imaging modality and artefactual findings are not uncommon, particularly in the presence of foreign bodies.
We conducted a retrospective analysis of all CT scans carried out in our trust in a 12-month period, identifying all reports containing the word “pacemaker”. There were 88 scans identified, six of which reported findings related to the pacemaker. In five cases right ventricular lead perforation was reported. All patients underwent further investigations, which did not show any evidence of true lead perforation.
In conclusion, it is important that both cardiologists and radiologists are aware of the possibility of artefactual lead perforation on CT.
June 2020 Br J Cardiol 2020;27:51–54 doi:10.5837/bjc.2020.017
Impact of COVID-19 on primary percutaneous coronary intervention centres in the UK: a survey
Ahmed M Adlan, Ven G Lim, Gurpreet Dhillon, Hibba Kurdi, Gemina Doolub, Nadir Elamin, Amir Aziz, Sanjay Sastry, Gershan Davis

During the coronavirus disease (COVID-19) pandemic, the British Cardiovascular Society/British Cardiovascular Intervention Society and the British Heart Rhythm Society recommended to postpone non-urgent elective work and that primary percutaneous coronary intervention (PCI) should remain the treatment of choice for patients with ST-segment elevation myocardial infarction (STEMI). We sought to determine the impact of COVID-19 on the primary PCI service within the United Kingdom (UK).
A survey of 43 UK primary PCI centres was performed and a significant reduction in the number of cath labs open was found (pre-COVID 3.6±1.8 vs. post-COVID 2.1±0.8; p<0.001) with only 64% of cath labs remained open during the COVID-19 pandemic. Primary PCI remained first-line treatment for STEMI in all centres surveyed.
June 2020 Br J Cardiol 2020;27:55–9 doi:10.5837/bjc.2020.018
COVID-19: the heart and other issues
Cormac T O’Connor, David Mulcahy

From the time that the first cases were reported from Wuhan, China on the 31st December 2019,1 our knowledge of the clinical and virological associations of the novel coronavirus (COVID-19) has been evolving at a rapid pace. On 18th May 2020, COVID-19 had caused over 4.82 million cases worldwide and resulted in 316,959 deaths.2 Whilst the primary focus of management for patients with COVID-19 remains close monitoring of respiratory function, there have been high levels of cardiac dysfunction in emerging cross-sectional and observational analyses, suggesting the need for heightened awareness in patients who may require cardiac input as part of a multidisciplinary approach. We review the current data on the association of COVID-19 and the heart.
June 2020 Br J Cardiol 2020;27:67–70 doi:10.5837/bjc.2020.020
An exercise-based cardiac rehabilitation programme for AF patients in the NHS: a feasibility study
Mark Mills, Elizabeth Johnson, Hamza Zafar, Andrew Horwood, Nicola Lax, Sarah Charlesworth, Anna Gregory, Justin Lee, Jonathan Sahu, Graeme Kirkwood, Nicholas Kelland, Andreas Kyriacou

There is increasing evidence for the role of exercise-based cardiac rehabilitation in the management of patients with atrial fibrillation (AF). However, this intervention has not yet been widely adopted within the National Health Service (NHS).
We performed a feasibility study on the utilisation of an established NHS cardiac rehabilitation programme in the management of AF, and examined the effects of this intervention on exercise capacity, weight, and psychological health. We then identified factors that might prevent patients from enrolling on our programme.
Patients with symptomatic AF were invited to participate in an established six-week exercise-based cardiac rehabilitation programme, composed of physical activity and education sessions. At the start of the programme, patients were weighed and measured, performed the six-minute walk test (6MWT), completed the Generalised Anxiety Disorder Questionnaire (GAD-7), and the Patient Health Questionnaire (PHQ-9). Measurements were repeated on completion of the programme.
Over two years, 77 patients were invited to join the programme. Twenty-two patients (28.5%) declined participation prior to initial assessment and 22 (28.5%) accepted and attended the initial assessment, but subsequently withdrew from the programme. In total, 33 patients completed the entire programme (63.9 ± 1.7 years, 58% female). On completion, patients covered longer distances during the 6MWT, had lower GAD-7 scores, and lower PHQ-9 scores, compared with their baseline results. Compared with patients that completed the entire programme, those who withdrew from the study had, at baseline, a significantly higher body mass index (BMI), covered a shorter distance during the 6MWT, and had higher PHQ-9 and GAD-7 scores.
In conclusion, enrolling patients with AF into an NHS cardiac rehabilitation programme is feasible, with nearly half of those invited completing the programme. In this feasibility study, cardiac rehabilitation resulted in an improved 6MWT, and reduced anxiety and depression levels, in the short term. Severe obesity, higher anxiety and depression levels, and lower initial exercise capacity appear to be barriers to completing exercise-based cardiac rehabilitation. These results warrant further investigation in larger cohorts.
May 2020 Br J Cardiol 2020;27:64–6 doi:10.5837/bjc.2020.011
Hypertrophic cardiomyopathy and exercise restrictions: time to let the shackles off?
Yuen W Liao, James Redfern, John D Somauroo, Robert M Cooper

The health benefits of physical activity are well documented. Patients with hypertrophic cardiomyopathy (HCM) are often discouraged from participating in physical activity due to a perceived increase in the risk of sudden cardiac death (SCD). As a result, only 45% of patients with HCM meet the minimum guidelines for physical activity, and many report an intentional reduction in exercise following diagnosis. Despite most SCD being unrelated to HCM, guidelines traditionally focused on the avoidance of potential risk through restriction of exercise, without clear recommendations on how to negate the negative health impact of inactivity. Retrospective reviews have demonstrated that the majority of cardiac arrests in patients with HCM occurred at rest or on mild exertion and that the overall incidence of HCM-related SCD is significantly lower than previously reported. We will discuss current international guidelines and recommendations and consider the outcomes of various studies that have investigated the effects of exercise of different intensities on patients with HCM. In light of the growing evidence suggesting that carefully guided exercise can be both beneficial and safe in patients with HCM, we ask whether it is time to let the shackles off exercise restriction in HCM.
May 2020 Br J Cardiol 2020;27:60–3 doi:10.5837/bjc.2020.012
A multi-disciplinary care pathway improves symptoms, QoL and medication use in refractory angina
Kevin Cheng, Ranil de Silva

Refractory angina (RA) is a growing clinical problem. Long-term mortality is better than expected and focus has shifted to improving symptoms, quality of life and psychological morbidity. We established a dedicated multi-disciplinary care pathway for patients with RA and assessed its effect on psychological outcomes, quality of life and polypharmacy. We reviewed electronic health records to capture demographics, changes in medication use, and patient-related outcome measures (Seattle Angina Questionnaire [SAQ] and Hospital Anxiety and Depression Scale) before and after enrolment.
One hundred and ninety patients were referred to our service. Pre- and post-questionnaire data were available in 83 patients. Anxiety and depression scores significantly improved (p<0.05) as well as quality of life and all subcategories of the SAQ (p<0.0001). Patients were most commonly on three or four anti-anginal drugs. In patients with no demonstrable reversible ischaemia, there was a significant reduction in anti-anginal usage (mean reduction of two drugs) after completion of our pathway (p<0.025).
In conclusion, a dedicated multi-disciplinary pathway for RA is associated with improvements in quality of life, mental health and polypharmacy. An ischaemia-driven method to rationalise medication may reduce polypharmacy in patients with RA, particularly in patients with no demonstrable ischaemia.
May 2020 Br J Cardiol 2020;27:71 doi:10.5837/bjc.2020.013
Ezekiel’s heart
JJ Coughlan, Max Waters, David Moore, David Mulcahy

“I will give you a new heart and put a new spirit in you; I will remove from you your heart of stone and give you a heart of flesh” – Ezekiel 36:26
May 2020 Br J Cardiol 2020;27:72–3 doi:10.5837/bjc.2020.014
Can a giant U-wave be innocent?
Sinead Curran, Waleed Arshad, Arvinder Kurbaan, Han B Xiao

The U-wave on electrocardiogram (ECG) is a small deflection following the T-wave, the sixth wave. It is 25% or less of the preceding T-wave in amplitude.1,2 While the genesis of the U-wave is uncertain, it is said to represent repolarisation of the Purkinje fibres.1,2 Disproportionally large U-waves may indicate underlying cardiac or non-cardiac pathology. A relatively frequent cause for a large U-wave is hypokalaemia. It is observed in patients with bradycardia, ventricular hypertrophy, hypothyroidism, hypocalcaemia, hypomagnesaemia, mitral valve prolapse, hypothermia, increased intracranial pressure, or patients on anti-arrhythmic medicine.2 A negative U-wave, on the other hand, may represent early myocardial ischaemia, specifically in the context of a lesion in the left main or proximal left anterior descending coronary artery.2,3
March 2020 Br J Cardiol 2020;27:27–30 doi:10.5837/bjc.2020.006
Rise of the machines: will heart failure become the first cyber-specialty?
Shirley Sze

Digital healthcare is being introduced to the management of heart failure as a consequence of innovations in information technology. Advancement in technology enables remote symptom and device monitoring, and facilitates early detection and treatment of heart failure exacerbation, potentially improving patient outcomes and quality of life. It also provides the potential to redesign our heart failure healthcare system to one with greater efficacy through resource-sparing, computer-aided decision-making systems. Although promising, there is, as yet, insufficient evidence to support the widespread implementation of digital healthcare. Patient-related barriers include user characteristics and health status; privacy and security concerns; financial costs and lack of accessibility of digital resources. Physician-related barriers include the lack of infrastructure, incentive, knowledge and training. There are also a multitude of technical challenges in maintaining system efficiency and data quality. Furthermore, the lack of regulation and legislation regarding digital healthcare also prevents its large-scale deployment. Further education and support and a comprehensive workable evaluation framework are needed to facilitate confident and widespread use of digital healthcare in managing patients with heart failure.
March 2020 Br J Cardiol 2020;27:31–3 doi:10.5837/bjc.2020.007
Primary prevention aspirin among the elderly: challenges in translating trial evidence to the clinic
J William McEvoy, Michael Keane, Justin Ng

The ASPirin in Reducing Events in the Elderly trial (ASPREE) contributed important knowledge about primary cardiovascular disease (CVD) prevention among healthy older adults. The finding that daily low-dose aspirin (LDA) does not statistically prevent disability or CVD among adults aged over 70 years when compared with placebo, but does significantly increase risk of haemorrhage, immediately influenced clinical practice guidelines. In this article, we discuss nuances of the trial that may impact the extrapolation of the ASPREE trial results to the everyday individual clinical care of older adults.
March 2020 Br J Cardiol 2020;27:40 doi:10.5837/bjc.2020.008
Can you smell too good at work?
Grace Lydia Goss, Tarik Salem Ahmed Salim, John Huish, Gethin Ellis

A 78-year-old man presented to the emergency department with recurrent episodes of syncope precipitated by a variety of strong aromas. He denied chest pain, breathlessness or palpitations. There were no headaches, no blurred vision or limb weakness or seizure-like activity. On recovery, he had no post-ictal symptoms. He was initially discharged after initial investigations, including electrocardiogram (ECG), were normal. On the way to the main entrance, while passing cleaning equipment (which included strongly smelling bleach), he experienced a further syncopal episode. He was taken into the resuscitation bay, attached to cardiac monitoring and referred to the medical on-call team. When approached by the medical registrar on call (who was wearing ‘powerful’ aftershave), the patient commented the scent was precipitating a further attack. The registrar reviewed the cardiac monitor captured in figure 1 and witnessed a prolonged pause followed by asystole. Cardiopulmonary resuscitation (CPR) was commenced for approximately one minute, at which point there was a spontaneous recovery of cardiac output and a quick recovery to baseline.
March 2020 Br J Cardiol 2020;27:37–40 doi:10.5837/bjc.2020.009
Progestogen-only pill associates with false-positive aldosterone/renin ratio screening test
Alexander Birkinshaw, Pankaj Sharma, Thang S Han

Aldosterone/renin ratio (ARR) is commonly used to screen for primary hyperaldosteronism (Conn’s disease). A number of drugs can alter ARR measurements, thus requiring omission before testing. However, hormonal agents such as the combined oral contraceptive (COCP) or progestogen-only pill (POP) are not listed for omission. A 20-year-old woman was referred to the endocrinology team, following investigations for syncope by her cardiologist, when ARR was found to be elevated. She was taking POP (Cerelle®) while having ARR measured. After omitting POP for four weeks, plasma aldosterone concentration was reduced by 52% (from 560 pmol/L to 271 pmol/L, reference range: 100–450 pmol/L), plasma renin concentration increased by 253% (from 3.6 mU/L to 12.7 mU/L, reference range: 5.4–30 mU/L) and ARR reduced from 156 to 21 (–86.5%) (reference range: <80 suggests Conn’s unlikely). To the best of our knowledge, this is the first reported case of POP-related false-positive ARR screening for primary hyperaldosteronism. Omission of POP should, therefore, be considered in women undergoing ARR measurement.
January 2020 Br J Cardiol 2020;27:19–23 doi:10.5837/bjc.2020.002
Cancer immunotherapy and its potential cardiac complications
Simon G Findlay, Ruth Plummer, Chris Plummer

Recent advances in immune therapy for cancer have significantly improved the clinical outcomes of patients with advanced cancers, where prognosis has historically been very poor. With these new treatments have come new toxicities and, as the use of immunotherapy increases, we will see an increasing incidence of immune-related adverse events, with patients presenting as an emergency. It is important that all cardiologists, and other physicians who see these patients, are aware of life-threatening immune-related toxicities, in addition to their recommended investigation and treatment.
We describe a patient with acute cardiotoxicity secondary to immune therapy to illustrate the complexity of these adverse cardiovascular events, providing recommendations for screening, diagnosis and management.
January 2020 Br J Cardiol 2020;27:24–5 doi:10.5837/bjc.2020.003
Cardiac tumours – a brief review
Amaliya A Arakelyanz, Tatiana E Morozova, Anna V Vlasova, Roman Lischke

This short review of cardiac tumours presents a case that clearly demonstrates the manifestation of embolic and cardiac symptoms of an intracardiac mass. Acute onset and rapid progression of a neoplastic process in the heart leading to arrhythmia, cardiac conduction disorders and heart failure combined with highly mobile fragments of tumour, which can cause emboli in cerebral vessels, are characteristic signs of an intracardiac mass. Early diagnosis and immediate treatment may improve the long-term prognosis, but overall the prognosis is poor. Cardiac tumours present to the cardiologist when the patient presents with cardiac symptoms, and the neurologist when there are cerebral symptoms. Most cardiac masses are not amenable to percutaneous biopsy; therefore, definitive diagnosis often awaits surgical excision.
January 2020 Br J Cardiol 2020;27:34–6 doi:10.5837/bjc.2020.004
Successful treatment of ischaemic ventricular septal defect and acute right ventricular failure: a challenging case in the modern NHS
Renata Greco, Andrew Johnson, Xy Jin, Rajesh K Kharabanda, Adrian P Banning, Mario Petrou

A 52-year-old man, previously fit and well, presented with myocardial infarction complicated by ischaemic ventricular septal defect (VSD) and acute right ventricular failure, was successfully treated with early percutaneous coronary reperfusion, surgical VSD repair and temporary right ventricular assist device (VAD) support.
This case is an example of how a modern healthcare system can successfully manage complex emergency cases, combining high levels of clinical care and medical technology. Access to temporary mechanical support played a vital role in this case. We believe that wider access to VADs may contribute to improvement in the, widely recognised, poor outcome of ischaemic VSD.
November 2019 Br J Cardiol 2019;26:130–2 doi:10.5837/bjc.2019.039
Depression screening in CAD may provide an opportunity to decrease health outcomes disparities
Adam Prince, Umair Ahmed, Nikhil Sharma, Rachel Bond

Depressive symptoms in coronary artery disease (CAD) are known to associate with increased mortality. We evaluated management of depression screening in the outpatient setting for patients with known CAD at ambulatory visits. We assessed whether depression screening was performed with a patient health questionnaire, as well as what was done with positive results. Our study identified 355 patients who visited an ambulatory primary care clinic over a three-year period, 57% of whom were screened at least once. Positive scores for depression were found in 20% of patients screened, with 54% of screening-positive patients given plans for additional care. We found disparities between screening rates, with whites screened least for depression, as well as in management plans, with whites given highest probability of mentioned treatment in their assessment and plan if depression screening was positive. Given the association with increased mortality in known CAD, depression screening may represent an opportunity to decrease health outcomes disparities and to improve outcomes for patients with CAD in the outpatient setting.
November 2019 Br J Cardiol 2019;26:133–6 doi:10.5837/bjc.2019.040
Unscheduled care bed days can be reduced with a syncope pathway and rapid access syncope clinic
Bruce McLintock, James Reid, Eileen Capek, Lesley Anderton, Lara Mitchell

A syncope pathway for secondary care was launched in the Queen Elizabeth University Hospital (QEUH), Glasgow, in 2016. The pathway aims to risk stratify patients into three categories: high risk (requiring admission), intermediate risk (suitable for discharge ± outpatient review) or low risk (no further investigation required). There are clear referral procedures to the rapid access syncope clinic (RASCL). Our aim was to assess the impact of the pathway on unscheduled care in terms of admission rates, length of stay and referrals to RASCL.
Data were collected on three occasions: before the introduction of the pathway, immediately after and again 14 months later. Those patients with a diagnostic ICD-10 code of ‘syncope and collapse’ or ‘orthostatic hypotension’ presenting to the QEUH (both emergency department and immediate assessment unit, via GP referral) were identified.
There were 779 patients identified, 538 were included for analysis once other diagnoses were excluded: 46% were male with an age range from 16 to 95 years with a median age of 65.5 years.
All high-risk patients were admitted. For intermediate-risk patients the admission rate fell from 62% to 52% immediately after pathway introduction and after one year to 42%, suggesting sustained improvement (p=0.08). Admission for low-risk patients after one year of pathway roll out fell from 27% to 12% (p=0.04). The median length of stay prior to introduction was three days, this fell to one day one-year post-pathway, saving 56 bed days per month.
In conclusion, a syncope pathway and RASCL has reduced admission of low-risk patients, provided appropriate follow-up for intermediate risk, and reduced length of stay for those requiring admission.
November 2019 Br J Cardiol 2019;26:141–4 doi:10.5837/bjc.2019.041
Lipid testing and treatment after acute myocardial infarction: no flags for the flagship
Louise Aubiniere-Robb, Jonathan E Dickerson, Adrian J B Brady

National guidelines on lipid modification for cardiovascular disease advise checking a lipid profile in all patients admitted with acute coronary syndrome (ACS). It has been demonstrated that ACS can impact lipid profiles in an unpredictable fashion, so cholesterol measurements should be taken within 24 hours of an infarct. National guidelines also recommend initiating early high-intensity lipid-lowering therapy (i.e. statins) in ACS for secondary prevention of cardiovascular disease. We first assess compliance with these guidelines in a large city-centre teaching hospital and identify the need for any improvement. Following varied interventions aimed at highlighting the need for adherence to these guidelines we demonstrate a large increase in the number of ACS patients having lipids checked within 24 hours of their admission. In some instances, baseline cholesterol was not measured (either at all or prior to statin therapy), potentially leaving familial and non-familial hypercholesterolaemia undiagnosed. Encouragingly, statins are already prescribed in accordance with guidelines for the majority of ACS patients regardless of our campaign. We ultimately demonstrate there is still much work to be done locally to improve cholesterol management in ACS and hope that our findings will encourage others to ensure compliance and ultimately improve patient outcomes.
November 2019 Br J Cardiol 2019;26:153–6 doi:10.5837/bjc.2019.042
The permanent decline of temporary pacing
Richard Baker, David Wilson

Emergency transvenous temporary pacing is a potentially lifesaving procedure that can be associated with significant complications. Historically, this procedure was performed by relatively inexperienced doctors. In recent years, there have been moves to improve the delivery of emergency pacing in UK hospitals.
We aimed to identify trends in temporary pacing experience among medical registrars in the southwest of England between 2008 and 2016. Registrars currently or previously accrediting with General Internal Medicine (GIM) were surveyed about experience in emergency transvenous pacing.
There have been significant changes in the delivery of temporary pacing over the two time points. Significantly fewer temporary pacing wires had been inserted by medical registrars in 2016 compared with 2008: mean 4.51 versus 9.82 (p<0.0001). Significantly more medical registrars had never inserted a temporary pacing wire in 2016 compared with 2008: 57/84 (67.9%) versus 18/94 (19.1%), p<0.0001. Registrars increasingly did not rate themselves to be fully competent to perform the procedure in 2016, 76/84 (90%), compared with 54/92 (59%) in 2008, p=0.0097. Perceptions regarding who should provide this service have changed. In 2008, 65/92 (79.6%) thought cardiologists should be the sole operators compared with 81/84 (96.4%) in 2016.
In conclusion, there has been a significant change in the provision of emergency temporary pacing services from 2008 to 2016. UK medical registrars no longer have the experience to perform this procedure. It is hoped that a rapidly delivered, cardiology-led pacing service will continue to improve safety and patient care.
October 2019 Br J Cardiol 2019;26:149–52 doi:10.5837/bjc.2019.033
Transcatheter aortic valve replacement in patients with systolic heart failure
Tariq Enezate, Jad Omran, Obai Abdullah, Ehtisham Mahmud

New York Heart Association (NYHA) class IV heart failure is one of the factors used in predicting in-hospital mortality in patients undergoing transcatheter aortic valve replacement (TAVR). The effect of systolic heart failure (SHF), aside from NYHA classification, on peri-procedural outcomes is unclear.
The study population was identified from the 2016 Nationwide Readmissions Data database using International Classification of Diseases-Tenth Revision codes for TAVR and SHF. Study end points included in-hospital all-cause mortality, the length of hospital stay, cardiogenic shock, acute myocardial infarction (AMI), acute kidney injury (AKI), mechanical complications of prosthetic valve, bleeding, and 30-day readmission rate. Propensity matching was used to create a control group of TAVR patients without a SHF diagnosis (TAVR-C).
A total of 5,674 patients were included in each group (mean age 79.9 years; 35.6% female). The groups were comparable in terms of baseline characteristics and comorbidities. TAVR-SHF was associated with significantly higher in-hospital all-cause mortality (2.7% vs. 1.9%, p<0.01), longer hospital stay (7.5 vs. 5.5 days, p<0.01), higher cardiogenic shock (5.1% vs. 1.6%, p<0.01), AMI (4.0% vs. 1.9%, p<0.01), AKI (18.7% vs. 12.4%, p<0.01) and mechanical complications of prosthetic valve (1.2% vs. 0.6%, p<0.01). There was no significant difference between TAVR-SHF and TAVR-C in terms of bleeding (19.5% vs. 18.2%, p=0.08) and 30-day readmission rate (10.8% vs. 10.2%, p=0.29).
Compared with TAVR-C, TAVR-SHF was associated with higher in-hospital peri-procedural complications and all-cause mortality.
October 2019 Br J Cardiol 2019;26:157–8 doi:10.5837/bjc.2019.034
The effect of ageing on the frontal QRS-T angle on the 12-lead ECG
Sadia Chaudhry, Jagan Muthurajah, Keoni Lau, Han B Xiao

The frontal QRS-T angle (QTA) is widely available on routine 12-lead electrocardiograms (ECGs), but its practical significance is little recognised. An abnormally wide QTA is known to be a prognostic predictor of cardiovascular events. It has even been considered as a stronger prognostic predictor than the commonly used ECG parameters including ST-T abnormality and QT prolongation. The aim of this study was to investigate the influence of ageing on the QTA in a low-risk population where there were no obvious ECG abnormalities. Having analysed 437 consecutive patients, we found a positive correlation between age and QTA, but no age difference in heart rate, QRS duration, QT interval and P-wave axis. As hypertension was more prevalent in older patients, we compared patients with hypertension to those without and found no significant difference in QTA. Therefore, ageing alone is a significant contributory factor to the widening of QRS-T angle. Further study to confirm QTA as a prognostic predictor for all-cause mortality, independent of age itself and in the absence of ECG abnormalities, in an older population would be significant.
October 2019 Br J Cardiol 2019;26:145–8 doi:10.5837/bjc.2019.035
Clinical CMR: one-year case mix, outcomes and stress-testing accuracy from a regional tertiary centre
Protik Chaudhury, Min Aung, Rossella Barbagallo, Edward Barden, Swamy Gedela, Stuart J Harris, Henry O Savage, Jason N Dungu

Cardiac magnetic resonance (CMR) imaging has developed into a crucial diagnostic tool in all patients with known or suspected heart disease. The aim of this study was to review real-world data regarding the case mix and performance of stress CMR for the large Essex region, a population of 1.4 million.
All studies from April 2017 to April 2018 were reviewed. All scans were performed on a 1.5-T scanner (Siemens MAGNETOM Aera). We have not included research scans or repeat studies. A total of 1,706 clinical studies were performed, including 592 adenosine stress perfusion scans (35%). Mean age of patients was 59 years ± 16 (range 16–97) and the majority were male (66%). Ischaemic heart disease (IHD) was diagnosed in 28% of patients. Objective ischaemia was evident in 226 cases (38% of all stress scans). The positive predictive value of stress imaging was 91%. Non-ischaemic cardiomyopathies were diagnosed in 598 patients (35%), including dilated cardiomyopathy (DCM, 23%) and hypertrophic cardiomyopathy (HCM, 8%) as the most common phenotypes. The mean left ventricular ejection fraction (LVEF) was 51% across all groups (range 3–78%) with a significant difference between ischaemic and non-ischaemic cardiomyopathy (48% vs. 41%, p<0.0001); despite this, there was no significant difference in survival (p=0.177).
In conclusion, stress perfusion imaging accurately identifies true-positive ischaemia, as well as offering additional information regarding cardiac structure. The burden of non-ischaemic cardiomyopathy in Essex is significant, with 50 new diagnoses per month, across five hospitals. Coordination of services is needed to standardise practice and management of cardiomyopathy patients.
October 2019 Br J Cardiol 2019;26:137–40 doi:10.5837/bjc.2019.036
PCSK9 inhibitors in familial hypercholesterolaemia: a real-world experience and a meta-analysis
Harshal Deshmukh, Deepa Narayanan, Maria Papageorgiou, Yvonne Holloway, Sadaf Ali, Thozhukat Sathyapalan

Proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors have opened a new avenue in the management of dyslipidaemia in patients with familial hypercholesterolaemia (FH), but real-world experience with PCSK9 inhibitors is limited.
We aimed to explore the efficacy and safety of PCSK9 inhibitors in a single-centre study, and to conduct a meta-analysis of the available observational studies to report pooled data on these efficacy and safety parameters.
The Hull PCSK9 inhibitor study consisted of patients from the Lipid Clinic at the Hull Royal Infirmary–Hull University Teaching Hospitals NHS Trust during the period 2016–2018. Patients with FH and atherosclerotic cardiovascular disease (ASCVD) were screened for eligibility and were prescribed PCSK9 inhibitors. Lipid profile, liver function, renal function, and creatine kinase levels were measured at baseline and after a 12-week follow-up. For the meta-analysis, review of the literature identified six additional observational studies for FH, which were used to calculate pooled percentage low-density lipoprotein (LDL)-cholesterol (LDL-C) reduction.
The Hull PCSK9 inhibitor study consisted of 16 patients with definite FH (LDL-receptor mutation-positive), 20 patients with clinical FH and 15 patients with ASCVD with a mean age of 60.6 ± 13.9 years, 60% female. Baseline median (interquartile range) LDL-C levels (mmol/L) in the definite FH, clinical FH and ASCVD were 4.9 (4.6–5.9), 6.7 (5.3–7.1) and 4.4 (4.1–4.7). After 12 weeks, the LDL-C levels (mmol/L) dropped significantly (p<0.0001) in all three groups to 2.0 (1.6–3.4), 2.3 (1.9–2.6) and 2.2 (1.7–2.8) in the definite FH, clinical FH and ASCVD groups, respectively. The meta-analysis of the seven observational studies in 446 patients with FH showed pooled mean reduction of 55.5 ± 18.1% in the LDL-C levels, with 58% of patients reaching treatment targets. Treatment-associated side effects occurred in 6% to 45% of patients, and 0–15% of patients discontinued treatment due to intolerable side effects.
In conclusion, we showed that PCSK9 inhibitors are overall well-tolerated when used in real-world settings, and their efficacy is comparable with that reported in clinical trials. Longitudinal population-based registries are needed to monitor responses to treatment, treatment adherence and side effects of these lipid-lowering agents.
October 2019 Br J Cardiol 2019;26:159–60 doi:10.5837/bjc.2019.037
Atypical presentation of STEMI with pericardial effusion causing cardiac tamponade related to malignancy
Matthew J Johnson, Rohan Penmetcha

Cardiac tamponade and myocardial infarction (MI) are rare as the initial presentation of a malignancy. ST-elevation myocardial infarction (STEMI) and cardiac tamponade have been described to present together in the setting of a type-A aortic dissection causing coronary malperfusion. We describe a case with an atypical presentation of an MI due to a thrombus in the right coronary artery occurring simultaneously with a pericardial effusion causing tamponade physiology, related to malignancy. We present this unique case of MI and cardiac tamponade as it was not caused by a type-A aortic dissection. We suggest that malignancy be considered in the differential diagnosis when these findings present together.
September 2019 Br J Cardiol 2019;26:99–100 doi:10.5837/bjc.2019.028
My 60-year relationship with aortic stenosis
Anthony P C Bacon, Harry Rosen, Neil Ruparelia

The management of aortic stenosis has dramatically changed over the last 60 years. We briefly describe these remarkable advances from the personal perspective of Anthony P C Bacon (APCB) who was one of the first physicians to observe the importance of this pathological process and who watched, first-hand, some of the first surgical aortic valve procedures being performed in the UK. He most recently benefited from treatment with transcatheter aortic valve implantation (TAVI) himself, and provides a personal perspective of his experiences.
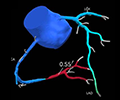
September 2019 Br J Cardiol 2019;26:105–9 doi:10.5837/bjc.2019.029
CT coronary angiography with HeartFlow®: a user’s perspective
Paul Brady, Andrew Kelion, Tom Hyde, Edward Barnes, Hazim Rahbi, Andy Beale, Steve Ramcharitar

![]() This article is available as a 'Learning with reflection' CPD activity
This article is available as a 'Learning with reflection' CPD activity
In November 2016, the National Institute for Health and Care Excellence (NICE) published an update of its guideline for the investigation of chest pain of recent onset (CG95), bringing computed tomography coronary angiography (CTCA) to the forefront as the first-line investigation. CTCA has a high negative-predictive value for the identification of obstructive coronary artery disease (CAD), but its positive-predictive value may be as low as 48%. Moreover, until recently it was unable to determine the functional significance of stenoses identified by CTCA. Using advanced computational fluid dynamics (CFD), HeartFlow® has pioneered a system that can predict the invasive fractional flow reserve (FFR) from a standard CTCA acquisition (FFRCT). The PLATFORM study has demonstrated that the use of CTCA with FFRCT was associated with equivalent clinical outcomes in terms of major adverse cardiovascular events (MACE) and quality of life at one year compared with usual testing. The global ADVANCE registry, and other long-term follow-up studies in over 9,000 patients, have demonstrated extremely good long-term outcomes when patients with CAD but negative FFRCT are managed conservatively without invasive testing. In a technology appraisal (MTG32), NICE projected that the adoption of this technology within the NHS in England could save at least £9.1 million by 2022. While it is accepted that the HeartFlow® FFRCT shows a lot of promise, there are a number of limitations that need to be considered.
September 2019 Br J Cardiol 2019;26:114–8 doi:10.5837/bjc.2019.030
Coronary artery bypass angiography: the exception to the radial access rule?
Amir Orlev, Amna Abdel-Gadir, Graeme Tait, Jonathan P Bestwick, David S Wald

Radial artery access coronary angiography is associated with high procedural success and lower rates of complications, compared with femoral access, in patients without prior coronary artery bypass surgery (CABG). Whether or not this applies to patients who have undergone CABG is not known.
We retrospectively examined hospital records of 5,993 consecutive patients undergoing coronary angiography to identify patients with previous CABG undergoing the procedure by the radial or femoral access routes. We compared clinical characteristics, procedural success and complications up to 30 days, adjusting for significant baseline differences.
Among the 5,993 patients undergoing angiography, 471 (8%) had previous CABG; 164 (35%) underwent angiography by the radial and 307 (65%) by the femoral artery. Procedural success was lower in the radial than femoral groups; 28/164 (17%) radial versus 1/307 (0.3%) femoral patients required access-site cross-over (p<0.001) and 254/347 (73%) versus 496/594 (84%) bypass grafts were selectively identified without the need for further imaging investigations (p=0.008), respectively. Access-site bleeding requiring compression affected 1/164 (0.6%) in the radial group and 12/307 (3.9%) in the femoral group (p=0.04 for difference) with no significant differences in other major complications.
About one in 12 patients undergoing coronary angiography have had previous CABG surgery. In such patients, the radial access route was associated with lower procedural success than the femoral route but also a lower rate of bleeding complications.
September 2019 Br J Cardiol 2019;26:119 doi:10.5837/bjc.2019.031
Primary meningococcal Y pericarditis with pericardial effusion resulting in cardiac tamponade
Nicolas Buttinger, Mark Forde, Timothy Williams, Sally Curtis, James Cockburn

We describe a case of primary meningococcal Y effusive pericarditis in a previously fit and well 35-year-old man who presented with a rapidly developing pericardial effusion resulting in cardiac tamponade. This is a rare, but important, cause of primary pericardial disease, and only the fourth documented case of primary meningococcal pericarditis due to Neisseria meningitidis serotype Y. Our patient was successfully treated with a pericardial drain and intravenous ceftriaxone. Our case highlights the importance of adverse clinical features such as temperature >38°C, subacute course, large effusion or tamponade, and non-steroidal anti-inflammatory drug (NSAID)/aspirin failure, which can identify patients who require close observation as they are at higher risk of complications.
July 2019 Br J Cardiol 2019;26:110–3 doi:10.5837/bjc.2019.024
A simple technique for IMA graft angiography and PCI using contralateral radial access
Matthew E Li Kam Wa, Pitt O Lim

Angiography of internal mammary artery (IMA) grafts continues to be a common indication for upfront femoral access. This is particularly the case for bilateral pedicled IMAs, or when the left radial artery has been grafted. While the right radial artery is ideally suited in these situations for cannulation of the right IMA, accessing the left IMA (LIMA) by this route is often perceived as challenging and for ‘radial evangelists’ only. We describe a case series showing a simple technique for selective cannulation of the LIMA from the right radial artery using a single catheter that provides sufficient backup for percutaneous coronary intervention (PCI).
July 2019 Br J Cardiol 2019;26:101–4 doi:10.5837/bjc.2019.025
Managing gastrointestinal manifestations in patients with PoTS: a UK DGH experience
Jeremy S Nayagam, Viral A Sagar, Maxwell Asante

Gastrointestinal (GI) symptoms are common in patients with postural orthostatic tachycardia syndrome (PoTS). Our understanding of managing GI symptoms in PoTS is very limited. Our objectives were to evaluate common GI symptoms, diagnostic work-up, diagnosis and management strategy in patients with PoTS.
We retrospectively reviewed medical records of all patients referred to the gastroenterology clinic (2014 to 2017) with GI symptoms and known or suspected PoTS: 85 patients with PoTS and GI symptoms were seen in our clinic. Bloating (75%), constipation (74%) and abdominal pain (60%) were the most common GI symptoms. Endoscopy, high-resolution manometry, gastric-emptying studies and colonic-transit studies were commonly performed investigations. Over two-thirds of patients had confirmed or suspected GI dysmotility, 5.9% had organic GI disease (e.g. inflammatory and acid peptic disorders).
In conclusion, the majority of patients with PoTS have a functional disturbance and reduced GI motility, however, a small proportion have organic disease that needs systematic evaluation. Dietary modifications and laxatives are the main modalities of therapy.
July 2019 Br J Cardiol 2019;26:92–6 doi:10.5837/bjc.2019.026
Identifying prognostically significant CAD in end-stage renal disease patients
Subodh R Devabhaktuni, Ali O Malik, Ji Won Yoo, Xibei Liu, Vipul Shah, Syed I Shah, John M Ham, Bejon T Maneckshana, Jimmy Diep, Chowdhury H Ahsan

False-negative results either from balanced ischaemia or from failure to induce optimal hyperaemia is a known limitation of vasodilator myocardial perfusion imaging (MPI). We sought to identify the prevalence of false-negative results in the kidney transplant population and to identify the risk factors predictive of false-negative MPI results at our institution.
We retrospectively studied 133 consecutive patients who were referred to us for pre-operative evaluation. Mean age was 56 years and 70% of the subjects were males. All patients who underwent vasodilator MPI and computed tomography coronary angiography (CTCA) were included.
In the studied population, false-negative vasodilator MPI test result prevalence was around 13%. In uni-variable and multi-variable analysis, diabetes and cardiovascular disease (CVD) were predictive of false-negative vasodilator MPI testing results. CTCA had a positive-predictive value (PPV) of 82%.
In conclusion, false-negative results, either from balanced ischaemia or from failure to induce optimal hyperaemia, are a major problem in the pre-operative evaluation of renal transplant patients when the vasodilator MPI test is used. CTCA could be a useful imaging modality in this patient population. We found that diabetes and CVD are significantly associated with false-negative MPI results.
July 2019 Br J Cardiol 2019;26:120 doi:10.5837/bjc.2019.027
Congenital absence of the right pericardium: managing patients long term
Jenny McKeon, Richard Mansfield, Mark Hamilton, Benjamin J Hudson

Absence of the pericardium is a rare defect that can be both congenital and acquired. Defects occur through abnormal development of the pleuro-pericardial membranes, which should fuse at the midline and separate the pericardial and pleural cavities.1 Congenital incidence is thought to be less than one in 10,000,2 however, prevalence is uncertain due to the incidental findings of many diagnoses. With increasing use of cardiac magnetic resonance imaging (CMR) and cardiac computed tomography (CT), diagnosis of pericardial absence is becoming more frequent, however, little is known about the long-term management of these patients.
May 2019 Br J Cardiol 2019;26:59–62 doi:10.5837/bjc.2019.018
Rapid rule-out of NSTEMI: clinical characteristics and outcome of patients with undetectable troponin
Sally Youssef, Mariam Ali, Kim Heathcote, Alistair Mackay, Chris Isles

Studies have suggested that acute coronary syndrome (ACS) may be excluded by a single undetectable high-sensitivity troponin (hs-TnT) taken at least three hours after the onset of symptoms in patients with non-pleuritic chest pain whose electrocardiogram (ECG) is non-ischaemic.
During a six-month period between April and September 2015, we identified 147 consecutive patients with non-pleuritic chest pain and non-ischaemic ECG whose first hs-TnT was less than 5 ng/L at least three hours after the onset of symptoms. We used the Elecsys hs-TnT assay, which has a lower limit of detection of 5 ng/L and a 99th centile of <14 ng/L.
Sixty-seven of 147 (46%) patients were male. The average age of our cohort was 52 years, range 19–83 years. Coronary heart disease (CHD) was known to have been present in 24 (16%) before the index admission. Median length of hospital stay was 15.4 hours (mean 22.5 hours) with 86 (59%) patients spending more than 12 hours in hospital. We referred 60 (41%) patients to cardiology for further assessment, either during or after admission, in order to rule out unstable angina. No patient was readmitted with hs‑TnT positive ACS, one patient underwent elective revascularisation and no patient died during one year of follow-up. Only one patient was lost to follow-up.
In conclusion, patients with non-pleuritic chest pain, non-ischaemic ECG and undetectable hs-TnT at least three hours after the onset of symptoms have a low risk of hs-TnT positive ACS, revascularisation and death during one year of follow-up. Most such patients could safely be discharged from hospital after a few hours of observation, without the need for a second hs-TnT.
May 2019 Br J Cardiol 2019;26:63–6 doi:10.5837/bjc.2019.019
Use of Frailsafe criteria to determine frailty syndrome in older persons admitted with decompensated HF
Janine Beezer, Titilope Omoloso, Helen O’Neil, John Baxter, Deborah Mayne, Samuel McClure, Janet Oliver, Zoe Wyrko, Andy Husband

Frailsafe was developed by the British Geriatrics Society as clinical criteria to accurately identify patients at risk of frailty-associated harm on admission to hospital. There is no single validated tool for assessing frailty in heart failure on admission to hospital. The aim is to determine the prevalence of frailty-associated harm and the outcomes of older persons admitted to hospital with decompensated heart failure using Frailsafe screening criteria.
A retrospective cohort study of consecutive patients aged 75 years and over, admitted to hospital with decompensated heart failure within a six-month period was performed. Frailsafe screening criteria were applied to each patient retrospectively and data on length of stay, inpatient mortality, six-month mortality and readmission at six months was collected for all patients. The outcomes were analysed using univariate analysis comparing the patients ‘at risk of frailty-associated harm’ with those ‘not at risk’.
There were 103 patients identified as 75 years or older and admitted with a primary diagnosis of heart failure, 27% (28) were identified as at risk of frailty-associated harm. This cohort had a significantly longer length of stay (3.5 days, p=0.0496), worse six-month mortality (57% vs. 33%, p=0.0274) and more frequent emergency readmissions (2.04 vs. 0.97, p=0.0031).
In conclusion, prevalence of patients at risk of frailty-associated harm measured by Frailsafe in an older population admitted with decompensated heart failure was 27%. Such patients had a longer length of stay, and were at increased risk of readmission and mortality within the following six months. Future research should include analysis of confounding variables, such as comorbidity, in a larger population to aim to identify how to improve outcomes in this particularly high-risk group.
May 2019 Br J Cardiol 2019;26:67–8 doi:10.5837/bjc.2019.020
Incidence and epidemiology of infective endocarditis from 2010 to 2017 in a rural UK hospital
Laura A Hughes, Andrew Epstein, Neeraj Prasad

Infective endocarditis (IE) is an increasingly common disease associated with significant morbidity and mortality. It is known that the incidence of IE has been rising globally, but the reasons for this rise are not fully understood. This study sought to investigate the epidemiology of IE in a UK population, with a review of mortality outcomes based on current clinical practice.
May 2019 Br J Cardiol 2019;26:69–71 doi:10.5837/bjc.2019.021
What are we?* The BMI should accept terms for a graceful retirement
*with apologies to The Bunyip of Berkeley’s Creek
Michael E J Lean, Thang S Han

Body mass index (BMI) was first proposed in 1835 as a way to standardise body composition assessment for people of different heights, at a time when malnutrition was the main public health concern. BMI has been considered appropriately as a part of nutritional assessment in populations. It is not, however, a useful tool for assessment of individuals because there is so much individual variability in body composition and in its impact on health outcomes. Similarly, high BMI does not distinguish between excess body fat (bad for health) and large muscle mass (good). In contrast, we propose that individuals need to be assessed using clinical criteria, monitored over time to trigger different interventions. A diagnosis of obesity should be based on estimates of body fat (BMI, now being replaced by percentage body fat) at a particular age, and a clinical staging system.
May 2019 Br J Cardiol 2019;26:72–5 doi:10.5837/bjc.2019.022
Practical basics of coronary physiology
Max B Sayers, Cristopher M Cook, Takayuki Warisawa, Justin E Davies

Coronary physiology is the collective term for a group of indexes aimed at directly measuring the intracoronary haemodynamic changes that occur across a stenosis in order to guide revascularisation decision-making. Fractional flow reserve (FFR) uses pharmacological dilatation and miniaturised pressure-wires to measure coronary pressure proximal and distal to a stenosis, thereby estimating flow reduction across a stenosis. Several clinical trials have shown that FFR-guided revascularisation improves clinical outcomes, and that deferring revascularisation in patients shown by FFR to have non-haemodynamically significant lesions is safe. Instantaneous wave-free ratio (iFR) is a novel technique that measures the ratio of distal coronary to aortic pressure during a specific period in diastole that obviates the need for pharmacological vasodilatation. Recent randomised-controlled trials have shown iFR to be non-inferior to FFR with respect to major adverse cardiac events, while reducing adverse procedural symptoms and procedure duration.
April 2019 Br J Cardiol 2019;26:53–8 doi:10.5837/bjc.2019.012
Safety, effectiveness and quality of nurse diagnostic coronary angiography
Ghazala Yasin, Mark Davies, Piers Clifford, Soroosh Firoozan

Advanced nursing roles supported by competency-based training have been pioneered over the last 25 years, with emphasis on the development of specific medical skills. This has largely been influenced by increasingly complex medical needs, costs of healthcare and the significant reduction in available doctors. With this reduction of doctors in training and departmental support for expanding nursing roles, we devised a local initiative to train an experienced nurse to perform diagnostic coronary angiography. Our aim was to provide a safe and enhanced service and improve procedural efficiency within the cardiac day unit.
A prospective audit of 250 coronary angiography procedures was performed in the training period between 24 September 2014 and 9 October 2015. Post-training, 143 procedures were performed between 12 October 2015 and 20 July 2016. The prospective audit was performed to explore the safety, effectiveness and quality of nurse-delivered diagnostic coronary angiography. An audit form was created to assess each component of the procedure. This included, gaining patient consent, success in gaining arterial access, success in intubating the left and right coronary arteries, observation of haemodynamics, observation of complications and reporting the findings. Financial impact, patient satisfaction and staff perception outcomes were also audited.
When directly compared with contemporaries, nurse-delivered diagnostic coronary angiography resulted in successful and appropriate arterial access, successful intubation of both coronary arteries, safe monitoring throughout the procedure and correct reporting of each study, with a similar level of patient satisfaction.
In conclusion, this study demonstrates that nurses can, under the right supervision and governance, perform diagnostic coronary angiography to a safe, highly effective standard, which is equivalent to contemporaries.
April 2019 Br J Cardiol 2019;26:97–8 doi:10.5837/bjc.2019.015
Avoiding needless deaths in aortic stenosis
John B Chambers

Echocardiography is key for the assessment of aortic stenosis (AS), but taking a good history is also crucial and requires specialist competency. Symptomatic AS requires surgery and, if physicians miss the onset of symptoms, the risk of death rises from 1% per annum in patients without symptoms to 14% on a six-month surgical waiting list. A case is described illustrating the difficulty of obtaining the history in a patient with AS, and suggests how to take a careful history and questions to ask. Patients with a murmur suggesting AS should be considered for a specialist valve clinic.
April 2019 Br J Cardiol 2019;26:76–8 doi:10.5837/bjc.2019.016
Fatal anaphylaxis following teicoplanin administration during pacemaker implantation
Michael Chapman, Andrew Turley, Thanh Phan, Nicholas Linker

Over 50,000 cardiac implantable electronic device procedures are undertaken annually in the UK. Despite prophylactic measures, device infection still occurs. Anaphylaxis following teicoplanin is extremely rare with evidence limited to case reports and one case series. We present two fatal cases of anaphylaxis following teicoplanin administration. Both cases meet the World Allergy Organisation definition of anaphylaxis. These cases highlight the importance of anaphylaxis to teicoplanin as a procedural complication. Despite prompt treatment, this reaction was fatal. Operators should be aware of this risk in an era of increasing procedures and rising incidence of anaphylaxis.
April 2019 Br J Cardiol 2019;26:79–80 doi:10.5837/bjc.2019.017
An unusual cause of pericardial tamponade in pregnancy
Bishav Mohan, Hasrat Sidhu, Rohit Tandon, Rajesh Arya

Pericardial involvement is sporadic during pregnancy. We present the case of a young woman who presented to the emergency department with a short history of rapidly progressive dyspnoea in her 38th week of pregnancy. Coronary arteriovenous fistula (CAVF) has been uncommonly described as a cause of pericardial effusion. We believe this is a rare case of a CAVF presenting as cardiac tamponade in pregnancy.

February 2019 Br J Cardiol 2019;26:23–6 doi:10.5837/bjc.2019.007
Non-prescription of anticoagulants in patients discharged with stroke and atrial fibrillation
Calum Creaney, Karissa Barkat, Christopher Durey, Susan Gallagher, Linda Campbell, Ashish MacAden, Paul Findlay, Gordon F Rushworth, Stephen J Leslie

Atrial fibrillation (AF) increases stroke risk fivefold. Oral anticoagulation (OAC) with warfarin reduces the risk of stroke by 64%. Direct oral anticoagulants are non-inferior to warfarin in preventing stroke in non-valvular AF, but have a lower risk of fatal intracranial haemorrhage. We determined how many patients discharged with a diagnosis of ischaemic stroke and AF were prescribed OAC, and established reasons for, and associations with, non-prescription of OAC.
All patients discharged with a diagnosis of ischaemic stroke and AF during the four-year period between 2013 and 2016 within NHS Highland were included in the study. Patients who started OAC after a period of treatment with antiplatelets were considered as being treated with OAC. Electronic patient records provided demographics, CHA2DS2-VASc and HAS-BLED scores and information on why patients were not started on OAC.
A total of 181 patients were discharged with a diagnosis of ischaemic stroke and AF over the study period: 52.5% (n=95) were female (p=0.45); 35.4% (n=64) were discharged without OAC. The median CHA2DS2-VASc score for patients not treated with OAC was 5 (interquartile range [IQR] 4–6). The median HAS-BLED score was 3 (IQR 2.5–4). There was no difference in rate of OAC prescription between men and women (67% vs. 62%, p=0.45). Patients 80 years of age or older were significantly less likely to be prescribed OAC on discharge than those under 80 years (54% vs. 76%, p=0.002). The two most common reasons for withholding OAC were concern over bleeding risk and falls. Patients treated at a hospital with a stroke unit were no more likely to be discharged on OAC compared with those treated at hospitals without a stroke unit (66% vs. 62%, p=0.64). Of patients not treated with OAC, 64% (n=41) were discharged on long-term antiplatelet drugs.
In conclusion, raising awareness of the relatively low risk of major bleeding, even in elderly patients and in those at risk of falls, might help increase OAC usage and reduce recurrent strokes.
February 2019 Br J Cardiol 2019;26:34 doi:10.5837/bjc.2019.008
Is six weeks too long for the first outpatient review after cardiac surgery? FORCAST6
Dumbor L Ngaage, Michael R Gooseman, Kerry L Bulliment, Martin A Jarvis, Mubarak A Chaudhry, Alexander R Cale, Michael E Cowen

The traditional practice of conducting the first outpatient review six weeks after cardiac surgery is not evidence-based. This study was designed to determine mortality and morbidity in the interval between hospital discharge and the first outpatient follow-up.
We enrolled patients undergoing non-emergency cardiac surgery from June 2016 to May 2017 into this prospective observational study. Prior to hospital discharge, patients were consented and given a questionnaire to document attendance at any healthcare facility. Ethical approval was obtained from the Health Research Authority.
The mean age of the 72 study patients was 68 ± 4 years. The majority underwent coronary artery bypass grafting (56.9%). The six-week postoperative morbidity rate was 38.9% and hospital readmission 15.3%. Morbidity, highest in the first week after discharge, declined to its lowest level by four weeks. Surgical site (13.9%) and respiratory complications (13.9%) were predominant causes of late morbidity. There was no mortality. Most patients (50%) expressed satisfaction with current practice, but a significant number (44.4%) would prefer earlier review.
In conclusion, morbidity during the six-week wait for the first outpatient review after cardiac surgery is not insignificant, but declines over time. Current practice does not seem to enable a positive specialist influence of the post-surgery recovery pathway.
Clinical Trials.gov registration number: NCT02832427

February 2019 Br J Cardiol 2019;26:31–3 doi:10.5837/bjc.2019.009
The future of atrial fibrillation: does the answer lie in ablation or anti-arrhythmics?
Mark T Mills

Anti-arrhythmic drugs and pulmonary vein isolation (with radiofrequency ablation) are established treatment options in the management of atrial fibrillation. Both methods have their advantages and drawbacks. Atrial fibrillation is the consequence of complex systemic and atrial factors, resulting in atrial remodelling. Emerging treatment strategies that target and reverse atrial remodelling may offer a promising alternative to anti-arrhythmics and ablation.
February 2019 Br J Cardiol 2019;26:38–40 doi:10.5837/bjc.2019.011
Coronary vasospasm and concurrent Takotsubo cardiomyopathy
Anthony Brennan, Heath Adams, John Galligan, Robert Whitbourn

Takotsubo cardiomyopathy (TTC) is characterised by transient left ventricular dysfunction accompanied by apical ballooning of the ventricle. Takotsubo pathophysiology is poorly understood and is often triggered by an emotional or physical stressor. This is a case of a 71-year-old woman who presented with sudden-onset exertional chest pain leading to inferior ST-elevation on electrocardiography (ECG) with a significant troponin rise. Immediate coronary angiography revealed a severe mid-posterior left ventricular (PLV) branch of the right coronary artery stenosis. The left coronary system was normal. Left ventriculogram revealed mid-to-apical ballooning typical of TTC. Considering the disconnect between the coronary and ventriculogram findings, a decision was made to delay percutaneous coronary intervention (PCI). The patient was treated with heart failure medications and symptoms improved. Repeat angiogram of the mid-PLV after a short period of medical therapy revealed no coronary lesion and the left ventricular function had normalised. These findings suggest that coronary artery vasospasm may have contributed to the aetiology in this case of TTC. This case adds weight to previous theories of an interplay between TTC and coronary vasospasm.

January 2019 Br J Cardiol 2019;26:14–8 doi:10.5837/bjc.2019.002
A survey of post-cardiac rhythm device implantation: movement and mobilisation advice in the UK
George Collins, Sarah Hamill, Catherine Laventure, Stuart Newell, Brian Gordon

Movement restrictions are given to patients after cardiac rhythm device implantation, despite little consensus, or evidence that they reduce complications. We conducted a UK survey assessing the nature of the advice and if it varies between individuals and institutions. A survey was distributed to cardiac rhythm teams at UK implanting centres. Questions concerned the advice that is given, its source, and who is responsible for providing it.
There were 100 responses from 42 centres. Advice is given by physiologists, nurses, and cardiologists. Advice comes from local protocols, information leaflets, current hospital opinion, manufacturers, national leaflets, published research and audit data. Within and between centres there was little agreement on what the advice should be. Depending on who gives the advice, a number of leisure pursuits were either completely unrestricted or restricted indefinitely. Cardiologists were less restrictive than others.
In conclusion, this is the first UK survey to assess the movement and mobilisation advice given to patients after device implantation. There is variation in the source and nature of advice. Over-restriction could impact on patients’ quality of life. Contradictory advice could cause uncertainty. Further work should determine the impact of this variation and how the effects could be safely mitigated.
January 2019 Br J Cardiol 2019;26:19–22 doi:10.5837/bjc.2019.003
ICMs can be routinely implanted in a non-theatre environment by a cardiac physiologist
Varun Sharnam, Stelios Iacovides, Luisa Cleverdon, Wasing Taggu, Philip Keeling

Implantable cardiac monitors (ICMs), also known as implantable loop recorders (ILRs), are used for long-term heart rhythm monitoring of unexplained syncope or in the detection of arrhythmias. These devices are implanted by cardiologists within a cardiac catheter suite environment. The newer generation devices are miniaturised and inserted using a specific tool kit via a minimally invasive procedure. This paper describes the changes we have made to allow these devices to be implanted in a non-theatre environment by a cardiac physiologist and the benefits and cost reduction of this service redesign.
A cardiac physiologist (LC, Band 6) undertook specific training beginning in September 2015. A standard operating procedure (SOP) was developed and patient information videos were commissioned. The new service was introduced in September 2016 in the screening room of our critical care unit (CCU). Data were collected prospectively on the clinical outcome, patient satisfaction and costs.
Over a 13-month period LC independently performed 116 procedures (113 Medtronic Reveal LINQ™ ICMs and 3 St. Judes SJM CONFIRM™) with only one minor complication. Patients were highly satisfied with the redesigned service, which showed a reduction in cost of £241.27 per case.
ICMs/ILRs can be implanted safely and cost-effectively outside a cardiac catheter suite environment by a cardiac physiologist. This requires some specific training, a clinical SOP and is supported by use of dedicated patient information videos.
January 2019 Br J Cardiol 2019;26:27–30 doi:10.5837/bjc.2019.004
Outcome of investigations into patients who attended the emergency department due to palpitations
Alexander J Gibbs, Andrew Potter

Previous research estimates that up to 40% of palpitation presentations to the emergency department (ED) have cardiac aetiology. This study was performed to determine the proportion of patients referred on for cardiology investigations that consequentially had new significant pathology diagnosed; and the effect of follow-up investigation on patient re-attendance to the ED with the complaint of palpitations.
Patients referred to a community cardiology centre in 2016 for investigation into palpitations following an ED presentation were included. The diagnosis that each patient received from these investigations was analysed to see whether: (a) new underlying cardiac abnormality was identified and (b) that abnormality was significant, requiring follow-up.
There were 93 patients meeting criteria for analysis: 28% had a cardiac cause for their palpitations elicited, including 11% with new significant pathology identified. Rate of re-attendance to the ED was reduced once cardiology investigations were completed (0.11 presentations/patient; 95% confidence interval [CI] 0.04 to 0.18) compared with the investigation period (0.75 presentations/patient; 95%CI 0.3 to 1.2).
In conclusion, although only one tenth of patients referred for investigations had new significant cardiac pathology identified, completing cardiology investigations reduced ED re-attendance.
January 2019 Br J Cardiol 2019;26:35 doi:10.5837/bjc.2019.005
Association of subclinical hypothyroidism in heart failure: a study from South India
Pramod Kumar Kuchulakanti, VCS Srinivasarao Bandaru, Anurag Kuchulakanti, Tallapaneni Lakshumaiah, Mehul Rathod, Rajeev Khare, Parsa Sairam, Poondru Rohit Reddy, Athuluri Ravikanth, Avvaru Guruprakash, Regalla Prasada Reddy, Banda Balaraju

Recent studies have associated subclinical hypothyroidism with heart failure (HF) and increased mortality. To investigate the relationship between subclinical hypothyroidism and HF in Indian patients we prospectively recruited 350 HF patients between March 2013 and February 2017 at the department of cardiology Yashoda Hospital, Hyderabad, India. All patients underwent fasting serum glucose, lipid profile, N-terminal-pro-brain natriuretic peptide (NT-proBNP), and thyroid hormone levels. Risk factors and clinical evaluation were undertaken. We divided thyroid-stimulating hormone (TSH) levels into severity grade 1 (≤9.9 mIU/L) and grade 2 (≥10 mIU/L).
Out of 350 HF patients, 191 (54.5%) were men, mean age was 60.4 ± 10.2 years (range 36–85 years). The incidence of subclinical hypothyroidism was 18.5%, 69.4% had normal thyroid function, and 12% had overt hypothyroidism. Mean NT-proBNP levels were 3561 ± 5553 pg/mL and 10.5% suffered in-hospital mortality. Dyslipidaemia (p=0.004), elevated NT-proBNP levels (p<0.0001) and mortality (p<0.0001) were significantly associated with subclinical hypothyroidism compared with euthyroidism. After multi-variate analysis, hypertension (odds ratio [OR] 3.5; 95% confidence interval [CI] 2.32, 3.8), dyslipidaemia (OR 1.7; 95%CI 1.12, 2.8), subclinical hypothyroidism (OR 1.39; 95%CI 0.99, 1.82) and NT-proBNP >600 pg/mL (OR 1.98; 95%CI 1.23, 2.04) were significantly associated with HF. Grade 2 TSH (OR 4.16; 95%CI 2.04, 8.48), elevated NT-proBNP >1800 pg/mL (OR 2.18; 95%CI 1.53, 4.82), and severe left ventricular dysfunction (OR 2.51; 95%CI 1.24, 2.07) were significantly associated with poor outcome.
In conclusion, our study has established that subclinical hypothyroidism is associated with HF and grade 2 TSH has an independent association with in-hospital mortality in Indian patients.
January 2019 Br J Cardiol 2019;26:36–7 doi:10.5837/bjc.2019.006
Significant suppression of premature ventricular ectopics with ivabradine in dilated cardiomyopathy
Lal H Mughal, Andrew R Houghton, Jeffrey Khoo

Ivabradine is an I(f)-channel blocker currently used for the treatment of angina and heart failure. Although these channels are known to be found within the sino-atrial node, recent studies have also found localisation within the ventricular myocardium, and there have been reports of ventricular arrhythmia suppression in animal models. We describe an unusual case of significant ventricular ectopy suppression in a patient with non-ischaemic dilated cardiomyopathy. This was accompanied by a significant improvement in percentage pacing from her cardiac resynchronisation device, with corresponding improvement in her functional status. This report suggests, first, that the morbidity and mortality benefit of ivabradine in heart failure may not be solely due to its sino-atrial heart-rate lowering effect, and, second, highlights a potential role for ivabradine in the management of ventricular arrhythmias, which requires further studies to substantiate.
December 2018 Br J Cardiol 2018;25:140–2 doi:10.5837/bjc.2018.031
Quality of life in postural orthostatic tachycardia syndrome (PoTS): before and after treatment
Toby Flack, Jamie Fulton

Postural orthostatic tachycardia syndrome (PoTS) can be defined as tachycardia with or without hypotension in the upright posture, and more comprehensively as a manifestation of a wider dysautonomia. The scope of this article is to characterise patients with PoTS and look at patient-rated responses to treatment.
This research comprised a postal survey, sent to patients with diagnosed PoTS at a tertiary hospital in Southwest England. We collected data on the demographics of patients, time to diagnosis, methods of diagnosis, treatments and response to treatment.
PoTS has an impact on quality of life, with patients communicating a drop in quality of life from 7.5 to 3.75 on a 10-point scale. From 40 respondents, 29 patients describe their symptoms improving since diagnosis, with self-rated day-to-day function improving from 3.21 to 6.14 (on a 10-point scale) after initiating treatment.
Many patients experience a delay in receiving a diagnosis with PoTS, and present multiple times to a variety of healthcare professionals. With a simple bedside diagnostic test (sitting and standing heart rate), there is scope to improve the time taken from developing initial symptoms to diagnosis, treatment and an improvement in quality of life.

December 2018 Br J Cardiol 2018;25:152–6 doi:10.5837/bjc.2018.032
Thrombus aspiration in primary percutaneous coronary intervention: to use or not to use?
Telal Mudawi, Mohamed Wasfi, Darar Al-Khdair, Muath Al-Anbaei, Assem Fathi, Nikolay Lilyanov, Mohammed Elsayed, Ahmed Amin, Dalia Besada, Waleed Alenezi, Waleed Shabanh

Thrombus aspiration during primary percutaneous coronary intervention (PCI) has been extensively studied. Conflicting results have consistently emerged, hence, no clear guidance has been produced. The authors have examined several key clinical trials and meta-analyses, and discovered, arguably, major flaws within the designs of most trials, thus, accounting for the persistently discordant results. The authors conclude that there is some evidence to support the selective use of thrombectomy in primary PCI but a large-scale trial with the appropriate patient selection criteria is needed in order to substantiate or refute the argument.
December 2018 Br J Cardiol 2018;25:159–60 doi:10.5837/bjc.2018.033
Percutaneous endovascular repair of congenital interruption of the thoracic aorta
Richard Armstrong, Kevin Walsh, David Mulcahy

Presentation of an interrupted aortic arch in adulthood is rare, and, up until, recently the only treatment strategy was through surgical repair. Advances in percutaneous interventions for congenital heart disease have included the percutaneous repair of coarctation of the aorta – from straightforward luminal narrowing through to full aortic interruption.1-3 We present a case of a 28-year-old man who was diagnosed with a complete aortic interruption and successfully percutaneously treated.
October 2018 Br J Cardiol 2018;25:147–9 doi:10.5837/bjc.2018.026
Transitions of an open-heart surgery support lab in a resource-limited setting: effect on turnaround time
Ijeoma Angela Meka, Williams Uchenna Agu, Martha Chidinma Ndubuisi, Chinenye Frances Onyemeh

Open-heart surgery is a major surgical procedure that requires intensive patient monitoring. Clinicians require prompt laboratory test results to assist them in this monitoring. Timeliness of result delivery is of great importance in taking prompt clinical decisions. We set out to evaluate the performance of the support laboratory before and after domiciliation at the cardiac centre using turnaround time (TAT) of electrolytes and liver function tests as benchmarks.
This hospital-based descriptive study was carried out at the University of Nigeria Teaching Hospital (UNTH), Enugu. The authors conducted a desk review of laboratory records for electrolytes and liver function tests from March 2013 to July 2017. Relevant laboratory personnel were also interviewed to ascertain types of equipment used and possible causes of delay at different stages of transition during the period under review. The TAT was calculated as the time from sample reception to time of dispatch of results.
Between 2013 and 2014, TAT for electrolytes and liver function tests were ~2 and ~6 hours, respectively. In 2015, TAT reduced to ~1 hour for electrolytes and ~1½ hours for liver function tests. Between 2016 and July 2017, TAT further reduced to ~10 minutes for electrolytes and ~30 minutes for liver function tests.
In conclusion, we were able to demonstrate improvement in performance of the support laboratory as shown by a reduction in TAT following the transition from the main laboratory to being domiciled in the cardiac centre.

October 2018 Br J Cardiol 2018;25:150–1 doi:10.5837/bjc.2018.027
Utility of MPS in AAA repair and prognostication of cardiovascular events and mortality
Mark G MacGregor, Neil Donald, Ayesha Rahim, Zara Kwan, Simon Wong, Hannah Sharp, Hannah Burkey, Mark Fellows, David Fluck, Pankaj Sharma, Vineet Prakash, Thang S Han

Myocardial perfusion scintigraphy (MPS) is a non-invasive method that can be used to assess reversible left ventricular myocardial perfusion defect (<20% indicates limited and ≥20% indicates extensive ischaemia), and left ventricular ejection fraction (LVEF) at rest and at stress. Data on the utility of MPS used to stratify cardiac risk prior to abdominal aortic aneurysm (AAA) repairs are limited. We evaluated MPS as a stratification tool for patients scheduled for endovascular aneurysm repair (EVAR) or open repair, between 2013 and 2016 at Ashford and St Peter’s NHS Foundation Trust, and 4.9 years (median 2.8 years, interquartile range [IQR] 2.1–3.8) cardiovascular events (n=15, 17.9%) all-cause mortality (n=17, 22.6%). Of the 84 patients recruited (median age 75.7 years, IQR 69.4–79.6), 57 (67.9%) had limited and 27 (32.1%) extensive ischaemia, 62 (73.8%) underwent EVAR and 22 (26.2%) open repair. Compared with open repair patients, EVAR patients were older (median age 70.6 years vs. 76.4 years, p=0.015), had higher rates of extensive ischaemia (13.6% vs. 38.7%, p=0.025), and abnormal LVEF reserve (LVEF at stress minus LVEF at rest ≤0: 40.0% vs. 76.6%, p=0.011), while having lower rates of 30-day postoperative major adverse cardiac events (13.6% vs. 3.3%, p=0.040) but no difference for cardiovascular events (p=0.179) or 4.9 year all-cause mortality (22.7% vs. 22.6%, adjusted hazard ratio 0.80, 95% confidence interval [CI] 0.22 to 3.20, p=0.799). Our findings indicate that MPS provides valuable information for AAA repair procedure.
October 2018 Br J Cardiol 2018;25:143–6 doi:10.5837/bjc.2018.028
New-onset giant T-wave inversion with prolonged QT interval: shared by multiple pathologies
Debjit Chatterjee, Priya Philip, Kay Teck Ling

This is a case series of 10 patients who presented with the same electrocardiogram (ECG) manifestation of new-onset giant T-wave inversion and QT prolongation over a period of 24 months in a district general hospital. This unique ECG manifestation has been described with several cardiac and non-cardiac conditions.
October 2018 Br J Cardiol 2018;25:157–8 doi:10.5837/bjc.2018.029
A case report of transient acute left ventricular dysfunction
Allam Harfoush

Stunned myocardium is a rare, but serious, medical condition, and requires emergency intervention. Short periods of hypoperfusion may lead to a prolonged cardiac hypokinesia (hours to days), even though the perfusion is retained eventually. In other words, although the coronary circulation is retained, the hypokinesia remains. It might be considered as a case of prolonged post-ischaemic dysfunction.
In this case, a 60-year-old woman, visiting her siblings, presented with severe dyspnoea and cyanosis to the emergency department. Pulmonary oedema was diagnosed, and transthoracic echocardiography (TTE) showed general hypokinesia and reduced ejection fraction (15%), nevertheless, sequential TTE monitoring after the required medical intervention revealed a continuous improvement, with a 45% ejection fraction three days later and a specific anterior wall hypokinesia, solely.
In conclusion, rapid diagnosis and treatment are essential for stunned myocardium, as these could change the progress of the clinical condition.
August 2018 Br J Cardiol 2018;25:86–7 doi:10.5837/bjc.2018.024
Artificial intelligence in cardiology: applications, benefits and challenges
Panos Constantinides, David A Fitzmaurice

The introduction of such digital technologies as robotic implants, home monitoring devices, wearable sensors and mobile apps in healthcare have produced significant amounts of data, which need to be interpreted and operationalised by physicians and healthcare systems across disparate fields.1 Most often, such technologies are implemented at the patient level, with patients becoming their own producers and consumers of personal data, something which leads to them demanding more personalised care.2
This digital transformation has led to a move away from a ‘top-down’ data management strategy, “which entailed either manual entry of data with its inherent limitations of accuracy and completeness, followed by data analysis with relatively basic statistical tools… and often without definitive answers to the clinical questions posited”.3 We are now in an era of a ‘bottom-up’ data management strategy that involves real-time data extraction from various sources (including apps, wearables, hospital systems, etc.), transformation of that data into a uniform format, and loading of the data into an analytical system for final analysis.3
August 2018 Br J Cardiol 2018;25:97–101 doi:10.5837/bjc.2018.025
Impact of hyperkalaemia in managing cardiorenal patients – a healthcare professional perspective
Navneet Kalsi, Sarah Birkhoelzer, Philip Kalra, Paul Kalra

A recent survey of healthcare professionals confirms that hyperkalaemia is considered as a common and important clinical issue for patients receiving renin-angiotensin-aldosterone-system (RAAS) inhibitors in particular. Successful interventions to manage hyperkalaemia appear beneficial rather than avoidance or dose reduction of these RAAS inhibitors in patients with chronic heart failure, diabetic nephropathy or prior myocardial infarction.
Two newer potassium exchange resins, patiromer and sodium zirconium cyclosilicate (ZS-9), may offer improved predictability, tolerability, and efficacy for managing patients with hyperkalaemia.
July 2018 Br J Cardiol 2018;25:115–7 doi:10.5837/bjc.2018.018
A pulmonary triad in a patient with a giant left atrial myxoma
Andrea Calo, Madeleine Openshaw, Timothy J Bowker, Han B Xiao

A 55-year-old man with suspected community-acquired pneumonia and atrial fibrillation was found to have a very large left atrial myxoma complicated with a pulmonary triad – pulmonary hypertension, pulmonary infarction, and pulmonary lymphadenopathy. The myxoma was successfully removed and complete resolution of all three pulmonary complications followed. He re-presented two weeks post-surgery with atrial flutter, which was medically treated and considered for ablation. We have taken the opportunity to undergo a mini-literature review on myxoma and its pulmonary complications.

July 2018 Br J Cardiol 2018;25:107–9 doi:10.5837/bjc.2018.019
Opinions on the expanding role of CTCA in patients with stable chest pain and beyond: a UK survey
Saad Fyyaz, Alexandros Papachristidis, Jonathan Byrne, Khaled Alfakih

The National Institute for Health and Care Excellence (NICE) released an updated guideline on stable chest pain in 2016. They recommended that all patients with chest pain, typical or atypical, should be investigated with computed tomography coronary angiography (CTCA) in the first instance. Functional imaging tests were reserved for the assessment of patients with chest pain and known coronary artery disease (CAD) and for patients where the CTCA is equivocal or has shown CAD of uncertain significance. The European Society of Cardiology (ESC) guidelines on stable chest pain, however, recommend functional imaging tests for all stable chest pain patients, with CTCA as an alternative in patients with low-to-intermediate likelihood of CAD. The ESC guidelines also allow for the use of the exercise electrocardiogram (ECG) as an alternative to functional imaging tests in patients with low-to-intermediate likelihood of CAD, if functional imaging tests are not available.
Furthermore, traditionally, the aetiology of heart failure or left ventricular (LV) dysfunction was investigated with diagnostic invasive coronary angiography. More recently, cardiac magnetic resonance imaging (MRI) tissue characterisation was proposed as an effective alternative test. We conducted a survey of UK cardiologists’ opinions on the use of CTCA in patients with stable chest pain and in the investigation of the aetiology of heart failure.
July 2018 Br J Cardiol 2018;25:110 doi:10.5837/bjc.2018.020
Comprehensive study of routine clinical use of cardiac MRI in a district general hospital setting
George Abraham, Aamir Shamsi, Yousef Daryani

The study sought to evaluate the indications, image quality, safety and impact on patient management of cardiac magnetic resonance imaging (CMR) in a district general hospital setting. The database was developed using retrospective analysis of patient records from the start of the local CMR service in January 2014 until January 2017. All 791 consecutive patients were included in the dataset.
The most important indications were the investigation of myocarditis/cardiomyopathies (54.5%), work-up of suspected coronary artery disease (CAD)/ischaemia (27.1%), and assessment of viability (9.1%). Image quality was diagnostic in 99.9% of cases. Mild adverse effects were reported for 3.8% of patients for stress CMR and in 1.1% of non-stress CMR. No serious adverse events were reported in this study population. In 26.5% of cases, CMR findings resulted in therapeutic modifications. In 18.1%, the final diagnosis based on CMR was different to that suspected before the CMR.
In conclusion, the findings of this study emphasise that CMR is a safe procedure with high image quality. In many cases, CMR can be shown to change a patient’s management plan.
July 2018 Br J Cardiol 2018;25:111–4 doi:10.5837/bjc.2018.021
Hypertension in pregnancy as the most influential risk factor for PPCM
Hawani Sasmaya Prameswari, Triwedya Indra Dewi, Melawati Hasan, Erwan Martanto, Toni M Aprami

Peri-partum cardiomyopathy (PPCM) is one of the leading causes of maternal mortality worldwide, but the exact cause of PPCM is still unknown. PPCM is often associated with many risk factors, especially hypertension in pregnancy. This study aimed to evaluate the most influential risk factors of PPCM in Javanese ethnic patients.
The study was a case-control study involving 96 PPCM patients and 96 healthy non-PPCM parturients (control group) in the Hasan Sadikin Central General Hospital, West Java, Indonesia in the period from 2011 to 2014. A multiple logistic regression analysis was performed to evaluate the most influential risk factors for PPCM.
There were four significant and independent risk factors in this study, which were low socioeconomic status (adjusted odds ratio [OR] 3.312; confidence interval [CI] 1.383, 7.932), history of hypertension in previous pregnancy (adjusted OR 4.862; CI 1.245, 8.988), hypertension in current pregnancy (adjusted OR 2.311; CI 1.164, 4.590), and multi-foetal pregnancy (adjusted OR 7.057; CI 0.777, 64.097). Multiple logistic regression analysis showed the history of hypertension in previous pregnancy or hypertension in current pregnancy were the most influential independent risk factors of PPCM based on the narrowest confidence interval range, and after adjustment for other significant risk factors.
In this study, history of hypertension in previous pregnancy and hypertension in current pregnancy were the most influential and independent risk factors for PPCM. This study may increase awareness of treatment required for patients with hypertension in pregnancy, and also supports the pathogenesis of hypertension in pregnancy associated with PPCM, especially pre-eclampsia.
July 2018 Br J Cardiol 2018;25:118–20 doi:10.5837/bjc.2018.022
A transitory right bundle branch block
Cristina Aguilera Agudo, Silvia Vilches Soria, Jorge Enrique Toquero Ramos

The clinical presentation of patients with cardiac tamponade largely depends upon the length of time over which pericardial fluid accumulates and the clinical situation. It can result in a clinical picture ranging from cardiogenic shock to general malaise, including dyspnoea, chest discomfort or fullness, peripheral oedema and fatiguability.
Although cardiac tamponade is a clinical diagnosis, two-dimensional and Doppler echocardiography play major roles in the identification of pericardial effusion and in assessing its haemodynamic significance. Despite this, some other imaging techniques or diagnostic tools could also be used for diagnosis. With this case we want to highlight not only the role of the electrocardiogram (ECG), but also its utility in assessing the haemodynamic changes in this clinical entity.

June 2018 Br J Cardiol 2018;25:73–6 doi:10.5837/bjc.2018.016
Prescribing glucose-lowering drugs for patients with cardiac disease
Miles Fisher, Emma Johns, Gerry McKay

The past decade has seen the emergence of several new classes of drugs for the treatment of type 2 diabetes mellitus (T2DM). Despite the increasing use of these agents, metformin and sulfonylureas remain the most commonly prescribed glucose-lowering drugs in people with T2DM. This reflects the National Institute for Health and Care Excellence (NICE) guideline from 2015 and the Scottish Intercollegiate Guidelines Network (SIGN) guideline from 2010, which recommended metformin as first-line treatment and sulfonylureas as the ‘usual’ second-line treatment for patients with T2DM. SIGN has recently provided an updated guideline on the pharmacological management of glycaemic control in people with T2DM. For the first time in UK guidelines, this recommends that in individuals with diabetes and cardiovascular disease, sodium-glucose co-transporter 2 (SGLT2) inhibitors and glucagon-like peptide-1 (GLP-1) receptor agonists with proven cardiovascular benefit (currently empagliflozin, canagliflozin and liraglutide) should be considered. It is anticipated that implementation of these new guidelines will lead to increased prescribing of these drugs in people with diabetes and cardiac disease, with reductions in prescribing of dipeptidyl peptidase-4 (DPP-4) inhibitors and other drugs in the GLP-1 receptor agonist class, where cardiovascular benefits have not been clearly demonstrated.
June 2018 Br J Cardiol 2018;25:77–80 doi:10.5837/bjc.2018.017
‘Normal’ blood pressure: too good to be true? Case series on postural syncope and the ‘white-coat’ effect
Haqeel A Jamil, Noman Ali, Mohammad Waleed, Yvonne Blackburn, Caroline Moyles, Christopher Morley

Ambulatory blood pressure monitoring (ABPM) can confirm diagnosis in essential hypertension (HTN) and mitigate the ‘white-coat’ effect, preventing erroneous antihypertensive therapy. We aimed to collect a case series of over-treated hypertension in the context of ‘white-coat’ effect, resulting in pre-syncopal or syncopal episodes. We collected data retrospectively from patients presenting to syncope clinic between January 2016 and March 2017. ABPM was used at baseline and repeated at three months, following withdrawal of one or more antihypertensive agents.
There were 39 patients with orthostatic symptoms of syncope/pre-syncope, previous HTN diagnosis and ‘white-coat’ effect included. Reducing antihypertensive therapy increased daytime ABPM (baseline vs. three months: systolic 119 ± 11 vs. 128 ± 8 mmHg, p<0.05; diastolic 70 ± 9 vs. 76 ± 9 mmHg, p<0.05) and resolved symptoms.
In conclusion, some patients exhibit pre-syncope or syncope due to over/erroneous HTN treatment resulting in orthostatic hypotension. Our findings suggest that reducing antihypertensive medications may resolve symptoms, without rendering them hypertensive.
May 2018 Br J Cardiol 2018;25:63–8 doi:10.5837/bjc.2018.014
3D echocardiography: benefits and steps to wider implementation
Kevin Cheng, Mark J Monaghan, Antoinette Kenny, Bushra Rana, Rick Steeds, Claire Mackay, DeWet van der Westhuizen

Advancements in computer and transducer technologies over the past two decades have allowed the development of three-dimensional (3D) echocardiography (3DE), which offers significant additional clinical information to traditional two-dimensional (2D) echocardiography (2DE). However, the majority of departmental studies today remain 2D, and adoption of 3DE as a complementary tool into mainstream clinical practice has not been without its difficulties. Although cardiologists have a range of alternative imaging modalities at their disposal to investigate cardiovascular structure and function, given the pace of technological innovation and improvements in data analysis, the field of 3DE is one of great expectation and is likely to be of increasing clinical importance. In this review, we discuss the role of 3DE, its advantages and limitations, and how novel technology will help workflow and expand its routine use.
April 2018 Br J Cardiol 2018;25:69–72 doi:10.5837/bjc.2018.011
The effect of EECP on functional exercise capacity and symptom burden in refractory angina
Noman Ali, Haqeel A Jamil, Mohammad Waleed, Osama Raheem, Peysh Patel, Paul Sainsbury, Christopher Morley

Refractory angina (RA) is characterised by persistent anginal symptoms despite optimal medical therapy and revascularisation. Enhanced external counterpulsation (EECP) is a technique that has shown promise in the treatment of this condition but is poorly utilised in the UK. The aim of this study is to assess the effect of EECP on anginal symptoms in patients with RA from a UK centre.
This retrospective study assessed the effectiveness of EECP at improving exercise capacity, anginal symptom burden and anginal episode frequency using pre- and post-treatment six-minute walk test (6MWT) results, Canadian Cardiovascular Society (CCS) scores and symptom questionnaires, respectively.
Fifty patients with a median age of 67 years (interquartile range [IQR] 14) underwent EECP between 2004 and 2015. The majority had undergone prior revascularisation (84%; 42/50) via percutaneous coronary intervention (PCI) and/or coronary artery bypass grafting (CABG). Significant improvements were noted in 6MWT result (282 vs. 357 m; p<0.01), CCS score (3.2 vs. 2.0; p<0.01) and weekly anginal episode frequency (20 vs. 4; p<0.01). No adverse outcomes related to EECP were noted.
Our study demonstrates use of EECP to be associated with significant improvements in exercise capacity and anginal symptom burden.
April 2018 Br J Cardiol 2018;25:54–7 doi:10.5837/bjc.2018.012
A study in the diagnosis and management of syncope: a retrospective review
Joseph Wilson, Donna Dalgetty, Selda Ahmet, Nida Taher, Mehran Asgari

A study of 500 patients was conducted to ascertain how syncope is managed at the Ipswich Hospital NHS Trust. This was based on the variation in approach across the country despite the guidance from the European Society of Cardiology (ESC), National Institute for Health and Care Excellence (NICE) and the Heart Rhythm Society. Similar studies in the UK have indicated a number of inconsistencies in both the management and diagnosis of patients with suspected syncope.
We discuss the role of a syncope pathway, the need for a separate syncope clinic and for syncope experts.
April 2018 Br J Cardiol 2018;25:58–62 doi:10.5837/bjc.2018.013
A novel ambulatory syncope assessment unit is safe and cost-effective in a low-risk patient cohort
Hamish I MacLachlan, Christopher J Allen, Gothandaraman Balaji

A retrospective analysis of 50 inpatients admitted with syncope was undertaken to evaluate the safety and cost-effectiveness of a novel outpatient syncope clinic recently introduced within an emergency ambulatory care unit at a northwest London hospital together with review of echocardiographic parameters in syncope. Outcome measures included length of inpatient admission, frequency of cardiology review, 30-day readmission and 90-day mortality rates. The same variables were assessed prospectively in 50 inpatients referred to the syncope assessment unit (SAU). All 100 patients were deemed low risk, as defined by the San Francisco syncope rule. Patients under the age of 18 years and those investigated for conditions other than syncope were excluded. Echocardiographic parameters such as E/A ratio, left atrial (LA) dimension, left ventricular (LV) ejection fraction and E/E′ ratio were statistically analysed for their association with episodes of syncope.
The standard-care group remained in hospital for a median four days at a cost of €582 (£512). Waiting time for an SAU appointment was a median two days. Inpatient waiting time for 24-hour Holter and transthoracic echocardiography (TTE) investigations were significantly longer for the standard-care group (p<0.05). There was no significant difference in the rates of cardiology review, diagnostic yield, hospital readmission and mortality between the two groups. The SAU will save a projected annual cost of €108,371 (£95,232) on inpatient bed days. The fractional cost of clinical assessment on the SAU is €35 (£31) per patient. Among the echocardiographic parameters analysed, increased E/E′ ratio was associated with syncope (p=0.001).
In conclusion, the introduction of a novel low-risk SAU promotes early discharge from hospital with prompt outpatient medical review and shorter inpatient waiting times for diagnostic investigations. Our data suggest this is both cost-effective and safe. E/E′ echo parameter was observed as a significant parameter in low-risk syncope.

March 2018 doi:10.5837/bjc.2018.005
Rhythm analysis of direct access 12-lead ECGs in patients complaining of palpitation
Morgan A Hughes, Peter J Bourdillon

Rhythm disturbances in healthy subjects undergoing Holter recording are well described. The purpose of this study has been to determine the frequency of rhythm disturbances, in particular of multi-focal atrial rhythm, on the 12-lead ECG of patients complaining of palpitation presenting to their GP.
There were 500 electrocardiograms (ECGs) studied. Rhythms were categorised as supraventricular rhythm disturbances, ventricular rhythm disturbances, multi-focal atrial rhythm, sinus arrhythmia and sinus rhythm. Multi-focal atrial rhythm was diagnosed either if there were a minimum of two complexes of each of three or more distinct P-wave shapes, none of which were obvious atrial ectopics, or if an ectopic atrial rhythm morphed into an ectopic atrial rhythm from another atrial focus.
Supraventricular rhythm disturbances (8.6%) were more common than ventricular rhythm disturbances (5.2%). Multi-focal atrial rhythm was found in 12.7% of ECGs and sinus arrhythmia in 4.0%. The relative frequency of the rhythms varied significantly with age, but not by gender or by ethnicity.
In conclusion, a quarter of the subjects with palpitation had a rhythm disturbance on a 10-second 12-lead ECG. Multi-focal atrial rhythm should be considered as a potential cause of palpitation.

March 2018 doi:10.5837/bjc.2018.006
Diagnostic utility of real-time smartphone ECG in the initial investigation of palpitations
Anthony D Dimarco, Eunice N Onwordi, Conrad F Murphy, Emma J Walters, Lorraine Willis, Nicola J Mullan, Nicholas S Peters, Mark A Tanner

Palpitations are a common symptom leading to primary care consultation. Establishing a symptom-rhythm correlation is important for providing a diagnosis. The Kardia Mobile personalised smartphone electrocardiogram (ECG) can provide patient-driven real-time ECG recording over extended periods. We investigated if this device might provide an effective alternative to conventional ECG recorders as the first-line investigation of low-risk palpitations.
Patients referred to our institution for investigation of intermittent palpitations but without syncope were supplied with a Kardia Mobile device if they had access to a compatible smartphone. Patients were asked to record an ECG when symptomatic.
Between March 2015 and June 2016, 148 patients were issued with a Kardia Mobile: 113 (76.4%) patients made symptomatic recordings during this period. A symptom-rhythm correlation was possible for all patients who submitted downloads. Median time to diagnosis was nine days (1–287 days). Diagnoses were: sinus rhythm n=47 (41.6%), sinus tachycardia n=21 (18.6%), supraventricular/ventricular ectopics n=31 (27.4%), atrial fibrillation n=8 (7.1%), and supraventricular tachycardia n=6 (5.3%).
In conclusion, the Kardia Mobile diagnosed the cause of intermittent palpitations in the majority of patients referred for specialist evaluation. Use of the Kardia Mobile may permit patients with palpitations to be evaluated in primary care.

March 2018 doi:10.5837/bjc.2018.007
Older antidiabetic drugs
Emma Johns, Gerry McKay, Miles Fisher

In this article we review the latest cardiovascular outcomes trials performed using older diabetes drugs.
March 2018 doi:10.5837/bjc.2018.008
Percutaneous transcatheter closure of the aortic valve to treat aortic insufficiency after LVAD implantation
Wala Mattar, Christopher Walker, Shelley Rahman Haley, Andre Simon, Charles Ilsley

We present a patient with progressive aortic regurgitation that developed following successful implantation of a left ventricular assist device (LVAD). We were able to correct this known complication of LVAD by occluding the aortic valve percutaneously with an AmplatzerTM multi-fenestrated septal occluder – Cribriform. This is the first such case to be reported in the UK.

January 2018 doi:10.5837/bjc.2018.001
Cardio-oncology: a new sub-specialty
Jonathan Bennett, Alexander R Lyon, Chris Plummer, Stuart D Rosen, Kai-Keen Shiu

This review aims to summarise the cardiovascular complications from cancer treatments and the methods used to prevent, identify, and treat them.
While the field of cardio-oncology is relatively new, it is developing rapidly in the UK. There is a need to develop services to care for the patients with current cardiac problems, to undertake research and education to identify those patients at higher risk of complications, and to apply modern imaging methods and biomarkers to detect problems early and implement prevention strategies. An evidence-based approach is required to enhance delivery of care and prevent cardiovascular toxicity in this patient population.
January 2018 doi:10.5837/bjc.2018.002
Variability in use of IV nitrates and diuretics in acute HF: a ‘virtual patient’ clinical decision-making study
Alison Carr, Fosca De Iorio, Martin R Cowie

Despite guidelines on the treatment of acute heart failure (AHF), treatment remains heterogeneous, particularly regarding intravenous (IV) nitrate use. This clinical decision-making study assessed the use of IV nitrates and diuretics by 40 UK hospital physicians, each ‘treating’ the same 10 virtual patients. Semi-structured interviews were performed to investigate participants’ decision-making rationale.
IV nitrates were prescribed in 37% of clinical decisions. Considerable variability was seen in the administration of IV nitrates among physicians. Interview data revealed polarised opinions regarding the efficacy of IV nitrates and the evidence base supporting their use. Physicians’ treatment decisions were more heavily influenced by their perceptions and beliefs regarding IV nitrates than by consideration of the evidence. In contrast, diuretics were prescribed more frequently (78%) and more consistently.
In conclusion, where there is a limited evidence base and no strong recommendation from clinical guidelines, prescribing behaviour for AHF therapies such as IV nitrates are likely to reflect variability in physicians’ beliefs, experiences, and decision-making styles.
January 2018 doi:10.5837/bjc.2018.004
Recognition and management of aVR STEMI: a retrospective cohort study
Ruan Vlok, Joshua Wall, Hannah Kempton, Thomas Melhuish, Astin Lee, Leigh White

Identification of ST elevation on the electrocardiogram (ECG) is the cornerstone of diagnosis of ST-elevation myocardial infarction (STEMI). While lesion localisation can usually be achieved by regional ST-elevation patterns on ECG, clinicians often neglect changes in the ST segment of lead aVR, possibly contributing to delayed recognition and poorer outcomes for these patients.
This study compared the ‘door-to-balloon time’ and peak troponins – as a surrogate marker of infarct size – for patients presenting with STEMI with ST-segment elevation in aVR compared with those patients without elevation in aVR. A total of 179 patients, including 17 patients presenting with ST-elevation in aVR, were included in this study. Patients presenting with elevation in aVR had significantly longer door-to-balloon times than those patients presenting with ‘traditional’ patterns of ST-elevation. There was, however, no significant difference in peak troponin as a marker of infarct size. While patients presenting with ST-elevation in lead aVR may have a delayed time to intervention, the present study does not suggest the use of aVR elevation as an indication for urgent angiography.

November 2017 Br J Cardiol 2017;24:152–5 doi:10.5837/bjc.2017.030
Glucagon-like peptide-1 (GLP-1) receptor agonists
Emma Johns, Gerry McKay, Miles Fisher

Glucagon-like peptide-1 (GLP-1) receptor agonists are an injectable glucose-lowering therapy used in the treatment of type 2 diabetes mellitus (T2DM). Alongside dipeptidyl peptidase-4 (DPP-4) inhibitors, they exert their effect by augmenting the incretin pathway. GLP-1 receptor agonists offer reductions in glycosylated haemoglobin (HbA1c) and weight alongside a low risk of hypoglycaemia. The cardiovascular safety of GLP-1 receptor agonists in patients at elevated cardiovascular risk has been examined in large double-blind, placebo-controlled cardiovascular safety trials. Liraglutide demonstrated superiority over placebo with reduced major adverse cardiovascular events (MACE) in the treatment group. Exenatide, lixisenatide and semaglutide have shown non-inferiority versus placebo for MACE. These trials demonstrated no association between GLP-1 agonist therapy and hospitalisation for heart failure.

November 2017 Br J Cardiol 2017;24:156–60 doi:10.5837/bjc.2017.031
Beta blocker usage in cardiac CT: a survey of BCSI members
Baltej S Pandher, Samuel D Cripps, Andrew Edwards, Nicholas Hollings, Robin van Lingen

To examine the current practice of British Society of Cardiovascular Imaging (BSCI) members in the administration of beta blockers in computed tomography (CT) coronary angiography (CTCA) a 10-point online questionnaire was emailed to all registered members of the British Society of Cardiovascular Imaging. There were 61 respondents: 75% give intravenous (IV) metoprolol in the CT department, the rest a combination of oral and/or IV dosing. Over 50% were happy to administer 50 mg or more. No serious complications related to drug administration had been seen by 82%. Of the remaining 18%, half (six reports) documented severe hypotension and two reported a death. No physical observations were taken by 25%, at any point. Another 27% checked blood pressure before the scan only, 17% measured blood pressure before the scan and immediately after and 28% measured before the scan and after with a delay.
In conclusion, among BSCI members, there is no uniform strategy regarding the route or dose of beta blocker administration, or if, when and what physical observations should be performed. Several severe adverse events have been documented, including two deaths. This, however, is in the context of the large volume of CTCAs performed nationally, and so, despite some doses of beta blocker exceeding British National Formulary recommendations, this appears safe.

October 2017 Br J Cardiol 2017;24:137–41 doi:10.5837/bjc.2017.025
Heart rate monitors and fitness trackers: friend or foe?
Edward Doris, Iain Matthews, Honey Thomas

Wearable and smartphone-based activity and heart rate (HR) monitors are becoming increasingly common, with around 80 million devices in use in 2017. Wearable and smartphone-based devices may be dedicated HR monitors or part of an activity tracker system. One of the main aims of these devices is to encourage exercise and increase fitness, which is clearly desirable in a society with high levels of inactivity and obesity. These devices provide individuals with large amounts of data including HR information. This may, therefore, give an opportunity to document or diagnose arrhythmias. Undiagnosed atrial fibrillation is a common problem and is associated with a huge burden of potentially preventable stroke. Wearable HR monitors may provide the opportunity to identify these individuals and allow them to receive stroke prevention treatment. However, the consumer fitness market is unregulated and the manufacturers emphasise that their devices are not intended to be used for detecting heart rhythm problems. The reliability, sampling frequency and algorithms for the HR data these devices provide are hugely variable. Detected ‘abnormalities’ may inform clinical decision making but it may also trigger unnecessary anxiety and costly investigations in healthy people.
October 2017 Br J Cardiol 2017;24:(4) doi:10.5837/bjc.2017.026
How hard do we look for atrial fibrillation?
Ioannis Merinopoulos, Sajid Alam, David Bloore

Atrial fibrillation (AF) is one of the most common arrhythmias, affecting approximately 2% of the general population. Identifying AF after an ischaemic stroke is particularly important as it changes the recommended antithrombotic therapy from antiplatelets to anticoagulation. Currently, there is no clear consensus with regards to the duration of rhythm monitoring post-stroke. In our study, we aim to review some of the pivotal studies regarding rhythm monitoring after an ischaemic stroke and identify the percentage of patients who get referred for prolonged rhythm monitoring after a stroke by providing real-world data from the Ipswich hospital. To our surprise, we did not identify any patients who got referred for prolonged rhythm monitoring (ILR) and the proportion of patients who did not have a 24-hour tape was unexpectedly high. In addition, there was a clear tendency for patients with lacunar strokes not to get investigated with 24-hour tape.
October 2017 Br J Cardiol 2017;24:(4) doi:10.5837/bjc.2017.027
The PACI survey: Patient adherence to cardioprotective lifestyle interventions in myocardial infarction patients treated with primary percutaneous coronary intervention
Justin L Mifsud

Despite documented evidence of benefits of lifestyle cardioprotective interventions in reducing recurrent coronary heart disease (CHD) events, many patients still fail to adhere to proposed lifestyle interventions. To determine the percentage adherence rate and to identify the perceived barriers influencing adherence rate to cardioprotective lifestyle interventions among patients treated with primary percutaneous coronary intervention (PPCI) a cross-sectional survey was designed.
A total of 193 consecutive patients, with a clinical diagnosis of CHD who had a PPCI, were identified retrospectively between 2008 and 2013, and were subsequently telephone surveyed. Data were analysed using chi-square tests and Fisher’s exact tests. At survey, 21.8% of patients smoked cigarettes, 30.6% were adhering to physical activities as per guidelines, 36.3% were consuming five portions of fruits and vegetables per day, and 9.8% were consuming three portions of oily fish per week. Negative stress, low mood, advanced age, poor health, lack of enjoyment from physical activities, low expectations from physical activity benefits, obesity and diabetes, were associated with non-adherence to physical activities as per guidelines.
In conclusion, risk factor targets for secondary prevention were not reached by a large proportion of patients. Several barriers exist among these individuals. Thus, there is still considerable potential for cardiac rehabilitation clinicians to improve standards of preventive cardiology by clearly identifying barriers and ways to overcome them.
October 2017 Br J Cardiol 2017;24:(4) doi:10.5837/bjc.2017.028
Current diagnostic yield of invasive coronary angiography at a district general hospital
Ali Rauf, Sarah Denny, Floyd Pierres, Alice Jackson, Nikolaos Papamichail, Antonis Pavlidis, Khaled Alfakih

Invasive coronary angiography (ICA) is an important diagnostic test in the diagnosis of coronary artery disease (CAD). However, it is associated with a small risk and is a relatively expensive procedure. National Institute for Health and Care Excellence (NICE) 2010 guidelines on stable chest pain recommended that patients with stable chest pain and high probability of CAD should be investigated with ICA.
We audited our own practice at a district general hospital (DGH), with a single catheter lab, to assess the yield of significant CAD at ICA in patients presenting with stable chest pain and acute coronary syndromes (ACS). There were 457 patients who were referrals for ICA with stable chest pain and 250 were inpatients undergoing ICA for ACS. The incidence of severe CAD in the whole cohort was 41%, with a further 20% found to have moderate CAD. The prevalence was higher in the ACS subgroup with 55% of patients having severe CAD compared with 33% in the stable chest pain sub-group. Of the patients having ICA for stable chest pain, 72% were direct referrals, with 30% found to have severe CAD. Our data show that overall detection rate of severe CAD in patients presenting with stable chest pain, at ICA, is relatively low.
August 2017 Br J Cardiol 2017;24:117 doi:10.5837/bjc.2017.023
Brugada syndrome in the context of a fever: a case study and review of current knowledge
Saad Ahmad, Irfan Ahmed

Brugada syndrome is a distinct arrhythmogenic disorder widely recognised as a sudden cause of death in the young. It is identified by a classical ST-segment elevation on electrocardiogram (ECG) that may be provoked in the context of a fever or vagal stimulation. The pathophysiology and genetic basis have been elucidated as an abnormality in ion channels. Diagnosis takes into account, not only the ECG, but clinical features and modulating factors; the inducibility of a suspect ECG when febrile is one such observation. Anti-arrhythmic drugs like ajmaline can also induce Brugada syndrome and have a role in its work-up. Electrophysiology studies may be useful in assessment and risk stratification of select cases. The management is centred around device therapy with the implantable cardioverter defibrillator (ICD), though pharmacological treatments are being actively pursued.
August 2017 Br J Cardiol 2017;24:120 doi:10.5837/bjc.2017.024
Multiple left atrial masses in a patient with breast cancer
Debjit Chatterjee

This is a rare case with dramatic image of multiple clot formation in the left atrium in a patient with mitral stenosis when anticoagulation was stopped for a few days before cancer surgery.
July 2017 Br J Cardiol 2017;24:105–7 doi:http://doi.org/10.5837/bjc.2017.017
The age of diagnostic coronary angiography is over
Andrew J M Lewis

This article won first prize in the recent British Junior Cardiologists’ Association (BJCA) essay competition.
Coronary angiography stubbornly bucks the hospital-wide trend to non-invasive diagnostic tests. New imaging technologies offer paths to better ways to investigate and manage ischaemic heart disease.
July 2017 Br J Cardiol 2017;24:100–4 doi:http://doi.org/10.5837/bjc.2017.020
Randomised clinical trial comparing transradial catheterisation with or without prophylactic nitroglycerin
Roberto Léo da Silva, Luis Sérgio Carvalho Luciano, Daniel Medeiros Moreira, Tammuz Fattah, Ana Paula Trombetta, Luciano Panata, Leandro Waldrich, Luiz Eduardo Koenig São Thiago, Luiz Carlos Giuliano

Spasm after transradial approach for catheterisation decreases procedural success and offers discomfort to the patient. Nitroglycerin is one of the drugs applied prophylactically to prevent spasm. The aim of this study was to assess the effect of preventive nitroglycerin on the comfort of patients during cardiac catheterisation.
A total of 328 patients were randomly assigned to receive either 200 µg nitroglycerin (n=164) or placebo (n=164). The main outcome was the evaluation of spasm using a visual analogue scale to measure the pain of the patient, and procedural time and radiation used to measure the operator difficulty during the examination.
The pain evaluation was equal in both groups (nitroglycerin 24.74 vs. placebo 24.75, p=0.72). Using the operator’s impression, there was a higher incidence of spasm in the placebo group (9.1% grade 3 or 4 vs. 2.4% in the nitroglycerin group, p=0.004), while procedural time (21.36 minutes vs. 22.24 minutes, p=0.23) and radiation exposure (655.61 mGy vs. 660.92 mGy, p=0.63) were comparable in both arms.
In conclusion, the prophylactic use of nitroglycerin offers no advantage in terms of comfort to the patient during cardiac catheterisation by a transradial approach. Although there was difference in operators’ perception of spasm, omission of vasodilator does not cause any objective difficulty to operators.
July 2017 Br J Cardiol 2017;24:108–12 doi:http://doi.org/10.5837/bjc.2017.019
A review of endomyocardial biopsy and current practice in England: out of date or underutilised?
Alex Asher

Endomyocardial biopsy (EMB) has been long established as a diagnostic tool in myocardial disease. EMB surveillance for rejection of cardiac allografts continues to be routinely performed. However, the use of EMB beyond transplant monitoring is controversial. In recent years, the procedure has fallen out of favour. This is most likely due to the growing capabilities of non-invasive imaging modalities and the questionable impact of EMB findings on treatment.
This article aims to examine current practice of EMB in England, discuss the utility of EMB in myocardial diseases and compare prominent society guidelines from recent years. Information gained from freedom of information requests shows just 18% of NHS trusts reported performing EMB, and only 46% referred to other centres for EMB in England in 2014–2015. Despite the limitations of EMB, it remains the only procedure capable of obtaining a histological diagnosis of cardiac disease.

July 2017 Br J Cardiol 2017;24:113–16 doi:http://doi.org/10.5837/bjc.2017.018
Glitazones (thiazolidinediones)
Emma Johns, Gerry McKay, Miles Fisher

Glitazones improve glycaemic control in type 2 diabetes mellitus (T2DM) by increasing whole-body insulin sensitivity. They can cause fluid retention and are, therefore, contraindicated in heart failure. A 2007 meta-analysis linked rosiglitazone with an increased risk of myocardial infarction, leading to its European marketing authorisation being suspended in 2010. Pioglitazone has demonstrated cardiovascular safety for atherosclerotic events in a large, randomised, placebo-controlled trial. A 2016 study in patients with insulin resistance and recent cerebrovascular event showed pioglitazone was associated with reduced risk of further stroke or transient ischaemic attack when compared with placebo, as well as reduced diabetes incidence.
July 2017 Br J Cardiol 2017;24:118–9 doi:http://doi.org/10.5837/bjc.2017.016
Hypertrophic cardiomyopathy and coronary fistulae
Deidre F Waterhouse, Theodore M Murphy, Charles McCreery, Rory O’Hanlon

A sixty-two-year-old asymptomatic man presented for a routine insurance medical. He had no previous cardiac history, nor any significant cardiac risk factors. His examination was normal. His electrocardiogram (ECG), however, was noted to be significantly abnormal, with deep anterior T-wave inversion in the precordial leads (figure 1). Given this abnormality and the potential differential diagnoses, a cardiovascular magnetic resonance (CMR) (Siemens Aera 1.5 T) with regadenosine stress perfusion was performed and images analysed using CMR 42 software (Circle CVI, Calgary).
June 2017 Br J Cardiol 2017;24:62-5 doi:http://doi.org/10.5837/bjc.2017.013
Transient loss of consciousness (TLoC) in primary care: a review of patients presenting with first blackout
Lesley Kavi

Blackouts are common, affecting up to 50% of the population. However, little is known about the incidence and initial management of blackouts in primary care. A retrospective computerised search of the medical records of 16,911 patients in two UK practices found the incidence of first presentation with blackout to the GP to be 3.4/1,000 patients/year. Affected patients’ records were then individually reviewed to assess whether key aspects of National Institute of Health and Care Excellence (NICE) blackouts and European Society of Cardiology syncope guidelines had been followed during that initial consultation. GPs were generally better at enquiring about features that differentiate between vasovagal syncope and epilepsy. They were not as good at detecting syncope red flags, which help to identify the cardiac causes of syncope that are associated with higher mortality. Raising awareness of these red flags in primary care was recommended.
June 2017 Br J Cardiol 2017;24:75-78 doi:http://doi.org/10.5837/bjc.2017.015
Improving the quality of heart failure discharge summaries
Neil Bodagh, Fahad Farooqi

A discharge summary is intended to communicate relevant clinical information to GPs after hospital admission. High-quality discharge summaries are especially important in complex clinical syndromes, such as chronic heart failure, where effective communication between multi-disciplinary teams is necessary to coordinate safe community care and reduce re-hospitalisation risk. The aim of this study was to audit the existing quality of heart failure discharge summary documentation at our Trust and test whether a 10-point checklist poster could improve performance. All heart failure discharge summaries issued from Barking, Havering and Redbridge University Hospitals’ NHS Trust over a three-month period were assessed. The content of each heart-failure-verified discharge summary was objectively analysed using a points-based scoring technique. A single checklist poster providing guidance on composing heart failure discharge summaries was positioned in a medical ward. The scores from every summary issued by doctors exposed to the checklist poster (n=24) on that ward were compared against discharge summaries scores issued by doctors working on all other (non-exposed) wards (n=84). Of discharge summaries with heart failure listed as a primary diagnosis, 28% were found to have an alternate cause for symptoms and no verifiable evidence to support a heart failure diagnosis. Discharge summaries issued by doctors working on the ward exposed to the checklist poster had a mean discharge summary score of 5.2 ± 0.59. Discharge summaries issued by doctors working on wards that were not exposed to the checklist poster had a mean score that was significantly poorer 1.7 ± 0.11 (p<0.001). This study demonstrates that a primary heart failure diagnosis may be inaccurate in approximately a quarter of all discharge summaries. The provision of a 10-point checklist was associated with a statistically significant improvement in the quality of heart failure discharge summaries issued from our Trust. This intervention was simple to implement at minimal cost and helps junior doctors communicate more effectively with primary care.
April 2017 Br J Cardiol 2017;24:66-7 doi:http://doi.org/10.5837/bjc.2017.009
Does CTCA improve the diagnostic yield from conventional coronary angiography? A DGH experience
Colin Reid, Mark Tanner, Hatef Mansoubi, Conrad Murphy

Our objective was to determine whether the development of a computed tomography coronary angiogram (CTCA) service has improved the yield of significant coronary artery disease (CAD) and subsequent referral for revascularisation following conventional invasive coronary angiography (ICA).
A retrospective audit comparing angiographic findings in a cohort of 2,094 patients investigated between 2007 and 2012 with findings from a cohort of 554 patients investigated in 2014 and 2015 during which time a CTCA service had been established. Cases included were those patients undergoing elective angiography for the assessment of possible coronary disease without any history of previous revascularisation.
In the pre-CTCA and CTCA cohorts the rates of one-vessel, two-vessel, three-vessel and left main stem disease were 20% vs. 18%, 14% vs. 14%, 10% vs. 11%, 2% vs. 3%, respectively, with overall yield of obstructive CAD of 46% in both cohorts (p>0.05 for all groups).
In conclusion, the availability of a CTCA service has not had any significant effect on the diagnostic yield of ICA. We propose that, adherence to current guidelines, results in a potential underuse of CTCA in the investigation of suspected stable CAD because a sizeable proportion of patients undergoing ICA have non-significant disease.

April 2017 Br J Cardiol 2017;24:68-71 doi:10.5837/bjc.2017.010
SGLT2 inhibitors
Emma Johns, Gerry McKay, Miles Fisher

Sodium-glucose co-transporter 2 (SGLT2) inhibitors are a novel insulin-independent therapy for type 2 diabetes mellitus (T2DM). By inhibiting renal glucose re-absorption, they improve glycaemic control and have beneficial effects on weight and blood pressure. Current guidance states that any new diabetes medication must be shown not to unacceptably increase cardiovascular risk. The landmark EMPA-REG OUTCOME (Empagliflozin Cardiovascular Outcome Event Trial in Type 2 Diabetes Mellitus Patients) trial demonstrated that treatment with the SGLT2 inhibitor empagliflozin compared with placebo showed a significant reduction in the risk of major cardiovascular end points and hospitalisation for heart failure for patients with T2DM and existing cardiovascular disease. A positive impact on several renal outcomes was also demonstrated in secondary analysis. These milestone results are set to have significant implications on prescribing practice in T2DM, with potential benefits for many patients with existing cardiovascular disease.
April 2017 Br J Cardiol 2017;24:72-4 doi:10.5837/bjc.2017.011
Recognition and management of posterior myocardial infarction: a retrospective cohort study
Leigh D White, Joshua Wall, Thomas M Melhuish, Ruan Vlok, Astin Lee

Characteristic electrocardiogram (ECG) features of posterior myocardial infarction (PMI) do not include typical ST-segment elevation and, therefore, carries the risk of delayed diagnosis and management. The aim of this study was to investigate how well PMIs are recognised and whether a lack of recognition translates to a larger infarction. This was a retrospective cohort study of patients sourced from a cardiac catheterisation database. Based on ECG analysis, patients included in this study included those meeting PMI criteria and those meeting ST-elevation myocardial infarction (STEMI) criteria as the control group. Door-to-balloon times were used as an outcome measure for differences in recognition between PMIs and other STEMIs. Troponin was used as a surrogate marker to measure degree of myocardial damage. There were 14 patients meeting PMI criteria and 162 meeting STEMI criteria. PMI patients had significantly longer door-to-balloon times. There was no statistically significant difference between PMI and STEMI group initial troponins t(169)=1.05, p=0.30, or peak 24-hour troponins t(174)=–1.73, p=0.09. In conclusion, using door-to-balloon times as a marker for recognition, this study illustrated that patients suffering PMI experience delayed recognition and management compared with non-PMI STEMIs. This did not, however, result in a significantly larger size of infarction as shown by peak troponin levels.
April 2017 Br J Cardiol 2017;24:79-80 doi:10.5837/bjc.2017.012
Dedicated side-branch stent: what could go wrong?
Usha Rao, Simon C Eccleshall

Bifurcation lesions are complex, technically difficult, have a higher rate of adverse events and lower success rates. This has led to the introduction of dedicated bifurcation stents, generally deployed along with main-vessel stent. Cappella Sideguard® is a dedicated bifurcation stent for treatment of bifurcation lesions, which otherwise could be technically challenging and may have low success rates. We report a very interesting case that resulted in a unique complication following the use of a dedicated bifurcation stent.

March 2017 Br J Cardiol 2017;24:25–9 doi:10.5837/bjc.2017.006
Cardiorespiratory fitness, oxygen pulse and heart rate response following the MyAction programme
Tim P Grove, Jennifer L Jones, Susan B Connolly

Improvements in cardiorespiratory fitness (CRF) are associated with better health outcomes. The Chester step test (CST) is used to assess the changes in CRF following a protocol-driven cardiovascular prevention and rehabilitation programme (CPRP) entitled MyAction. CRF expressed as predicted VO2max, can be influenced by physiological adaptations and/or retest familiarity-efficiency. Therefore, we employed an index ratio between oxygen uptake and heart rate (O2 pulse) to determine if the improvement in CRF is related to a true physiological adaptation.
In total, 169 patients, mean age 66.8 ± 7.3 years attended a 12-week MyAction CPRP. All were assessed using the CST on the initial and end-of-programme assessment. O2 pulse was estimated from the CST and was calculated by dividing VO2 into the exercise heart rate multiplied by 100.
Following the CPRP, VO2max increased by 2.8 ml/kg/min. These changes were associated with an overall increase in O2 pulse by 0.6 ml/beat (p≤0.001) and a 4.1 beats/min (p≤0.001) reduction in the exercise heart rate response on the CST.
In conclusion, O2 pulse provides transparency on the physiological adaptations following a CPRP and can be used to help patients recognise the benefits of exercise training. For example, the average patient increased his/her O2 pulse by 0.6 ml/beats and saved 4–7 heart-beats on the CST.
March 2017 Br J Cardiol 2017;24:30–4 doi:10.5837/bjc.2017.007
Impact of HF on HRQoL in patients and their caregivers in England: results from the ASSESS study
Iain Squire, Jason Glover, Jacqueline Corp, Rola Haroun, David Kuzan, Vera Gielen

Heart failure (HF) is a chronic, symptomatic and progressive disease associated with reduced health-related quality of life (HRQoL) in both patients and their caregivers. This study assessed the HRQoL of HF patients (n=191; mean age 70 [range 21–95] years; New York Heart Association [NYHA] class II–IV) and their caregivers (n=72; mean age 69 [range 43–88] years) in England. Patients had poor HRQoL assessed by the EQ-5D-5L weighted index (mean ± standard deviation [SD] 0.60 ± 0.25 [normal 0.78 ± 0.26 for people aged 65–74 years]). The impact of HF on patients’ HRQoL varied markedly; importantly, the extent of comorbidity most influenced the reduction in patients’ HRQoL, as well as disease-related symptoms. The impact on HRQoL on caregivers of patients with HF was on average limited, with the EQ-5D-5L index for caregivers (0.75 ± 0.18) in-line with the normal values for their age range. However, as with the patients, the impact on HRQoL varied markedly, with some caregivers having a bad caregiving experience as measured by the Carer Experience Scale weighted index. This study provides important information on the impact on HRQoL and burden of HF for patients and their caregivers.
March 2017 Br J Cardiol 2017;24:35–8 doi:10.5837/bjc.2017.008
Reperfusion, conditioning and the ongoing search for the holy grail
Robert L Yellon, Rob M Bell

Ischaemic conditioning is the phenomenon of protection against reperfusion injury via the application of brief, repeated episodes of non-lethal ischaemia. This review has three aims: 1) to briefly explain the various categories of ischaemic conditioning; 2) to explore past clinical trials and their failures; 3) to explore the future of clinical trials in the realm of ischaemic conditioning.

January 2017 Br J Cardiol 2017;24:(1) doi:10.5837/bjc.2017.001
Dipeptidyl peptidase-4 (DPP-4) inhibitors
Emma Johns, Gerry McKay, Miles Fisher

Dipeptidyl peptidase-4 (DPP-4) inhibitors are one of two classes of antidiabetes drugs that mediate their glucose-lowering effect through the incretin pathway. They are administered orally and offer significant glucose-lowering with a neutral weight profile and a low risk of hypoglycaemia. Three large randomised-controlled trials have demonstrated cardiovascular safety, with no increase in major adverse cardiovascular events comparing DPP-4 inhibitors (saxagliptin, alogliptin and sitagliptin) with placebo. An increase in heart failure hospitalisation was noted with saxagliptin compared with placebo, and a similar increase was also noted in one subgroup receiving alogliptin compared with placebo. Further cardiovascular safety trials with DPP-4 inhibitors are ongoing, including a trial comparing the DPP-4 inhibitor linagliptin with the sulphonylurea glimepiride.

January 2017 Br j Cardiol 2017;24(1) doi:10.5837/bjc.2017.003
Setting up cardio-oncology services
Arjun K Ghosh, Charlotte Manisty, Simon Woldman, Tom Crake, Mark Westwood, J Malcolm Walker

In this article, we explain the clinical requirement for cardio-oncology services and reflect on our experiences in setting these up at Barts Heart Centre and at University College London Hospital.
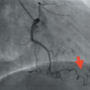
January 2017 Br J Cardiol 2017;24:39–40 doi:10.5837/bjc.2017.004
Multiple coronary cameral fistulae
Hasan Kadhim, Anita Radomski

A 61-year-old East European woman was admitted with atypical chest pain. Risk factors: smoker of 5–10 cigarettes per day, hypertension, hypercholesterolaemia and family history of ischaemic heart disease. Highly sensitive troponin-T, electrocardiogram (ECG) and exercise stress test were normal.

November 2016 Br J Cardiol 2016;23:138–40 doi:10.5837/bjc.2016.037
Improving communication with GPs post-STEMI
JJ Coughlan, Conor Hickie, Barbara Gorna, Ross Murphy, Peter Crean

The rationale behind secondary prevention post-ST-elevation myocardial infarction (STEMI) is well established. Guidelines recommend titration of several medications for secondary prevention up to a maximally tolerated dose in order to confer maximum benefit. Due to decreasing duration of inpatient stays post-myocardial infarction (MI), this up-titration must often take place in primary care. Guidelines also recommend clearly informing GPs regarding duration of dual antiplatelet therapy and monitoring cardiovascular risk factors. Clear communication between secondary/tertiary and primary healthcare practitioners is essential in order to ensure our patients are receiving optimum care.
We examined all discharge summaries for patients discharged post-STEMI in our tertiary referral centre. This encompassed rates of prescribing of the National Institute for Health and Care Excellence (NICE) recommended medications post-MI, rates of therapeutic prescribing of these medications and communication with GPs regarding duration of dual antiplatelet therapy, up-titration of medications and repeat checking of fasting lipid profiles. In order to improve compliance with guidelines, incoming junior staff were educated on guidelines for communication post-STEMI at our journal club. We then re-audited our practice in order to see if compliance with the guidelines improved.
Our results showed that, while the majority of our patients were discharged on the correct medications post-MI, most were receiving subtherapeutic doses of angiotensin-converting enzyme (ACE) inhibitors and beta blockers. In addition, we exhibited poor communication with primary healthcare practitioners. Compliance with the NICE guidelines on communication significantly improved after our intervention.
In conclusion, education of junior staff can significantly improve communication with GPs. This, in turn, could help optimise secondary prevention strategies post-MI.
November 2016 Br J Cardiol 2016;23:141–4 doi:10.5837/bjc.2016.038
Postural tachycardia syndrome: a UK occupational therapy perspective
Jenny Welford, Christopher McKenna

Postural tachycardia syndrome (PoTS) is a form of dysautonomia, a term used to describe dysfunction of the autonomic nervous system. The condition can cause marked physical and cognitive impairment that can significantly impact upon activity. Although the exact UK prevalence is unknown, its frequency has stimulated an increase in studies. Occupational therapy services should place themselves in a position to respond to the potential need.
This study aimed to determine how PoTS impacts upon activity, in order for occupational therapists to understand the implications of this condition and develop appropriate interventions.
We recruited 201 adults (aged 18–70 years) via two patient support charities to participate in an online quantitative survey. Participants rated their experiences pre-symptoms versus present day in relation to their occupations, producing ordinal data under self-care, leisure and productivity domains, including their physical ability, motivation and fatigue levels.
The pre-symptom versus present day probability scores of <0.001 can be viewed as ‘very significant’ and confirm that PoTS has a significant negative impact across all three occupational domains.
In conclusion, PoTS has a significant negative impact upon occupation and is associated with considerable morbidity. With their understanding of the central role of occupation in wellbeing, occupational therapists may need to support people with PoTS in achieving a satisfying balance of occupations that will support their health.

November 2016 Br J Cardiol 2016;23:151–4 doi:10.5837/bjc.2016.039
Implementation of a modified version of NICE CG95 on chest pain of recent onset: experience in a DGH
Peregrine Green, Stephanie Jordan, Julian O M Ormerod, Douglas Haynes, Iwan Harries, Steve Ramcharitar, Paul Foley, William McCrea, Andy Beale, Badri Chandrasekaran, Edward Barnes

National Institute for Health and Care Excellence (NICE) clinical guideline 95 (CG95) was introduced to rapid-access chest pain clinics (RACPC) to aid investigation of possible stable angina based on pretest probability of coronary artery disease (CAD). Following a six-month audit of its implementation we introduced a modified version: patients with low/moderate risk of CAD were referred for computed tomography coronary angiography (CTCA), while those at high/very high risk were referred for invasive angiography.
Patient records of 546 patients referred to our RACPC over a six-month period were retrospectively analysed. Pretest probability of CAD, referral for initial investigation, and outcomes at a minimum follow-up time of six months were documented.
Incidence of CAD correlated well with pretest probability. Moderate-risk patients had a low incidence of CAD and revascularisation. High/very high-risk patients had a high incidence of revascularisation, and this was predominantly for prognostically significant disease.
In conclusion, low rates of CAD in low- and moderate-risk groups justifies the use of CTCA as a first-line investigation in these patients. Routine investigation of very high-risk patients allows a high proportion to undergo revascularisation for prognostically significant disease. Strict adherence to NICE CG95 could lead to these patients being missed.
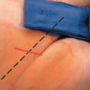
November 2016 Br J Cardiol 2016;23:155–8 doi:10.5837/bjc.2016.040
Risk factors for femoral arterial complications and management
Shabnam Rashid, Stephanie Hughes

Bleeding is one of the complications associated with percutaneous coronary intervention from the femoral route due to the use of potent antiplatelet therapies including adenosine diphosphate receptor blockers and glycoprotein IIb/IIIa inhibitors. Complications include haematoma, retroperitoneal haemorrhage, pseudoaneurysm, arteriovenous fistula, arterial occlusion, femoral neuropathy and infection. Complications for diagnostic procedures are lower due to the lack of antiplatelet therapies on board. Often, incorrect location of the femoral artery puncture site results in complications. Puncturing below the femoral bifurcation can result in psedoaneurysm, haematoma and arteriovenous fistulas, whereas retroperitoneal haemorrhage is caused by high femoral punctures. Identification of bleeding and vascular complications is paramount as bleeding is associated with adverse events. Techniques to reduce the risk of femoral arterial complications include the use of ultrasound scan or fluoroscopy guided femoral punctures. Furthermore, the micropuncture technique has been shown to reduce complications but is not widely adopted. Ultimately, the radial route is preferable to the femoral route as vascular complications are significantly lower.
October 2016 Br J Cardiol 2016;23:151–4 doi:10.5837/bjc.2016.032
Suitability for sacubitril/valsartan at discharge from hospital: an audit
Thomas Green, Kaushiki Singh, Hugh F McIntyre

National Institute for Health and Care Excellence (NICE) guidance supports the introduction of sacubitril/valsartan under the supervision of a heart failure specialist with access to a multi-disciplinary heart failure team. Clinical information was obtained retrospectively on all patients with a primary coded diagnosis of heart failure discharged from the Conquest Hospital, Hastings, UK during the calendar year 2015. We recorded the proportion of patients meeting the NICE recommendation and those patients meeting the additional PARADIGM-HF (Prospective comparison of ARNI with ACEI to Determine Impact on Global Mortality and morbidity in Heart Failure) study inclusion criteria.
In a total of 205 assessable patients discharged with a primary diagnosis of heart failure during the calendar year 2015, inpatient mortality was 11%, with a crude readmission rate during the year of 17%. The number of patients meeting the NICE criteria was 26 (13%). In hierarchical analysis taking the major PARADIGM-HF inclusion criteria, 20 patients (10%) patients met the inclusion criteria.
In conclusion, the findings from this audit suggest that the number of patients potentially suitable for sacubitril/valsartan therapy is low. Given the PARADIGM-HF study run-in design, the optimal dose and stability of angiotensin-converting enzyme (ACE) inhibitor and angiotensin-receptor blocker medication may need to be clarified if sacubitril/valsartan is to be commenced during or shortly after hospitalisation.
October 2016 Br J Cardiol 2016;23:148–50 doi:10.5837/bjc.2016.033
Eligibility of patients for sacubitril/valsartan in a secondary care heart failure service
Freya M Lodge, Julie Phillips, Tristan Groves, Zaheer R Yousef

The first-in-class drug sacubitril/valsartan (EntrestoTM) has been recommended for use in the UK by the National Institute for Health and Care Excellence (NICE) following evidence from the PARADIGM-HF (Prospective comparison of ARNI with ACEI to Determine Impact on Global Mortality and morbidity in Heart Failure) trial. To qualify, patients should have severe left ventricular dysfunction (ejection fraction ≤35%), New York Heart Association (NYHA) grade II–IV symptomatic heart failure, and be on a stable dose of angiotensin-converting enzyme inhibitor (ACEi) or angiotensin-receptor blocker (ARB). We evaluated all patients seen in our nurse-led heart failure clinics over a six-month period to assess suitability for sacubitril/valsartan and the resulting cost implication.
Of 553 patients seen, more than two thirds (69%) were unsuitable, of whom most had an ejection fraction greater than 35%. Other reasons included hypotension, NYHA class I, renal dysfunction, intolerance of ACEi/ARB and compliance concerns. There were 49 patients who died within nine months of the study period end. Of these, most (84%) were unsuitable for sacubitril/valsartan. Compared with current local use of ACEi and ARB, switching the 174 suitable patients to sacubitril/valsartan would cost £171,816 per year.
In our real-world experience, 31–37% of patients attending a specialist nurse-led heart failure clinic may be suitable for sacubitril/valsartan therapy. While the clinical benefits of this treatment are well proven and a recent NICE technology assessment has demonstrated cost-effectiveness, the medication has significant upfront cost implications for healthcare commissioners.
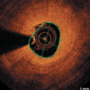
October 2016 Br J Cardiol 2016;23:159–60 doi:10.5837/bjc.2016.034
A novel method of treating stent fractures
Usha Rao, Timothy J Gilbert, Simon C Eccleshall

Drug-eluting stents (DES) have revolutionised the treatment of acute coronary syndrome, resulting in improvement in mortality and morbidity. However, there have been safety concerns, mainly involving a small, but long-term, risk of stent thrombosis (ST) and in-stent restenosis (ISR). Stent fracture (SF) is a lesser-known complication that can predispose to both ST and ISR and for which there is no general consensus for treatment. We present an interesting case and a new approach to treating this complex problem.
August 2016 Br J Cardiol 2016;23:110–3 doi:10.5837/bjc.2016.028
Optimal angiographic views for invasive coronary angiography: a guide for trainees
Peregrine Green, Paul Frobisher, Steve Ramcharitar

The ability to perform invasive diagnostic coronary angiography is a core requirement for cardiologists and fellows in training programmes. However, although key to their independence is the ability to obtain high-quality images that allow visualisation of the entire coronary vasculature, there exists no formal systematic method or teaching aid. This article provides an overview of the radiological equipment used in the catheter laboratory, details the naming of the different angiographic projections, and gives key tips and tricks to improve image quality. In addition, the coronary vasculature is broken down into segments, with descriptions provided of the essential views required to image each one. Using this approach, it aims to provide an essential aid to trainees and other healthcare professionals at the start of their careers.

August 2016 Br J Cardiol 2016;23:114–8 doi:10.5837/bjc.2016.029
Evaluation of a new same-day discharge protocol for simple and complex pacing procedures
Thomas A Nelson, Aaron Bhakta, Justin Lee, Paul J Sheridan, Robert J Bowes, Jonathan Sahu, Nicholas F Kelland

There is variable adoption in same-day discharge for pacing procedures across Europe. We compared length of hospital stay and complication rates in two cohorts, using a same-day and next-day discharge protocol. Case notes were reviewed for 229 consecutive patients attending our tertiary centre for device implantation to establish the rate of hospital readmission and complications. These comprised 106 patients in the next-day discharge cohort, and 123 from the same-day cohort. All pacing procedures, including cardiac resynchronisation therapy (CRT) and implantable cardioverter-defibrillators (ICDs), were included.
No significant differences were observed between cohorts in age, gender, device indication, device type, procedure urgency or venous access route. Median length of stay post-implant significantly reduced from 1.2 days in the next-day cohort (25th–75th centile 1.06–3.24) to 0.99 days in the same day cohort (0.3–1.3) and from 1.08 days (0.94–1.2) to 0.36 (0.27–0.97), respectively, for the subgroup of elective patients (n=95). Death, complication, and readmission rates were similar between the two cohorts. Morning procedures were associated with shorter hospitalisation. No same-day cohort CRT recipients (n=28) suffered complications.
In conclusion, same-day discharge for pacing (including CRT and ICDs) results in decreased length of stay without increasing complications.
August 2016 Br J Cardiol 2016;23:119–20 doi:10.5837/bjc.2016.030
A challenging case of recurrent effusive pericarditis
Mohamed Abbas, Darrell Ramsey, Dariusz Koziara

A 22-year-old man was admitted to a general district hospital with a three-day history of epigastric pain and shoulder discomfort. He reported shortness of breath on exertion, but denied any chest pain or flu-like symptoms. He had no past medical history of note. Vital signs assessment confirmed low blood pressure of 90 mmHg systolic, and tachycardia of 130 beats per minute. Physical examination of the abdomen revealed mild epigastric tenderness. A computerised tomography (CT) scan for suspected cholecystitis showed a normal gall bladder, but revealed a large rim of pericardial effusion measuring 2.8 cm. He was then urgently transferred to a tertiary cardiac centre for assessment and consideration of pericardiocentesis.

July 2016 Br J Cardiol 2016;23:102–5 doi:10.5837/bjc.2016.024
Development of a UK National Certification Programme for Cardiac Rehabilitation (NCP_CR)
Gill Furze, Patrick Doherty, Carol Grant-Pearce

In 2012, the British Association for Cardiovascular Prevention and Rehabilitation (BACPR) published guidance on the standards and core components of cardiac rehabilitation (CR). However, annual reports from the UK National Audit of Cardiac Rehabilitation (NACR) have shown that, while there are examples of excellent practice in the UK, many CR programmes do not meet the BACPR standards. It is difficult for service managers, patients and commissioners to assess how a particular CR programme meets minimum standards of service delivery. These findings led the BACPR and NACR to work together to develop a UK National Certification Programme for CR that would be mainly based on assessment of quality-assured patient-level NACR data. The development of the certification process was built on surveys and interviews with CR service providers, patients and commissioners. Minimum standards for certification were developed by an expert group. The resulting process for certification of meeting minimum standards of CR service was then successfully pilot-tested with 16 CR programmes, of which 13 programmes have since met minimum certification standards. CR programmes that submit data to the NACR can now apply for assessment under the BACPR/NACR National Certification Programme.

July 2016 Br J Cardiol 2016;23:106–9 doi:10.5837/bjc.2016.025
Spinal cord stimulation for refractory angina: 100 case-experience from the National Refractory Angina Service
Blandina Gomes, Kamen Valchanov, William Davies, Adam Brown, Peter Schofield

Refractory angina represents an important clinical problem. Spinal cord stimulation (SCS) for refractory angina has been used for over two decades to improve pain and, thus, quality of life. This case series reports the clinical efficacy and safety profile of SCS.
We included patients who had a SCS device implanted between 2001 and 2015 following a rigorous selection process. Patients were prospectively followed. We performed a descriptive analysis and used paired t-test to evaluate the difference in Canadian Cardiovascular Society angina (CCS) class before and after SCS implant.
Of the 100 patients included, 89% were male, the mean age was 65.1 years and mean follow-up time was 53.6 months. The CCS class after SCS implant was statistically improved from before (p<0.05) and 88% of patients who gave feedback were very satisfied. Thirty-two patients died, 58% of those who had a documented cause of death, died from a non-cardiac cause.
This study shows the outcome of 14 years’ experience of SCS implantation. The anginal symptoms had a statistically significant improvement and the satisfaction rate was higher than 90%. The complication rate is within the range reported in the literature. SCS seems to be an effective and safe treatment option for refractory angina.
June 2016 Br J Cardiol 2016;23:57–60 doi:10.5837/bjc.2016.019
The short- and long-term impact of psychotherapy in patients with chronic, refractory angina
Peysh A Patel, Murad Khan, Chia Yau, Simerjit Thapar, Sarah Taylor, Paul A Sainsbury

Refractory angina (RA) describes those patients with persistence of symptoms despite optimal conventional strategies. It is often associated with a maladaptive psychological response, resulting in significant burden on hospital services. This observational study sought to assess the short- and long-term impact of psychotherapy on quality of life, mood and symptoms.
Between 2011 and 2012, consecutive attendees to a specialised RA service were recruited. Intervention consisted of a course of cognitive-behavioural therapy allied with an education programme. Outcome measures were collated pre-intervention, one month and two years post-intervention. Validated questionnaires were utilised for scoring assessments: SF-36 (Short-Form 36) for quality of life, HADS (Hospital Anxiety and Depression Scale) for anxiety/depression, and SAQ (Seattle Angina Questionnaire) for functional assessment.
There were 33 patients included. Median SF-36 scores increased and this effect remained in the long term. Levels of depression reduced, and improved further at subsequent review. Frequency of angina was comparable, both short and long term. Usage of glyceryl trinitrate (GTN) spray was similar at one-month follow-up and at two years.
In conclusion, a short course of psychotherapy appears to improve quality of life and mood in patients with RA, and is achieved independent of symptom control. Further research is warranted so that the debilitating morbidity associated with this disorder can be abrogated.
June 2016 Br J Cardiol 2016;23:61–4 doi:10.5837/bjc.2016.020
Clinical and psychological outcomes of an angina management programme
Deborah Tinson, Samantha Swartzman, Kate Lang, Sheena Spense, Iain Todd

Chronic refractory angina results in significant NHS costs due to chronic high use of resources. This audit evaluated the clinical effectiveness of a cognitive-behavioural (CBT) programme in reducing angina symptoms after maximal medical and surgical intervention. The primary outcome was self-reported angina. Additional questionnaire data comprised perceived quality of life/disability, angina misconceptions, self-efficacy and mood. Data from the electronic patient administration system was used to compare use of cardiology hospital resources in the two years before and two years after attendance. Patients completing questionnaires reported significant improvements in all areas post-group and at two months. Resource use was lower in the two years post-programme than the two years prior. A CBT-based approach to symptom management could offer additional clinical benefits in the cardiac rehabilitation menu.

June 2016 Br J Cardiol 2016;23:73–7 doi:10.5837/bjc.2016.021
Midodrine is safe and effective in the treatment of reflex syncope
Amir S Anwar, Yawer Saeed, Aly Zaki, Sanjiv Petkar, Sarah Collitt, Nicola Rice, Pam Iddon, Adam P Fitzpatrick

Reflex syncope is the most common cause of transient loss of consciousness. Practical manoeuvres may help, but additional measures are often required. In our experience, midodrine gives consistently good results in patients with reflex syncope. This study also provides reassurance that the effect on blood pressure is measureable, but small, and side effects are infrequent. UK prescribing may have been limited when midodrine was unlicensed, but midodrine is now licensed.
We treated 195 patients, age 40 ± 18 years, 72 (37%) aged under 30 years, 151 female (78%), who attended a Rapid Access Blackouts Triage Clinic and gave a clear history of reflex syncope. The median duration of symptoms was 28 months. A misdiagnosis of epilepsy had occurred in 39 patients and 42 had significantly low blood pressure.
Follow-up was 50 ± 42 months in 184 patients (93%), with 11 patients lost to follow-up. Twenty-eight patients had minor electrocardiogram (ECG) changes but had a normal echocardiogram. Overall, 143 (73%) patients improved on a mean dose of 10 mg a day of midodrine. Syncopal events fell from 16 ± 16 to 2.6 ± 5 per six months (p<0.05), and in 69 (35%) patients, syncope was eradicated. Nineteen (10%) patients were able to stop midodrine after 52 ± 42 months due to symptom resolution. Fifteen patients (7%) stopped midodrine because of side effects, while 17 (8%) patients failed to respond. Mean supine systolic blood pressure rose from 114 mmHg to 121 mmHg at final midodrine dose (p<0.05).
In conclusion, in patients with reflex syncope, midodrine shows clinical benefit in greater than 70%, with 24% having complete symptom resolution. Side effects are rare, and there is little evidence of a hypertensive effect.
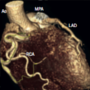
June 2016 Br J Cardiol 2016;23:79–81 doi:10.5837/bjc.2016.022
Anomalous origin of the left coronary artery from the pulmonary artery: case report and review
Kully Sandhu, David Barron, Hefin Jones, Paul Clift, Sara Thorne, Rob Butler

Anomalous origin of the left coronary artery from the pulmonary artery is a rare congenital condition that proves to be fatal in most individuals during childhood due to significant left ventricular ischaemia. However, there are case reports of individuals surviving into adulthood that have varying presenting symptoms. We report a case of a young male, who presented to our cardiology clinic with typical ischaemic cardiac pain, with no established risk factors, and was found to have anomalous origin of the left coronary artery from the pulmonary artery that was subsequently surgically corrected.
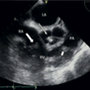
April 2016 Br J Cardiol 2016;23:65–7 doi:10.5837/bjc.2016.015
Triple-valve infective endocarditis
Azeem S Sheikh, Asma Abdul Sattar, Claire Williams

Despite the significant improvements in both diagnostic and therapeutic procedures in recent years, infective endocarditis (IE) remains a medical challenge due to poor prognosis and high mortality. Echocardiographically, the majority of the patients demonstrate vegetations on a single valve, while demonstration of involvement of two valves occurs much less frequently; triple-valve involvement is extremely rare. Reported operative mortality after triple-valve surgery is high and ranges between 20% and 25%.
Surgical treatment is used in approximately half of patients with IE because of severe complications. Reasons to consider early surgery in the active phase, i.e. while the patient is still receiving antibiotic treatment, are to avoid progressive heart failure and irreversible structural damage caused by severe infection, and to prevent systemic embolism. Prognosis in IE is influenced by four main factors: characteristics of the patient, the presence or absence of cardiac and non-cardiac complications, the infecting organism, and echocardiographic findings. Prognosis of right-sided native valve endocarditis is relatively good, with an in-hospital mortality rate of about 10%.
We present a case of a young man with triple-valve endocarditis followed by a brief review of the literature.
April 2016 Br J Cardiol 2016;23:68–72 doi:10.5837/bjc.2016.016
Strain imaging and anthracycline cardiotoxicity
Fatemeh Homaei Shandiz, Afsoon Fazlinezhad, Ahmad Tashakori Beheshti, Hesam Mostafavi Toroghi, Golkoo Hosseini, Maliheh Bakaiyan

This was a pilot study, in which 55 breast cancer patients were enrolled, to evaluate the alterations of strain and strain-rate parameters in breast cancer patients receiving doxorubicin and compare them with serial conventional echocardiography changes. A week prior to, and a week after, chemotherapy with doxorubicin, left ventricular ejection fraction (LVEF) and strain and strain-rate parameters were measured by conventional 2D echocardiography and tissue Doppler-based imaging, respectively.
Comparison of the results of pre- and post-chemotherapy evaluation demonstrated that strain and strain-rate parameters were significantly reduced. Mean difference (standard deviation) for the strain measurement of basal-septal, basal-lateral, basal-inferior, and basal-anterior values were 2.58% (2.15), 3.20% (1.94), 4.13% (3.48), and 2.86% (2.65), respectively; and for the strain-rate values were 0.18 s–1 (0.17), 0.17 s–1 (0.17), 0.24 s–1 (0.19), and 0.19 s–1 (0.14), respectively; all p values <0.001. There was no significant change in patients’ LVEF after chemotherapy (pre-intervention 61.10 (4.86), post-intervention 61.06 (4.82), p=0.857).
In conclusion, strain/strain-rate significant reduction, in the setting of normal range LVEF, suggests subclinical heart failure. Whether the strain and strain-rate imaging should replace the conventional echocardiography for early monitoring of cardiotoxicity of doxorubicin requires further investigations.
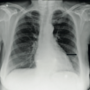
April 2016 Br J Cardiol 2016;23:78 doi:10.5837/bjc.2016.017
When you can’t obtain a history…
Luciano Candilio, Juliana Duku, Alexander W Y Chen

A 79-year-old lady was taken to the emergency department by her carer, who had noticed an acute deterioration of her general condition. Unfortunately, it was difficult to obtain an accurate history from the patient due to cognitive impairment, and her carer was not aware of her past medical history. However, she had been observed clenching her hands to her chest. She was not previously known to the admitting hospital.

March 2016 Br J Cardiol 2016;23:16–20 doi:10.5837/bjc.2016.008
Are the current guidelines for performing sports with an ICD too restrictive?
Theresia A M Backhuijs, Hilde Joosten, Pieter Zanen, Hendrik M Nathoe, Mathias Meine, Pieter A Doevendans, Frank J G Backx, Rienk Rienks

Current guidelines recommend against vigorous sports for all patients with an implantable cardioverter defibrillator (ICD). In this study, we established the risk of life-threatening arrhythmias and shocks in patients with an ICD participating in sports.
In this single-centre, cohort survey with 71 patients (59% male) ≤40 years old at ICD implantation and with a left ventricular ejection fraction (LVEF) ≥35%, 16 patients were defined as athlete (exercise ≥5 hours per week). Sports-related and clinical data were obtained using questionnaires and medical records. Median age was 38 years (19–53 years). Median follow-up period was 67 months (11–249 months). Idiopathic ventricular fibrillation (VF) was the most frequent indication (20%) for implantation. There were 22 patients (31%) who experienced 127 shock episodes, of which 112 were appropriate: 15% of shocks occurred during physical exercise. Shocks did not occur more frequently in athletes (25%) compared with non-athletes (33%, p=0.760). Intensity of exercise and appropriateness of shocks were not associated.
In conclusion, we found no evidence that participation in sports contributed to the risk of life-threatening arrhythmias and (in)appropriate ICD shocks in patients with an ICD. In individual cases, the advice to participate in sports could be more lenient compared with current guidelines.
March 2016 Br J Cardiol 2016;23:21–6 doi:10.5837/bjc.2016.009
Advances in transcatheter options in the management of mitral valve disease
Mamta H Buch

Current transcatheter mitral valve techniques are at the beginning of an era of innovation before their full potential is realised. The broadening of available options for mitral regurgitation (MR) reduction is welcome and transcatheter mitral valve interventions provide complementary strategies in the drive for more safe and effective therapies for patients. In this article, the evidence and indications for MitraClip® are reviewed.

March 2016 Br J Cardiol 2016;23:33 doi:10.5837/bjc.2016.010
A profile of patients with postural tachycardia syndrome and their experience of healthcare in the UK
Lesley Kavi, Michaela Nuttall, David A Low, Morwenna Opie, Lorna M Nicholson, Edward Caldow, Julia L Newton

Postural tachycardia syndrome (PoTS) is a recently recognised condition that usually affects younger women, who develop symptoms of orthostatic intolerance and a persistent tachycardia on standing upright. Healthcare professionals, patients and the national patient support group (PoTS UK) together created a survey, and the responses of 779 UK PoTS patients were analysed. The most common symptoms of PoTS at presentation were the triad of fatigue, lightheadedness and palpitations. Mobility, ability to work or attend education, and quality of life were significantly restricted. Cardiologists, followed by patients, were most likely to be the first to suggest the diagnosis of PoTS. Patients waited a mean of almost four years from presentation to obtain their diagnosis and, meantime, psychiatric mislabeling was common. Advice given to patients regarding lifestyle changes was variable, and those referred to specialist practitioners for help, found practitioners had limited knowledge about management of PoTS. Increased education of healthcare professionals and improved services for patients are recommended.
March 2016 Br J Cardiol 2016;23:37 doi:10.5837/bjc.2016.011
The clinical and cost impact of implementing NICE guidance on chest pain of recent onset in a DGH
Boyang Liu, Regina Mammen, Waleed Arshad, Paivi Kylli, Arvinder S Kurbaan, Han B Xiao

In 2010, the National Institute for Health and Care Excellence (NICE) introduced new guidelines for the assessment of people with recent-onset chest pain, recommending investigations based upon one’s pre-test likelihood of having coronary artery disease. We aim to determine the impact these guidelines have made on the numbers of patients being discharged and referred for further investigations. We retrospectively analysed a database of 337 consecutive patients seen in the rapid access chest pain clinic: 162 patients were seen in the three months preceding, and 175 were seen in the three months following implementation of the new guidelines. We found that after implementation of the new guidelines, fewer patients (25% vs. 37%, p=0.018) were discharged at the first visit, and a greater number of patients were referred for an angiogram (20% vs. 6%, p=0.0001). The number of referrals for stress imaging significantly reduced from 57% to 37%. According to the new guidelines, 18% of patients were referred for coronary calcium scoring. This reflects a definite change in clinical practice with reduced direct discharges from the chest pain clinic, reduced reliance on functional imaging and increased direct referrals for invasive coronary angiography, resulting in higher investigational costs of the chest pain service.
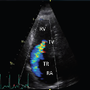
March 2016 Br J Cardiol 2016;23:39 doi:10.5837/bjc.2016.012
A challenging case of collapse with tri-fascicular block: from permanent pacemaker to thrombolysis
Luciano Candilio, Kavitha Aggarwal, Alexander W Chen, Nandkumar Gandhi, Shrilla Banerjee

A 90-year-old man with a history of prostate cancer was admitted with haematuria and mild normocytic anaemia on routine blood tests. Baseline observations were normal and chest X-ray was unremarkable. Electrocardiogram (ECG) showed tri-fascicular block. He underwent successful bladder irrigation. Prior to discharge, he suffered a syncopal episode: ECG confirmed tri-fascicular block, for which he was discussed with the cardiology team for consideration of permanent pacemaker implantation. Pre-procedural transthoracic echocardiogram (TTE) revealed a large mobile thrombus attached to the tricuspid valve (TV) and extending to the right ventricle (RV), significant RV impairment and severe TV regurgitation (figure 1A–B). Following discussion between urology and cardiology teams and, in view of the significant risk of massive pulmonary embolism (PE), the patient underwent urgent thrombolysis. This was not complicated by significant haematuria. Post-intervention TTE demonstrated complete dissolution of the right-sided thrombus and mild TV regurgitation only (figure 1C–D). Warfarin was started and no further haematuria or syncope was reported on subsequent follow-up.

March 2016 Br J Cardiol 2016;23:40 doi:10.5837/bjc.2016.013
Congenital LAD stenosis associated with a bicuspid aortic valve
Hasan Kadhim, Anita Radomski

A 47-year-old woman had been referred to the cardiology department with a six-month history of intermittent chest discomfort not specifically related to exertion. Her risk factors: current smoker 10–15 per day and family history of ischaemic heart disease. She had no history of diabetes or hypertension. Lipid levels had not been tested.
February 2016 Br J Cardiol 2016;23:(1) doi:10.5837/bjc.2016.002
‘Quick-scan’ cardiac ultrasound in a high-risk general practice population
Nora C Fabich, Harpal Harrar, John B Chambers

Structural heart disease may be missed using clinical examination alone and limited echocardiograms or ‘quick-scans’ may be a way to improve rates of detection. To evaluate the finding of clinically unexpected abnormalities using ‘quick-scans’, scans were performed in a general practice by a level 7 sonographer using a GE V scan system. Indications were: murmur; potentially cardiac symptom (e.g. chest pain or breathlessness); cardiac history in the GP notes (e.g. myocardial infarction); atrial fibrillation; chronic obstructive pulmonary disease with disproportionate dyspnoea; age ≥75 years. Standard transthoracic echocardiograms were performed if clinically indicated or if the ‘quick-scan’ detected a significant abnormality.
There were 163 ‘quick scans’ indicated, which were normal in 80 (49%), mildly abnormal in 67 (41%) and significantly abnormal in 16 (10%). Abnormalities were moderate left ventricular (LV) systolic dysfunction, moderate mitral regurgitation, moderate-to-severe aortic stenosis and mild aortic dilatation. Within the 90 patients without agreed indications the ‘quick-scans’ were normal in 64 (71%) and mildly abnormal in 26 (29%) while none were significantly abnormal.
In conclusion, ‘quick scans’ can detect clinically unexpected pathology. These results are consistent with a global move to use the hand-held ultrasound machine as an extension of the clinical examination.
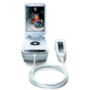
February 2016 Br J Cardiol 2016;23:(1) doi:10.5837/bjc.2016.003
Massive pulmonary embolism diagnosed by focused cardiac ultrasound (V scan)
Andrew Workman, Gavin Lewis, Peter Currie

Focused cardiac ultrasound using a pocket-sized imaging device (V scan) is increasingly being used to screen patients in the emergency setting for structural heart disease. We describe a patient who presented with light-headedness and pallor with elevated high-sensitivity troponin T (hs-TnT) and was initially thought to have acute coronary syndrome. A screening focused cardiac ultrasound revealed a dilated right ventricle with normal left ventricular function, and a computerised tomography pulmonary angiogram (CTPA) demonstrated a large saddle pulmonary embolus. The case highlights the application and utility of focused cardiac ultrasound and provides an overview of its current role in the acute setting reinforced by current guidelines from the European Society of Cardiology.

February 2016 Br J Cardiol 2016;23:(1) doi:10.5837/bjc.2016.004
Delivering early rehabilitation after an exacerbation of heart failure: is it feasible? A short report
Linzy Houchen-Wolloff, Amye Watt, Sally Schreder, Sally Singh

People with chronic heart failure (CHF) often experience exacerbations of their symptoms that require hospitalisation. The feasibility, safety and efficacy of early post-exacerbation rehabilitation are largely unknown in this population.
This was a single-centre, feasibility trial of early rehabilitation versus usual care. Those assigned to the intervention started rehabilitation within 10 days of discharge and attended supervised sessions twice per week for eight weeks. The primary outcomes were feasibility of uptake and safety. Assessments were performed at baseline and three months: exercise tolerance (shuttle walking tests) and health status (questionnaire).
There were 1,298 patients screened, 16 patients recruited (<1% of those screened) and 11 randomised (five rehabilitation, six control). The primary reasons for exclusion were contraindication to exercise and normal ejection fraction. There were improvements in exercise tolerance and health status in both groups at three months; however, the study was not powered to report any within- or between-group significance. The early rehabilitation intervention was safe with no adverse events reported.
In conclusion, early rehabilitation, for patients with CHF, was unfeasible. The 10-day recruitment target was too restrictive in this population. This is important because there has been a drive towards early rehabilitation in CHF guidelines.

February 2016 Br J Cardiol 2016;23:(1) doi:10.5837/bjc.2016.005
Prevalence, clinical characteristics and outcomes of HF with preserved versus reduced ejection fraction
Rajdip Dulai, Azeem S Sheikh, Amer Qureshi, Shanit Katechia, Yulia Peysakhova, Moira Johns, Sajjad Mazhar

The proportion of patients with heart failure with preserved ejection fraction (HFPEF), compared with those with reduced ejection fraction (HFREF), is significant and rising. Studies have used an ejection fraction (EF) >50% as the sole criteria for identifying patients with HFPEF. However, European Society of Cardiology (ESC) guidelines include the diagnostic criteria of EF >50% and evidence of diastolic dysfunction.
In this retrospective cohort study based on admissions in 2012; we compared characteristics, treatment and outcomes between HFPEF and HFREF patients. One year readmission and survival rate was also assessed.
Overall, 41 (17%) patients had HFPEF (EF >50% and either medial or lateral E/E’ >15) compared with 200 (83%) with HFREF. Age was similar between the two groups (HFPEF: 84 ± 9 vs. HFREF: 82 ± 14, p=0.106). HFPEF patients were significantly more likely to be female (71% vs. 41.5%, p=0.001) and significantly less likely to have ischaemic heart disease (34% vs. 52%, p=0.043). Patients with HFPEF were significantly less likely to be taking loop diuretics, potassium-sparing diuretics, angiotensin-converting enzyme (ACE) inhibitors and aspirin on discharge. Ischaemic heart disease was a significant predictor of mortality in HFPEF patients (hazard ratio [HR] 7.14; 95% confidence interval [CI] 1.51–33.85, p=0.01). There was no difference in readmission and one-year survival rate (p=0.68 and p=0.551, respectively).
In conclusion, HFPEF patients are more likely to be female but less likely to have an ischaemic aetiology. There were significant differences in treatment of both phenotypes. Both groups have a similar poor prognosis.
February 2016 Br J Cardiol 2016;23:(1) doi:10.5837/bjc.2016.006
Comparison of warfarin dosage needed to achieve target INR before and after cardiac surgery
Cindy San, Doson Chua, Hilary Wu, Jian Ye

Delays in achieving target international normalised ratio (INR) with warfarin after cardiac surgery can lead to suboptimal outcomes. The aims of the study are to determine the difference in warfarin dosage requirements, before and after cardiac surgery, needed to achieve therapeutic anticoagulation.
A single-centre, retrospective review was conducted from 2012 to 2014 in cardiac surgery patients who were on warfarin pre-operatively and who had warfarin therapy resumed postoperatively in hospital. The primary outcome was the difference in warfarin dosage needed to achieve target INR before and after cardiac surgery.
Ninety-five patients were included in the study. The mean daily postoperative warfarin dose needed for achieving a therapeutic INR was 0.18 mg lower than the mean pre-operative dose (5.03 ± 2.10 vs. 4.85 ± 2.25 mg; p=0.358).
In conclusion, there was no statistically significant difference in the warfarin dosage before and after cardiac surgery needed to achieve target INRs.
February 2016 Br J Cardiol 2016;23:(1) doi:10.5837/bjc.2016.007
The barriers facing medical research in the UK
Aaron Koshy, Andrew L Clark

Conducting clinical research is an ambition of many cardiologists and academic clinicians. Over the last decade, the National Health Service (NHS) has indicated that research is a clear priority in improving healthcare for patients. The processes leading to permission to start a clinical trial in the UK are, however, poorly understood, labyrinthine and fraught with difficulty. In this article, we aim to share our knowledge of initiating a clinical trial using a case study, with a focus on the essential documents and the communication required with different organisations.

December 2015 Br J Cardiol 2015;22:155 doi:10.5837/bjc.2015.041
Latest NICE guidelines on CRT and ICD devices in heart failure may significantly increase implant rates
Thabo Mahendiran, Oliver E Gosling, Judith Newton, Dawn Giblett, Dan McKenzie, Mark Dayer

In June 2014 the National Institute for Health and Care Excellence (NICE) released new guidelines (TA314) on the use of implantable cardioverter defibrillators (ICDs) and cardiac resynchronisation therapy devices (CRTs) in the management of heart failure. These guidelines replaced the previous TA95 and TA120 guidelines. We evaluated the potential impact on implant rates in our institution.
Clinical records of 396 consecutive patients were reviewed, with 100 patients included in the final analysis. Device indications and associated costs were calculated using both existing and new criteria.
NICE TA95/TA120 criteria recommended 37 devices: 20 ICDs, 9 CRTs with pacing (CRT-Ps), and 8 CRTs with defibrillator (CRT-Ds). The new NICE 2014 criteria recommended 97 devices: 56 ICDs, 7 CRT-Ps, and 34 CRT-Ds. Comparison of the new and old guidelines suggested a significant increase in total devices (p<0.0001). This corresponded primarily to an increase in ICDs and CRT-Ds, with an associated £661,708 increase in total spend (£407,205 increase per annum).
This study confirms the significant increase in ICDs and CRT-Ds indicated by NICE. This will have significant financial and workforce implications.

December 2015 Br J Cardiol 2015;22:136 doi:10.5837/bjc.2015.040
Barriers to cardiac device innovation
Nick Linker

The UK population is getting older and the amount of cardiovascular disease is increasing significantly, fuelled by a steep rise in the incidence of obesity and diabetes. Heart failure is increasing in incidence because of improved survival rates following myocardial infarction and more effective treatments, with an estimated 500,000 sufferers.1 People with heart failure are more at risk of sudden cardiac death and many can benefit from cardiac devices such as implantable cardioverter defibrillators (ICDs) and cardiac resynchronisation devices (CRT-D/Ps). This increasing need was recognised by the National Institute of Health and Care Excellence (NICE) in 2014 with the publication of the revised guidelines for the use of such devices.2 Nevertheless, the UK remains well below the European average for ICD implants, although is improving in terms of CRT devices;3 the latter due to a higher than average implant rate of CRT pacemakers. However, the rate of implantation of all high-energy devices (ICD + CRT-D) is only slightly more than half the European average.
December 2015 Br J Cardiol 2015;22:156 doi:10.5837/bjc.2015.042
Healthcare professional’s guide to cardiopulmonary exercise testing
Sathish Parasuraman, Konstantin Schwarz, Nicholas D Gollop, Brodie L Loudon, Michael P Frenneaux

Cardiopulmonary exercise testing (CPEX) is a valuable clinical tool that has proven indications within the fields of cardiovascular, respiratory and pre-operative medical care. Validated uses include investigation of the underlying mechanism in patients with breathlessness, monitoring functional status in patients with known cardiovascular disease and pre-operative functional state assessment. An understanding of the underlying physiology of exercise, and the perturbations associated with pathological states, is essential for healthcare professionals to provide optimal patient care. Healthcare professionals may find performing CPEX to be daunting, yet this is often due to a lack of local expertise and guidance with testing. We outline the indications for CPEX within the clinical setting, present a typical protocol that is easy to implement, explain the key underlying physiological changes assessed by CPEX, and review the evidence behind its use in routine clinical practice. There is mounting evidence for the use of CPEX clinically, and an ever-growing utilisation of the test within research fields; a sound knowledge of CPEX is essential for healthcare professionals involved in routine patient care.

December 2015 Br J Cardiol 2015;22:158 doi:10.5837/bjc.2015.043
A region-wide audit of cardiac rehabilitation services
M Justin S Zaman on behalf of all ACRAN healthcare professionals

This is an audit of 10 Anglia region cardiac rehabilitation (CR) programmes against the British Association of Cardiovascular Prevention and Rehabilitation (BACPR) seven core standards. Methods included a questionnaire that encapsulated these standards, a SWOT (strengths, weaknesses, opportunities, threats) analysis and assessment of local outcomes.
Overall, all 10 CR services were compliant with the vast majority of basic standards set by BACPR but the audit also highlighted gaps in ideal care processes, such as a shortage of psychologists, occupational therapists and pharmacists, and inadequate audit processes. Local strengths were highlighted that will encourage future cross-pollination across the network. Outcomes were collected variably ad hoc but there was some consistency that CR across the region improved exercise tolerance, reduced anxiety and reduced smoking, but had little effect on blood pressure and body mass index, comparable to the national audit.
Anglia CR services were shown to be fit-for-purpose and there were local areas of excellence, but local areas of need and gaps in CR were highlighted that will cross-pollinate to improve all CR services in East Anglia.

October 2015 Br J Cardiol 2015;22:147–54 doi:10.5837/bjc.2015.034
Treatment patterns and lipid levels among patients with high-risk atherosclerotic CVD in the UK
Beth L Nordstrom, Jenna M Collins, Robert Donaldson, William A Engelman, Antje Tockhorn, Yajun Zhu, Zhenxiang Zhao

High-risk atherosclerotic cardiovascular disease (ASCVD), including recent history of acute coronary syndrome, cerebrovascular atherosclerotic disease, peripheral arterial disease, and coronary artery disease with diabetes mellitus, requires lipid-level monitoring and treatment. Data for patients with high-risk ASCVD from 2008–2011 were obtained from the UK Clinical Practice Research Datalink. Across two years of follow-up, analyses examined lipid-altering drug use, statin adherence (medication possession ratio [MPR]), and persistence (continuous time on drug). Initial statin dose, upward dose titration, and use of high-intensity statins were also studied. Lipid levels were examined overall and by statin use. A total of 131,603 high-risk ASCVD patients were included. Within six months of diagnosis, 63.1% of patients received a statin prescription. Patients typically remained on the initial statin (MPR ≥80% for 71.3% of patients at two years) and dose; 16.4% of patients used high-intensity statins. During the first year of follow-up, 69.3% of patients were either at the low-density lipoprotein cholesterol goal of <2.5 mmol/L or using a high-intensity statin. Considerable room for improvement remains with respect to optimal management of patients with ASCVD.

October 2015 Br J Cardiol 2015;22:157 doi:10.5837/bjc.2015.035
Pre-alert calls for primary PCI: a single-centre experience
Jennifer A Rossington, Stephen F Cole, Yasmin Zaidy, Michael S Cunnington, Richard M Oliver

Hull and East Yorkshire Hospitals NHS Trust offers a primary percutaneous coronary intervention (PPCI) service accessed via a coronary care unit (CCU) nurse-based pre-alert system. We reviewed our pre-alert calls for 2013 to determine their appropriateness and assess whether patients were being correctly accepted/declined for PPCI by comparison with final discharge diagnosis.
There were 1,343 calls received, only 52% had chest pain and electrocardiogram (ECG) changes meeting criteria. There were 508 patients with a discharge diagnosis of ST-elevation myocardial infarction (STEMI), 89% of whom were accepted directly.
There were 54 cases with a final diagnosis of STEMI initially declined: 14 in cardiac arrest were directed to the emergency department (ED) as per policy; 18 had documented clinical reasons for declining; seven did not meet the criteria. There were 15 patients (3%) with chest pain and ECG criteria declined without a documented reason; three were subsequently accepted after assessment at their local hospital. Patients >80 years, female and with atypical presentation were more likely to be declined.
Of accepted patients, 132 (23%) had a diagnosis other than STEMI at discharge, 65% with an alternative cardiac diagnosis.
In conclusion, patients are frequently referred who do not meet symptom or ECG criteria. Most STEMI patients are appropriately accepted via our pre-alert pathway. Review of pre-alert services is essential to ensure timely and appropriate PPCI.
October 2015 Br J Cardiol 2015;22:159 doi:10.5837/bjc.2015.036
Atypical chest pain in young adult patients: dropped shoulder syndrome as a cause
Ali Abdul-Latif, Adnan Shakir

Left-sided dropped shoulder syndrome (DSS) can present with anterior chest pain that radiates to the left scapula and arm. Patients with atypical chest pain (ACP) of unknown cause (n=47) were investigated for left-sided DSS. Sixteen patients (34%) were diagnosed with left DSS. All the 47 patients were provided physiotherapy in two groups: the left DSS patients group (n=16) and a control group of 31 patients who did not show the criteria for the diagnosis of DSS.
Fourteen (87.5%) patients reported a satisfactory improvement of the ACP after physiotherapy. Satisfactory improvement has been judged by the reduction of the pain intensity, duration and frequency according to the patient’s report. Two (12.5%) patients showed no satisfactory improvement of the ACP. The control group showed no beneficial effect regarding their ACP after physiotherapy.
Physiotherapy aimed to strengthen the muscles that elevate the shoulder, could provide a treatment for atypical chest pain caused by left-sided DSS.

October 2015 Br J Cardiol 2015;22:160 doi:10.5837/bjc.2015.037
Coenzyme Q10 and cardiovascular disease: an overview
David Mantle

Coenzyme Q10 (CoQ10) is a naturally occurring vitamin-like substance that has three functions of relevance to cardiovascular function: (i) its key role in the biochemical process supplying cardiac cells with energy; (ii) its role as a cell membrane protecting antioxidant; (iii) its direct effect on genes involved in inflammation and lipid metabolism. Although some CoQ10 is obtained from the diet, most is manufactured within the liver, the capacity for which declines with age. These data therefore provide a rationale for the importance of CoQ10 in cardiovascular function, and its dietary supplementation. The objective of this article is therefore to provide a brief overview of the pharmacology of CoQ10, and its role in the prevention and treatment of cardiovascular disease.
August 2015 Br J Cardiol 2015;22:101–4 doi:10.5837/bjc.2015.029
Inflammation is associated with myocardial ischaemia
Kushal Pujara, Ashan Gunarathne, Anthony H Gershlick

Inflammation plays an important role in the pathogenesis of coronary heart disease (CHD). Several inflammatory cytokines have shown a direct association with the development of atherosclerosis. Recently, there have been a number of experimental studies exploring the potential anti-inflammatory role of currently used therapeutic agents including antibiotics, immuno-suppressive drugs and non-steroidal anti-inflammatory medications. This review summarises the available evidence base and the potential role of these agents in current clinical practice.
August 2015 Br J Cardiol 2015;22:105–9 doi:10.5837/bjc.2015.030
Oral anticoagulation in hospitalised patients with newly diagnosed AF: a story of too little, too late
Shohreh Honarbakhsh, Leigh-Ann Wakefield, Neha Sekhri, Kulasegaram Ranjadayalan, Roshan Weerackody, Mehul Dhinoja, R Andrew Archbold

Current guidelines make no recommendations regarding the strategy for initiation of oral anticoagulant (OAC) therapy in patients who are hospitalised with newly diagnosed atrial fibrillation (AF). This was a single-centre, retrospective, observational study that included patients admitted in 2013 with newly diagnosed AF (ICD-10 I48). There were 234 patients hospitalised with newly documented AF. The mean CHA2DS2-VASc score was 3.8: 201 (86%) patients had a CHA2DS2-VASc score ≥2. Out of the 179 patients considered for anticoagulation, only 115 patients were intended to receive OAC therapy: 56 (49%) as an inpatient and 59 (51%) as an outpatient, either by anticoagulation clinic or primary care. In the outpatient group, only 41 patients (69%) were actually initiated on OAC, with a mean time delay of 10 and 93 days in anticoagulation clinic and primary care group, respectively. During mean follow-up of 194 days, there were two strokes in the outpatient group in patients intended to start anticoagulation but did not (2/59), while no episodes occurred in the inpatient group.
In summary, only 82% of patients with newly diagnosed AF and CHA2DS2-VASc score ≥2 were referred for initiation of OAC, and still fewer actually received such therapy. Outpatient anticoagulation is associated with poor uptake and significant delays.
August 2015 Br J Cardiol 2015;22:118 doi:10.5837/bjc.2015.031
UK experience of conversion of radial to femoral access in coronary interventions
Shana Tehrani, David Hackett

Transradial access for coronary procedures is associated with less vascular access site complications. Occasionally, radial access fails and makes conversion to a transfemoral route inevitable. In this paper, which updates UK radial experience, we report the outcomes in a single UK centre in developing a transradial access programme.
We analysed 3,225 consecutive patients who underwent transradial coronary procedures over a five-year period. The primary outcome measure was rate of conversion from transradial to transfemoral access route. Of 3,225 radially approached cases, conversion from radial to femoral access route occurred in 148 patients (4.6%). With experience after the learning curve, the conversion rate fell to 2.0%.
In conclusion, after an initial learning curve, procedural success rate is high with low cross-over rate from radial to femoral entry site.

July 2015 Br J Cardiol 2015;22:(3) doi:10.5837/bjc.2015.023
FY1 in heart failure: the good, the bad and the ugly! Reflections by the FY1 doctors in heart failure and their supervisor on the first year of a new post
Laura Styles, Sarah Soar, Philippe Wheeler, Abdallah Al-Mohammad

With the expansion of the heart failure services to meet the rise in demand, we established, in Sheffield, a new training post for the junior medical staff in their first year of training. This is a four-month post for the Foundation Year one (FY1) doctors in heart failure. The post differs from the classic FY1 posts in that it is based in the heart failure multi-disciplinary team (HF-MDT) rather than being ward-based. Thus, the trainee works under the supervision of a consultant cardiologist with an interest in heart failure, and works alongside a group of heart failure specialist nurses screening new admissions for heart failure, and offering advice and follow-up of patients with heart failure who are not under the care of the cardiologists. The trainee attends the heart failure diagnostic clinic along with the consultant cardiologist, and participates in the work of the HF-MDT ward round. These are the collective personal views of the first three trainees who have worked in this post in the year 2013–2014; with a footnote from their supervisor.

July 2015 Br J Cardiol 2015;22:(3) doi:10.5837/bjc.2015.024
The use of EKOS-catheter-directed thrombolysis in the management of extensive thromboembolism
Lisa Leung, Aerakondal B Gopalamurugan

This case report invites discussion on the challenges of the management of extensive thromboembolism despite standard anticoagulation.
A previously healthy 49-year-old male had an acute pulmonary embolism (PE) and was managed with rivaroxaban anticoagulation and an inferior vena cava (IVC) filter implantation. This patient re-presented with occlusion of his IVC filter with extensive thrombus extending down to his femoral veins bilaterally.
We performed catheter-directed thrombolysis using the EKOSonic Endovascular system. The patient had invasive monitoring alongside use of peri-operative cardiac imaging (TOE). A valvuloplasty balloon was used to prevent upward migration of thrombus.
There is potential for the wider use of the EKOSonic Endovascular system and catheter-directed thrombolysis in centres where there is surgical support available, and in selected patients where there is extensive thrombotic burden with risk of recurrence or long-term complications.

July 2015 Br J Cardiol 2015;22:(3) doi:10.5837/bjc.2015.025
Calling the cardioverted: an audit of long-term anticoagulation in patients attending for DCCV
Philippa Howlett, Michael Hickman, Edward Leatham

Direct current cardioversion (DCCV) is a method to restore sinus rhythm in patients diagnosed with atrial fibrillation (AF). Despite having high initial efficacy, the long-term success rate of this procedure is lower. Consequently, the European Society of Cardiology (ESC) guidelines recommend indefinite anticoagulation in patients with a high risk of recurrence. We sought to establish whether these guidelines had been adhered to in a district general hospital.
Anticoagulation data were provided by GP practices for 208 patients who had undergone a DCCV for AF between 2008 and 2010. One hundred and sixty-five patients (79%) were prescribed warfarin. The remaining 43 patients were invited to a screening clinic with 21 subsequently attending (49%). Eleven of the patients were in AF (p=0.0002) and in five of the 11 patients this had not previously been documented (p=0.035). Nine of the 11 patients in AF (82%) met ESC criteria for anticoagulation with a mean CHA2DS2‑VASc score =2.18 ± 1.48.
Our findings suggest that nearly half of patients not on anticoagulation following DCCV have recurrence of AF warranting antithrombotic therapy. We propose similar screening is adopted in other centres in order to ensure that ESC guidelines are being met.

July 2015 Br J Cardiol 2015;22:(3) doi:10.5837/bjc.2015.026
Single-dimensional estimation of LV size using echo and MRI: effect of measurement location
Cheng William Hong, Zoran B Popovic, Amanda R Vest, Scott D Flamm, Michael A Bolen

Typical echocardiographic assessment of left ventricle (LV) size is based on single-dimensional measurements at mitral valve leaflet tips. In ischaemic and non-ischaemic cardiomyopathy (ICM and NICM) and aortic regurgitation (AR) where spherical remodelling is observed, this single-dimensional measurement at the LV base may underestimate LV volume. We hypothesised the maximum diameter would provide a closer approximation. A retrospective analysis of 1,680 consecutive cardiovascular magnetic resonance (CMR) examinations identified 82 patients with substantial LV dilation (LVEDVi >130 ml/m2) and 23 controls. LV end-diastolic and end-systolic diameters were measured using echocardiography and CMR at the standard level (EDDMV and ESDMV) and the maximum diameter (EDDmax and ESDmax). Indexed diameters were fitted to indexed volumes using cubic regressions. Maximum diameters had higher R2 values in fitting LV volume, and improved categorisation of subjects with chamber enlargement without substantially increasing the false-positive rate. Standard measurements may underestimate LV volume in cases of spherical remodelling, use of the maximum dimension may be a straightforward approach to improve assessment of LV volume and remodelling.
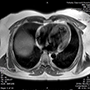
July 2015 Br J Cardiol 2015;22:(3) doi:10.5837/bjc.2015.027
Syncope in a patient with cardiac sarcoidosis
Khwaja Nizamuddin, Farhan Shahid, Richard P W Cowell

A 46-year-old man with cutaneous sarcoidosis and pulmonary involvement was referred to a cardiologist for possible pulmonary hypertension in view of increasing shortness of breath. Echocardiogram findings and electrocardiogram (ECG) changes prompted the need for coronary angiography, which was subsequently normal.
Cardiac sarcoidosis was one of the differential diagnoses. The patient was booked for a treadmill test. Unfortunately, in the interim, the patient had an episode of collapse while playing football. The local district hospital discharged the patient after finding normal computed tomography (CT) brain scan and negative troponin. He was re-admitted with a pre-syncopal episode and ambulatory ECG monitoring revealed non-sustained ventricular tachycardia. A cardiac magnetic resonance imaging (MRI) scan was arranged followed by insertion of an implantable cardioverter defibrillator (ICD).
This case report and literature review highlights the importance of cardiac screening in patients deemed ‘high risk’ for sudden cardiac death, and the need for immediate investigation and treatment. Current guidelines are yet to be universally accepted, so such cases are important in highlighting current methods of investigation and treatment.

June 2015 Br J Cardiol 2015;22:75–7 doi:10.5837/bjc.2015.020
Introducing integrated care: potential impact on hospital cardiology clinic workload
Ahmad Khwanda, Kevin O’Gallagher, Madalina Garbi, Stefan Karwatowski, Edward Langford

Integration of healthcare services has been advocated to improve quality and cost-effectiveness. Different models of integrated care for cardiology have been suggested, but the cost-effectiveness of a consultant-run service has been questioned. We assessed the potential impact on secondary-care outpatient volumes of introducing a service run by GPs with a special interest, with support from consultant cardiologists. We retrospectively reviewed all cardiology outpatient attendances at the South London Healthcare NHS Trust for a period of three months in 2011. Using National Institute for Health and Care Excellence (NICE) guidelines and discussions between cardiologists and GPs, a novel outpatient referral triage protocol was drawn-up to decide the appropriate minimum level of care required for a range of cardiac conditions. Anonymised clinic letters were divided into new referrals and follow-ups, and were assessed to establish the diagnosis and clinical complexity. Implementing such an integrated community care service (ICC) would reduce new referrals to secondary care by 33%, and would enable transfer of 44% of patients currently followed up in secondary care to ICC. The study confirms that there is scope for significant transfer of care with the greatest gains in patients with valve disease, ischaemic heart disease and atrial fibrillation.

June 2015 Br J Cardiol 2015;22:78 doi:10.5837/bjc.2015.021
Treatment of VTE in primary care: building a new approach to patient management with rivaroxaban
Rosie Heath

Venous thromboembolism (VTE) is a common cardiovascular disorder associated with considerable morbidity and mortality. The standard treatment for VTE comprises parenteral heparin overlapping with, and followed by, a vitamin K antagonist, which, although effective, has several limitations. Currently, many patients commence treatment for VTE in hospital and are discharged after 5–10 days to ongoing care in the community. With the introduction of non-vitamin K oral anticoagulants (NOACs), there is now the possibility for the complete management of patients with uncomplicated VTE to be undertaken by primary care, reducing the burden on hospitals and improving the patient experience. The NOAC rivaroxaban, a direct factor Xa inhibitor, has been widely approved for the treatment of VTE. This article offers guidance to general practitioners on the practical use of rivaroxaban for the treatment of patients with VTE, along with a discussion of its potential benefits compared with standard therapy.
June 2015 Br J Cardiol 2015;22:79 doi:10.5837/bjc.2015.022
Implementation of point-of-care troponin T testing in clinical practice
Faheem A Ahmad, Stephen Dobbin, Allister D Hargreaves

Troponin testing is the cornerstone diagnostic test for evaluating acute coronary syndromes (ACS). Evidence suggests this test is increasingly being utilised in a less specific fashion. We sought to evaluate the appropriateness of bedside point-of-care (POC) troponin T (TnT) sampling in our hospital.
We examined the case records for 109 consecutive patients who underwent admission troponin testing. We reviewed the clinical presentation, baseline electrocardiogram (ECG) and final diagnoses.
Only 55% of patients presented with actual cardiac chest pain. A troponin-positive result was found in 19.2% of patients (n=21); however, only half of these had a final diagnosis of ACS. The troponin assay was negative in 80.8% of patients (n=88); under one-quarter of these (n=16) underwent further ischaemia assessment. Almost one-third of patients had neither chest pain nor ECG changes (n=35), but still underwent troponin testing. None had a final diagnosis of coronary artery disease.
Troponin assays are requested for patients with a relatively low suspicion of an ACS. A failure to undertake further ischaemia assessment suggests a lack of initial conviction of a cardiac diagnosis. True ACS was diagnosed in less than half of troponin-positive cases. These data support a need for more selective usage.

April 2015 Br J Cardiol 2015;22:70–2 doi:10.5837/bjc.2015.013
The effectiveness of a mobile ECG device in identifying AF: sensitivity, specificity and predictive value
Jonathan Williams, Keith Pearce, Ivan Benett

Early identification of atrial fibrillation (AF), especially when asymptomatic, is increasingly important when there are interventions that can reduce the risk of stroke. One mobile ECG device that has the potential for doing just that is the AliveCor® device, which is non-invasive and easy to use. We aimed to assess its utility in primary care by establishing its sensitivity and specificity, and consider the predictive value for identifying AF in a general practice population.
We used the device on a population known to have AF in order to calculate the sensitivity, and on a population who did not have AF at the time of recording, to establish specificity. Using the known prevalence of AF in a UK population, we were able to calculate the predictive values for identification of AF. All AliveCor® traces we compared with a gold-standard 12-lead electrocardiogram (ECG).
The device has a high sensitivity and specificity in the hands of experienced clinicians. In particular, the sensitivity was consistently high, which would ensure a high true-positive rate of identification. Furthermore, the negative predictive value in populations with a prevalence of AF as in the UK is sufficiently high to be useful.
In conclusion, the AliveCor® device should be considered as an option for early identification of patients with unknown AF. It has a high negative-predictive value and is sufficiently sensitive to be useful in a general practice population, but does not rule out the need for a definitive ECG in suspected cases.
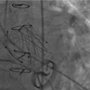
April 2015 Br J Cardiol 2015;22:(2) doi:10.5837/bjc.2015.015
Patients with a mechanical mitral valve are potential candidates for TAVI
Katie E O’Sullivan, Eoghan T Hurley, Declan Sugrue, John P Hurley

We present a review of transcatheter aortic valve implantation (TAVI) in the presence of a mechanical mitral valve. We conclude that in patients with a prior mechanical prosthesis, TAVI is feasible and can be carried out without complication. Based on proof of feasibility, evidence to date would suggest that patients with mechanical prostheses be actively considered for TAVI going forward.
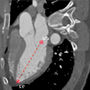
April 2015 Br J Cardiol 2015;22:(2) doi:10.5837/bjc.2015.016
Cardiac orientation: is there a correlation between the anatomical and the electrical axis of the heart?
Gnalini Sathananthan, Simmi Zahid, Gunjan Aggarwal, William Chik, Daniel Friedman, Aravinda Thiagalingam

Data have suggested that in vivo cardiac orientation has the greatest effect on the cardiac electric field, and, thus, surface electrical activity. We sought to determine the correlation between in vivo cardiac orientation using cardiac computed tomography (CT) and the electrical cardiac axis in the frontal plane determined by surface electrocardiogram (ECG).
Patients aged between 30 and 60 years old with a normal body mass index (BMI), who underwent CT coronary angiography between July 2010 and December 2012 were included. Patients with diabetes, hypertension, arrhythmias, structural heart disease or thoracic deformities were excluded. In vivo cardiac orientation was determined along the long axis and correlated with the electrical cardiac axis on surface ECG.
There were 59 patients identified, with 47% male, mean age of 49.9 years and a mean BMI of 22.39 kg/m2. The mean cardiac axis on CT was 38.1 ± 7.8°, while the mean electrical cardiac axis on ECG was 51.8 ± 26.6°. Bi-variate analysis found no correlation between the two readings (Pearson r value 0.12, p=0.37).
We conclude, there is no simple relationship between the anatomical cardiac axis and the ECG determined electrical axis of the heart. The electrical axis of the heart, however, showed more variability, reflecting possible underlying conduction disturbances.

April 2015 Br J Cardiol 2015;22:(2) doi:10.5837/bjc.2015.017
Coronary and bypass graft angiography using a single catheter via the left trans-radial artery
Hasan Kadhim, Anita Radomski

Using the left trans-radial artery access route for coronary and bypass angiography has been frowned upon by the majority of operators due to several catheter changes during the procedure, patient discomfort because of spasm, positioning of the patients left arm and longer radiation exposure times, to name a few reasons. This short scientific article demonstrates one of a series of 22 cases where a single catheter was successfully used via this access route.
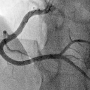
March 2015 Br J Cardiol 2015;22:40 doi:10.5837/bjc.2015.012
MI with multiple distal occlusions associated with use of the synthetic cannabinoid 5F-AKB48
Jason L Walsh, Benjamin H L Harris, Nicholas Ossei-Gerning

A 26-year-old man presented to the emergency department with central chest pain radiating to the left arm. An electrocardiogram (ECG) revealed inferior ST elevation. He had no major risk factors for cardiovascular disease, but habitually used synthetic cannabinoids (AKB48 and 5F-AKB48). A subsequent coronary angiogram showed occlusions in four obtuse marginal branches of the left circumflex artery and a large clot in the distal right coronary artery. The patient was treated with aspirin, ticagrelor, rivaroxaban and tirofiban infusion, and these occlusions were demonstrated to have resolved on a follow-up angiogram. The patient admitted smoking 5F-AKB48 four hours before the onset of chest pain. This case further strengthens the association between the use of synthetic cannabinoids and embolic-appearing myocardial infarction. This is the first report of myocardial infarction associated with the currently ‘legal-high’ 5F-AKB48, and may indicate the need for tighter regulation of this compound.

March 2015 Br J Cardiol 2015;22:26 doi:10.5837/bjc.2015.008
Trainee experiences of delivering end-of-life care in heart failure: key findings of a national survey
Yasmin Ismail, Kate Shorthose, Angus K Nightingale

It is widely accepted that end-of-life care for non-cancer conditions has lagged behind that for cancer. The purpose of this survey was to evaluate the confidence of trainees in managing end-of-life issues. An online questionnaire was distributed to all registrar-grade British Junior Cardiac Association members in the UK.
A total of 219 trainees responded. Overall, 73% of trainees feel the care they provide patients with advanced heart failure is poor/adequate. Over 50% of trainees do not feel equipped to discuss advanced-care planning and end-of-life issues. There are 45% who report receiving no training in palliation of advanced heart failure symptoms, while 57% are unhappy with current provision of training. Trainees’ suggestions include more workplace-based supervision with additional regional and national training days, closer links with local hospices, and fellowships for cardiology trainees in palliative care.
Despite being part of the national curriculum for training in cardiology since 2010, trainees’ level of confidence in delivering end-of-life care in advanced heart failure and discussing prognosis is poor. This could be rectified by closer links with palliative care and formal teaching programmes.

March 2015 Br J Cardiol 2015;22:31–3 doi:10.5837/bjc.2015.009
The efficacy of a smartphone ECG application for cardiac screening in an unselected island population
Pierre Le Page, Hamish MacLachlan, Lisa Anderson, Lee-Ann Penn, Angela Moss, Andrew R J Mitchell; from the Jersey International Centre for Advanced Studies

Cardiac screening in the community is limited by time, resources and cost. We evaluated the efficacy of a novel smartphone application to provide a rapid electrocardiogram (ECG) screening method on the Island of Jersey, population 98,000.
Members of the general public were invited to attend a free heart screening event, held over three days, in the foyer of Jersey General Hospital. Participants filled out dedicated questionnaires, had their blood pressure checked and an ECG recorded using the AliveCor (CA, USA) device attached to an Apple (CA, USA) iPhone 4 or 5.
There were 989 participants aged 12–99 years evaluated: 954 were screened with the ECG application. There were 54 (5.6%) people noted to have a potential abnormality, including suspected conduction defects, increased voltages or a rhythm abnormality requiring further evaluation with a 12-lead ECG. Of these, 23 (43%) were abnormal with two confirming atrial fibrillation and two showing atrial flutter. Other abnormalities detected included atrial and ventricular ectopy, bundle branch block and ST-segment abnormalities. In addition, increased voltages meeting criteria for left ventricular hypertrophy (LVH) on 12-lead ECG were detected in four patients leading to one diagnosis of hypertrophic cardiomyopathy.
In conclusion, this novel ECG application was quick and easy to use and led to the new diagnoses of arrhythmia, bundle branch block, LVH and cardiomyopathy in 23 (2.4%) of the total patients screened. Due to its highly portable nature and ease of use, this application could be used as a rapid screening tool for cardiovascular abnormalities in the community.

March 2015 Br J Cardiol 2015;22:37 doi:10.5837/bjc.2015.010
Long-term cardiac rehabilitation and cardioprotective changes in lifestyle
Wolfgang Mastnak

Sustainability of health benefits from cardiac rehabilitation (CR) requires adequate changes in lifestyles. Preventive medicine highlights a triadic guideline referring to cardioprotective behaviour, avoidance of associated polymorbid developments (e.g. depression), and improvement of life-quality. To assess the influence of long-term CR management (in Austria phase 4) offered by the Austrian Heart Association (ÖHV) on changes in lifestyles according to the INTERHEART CHD-risk parameters, a questionnaire measuring the extent of phase 4 influences on lifestyle modifications according to the INTERHEART parameters physical activity, stress, nutrition, body mass index (BMI), smoking, and alcohol was developed. Data were gained from a non-preselected sample of cardiac patients with various diagnoses (n=204; age 41–91, average 71.8; standard variation 7.8, 48% cardiovascular).
ÖHV activities were found to exert a strong influence on health sports (various indoor and outdoor aerobic activities and mobility exercises), stress-reduction, and nutritional adjustment, contrasting low influence on the awareness of diabetes risks and alcohol/nicotine consumption. Social inclusion is considered an important life-quality factor supporting also the sense of security.
Long-term CR management is an efficient instrument for cardioprotective lifestyle modification. The important influence on patients requires especially high sports cardiologic standards and psycho-educational competence. Close collaboration between different phases/stages of CR, as well as similar international organisation should be fostered.
March 2015 Br J Cardiol 2015;22:38 doi:10.5837/bjc.2015.011
Optimising self-management to reduce chronic pain and disability after cardiac surgery
Michael Hugh McGillion, Andrew Turner, Sandra L Carroll, Gill Furze, Jason W Busse, Andre Lamy

While the primary aims of cardiac surgical procedures are to improve survival and ameliorate symptoms, chronic post-surgical pain (CPSP) is a prevalent problem requiring focused attention. Recent years have seen a global emphasis on the development and implementation of self-management (SM) interventions to combat the negative consequences of multiple chronic conditions, including chronic pain. This short report makes recommendations for optimising SM following cardiac surgery to improve pain and related functional outcomes and reduce the risk and impact of CPSP.

February 2015 Br J Cardiol 2015;22:36 doi:10.5837/bjc.2015.004
Experiences from a non-medical, non-catheter laboratory implantable loop recorder (ILR) service
Alun Roebuck, Cara Mercer, Joanne Denman, Andrew R Houghton, Richard Andrews

This paper describes the experiences of developing a non-medical, non-catheter laboratory (cath lab) based implantable loop recorder (ILR) service. ILRs are small subcutaneous single-lead electrocardiogram (ECG) monitoring devices that are placed in a left pectoral pocket under local analgesia. Traditionally, devices have been implanted by medical staff in the cath lab. Each implant can take between 30 and 45 minutes depending on operator skill and patient anatomy. The development of this service has had several major patient and organisational benefits that include shorter waiting times, less cancellations and increased flexibility to implant ‘urgent’ devices in transient loss of consciousness (TLOC). The latter has reduced length of stay within our emergency assessment unit (EAU). Moreover, this service means that the department has been able to undertake more procedures in the cath lab. Data from 2013–14 suggest that an additional 32 × four-hour cath lab sessions were made available for alternative use. Adverse events (infection/erosion) are comparable with published data at less than 1%. To conclude, non-medical, non-cath lab based implantation is safe, cost-effective and has the potential to improve patient experience while increasing both cardiologist and cath lab capacity.
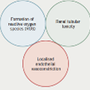
February 2015 Br J Cardiol 2015;22:34 doi:10.5837/bjc.2015.001
Contrast-induced nephropathy in PCI: an evidence-based approach to prevention
Asad Shabbir, Jamie Kitt, Omar Ali

Contrast-induced nephropathy is the third most common cause of in-hospital acute kidney injury and accounts for 10% of total cases. It is commonly encountered following coronary angiography and this systematic review aims to use current evidence to ascertain which treatment modalities are most effective in the prevention of the disease.
A PubMed literature search was conducted in March 2014 using search terms, ‘contrast nephropathy and coronary angiography’. The data analysed included 15 trials and two meta-analyses in order to determine whether patients given N-acetylcysteine (NAC), sodium chloride or sodium bicarbonate had better clinical outcomes. Study data were reviewed and quality of data discussed.
Current data indicate that sodium bicarbonate is as effective as sodium chloride when used in patients with estimated glomerular filtration rate (eGFR) <60 ml/min. NAC adds no statistically significant benefit in mild-to-moderate renal disease regardless of whether it is used in isolation or as an adjunct therapy with fluid.
February 2015 Br J Cardiol 2015;22:35 doi:10.5837/bjc.2015.002
An arrhythmia specialist nurse improves patient care in arrhythmias treated with dronedarone
Moira Allison, Robert T Gerber, Steve S Furniss, Conn Sugihara, A Neil Sulke

The European Medicines Agency (EMA) has mandated that patients treated with dronedarone have regular monitoring. An arrhythmia specialist nurse (ASN) took over the care of patients on dronedarone in 2012.
Patients on dronedarone were identified from hospital notes and pharmacy records. Adherence to EMA guidelines on monitoring before and after the appointment of an ASN were compared. In 112 patients on dronedarone in the year prior to the appointment of an ASN, only 478 of the 1,275 (37%) required tests were actually done. With the ASN, 382 of 422 (92%) tests in 53 patients were performed. This was significantly better (p<0.001). Dronedarone was more likely to be stopped due to contraindications (p<0.017) prior to the appointment of ASN, but afterwards was more likely to be stopped due to side effects (p<0.001).
The ASN significantly improved adherence to EMA-mandated monitoring in patients on dronedarone. Involvement of an ASN had no overall impact on the likelihood of dronedarone being stopped. Patients were more likely to have the drug stopped due to side effects, and were less likely to stop for safety reasons. ASN care is superior to conventional follow-up, and is the gold standard for patients treated with dronedarone.
February 2015 Br J Cardiol 2015;22:27–30 doi:10.5837/bjc.2015.003
Incidence of cardiac surgery following PCI: insights from a high-volume, non-surgical, UK centre
Andrew Whittaker, Peregrine Green, Giles Coverdale, Omar Rana, Terry Levy

Percutaneous coronary intervention (PCI) has established itself as an effective alternative to coronary artery bypass graft surgery (CABG) in appropriate patients. However, the proportion of patients that undergo CABG and/or valve surgery (VS) following PCI in the short and long term is currently unknown.
We conducted a single-centre, retrospective study examining the indications and number of patients requiring CABG and or VS following successful PCI between 2009 and 2012. The surgical procedure was categorised as early (referred within <1 month of the index PCI), mid-term (referred 1–12 months after index PCI) and remote (referred >1 year and up to four years following the index PCI).
During each three-year period (2008–2010, 2009–2011), 5,244 PCIs were performed at our centre. The total number of patients referred for cardiac surgery post-PCI was 63 (1.2%). The number of patients referred for early, mid-term and remote cardiac surgery was 21 (0.4%), 14 (0.26%) and 28 (0.53%), respectively. Within the early group, eight patients had extensive three-vessel disease stabilised with emergency/urgent PCI to allow subsequent CABG, while 10 patients had failed PCI to a chronic total occlusion. In the mid-term group, the main reason for surgery was rapid progression in coronary disease. In the remote group, the majority of patients underwent surgery for progression of valve disease.
Our data suggest that the number of patients requiring CABG and/or VS following PCI is small, and the indications differ with time following the index PCI. We hope that these results will provide reassurance and interest to our interventional colleagues.
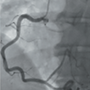
February 2015 Br J Cardiol 2015;22:39 doi:10.5837/bjc.2015.005
Anomalous coronary artery origin: all three arising from right coronary cusp from separate ostia
Vickram Singh, Jeffrey Khoo

A 53-year-old woman presented with history of exertional chest pain. A coronary angiogram subsequently showed an unusual and rare coronary artery anatomy: all of her coronary arteries originate from the right coronary cusp, with separate ostia. In addition, the left anterior descending (LAD) artery was hypoplastic resulting in ischaemia.
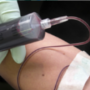
December 2014 Br J Cardiol 2014;21:147–52 doi:10.5837/bjc.2014.035
Predicting long-term morbidity of ACS patients: can NT-proBNP succeed where other biomarkers have failed?
Anna Kate Barton, Stephanie H Rich, Keith A A Fox

Identification of those at low risk of developing heart failure (HF) after acute coronary syndrome (ACS) would aid clinical management, but it is unclear whether N-terminal pro-brain natriuretic peptide (NT-proBNP) adds to the predictive accuracy of troponin. There were 229 subjects recruited into a prospective cohort study. Subjects were assessed for acute heart failure (AHF) prior to discharge and for readmission within 30 days of their ACS event (cohorts A+B). Cohort A (n=116) were further assessed for readmission within 12 months. Troponin I (TnI) and NT-proBNP levels were measured at ACS onset and at 6–12 hours. Readmissions were identified using electronic records. In total, 23.6% of subjects developed AHF during the index admission: 10.0% were readmitted within 30 days of admission; 17.2% within three months; 26.7% within six months and 36.2% within 12 months. At presentation, NT-proBNP, but not TnI, was significantly elevated among subjects who developed AHF compared with non-AHF subjects. Compared with non-readmitted subjects, readmission within 30 days was associated with significantly lower baseline NT-proBNP, and readmission after 30 days with higher baseline NT-proBNP. For all periods, TnI level was lower among readmitted compared with non-readmitted subjects. In conclusion, NT-proBNP has a potential role for rule out of those at low risk of AHF development and readmission.
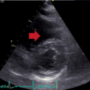
December 2014 Br J Cardiol 2014;21:160 doi:10.5837/bjc.2014.037
Troponin biomarkers: the benefits of echocardiography in a presumed diagnosis of NSTEMI
Mark R Jordan, Farhan Shahid, Richard P W Cowell

In a previous issue of the BJC, key issues regarding the use of high-sensitivity troponin and its use in clinical context were raised.1 Despite the clear benefits with regards to earlier identification of ‘troponin-positive patients’, it is vital to highlight that troponin is specific for myocardial injury, but is not specific for the diagnosis of acute myocardial infarction (MI). Echocardiography is increasingly being used in cases where a ‘troponin-positive event’ is out of keeping with the history and examination for a type I MI. Competent use of this imaging modality can have drastic alterations in the management of patients and potentially prevent invasive cardiological procedures that may later provide more risk than benefit. This case report highlights the caution we must take when requesting troponin biomarkers and the use of echocardiography to aid in the management of the haemodynamically unstable patient.
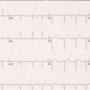
December 2014 Br J Cardiol 2014;21:158 doi:10.5837/bjc.2014.036
Risk of mortality and cardiovascular outcomes among patients newly diagnosed with atrial fibrillation
Debra E Irwin, Michelle Johnson, Simon Hogan, Mark Davies, Chris Arden

This study aimed to assess mortality and cardiovascular (CV) outcomes of patients with newly diagnosed atrial fibrillation (AF) managed in the UK primary care setting. Electronic patient records in The Health Improvement Network were used to identify incident AF (n=9,418, 52.1% male, mean age 73.8 years [standard deviation 11.2]) and matched (gender, age and locality) controls (n=47,090) aged ≥40 years. Three main study outcomes were assessed within two years of follow-up: incident CV outcomes, CV mortality and all-cause mortality. AF cases had an increased risk of developing all investigated CV outcomes when compared with controls (systemic hypertension relative risk [RR]=1.9 [95% confidence interval 1.7–2.1]; peripheral thromboembolic events RR=2.0 [1.8–2.4]; congestive heart failure RR=13.1 [11.5–14.8]; valvular heart disease RR=7.0 [6.0–8.1]; ischaemic heart disease RR=4.3 [3.8–4.8]; stroke RR=3.7 [3.3–4.2]; myocardial infarction RR=3.1 [2.6–3.6]). AF patients were also twice (RR=2.0 [1.8–2.1]) as likely to die from all causes and almost three times (RR=2.7 [2.4–3.1]) more likely to die from CV reasons than controls. AF cases demonstrated consistently worse prognosis across all of the main outcomes assessed when compared with the control patients.

December 2014 Br J Cardiol 2014;21:128–30 doi:10.5837/bjc.2014.031
Hypoglycaemia: patient inconvenience or serious cardiovascular risk?
Vidya Srinivas, Kashif Kazmi, Ketan Dhatariya

Hypoglycaemia is defined as a lower than normal level of blood glucose, and in patients on glucose-lowering therapy, defined as glucose levels less than 4 mmol/L. In the UK, it is usually classified as ‘mild’, if the episode is self-treated, or ‘severe’, if the individual requires third-party assistance. However, the American Diabetes Association definition of hypoglycaemia is different.1 They classify hypoglycaemia into five categories. These are shown in table 1.

October 2014 Br J Cardiol 2014;21:153–7 doi:10.5837/bjc.2014.033
Acute coronary syndromes among South Asian subgroups in the UK: symptoms and epidemiology
Simon W Dubrey, Sarah Ghonim, Molly Teoh

Earlier reports suggest differences in presentation between South Asians and white Europeans experiencing acute coronary syndromes. To compare the demographics and presentation of British South Asians, a long-term prospective survey of a consecutive series of British South Asians was conducted. South Asian patients were analysed as six distinct subgroups, with an overall comparison to a white European cohort.
South Asian patients were of similar mean age, and male predominance (66%), across all subgroups, but as a whole, were younger (62 ± 13 years) than white Europeans (69 ± 14 years), p<0.001. Diabetes was markedly more prevalent in South Asians (range 42–55%) compared with white Europeans (17%), p<0.001. South Asians, as a whole, reported a larger average area of discomfort (5.2 ± 3.5) than did white Europeans (4.4 ± 3.1), p<0.001. Posterior chest discomfort was reported by 38% of all South Asians (range 35–44%) and by 25% of white Europeans, p<0.001. The average intensity of discomfort was similar between white Europeans (6.4 ± 3.2) and South Asian cohorts (6.4 ± 3.0), p=0.80. Differences in ‘intensity of discomfort’ between South Asian subgroups did not reach significance. Silent cardiac events were more common in white Europeans (12.7%) than in South Asians (9.0%), p<0.001.
In conclusion, Asian patients were younger, more likely to be diabetic and tended to report discomfort over a greater area of their body, than did white Europeans. No differences were found between individual South Asian subgroups for pain distribution (extent), character or intensity. South Asian women tended to report a wider distribution of discomfort and intensity than did men across all subgroups.

October 2014 Br J Cardiol 2014;21:159 doi:10.5837/bjc.2014.034
The utilisation of ECG in the Emergency Department
Simiao Liu, Boyang Liu, Han B Xiao

We present an investigation into the use of electrocardiograms (ECGs) in an emergency setting.
September 2014 Br J Cardiol 2014;21:113–14 doi:10.5837/bjc.2014.027
Provision of cardiopulmonary bypass and surgical backup during TAVI: impact on surgical services
Jon R Spiro, Vinod Venugopal, Peter F Ludman, John N Townend, Sagar N Doshi; on behalf of the UK TAVI Steering Group

Providing cardiopulmonary bypass and surgical back-up for transcatheter aortic valve implantation has significant implications for surgical services. It is unclear how practice varies around the UK and whether valve-type influences practice. We performed an email-based survey to gain a UK-wide snapshot of current practice. We found that bypass was available in the catheter lab in 94% of Edwards versus 30% of CoreValve centres (p=0.0003), and that a full surgical team and theatre were kept free in 89% of Edwards versus 20% of CoreValve centres (p=0.008). Further research is required to understand whether this difference in surgical provision, related to valve-type, confers outcome benefit.

September 2014 Br J Cardiol 2014;21:117 doi:10.5837/bjc.2014.028
Is Alice still in Wonderland of the ‘smoker’s paradox’? A meta-analysis of mortality following ACS
Hisato Takagi, Takuya Umemoto; for the ALICE (All-Literature Investigation of Cardiovascular Evidence) Group

To determine whether the ‘smoker’s paradox’ exists in the acute coronary syndrome (ACS) population, we performed the first meta-analysis of adjusted risk estimates separately for early and late mortality. Eligible studies were comparative studies of smokers versus non-smokers enrolling patients hospitalised for ACS and reporting adjusted risk estimates for all-cause mortality.
Twenty-six risk-adjusted studies of smokers versus non-smokers enrolling >700,000 patients with ACS were identified and included. Pooled analysis suggested that smoking was associated with a statistically significant reduction in early (in-hospital or 30-day) mortality for the comparison of current versus never smokers (odds ratio [OR] 0.85; 95% confidence interval [CI] 0.75 to 0.96), any comparisons (current vs. never, former vs. never, current vs. former/never, and current/former vs. never smokers; OR 0.89; 95% CI 0.84 to 0.94), and patients with exclusive ST-segment elevation myocardial infarction (OR 0.80; 95% CI 0.73 to 0.87) and acute myocardial infarction (OR 0.87; 95% CI 0.82 to 0.92). Smoking was associated with a statistically non-significant increase in late mortality for any comparisons (hazard ratio 1.07; 95% CI 0.95 to 1.21).
In conclusion, the ‘smoker’s paradox’ for mortality may exist in the early phase following ACS but it may vanish in the late phase.
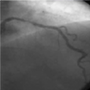
September 2014 Br J Cardiol 2014;21:118–19 doi:10.5837/bjc.2014.029
Audit of cardiac catheterisation in a DGH: implications for training and patient safety
Yasir Parviz, Alex Rothman, C Justin Cooke

We present an investigation into the safety of providing training in coronary angiography within a district general hospital setting.
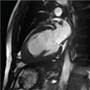
September 2014 Br J Cardiol 2014;21:120 doi:10.5837/bjc.2014.030
Endomyocardial fibrosis in hypereosinophilic syndrome
Theodore M Murphy, Deirdre F Waterhouse, Stephanie James, Niamh Murphy, Rory O’Hanlon

An unusual case of endomyocardial fibrosis presenting secondary to idiopathic hypereosinophilic syndrome, diagnosed with the aid of cardiovascular magnetic resonance (CMR) imaging. This case highlights how CMR imaging is a powerful addition to current non-invasive diagnostic tools, for early clinical diagnosis of eosinophilic endomyocardial disease, and may potentially obviate the need for cardiac biopsy in the future.
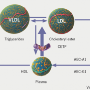
July 2014 Br J Cardiol 2014;21:108–12 doi:10.5837/bjc.2014.023
Targeting residual risk: a new approach to treating CVD?
Alan Begg, Iain Findlay

Lipoproteins play a pivotal role in the development of atherosclerosis, where apolipoprotein B-containing lipoproteins are considered pro-atherogenic and high-density lipoprotein anti-atherogenic. The retention and accumulation of modified low-density lipoprotein in foam cells within the intima of the arterial vessel wall is characteristic of the atherosclerotic process. Conversely, high-density lipoprotein plays an important role in the efflux of excess free cholesterol from the arterial wall through the process of reverse cholesterol transport. High-density lipoprotein also has antioxidant and anti-inflammatory properties that may also confer a protective effect on the vasculature. Statins are the first-line treatment for lowering low-density lipoprotein, but the residual risk of disease remains high. Novel therapies are under investigation that may offer a new therapeutic approach to treating atherosclerosis and additional protection against cardiovascular disease.

July 2014 Br J Cardiol 2014;21:116 doi:10.5837/bjc.2014.025
A survey on the implementation of the NICE guidelines on chest pain of recent onset
John Whitaker, Andrew Wragg, Khaled Alfakih

In 2010, the National Institute of Health and Care Excellence (NICE) published a new guideline for the investigation of patients with chest pain of recent onset. The guidelines were the first to recommend the use of a pre-test probability (PTP) and the first to recommend the use of cardiac computed tomography (CT) in patients with low PTP.
We carried out an online survey of nurses who deliver rapid access chest pain (RACP) clinics and consultant cardiologists to establish current practice and response to the guidelines. Our results demonstrate that assessing PTP is now accepted as a key part of management. The first-choice investigations, at present, for low PTP patients are cardiac CT (used by 44%) and exercise tolerance tests (ETT 43%) with further use of cardiac CT limited only by availability. There is a broad range of investigations used in the medium PTP group including use of all modalities of functional imaging, ETT and cardiac CT. Cardiologists continue to use functional tests including ETT in the high PTP group, but the majority use invasive coronary angiography (ICA) as a first-line test.
This survey shows that the NICE guidelines have been broadly accepted and there are ongoing efforts to implement them, subject to availability of tests and resources. There is some disagreement with the guidelines, with some cardiologists still preferring to use the ETT in all risk groups, and some preferring to use functional imaging tests in higher risk patients, in preference to ICA.
In conclusion, there is very good uptake of the NICE guidelines on management of patients with chest pain. The reasons the guidelines are not fully implemented revolves around availability of resources, as well as a preference for functional tests for the additional prognostic information. This point is supported by the European Society of Cardiology (ESC) guidelines, which have built on and added to the NICE guidelines.
July 2014 Br J Cardiol 2014;21:115 doi:10.5837/bjc.2014.024
Cyanoacrylate topical tissue adhesive for closure of permanent pacemaker wounds
Timothy Watson, Vikrant Nayar, Rachana Prasad, Andrew Ladwiniec, Isma Rafiq, Richard Price, Mark R D Belham, Peter J Pugh

It is unknown whether topical tissue adhesive provides comparable wound healing to absorbable sutures following cardiac device implant. This study was designed to compare wound closure using cyanoacrylate topical tissue adhesive with standard wound closure using absorbable sutures in patients receiving an elective permanent pacemaker implant.
Patients admitted for elective pacemaker implant were randomised to receive wound closure with either absorbable sutures or topical tissue adhesive (glue). Procedure duration, wound closure duration and wound size were recorded. Patients were evaluated at six and 12 weeks post-implant using validated wound evaluation scores by an experienced plastic surgeon who was blinded to the closure method.
Of 122 patients enrolled, 64 received topical tissue adhesive and 58 received absorbable sutures. Patients were well matched for baseline demographics. Use of topical adhesive was associated with shorter wound closure time (117 s, interquartile range [IQR] 92–136 vs. 277 s, IQR 231–311); no difference was seen in overall procedure duration. A total of 100 subjects completed review at 12 weeks. There was no significant difference in any of the wound evaluation scores measured. There was a trend to improvement in cosmetic appearance in patients who received topical adhesive, as judged subjectively by the blinded plastic surgeon. There was no difference in adverse event rates between the two groups.
In conclusion, use of topical tissue adhesive for wound closure following permanent pacemaker implant was not superior to traditional closure techniques with absorbable sutures with regard to cosmetic outcome.
June 2014 Br J Cardiol 2014;21:64–8 doi:10.5837/bjc.2014.015
Using limb-lead ECGs to investigate asymptomatic atrial fibrillation in primary care
Wasim Javed, Matthew Fay, Mark Hashemi, Steven Lindsay, Melanie Thorpe, David Fitzmaurice

Atrial fibrillation (AF) is a dangerous, prevalent condition whose first presentation may be ischaemic stroke. Anticoagulation dramatically reduces stroke risk if patients are first identified. While screening enhances AF detection, it is unclear whether opportunistic pulse palpation or systematic electrocardiogram (ECG) screening is superior.
Patients across 15 general practices in the Bradford and Airedale primary care trust aged over 65 years were invited for a limb-lead ECG. A total of 6,856 patients were subjected to an ECG. This study aimed to determine if screening improved AF detection and the prevalence of cardiac rhythms that may cause an irregular radial pulse.
There were 248 patients diagnosed with AF (3.6%): 153 out of 207 traceable patients were previously diagnosed, hence, screening increased AF detection by 26.1%. Further abnormalities capable of causing an irregular pulse (i.e. ectopy) were highly prevalent at 18.3%. Overall, 99.0% of recorded ECGs were interpretable.
In conclusion, limb-lead ECG screening improved detection rates in a simple and feasible screening strategy, avoiding the need for more costly and cumbersome 12-lead ECG screening. Furthermore, the high prevalence of ectopy suggests systematic ECG screening is more specific than opportunistic screening. This study demonstrates simple ECG models may have a promising potential role in improving AF detection, particularly if asymptomatic.

June 2014 Br J Cardiol 2014;21:75 doi:10.5837/bjc.2014.017
Do NICE tables overestimate the prevalence of significant CAD?
Jaffar M Khan, Rowena Harrison, Clare Schnaar, Christopher Dugan, Vuyyuru Ramabala, Edward Langford

National Institute for Health and Care Excellence (NICE) CG95 guidelines recommend a diagnostic algorithm based on pre-test probability of significant coronary artery disease (SCAD). We hypothesised that these probabilities overestimate the risk of SCAD in our population leading to unnecessary invasive coronary angiography.
Data were collected prospectively for every adult patient attending the rapid access chest pain clinic (RACPC) at a South London acute general hospital from 1 April 2012 to 31 March 2013. SCAD was defined as a luminal narrowing of ≥70% in a major coronary artery or >50% in the left main stem.
There were 551 people assessed with a mean age of 59.9 years; 52% were female. In total, 140 patients underwent coronary angiography. Of these, 79 patients fell within the 61–90% risk bracket, but only 32 (40.5%; 95% confidence interval [CI] 29.7–51.3%) had SCAD. Of patients undergoing angiography, 48 had a risk of >90% but only 26 (54.2%; 95% CI 40.1–68.3%) had SCAD. No individual component of the pre-test probability calculation (age, gender, typicality of symptoms, and cardiac risk factors) predicted an increased chance of SCAD.
We conclude that NICE prediction tables overestimate the risk of SCAD in our patient population. We recommend that the risk tables be updated to represent contemporary patient cohorts in order to reduce the number of potentially unnecessary angiograms.
June 2014 Br J Cardiol 2014;21:72–4 doi:10.5837/bjc.2014.016
Radiation dose reduction among sub-speciality cardiologists and the importance of tibial protection
Thanh T Phan, Muhammad Awan, Dave Williams, Simon James, Andrew Thornley, Andrew G C Sutton, Mark de Belder, Nicholas J Linker, Andrew J Turley

Occupational radiation exposure in fluoroscopy-guided procedures is highest among medical staff, particularly cardiologists involved in interventional procedures. The danger of radiation-induced cataracts in operators, and the suggestion of a higher incidence of malignancy among interventional cardiologists, have led to a significant focus on radiation safety in the cardiac catheterisation laboratory. We examined our mean eye and tibia dosimeter reading trends between 1993 and 2011 (among different sub-specialised cardiologists), and the impact of shin tibia lead protectors. During the period 1993 to 2011 there was a steady decline in radiation doses. The dosimeter readings level fell from a peak of 34 to 6.0 mSv per year and 29 to 1.0 mSv per year at the eye and at the tibia, respectively. Interventional and electrophysiology/pacing cardiologists tend to have a trend of higher radiation doses at the tibia level as compared with non-interventional cardiologists. The introduction of shin leg protectors further reduced radiation exposure from a peak of 6.0 mSv per annum in 2008 to ≤1.0 mSv per annum. Radiation safety awareness and policies have led to a significant fall in operator radiation exposure. The shins, not protected by conventional lead aprons, receive a significant exposure. We have demonstrated that the routine wearing of shin protectors reduces radiation exposure to a minimal level.
June 2014 Br J Cardiol 2014;21:78 doi:10.5837/bjc.2014.018
A UK cardiac centre experience of low-risk, stable chest pain patients with calcium score of zero
Muhammad Ali Abdool, Reza Ashrafi, Michael Davies, Santosh Raga, Huw Lewis-Jones, Erica Thwaite, Peter Wong, Gershan Davis

The 2010 UK National Institute of Health and Care Excellence (NICE) guidelines for assessing patients with ‘chest pain of recent onset’ recommend coronary artery calcium scoring (CACS) to assess patients with a low risk of coronary artery disease (CAD) according to defined criteria. This study aims to evaluate the implementation of these guidelines in an area with a prevalence of CAD higher than the national average.
Consecutive patients with recent onset stable chest pain were assessed by cardiologists in outpatient clinics at University Hospital Aintree, Liverpool, between January and December 2011. A total of 186 patients with a low risk of CAD underwent CACS and follow-on computed tomography coronary angiography (CTCA) if CACS <400.
A CACS of zero was found in 94 patients and three of these were excluded due to motion artefacts. Of the remaining 91 patients, 75 (82.4%) had no visible atheroma, 10 (11%) had minor plaque, five (5.5%) had moderate disease and one (1.1%) had apparent severe disease, which was shown to be a false-positive result on subsequent invasive coronary angiography.
This study shows a negative predictive value for severe disease of 99% for a CACS of 0 in stable patients with a low pre-test probability of CAD. This supports the NICE guidelines, with CACS being the investigation of choice in the UK to rule out significant CAD in selected patient populations. The fact that almost half of all the patients referred for CTCA had a CACS of zero makes this a good quick rule-out tool and, hence, avoids the need for follow-on CTCA.
June 2014 Br J Cardiol 2014;21:80 doi:10.5837/bjc.2014.019
Mahaim fibre tachycardia in a patient with type B Wolff-Parkinson-White syndrome
Rhys Jones, Farhan Shahid, Richard P W Cowell

A 56-year-old male with no previous significant medical history initially presented to his general practitioner for a routine health check prior to starting a new occupation. An electrocardiogram (ECG) was taken that was found to be unusual and, hence, a referral to cardiology outpatients was made. Initial recommendation was made for ablation therapy based on the finding of Wolff-Parkinson-White (WPW) syndrome. After a successful procedure, the patient developed significant palpitations with haemodynamic compromise that required emergency direct current (DC) cardioversion. Subsequent re-investigation found a previously unmasked uncommon form of accessory tachyarrhythmia. This case report highlights the finding of Mahaim pathway in a patient initially treated for WPW syndrome.

April 2014 Br J Cardiol 2014;21:69–71 doi:10.5837/bjc.2014.009
The new oral anticoagulants and management of bleeding
Raza Alikhan

Atrial fibrillation (AF) is the most common sustained arrhythmia faced by clinicians in primary and secondary care. Patients with AF face a significant risk of stroke and thromboembolic complications with associated morbidity and mortality. The role of antiplatelet agents is diminishing, while the use of oral anticoagulants is being actively encouraged. Warfarin has provided the mainstay of oral anticoagulation for more than half a century. New oral direct inhibitors (ODIs) of thrombin and activated factor X – commonly referred to as the new oral anticoagulants (NOACs) – are being prescribed with increasing frequency. These ODIs have a number of advantages over warfarin, including predictable response, no need for monitoring or dose changes and fewer drug and food interactions. Although the risk of intracranial bleeding is reduced, there is still a risk of major haemorrhage as patients are fully anticoagulated. An understanding of the ODIs’ metabolism and excretion, as well as their effects on coagulation tests, is paramount to the management of patients, particularly in emergency situations.
April 2014 Br J Cardiol 2014;21:77 doi:10.5837/bjc.2014.012
Is angiography overused for the investigation of suspected coronary disease? A single-centre study
Colin J Reid, Mark Tanner, Conrad Murphy

The possible overuse of coronary angiography in the investigation of suspected coronary artery disease has been raised as a concern in the literature. We examined our own coronary angiography database to assess the diagnostic yield from angiography in the investigation of patients with suspected coronary artery disease and also the subsequent rate of referral for revascularisation. Some coronary artery disease was found in 66% of patients. However, in spite of an overall diagnostic yield in keeping with National Institute for Health and Care Excellence (NICE) guidelines, only 28% of patients were referred for any form of revascularisation. The optimal use of coronary angiography has important resource implications and the rate of revascularisation may be a useful quality metric.

April 2014 Br J Cardiol 2014;21:76 doi:10.5837/bjc.2014.011
Home- versus hospital-based exercise training in heart failure: an economic analysis
Aynsley Cowie, Owen Moseley

Heart failure (HF) accounts for 5% of all emergency hospital admissions in the UK. To ensure cost-effectiveness, the potential for any intervention to reduce admissions must be balanced against its required investment. This economic analysis compared cost-effectiveness of home- versus hospital-based exercise training as delivered within a randomised-controlled trial (RCT) for HF. The additional costs of delivering eight weeks of home- versus hospital-based training for 46 people with HF, within an established cardiac rehabilitation service, were balanced against emergency hospital admission costs incurred by home-training (n=15), hospital-training (n=15) and control (n=16) groups over five years. The total cost of home-training was £3,244.47 (£196.53 per patient) – much of which was a fixed cost attributed to producing the home-training package. Hospital-training cost £3,656.06 (£221.58 per patient). Over five years, total admission costs for controls (of £157,305.23) were considerably higher than for both home- (£115,735.43) and hospital- (£108,117.51) training groups. In conclusion, both training programmes incurred similar costs, which were offset by a reduction in emergency admission costs, compared with controls. Although hospital-training offered greater potential for reducing admission costs, with larger patient numbers, the cost of home-training per patient would decrease, increasing its likelihood of being the more cost-effective option.

April 2014 Br J Cardiol 2014;21:79 doi:10.5837/bjc.2014.013
Torsades de pointes cardiac arrest associated with severe hypothyroidism
Jakub Lagan, Louise Cutts, Diane Barker, Peter Currie

We present a rare case of cardiac arrest caused by torsades de pointes in relation to severe hypothyroidism, which highlights the importance of thyroid replacement therapy compliance.

March 2014 Br J Cardiol 2014;21:22–8 doi:10.5837/bjc.2014.004
The importance of pre-pregnancy counselling in cardiac disease
P Rachael James

Cardiac disease remains the commonest cause of maternal death in the UK. While some deaths are unavoidable, pre-pregnancy counselling for women with acquired or congenital heart disease is important and counselling should be viewed as the mainstay of clinical practice. It provides women with information about the risk a pregnancy may pose to their health and to that of a foetus and provides an opportunity for an up-to-date assessment of the cardiac condition and a medication review. All cardiologists should recognise the need to raise the issue of pregnancy whenever a diagnosis of acquired heart disease is made in a woman of childbearing age. Although women with heart disease are at increased risk during pregnancy, the majority of women will have a good outcome with careful management.
March 2014 Br J Cardiol 2014;21:33–6 doi:10.5837/bjc.2014.005
High-sensitivity troponin T is detectable in most patients with clinically stable heart failure
Kristopher S Lyons, Gareth McKeeman, Gary E McVeigh, Mark T Harbinson

Troponin levels are used in the diagnosis of acute coronary syndromes (ACS), however, levels may be elevated in many other conditions. A significant proportion of patients with stable heart failure (HF) have detectable levels of troponin using standard assays, however, the incidence of detectable levels of high-sensitivity troponin T (hsTnT) in HF patients is not extensively studied. As part of a trial assessing vascular function in stable HF patients, 32 subjects had hsTnT levels measured at baseline using a multi-channel analyser (Roche E Module). At baseline, 27 (84.4%) patients had detectable levels of hsTnT (median 13.8 ng/L, range 9.2–21.4): 12 (75%) patients in the non-ischaemic group and 15 (94%) in the ischaemic group. A total of 14 (43.8%) patients had levels above the 99th percentile of the normal range. The majority of patients with stable HF will have detectable levels of troponin T using new high-sensitivity assays. A significant proportion of these will be above the cut-off point used for diagnosis of ACS. If these patients present to hospital, modest elevations in hsTnT do not necessarily indicate recent ACS, and serial measurements should be undertaken if clinically indicated.

March 2014 Br J Cardiol 2014;21:39 doi:10.5837/bjc.2014.007
Patient understanding of frequently used cardiology terminology
Jonathan Blackman, Mohammad Sahebjalal

Effective communication is known to increase patient satisfaction and correlates with improved health outcomes. Efforts have been made in recent years to improve communication skills through the use of less complex terminology. This study tests the hypothesis that patient understanding of more simplified terms can be limited and overestimated by doctors. Questionnaires were distributed to hospital inpatients. Patients were asked to define 10 commonly used cardiology terms. The definitions were graded individually according to their accuracy. Doctors were then asked to predict the percentage of patients who they thought would correctly define each term via an online questionnaire. A total of 57 questionnaires were returned. The most poorly understood terms were ‘heart attack’, ‘echo’, ‘leaking heart valve’ and ‘heart failure’ with partially or completely correct definitions offered in only 24.6%, 17.5%, 22.8% and 22.8%, respectively. Approximately 40% of patients felt that too much terminology was used and that explanations offered were inadequate. Doctors’ estimations of patient understanding of these terms were generally inaccurate and prone to overestimation. In conclusion, the cardiology terms chosen were poorly understood by the surveyed patient population, and understanding was frequently overestimated. Caution should be used when using these terms without further clarification.
March 2014 Br J Cardiol 2014;21:38 doi:10.5837/bjc.2014.006
Pacing in patients with congenital heart disease: part 3
Khaled Albouaini, Archana Rao, David Ramsdale

W e continue our series looking at pacing in patients with congenital heart disease. In this final article, we discuss the challenge of device implantation in patients with more complex congenital structural cardiac defects.

March 2014 Br J Cardiol 2014;21:40 doi:10.5837/bjc.2014.008
Statins: are they wonder drugs?
Veena Dhawan, Harsimran Sidhu

Statins are ‘HMG-CoA reductase’ (3-hydroxy-3-methylglutaryl-CoA reductase) inhibitors and attenuate the intracellular levels of cholesterol. By virtue of their multiple pleiotropic modes of action in cardiovascular diseases, statins have also been considered and used for treating various other disorders, with convincing beneficial results, though a few contradictory reports do exist. Taking into account the positive and negative effects of statins, the data need to be viewed with a ‘pinch of salt’ for statins to be labelled as wonder drugs.
February 2014 Br J Cardiol 2014;21:37 doi:10.5837/bjc.2014.003
Outcome and complications following diagnostic cardiac catheterisation in older people
Jenny Walsh, Mark Hargreaves

In a retrospective, case-controlled study, we examined the influence of diagnostic cardiac catheterisation (DCC) on the management of a cohort of very elderly patients (aged over 80 years). Peri-procedure complications were also determined. Study and control patients (aged less than 70 years) were randomly selected from patients who had undergone DCC over the previous five years. Data were collected on the primary treatment outcome (immediately following DCC) and the secondary outcome – the treatment the patient eventually received. We found that, while those in the very elderly group (n=100) were more likely to be referred for surgical intervention as a primary outcome, there was no overall difference in secondary outcome between the two groups. There was no difference in peri-procedural complications between the two groups. We observed that, in very elderly patients, DCC is both safe and contributes to clinical management to a similar degree compared with younger patients.
February 2014 Br J Cardiol 2014;21:29–32 doi:10.5837/bjc.2014.002
Dabigatran improves the efficiency of an elective direct current cardioversion service
Wai Kah Choo, Shona Fraser, Gareth Padfield, Gordon F Rushworth, Charlie Bloe, Peter Forsyth, Stephen J Cross, Stephen J Leslie

Anticoagulation prior to direct current cardioversion (DCCV) is mandatory to reduce the risk of thromboembolism. We examined the impact of the use of dabigatran as an alternative to warfarin on the efficiency of an outpatient DCCV service. A total of 242 DCCVs performed on 193 patients over a 36-month period were analysed. Patients were divided into two cohorts; cohort A included cases in the 22-month period before the introduction of dabigatran and cohort B included cases in the 14-month period after the introduction of dabigatran. All patients in cohort A received warfarin. In cohort B, 48.4% received dabigatran. A larger number of patients from cohort A were rescheduled due to subtherapeutic international normalised ratios (INRs) compared with cohort B (42.1% vs. 15.6%, p<0.001). Those who received dabigatran had significantly lower rates of rescheduling compared with those who received warfarin (9.7% vs. 34.4%, p<0.001). The length of time between initial assessment and DCCV was 24 days shorter in cohort B than cohort A (p<0.001) and 22 days shorter with those who took dabigatran than warfarin (p=0.0015). Outcomes in achieving and maintaining sinus rhythm were comparable in both cohorts and anticoagulants (all p>0.05). This study demonstrates that the use of dabigatran can improve the efficiency of an elective DCCV service.
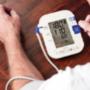
December 2013 Br J Cardiol 2013;20:142–7 doi:10.5837/bjc.2013.33
Renal denervation for hypertension: where are we now?
Hitesh C Patel, Carlo di Mario

Hypertension is a growing clinical burden associated with significant morbidity and mortality. Those patients who remain with uncontrolled blood pressure despite multiple appropriate tablets are labelled as resistant hypertension. This cohort faces the highest risk. A key driving factor in resistant hypertension is an abnormally elevated sympathetic nervous system (SNS). It is now possible to attenuate this non-pharmacologically by performing radiofrequency ablation to the renal sympathetic nerves using a transcatheter approach. Currently available trial data show impressive blood pressure reductions with this therapy and, more importantly, its relative safety. The National Health Service (NHS) experience with this procedure is at an early stage, but is likely to grow with guidance already published by the joint British Societies and National Institute for Health and Care Excellence (NICE).
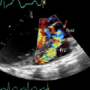
December 2013 Br J Cardiol 2013;20:156 doi:10.5837/bjc.2013.35
Giant aortic sinus fistula
Jason M Tarkin, Waleed Arshad, Arvinder Kurbaan, Timothy J Bowker, Han B Xiao

A 34-year-old Filipino computer engineer with no previous medical history presented to the emergency department with sudden onset exertional breathlessness and intermittent palpations for 10 days. He had no associated dizziness, syncope or chest pain, and no significant family history or recent travel. Blood pressure was 126/69 mmHg and pulse 104 bpm, regular with normal volume and character. The jugular venous pressure was normal. A 4/6 continuous murmur with diastolic accentuation was heard loudest at the left lower sternal edge, associated with a diastolic thrill. Electrocardiogram (ECG) showed sinus tachycardia and no other abnormality.
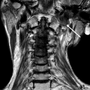
December 2013 Br J Cardiol 2013;20:157–9 doi:10.5837/bjc.2013.36
Recurrent syncope in head and neck cancer: a case report with literature review
James Maurice, Hariharan Kuhan, Han B Xiao

A 68-year-old male with a background fhistory of squamous cell carcinoma of the epiglottis presented with recurrent syncope. During a witnessed collapse in Accident and Emergency (A&E), his heart rate decreased to 38 bpm and blood pressure dropped to 74/50 mmHg. Electrocardiogram (ECG) confirmed sinus bradycardia. Magnetic resonance imaging (MRI) of his neck revealed disease recurrence with a mass encasing the left internal carotid artery. He was diagnosed with reflex syncope secondary to mechanical stimulation of the carotid sinus. He had a dual-chamber pacemaker inserted, and re-presented with one further episode of collapse shortly afterwards. This report discusses the different options in managing this rare but debilitating symptom in head and neck cancers invading the carotid sinus.

November 2013 Br J Cardiol 2013;20:140–1
The art of bluffing
Heather Wetherell

In this new regular series ‘ECGs for the fainthearted’ Dr Heather Wetherell will be interpreting ECGs in a non-threatening and simple way. She hopes this will help keep the art alive in primary care. In this first article, she looks at ECG methodical analysis
November 2013 Br J Cardiol 2013;20:149–150 doi:10.5837/bjc.2013.30
Echocardiography is not indicated for an enlarged cardiothoracic ratio
Lucinda Wingate-Saul, Yassir Javaid, John Chambers

An increased cardiothoracic ratio (CTR) on chest X-rays is a not uncommon reason for requesting echocardiography. To assess how often the echocardiogram was abnormal in patients with an increased CTR, the results of 62 open-access echocardiograms requested with this indication were analysed. Means, standard deviations and 95% confidence intervals were calculated for the left ventricular diameters of the patient group investigated. Two-tailed t-tests were used to compare those with and without reported breathlessness, and those with additional radiology consistent with heart failure. Positive predictive values (PPVs) were calculated. Only four echocardiograms were abnormal, giving a PPV for CTR of 6%. This increased only slightly to 15% with the inclusion of another radiological abnormality, and to 19% with a symptom or sign. We, therefore, conclude that an increased CTR alone is not a valid reason for requesting echocardiography.
November 2013 Br J Cardiol 2013;20:151–3 doi:10.5837/bjc/2013.31
Pacing in patients with congenital heart disease: part 2
Khaled Albouaini, Archana Rao, David Ramsdale

We continue our series looking at pacing in patients with congenital heart disease. In the second article, we discuss the challenge of device implantation in patients with more complex congenital structural cardiac defects.
November 2013 Br J Cardiol 2013;20:155 doi:10.5837/bjc.2013.34
A comparison between CTCA and functional testing for stable chest pain and moderate-to-high CAD risk
Andrew Cai, Peter Dobson, Phoebe Leung, Kathy Marshall, Mohamed Albarjas, Toby Rogers, Sumit Basu, Khaled Alfakih

The National Institute for Health and Care Excellence (NICE) guidelines on chest pain recommended the use of computed tomography coronary angiography (CTCA) in patients with low pre-test probability, functional tests in patients with moderate pre-test probability, and invasive coronary angiography (ICA) in patients with high pre-test probability, of having coronary artery disease (CAD). A previous audit demonstrated low incidence of CAD in patients with moderate and high pre-test probabilities. We investigated these patients non-invasively and assessed outcome. We retrospectively reviewed 213 consecutive patients who were seen in the outpatient setting and had a moderate or high risk of CAD based on NICE CAD score. We compared the performance of the tests. CTCA was performed in 107, stress echo in 67 and myocardial perfusion scintigraphy (MPS) in 39 patients. The MPS group were older (p<0.01) and had a higher incidence of risk factors (p<0.01). Of the patients undergoing CTCA, 9.4% were found to have significant CAD requiring revascularisation. Functional testing led to revascularisations in 4.7%. The higher rate of revascularisation in the CTCA cohort was not statistically significant (p=0.28). Our real-world data suggest that CTCA can be at least as effective as functional tests in detecting significant CAD and may lead to more revascularisations than functional tests. CTCA should be considered as an effective alternative to functional tests in patients with higher pre-test probability of CAD in hospitals with limited access to functional tests.

September 2013 Br J Cardiol 2013;20:148 doi:10.5837/bjc.2013.029
Dual antiplatelet therapy and upper gastrointestinal bleeding risk: do PPIs make any difference?
Inamul Haq, Fazal-ur-Rehman Ali, Shakeel Ahmed, Steven Lindsay, Sudantha Bulugahapitiya

Dual antiplatelet therapy (DAT) with aspirin and clopidogrel is recommended for up to one year following acute coronary syndrome (ACS). Gastrointestinal bleeding is the main hazard of this treatment and proton pump inhibitors (PPIs) are often prescribed in selected patients to reduce this risk. The main purpose of this study was to analyse the effect of PPIs in reducing the subsequent risk of gastrointestinal bleeding.
The medical records of 177 consecutive patients treated with DAT following ACS, were specifically reviewed for the study parameters over a 12-month period.
The mean age was 66 years (range 24–96) with a median value of 68 years; 67% were males and 33% females, 74% Caucasians and 26% Asians. Patients were divided into two groups: the PPI group (patients on DAT and PPIs, n=91) and the control group (patients on DAT only, n=86). In the PPI group, 55% were on lansoprazole, 34% on pantoprazole and 11% on omeprazole.
Out of the 177 patients, evidence of upper gastrointestinal bleeding was found in 10 patients, with the mean age of these patients being 77 years in the PPI group and 53 years in the control group. In the PPI group, endoscopy findings from six patients (6.6%) revealed gastritis in four, bleeding angiodysplasia in one, and bleeding oesophagitis in one; while the findings for the four patients in the control group (4.6%) showed gastritis in two, gastric ulcer in one and Mallory Weiss tear in one (odds ratio: 1.45, 95% confidence interval 0.39–5.32, p=0.58). None of these patients had a previous history of gastrointestinal bleeding.
In conclusion, empirical prophylactic prescription of PPIs for patients on DAT following ACS is of no significant benefit in reducing their predisposition to upper gastrointestinal bleeding. However, studies utilising larger populations are warranted to confirm this conclusion.
September 2013 Br J Cardiol 2013;20:103-5 doi:10.5837/bjc.2013.022
Cardiovascular magnetic resonance training in the UK: an update from the BSCMR trainee observers
David P Ripley, Nigel J Artis, John Paul Carpenter, Francisco Leyva

Cardiovascular magnetic resonance (CMR) imaging is a rapidly developing subspecialty with a clear training structure and good career prospects. Demand for CMR demand is growing rapidly, with an 85% increase in cases scanned nationally in only two years, and this demand is predicted to continue with the British Cardiovascular Society working group predicting a further trebling of demand in the five years from 2010 to 2015. The most recent British Junior Cardiology Association survey identified cardiovascular imaging as an increasing preference for subspecialty training with 22% of trainees choosing imaging in 2012 (up from 10% in 2005) and CMR as the preferred imaging modality (selected by 45%). However, it was highlighted that there were still difficulties in accessing training by around one third of trainees. We describe the common indications for CMR, what CMR training involves (including the accreditation process), as well as how trainees can access current training opportunities.

September 2013 Br J Cardiol 2013;20:109–12 doi:10.5837/bjc.2013.026
High-sensitivity troponin: six lessons and a reading
James H P Gamble, Edward Carlton, William Orr, Kim Greaves

New high-sensitivity troponin assays will reduce the threshold for the diagnosis of myocardial infarction (MI), as specified in the 2012 third Universal Definition of MI. They will also allow earlier diagnosis of MI, but serial testing is required for adequate specificity. They convey prognostic information in both MI and in other acute conditions. Interpretation of troponin results must be in combination with a full assessment of the clinical context.
This review discusses these concepts and developments in this area.
September 2013 Br J Cardiol 2013;20:117–20 doi:10.5837/bjc/2013.028
Pacing in patients with congenital heart disease: part 1
Khaled Albouaini, Archana Rao, David Ramsdale

Only a small proportion of patients requiring pacemaker or defibrillator implantation have congenital cardiac abnormalities. Patients with such anomalies can be divided into two categories: those with undiscovered congenital abnormalities, which had not given rise to symptoms or other obvious physical signs, and those known to have congenital abnormalities having had surgical intervention or not.
Pacemaker implantation in these two groups of patients may give rise to practical challenges and the implanting physician should be familiar with them so that potential problems can readily be recognised. In this, and the subsequent articles, we will cover the most common congenital cardiac anomalies with relevance to cardiac device implantation.

September 2013 Br J Cardiol 2013;20:116
Audit of communication with GPs regarding renal monitoring in CHF patients: a comment from primary care
Dr John B Pittard

Dr John B Pittard, a general practitioner in Staines, comments on whether implementing these research findings is achievable in primary care

July 2013 Br J Cardiol 2013;20:106 doi:10.5837/bjc.2013.021
National survey of patients with AF in the acute medical unit: a day in the life survey
John Soong, Anjali Balasanthiran, Donald C MacLeod, Derek Bell

Atrial fibrillation (AF) is the most common cardiac dysrrhythmia. The evidence base and expert consensus opinion for management have been summarised in several international guidelines. Recent studies suggest a disparity between contemporary practice and perceived best practice.
An electronic questionnaire was constructed to capture details of patient demographics and current practice, including risk assessment for stroke and major bleeding. All patients >18 years with AF as a primary or secondary diagnosis admitted from midday on the 14th September 2011 to midday on the 15th September 2011, were included in the survey. Participating units were recruited from the Society for Acute Medicine registry, and provided with an electronic link and password to enter data for individual patient episodes.
The electronic questionnaire was completed for 149 patient episodes from 31 acute medical units (AMUs) across the UK. The typical patient with AF presenting to the AMU is older, has important medical comorbidities (sepsis in almost a third) and frequently presents out of hours. Initial management was digoxin alone in 22% and 23% had a documented stroke risk assessment, not in-keeping with current guidelines.
This relatively simple methodology yields valuable insight into the real world management of AF, providing an additional evidence base.
July 2013 Br J Cardiol 2013;20:107 doi:10.5837/bjc.2013.024
An update on treatments for amyloid heart disease
Simon W Dubrey

Patients with amyloid heart disease have historically been considered to have a very poor prognosis and were considered almost untreatable. However, recent therapeutic advances are encouraging and likely to have a marked effect on management across the amyloid spectrum. This message needs to be conveyed to cardiologists, not least because there is now benefit to performing an endomyocardial biopsy to determine amyloid type. We provide an update on the significant progress in managing the three most common forms of amyloid heart disease in the UK.

July 2013 Br J Cardiol 2013;20:108 doi:10.5837/bjc.2013.025
CTCA outperforms ETT in patients with stable chest pain and low-to-intermediate predicted risk
Toby Rogers, Michael Michail, Simon Claridge, Andrew Cai, Kathy Marshall, Jonathan Byrne, Narbeh Melikian, Khaled Alfakih

Our objective was to compare the performance of computed tomography coronary angiography (CTCA) with exercise tolerance testing (ETT) in patients presenting with stable chest pain with low-to-intermediate predicted risk of coronary artery disease (CAD) as defined by the UK National Institute for Health and Care Excellence (NICE) clinical guideline 95. We investigated 85 patients with ETT and 102 patients with CTCA as first-line investigations after clinical assessment. Outcome measures assessed were diagnosis or exclusion of CAD, referral for second-line investigations, false-positive rate and cost of investigation to reach diagnosis for each modality.
CTCA was diagnostic in more patients than ETT (95.1% vs. 80.0%, p<0.05), had a lower false-positive rate (2.9% vs. 17.6%), led to fewer referrals for second-line investigations (4.9% vs. 21.2%, p<0.05) and resulted in overall comparable cost of investigation per patient (£183.44 vs. £165.16, p=0.49).
In conclusion, CTCA outperforms ETT as a first-line investigation in the investigation of patients presenting with stable chest pain with low-to-intermediate predicted risk of CAD as defined by NICE clinical guideline 95.

June 2013 Br J Cardiol 2013;20:61–4 doi:10.5837/bjc.2013.16
Assessing kidney function in oral anticoagulant prescribing: an aid for safer drug and dose choices
Su Wood, Duncan Petty, Matthew Fay, Andrew Lewington

Incidence of stroke attributable to atrial fibrillation increases from 1.5% at age 50–59 years to 23.5% at age 80–89 years. The use of oral anticoagulants to reduce the risk of stroke is well established, but all the available agents can cause bleeds if used in excess dose, in high-risk patients or in patients with reduced kidney function.
This article highlights the need to assess kidney function as stated in the newly published European Heart Rhythm Association (EHRA) of the European Society of Cardiology (ESC) practical guide on the use of the new oral anticoagulants (NOACs).1 The EHRA guide has a section on NOACs for patients with chronic kidney disease (CKD) where it is stated that “a careful follow-up of renal function is required in CKD patients, since all (NOACs) are cleared more or less by the kidney”. It continues “in the context of NOAC treatment, creatinine clearance is best assessed by the Cockcroft method, as this was used in most NOAC trials”.
The authors discuss the issues and present a simple guide on why and how to use the Cockcroft Gault equation for kidney function estimation. They also note that for drug and dosing decisions, reduced kidney function, for whatever reason (not just where a patient has been assessed as having CKD), needs to be assessed to reduce the risk of harm.
June 2013 Br J Cardiol 2013;20:65 doi:10.5837/bjc.2013.17
Prognostic value of renal function in STEMI patients treated with primary PCI: ANIN Registry
Magdalena Polanska-Skrzypczyk, Maciej Karcz, Pawel Bekta, Cezary Kepka, Jakub Przyluski, Mariusz Kruk, Ewa Ksiezycka, Andrzej Ciszewski, Witold Ruzyllo, Adam Witkowski

Chronic kidney disease (CKD) adversely affects cardiovascular outcomes and mortality in the general population. We sought to determine the impact of renal function on angiographic and clinical results in ST-elevation myocardial infarction (STEMI) patients treated with primary percutaneous coronary intervention (pPCI).
Analyses were based on the prospective ‘all-comer’ registry of 1,064 consecutive STEMI patients treated with pPCI in our tertiary centre between February 2001 and October 2002. Admission serum creatinine concentration was known in 894 patients (84%). Mean serum creatinine was 105 ± 27 µmol/L and estimated glomerular filtration rate (eGFR) was 67 ± 18 ml/min/1.73 m2. Thrombolysis in Myocardial Infarction grade 3 (TIMI3) flow was achieved in 751 patients (84%). During hospitalisation, 29 (3%) major bleedings, five (1%) strokes and 12 (1%) re-infarctions occurred. By day 30, two patients were lost to follow-up and 41 (5%) were dead. Renal function was independently associated with 30-day mortality (hazard ratio [HR] 1.6, 95% confidence interval [CI] 1.2–2.1, p=0.003). In CKD patients (eGFR <60 ml/min/1.73 m2), TIMI3 flow was restored less frequently (79% vs. 87%), in-hospital major adverse cardiac and cerebrovascular events (MACCE) were more frequent (15% vs. 4%) and 30-day mortality was higher than in non-CKD patients (9% vs. 2%). Lower eGFR was associated with increased risk of major bleeding (HR 1.6, 95% CI 1.3–2.1, p<0.0005). In the subgroup of conscious patients with normal serum creatinine, eGFR remained significantly associated with 30-day mortality.
In conclusion, renal function expressed by eGFR is an independent predictor of procedural success and short-term outcomes in STEMI patients treated with pPCI, even in patients with normal serum creatinine. Thus, eGFR should be estimated in all STEMI patients to help identify a high-risk subgroup.

June 2013 Br J Cardiol 2013;20:67–71 doi:10.5837/bjc.2013.18
Iterative reconstruction algorithms allow greater diagnostic certainty in 64-slice platforms: CAPIR results
Peter McKavanagh, Lisa Lusk, Peter A Ball, Tom R Trinick, Ellie Duly, Gerard M Walls, Sarah McCusker, Mohammad Alkhalil, Claire Louise McQuillan, Mark T Harbinson, Patrick M Donnelly

This study was designed to evaluate the impact of a novel iterative reconstruction (IR) algorithm on an established UK cardiac computerised tomography (CT) service. Areas assessed included image quality and effective radiation dose (ED). A total of 250 consecutive patients with suspected coronary artery disease were enrolled as a substudy of a larger trial. Examinations were performed on a 64-channel detector CT with data sets reconstructed with the standard filtered back projection (FBP) or IR technique. Image noise was measured within predefined regions of interest (ROI), and image quality qualitatively assessed by two clinicians blinded to the reconstruction method. ED was calculated using a chest-specific conversion coefficient. Four patients withdrew. So, 246 patients (140 males) underwent cardiac CT: 124 consecutive patients underwent a routine scanning protocol, with images reconstructed with FBP, and 122 patients with IR technique. The mean estimated EDs were 6.5 mSv (FBP) and 4.3 mSv (IR) (dose savings 34%) for all patients (p<0.00001). There was no statistical difference in noise or mean attenuation between the IR and FBP images. The mean IR image quality score was 3.67 ± 1.04 compared with 3.29 ± 1.17 for FBP images (p<0.001). IR in cardiac CT offers substantial ED reduction without compromise in image quality.

June 2013 Br J Cardiol 2013;20:79 doi:10.5837/bjc.2013.19
Large mass in right atrium after CABG – myxoma, adrenal metastasis or in-transit thrombus?
Pankaj Kaul, Rodolfo Paniagua, Subbarayulu Balaji, Phil Batin

A 73-year-old woman, with a history of deep vein thrombosis (DVT) in her legs, presented two years following coronary artery bypass graft (CABG) with left internal mammary artery (LIMA), left radial artery and left cephalic vein, with a massive right atrial mass. Pre-operative work up also showed a left adrenal mass on computed tomography (CT) scan. We discuss the diagnostic possibilities within such a scenario and review the literature for right atrial masses of diverse aetiology, including right atrial myxomas, benign and malignant tumours of right atrium and right atrial thrombosis. The case is unusual on account of the concomitant history of DVT and the presence of left adrenal mass, rapid growth of the mass within two years following CABG, the atypical origin of the myxoma near inferior vena caval opening and the near total obliteration of the right atrial myxoma by rapid growth of myxoma to a massive size.

April 2013 Br J Cardiol 2013;20:72–6 doi:10.5837/bjc.2013.013
Assessing the health-related quality of life in patients hospitalised for acute heart failure
Paul Swinburn, Sarah Shingler, Siew Hwa Ong, Pascal Lecomte, Andrew Lloyd

Acute heart failure (AHF) is a common cause of hospitalisation, presenting substantial economic and humanistic burden for healthcare systems and patients. This study was designed to capture proxy UK health-related quality of life (HRQoL) data for hospitalised patients with AHF.
Proxy assessments of HRQoL for patients were obtained from 50 experienced UK cardiac nurses (formal caregivers) and from 50 UK individuals who acted as caregivers for patients who had experienced an AHF event leading to hospitalisation (informal caregivers). Data were collected retrospectively for four time points (days 1, 3, 5 and 7 post-hospital admission for AHF event) using the EQ-5D. Results show a disparity in reported HRQoL at day 1 values between caregiver types (mean single utility index 0.20 vs. 0.68, respectively, p<0.001). By day 7, formal caregivers rated typical patients’ HRQoL as being comparable to informal caregivers’ assessments (0.82 vs. 0.73, respectively, p=0.145).
In conclusion, collection of utility data in severe acute conditions is challenging. This study captures values through the use of proxy assessment. Data suggest that AHF hospitalisation is associated with a significant HRQoL burden and that there exists a need for development of new treatments aimed at improving hospitalisation outcomes.

April 2013 Br J Cardiol 2013;20:78 doi:10.5837/bjc.2013.012
A pilot study to investigate the safety of exercise training and testing in cardiac rehabilitation patients
Garyfallia Pepera, Paul D Bromley, Gavin R H Sandercock

We conducted a pilot study to evaluate the safety of the shuttle walking test (SWT) and exercise training for cardiac patients in community-based cardiac rehabilitation settings. Overall, 33 cardiac patients were tested (19 males and 14 females, 67 ± 8 years). Eleven cardiac patients (testing group) and 22 cardiac patients (training group) underwent ambulatory electrocardiogram (ECG) monitoring during the SWT and exercise training during a long-term cardiac rehabilitation programme. Frequency of ECG events was reported for the two groups. Chi-square test was performed to determine associations between the incidence of cardiovascular events and poor functional capacity (SWT <450 m).
The findings showed only minor events provoked during the SWT or exercise training, and no event-related hospitalisation, syncope episodes or fatality. The most important cardiac event was silent myocardial ischaemia (testing group: 27.3%; training group: 18%). Poor functional capacity was not associated with the risk of a cardiac event during exercise (testing group: χ2=0, p=0.99, phi=0.24; training group: χ2=2.1, p=0.15, phi=–0.42).
In conclusion, supervised exercise testing and training are accompanied only by minor cardiovascular events and they can be carried out safely in community-based cardiac rehabilitation settings.
March 2013 Br J Cardiol 2013;20:27–31 doi:10.5837/bjc.2013.006
Percutaneous coronary intervention in the very elderly (≥85 years): trends and outcomes
Omar Rana, Ryan Moran, Peter O’Kane, Stephen Boyd, Rosie Swallow, Suneel Talwar, Terry Levy

This single-centre, retrospective, cohort study aims to provide insight into the long-term survival of patients ≥85 years old undergoing percutaneous coronary intervention (PCI) over a four-year observational period in a high-volume PCI centre. Between 2006 and 2010, 294 patients (mean age 88 ± 2 years, 56% male) underwent PCI at our institute. A total of 180 patients (61.2%) had an acute coronary syndrome (ACS) defined as unstable angina, non-ST elevation myocardial infarction (NSTEMI) or ST-elevation myocardial infarction (STEMI). One hundred and fourteen patients underwent PCI electively (38.8%). The primary outcome was all-cause 30-day and one-year mortality rates. In-hospital, 30-day and one-year mortality rates were 2.4% (7 patients), 4.4% (13 patients) and 17.7% (52 patients), respectively, in the entire cohort. In addition, 30-day (5.6% vs. 3.4%, p=0.24) and one-year (20.0% vs. 14.0%, p=0.19) mortality rates were similar between the ACS and elective patients, respectively. Following multi-variable analysis, age (hazard ratio [HR] 1.14, 95% confidence interval [CI] 1.04 to 1.26), male sex (HR 1.85, 95% CI 1.01 to 3.42), previous PCI (HR 2.74, 95% CI 1.36 to 5.56) and the presence of shock (HR 15.39, 95% CI 6.67 to 35.50) emerged as independent predictors of one-year mortality rates. We conclude that PCI appears to be a safe treatment option in very elderly patients with good one-year survival rates. Future randomised-controlled trials should specifically include this age group to guide interventional cardiologists in making decisions when faced with this very challenging cohort.

March 2013 Br J Cardiol 2013;20:32–7 doi:10.5837/bjc.2013.007
Primary angioplasty for acute STEMI in secondary care: feasibility, outcomes and potential advantages
Andrew Whittaker, Lee Rowell, Olayiwola Olatawura, Petra Poliacikova, Jason Glover, Carl I Brookes, Andrew J Bishop

Primary percutaneous coronary intervention (PCI) has become treatment of choice for ST-elevation myocardial infarction (STEMI) in England. The assumption in most trials, and in their translation into clinical practice, is that centralisation of primary PCI for STEMI into large facilities is inevitable and essential. We feel that a successful and preferable primary PCI service can be delivered in a medium-sized district general hospital (DGH).
We performed a retrospective analysis of the first 18 months of primary PCI for STEMI in our unit. We compared our results with standards set out in the National Infarct Angioplasty Project report. Our median call-to-balloon time was 95 minutes and median door-to-balloon time was 50 minutes. Door-to-balloon times were shorter during working hours than out of hours, and were shorter for patients taken directly to the catheterisation laboratory than those admitted via A&E. During the period of assessment, 14% of patients experienced a major adverse cardiovascular and cerebrovascular event (MACCE). The overall mortality rate was 6.7%. No patients were transferred to our surgical centre for emergency treatment.
We believe our data demonstrate that a system utilising regional Heart Attack Centres is not essential for satisfactory clinical outcomes, and may not be the preferred choice for patients and their ongoing post-myocardial infarction care. Expansion of PCI services in well-organised DGHs may be an equally good solution.

March 2013 Br J Cardiol 2013;20:38 doi:10.5837/bjc.2013.008
How to untie a transfemoral catheter knot with a transradial Lasso
John Rawlins, Nimit Shah, Suneel Talwar, Peter O’Kane

Diagnostic coronary angiography (CA) remains the gold-standard assessment of coronary artery disease (CAD). Transfemoral access remains a commonly used approach. Arterial tortuosity can lead to difficulties in coronary engagement, particularly when intubating the right coronary artery (RCA). Excessive catheter manipulation may result in knotting.

March 2013 Br J Cardiol 2013;20:40 doi:10.5837/bjc.2013.009
Eliminate non-cardiac chest pain
Richard A Best

Eliminate non-cardiac chest pain. Or rather, eliminate the expression. Cumulative irritation over several years leads me to comment on the readiness of doctors to use this, and ‘atypical chest pain’, as a diagnosis, and even carry out trials to assess treatment. To study a condition defined by what it is not seems weird; perhaps some people also describe non-brain head pain or atypical abdominal pain?
February 2013 Br J Cardiol 2013;20:39 doi:10.5837/bjc.2013.002
Feasibility of using CTCA in patients with acute low-to-intermediate likelihood chest pain in a DGH
Michael Michail, Shubra Sinha, Mohamed Albarjas, Kate Gramsma, Toby Rogers, Jonathan Hill, Khaled Alfakih

Current European Society of Cardiology guidelines state that in troponin-negative acute coronary syndrome with no ST-segment change on electrocardiogram (ECG), a stress test is recommended. In the UK, exercise tolerance testing (ETT) is currently the most common first-line test. The high proportion of false-positive and inconclusive results often mandates second-line tests. We compared the diagnostic accuracy and cost implication of computed tomography coronary angiography (CTCA) as first-line investigation compared with ETT. We hypothesised that CTCA would outperform ETT because of its excellent negative-predictive value.
Our results suggest that it is feasible to use CTCA to investigate patients with acute low-to-intermediate likelihood chest pain in place of ETT at no extra cost. Moreover, this cost analysis only took into consideration the actual cost of investigation. Three US clinical trials have shown that CTCA in the emergency room can substantially reduce patient length of stay, reducing overall cost further. CTCA also recognises non-obstructive coronary atheroma, which, combined with clinical risk factors, may prompt the physician to initiate secondary prevention medication earlier.
November 2012 Br J Cardiol 2012;19:167–9 doi:10.5837/bjc.2012.029
Secondary prevention regimens and risk factors are not optimised in patients re-admitted with ACS
Krishnaraj S Rathod, Shoaib Siddiqui, Barron Sin, John Hogan, Sandy Gupta

An observational study was conducted on patients with pre-existing coronary heart disease who were re-admitted to an acute district general hospital with a further acute coronary event. Their demographics, admission drug therapies and cardiovascular risk factor parameters were recorded and analysed. Of the 100 patients admitted over a nine-month period, more than a quarter of them were taking suboptimal secondary prevention drug therapies. Furthermore, a proportion of patients were not achieving adequate cholesterol, blood pressure and heart rate targets, which, in turn, may be a major contributory factor for their re-presentation to hospital.

November 2012 Br J Cardiol 2012;19:170–2 doi:10.5837/bjc.2012.030
Incidence screening for primary prevention ICDs based on UK guidelines following STEMI
Ellen Berry, Helen Padgett, Melanie Doyle, Arif J Ahsan, Andrew D Staniforth

We conducted an observational study within a cardiology tertiary centre with the aim of increasing the primary prevention implantable cardioverter defibrillator (ICD) implantation rate in line with Heart Rhythm UK (HRUK) national target.
A total of 326 patients experienced ST-elevation myocardial infarction (STEMI) over a 14-month time period and were offered incidence screening for implantation of a primary prevention ICD at six weeks according to National Institute for Health and Clinical Excellence (NICE) guidelines (TA095). There were 273 (84%) patients who completed the screening process; 26 (8%) had an ejection fraction (EF) of <35%. Two patients had an EF of <30% with a QRS duration >120 msec. Two of 22 subjects had evidence of non-sustained ventricular tachycardia on 24-hour Holter monitoring; one had a positive ventricular tachycardia stimulation test. Overall, three patients received an ICD (0.9%).
In conclusion, this process was labour intensive and had a lower than expected yield.
November 2012 Br J Cardiol 2012;19:173–7 doi:10.5837/bjc.2012.031
Trends in atrial fibrillation hospitalisation in Scotland: an increasing cost burden
Martin Keech, Yogesh Punekar, Anna-Maria Choy

The objective of our study was to evaluate the impact of atrial fibrillation (AF) on secondary care costs in Scotland. Patient hospitalisation data from the Information and Statistics Division (ISD) of the Scottish National Health Service (NHS) from 2004 to 2008 were analysed to estimate trends in hospital episodes in the 5.2 million population of Scotland. The associated costs were estimated using the tariff prices in Scotland for the respective years.
Over the five-year period, AF-related hospital discharges increased by 33% compared with 20% for all cardiovascular discharges (29 and 37 per 1,000 population respectively). There were increases of: 21% in number of patients hospitalised; 27% in AF-related hospital admissions; and 15% in total patient bed days. Despite decreasing trends, mean length of inpatient stay for AF remained higher than for total cardiovascular conditions (10.9 vs. 8.7 days), as did inpatient cost per patient (£6,009 vs. £5,586). AF-related hospital costs increased from £138.9 million in 2004 to £162.5 million in 2008, accounting for 24% of all cardiovascular hospital costs. Overall, the burden of AF was higher among women and increased progressively with age.
In conclusion, AF presents a significant and increasing burden on hospital care in Scotland. At 25% of the total cardiovascular burden, AF costs are increasing relatively faster.

November 2012 Br J Cardiol 2012;19:178–9 doi:10.5837/bjc.2012.032
Cardiovascular innovations: role, impact and first-year experience of a physician assistant
Susan Collett, Devan Vaghela, Ameet Bakhai

Improving patient access and implementation of the European Working Time Directive has proved a challenge for the National Health Service (NHS), particularly adding to workforce pressures and reducing continuity of care for patients. Innovative service and workforce redesign led to the introduction of new and extended roles based on service need. This paper outlines the introduction of one such new role, physician assistant (PA), introduced in the NHS in 2006, based on the established US PA model. UK-trained PA graduates are taking up newly created posts in primary and acute healthcare trusts and the aim of this paper is to share the first-year experience of introducing a newly qualified UK-trained PA within a busy district general hospital cardiology department, describing the internship year, achievements, limitations and how the role has evolved in line with service need. We believe the role has ideal potential in a cardiology department and, in particular, in the management of long-term chronic conditions, such as heart failure, where the number of specialist contacts with the patient can directly impact admissions, re-admissions, length of stay, adherence to medications and protocols of care positively.

November 2012 Br J Cardiol 2012;19:180–3 doi:10.5837/bjc.2012.033
Sheffield’s nurse-led heart failure clinic: the patients’ opinions
Kathryn Drewry, Louisa Yates, Andrew Birchall, Donna Barnett, Natalie Buckley, Meg Warriner, Laurence O’Toole, Abdallah Al-Mohammad

A new heart failure service was established in Sheffield in 2008. The service provides specialist advice on the management of inpatients with heart failure, and optimises their medical therapy in a heart failure clinic led by heart failure nurse specialists. We undertook a survey of patients’ perception of the service provided by these clinics.
A postal survey was sent to the patients who attended the nurse-led heart failure clinics more than once in the first two years of the service. There were two types of questions: multiple-choice questions and those allowing free text answers. We approached 228 patients. We received responses from 192 (84%). Of these patients, the majority (80–90%) responded positively to most of the questions. The vast majority of patients regarded the service as providing excellent care, that the staff were courteous and professional, and they were able to establish a good relationship. The negative remarks were related to facilities such as parking spaces in the hospital, and to the label of heart failure. The team endeavours to make improvements to the service.
In conclusion, the nurse-led heart failure clinic was positively received by heart failure patients.
November 2012 Br J Cardiol 2012;19:184 doi:10.5837/bjc.2012.034
Massive inferior venacavo-atrial thrombus following neoadjuvant chemotherapy
Pankaj Kaul, Robert George, Rodolfo Paniagua, Subbarayulu Balaji, Mohan Sivananthan, Rob Sapsford

A 26-year-old man presented with T4 adenocarcinoma of sigmoid colon, which was initially treated with a covering ileostomy and neoadjuvant chemotherapy with oxaliplatin and infusional 5-fluorouracil delivered through a right subclavian Hickman line. While receiving chemotherapy, he developed a massive right atrial thrombus, adherent to the inferior venacaval opening and the adjoining right atrial wall, mimicking a metastatic deposit, which was removed surgically on cardiopulmonary bypass. The patient subsequently underwent successful high anterior resection of the sigmoid cancer followed by adjuvant chemotherapy with oxaliplatin and capecitabine. The unusual features of this patient’s presentation include the extremely rapid growth of thrombus despite aggressive anticoagulation, the unusual site of thrombus on the inferior vena caval opening rather than around the Hickman line, and possible facilitation of thrombus formation by chemotherapeutic agents. We also discuss the diagnostic and therapeutic dilemmas in a patient with a concurrent malignancy and a right atrial mass.
August 2012 Br J Cardiol 2012;19:122–3 doi:10.5837/bjc.2012.020
Translating regulatory advice into practice: use of dronedarone and older anti-arrhythmics in AF management
A consensus position statement. A John Camm, Chris Arden, Anna-Maria Choy, Riyaz A Kaba, David Keane, Khalid Khan, Ernest Lau, Gregory Y H Lip, Francis Murgatroyd, G Andre Ng, Nicholas Peters, Henry Purcell, Peter Stafford, Neil Sulke, Helen Williams

There is a lack of clarity around the current use of anti-arrhythmic drugs (AADs), highlighted by the recent changes to the European Medicines Agency (EMA) and US Food and Drug Administration (FDA) recommendations for dronedarone use, which were in response to the early termination of the Permanent Atrial Fibrillation Outcome Study Using Dronedarone On Top Of Standard Therapy (PALLAS) trial due to increased mortality in the dronedarone arm. A UK- and Ireland-based multi-disciplinary expert group was convened by Sanofi*, the manufacturers of dronedarone, to address the need for guidance in the practical implementation of guidelines for AADs. This position statement provides the group’s evidence-based recommendations for the practical use of AADs and dronedarone in particular. Since AADs are not always used in line with recommendations, the guidelines for the use of AADs, and the evidence base supporting them, are reviewed. The current recommendations for dronedarone use are set within this context. On consideration of the evidence, the recommendation for dronedarone use is for the maintenance of sinus rhythm in non-permanent atrial fibrillation (AF) patients, without severe heart failure, or amiodarone-related liver or lung toxicities, and with appropriate anticoagulation. Given that there have been no new AADs available in 25 years to address the need for an effective anti-arrhythmic with reduced side effects, dronedarone has a place in the treatment of non-permanent AF to provide options for clinicians and patients.
* Further detail of Sanofi's support is declared in the conflict of interest statement at the end of this article.
August 2012 Br J Cardiol 2012;19:124–5 doi:10.5837/bjc.2012.023
Left pleuropericardial agenesis and coronary artery disease
Pankaj Kaul

We present a 37-year-old man who underwent coronary artery bypass grafting for severe left main stem stenosis and right coronary artery disease and was found to have left pleuropericardial agenesis with luxation of heart to the left in the left common pleuropericardial cavity. Although complete absence of pericardium is found in one out of 14,000 patients, agenesis of left pericardium as well as left pleura is extremely rare. Despite a number of related and unrelated pathologies having been described with this condition, there are only two or three reports of co-existence of coronary artery disease. We describe the technicalities of coronary artery surgery in this condition and also review the literature for clinical diagnosis, associated conditions and complications.

August 2012 Br J Cardiol 2012;19:126–33 doi:10.5837/bjc.2012.024
Cholesteryl ester transfer protein (CETP) inhibitors
Paul N Durrington

Despite statin use to lower low-density lipoprotein cholesterol, a residual cardiovascular risk remains in dyslipidaemic patients, particularly when high-density lipoprotein (HDL) levels are low. Increased cholesteryl ester transfer protein (CETP) activity is a major determinant of low HDL-cholesterol. CETP inhibition with anacetrapib, evacetrapib and dalcetrapib produces plasma HDL increases of approximately 140%, 80% and 30%, respectively, in patients already receiving statin therapy. However, recent research challenges whether raising HDL-cholesterol is in itself beneficial unless anti-atherogenic properties of HDL, such as cholesterol removal from arterial walls, stimulation of endothelial nitric oxide production or protection against oxidation and inflammation, are enhanced. Potentially important differences are emerging in the mechanisms by which CETP inhibitors operate, which may lead to variation in their anti-atherogenicity unrelated to the changes in HDL-cholesterol they induce. The outcome of clinical trials with CETP inhibitors may thus depend on the mechanisms by which they inhibit CETP. This review discusses clinical implications of CETP inhibition.
August 2012 Br J Cardiol 2012;19:134–8 doi:10.5837/bjc.2012.025
Early and late survival after surgical revascularisation for left main coronary artery stenosis in stent era
Dumbor L Ngaage, Franco Sogliani, Augustine Tang

We report the early and late results of coronary artery bypass graft (CABG) for protected and unprotected left main coronary artery (LMS) stenosis in an era of growing interest in LMS stenting.
We identified 1,707 patients who had CABG for LMS stenosis between February 1996 and December 2009, and compared their clinical characteristics and outcomes with a contemporaneous group of 6,260 people with non-LMS disease. A subgroup analysis of protected versus unprotected LMS cohorts was also performed. Follow-up data were 99.9% complete.
The LMS group, often male (82% vs. 79%, p=0.01) and older (mean 65.3 ± 9 vs. 63.6 ± 9 years, p<0.0001), frequently had ejection fraction <0.50 (25.2% vs. 23.9%, p=0.002) and urgent/emergency surgery (40% vs. 24%, p<0.0001). Overall, operative mortality was higher for the LMS group (2.7% vs. 1.1%, p<0.0001), and there was improvement over time (2.3% vs. 0.8% in the later period). There was no difference between protected and unprotected LMS cohorts (operative mortality 2.2 vs. 2.8, p=0.54).
The respective 10-year survival rates for LMS and non-LMS patients were 75% and 79% (p=0.001). By multi-variate analysis, LMS stenosis was a predictor of operative mortality (odds ratio 2.05, 95% confidence interval 1.29–3.25, p=0.002) but not a determinant for late death.
In conclusion, CABG yields good early and late survival benefit for LMS stenosis (protected and unprotected), although operative result is adversely affected by LMS disease.
August 2012 Br J Cardiol 2012;19:139–40 doi:10.5837/bjc.2012.026
Does CT coronary angiography have a role in the evaluation of patients with CABG?
Mohamed Albarjas, Khaled Alfakih, Jonathan Hill

Multi-detector computed tomography coronary angiography (CTCA) is now an established highly effective non-invasive test in patients with chest pain and a low-to-intermediate pre-test likelihood of having coronary artery disease (CAD), as it has excellent sensitivity and negative predictive value (NPV).1 The limiting factors for CTCA are fast or irregular heart rate, a very high body mass index (BMI), the presence of extensive calcium in the coronary arteries and radiation. Recent introduction of prospectively gated acquisition in CTCA, where the acquisition is limited to 10% of the cardiac cycle at end-diastole, has dramatically reduced the radiation dose to 2–3 mSv for CTCA of the native coronary arteries, but this is only possible in patients with a regular rhythm below 60 bpm. Otherwise, retrospectively gated CTCA with electrocardiographically controlled tube current modulation (ECTCM) during the cardiac cycle keeps the dose below 10 mSv. The CTCA scan range in patients with coronary artery bypass grafts (CABG) is from the level of the subclavian arteries to below the diaphragm, which is twice the length of a CTCA for the native coronary arteries, and, hence, doubles the radiation dose. However, while the low-dose prospectively gated CTCA technique may not be possible in all patients having CTCA of the native coronary arteries, the minimal motion of the grafts means that CABG patients can be adequately imaged even with higher or irregular heart rates or higher BMI with the low-dose technique. The American College of Cardiology (ACC) has recently published appropriateness criteria for the use of CTCA, which included the use in patients with recurrent symptoms after CABG.2

August 2012 Br J Cardiol 2012;19:141–3 doi:10.5837/bjc.2012.027
Lessons learnt from a tragic loss – but will things improve?
Stephen Westaby, Ravi De Silva, Shane George, Duncan Young, Yaver Bashir

The very public resuscitation of a premier league footballer drew nationwide attention to fatal dysrrhythmias in the young. Survival was achieved by effective bystander cardiopulmonary resuscitation (CPR), rapid transportation and targeted resuscitation in a cardiac centre. In Emergency Departments in the UK, resuscitation from shockable dysrrhythmias follows the Advanced Life Support (ALS) protocol, using biphasic defibrillation (150–200 J) with subsequent adrenaline boluses and amiodarone. In patients with hypertrophic cardiomyopathy or primary ventricular arrhythmias without structural heart disease, high energy defibrillation (up to 360 J) is sometimes required and catecholamines predispose to recurrent dysrrhythmia.1 On occasion, more can be learnt from failure than success. For this reason we present the following case.

May 2012 Br J Cardiol 2012;19:65–9 doi:10.5837/bjc.2012.013
What do angina patients understand of options for myocardial revascularisation?
Vedat Barut, Kevin Fox, Alison Mead

Patient knowledge and understanding of their condition is important in every field of medicine. It is particularly relevant in cardiology where choices between treatment options must be made and where patient participation in prevention of disease progression is a key part of therapy. In this study, knowledge and understanding of angina patients on options for revascularisation was explored. The aim was to reveal trends that may identify opportunities to improve care. This was a qualitative study utilising depth semi-structured interviews of angina patients who have had revascularisation (excluding primary percutaneous coronary intervention [PCI] for ST elevation myocardial infarction). The main outcome measure was patient perception on revascularisation options. It was conducted in an out-patient setting at the cardiac prevention and rehabilitation centre at Charing Cross Hospital, West London. Angina patients are referred to the centre before and after their revascularisation for rehabilitation and education sessions. Several themes emerged from this study. First, patients are not fully aware of angina pathophysiology. Second, awareness of options for angina treatment is limited and their understanding heavily relies on the recommended option of the doctor. Other options are only briefly mentioned by healthcare professionals, and patients tend to turn to other sources, such as the internet and family/friends, for information. Despite the lack of understanding, all patients were happy with the way their treatment was chosen and were not too concerned about the level of information they had received. In conclusion, patients have limited understanding of angina and options for treatment but are generally satisfied with their care. However, it is likely that impaired patient understanding will impact on their ability to maintain secondary prevention, especially lifestyle changes and medication concordance.

May 2012 Br J Cardiol 2012;19:71–5 doi:10.5837/bjc.2012.014
Planning for end-of-life care in heart failure: experience of two integrated cardiology-palliative care teams
Miriam Johnson, Anne Nunn, Tracey Hawkes, Sharon Stockdale, Andrew Daley

We previously reported retrospective data on the place of death for people with heart failure (HF) known to heart failure nurse specialists (HFNS) working in two integrated cardiology palliative care teams. Here, we present prospective data on place of death, the supportive services accessed, and the role of HFNS. We collected prospective data on all patients known to the HFNS, who died during one year (n=126): length of HFNS involvement; planning for end-of-life care; preferred and actual place of death; services accessed. Outcomes were compared for the two teams. The Surprise Question was applicable in 70% of patients; 89% of whom died within 12 months. Overall, 33% died in hospital. Planning for end-of-life care was evident for 64% and half were referred for specialist palliative care; mostly initiated by HFNS. Preferred place of death was achieved for 61%. Home death was more common where there was greater access to hospice-at-home and Marie Curie nurses. Hospital death was least likely in the team with an out-of-hours palliative care telephone service. In conclusion, recognition and planning for the end of life is possible for many with HF. HFNS were central in discussing patients’ concerns, providing and coordinating end-of-life care.

May 2012 Br J Cardiol 2012;19:76–8 doi:10.5837/bjc.2012.015
Routine follow-up for patients with prosthetic valves: the value of a nurse-led valve clinic
Denise Parkin, John B Chambers

To see whether a nurse-led clinic might be useful we audited how often patients discharged from follow-up were elsewhere seen in the community and how often events were picked up in patients being seen in a nurse-led valve clinic. We audited patients implanted with an OnX bileaflet mechanical heart valve between 1999 and 2010 by postal audit asking for details of follow-up and adverse events. We also analysed the outcome and adverse events from our nurse-led clinic over 30 months between 2009 and 2011 using our valve clinic audit database. There were 188 OnX patients of whom only 125 (66%) were receiving regular cardiology follow-up. Of those in regular follow-up, there were 16 (13%) valve-related adverse events, and this was similar to those not receiving follow-up, 9 (14%). Only 126 (67%) had regular dental surveillance. In the valve clinic, there were 199 visits by 132 patients. Echocardiograms were required on eight visits (4%). There were three hard events (as defined by International Guidelines), 19 visits (10%) revealed adverse events requiring a cardiologist and six (3%) revealed events not requiring a cardiologist. In conclusion, a nurse-led clinic provides effective long-term monitoring of valve patients. Large proportions of patients are discharged from cardiology/surgical units and are at risk of adverse valve-related events
May 2012 Br J Cardiol 2012;19:79–84 doi:10.5837/bjc.2012.016
Omega-3 fatty acids in cardiovascular disease: re-assessing the evidence
Alan Begg, Susan Connolly, Julian Halcox, Agnes Kaba, Linda Main, Kausik Ray, Henry Purcell, Helen Williams, Derek Yellon

With conflicting findings from studies of omega-3 fatty acids in cardiovascular disease, many healthcare professionals are uncertain of whether they show any benefit. BJC seminars are held to promote evidencebased practice and we recently convened a meeting of UK professionals working in cardiovascular disease to review the evidence for omega-3 fatty acids supplementation, as well as review some of the data relating to dietary fish oils. The panel considered how supplementation with omega-3 fatty acids might be used in the future. The meeting was sponsored with an unrestricted educational grant from Abbott Laboratories.

May 2012 Br J Cardiol 2012;19:85–9 doi:10.5837/bjc.2012.017
Drugs for diabetes: part 9 prescribing for patients with cardiac disease
Anna White, Gerard A McKay, Miles Fisher

Up to one-third of patients with heart disease have diabetes. Cardiological status should be considered when deciding on treatment for diabetes. Patients with stable coronary disease can be treated with metformin, sulphonylureas or pioglitazone. Following an acute coronary syndrome, intensive insulin therapy with multi-dose insulin has been shown to reduce mortality, and longerterm treatment with pioglitazone may reduce recurrent events. There is little trial information for glycaemia control in patients with chronic heart failure, and metformin and insulin are both frequently used. Dipeptidylpeptidase-4 (DPP-4) inhibitors are new oral antidiabetic drugs, which are weight neutral, and the injected glucagon-like peptide-1 (GLP-1) receptor agonists reduce weight. Long-term outcome studies are awaited to see if they have cardiovascular advantages in any particular group of patients.
May 2012 Br J Cardiol 2012;19:90–4 doi:10.5837/bjc.2012.018
Pacemaker complications in a district general hospital
Richard Bond, Daniel Augustine, Mark Dayer

Pacemakers are being implanted with increasing frequency. As with every procedure, there is the potential for complications. There are little recent data on implant complications and consequently we may be misinforming patients when we consent them. Data from all pacing procedures performed from February 2007 to January 2010 were analysed retrospectively. All chest X-rays and their reports were inspected for pneumothoraces and lead displacements. Correspondence to our local pacemaker extraction centre was used to identify patients with pacemaker infections requiring extraction. Discharge summaries were also used to identify patients with other complications that were not discovered by the above methods. A total of 1,286 procedures took place over the three-year period. There were a total of 94 (7.5%) complications. Lead displacement was the most common complication occurring in 39 (4.8%) procedures requiring leads. Pneumothorax occurred in 30 (3.7%) patients. Infection occurred in 19 (1.5%) patients. Perforation occurred in three (0.37%) patients. These are unselected data from a high volume district general hospital (DGH). Infection rates are low. Lead displacement rates are higher than other similar studies. Pneumothorax rates are also high, reflecting the fact that almost all access is via the subclavian vein.

May 2012 Br J Cardiol 2012;19:95–6 doi:10.5837/bjc.2012.019
Post-myocardial infarction (Dressler’s) syndrome following early reperfusion
Ali Boushahri, Richard J Katz

We present a case of a 55-year-old female with a successfully reperfused myocardial infarction in whom Dressler’s syndrome was subsequently diagnosed. There have been no reported cases in the literature of Dressler’s syndrome following documented early coronary reperfusion, and its continued existence in the era of reperfusion has been questioned. In conclusion, this case demonstrates that this syndrome is still a possibility in the current realm of thrombolysis and cardiac catheterisation.

March 2012 Br J Cardiol 2012;19:21–3 doi:10.5837/bjc.2012.001
Optimised beta blocker therapy in heart failure: is there space for additional heart rate control?
Stuart James Russell, Maria Oliver, Linda Edmunds, Joanne Davies, Hayley Rose, Helen Llewellyn-Griffiths, Victor Sim, Adrian Raybould, Richard Anderson, Zaheer Raza Yousef

The importance of heart rate reduction in chronic stable heart failure (HF) has been highlighted in the recently published Systolic Heart Failure Treatment with If Inhibitor Ivabradine Trial (SHIFT). Patients with an elevated resting heart rate (HR) benefited from additional HR control despite optimal doses of beta blockers. The aim of this study was to define the prescribing patterns of beta blockers and the scope for additional HR control in a ‘real life’ HF population.
We conducted a retrospective analysis of two HF clinics, where patients were referred for protocol-guided, up-titration of HF medications. At each assessment we documented: HR, blood pressure, and HF medications including potential side effects. The primary objective was to identify the proportion of patients who had suboptimal HR control (HR ≥70 bpm) despite optimal conventional HF therapy.
From 172 patient records, 145 (84.3%)could tolerate long-term beta blockade with 57 (33.1%) prescribed the maximum recommended dose. Overall, 101 patients were in sinus rhythm with 31/101 (30.7% having an ejection fraction ≤35% and a resting HR ≥70 bpm.
In conclusion, suboptimal HR control is evident in approximately one in three HF patients in sinus rhythm despite aggressive optimisation of beta blocker therapy. This cohort may benefit from additional HR control.

March 2012 Br J Cardiol 2012;19:24 doi:10.5837/bjc.2012.003
Current prescribing of statins and persistence to statins following ACS in the UK: a MINAP/GPRD study
Rachael Boggon, Susan Eaton, Adam Timmis, Harry Hemingway, Zahava Gabriel, Iqbal Minhas, Tjeerd P van Staa

National Institute for Health and Clinical Excellence (NICE) guideline CG67 recommends that acute coronary syndrome (ACS) cases are treated with high-intensity statins (defined as statins used in doses that produce greater cholesterol lowering than simvastatin 40 mg). The objective of this study was to describe current UK prescribing of statins following ACS. This study used data from linkage between the Myocardial Ischaemia National Audit Project (MINAP) database and the General Practice Research Database (GPRD). The study included adults aged 40+ with a discharge diagnosis in MINAP of myocardial infarction, troponin positive or negative ACS discharged alive to home. A total of 6,138 ACS cases were included. Most ACS cases were prescribed both a statin at hospital discharge and by their GP, however, 340 of the 6,138 ACS cases (5.5%) had no record of statin prescription from either source. Of the ACS cases prescribed a statin by their GP, 30.1% received a high-intensity statin dose. At year four, 43% (95% confidence interval [CI] 41–45%) of ACS cases prescribed a statin remained on treatment (42% for those starting low and 45% for high intensity). In conclusion, statin therapy is provided to most ACS cases in the UK but duration and dosage is shorter and lower than recommended.
March 2012 Br J Cardiol 2012;19:25 doi:10.5837/bjc.2012.004
Hearing the voice of the heart failure patient: key experiences identified in qualitative interviews
Chad J Gwaltney, Ashley F Slagle, Mona Martin, Rinat Ariely, Yvonne Brede

Although morbidity and mortality are the most commonly used end points in clinical trials of heart failure treatments, it is also important to consider how patients experience their illness when assessing treatment efficacy. The goal of this study was to use qualitative interviews to identify key experiences that may be targeted as end points in future heart failure trials.
Interviews were conducted with 63 chronic heart failure patients. Interview responses were coded using ATLAS.ti software. Code frequency and bother ratings were used to identify salient patient experiences. Key symptoms included shortness of breath, tiredness, swelling of the lower extremities, and pain (chest and other). Shortness of breath and tiredness were often described as being related to physical activities. Key areas impacted by heart failure included physical activity and mobility limitations, and a variety of emotional effects.
In conclusion, patients report a number of symptoms and impacts related to heart failure. Although some experiences are already widely captured in clinical and patient-reported heart failure assessments, others, such as pain, are not. These findings support the use of patient-reported outcome instruments as end points when assessing the efficacy of heart failure treatments.

March 2012 Br J Cardiol 2012;19:26–9 doi:10.5837/bjc.2012.005
Drugs for diabetes: part 8 SGLT2 inhibitors
Alison MacEwen, Gerard A McKay, Miles Fisher

SGLT2 inhibitors are a new class of oral drugs for the treatment of type 2 diabetes mellitus currently in phase III studies. They inhibit glucose re-absorption in the proximal renal tubules providing an insulin independent mechanism to lower blood glucose. Their use in clinical practice is associated with improved glycaemic control, weight loss and a low risk of hypoglycaemia. Phase III cardiovascular safety studies are ongoing.

March 2012 Br J Cardiol 2012; 19 :30–3 doi:10.5837/bjc.2012.006
Low pulse pressure does not reduce the efficacy of a heart failure exercise programme
Rosalind Leslie, John P Buckley

Patients with chronic heart failure (CHF) may have low pulse pressures (PP). This retrospective study was undertaken to analyse the relationship between PP and outcomes of a 12-week exercise training programme. Data analysed from 86 patients (69 male) aged 40 to 86 years, included: PP, functional capacity (metabolic equivalents [METS]) and quality of life (QoL) using the Minnesota Living with Heart Failure Questionnaire (MLHFQ).
Median pre-training PP was 54 ± 19 mmHg. Functional capacity for the same heart rate (estimated 60% heart rate reserve) and Borg rating of 13 increased from 3.6 ± 1.1 to 4.0 ± 1.2 METS (p=0.0005); MLHFQ scores improved from 26 ± 19 to 22 ± 20 (p=0.0005). There was a high correlation between PP and systolic blood pressure pre- and post-training (pre: r=0.77, p=0.0005; post: r=0.80, p=0.0005). Changes in all the above outcomes were independent of pre-training PP.
In conclusion, low PP did not reduce the efficacy of an exercise training programme, indicating that CHF patients with low PP can benefit similarly to those with normal/raised PP.
March 2012 Br J Cardiol 2012;19:34–7 doi:10.5837/bjc.2012.007
Midodrine: use and current status in the treatment of hypotension
Jacqueline F Doyle, Richard Grocott-Mason, Timothy C Hardman, Omar Malik, Simon W Dubrey

Midodrine is a sympathomimetic agent used in the treatment of hypotension resulting from various aetiologies. Debate around the use of midodrine recently increased after it was threatened with a licence withdrawal in the USA. The reason cited was a failure of the manufacturing drug companies to provide previously agreed post-market studies. Conversely, midodrine has never received a licence from the UK regulatory authorities.
We provide a review of its current status and a brief description of our own experience with midodrine over the last 11 years.
March 2012 Br J Cardiol 2012;19:38–40 doi:10.5837/bjc.2012.008
The gap between training and provision: a primary-care based ECG survey in North-East England
Andreas R Wolff, Sue Long, Janet M McComb, David Richley, Peter Mercer

Electrocardiogram (ECG) is the most common cardiac investigation provided in primary care and accepted as core medical practice, yet little research evidence exists. In order to gather information on ECG provision in primary care and provide a training and competence analysis, a postal survey of 395 general practices within the North of England Cardiovascular Network area was conducted.
A total of 119 practices responded (30.1%) of which 91 (76.5%) recorded ECGs in-house. An average of 34.7 ECGs per 1,000 patients were recorded within 12 months (1.4–114/1,000). Of practices recording ECGs, 86% also interpreted the results themselves. Of staff recording ECGs, 72% received training, which was carried out mostly in-house, and 52.9% of practitioners interpreting results had received some training. A low level of confidence to recognise 10 important ECG abnormalities was reported.
Our survey confirmed that the majority of GP practices record and interpret ECGs. Few received formalised training and assessment in recording and interpreting ECGs. This was reflected in a low level of confidence to recognise critical ECG abnormalities.
March 2012 Br J Cardiol 2012;19:41–5 doi:10.5837/bjc.2012.009
Fabry disease
Cristina Golfomitsos, Anshuman Sengupta, Usha Prasad, David Gray

Anderson-Fabry disease is a rare X-linked recessive lysosomal storage disease that may cause a wide range of symptoms affecting multiple systems. It is due to a DNA mutation in the enzyme alpha-galactosidase A; this causes an accumulation of a glycolipid, globotriaosylceramide, within blood vessels, tissues, and organs, impairing their function.
Typically, males experience severe symptoms, but the impact on women is variable, with some being asymptomatic and others having severe symptoms. Although the diagnosis can often be readily made in males by measuring the blood level of alpha-galactosidase activity, in females, gene sequencing is preferred as enzyme activity may be within the normal range. However, the disease may not be suspected as many symptoms are shared with other disease processes. Important clues are multi-system symptoms that vary in age of onset, severity and manner of progression; early onset of kidney failure; and stroke or heart disease in the absence of conventional vascular risk factors. Enzyme replacement therapy is available.
March 2012 Br J Cardiol 2012;19:46–7 doi:10.5837/bjc.2012.010
Aortic root fistula complicating infective endocarditis: role of 64-multi-detector CT cardiac angiography
Andrew J Howe, John A Purvis

A 47-year-old man with known bicuspid aortic valve was admitted with a six-week history of night sweats and malaise. Clinically, aortic systolic and diastolic murmurs were present. Temperature was 38ºC, white cell count was elevated at 13.8 x 109/L, erythrocyte sedimentation rate (ESR) was 44 mm/hr, and three consecutive blood cultures grew Streptococcus parasanguinis. Transthoracic (TTE), then transoesophageal (TOE) echocardiography was performed.
March 2012 Br J Cardiol 2012;19:48–9 doi:10.5837/bjc.2012.011
Ortner’s syndrome: an unusual cause of cough
Claire J Grout, Katherine A Simpson, Michael R Clements

A 57-year-old woman presented with a six-week history of non-productive cough associated with sharp chest pain. Her past medical history included a metallic aortic valve replacement for aortic regurgitation, hypertension and hypercholesterolaemia. The patient had a blood pressure of 97/60 mmHg and was afebrile. On examination, the metallic valve was audible with no added heart sounds. Examination of other systems was normal. Electrocardiogram (ECG) showed a normal sinus rhythm with no ischaemic changes. Admission blood tests showed an elevated white cell count (11.4 x 109 per litre) and a C-reactive protein of 225.8 mg/L. Her chest radiograph demonstrated a widened mediastinum, evidence of previous cardiac surgery and a metallic valve (figure 1). Transthoracic echocardiography showed a dilated aortic root measuring 62 mm at the level of the sinotubular junction. In addition, a thrombus was visualised in the ascending aorta with a dissection flap, which was confirmed by computed tomography (CT) scan (figure 2). The patient was transferred to a cardiothoracic unit to undergo surgical repair of the dissection and replacement of the metallic valve. The dissection was shown to arise from the suture line of the previous valve replacement.
October 2011 Br J Cardiol 2011;18:219–22 doi:10.5837/bjc.2011.002
Patent foramen ovale: diagnosis, indications for closure and complications
Sudhakar George, David Hildick-Smith

The purpose of this review is to give a broad overview of the role of patent foramen ovale (PFO) in disease. The embryological origins of PFO are described before reviewing the different diagnostic modalities available, including transthoracic echocardiography, trans-oesophageal echocardiography and transcranial ultrasound scanning. The role, or proposed role, of PFO in conditions including cryptogenic stroke, decompression sickness and migraine are discussed, as well as different treatment options, including the evidence for closure of PFO. Some of the range of methods and devices used to close PFO are described, as are the possible complications when attempting closure.
October 2011 Br J Cardiol 2011;18:224-228 doi:10.5837/bjc.2011.003
Drugs for diabetes: part 7 insulin
Nicholas D Barwell, Gerard A McKay, Miles Fisher

Insulin remains an important treatment for patients with type 1 and type 2 diabetes. Insulin is given to patients with type 1 diabetes as a form of hormone replacement therapy to replace the loss of endogenous insulin secretion. Intensive insulin treatment with either continuous subcutaneous insulin infusion or basal–bolus therapy reduces diabetic complications, including macrovascular complications. For patients with type 2 diabetes, insulin therapy is given to try and overcome the combination of insulin resistance and beta-cell dysfunction that are the pathological hallmarks of the disease. There are concerns that weight gain and hypoglycaemia, which are common side-effects of intensive insulin therapy, may reduce or negate direct benefits of controlling hyperglycaemia on macrovascular outcomes. The best insulin regimen for patients with type 2 diabetes is not clear, and treatment should aim to minimise weight gain and the occurrence of hypoglycaemia.
October 2011 Br J Cardiol 2011;18:231–2 doi:10.5837/bjc.2011.004
Multi-disciplinary valve clinics with devolved surveillance: a two-year audit
John B Chambers, Guy Lloyd, Helen M Rimington, Denise Parkin, Anna M Hayes, Gemma Baldrock-Apps, Ann Topham

Sonographer- and nurse-led clinics were developed at a cardiothoracic centre and a sonographer-led clinic at a district general hospital (DGH). Common database fields were adopted in 2007 and this is an audit over the subsequent two years. Data were analysed for the two-year period from 1 September 2007 to 31 August 2009. A total of 683 visits by 388 patients occurred at the cardiothoracic centre and 1,306 visits by 726 patients at the DGH. There were no unexpected adverse events. Cross-referral to a cardiologist occurred in 13% of visits at the cardiac centre and 11.5% at the DGH. The mortality rates were 2% and 3%, the discharge rates 6% and 2%, and the surgical rates 16% and 4% at the cardiac centre and the DGH, respectively. No unexpected events occurred. Our observations suggest that devolved surveillance clinics are feasible, safe and generalisable as part of a specialist valve service.
October 2011 Br J Cardiol 2011;18:233-237 doi:10.5837/bjc.2011.005
Alcohol septal ablation in hypertrophic obstructive cardiomyopathy
Tahir Hamid, Matthew Luckie, Rajdeep S Khattar

Alcohol septal ablation (ASA) is an alternative therapeutic method to the gold-standard surgical myectomy in the treatment of symptomatic left ventricular outflow tract (LVOT) obstruction in patients with hypertrophic cardiomyopathy (HCM). ASA is performed by injecting alcohol into the target septal branch of the left anterior descending coronary artery. In this article, we review the rationale and indications for ASA, provide a practical description of the technique and give an overview of the published data placing it in context with the surgical approach. We also report our experience of the technique in a typical sample of patients referred to a tertiary centre providing demographic, echocardiographic and clinical outcomes data during an average follow-up period of three years. Our data confirm that ASA is an effective non-surgical technique for treatment of symptoms related to LVOT obstruction in HCM. Medium-term follow-up demonstrates persistent reduction in LVOT obstruction and improvement in New York Heart Association (NYHA) functional class. Long-term studies of larger populations are necessary to determine the wider prognostic significance of the procedure.

October 2011 Br J Cardiol 2011;18:238-240 doi:10.5837/bjc.2011.006
Aspirin taking in a south Wales county
Peter Elwood, Gareth Morgan, James White, Frank Dunstan, Janet Pickering, Clive Mitchell, David Fone

In order to determine the taking of regular aspirin within a representative community sample of adults residing in the south Wales county of Caerphilly, we conducted a survey of a sample 9,551 adults resident in the county aged ≥18 years. Questionnaires were returned by 4,558 individuals aged between 25 and 82 years. Nearly 12% of the respondents reported a previous vascular event. Of these, 68% of the men and 55% of the women stated that they took aspirin regularly. Among those with no previous vascular event, 22% of the men and 13% of the women stated that they took aspirin regularly. For those over 50 years of age, the respective figures were 28% of men and 19% of women. Of those taking aspirin, 47% stated that they took 300 mg tablets. There was a small inverse relationship found between aspirin taking and social class, namely 67% and 56% in the manual and non-manual classes respectively. The prevalence of prophylactic aspirin taking by persons who have had a vascular event should be increased, particularly in women. Knowledge of the benefits and the risks of aspirin prophylaxis could be promoted through the community and there should be ongoing monitoring of aspirin taking.
October 2011 Br J Cardiol 2011;18:246-248 doi:10.5837/bjc.2011.009
Recurrent stent thrombosis with dual antiplatelet resistance: the role of platelet function testing
Sunil Nadar, Farhan Gohar, James Cotton

Platelet activation is an important part of the pathophysiology of acute coronary syndromes. Inhibition of this by antiplatelet agents forms an important part of the management of this condition. Recently, there has been considerable interest in the variability of platelet response to these drugs and the need to tailor the dose of antiplatelet agents according to the response. Here, we present a patient who had repeated episodes of stent thrombosis and was found to have decreased response to clopidogrel and aspirin (clopidogrel and aspirin resistance) with the use of the Accumetrics VerifyNowTM analyser. We have also reviewed the literature on this subject. Our recommendation is that patients who have recurrent stent thrombosis or thrombotic events on dual antiplatelet agents should have their antiplatelet therapy response checked and have their antiplatelet agents tailored accordingly.
October 2011 Br J Cardiol 2011;18:241-242 doi:10.5837/bjc.2011.007
Mitral valve leaflet and free-floating left atrial thrombi with ‘rhupus’ and antiphospholipid syndrome
Panduranga Prashanth, Mohammed Mukhaini

A 27-year-old Arab woman with history of seronegative rheumatoid arthritis for four years presented with a three-day history of multiple joint pains and swelling, along with fever. Clinically, she had bilateral rheumatoid hand deformities with signs of active arthritis of elbows, hands and knee joints. She was in sinus rhythm with normal cardiac examination. She was treated with steroids and was responding well except for mild fever, for which an echocardiogram was requested to rule out infective endocarditis.
October 2011 Br J Cardiol 2011;18:243-245 doi:10.5837/bjc.2011.008
Cabergoline as an adjunct for early left ventricular recovery in peripartum cardiomyopathy
Masliza Mahmod, Cheuk F Chan, Aamir Ali, Sadaf Raza, Nik R Wan-Ibrahim, Georgios Manolis, Rahana Abd Rahman, Ankur Gulati

Outcome in patients with peripartum cardiomyopathy (PPCM) is variable. Recovery of left ventricular function is observed in between 23% and 51% of cases at six months after diagnosis. Despite standard medical therapy, both morbidity and mortality remain high. Recent evidence has suggested that dopamine-receptor agonists may be beneficial in the treatment of this condition. We describe a case of a patient with PPCM who developed rapid normalisation of left ventricular function following addition of carbergoline, a long-acting dopamine-receptor agonist, to her conventional heart failure therapy.

August 2011 Br J Cardiol 2011;18:167–69
Drugs for diabetes: part 6 GLP-1 receptor agonists
Claire McDougall, Gerard A McKay, Miles Fisher

The glucagon-like peptide-1 (GLP-1) receptor agonists are a new class of injected drugs for the treatment of type 2 diabetes. They mimic the action of GLP-1 and increase the incretin effect in patients with type 2 diabetes, stimulating the release of insulin. They have additional effects in reducing glucagon, slowing gastric emptying, and inducing satiety. In clinical practice they are associated with significant reductions in glycosylated haemoglobin (HbA1c), weight loss and a low risk of hypoglycaemia. Beneficial effects have also been observed on blood pressure and lipids. The possibility of cardiovascular benefit is now being formally examined in large randomised-controlled trials with primary cardiovascular end points.
August 2011 Br J Cardiol 2011;18:171–76
MyAction: an innovative approach to the prevention of cardiovascular disease in the community
Susan Connolly, Annie Holden, Elizabeth Turner, Gillian Fiumicelli, Juliet Stevenson, Mandeep Hunjan, Alison Mead, Kornelia Kotseva, Catriona Jennings, Jennifer Jones, David A Wood

We developed and piloted an innovative family-centred preventive cardiology programme (MyAction) that aimed to both integrate the care of patients with vascular disease with that of individuals identified at high multi-factorial risk and help them achieve recommended lifestyle, medical risk factors and therapeutic targets. The 16-week nurse-led programme was delivered by a multi-disciplinary team, including a dietitian, physical activity specialist and cardiologist, in a community setting. Of 206 patients who attended the initial assessment, 54% attended with their partner and 142 patients completed the programme (69%). By the end of the programme, there was a significant improvement seen in adherence to a Mediterranean diet, as well as substantial increases in physical activity levels supported by objective evidence of improved functional capacity. These changes contributed to significant reductions in body mass index (BMI), weight and abdominal obesity. Very similar changes were seen in partners. Blood pressure control also improved significantly, as did achievement of the low-density lipoprotein (LDL)-cholesterol target, and there was a significant increase in the use of cardioprotective medication. Quality of life also improved in both patients and partners. The significant changes achieved by the MyAction preventive cardiology programme should substantially reduce the cardiovascular risk of these patients and their partners in the future.
August 2011 Br J Cardiol 2011;18:178
Lifestyle advice and drug therapy post-myocardial infarction: a survey of UK current practice
Julian Halcox, Steven Lindsay, Alan Begg, Kathryn Griffith, Alison Mead, Beverly Barr

Reducing morbidity and mortality among post-myocardial infarction (MI) patients requires the implementation of effective secondary measures. This survey examined current practice by assessing the view on, and adherence to, National Institute for Health and Clinical Excellence (NICE) guidance on MI secondary prevention in a sample of general practitioners (GPs) and cardiologists. There were 303 respondents from Scotland and England, including at least 10 GPs and one cardiologist from each English Strategic Health Authority. Although drug treatment post-MI generally complied with NICE recommendations, diet and lifestyle aspects were not implemented fully. There appeared to be sub-optimal integration between primary and secondary healthcare providers. Both GPs and cardiologists underestimated the importance of tailoring secondary prevention services to the individual and the role of omega-3 fatty acid treatments (where required) to supplement dietary intake. There is a clear need to improve compliance of healthcare professionals with many of the key priorities for implementation outlined in the NICE guidelines. In addition, patient-centred cardiac rehabilitation services should be standardised and include strategies to improve patient uptake.
August 2011 Br J Cardiol 2011;18:179
Ranolazine in the management of chronic stable angina
Khalid Khan, Matthew Jones

Ranolazine has been evaluated in three trials in patients with stable angina (MARISA, CARISA and ERICA) and one large trial of patients with non-ST elevation acute coronary syndromes (MERLIN-TIMI 36). It has shown an improvement in exercise performance and a decrease in angina attacks. Ranolazine has similar efficacy in younger and elderly patients. Observational experience with ranolazine from a large UK centre is described.

August 2011 Br J Cardiol 2011;18:180–84
Community-based cardiovascular risk reduction: age and the Framingham risk score
Gill Richardson, Hugo C van Woerden, Rhiannon Edwards, Lucy Morgan, Robert G Newcombe

This study examined the effect of a community-based intervention on the natural rise with age of the Framingham 10-year risk score. Patients in the 45–64-year-old age group from 10 general practices were sent an invite card including five self-screening questions. Those with any of the prescribed risk factors were invited to arrange an appointment to assess their risk of heart disease, where a Framingham risk score was calculated and advice given, and then invited for re-assessment around 18 months later.
Of 6,704 individuals contacted, 2,017 individuals (30.1%) arranged a health check, 982 followed up, and risk scores were calculated on 727. A significant reduction in the geometric mean Framingham risk was observed (from 10.65% to 10.34%), largely attributable to improvements in systolic blood pressure, high-density lipoprotein (HDL), reduced smoking and, perhaps, increased fruit and vegetable consumption. Although participants were 1.5 years older at follow-up, their risk profile corresponded to being 0.55 years younger, and, arguably, progression of risk was wound back by just over two years. Some self-selection bias was apparent, as those followed up had higher mean anxiety/depression scores at baseline.
In conclusion, community interventions can reduce cardiovascular risk even in deprived communities, although further analysis is required to establish cost-effectiveness.

August 2011 Br J Cardiol 2011;18:185–88
Implementation of the new NICE guidelines for stable chest pain: likely impact on chest pain services in the UK
Dominic Kelly, Stephen Cole, Fiona Rossiter, Karen Mallinson, Anita Smith, Iain Simpson

National Institute for Health and Clinical Excellence (NICE) guidelines for the management of chest pain suggest a care pathway based on symptoms and clinical risk, which differs from that currently used in most hospitals. To compare the impact on workload, and costs of these guidelines with the current ‘exercise electrocardiogram (ECG)’-based service, a retrospective review of 150 patients referred to our rapid access chest pain clinic was performed. We compared investigations under the current system with that expected under the NICE guidelines. Cost analysis was performed to compare the two methods. GP questionnaires investigated likely changes in primary care referrals.

August 2011 Br J Cardiol 2011;18:189–92
Audit of the NT-ProBNP guided transthoracic echocardiogram service in Southend
Abdul M Mozid, Sofia A Papadopoulou, Alison Skippen, Azhar A Khokhar

Heart failure is one of the most common conditions in industrialised society. Plasma N-terminal prohormone of brain natriuretic peptide (NT-ProBNP) levels are raised in heart failure and increase with severity and New York Heart Association functional class. A NT-ProBNP level guided community echocardiogram service has been in place at Southend University Hospital since 2005. A previous audit of the service in 2006 showed that a cut-off point of 300 pg/ml provided a negative predictive value of 97% for detecting significant left ventricular systolic dysfunction, defined as an estimated ejection fraction of less than 40%. We have now repeated the audit for the calendar year 2008 and have shown that an additional cut-off point of 450 pg/ml can be applied to the over 75 age group with a reassuring negative predictive value of 96%.
June 2011 Br J Cardiol 2011;18:120–3
Could coronary artery calcium scores replace exercise stress testing? A DGH analysis
John A Purvis, Sinead M Hughes

The National Institute for Health and Clinical Excellence (NICE) has issued guidance on the investigation of patients with recent onset of chest pain, recommending CT calcium scoring (CAC) as the preferred test in some low-risk groups. This reflects concern about the low sensitivity (high false positive rate) of exercise stress tests (EST). This represents a major shift away from traditional rapid-access EST clinics and has generated concern. We looked at 125 consecutive ungraded patients with equivocal ESTs referred for CAC, and CT coronary angiography (CTA), if required. We found that 53% of patients had a CAC = 0 and would need no further testing under the NICE protocol. We estimate this would rise up to 70–80% if only low likelihood patients were studied. Two per cent of patients with a CAC = 0 required coronary intervention.
As per NICE protocol, all patients with a CAC between 1 and 400 underwent CTA, and, of these, 25% required invasive coronary angiography (ICA) and 17% underwent coronary intervention.
The overall strategy of CAC followed by CTA (if CAC between 1 and 400) and ICA (if CAC >400) produced a final sensitivity of 88% (higher than EST) and a negative predictive value of 98% (similar to EST). We believe the strategy is a useful way to assess recent onset chest pain but concerns about radiation dose, availability and patients with obstructive non-calcific plaque remain.
June 2011 Br J Cardiol 2011;18:124–9
Varicose veins, haemorrhoids and the risk of circulatory diseases: record-linkage study
Faisal Rahman, Clare J Wotton, Michael J Goldacre

Varicose veins and haemorrhoids both involve the venous circulatory system, but it is unclear whether they are predictors of elevated rates of other circulatory diseases. Our aim was to determine whether they are.
We analysed an epidemiological database of hospital admission and day-case statistics, constructing cohorts of people admitted for care for varicose veins or haemorrhoids, and comparing their experience of subsequent circulatory diseases with a control cohort. Compared with the control cohort, there was an elevated risk of deep vein thrombosis (DVT) in the varicose veins cohort (rate ratio 1.20; 95% confidence interval 1.08–1.33) but not in the haemorrhoids cohort (0.90; 0.78–1.03). No other circulatory diseases showed significantly elevated risks associated with varicose veins or haemorrhoids. The rate ratio for coronary heart disease in the varicose veins cohort was 0.91 (95% confidence interval 0.88–0.95) and that in the haemorrhoids cohort was 0.98 (0.94–1.03).
We conclude that neither varicose veins nor haemorrhoids showed strong association, either positive or negative, with other circulatory diseases. There was a significant, but numerically modest, elevated risk of DVT associated with varicose veins. The risk of coronary heart disease in people with varicose veins was, if anything, a bit low.

June 2011 Br J Cardiol 2011;18:130–2
Drugs for diabetes: part 5 DPP-4 inhibitors
Claire McDougall, Gerard A McKay, Miles Fisher

The dipeptidyl peptidase-4 (DPP-4) inhibitors are a new class of oral drugs for the treatment of type 2 diabetes. They inhibit the breakdown of glucagon-like peptide-1 (GLP-1) and increase the incretin effect in patients with type 2 diabetes. In clinical practice they are associated with significant reductions in HbA1c, no weight gain and a low risk of hypoglycaemia. Initial cardiovascular safety studies have shown no increase in cardiovascular risk. Indeed, the suggestion of possible cardiovascular benefit seen in the safety studies is now being formally examined in large randomised-controlled trials with primary cardiovascular end points.

June 2011 Br J Cardiol 2011;18:133–7
Mild hyponatraemia and short-term outcomes in patients with heart failure in the community
Sudip Ghosh, Jude Smith, Jonathan Dexter, Colette Carroll-Hawkins, Noel O’Kelly

Hyponatraemia has been shown to be an independent predictor of mortality in selected patients with heart failure (HF) enrolled in clinical trials. The predictive value of hyponatraemia has not been evaluated in ambulatory heart failure patients in the community.
We evaluated 426 patients with left ventricular systolic dysfunction and hyponatraemia (between 125 and 135 mmol/L) under the care of a regional nurse-led community heart failure team between June 2007 and November 2008. Of all patients, 92% were on loop diuretics, 81% on angiotensin-converting enzyme (ACE) inhibitors, 90% on beta blockers and 48% on aldosterone antagonists. Mean age of the patients was 78.9 ± 4.7 years, 43% were females and mean New York Heart Association (NYHA) class was 2.3 ± 0.7. Patients were assigned into four groups based on their serum sodium: Group 1 (n=210), 133–135 mmol/L; Group 2 (n=123), 129–132 mmol/L; Group 3 (n=93), 125–128 mmol/L; Group 4 (n=200), >135 mmol/L. Mean follow-up was 12.2 ± 4.9 months. One-year survival was 93% in patients in Groups 1 and 2, 88% in those in Group 3 and 97% in Group 4 (p<0.0001). Risk-adjusted hazard ratios for six and 12-month re-hospitalisations for worsening HF were 2.9 (1.4–3.8) for Group 1 and 2 and 3.6 (1.4–4.2) for Group 3.
Persistent hyponatraemia is common in ambulatory HF patients in the community and is associated with worse clinical outcomes. It is also an independent predictor for mortality and HF hospitalisations. General practitioners are uniquely positioned to identify patients with hyponatraemia and ensure regular monitoring and appropriate referrals are instigated.
June 2011 Br J Cardiol 2011;18:138–41
Unrecognised mitral valve stenosis in a London multi-ethnic community
Abdul-Majeed Salmasi, Mark Dancy

Mitral valve stenosis (MS) is attributed mainly to rheumatic fever and may remain unrecognised for several years. Early diagnosis of this lesion is important in order to implement the necessary management when either severe or complicated by atrial fibrillation. However, its incidence in a multi-ethnic community has not yet been recognised. We retrospectively studied 2,099 consecutive subjects for the presence of MS. All the patients were newly referred by general practitioners to a community general cardiology clinic and hypertension clinic in a district of London because of different cardiac symptoms, significant cardiac history or because of uncontrolled hypertension. All the patients underwent echocardiography routinely. Classical clinical signs of MS were present in four patients. Echocardiography showed MS in eight patients, in four of whom the MS was mild, moderate in three and severe in one patient. None of the patients had symptoms related to the MS and all were in sinus rhythm both clinically and during Holter monitoring. Only one patient was Caucasian, two were of Caribbean origin and five were of Indo-Asian origin. Subsequent cardiac catheterisation and mitral valve replacement were successfully carried out in two patients. It is concluded that rheumatic MS is still prevalent in the UK population and is more common in subjects of Indo-Asian origin than either Caucasian or Afro-Caribbean subjects. MS was not recognised by the general practitioners: its diagnosis was only made possible by echocardiography.
June 2011 Br J Cardiol 2011;18:142–4
Coronary artery dissection secondary to cocaine abuse
Ayyaz Sultan, Abdul K Jahangir, Amal A Louis, Rangasamy Muthusamy

Spontaneous coronary artery dissection is a rare entity leading to acute coronary syndrome and sudden cardiac death. Most of these reported cases have occurred in young pregnant women and therapeutic management options are variable. We describe a case of a young patient who presented with ST-elevation myocardial infarction (STEMI) due to coronary artery dissection secondary to cocaine abuse.
April 2011 Br J Cardiol 2011;18:94−6
The great imposter, the great imitator
Shahid Aman, Philip Hasleton, Azad Hanna

Syphilis is a venereal disease that can also be acquired by exposure to infected blood and body fluids. The organism can cross the placenta and infect the unborn child. Untreated syphilis progresses through four stages: primary, secondary, latent, and tertiary stages. Syphilis is a great imitator; patients with syphilis can be a diagnostic challenge because of their wide-ranging clinical presentations. Although the incidence of syphilis has declined dramatically following the advent of penicillin therapy, it is still prevalent due to unsafe sex, multiple sexual partners and intravenous drug abuse. Primary and secondary syphilis can present with minor symptoms while tertiary syphilis can cause mortality in up to 20% of untreated patients due to neurological and cardiovascular complications.

April 2011 Br J Cardiol 2011;18:88−93
Public perception of atrial fibrillation and treatment-related adverse events in the UK
Scott Doyle, Andrew Lloyd, Mark Davis

This study aimed to describe adverse events associated with atrial fibrillation (AF), and the medications used to treat it, and to estimate the importance of these adverse events from the perspective of the condition-naïve general public. Fourteen adverse event health state descriptions associated with paroxysmal/persistent and permanent AF were produced based on EQ-5D survey data, a literature review, and qualitative input from patients and clinicians. Further interviews with clinicians and AF patients confirmed the content of the health states as descriptions appropriate to AF. In total, 127 members of the general public valued the health states in a time trade-off interview and ranking task.
The study revealed how the public view the disutility of adverse health states associated with the treatment of AF. Each of the adverse events was associated with a perceived impairment from their respective base position. Interstitial lung disease showed the greatest perceived impact on quality of life (–0.17 paroxysmal/persistent base; –0.15 permanent base), whereas peripheral vasoconstriction had the least impact (–0.01 paroxysmal/persistent; –0.02 permanent).
In conclusion, this study provides insight into the importance of treatment-related adverse events in AF. The quality of life estimates collected in this study may prove useful in populating cost-effectiveness analyses and informing clinical treatment decisions.

April 2011 Br J Cardiol 2011;18:84−7
Clopidogrel and proton-pump inhibitor interaction: viewpoint and practical clinical approach
Mohaned Egred

The role of clopidogrel after percutaneous coronary intervention (PCI) or acute coronary syndrome (ACS) is well supported by strong clinical evidence, which has led to a dramatic increase in its use.
The use of a combination of proton-pump inhibitors (PPIs) and clopidogrel has recently been questioned due to pharmacological interaction, with possible implications and effects on clinical outcome in patients using this combination. This has brought uncertainty and confusion into clinical practice. There is a definite interaction between the two drugs, at a pharmacodynamic level; however, the clinical relevance remains uncertain. In this article I will review the subject and suggest a management strategy, which I hope will be of help to clinicians dealing with these patients on a daily basis.

April 2011 Br J Cardiol 2011;18:82–3
Dose capping of enoxaparin results in sub-therapeutic anti-Xa level
Kristopher S Lyons, Vivienne Nesbitt, Ian B A Menown

Enoxaparin is recommended for treatment of patients with acute coronary syndromes (ACS). While plasma monitoring of enoxaparin is not usually required, it may be assessed by measuring plasma anti-Xa levels (therapeutic range 0.5–1.2 IU/ml). Low anti-Xa activity is independently associated with increased 30-day mortality. Although the typical ACS enoxaparin dose is 1 mg/kg twice daily, in clinical practice some treatment protocols dose cap to reduce bleeding risk (for example, some local units cap at 60 mg twice daily). We studied 20 consecutive patients admitted with ACS. All received enoxaparin 60 mg twice daily. Peak plasma anti-Xa activity was measured four to six hours after the morning dose of enoxaparin after at least two subcutaneous doses. Mean Thrombolysis in Myocardial Infarction (TIMI) risk score 4.2/7 and mean weight 81.9 kg. One third of patients (five male, two female) were found to have subtherapeutic anti-Xa levels (mean 0.35 IU/ml, range 0.2–0.49 IU/ml). The remainder had anti-Xa levels within the therapeutic range (mean 0.73 IU/ml, range 0.5–1.12 IU/ml). Mean weight was higher in those with subtherapeutic compared with therapeutic anti-Xa levels (89.9 vs. 77.6 kg; p=0.041). In conclusion, dose capping of enoxaparin at 60 mg twice daily in ACS patients may result in a significant proportion achieving subtherapeutic anti-Xa levels, potentially correlating with poorer outcome.

April 2011 Br J Cardiol 2011;18:78−81
Drugs for diabetes: part 4 acarbose
Ganesan Arungarinathan, Gerard A McKay, Miles Fisher

Acarbose is an alpha-glucosidase inhibitor acting in the gastrointestinal tract producing modest reductions in postprandial hyperglycaemia, with negligible risk of hypoglycaemia and weight gain. In a subgroup of the United Kingdom Prospective Diabetes Study (UKPDS), acarbose showed glycaemic benefits irrespective of the type of concomitant therapy. Acarbose was shown to produce a significant reduction in the progression to diabetes in patients with impaired glucose tolerance in the Study to Prevent Non-Insulin-Dependent Diabetes Mellitus (STOP-NIDDM) trial, and in a post-hoc analysis of STOP-NIDDM a reduction in cardiovascular events was observed. Gastrointestinal side effects are the main limiting factor in clinical practice, leading to high rates of non-compliance and discontinuation.
April 2011 Br J Cardiol 2011;18:73−6
Evolving trends in percutaneous coronary intervention
Ronak Rajani, Malin Lindblom, Gaynor Dixon, Muhammed Z Khawaja, David Hildick-Smith, Stephen Holmberg, Adam de Belder

As the proportion of patients above the age of 80 years in the UK is increasing it is likely that in the future cardiac centres will be treating an increasing number of octogenarians as part of their patient population. Despite this, there are little contemporary outcome data in this group of patients who often have complex coronary disease.
We aimed to assess, first, the change in demographics of patients undergoing percutaneous coronary intervention (PCI) over a 9-year period at a tertiary cardiac centre within the UK and, second, whether there has been a change in outcome for these patients in terms of major adverse cardiac and cerebrovascular events (MACCE). A retrospective review of registry data on patients who underwent PCI at our institute from 2000–2008 was undertaken. Patients were divided into three groups according to when they underwent PCI: Group A 2000–2002, Group B 2003–2005 and Group C 2006–2008. Demographic data were collected along with the nature of coronary disease treated and MACCE rates.
There were 3,108 patients in Group A, 4,744 patients in Group B and 3,860 patients in Group C. The use of rotablation increased from Group A (0.4%) to Group C (3.8%) (p<0.01), over-the-wire balloons from Group B (0.8%) to Group C (2.7%) (p<0.01), and microcatheters from Group B (0.1%) to Group C (1.25%) (p<0.01). This was accompanied by a decline in total MACCE rates from Group A (1%) to Group C (0.43%). The proportion of patients >80 years increased from Group A (5.8%) to Group C (12.2%) (p<0.01), and a similar decline in MACCE rates was also observed in this age group from Group A (4%) to group C (0.9%) (p<0.01).
In conclusion, the proportion of elderly patients requiring PCI is increasing. In this group of patients, PCI appears safe and is associated with declining complication rates.

February 2011 Br J Cardiol 2011;18:24-7
Drugs for diabetes: part 3 thiazolidinediones
David McGrane, Miles Fisher, Gerard A McKay

Thiazolidinediones (glitazones) are a relatively new addition to the type 2 diabetes drug armoury, but they have caused considerable controversy since they were introduced into the routine management of patients with type 2 diabetes. Until recently there were two thiazolidinediones licensed for use in the treatment of type 2 diabetes: rosiglitazone and pioglitazone, but the European Medicines Agency (EMEA) on the 23rd September 2010 removed rosiglitazone’s marketing authorisation across Europe because of concerns about cardiovascular safety. There is no evidence to show a similar cardiovascular safety concern for pioglitazone, apart from increased fluid retention and reported heart failure. Pioglitazone may still have a therapeutic role in the management of selected patients.
February 2011 Br J Cardiol 2011;18:28-32
The influence of an ageing population on care and clinical resource utilisation in cardiac surgery
Dumbor L Ngaage, George Britchford, Alexander R J Cale

The increasing population of elderly patients undergoing surgery has implications for care and resource utilisation, and the potential to meet operating targets. We prospectively reviewed collected data for 6,971 patients who underwent coronary bypass and/or heart valve operation from March 1998 through January 2007. Resource utilisation between young (<70 years) and elderly (≥70 years) patients was compared.
The elderly (n=2,664) were a higher operative risk than young patients (n=4,127). Peri-operative requirement for additional medications (inotropes, anti-arrhythmics, antibiotics), blood transfusions, further interventions (resternotomy, sternal re-wiring, gastrointestinal surgery, renal replacement therapy) and device implantation (intra-aortic balloon pump, ventricular assist device, Swan Ganz catheter, permanent pacemaker) in the elderly exceeded young patients by 32%, 20%, 5% and 2%, respectively. ‘Progression through care’ (intensive care management >24 hours, intensive care re-admission, hospitalisation >12 days, and discharge to convalescence) was delayed in elderly patients. The elderly had a 91% cumulative excess risk for incurring extra resource utilisation.
Clinical resource utilisation after cardiac surgery was substantially higher for elderly compared with young patients. With a growing elderly population of cardiac patients, new clinical measures and organisational changes are needed to maintain clinical productivity, the ability to meet targets, and improve operative outcomes.

February 2011 Br J Cardiol 2011;18:33
Survey of cardiac rehabilitation across the English Cardiac Networks 2007–2009
Muhammad Shahid, Anita Varghese, Abdul Moqsith, James Travis, Andrew Leatherbarrow, Russell I Tipson, Mark Walsh, Linda Binder, E Jane Flint

Cardiac Networks always promised to be effective health communities across which sharing good practice and ultimately redesigning ideal care pathways for patients including Cardiac Rehabilitation (CR) could be made. The Black Country Cardiovascular Network in collaboration with the NHS Improvement programme conducted this observational study aiming at assessing and encouraging CR development across the English Cardiac Networks.
February 2011 Br J Cardiol 2011;18:34-6
Aortic valvuloplasty – is a revival merited?
Richard J Jabbour, Dion Stub, Antony S Walton

Balloon aortic valvuloplasty (BAV), first developed last century for the management of symptomatic aortic stenosis, was met with great enthusiasm due to its new and minimally invasive technique, but it has now largely been abandoned due to suboptimal results and a high restenosis rate. However, with the development of new techniques and the arrival of transcatheter aortic valve implantation (TAVI), BAV’s use is starting to increase. In this article we put forward the case for a revival in BAV by exploring the traditional uses and safety of BAV as a procedure as well as a novel role as a bridge to TAVI.
February 2011 Br J Cardiol 2011;18:37-45
Efficacy and safety of extended-release niacin/laropiprant in patients with type 2 diabetes mellitus
Alexandra MacLean, James M McKenney, Russell Scott, Eliot Brinton, Harold E Bays, Yale B Mitchel, John F Paolini, Hilde Giezek, Kristel Vandormael, Rae Ann Ruck, Kendra Gibson, Christine McCrary Sisk, Darbie L Maccubbin

Cardiovascular disease is a major cause of death in patients with type 2 diabetes mellitus (T2DM) and multiple lipid abnormalities are common. Niacin effectively treats diabetic dyslipidaemia and reduces cardiovascular events in high-risk patients. We evaluated the lipid-altering efficacy and safety (especially, glycaemic control) of extended-release niacin/laropiprant (ERN/LRPT; a tablet containing 1 g ERN and 20 mg LRPT) in patients with T2DM. In this multi-centre, double-blind, placebo-controlled, 36-week study, patients (n=796) were randomised 4:3 to ERN/LRPT or placebo. After four weeks at 1 g/day, ERN/LRPT was doubled to 2 g/day (two tablets) for the remainder of the study. The vast majority of randomised patients (~90%) were dyslipidaemic based on medical history or baseline lipid levels; approximately 80% were taking statins and 99% were on an antihyperglycaemic regimen. At week 12, ERN/LRPT produced significant (p≤0.001 for all) percentage changes from baseline in low-density lipoprotein cholesterol (LDL-C) (–17.9%), high-density lipoprotein cholesterol (HDL-C) (23.2%), LDL-C:HDL-C (–32.0%), triglycerides (–23.1%), apolipoprotein (Apo) B (–17.1%), Apo A-I (8.2%) and total cholesterol (TC):HDL-C (–22.9%) versus placebo. The clinical and laboratory adverse events that occurred more frequently in the ERN/LRPT group versus the placebo group were pruritus, rash, flushing, gastrointestinal upset and elevations in alanine aminotransferase, aspartate aminotransferase, fasting plasma glucose (FPG) and glycosylated haemoglobin (HbA1c). From baseline to week 36, median FPG and HbA1c increased with ERN/LRPT from 7.31 to 7.88 mmol/L and 6.9 to 7.3%, respectively, consistent with known niacin effects. More patients in the ERN/LRPT group required intensified antihyperglycaemic therapy (17.6% vs. 8.2%; p≤0.001). In this population of patients with T2DM, ERN/LRPT produced significant, durable improvements in lipids/lipoproteins and had a safety profile consistent with ERN/LRPT and ERN alone in other populations.
February 2011 Br J Cardiol 2011;18:46-9
Contemporary coronary imaging from patient to plaque: part 5 a glimpse of the future
Scott W Murray

In this series of articles looking at contemporary ways to image atherosclerosis, we have covered the main techniques used in the UK as diagnostic tools and research modalities. For this final article, I have chosen to concentrate on new technologies that show promise for the future.
November 2010 Br J Cardiol 2010;17:271–6
Outcomes following catheter ablation of atrial fibrillation in the UK – a single-centre cohort analysis
Rohan Gunawardena, Stephen S Furniss, Ewan Shepherd, Giuseppe Santarpia, Stephen W Lord, John P Bourke

The outcome and complications of atrial fibrillation (AF) ablation in a UK patient cohort were investigated by offering symptomatic, drug-refractory patients ablation. Treatment goals were to disconnect all pulmonary veins electrically and improve symptoms using a state-of-the-art ablation method. Outcomes were defined as: 'success' (no symptoms or Holter AF); 'partial success' (substantially reduced AF symptoms); 'clinical success' ('success' and 'partial success'); 'failure' (no symptom improvement).

November 2010 Br J Cardiol 2010;17:279–82
Drugs for diabetes: part 2 sulphonylureas
Christopher J Smith, Miles Fisher, Gerard A McKay

Sulphonylureas are well established in the treatment of type 2 diabetes mellitus. They are effective in improving glycaemic control and preventing microvascular complications. Side effects that can restrict use include hypoglycaemia and weight gain. Although there is no clear evidence for reduction of cardiovascular disease from randomised-controlled trials, follow-up data from the United Kingdom Prospective Diabetes Study (UKPDS) shows reduced cardiovascular risk. Concerns about sulphonylureas causing inhibition of ischaemic preconditioning are relevant in primary angioplasty, but there is a lack of clear evidence, with a need for randomised-controlled trials to investigate this further.
November 2010 Br J Cardiol 2010;17:283–5
Cardiac auscultation: the past, present and future
Omar Asghar, Uazman Alam, Sohail Khan, Sajad Hayat, Rayaz A Malik

Cardiac auscultation is a critical part of the clinical examination. In this review we discuss the conventional approach to teaching and using the skill of cardiac auscultation. We then consider how recent technological advances may improve the teaching and implementation of this essential clinical skill.

November 2010 Br J Cardiol 2010;17:286–9
Establishing an aortic stenosis surveillance clinic
David Turpie, Matthew Maycock, Chiala Crawford, Kathleen Aitken, Marwen Macdonald, Colin Farman, Maimie L P Thompson, Jamie Smith, Stephen J Cross, Stephen J Leslie

The number of patients with aortic stenosis (AS) in the UK is increasing. Patients with non-significant AS can be safely reviewed in technician-led clinics. The potential impact of this on healthcare services is unreported. The aim of this study was to describe the impact of establishing an AS surveillance clinic in a district general hospital setting and consider the potential impact of widespread implementation.
November 2010 Br J Cardiol 2010; 17:290-92
Contemporary coronary imaging from patient to plaque: part 4 magnetic resonance imaging
Alistair C Lindsay, Scott W Murray, Robin P Choudhury

In recent years a large amount of research has focused on developing both invasive and non-invasive methods of assessing atherosclerosis. In this regard, magnetic resonance imaging (MRI) is safe, non-invasive, requires no ionising radiation, and is capable of giving high-resolution images of atherosclerotic plaque. As a result, MRI has been extensively applied to imaging of the vascular system – in particular, the carotid arteries – where it has been shown to have the ability to not only accurately quantify the extent of atherosclerotic plaque disease, but also to identify several compositional features suggestive of plaque vulnerability. Imaging of the relatively small coronary arteries has, until now, been limited by the problems of cardiac and respiratory motion, however, more recently, technological advancements have allowed more detailed plaque information to be acquired. This article will review the origins of MRI imaging of atherosclerotic disease, its current status, and its potential future applications.
November 2010 Br J Cardiol 2010; 17:293-95
Subxiphoid pericardiocentesis guided by contrast echocardiography in a patient with cardiac tamponade
Andrew J Turley, Byju Thomas, Richard J Graham

A 66-year-old male presented with increasing dyspnoea. He was an ex-smoker and had been diagnosed with stage IV undifferentiated large cell carcinoma of the left lung two months previously. Clinical examination revealed signs consistent with cardiac tamponade. Cardiac tamponade, a life-threatening condition, is a continuum of haemodynamic compromise, initiated by a collection of fluid in the pericardial space causing an increase in intra-pericardial pressure and cardiac compression. Transthoracic echocardiography confirmed the presence of a large global pericardial effusion with echocardiographic signs of cardiac tamponade (figure 1A and 1B).
September 2010 Br J Cardiol 2010;17:223–9
Epilepsy and the heart
Fergus J Rugg-Gunn, Diana Holdright

Cerebrogenic control of cardiac function is well recognised and acute neurological events, including epileptic seizures, may cause a disturbance of cardiac function even in the absence of significant cardiac structural or electrophysiological abnormalities. Sudden unexpected death in epilepsy (SUDEP) is a major cause of mortality in patients with epilepsy. Cardiac dysrhythmias are a potential cause of SUDEP.

September 2010 Br J Cardiol 2010;17:231–4
Drugs for diabetes: part 1 metformin
James G Boyle, Gerard A McKay, Miles Fisher

Metformin is one of the oldest oral treatments to reduce hyperglycaemia in people with diabetes. Gastrointestinal side effects are common, and metformin should be used with caution in patients with renal impairment because of the slight risk of lactic acidosis. In the United Kingdom Prospective Diabetes Study (UKPDS) patients treated with metformin had a significant reduction in myocardial infarction and mortality that was not demonstrated in patients treated with sulphonylureas or insulin. The fact that metformin significantly reduces cardiovascular events plus reduces weight has meant that metformin is the drug of first choice in guidelines for the treatment of type 2 diabetes. There are no longer concerns about using metformin in patients with chronic heart failure, other than in patients with associated renal failure, or during episodes of acute left ventricular failure when metformin should be temporarily stopped.
September 2010 Br J Cardiol 2010;17:235-9
Contemporary coronary imaging from patient to plaque: part 3 cardiac computed tomography
Daniel R Obaid, Scott W Murray, Nick D Palmer, James H F Rudd

The role of cardiac computed tomography (CT) in clinical practice is constantly evolving. Early machines were only capable of measuring coronary calcification. Advances in temporal and spatial resolution, especially the introduction of 64-detector rows, now mean that high-quality non-invasive angiograms are possible in most patients. This review will outline the capabilities and limitations of coronary artery imaging with CT, and also highlight areas that differentiate CT from X-ray angiography, including direct plaque visualisation and potential vulnerable plaque identification.

September 2010 Br J Cardiol 2010;17:240–3
A single defibrillation safety margin test is sufficient in most ICD patients: experience from a UK tertiary centre
Faizel Osman, Abubakar Habib, Mohamed Jeilan, Suman Kundu, Jiun Tuan, Rajkumar Mantravadi, J Douglas Skehan, Peter J Stafford, Ravi K Pathmanathan, G Andre Ng

Ventricular fibrillation (VF) is induced at the time of implantable cardioverter defibrillator (ICD) implantation in the UK, typically at least twice, with defibrillation ≥10 J below the maximum output. With the advent of modern leads/devices a single test may be sufficient.
September 2010 Br J Cardiol 2010;17:244
Aneurysmal saphenous vein graft rupture: late complication of coronary artery bypass surgery
Alice Wort, Matthew Bates

A 72-year-old man, who underwent coronary artery bypass grafting 14 years previously, presented with sharp posterior chest pain and presyncope.
September 2010 Br J Cardiol 2010;17:245–8
Ictal bradycardia and asystole associated with intractable epilepsy: a case series
Elijah Chaila, Jaspreet Bhangu, Sandya Tirupathi, Norman Delanty

Ictal bradycardia/asystole is a poorly recognised cause of collapse late in the course of a typical complex partial seizure. Its recognition is important as it might potentially lead to sudden unexpected death in epilepsy (SUDEP). We present five patients with intractable complex partial seizures who had associated ictal bradycardia/asystole. All the patients underwent cardiac pacing to potentially prevent SUDEP. It is important to recognise and treat ictal asystole early, and to achieve this there is need for both an increase in epilepsy monitoring beds and a recognition of the potential role of implantable loop recorders in the evaluation of patients with epilepsy who clinically appear to be at increased risk for ictal asystole.

July 2010 Br J Cardiol 2010;17:175-9
Meeting the psychological needs of cardiac patients: an integrated stepped-care approach within a cardiac rehabilitation setting
Alison Child, Jane Sanders, Paul Sigel, Myra S Hunter

Depression and anxiety are commonly experienced by cardiac patients and are associated with reduced quality of life and mortality, but the evidence for the effectiveness of medical and psychological treatments for depression has been mixed.
July 2010 Br J Cardiol 2010;17:181-3
Rehabilitation on the move: teaching cardiac rehabilitation in a novel way
Sher Muhammad, E Jane Flint, Russell I Tipson

Coronary heart disease is a leading cause of mortality and morbidity worldwide. Risk factor modification through a robust cardiac rehabilitation programme is rewarding and accounts for the major decline in mortality due to coronary heart disease in the long term,1 thus, making it an essential part of the curriculum. With this in mind, we conducted an observational study based on the feedback of 114 medical students over a four-year period about exercise tutorial in cardiac rehabilitation. Data were collected on a 10-point scale questionnaire. An overwhelming majority of students (more than 90%) were deeply impressed by this novel approach of being taught about cardiac rehabilitation. They strongly recommended this unique approach, as not only an effective tutorial on cardiac rehabilitation, but also advocated it enthusiastically as a general teaching method.

July 2010 Br J Cardiol 2010;17:185-9
‘Time is muscle’: aspirin taken during acute coronary thrombosis
Peter C Elwood, Gareth Morgan, Malcolm Woollard, Andrew D Beswick

Low-dose aspirin is of value in the long-term management of vascular disease, and the giving of aspirin to patients believed to be experiencing an acute myocardial infarction (AMI) is standard practice for paramedics and doctors in most countries. Given during infarction, aspirin may disaggregate platelet microthrombi and may reduce the size of a developing thrombus. Effects of aspirin other than on platelets have also been suggested and these include an increase in the permeability of a fibrin clot and an enhancement of clot lysis. Animal experiments have also shown a direct effect of aspirin upon the myocardium with a reduction in the incidence of ventricular fibrillation. Randomised trials have shown that the earlier aspirin is taken by patients with myocardial infarction, the greater the reduction in deaths. We suggest, therefore, that patients known to be at risk of an AMI, including older people, should be advised to carry a few tablets of soluble aspirin at all times, and chew and swallow a tablet immediately, if they experience severe chest pain.
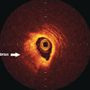
July 2010 Br J Cardiol 2010;17:190-3
From patient to plaque. Contemporary coronary imaging – part 2: optical coherence tomography
Sudhir Rathore, Scott W Murray, Rodney H Stables, Nick D Palmer

Intra-coronary imaging has become a cornerstone of visualising atherosclerotic coronary artery disease and also to guide the therapy in selected high-risk cases. Optical coherence tomography (OCT) is an imaging modality quite similar to intravascular ultrasound (IVUS), but uses light instead of sound. In the second article on contemporary coronary imaging, the potential of OCT is discussed.
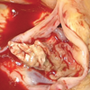
July 2010 Br J Cardiol 2010;17:195-200
The role of nucleic acid amplification techniques (NAATs) in the diagnosis of infective endocarditis
Gillian Rodger, Stephen Morris-Jones, Jim Huggett, John Yap, Clare Green, Alimuddin Zumla

Infective endocarditis (IE) causes high rates of morbidity and mortality. Clinical management is problematic if there are uncertainties over the identity, viability or antibiotic susceptibility of the causative organism. Between 10% and 30% of IE blood cultures are negative, usually a result of prior antimicrobial therapy, but also occurring when causative micro-organisms are non-cultivable or fastidious. While evidence-based guidelines exist for treatment of IE caused by defined agents, clinicians are often faced with the dilemma of IE of unproven aetiology. Duration of empirical therapy is usually titrated against overall clinical response and non-specific laboratory markers of inflammation, but these may bear little relation to ongoing microbial activity in the heart valve. There is an increasing need for more specific, sensitive and rapid tests for the identification of causative organisms. Nucleic acid amplification technologies (NAATs) show promise for rapid detection of pathogen nucleic acid in blood or tissue. This review discusses the developments in this field, and the potential for the application of NAATs to improve aetiological identification in IE.
May 2010 Br J Cardiol 2010;17:125-7
Safe combined intravenous opiate/benzodiazepine sedation for transoesophageal echocardiography
Kulveer Mankia, Rokas Navickas, Edward D Nicol, Sacha Bull, Junaid Khan, Sayeed Raza, Harald Becher, Paul Leeson, Christopher Palin

There is much debate about the optimal sedation strategy for transoesophageal echocardiography (TEE). Despite previous studies demonstrating the potential benefits of combining opiates and benzodiazepines for conscious sedation, and previous published national surveys and recommendations, sedation practice for TEE in clinical practice varies widely within the UK. All UK centres routinely use midazolam, but only 7% of centres use it in combination with an opiate: 14% of hospitals report no routine use of sedation for TEE. There is no British Society of Echocardiography (BSE) recommended TEE sedation protocol within the UK and even where guidelines exist locally, 82% of operators report being unaware of their details. Consequently, a wide range of sedative doses are used and many patients are reported to be over-sedated. We developed a new protocol for conscious sedation using intravenous pethidine and midazolam for TEE and have shown it to be safe and effective when implemented within an existing TEE service.

May 2010 Br J Cardiol 2010;17:129-32
Contemporary coronary imaging from patient to plaque part 1: IVUS-derived virtual histology
Scott W Murray

From the days of Virchow and the analysis of post-mortem coronary specimens, an enormous amount of knowledge has been built about coronary pathophysiology. In the 1950s the dream of in vivo coronary imaging became a reality with the invention of coronary arteriography under the guidance of Mason Sones. As we fast forward 50 years, it has become clear that angiography has helped us focus on areas of stenosis and flow limitation, but the main problem of coronary artery disease is much more complex than can appear on a luminal silhouette. The finding of ‘normal coronary arteries’ following angiography is short-sighted and does not take into account the potential of unstable disease lurking within the vessel wall. We begin the series with intravascular ultrasound.
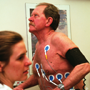
May 2010 Br J Cardiol 2010;17:133-7
Exercise heart rate guidelines overestimate recommended intensity for chronic heart failure patients
Louisa Beale, Helen Carter, Jo Doust, Gary Brickley, John Silberbauer, Guy Lloyd

In UK cardiac rehabilitation programmes, exercise training is often set at a percentage of maximal heart rate or heart rate reserve, either predicted or measured. Problems may arise when using this method for chronic heart failure (CHF) patients who often have chronotropic incompetence and are treated with beta blockers. A safer approach is to use cardiopulmonary exercise testing to prescribe training below the ventilatory threshold, thus ensuring that the exercise is moderate. The aim of this study was to determine whether British Association for Cardiac Rehabilitation (BACR) heart rate guidelines prescribe moderate intensity exercise for CHF patients. The only target heart rate range to prescribe exercise below the ventilatory threshold was 60–80% measured maximum heart rate. Target heart rates calculated from predicted maximum values were higher than those from measured values, and the heart rate reserve method resulted in the highest target heart rates. Cardiac rehabilitation exercise practitioners should be aware that these methods may well result in CHF patients performing heavy rather than moderate exercise.

May 2010 Br J Cardiol 2010;17:138-41
10 steps before you refer for diabetes
Brian Karet, Andrew Pettit

Diabetes mellitus is caused by an absolute or relative lack of insulin.1 This article covers people with type 2 diabetes, as most people with type 1 diabetes will be under the care of a secondary care team for at least some of their care. Type 2 diabetes is not primarily about sugar, but about moderating the vascular and neurological damage resulting from chronic hyperglycaemia. Many people with type 2 diabetes will also have components of the metabolic syndrome,2 namely hypertension, dyslipidaemia and obesity, all of which need separate and sometimes overlapping interventions.

May 2010 Br J Cardiol 2010;17:142-3
Achieving the dose: an audit of discharge medication for the secondary prevention of myocardial infarction
Kyle J Stewart, Pippa Woothipoom, Jonathan N Townend

To establish whether the medication received by patients post-myocardial infarction was prescribed at therapeutic doses, we performed a retrospective audit of discharge summaries. Over three quarters (75.1%) of all patients in the study group were discharged on sub-therapeutic doses of angiotensin-converting enzyme (ACE) inhibitors and beta blockers. In contrast, nearly all (94–97%) patients received a statin at a therapeutic dose. Aspirin and clopidogrel, where prescribed, were also within the therapeutic range in 100% of patients. These findings illustrate the difficulty in optimising the doses of drugs that have a wide range of possible doses during short hospital admissions.

May 2010 Br J Cardiol 2010;17:148-50
Atrial space-occupying lesions – the role of multi-modality imaging
Sanjay M Banypersad, Matthias Schmitt

Cardiac magnetic resonance (CMR) has much to offer in the clinical assessment of intra-cardiac space-occupying lesions (SOL). Below we describe the use of CMR as a second-line investigation complementing the use of other imaging modalities, using the example of three patients with atrial SOL. We briefly review the literature and discuss the use of CMR within the context of multi-modality imaging of cardiac SOL.
May 2010 Br J Cardiol 2010;17:144-7
Antibiotic prophylaxis for permanent pacemaker implantation: an observational study of practice in England
Jamal Nasir Khan, Veeran Subramaniam, Christopher Hee, Neeraj Prasad, James M Glancy

There are no guidelines on the practice of antibiotic prophylaxis in pacemaker implantation resulting in wide variation in practice. We sought to investigate this and identify areas for further study and improvement. Using an email questionnaire, followed up with a telephone call if no response, all 121 adult National Health Service hospitals in England implanting pacemakers were asked about use of systemic prophylactic antibiotics at implantation. Data were obtained from 61 hospitals (50.4% of total contacted), covering a wide geographic distribution.

March 2010 Br J Cardiol 2010;17:76–80
Recommendations on the clinical use of B-type natriuretic peptide testing (BNP or NTproBNP) in the UK and Ireland
Martin R Cowie, Paul O Collinson, Henry Dargie, FD Richard Hobbs, Theresa A McDonagh, Kenneth McDonald, Nigel Rowell

Plasma natriuretic peptide (NP) testing is not widely used in heart failure clinical practice in the UK or Ireland, despite a large evidence base. This article reports the views of a consensus group that was set up to develop guidance on the place of NP testing for clinicians in primary and secondary care.
March 2010 Br J Cardiol 2010;17:86–8
Whatever happens to the cardioverted? An audit of the success of direct current cardioversion for atrial fibrillation in a district general hospital over a period of four years
David A Sandler

Direct current cardioversion (DCCV) to restore sinus rhythm (SR) in patients with persistent atrial fibrillation (AF) remains a therapeutic option, though recent studies have questioned its need and value in the longer term.
March 2010 Br J Cardiol 2010;17:89–92
Audit of management of atrial fibrillation at a district general hospital
Joanna C E-S Lim, Ajay Suri, Sangeetha Sornalingham, Tuan Peng Chua

Atrial fibrillation (AF) is the most common cardiac arrhythmia and is a major risk factor for stroke. The 2006 National Institute for Health and Clinical Excellence (NICE) guidelines on management of AF recommended the use of beta blockers and calcium channel blockers in preference to digoxin for first-line rate control and emphasised the importance of appropriate thromboprophylaxis.
March 2010 Br J Cardiol 2010;17:93
Femoral artery dissection – an uncommon but well-recognised complication of coronary angiography
Alexander W Y Chen, Oliver J Rider, Anthony Li

Coronary angiography is commonly performed via the right femoral artery. Under local anaesthetic, the arterial lumen is initially cannulated with a wide-bore needle, then a long and soft J wire is inserted through the needle. The needle is then removed, and an arterial sheath is passed over the wire using a Seldinger technique.
March 2010 Br J Cardiol 2010;17:94–6
Brady/tachyarrhythmia preceding the diagnosis of cardiac sarcoid
Henry Oluwasefunmi Savage, Sheel Patel, Jonathan Lyne, Tom Wong

Cardiac sarcoid remains a notoriously difficult to diagnose condition and arrhythmias remain an important initial presentation. It is amenable to treatment therefore it is important to make an early diagnosis to reduce morbidity and mortality.
November 2009 Br J Cardiol 2009;16:281-6
Pharmaceutical salts: a formulation trick or a clinical conundrum?
Aateka Patel, Stuart A Jones, Albert Ferro, Nilesh Patel

The term pharmaceutical salt is used to refer to an ionisable drug that has been combined with a counter-ion to form a neutral complex. Converting a drug into a salt through this process can increase its chemical stability, render the complex easier to administer and allow manipulation of the agent’s pharmacokinetic profile. Salt selection is now a common standard operation performed with small ionisable molecules during drug development, and in many cases the drug salts display preferential properties as compared with the parent molecule. As a consequence, there has been a rapid increase in the number of drugs produced in salt form, so that today almost half of the clinically used drugs are salts. This, combined with the increase in generic drug production, means that many drugs are now produced in more than one salt form. In almost all cases where multiple drug salts of the same agent exist, they have been marketed as therapeutically equivalent and clinicians often treat the different salt forms identically. However, in many cases this may not be justified. This review describes why many pharmaceutical salts are, in fact, not chemically equivalent, and discusses whether such chemical differences may translate into differences in therapeutic effectiveness. It will also explore, with examples, what the clinical cardiologist should consider when prescribing such agents for their patients.
November 2009 Br J Cardiol 2009;16:288-91
10 steps before you refer for peripheral arterial disease
Michael Scott, Gerard Stansby

Peripheral arterial disease (PAD) is a condition that is frequently underdiagnosed and often the subject of suboptimal care. It can present with rest pain or gangrene (critical ischaemia), but this is not common. Intermittent claudication (IC), leg pain on walking, is its most common manifestation. Leg pain on walking is a presentation commonly seen in general practice, and has several potential causes other than PAD. IC has been shown to affect 4.5% of subjects between the ages of 45 and 65 years and is a marker for increased cardiovascular risk.1 In respect of the leg itself, IC is a relatively benign condition with most patients improving or stabilising and fewer than 5% progressing to major amputation. However, patients with IC are at increased risk of death, especially due to vascular events in the coronary and cerebral territories.2 PAD is caused by the occlusion or narrowing of large peripheral arteries, usually from atherosclerosis, and, as such, it shares all the major risk factors that can lead to myocardial infarction (MI) or stroke. Most patients with PAD will also have disease (either symptomatic or asymptomatic) in their coronary and cerebral circulation, and MI and stroke are common causes of death in patients with PAD. Vigilance for the condition will provide opportunities to reduce cardiovascular risk in a group who are high risk. Accurate diagnosis and assessment will reveal those who would most benefit from specialist intervention.
November 2009 Br J Cardiol 2009;16:292–4
The joint cardiology–cardiothoracic multi-disciplinary team (MDT) meeting: patient characteristics and revascularisation outcomes
Wai Kah Choo, Rajiv Amersey

The multi-disciplinary approach provides a forum for peer review of angiographic data. We aimed to examine the outcomes of our multi-disciplinary team (MDT) meetings in a two-year follow-up study. A total of 191 patients were studied and mainly divided into groups offering conservative therapy, percutaneous coronary intervention (PCI) or coronary artery bypass surgery (CABG). CABG was offered to 60% of patients with left main stem disease, 45% with proximal left anterior descending artery lesions and 59% with triple-vessel disease. PCI was offered to 40% of patients with single-vessel disease. One death was observed in the PCI group at two years, substantially lower than deaths in other groups. Overall mortality at two years was 6.4%. PCI conferred a significantly higher need for repeat revascularisation compared with surgery (odds ratio 5.71, p=0.005). Our results resonate with outcomes of published trial data comparing CABG and PCI.
November 2009 Br J Cardiol 2009;16:295–8
Colesevelam – where does it fit into our clinical practice?
Devaki Nair

The treatment of raised cholesterol has advanced significantly in the last 25 years: fibrates, statins, bile acid sequestrants, ezetimibe, and more. In October 2007, colesevelam hydrochloride was launched into the UK market. This article reviews where this product fits into everyday clinical practice, in which patients it is best suited, and discusses practical issues in the everyday use of this reformulated bile acid sequestrant.
November 2009 Br J Cardiol 2009;16:299–302
Lifespan and cardiology
Kiran Patel, Yin May Yan, Kamlesh Patel, Parminder Judge, Janki Patel, Sandeep Johal, Sukhdip Johal, Paul Do, Francisco Leyva

We undertook a seven-year in-depth review of all reported obituaries of medical practitioners in the BMJ to assess the age and disease distribution of mortality of medical practitioners in order to identify relationships between mortality and discipline, ethnicity and other demographic factors. In total, 3,342 obituaries reported in the BMJ from January 1997 to December 2004 were reviewed. The majority of obituaries were of male doctors. Doctors who qualified in the developed world appeared to live longer (mean age at death of 78 years) than those who qualified in Asia (mean age at death of 70 years). White-European doctors lived significantly longer than doctors from other ethnic groups. There was no significant difference in longevity between doctors working in the primary care sector and those in the secondary care sector. An eighth (12.5%) of doctors died between the ages of 60 and 70 years and, of these, nearly half died between the ages of 61 and 65 years. There were significantly more suicides and accidental deaths in Accident and Emergency (A&E) doctors compared with other specialties. In conclusion, cardiologists are not immortal and need to retire, as do their colleagues in other specialties. Retirement at ages of 65 years or above would disadvantage nearly one in six medical practitioners. Those likely to be most disadvantaged by a mandatory rise in any retirement age, in terms of reaping the benefits of their pension contributions, are those of a non white-European ethnicity.
November 2009 Br J Cardiol 2009;16:303–4
Contrast enhanced cardiac magnetic resonance in the decision making for revascularisation
Khaled Alfakih, Kate Pointon, Thomas Mathew

Contrast enhancement cardiac magnetic resonance (CE-CMR) is a new tool for the assessment of myocardial viability. The technique uses an inversion-recovery prepared T1-weighted gradient-echo pulse sequence after the intravenous administration of a gadolinium-chelate (Gd). Gd diffuses into the interstitium but not the myocardial cells, hence, infarcted myocardium has an increased concentration of Gd resulting in hyper-enhancement. CE-CMR was validated in animal models,1 and human studies confirmed that the technique identifies the presence and extent of myocardial infarction in addition to predicting reversible myocardial dysfunction in patients undergoing revascularisation.2-4 The CE-CMR images consist of short-axis and long-axis slices of the left ventricle (LV) and are analysed based on the 17-segment model of the LV. The non-viable myocardial tissue is hyper-enhanced and white. The degree of the transmurality of the contrast enhancement (CE) in each segment is scored, based on outcome data, where <25% transmurality is highly likely to recover function, 25–50% transmurality is potentially viable with 50% chance of recovering function, and >50% transmurality is unlikely to be viable.2-4 We present two cases, which illustrate the usefulness of this technique in detecting viable myocardium and facilitating the clinical decision-making process for revascularisation.
September 2009 Br J Cardiol 2009;16: 231-235
Abdominal aortic aneurysm screening in patients with established ischaemic heart disease
Rachel Abela, Ioannis Prionidis, Timothy Beresford, Gerald Clesham, Delphine Turner, Reto Gamma, Tom Browne

Within a prospective observational study we investigated whether patients undergoing coronary angiograms present a more accessible and significant cohort for abodominal aortic aneurysm (AAA) screening. With local research ethics committee approval, over 36 days, 106 consecutive patients consented to and underwent a five to eight minute aortic scan, using a portable ultrasound unit, during the recovery period after angiography. Anteroposterior and transverse, suprarenal and maximal infrarenal aortic diameters were measured. The ultrasonographer was blinded to the angiogram results. Of 104/106 successful scans 73 were conducted in male patients and 31 in female patients. Six males and 11 females had normal coronary arteries and no aneurysms. From 87 patients with ischaemic heart disease (IHD), eight males had aneurysms ≥3 cm diameter. Mean diameter was 4.2 cm (standard deviation [SD] 1.96, range 3–8.7 cm). Two additional males and two females had focal aortic dilatations of twice suprarenal aortic diameter yielding 14.9% and 10% incidence of aneurysmal change in scanned males and females with IHD. Average ages for patients with IHD were 62.2 years (SD 10.7, range 41–81 years) for males and 68.0 years (SD 10.6, range 47–88 years) for females. Average age for males with aneurysmal change was 68.8 years (SD 11.5, range 45–79 years). Results from this pilot study suggest that screening patients with IHD has a significantly higher yield than expected by the National Programme. These high-risk patients would benefit more than the general population from early detection and cardiovascular optimisation possibly with earlier AAA repair. Further expansion of the study would allow corroboration and qualification of these findings.
September 2009 Br J Cardiol 2009;16:237–40
Why are we so bad in primary care at initiating warfarin in atrial fibrillation patients?
John Havard

This article is an enlightened approach to reducing strokes in patients with atrial fibrillation (AF). It discusses some freely available software called ‘The Auricle’ and shows how this can easily be used to calculate the annual risk of a stroke. GPs and patients are supported in the careful decision about anticoagulation. To this end the programme has an e-consultation option to ask the opinion of a local cardiologist with the flexibility to attach an electrocardiogram (ECG), echo or clinic letter, if desired. All the details and the cardiologist’s opinion can be electronically filed in the patient’s notes to confirm that the pros and cons of warfarin were fully debated.
September 2009 Br J Cardiol 2009;16:241
The value of echocardiography in atrial fibrillation
Peadar McKeown, Kerri Toland, Ian B A Menown

A 29-year-old man was admitted with new onset atrial fibrillation (figure 1).
September 2009 Br J Cardiol 2009;16:242-5
10 Steps before you refer for: Lipids
Jonathan Morrell, Tony Wierzbicki

The impetus of national initiatives highlighting the importance of lipid modification, the sheer number of people involved, and the continuous nature of therapy, mean that lipid management has become an everyday primary care discipline.1 Most patients with dyslipidaemia can be investigated and treated effectively in primary care without referral to a specialist but, paradoxically, the increasing patient burden means an enhanced role for the specialist lipidologist as well. Patients who should be referred to a specialist lipid clinic include: Those with extreme values (primary care practitioners often feel less secure with mixed hyperlipidaemia and hypertriglyceridaemia than with pure hypercholesterolaemia). Generally, these can be defined as total cholesterol (TC) >7.5 mmol/L and/or fasting triglycerides (TG) >7.5 mmol/L. All patients with TG >20 mmol/L need to be referred given the risk of pancreatitis. Those who fail to show an effective response to treatment (whether by virtue of the type and severity of their dyslipidaemia or their intolerance of first-line agents). Those with familial dyslipidaemia (e.g. familial hypercholesterolaemia, familial combined hypercholesterolaemia and Fredrickson Types I or V [TG >20 mmol/L], or type III [TG=TC and >7 mmol/L]) should be managed by specialists as family tracking may be easier to co-ordinate, drug doses used are higher and combination therapies are more common. Special cases (such as those requiring the help of joint paediatric, nephrology, neurology, vascular surgery and HIV clinics) or those requiring special investigations such as apolipoproteins, enzyme testing, DNA genotyping, or more detailed vascular assessment.
September 2009 Br J Cardiol 2009;16:246
Catastrophic paradoxical embolism
Rohit Tandon, Naveen Kumar, Naved Aslam, Naresh K Sood, Sanjeev Mahajan, Gurpreet S Wander, Bishav Mohan

A 24-year-old male who had been bedridden for the last three weeks and was recovering from a traumatic injury to his leg presented to our echo lab for evaluation of abrupt onset dyspnoea preceded by presyncope. Clinically he was tachypnoiec, had a pulse rate of 142 beats per minute, blood pressure 100/70 mmHg, oxygen saturation at room air 97% and electrocardiogram (ECG) showing sinus tachycardia. Transthoracic echocardiography revealed dilated right heart chambers and a long multi-lobed vermicular mass in all four cardiac chambers. Trans-oesophageal echocardiography confirmed a large multi-lobed mass straddling the interatrial septum on both sides through a patent foramen ovale (figure 1). The highly mobile mass (consistent with thrombus) protruded like a worm into the aortic valve in systole through the left ventricular outflow tract (figure 2). Within three hours the patient had sudden bradycardia and cardiac arrest, probably from cerebral embolisation.
September 2009 Br J Cardiol 2009;16:247–9
Cardiac rehabilitation: are we putting our hearts into it?
Michael Pollard, Caroline Sutherland

We surveyed 510 patients to measure levels of patient satisfaction with our cardiac rehabilitation service and to compare health-related outcomes between patients who did, and did not, attend cardiac rehabilitation. Two hundred and sixty-five patients responded (52.4%). Our results showed that cardiac rehabilitation was associated with improved health behaviours, such as diet and exercise, and was popular with patients. The majority of non-attenders would have attended cardiac rehabilitation if certain features had been available. Following the survey, various improvements were made to the rehabilitation service, including a re-design of the patient literature and a designated lead consultant.
September 2009 Br J Cardiol 2009;16:250–53
Predicting adherence to phase III cardiac rehabilitation: should we be more optimistic?
Lesley A O’Brien, Morag K Thow, Danny Rafferty

Predicting uptake and adherence to cardiac rehabilitation (CR) continues to challenge providers of the service in the UK. This study included optimism with the more traditional predictors of adherence. The study included 61 eligible patients (37 men, 24 women) referred to an eight-week phase III CR programme. Socio-demographic data were collected including age, gender, diagnosis, employment, marital status and deprivation. Depression was measured using the Hospital Anxiety and Depression (HAD) scale. Dispositional optimism was measured using the Revised Life Orientation Test (LOT-R). Stages of change (SOC) for exercise were assessed. Attendance and completion of the eight-week CR programme were recorded for all patients. There was adherence to CR by 46 (75%; 27 men and 19 women) and non-adherence by 15 (25%; 10 men and 5 women). Dispositional optimism and SOC were found to be significant predictors of adherence (p=0.001 and p=0.038, respectively), with depression tending towards significance (p=0.0614). Socio-demographic variables were not significant. Greater optimism is associated with attendance at phase III CR. In addition, being in a higher stage of the SOC model is also associated with adherence. These findings can enable CR staff to identify patients at risk of failing to adhere, facilitating focused interventions to encourage adherence.
September 2009 Br J Cardiol 2009;16:254-55
Systemic amyloidosis with cardiac involvement leading to bi-atrial appendage thrombosis in sinus rhythm
Ansari Muhammad Jaffer, DaLi Feng, Jae K Oh, William D Edwards, Kyle Klarich

A 58-year-old woman presented with a five-month history of epigastric pain, lower extremity oedema and orthopnoea. On examination she had postural hypotension, raised jugular venous pressure, hepatomegaly and pitting pedal oedema. Electrocardiogram (ECG) showed sinus tachycardia, low QRS voltage and a Q-wave in precordial leads V1–V4. A coronary angiogram was normal. IgG kappa monoclonal protein was detected in her serum and urine
July 2009 Br J Cardiol 2009;16:175–80
Cardiac manifestations and sequelae of gastrointestinal disorders
Charlotte Manisty, Ynyr Hughes-Roberts, Sam Kaddoura

The relationship between cardiac and gastrointestinal disease is widely regarded as being a complex one – disorders of the two systems commonly co-exist, and the symptoms of angina pectoris are notoriously difficult to differentiate from gastro-oesophageal problems. In addition, it has commonly been observed that patients suffering with gastrointestinal disturbance suffer from cardiac symptoms whose aetiology can be attributed to their primary gut problems. Recent evidence has shown that this is a relatively common manifestation and that the incidence of these secondary cardiac complications has been underestimated in patients with gastroenterological disease. This article reviews the evidence for secondary cardiological complications of gastrointestinal disorders and discusses the potential mechanisms behind them. The three main areas outlined in the review include rhythm disturbances related to oesophageal disease, linked angina and the cardiac manifestations of inflammatory large bowel disorders.
July 2009 Br J Cardiol 2009;16:182-6
10 steps before your refer for palpitations
Andreas Wolff, Campbell Cowan

Palpitations are a common presentation in general practice(1) and a frequent reason for cardiology referrals. This symptom often causes considerable distress and anxiety for the patient(2) and can evoke a similar feeling in the consulted healthcare professional. However, palpitations are often benign.(3) Less than half of patients with palpitations suffer from an arrhythmia and not every identified arrhythmia is of clinical or prognostic significance.(4 )There is also a high incidence of anxiety disorders among patients presenting with palpitations.(5) The skill lies in identifying patients with a significant heart rhythm abnormality who can be either helped by treatment or are at risk of adverse outcome. This can be achieved in primary care by taking a careful history and simple investigations.(5) The provision of services for patients with arrhythmic illness has lagged behind those who suffer from coronary heart disease (CHD). This has been recognised by the addition of Chapter 8 to the National Service Framework for CHD.(6) Timely access to appropriate clinicians and patient support are among the quality requirements, which have been much welcomed by patients.
July 2009 Br J Cardiol 2009;16:187–91
Follow your heart: optimal care after a heart attack – a guide for you and your patients
Fran Sivers, Alan Begg, David Milne, Jonathan Morrell, Dermot Neely, Michael Norton, Michaela Nuttall, Malcolm Walker, Brian Ellis, Cathy Ratcliffe, Andrew Thomas, Ruth Bosworth, Seleen Ong, on behalf of the Follow Your Heart Steering Group

Considerable variation exists in adherence to and implementation of post-myocardial infarction (post-MI) clinical guidelines in the UK. The Follow Your Heart Steering Group has consolidated existing clinical evidence and published guidance into a consensus of succinct recommendations for optimal post-MI management, which includes separate healthcare professional and patient-focused components. This guidance should help encourage two-way dialogues between patients and healthcare professionals, reduce practice variation, raise standards of care, maximise healthcare resource utilisation and improve outcomes in post-MI patients. It is our intention to develop and widely disseminate a simple algorithm for healthcare professionals and for patients that summarises the guidance.
July 2009 Br J Cardiol 2009;16:192–3
Coronary artery disease – need for better terminology
George Thomas

In the case of coronary artery disease the glut of diagnostic terms like Q-wave infarction, non-Q infarction, ST elevation infarction, non-ST elevation infarction, intermediate syndrome, unstable angina, stable angina, silent ischaemia, and exertional angina do not reflect the present day realities and are neither rational nor systematic. The term ‘acute coronary syndrome’ is too vague. A diagnostic term should be based on the cause rather than the effects. The present terms are symptom and effect based. These were relevant when there was no effective treatment. With the availability of powerful treatments these terms have become outdated. Terminology relating to the present day realities is required. In this paper I propose a system of terminology based on the assumed pathology.
July 2009 Br J Cardiol 2009;16:194–6
Achieving preferred place of death – is it possible for patients with chronic heart failure?
Miriam J Johnson, Sharon Parsons, Janet Raw, Anne Williams, Andrew Daley

Most people do not wish to die in hospital, yet most people do. Patients with chronic heart failure (CHF) appear to be particularly disadvantaged in this regard, partly because it can be difficult to recognise when the issue should be broached. This review by two integrated cardiology–palliative care services of 235 CHF deaths, shows that only about a third of patients died in an acute hospital bed. End-of-life discussions were possible, with the majority of patients given the opportunity to express a preferred place of dying achieving their wish.
July 2009 Br J Cardiol 2009;16:197–8
An unusual ‘heart attack’ – Takotsubo cardiomyopathy
Jerzy Wojciuk, Ravish Katira, Ranjit S More, Roger W Bury

The authors describe a case of Takotsubo-like syndrome in a 59-year-old Caucasian woman.
July 2009 Br J Cardiol 2009;16:199–200
Evaluation of left ventricular non-compaction using multi-detector computed tomography
Edward T D Hoey, Nicholas J Screaton, Bobby S K Agrawal, Matthew J Daniels, Andrew A Grace, Deepa Gopalan

A 37-year-old man presented with palpitations and recurrent episodes of pre-syncope. He had a past medical history of atrial septal defect (ASD) repair aged seven.
May 2009 Br J Cardiol 2009;16:132–4
Nurse specialist-led management of acute coronary syndromes
Khaled Alfakih, Martin Melville, Jacqui Nainby, Jamie Waterall, Kevin Walters, John Walsh, Alun Harcombe

The management of acute coronary syndromes (ACS) has changed greatly over recent years. Trial evidence encouraged clinicians to consider early invasive management in high-risk patients and this has created a large clinical burden. We instituted a comprehensive system of nurse-led diagnosis and management of ACS. In-patients are seen by a cardiac outreach nursing team and depending on their risk profile may be managed in a designated acute cardiac unit (ACU) by cardiologists. We also piloted an ‘ACS clinic’ where patients with higher risk are seen within two weeks of discharge. We conducted audits to assess the impact of these new services. A total of 158 consecutive patients from ACU with unstable angina or non-ST elevation myocardial infarction (NSTEMI) were identified. The in-patient coronary angiography rate was 48%, percutaneous coronary intervention (PCI) rate 15% and coronary artery bypass graft (CABG) rate 4%. The six-month re-admission rate was 28.5%, of whom 44.4% were within one month of discharge. In-patient coronary angiography almost halved the rate of re-admission (20.0% vs. 36.6%; p=0.026). We also audited the first 12 months of the ACS clinic. The six-month re-admission rate was 14.2%, a significant reduction compared with the first audit (p=0.0002). In conclusion, the strategy of nurse-led identification and follow-up of ACS patients promotes effective use of resources and reduces re-admissions.
May 2009 Br J Cardiol 2009;16:135
Incidental radial endarterectomy
Mohaned Egred, Raphael A Perry

The transradial approach is increasingly used in a wide range of percutaneous coronary interventions (PCIs) with few reported complications. It is established as a safe procedure with improved patient comfort and early mobilisation.1-3 This has translated into early discharge with reduced procedural cost leading to out-patient day-case PCI.4,5 However, with this increasing use, unusual and new complications will be recognised.
May 2009 Br J Cardiol 2009;16:137–40
Early ambulation of patients post-angiography with femoral puncture
Olga Gillane, Michael Pollard

Research has shown that, following angiogram with femoral puncture, prolonged bed rest increases patient discomfort during recovery. This audit aimed to measure the effects of reducing the period of immobilisation from the local standard of four hours to only two hours. Almost 500 consecutive patients were selected for early ambulation at two hours post-angiogram. Overall, 86.8% of patients suffered no vascular complications. In addition to the beneficial effects on patient comfort, earlier ambulation will enable cardiology units to treat more patients, thereby maximising efficiency and income generation.
May 2009 Br J Cardiol 2009;16:147–150
The prognostic value of raised pre-operative cardiac troponin I in major vascular surgery
Gavin J Bryce, Christopher J Payne, Simon C Gibson, David B Kingsmore, Dominique S Byrne

Vascular surgery is associated with a substantial risk of cardiovascular events and death. Cardiac troponin I (cTnI) is a contractile protein that is a highly sensitive and specific marker of myocardial necrosis. This case series examines the clinical course of 10 patients who had an asymptomatic pre-operative elevation in cTnI and underwent a vascular surgical procedure. A prospective, two-year, observational, single-centre cohort study of all patients undergoing a vascular procedure with an expected cardiac event rate of >5% was performed. Pre-operative cTnI was carried out (cTnI >0.02 ng/ml positive). Post-operative screening for cardiac events at post-operative days two and five was performed. Two-hundred and thirteen patients were recruited, of whom 11 (5.2%) had an asymptomatic elevated pre-operative cTnI. Ten patients in whom the pre-operative cTnI was not known prior to surgery, or in whom a procedure could not be delayed proceeded with the operation. One patient had surgery deferred. Four patients suffered a post-operative cardiac event and five died. The outcome in this case series was poor with death in 50% of those taken to theatre and cardiac events in 40%. An elevated pre-operative cTnI in an otherwise asymptomatic patient identifies a very high-risk group of patients.
May 2009 Br J Cardiol 2009;16:142–6
Post-MI clinical guidelines: variation in availability, development, content and implementation across the UK
Seleen Ong, David Milne, Jonathan Morrell, on behalf of the Follow Your Heart Steering Committee

Clinical guidelines are vital to improving patient outcomes by helping reduce practice variation, raising care standards, improving efficiency and maximising resource utilisation. To investigate the implementation/local adaptation of national guidance and approaches to post-myocardial infarction (MI) care across the UK, an assessment of the availability and implementation of local post-MI guidelines in England among primary care trusts (PCTs) and cardiac networks (CNs) was conducted. Secondly, a survey of UK GPs and nurses (n=1,003) was performed to establish awareness of guidelines and to investigate whether there are regional variations in the management of post-MI patients. Fifteen post-MI clinical guidelines were obtained (PCTs – 8; CNs – 7) and analysed according to the following topics: lifestyle modifications, cardiac rehabilitation, therapeutic intervention, therapeutic targets and communication between primary and secondary care. Considerable regional variation in the recommendations were found – particularly with regard to therapeutic interventions and targets – with differing targets for blood pressure and cholesterol management. This was mirrored in the survey results, which also showed significant inconsistencies in clinical practice as reported by UK healthcare practitioners. In conclusion, little consistency in the availability and content of local post-MI clinical guidelines, coupled with disparities in national guidelines, suggest the need for national post-MI guidance, built on existing evidence, endorsed by clinicians and patients, which will promote optimal care and reduce practice variation.
May 2009 Br J Cardiol 2009;16:151–2
Ivabradine for inappropriate sinus tachycardia
David Wilson, Beresford Crook

A patient with inappropriate tachycardia is described who failed to respond to beta blockers or calcium channel blockade but had clinical improvement with ivabradine. The heart rate slowing with this drug was illustrated by the change in the R–R interval histogram.
March 2009 Br J Cardiol 2009;16:73-77
Long-term benefits of cardiac rehabilitation: a five-year follow-up of community-based phase 4 programmes
Katherine A Willmer, Mandy Waite

It is well recognised that phase 3 cardiac rehabilitation is beneficial, reducing both mortality and morbidity following acute myocardial infarction. The role of ongoing phase 4 cardiac rehabilitation is less clear. This study was designed to assess the effectiveness of phase 4 cardiac rehabilitation in acute myocardial infarction. Following acute myocardial infarction, 143 patients who had completed phase 3 cardiac rehabilitation were followed up. Analysis was divided into three groups: those who took up phase 4 rehabilitation, those offered who declined and those not offered phase 4 rehabilitation because it was not available locally. Risk factor profile, self-reported exercise and quality-of-life scores using the short form (SF)-36 were assessed in all patients. Body mass index (BMI) shows no overall change in the ‘accepted’ group, but shows a significant increase between pre and five-year levels in the ‘declined’ group (p=0.024) and in the ‘not offered’ group (p=0.014). All groups showed an increase of SF-36 scores following phase 3, which showed a trend towards significance. Both the ‘accepted’ and ‘not offered’ groups maintained this improvement, while the ‘declined’ group returned to baseline (p=0.05 vs. ‘accepted’ and p=0.03 vs. ‘not offered’). All groups had similar exercise levels initially and all showed significant improvements after phase 3 with some deterioration out to five years. This decline in exercise was significant in the ‘declined’ group (p=0.029) and shows a trend in the ‘not offered’ group (p=0.057). This small single-centre study suggests that there are observable benefits in participating in long-term phase 4 cardiac rehabilitation. Those who decline phase 4 cardiac rehabilitation clearly do less well. Whether the benefits seen can be attributed directly to phase 4 cardiac rehabilitation would require a different study design to address this issue.
March 2009 Br J Cardiol 2009;16:80-84
10 steps before you refer for chest pain
Sudhakar Allamsetty, Sreekala Seepana, Kathryn E Griffith

Chest pain is a common presentation in general practice. Each year about 1% of the UK population visit their GP with chest pain.1 The average GP will see, on average, four new cases of angina each year.2 The Euro heart survey of newly diagnosed stable angina patients showed that the incidence of death and myocardial infarction (MI) was 2.3/100 patient-years. This is increased in patients with a previous MI, short history, more severe symptoms and with heart failure or other co-morbidities, such as diabetes.3 The recognition of these patients as at high risk for cardiovascular events has led to the improvement of diagnosis and management of angina. Rapid access chest pain clinics have been developed to allow quick assessment of patients with new onset angina as part of a National Service Framework for coronary artery disease.
March 2009 Br J Cardiol 2009;16:85-89
Current concepts of anthracycline cardiotoxicity: pathogenesis, diagnosis and prevention
Brad Pfeffer, Constantine Tziros, Richard J Katz

Anthracyclines are commonly used antineoplastic drugs. However, their clinical utility is tempered by a dose-dependent risk of cardiotoxicity and congestive heart failure. Current preventive measures focus on dose reduction, use of less cardiotoxic anthracycline analogues and prophylactic use of dexrazoxane. Recent research has focused on early monitoring and risk stratification to identify patients that are ‘at risk’ for cardiotoxicity, using biochemical markers and the prophylactic use of novel cardioprotectants. This article reviews the clinical course, pathogenesis, cardiac monitoring and new concepts in diagnosing and preventing anthracycline cardiotoxicity.
March 2009 Br J Cardiol 2009;16:90–7
Efficacy and safety profile of co-administered ER niacin/laropiprant and simvastatin in dyslipidaemia
Gilbert Gleim, Christie M Ballantyne, Nancy Liu, Sally Thompson-Bell, Christine McCrary Sisk, Richard C Pasternak, Yale Mitchel, John F Paolini

Co-administered niacin and statin may offer additional lipid management; however, niacin is underutilised due to flushing, mediated primarily by prostaglandin D2 (PGD2). A combination tablet containing 1 g extended-release niacin and 20 mg laropiprant (ERN/LRPT), a PGD2-receptor (DP1) antagonist, offers improved tolerability. To assess the efficacy and safety of ERN/LRPT + simvastatin versus ERN/LRPT and simvastatin alone in dyslipidaemic patients, in this 12-week study, 1,398 patients were randomised equally to ERN/LRPT 1 g/20 mg, simvastatin (10, 20 or 40 mg), or ERN/LRPT 1 g/20 mg + simvastatin (10, 20 or 40 mg) once-daily for four weeks. At week five, doses were doubled in all groups except simvastatin 40 mg (unchanged) and ERN/LRPT 1 g/20 mg + simvastatin 40 mg (switched to ERN/LRPT 2 g/40 mg + simvastatin 40 mg). ERN/LRPT + simvastatin (pooled across simvastatin doses) significantly improved key lipid parameters versus ERN/LRPT and pooled simvastatin: mean percentage changes from baseline to week 12 for low-density lipoprotein cholesterol were –47.9%, –17.0% and –37.0%, respectively, and for high-density lipoprotein cholesterol were 27.5%, 23.4% and 6.0%, respectively. ERN/LRPT + simvastatin was generally well tolerated, with a low incidence of serious treatment-related adverse experiences (0.2%, 0.5% and 0.2% for ERN/LRPT + simvastatin, ERN/LRPT and simvastatin, respectively). In conclusion, ERN/LRPT + simvastatin significantly improved the lipid profile compared with ERN/LRPT and simvastatin alone and was generally well tolerated in dyslipidaemic patients.
March 2009 Br J Cardiol 2009;16:98–101
Cardiac disease in pregnancy: a District General Hospital perspective
Edward J Langford, Manoj K Makharia, Kate S Langford

Heart disease is the leading cause of death in pregnancy. Although women with high-risk cardiac conditions can be identified, the majority of deaths occur without such pre-existing severe cardiac disease. Coronary artery disease is an increasing cause. Previous reports on heart disease in pregnancy have focused on tertiary-centre and non-UK populations. We report a UK District General Hospital (DGH) experience. We recorded all pregnant women referred to a dedicated DGH cardiology service in Bromley between August 2004 and August 2007. One hundred and three women were referred, including 37 with murmurs or known valve disease, 31 palpitations or arrhythmias, 13 congenital heart disease and eight hypertension. Of the women presenting with a murmur, only one, a recent immigrant, had a significant cardiac condition requiring treatment. Three women with arrhythmias required admission but none were life-threatening. Four women required admission for heart failure, two with peri-partum cardiomyopathy and two with previous hypertension. Only two women were referred with chest pain, neither had ischaemia. Tertiary referral was required in cases of heart failure, an increased risk of aortic rupture or severe mitral stenosis, but all other women were managed safely in a DGH. Seventy per cent of women only needed one clinic visit. In conclusion, the majority of pregnant women referred to a DGH cardiology service are in the previously defined low-risk group. Cardiac symptoms or signs in UK-born pregnant women without known heart disease are unlikely to represent high-risk cardiac disease but recent immigrants may have significant undiagnosed disease. Chronic hypertension is a risk factor even if controlled at the start of pregnancy. Ischaemia is an increasing problem.
March 2009 Br J Cardiol 2009;16:102–4
Are angiotensin-blocking drugs being used in adequate doses?
Sunreet K Randhawa, Harleen K Dhillon, Tarvinder S Dhanjal, D Gareth Beevers

Angiotensin-receptor blocking drugs have been shown to be an effective therapeutic strategy in a number of cardiovascular diseases. Many randomised controlled trials have demonstrated optimal doses of these drugs. We therefore investigated the doses of angiotensin-converting enzyme inhibitors or angiotensin-receptor blockers in patients admitted to hospital. We found from a total of 60 consecutive patients, only 38% (n=23) were on the top recommended dose and the average daily dose was 63.1±4.5% of the recommended dose. This study confirms that a significant number of patients are receiving suboptimal doses of angiotensin-blocking drugs and this under-dosing is likely to result in a failure to achieve the maximal therapeutic benefit.
January 2009 Br J Cardiol 2009;16:21–8
Emergence of the rapid access blackout clinic
Ibrahim Ali, Trudie Lobban, Richard Sutton, Alex Everitt, Darrel P Francis

Blackout is a common, alarming symptom occurring across patients of all ages, and can create enormous psychological and social distress. In this review, we describe a new clinical approach that improves healthcare delivery to patients suffering blackouts.
January 2009 Br J Cardiol 2009;16:30–35
10 steps before you refer for heart failure
Ann Marie Johnson, Paul Brooksby

Congestive heart failure (CHF) is an increasingly widespread condition, the prognosis for moderate and severe heart failure is almost identical to colorectal cancer1 and worse than breast2or prostate cancer.3 CHF has an overall population prevalence of approximately 1–3% rising to approximately 10% in the very elderly CHF accounts for about 5% of all medical admissions and approximately 2% of total healthcare expenditure.4 Nearly one million new cases are diagnosed annually worldwide, making it the most rapidly growing cardiovascular disorder. The consequences of heart failure for primary care are profound. CHF has been reported to be second only to hypertension as a cardiovascular reason for a surgery appointment.5Despite improvements in medical management, undertreatment is common, many patients with CHF still do not receive treatment optimised according to current guidelines.4,6 The introduction of the 2009/10 heart failure Quality Outcomes Framework (QOF) additions will bring financial incentives for the prescribing of beta blockers for patients with a diagnosis of heart failure. This will apply to all diagnosed heart failure patients. There are, however, no additional QOF points for optimising medication or maximum tolerated levels, therefore, patient care will rely on good practice and receiving treatment according to current guidelines. The prevalence of heart failure nationally in QOF is just over 1%. Because of the increase in survival after acute myocardial infarction and ageing of the population, the number of patients with heart failure will increase rapidly in most industrialised countries. Heart failure will continue to be a challenge to healthcare. The profile of heart failure management has been raised with the publication of the Coronary Heart Disease (CHD) National Service Framework (NSF) Chapter 6 in 20007 and the National Institute for Health and Clinical Excellence (NICE) Heart Failure Clinical Guideline 2003.8 The heart failure publications have supported the development of community heart failure services, and heart failure specialist nurse roles. The development of the General Practitioner with Special Interest (GPSI) in cardiology qualification and the accreditation in community echocardiography in 2004 has enabled the development of community heart failure services. The training and development of the workforce in primary care has led to improvements in the treatment and management of heart failure patients. A referral to a community specialist heart failure service or secondary care will still be relevant in certain instances, however, the 10 steps will assist in the decision to continue the management in primary care or refer for expert advice and a future management plan.
January 2009 Br J Cardiol 2009;16:36-41
Amyloid heart disease
Simon Dubrey

The amyloidoses comprise a collection of disorders in which proteins, some native and some mutated, are deposited in tissues. These proteins self-assemble themselves to form an ordered fibrillar matrix termed amyloid. Currently, more than 20 different proteins have been identified, the most common with as many as 100 different mutations per protein. Despite these figures, the conditions that arise clinically are not that common. This undoubtedly results in a number of such individuals not being identified, or typically only when it is too late to effect a cure. This article describes the features, diagnosis and treatments for the different types of amyloid that affect the heart.
January 2009 Br J Cardiol 2009;16:43
Multi-modality imaging of myocardial infarction
Edward D Nicol, James Stirrup, Jonathan C Lyne

A 52-year-old man presented to the emergency department with increasingly frequent anginal chest pain. He had had an anterior ST elevation myocardial infarction two years previously, for which he received thrombolysis. He was an ex-smoker, hypercholestrolaemic and had a family history of ischaemic heart disease. During stress electrocardiography, he developed chest pain at nine minutes of a standard Bruce protocol, but no significant ST changes.
January 2009 Br J Cardiol 2009;16:44-46
A three-dimensional anatomy model of the heart organ using a gloved hand
Hope Gangata

Teaching and learning the three-dimensional anatomy of the heart can be challenging. The use of the hand to model structures in the heart has proven useful. In this article a more comprehensive model of the heart using a gloved hand is proposed.
January 2009 Br J Cardiol 2009;16:47
Otner’s syndrome: the controversial cardiovocal syndrome
Hussain Al-Sardar

The cardiovocal syndrome was first described by Otner, a Viennese physician, in 1897.1 It refers to a clinical syndrome of hoarseness due to dysfunction of the left recurrent laryngeal nerve, caused by cardiac diseases. Here, we describe a case of Otner’s syndrome following the second revision of mitral valve replacement.
November 2008 Br J Cardiol 2008;15:302–5
10 steps before you refer for atrial fibrillation
Rosie Heath, Gregory Y H Lip

Atrial fibrillation (AF) is a relatively common condition. The national prevalence for England on the latest quality and outcomes framework data is 1.3% and as many as 10% of patients aged over 75 may be in AF. On average, all of us have a 20–25% lifetime risk of developing AF. An average GP will have 16–20 cases on their personal list and can expect to diagnose three new cases per annum. However, it is recognised that many cases of AF go undiagnosed and opportunistic screening for AF has been recommended. Of note, AF is responsible for 45% of embolic strokes. With the increasing emphasis on AF from Chapter 8 of the National Service Framework for Coronary Heart Disease (NSF-CHD), the National Stroke Strategy1 and inclusion of AF in the Quality and Outcomes Framework – as well as publication of the National Institute for Health and Clinical Excellence (NICE) guidelines for AF management – it is important for GPs to diagnose, treat and refer AF patients correctly. There are three main areas to consider in AF patients: first, the diagnosis and treatment of any underlying co-morbid condition; second, symptom control by either a rate- or rhythm-control strategy; and third, the reduction of the accompanying risk of stroke and thromboembolism by appropriate prescription of antithrombotic therapy. Many straightforward cases of AF can be satisfactorily managed entirely in primary care, using the following structured approach.
November 2008 Br J Cardiol 2008;15:307-11
South East London Cardiac Prescribing Forum: working to improve clopidogrel prescribing across the South East London sector
Helen Williams, Rachel Hughes, Lucy Simkins, Katie Hatton, Michael Currie, Holly Chong, Victoria Hill, Christopher Boddy, Sara Nelson, Claire Foreman on behalf of the Cardiac Prescribing Forum of the South East London Cardiac and Stroke Network (SELCSN)

National guidance recommends specific durations for clopidogrel and aspirin dual therapy post ST elevation myocardial infarction (STEMI), non-ST elevation myocardial infarction (NSTEMI) and following percutaneous coronary intervention (PCI). Primary care clinicians highlighted that patients were frequently discharged from acute trusts without any communication as to the indication for or intended duration of clopidogrel therapy. An initial audit across four of the six acute trusts demonstrated significant variation in the use of clopidogrel and aspirin dual therapy across the sector, with 26% of discharge prescriptions giving no clear indication for therapy and 30% of discharge prescriptions giving no indication of the intended duration of therapy. The South East London Cardiac and Stroke Network (SELCSN) cardiac prescribing forum, with input from consultant cardiologists, GPs, pharmacists and others, developed and implemented a consensus guideline for the prescribing of clopidogrel across the sector. In addition, it was agreed that acute trust pharmacy departments would not dispense clopidogrel for discharge unless the duration was clearly documented on the discharge prescription. Re-audit demonstrated an increase in the proportion of discharge prescriptions with an indication for and duration of clopidogrel therapy: 92.5% and 85%, respectively. Failure to implement the SELCSN guidance in one trust had a significant impact on the overall results; however, four of the six trusts managed to achieve over 95% compliance in terms of communicating a clear indication for and duration of clopidogrel therapy. In addition, the number of different regimens in use was lower during the re-audit period indicating a move to more consistent prescribing of clopidogrel across the sector, although there remains significant variation between trusts. Next steps for the SELCSN are to address clopidogrel prescribing in the trust with poor outcomes in the audit to ensure full implementation of the local guidance, development of a tool to audit prescribing of clopidogrel in primary care to assess appropriate cessation of dual therapy and re-audit of acute trust discharge communication to ensure the good practice which has been implemented is maintained in the long term.
November 2008 Br J Cardiol 2008;15:312-15
Standby coronary angiography in elective patients with chest pain and the 18-week target: one solution to a national problem?
Daniel B McKenzie, Nicholas G Turner, Vikram Khanna, Runa Rahmat, Nick Curzen

In June 2004 the Department of Health made a commitment to reduce waiting times from GP referral to hospital treatment to less than 18 weeks by 2008. Patients with chest pain are often now seen within two weeks thanks to the success of rapid-access chest pain clinics. Around 10–25% of these patients are referred for diagnostic coronary angiography (CAG) and of these, about 30% require percutaneous coronary intervention (PCI) to treat coronary stenoses. Conventionally, UK practice has been that such patients occupy two waiting lists: one for the CAG, which is often performed by a non-interventional cardiologist, and one for the PCI. This pathway makes achieving the 18-week target challenging. We introduced a new care pathway whereby all elective chest pain patients referred for CAG to one of the interventional cardiologists were listed for a standby coronary angiogram (SBCA), during which if PCI was indicated then it was performed immediately. We present the results of an audit of 102 consecutive patients since this pathway was introduced that demonstrates one method of achieving the 18-week target for this group of patients. This can now be further refined by aiming to achieve a higher proportion of day-case PCI cases.
November 2008 Br J Cardiol 2008;15:316-21
Vascular calcification: mechanisms and management
Smeeta Sinha, Helen Eddington, Philip A Kalra

Chronic kidney disease (CKD) is thought to affect approximately one in 10 people. Patients with CKD have significantly increased cardiovascular morbidity and mortality in comparison with the general population. This is thought to occur from a combination of increased atherosclerotic disease and medial calcification of arterial walls. Vascular calcification (VC) is recognised as an active, cell-mediated process with similarities to osteogenesis. Numerous systemic and local factors have been identified as inhibitors of calcification including fetuin-A, matrix Gla protein and pyrophosphate. There is also increasing evidence that increased serum phosphorus, serum calcium x phosphorus product, and/or calcium load is associated with increased VC. Current treatment strategies focus on the correction of markers of mineral metabolism bone disease such as phosphate, calcium, parathyroid hormone and vitamin D. The use of agents such as bisphosphonates and cinacalcet show promise, but further data are awaited before their widespread use as a treatment for VC can be advocated. Imaging techniques currently used to assess VC are also discussed. Research into the mechanisms underlying VC are still being investigated and further insight into these mechanisms will lead to the development of therapeutic agents, which could improve cardiovascular outcomes in patients.
November 2008 Br J Cardiol 2008;15: 322–5
Co-morbid psychiatric disorders among subjects in stable state of heart failure in a West African teaching hospital
Amam C Mbakwem, Olatunji F Aina

Heart failure (HF) is an important cause of morbidity and mortality in the general hospital setting worldwide. The paucity of data on psychiatric co-morbidity in Nigeria necessitated this study. This study was carried out among adults in stable state of HF at the cardiology clinic of Lagos University Teaching Hospital (LUTH) with sex- and age-matched controls. Fifty-eight subjects were studied, made up of 27 (46.6%) males and 31 (53.4%) females. The mean age was 51.2±13.8 years. There were 44 age- and sex-matched controls with mean age of 50.1±13.6 years. Thirty-four of the subjects (58.6%) had General Health Questionnaire (GHQ) scores of ≥2 (cut-off score); out of which 14 (24.4%) were confirmed to have psychiatric disorders. One subject with GHQ score <2 also had a psychiatric diagnosis giving a sensitivity of 0.93 and specificity of 0.54 for GHQ-12 in this study. Thus, a total of 15 (25.9%) had psychiatric diagnoses which included: depression 7 (12.0%); generalised anxiety 6 (10.3%); paranoid schizophrenia 1 (1.7%), and somatisation disorder 1 (1.7%). It is concluded that clinically significant psychiatric co-morbidities exist among subjects with HF. The need for ‘liaison’ psychiatric services in the cardiology clinic is emphasised.
November 2008 Br J Cardiol 2008;15:326–8
The dark side of the drug-eluting stent: stent thrombosis with cessation of dual antiplatelet therapy
Mohaned Egred, Mohammed Andron, Raphael A Perry

The use of drug-eluting stents (DES) has increased exponentially in recent years. There appears to be little difference in short- to medium-term safety compared with bare-metal stenting (BMS). Coronary thrombosis after stent implantation is well recognised, resulting in acute myocardial infarction and not uncommonly in death. Late (>6 months) stent thrombosis is rare with BMS, but there is a concern that DES might be susceptible to thrombosis due to delayed endothelialisation. The prolonged use of dual antiplatelet therapy (APT) with aspirin plus a thienopyridine (e.g. clopidogrel) is recommended. The premature discontinuation of APT in patients with DES without consultation with the treating cardiologist can result in stent thrombosis and adverse outcome.
September 2008 Br J Cardiol 2008;15:244–47
Percutaneous coronary angioplasty in a district general hospital: safe and effective – the Bournemouth model
Dominic Kelly, Manas Sinha, Rosie Swallow, Terry Levy, Johannes Radvan, Adrian Rozkovec, Suneel Talwar

Recent studies have suggested that the safety, efficacy and feasibility of percutaneous coronary intervention (PCI) in hospitals without on-site surgical cover is equivalent to those with these facilities. In addition, recent UK figures suggest that PCI growth is in the region of 15% per year with a corresponding fall in coronary artery bypass grafts (CABGs) hence the ratio of PCI to CABG is increasing. In the UK 35% of PCI centres are without on-site surgical cover, however, these centres represent only 18% of total PCI procedures. The Dorset Heart Centre opened in April 2005 the nearest surgical centre being approximately 28 miles in distance. In addition to elective PCI, our centre provides a 9-to-5 Monday-to-Friday primary and rescue PCI service for the Dorset area. We compared the safety and efficacy of our newly opened non-surgical PCI centre with outcomes predicted using the North West Quality Improvement Programme (NWQIP) multi-variate prediction model to assess the risk of major adverse cardiac and cerebral events (MACCE) in patients undergoing PCI. Between opening and August 2006 we performed 1,454 PCIs. Our overall success rate was 1,363 (94%). Using the NWQIP multi-variate prediction model, the calculated MACCE estimate rate was 2.05%. The actual MACCE rate was 0.55%. We conclude that at our relatively new non-surgical centre we are able to provide an effective and high-volume PCI service to the Dorset region with MACCE rates below that expected for our patient population.
September 2008 Br J Cardiol 2008;15:249–52
The patient’s experience of heart palpitations and the cardiology consultation: an exploratory study
Jackie Gordon, Richard Vincent, Richard Bowskill

An exploratory study with individual interviews before seeing the cardiologist, one week after the appointment, and at three-month follow-up was conducted to explore how participants’ perception and experience of heart palpitations are affected by seeing a cardiologist. Eleven of 20 participants cited anxiety as a possible cause of palpitations. A similar number were worried about their heart. After seeing the cardiologist, 7/20 participants thought something serious may have been missed, only one out of seven of whom had a clinically significant arrhythmia. It was reported that cardiologists did not address the role of psychological factors. Seven of the 20 participants still had heart-related health concerns at three months. We conclude that many participants with palpitations without demonstrable cardiac pathology continued to experience high levels of health concern after seeing the cardiologist; this persisted at three months. The lack of resolution of the problem for these patients lay in not receiving a diagnosis or explanation. Participants reported that cardiologists did not address the possibility that psychological factors (particularly anxiety) could be relevant to the aetiology and management of palpitations. We suggest cardiologists should routinely address anxiety as a potential contributor to the cause of their patients’ symptoms.
September 2008 Br J Cardiol 2008;15:254-7
10 steps before you refer for: hypertension
Terry McCormack, Francesco P Cappuccio

The majority of patients with hypertension are treated in primary care and well controlled. Typically, a practice will achieve about 80% control as judged against the Quality Outcome Framework (QOF). The QOF only requires a practice to reach a target of 70%. A practice will need to control the blood pressure of about 18% of their patients and therefore about 3.5% of the practice population will not be controlled. Too many to refer to secondary care and therefore the practice needs a strategy to try and improve control in-house and to identify those in greatest need of referral.1
September 2008 Br J Cardiol 2008;15:258-60
Protecting the heart during myocardial revascularisation
Joo-Yeung Chun, Martin Euler, John Pepper

Much effort has been expended assessing the relative merits of percutaneous coronary intervention (PCI) and coronary artery bypass graft (CAGB) surgery. Much less energy has been directed towards understanding the potential of these two interventions for causing additional myocardial damage during the procedure and the means to avoid this injury. This review examines the impact of myocardial injury in elective PCI and CABG, principles of myocardial protection, and their efficacy in current coronary revascularisation. The objective of every coronary revascularisation should be a technically perfect result without producing myocardial damage. A patent graft that perfuses an area of myocardium with numerous pockets of myocyte necrosis serves no useful purpose.
September 2008 Br J Cardiol 2008;15:261-5
Renal and cardiac arterial disease: parallels and pitfalls
Timothy Bonnici, David Goldsmith

Renal artery stenosis is a condition that has significant effects on the progression and outcomes of co-existent cardiac disease. The most important cause of renal artery stenosis is atherosclerotic renovascular disease (ARVD). As the drugs and techniques used to manage ARVD are similar to those used to treat coronary artery disease, cardiologists are increasingly becoming involved in its management. However, while there are similarities, there are also significant differences in the management of ARVD and coronary artery disease. There are also many differing opinions on the best management. This review maps the minefield of conflicting evidence and gives clear, pragmatic guidelines regarding the management of patients with cardiorenal disease.
September 2008 Br J Cardiol 2008;15:266–8
Radiation dose from cardiac investigations: a survey of cardiac trainees and specialists
Edward D Nicol, Eliana Reyes, Katherine Stanbridge, Kate Latus, Claire Robinson, Michael B Rubens, S Richard Underwood

To identify the knowledge of ionising radiation doses and radiation-related risk in common cardiac procedures among cardiology trainees, cardiologists and general practitioners with a specialist interest in cardiology, a face-to-face questionnaire survey of 47 cardiac specialists, both regular referrers and practitioners of radiation-based procedures, was conducted at the British Cardiovascular Society Annual Conference 2006. Of the 47 medical professionals surveyed, 21 (45%) provided the correct radiation dose for at least one imaging procedure. Most reported doses were below the lower limit of the reference range: the median (interquartile range) radiation dose reported by the respondents was 2 mSv (0.4 to 10 mSv) for coronary angiography (CA) and 6 mSv (1 to 15.8 mSv) for percutaneous coronary intervention (PCI); 2 mSv (0.5 to 15 mSv) and 6 mSv (1 to 20 mSv) for myocardial perfusion scintigraphy (MPS) and computed tomographic angiography (CTA), respectively. A risk of malignancy from ionising radiation exposure of one in 10,000 for CA (actual risk 1:5,000) and of one in 5,000 for MPS and CTA (actual risk 1:1,000) was reported by the majority of respondents. We conclude that there is significant underestimation of both dose and radiation-related risk to patients. Patients are unable to make informed decisions when consenting for these common procedures, as clinical staff are unaware of the correct radiation dose and associated risk, and therefore are unable to advise patients properly.
September 2008 Br J Cardiol 2008;15:269-70
Occlusion of left main coronary artery diagnosed by computed tomography of the chest
Scot Garg, Christos Bourantas, Simon Thackray, Farqad Alamgir

A 55-year-old smoker with no significant past medical history was admitted following an episode of dyspnoea and intrascapular pain. Clinical examination was normal. His blood pressure (BP) was 80/40 mmHg and his electrocardiogram (ECG) showed a sinus tachycardia and right bundle branch block.
September 2008 Br J Cardiol 2008;15:271–2
Microscopic polyangiitis presenting as a pericardial effusion
Sajid Siddiqi, Sarah Rae, John Cooper

Microscopic polyangiitis is a systematic necrotising vasculitis that affects small vessels without granulomata. Typically the most common manifestation is renal involvement. We report an unusual presentation of microscopic polyangiitis in a young male.
July 2008 Br J Cardiol 2008;15:191–4
New data highlight burden of sub-optimal management of angina
BJCardio editorial team

New data gathered via a survey undertaken on behalf of the British Cardiac Patients Association (BCPA) confirm not only that angina itself has an adverse impact on lifestyle, but that the side effects associated with some of the currently prescribed therapies for angina may be exacerbating the situation for patients.
July 2008 Br J Cardiol 2008;15:199-204–6
Cost-consequences analysis of natriuretic peptide assays to refute symptomatic heart failure in primary care
Michael A Scott, Christopher P Price, Martin R Cowie, Martin J Buxton

In primary care, the significant burden of heart failure is exacerbated by problematic, inaccurate diagnosis that may produce inefficient triaging of patients to echocardiography. UK guidelines recommend using natriuretic peptides in the diagnostic pathway. The costs and consequences of providing a definitive diagnosis for symptomatic heart failure have not been established for peptide testing in primary care. We provide a cost-consequence analysis to compare alternative diagnostic strategies for symptomatic heart failure patients presenting to their GP. Health economic evaluation using decision-tree modelling taking a cohort of patients presenting in primary care with symptomatic heart failure to a definitive diagnosis was performed. The model compared a diagnostic strategy using electrocardiograms (ECGs) interpreted by consultants with the use of B-type natriuretic peptide (BNP) assays. The base-case used data from the UK Natriuretic Peptide (UKNP) study, which used a ‘point-of-care’ assay. Two alternative scenarios were modelled reflecting data from key studies, as was sensitivity to costs. The model demonstrates that, for the base-case scenario, an initial diagnostic strategy of BNP is superior to ECG in terms of diagnosis of symptomatic heart failure in patients presenting in primary care, despite slightly more initial false negatives and a marginally higher cost. The alternative scenarios and sensitivity analyses show that the results are very sensitive to test accuracies and costs, but that, under plausible assumptions, BNP could be both cheaper and clinically superior. The model suggests that, despite parameter uncertainty, the adoption of BNP in primary care is likely to be clinically preferable, be more satisfactory for most patients, and lead to fewer unnecessary echocardiography referrals, at a very small increase in cost.
July 2008 Br J Cardiol 2008;15:205–9
Efficacy of ezetimibe and future role in the management of refractory hyperlipidaemia in high-risk patients
Rizwan Sarwar, Clare Neuwirth, Shahenaz Walji, Yvonne Tan, Mary Seed, Gilbert R Thompson, Rossi P Naoumova

A clinical audit of ezetimibe in the treatment of refractory hyperlipidaemia was conducted in 100 high-risk patients who failed to achieve desirable levels of total and low-density lipoprotein (LDL)-cholesterol on statins. Of these, 59 had familial hypercholesterolaemia (FH), the remainder had other aetiologies (non-FH). The percentage of patients achieving the total and LDL-cholesterol targets of the International Panel on the Management of FH or the Second Joint British Societies’ guidelines in non-FH patients was determined. Ezetimibe significantly decreased mean LDL-cholesterol when used as an adjunct to statins or as monotherapy, from 3.9 to 3.1 mmol/L in FH, from 3.4 to 2.4 mmol/L in non-FH and from 6.0 to 4.4 mmol/L in statin-intolerant patients. The decrease in LDL-cholesterol on statins was inversely correlated with the decrement after adding ezetimibe (r= -0.67, p<0.0001) but 15% of patients showed no further decrease. The percentage of patients achieving target levels of LDL-cholesterol was 27% on statins and 63% on statins plus ezetimibe (p<0.007). None of the non-FH patients achieved target levels on statins but 33% did so when ezetimibe was added (p<0.001). Ezetimibe is an effective adjunct to statins for lowering LDL-cholesterol in refractory hyperlipidaemia, except in a minority of patients, and is a useful substitute in statin-intolerant subjects.
July 2008 Br J Cardiol 2008;15:210-14
Clinical experience with prolonged-release nicotinic acid in statin-treated patients managed in Ireland
Michael O’Reilly, Ulrike Hostalek, John Kastelein

Nicotinic acid (for treatment of low high-density lipoprotein [HDL]) combined with a statin has been shown previously to improve cardiovascular outcomes. To evaluate tolerability and safety of prolonged-release nicotinic acid added to statin therapy in patients at high cardiovascular risk, the Niaspan®-induced HDL-Elevation for Optimizing Risk Control (NEMO) study focused on 179 patients with atherogenic dyslipidaemia treated under usual-care conditions. Flushing was the most common treatment-related adverse drug reaction (ADR) in Ireland (32% flushed during the first month), followed by cutaneous (6.2%) and gastrointestinal (3.9%) ADRs. Mean HDL-cholesterol increased by 20%. Half of the patients elected to continue treatment after the study. In conclusion, the tolerability and safety of prolonged-release nicotinic acid was similar in Ireland compared with the overall NEMO population. It is important to take practical measures to optimise patient compliance to minimise overall cardiovascular risk.
July 2008 Br J Cardiol 2008;15:215-6
Syncope: role of CMR in evaluating the aetiology in a patient with dual pathology
Didier Locca, Ciara Bucciarelli-Ducci, Sanjay K Prasad

We present a case in which the use of cardiovascular magnetic resonance (CMR) allowed the full pathology underlying syncope to be established.
May 2008 Br J Cardiol 2008;15:141–4
Availability of cardiac equipment in general practice premises in a cardiac network: a survey
Alison Day, Carol Oldroyd, Sonia Godfrey, Tom Quinn

Despite the major role of primary care in the management of people with, or at risk of developing, cardiovascular disease, little is known about the availability and state of readiness of cardiovascular diagnostic and monitoring equipment in general practice premises. We surveyed 170 general practices in one cardiac network. Our findings suggest that both provision of cardiac equipment, and training of staff in its use, is variable.
May 2008 Br J Cardiol 2008;15:145–8
The management of patients with mechanical heart valves and intracerebral haemorrhage
Daniel B McKenzie, Kelvin Wong, Timothy Edwards

Patients with mechanical prosthetic heart valves require oral anticoagulation to reduce the risk of thromboembolic events, but this can be complicated by anticoagulant-associated intracerebral haemorrhage (ICH). In order to make appropriate decisions about the resumption of anticoagulation in patients with mechanical heart valves and ICH, the risks of further bleeding must be weighed against those of thromboembolic events. There is limited evidence available to guide clinical decision-making in this situation and each case must be assessed individually, ideally with a multi-disciplinary team approach.
May 2008 Br J Cardiol 2008;15:151–4
Performing a comprehensive echocardiogram study: audit of adherence to the British Society of Echocardiography minimum dataset guidelines
Lindsey Tilling, Ariana González Gómez, Juan Gros Otero, Harald Becher

The British Society of Echocardiography (BSE) Education Committee has published a minimum dataset of 24 views for acquiring a standard adult transthoracic echocardiogram. To establish adherence to the minimum dataset, and secondly to establish the indication for echocardiography, we performed a retrospective review of 961 patients’ echocardiogram images and a prospective review (re-audit) of 832 patients’ echocardiograms, following a programme of echocardiographer education. Images were obtained from a computerised database over three months. Subjects were adult patients referred to the cardiology department of a large tertiary hospital in Oxfordshire. Results showed 17 views were consistently obtained in over 78% of patients, irrespective of audit period. Seven views were obtained in less than 50% of patients; of these, five views were performed significantly more frequently during re-audit. Apical four chamber continuous wave Doppler across the tricuspid valve, and subcostal views were performed in less than 45% of patients; this did not increase during re-audit. The main indication for performing an echocardiogram was assessment of left ventricular function, followed by assessment of valve function and investigation of arrhythmia. In conclusion, all echocardiographers need to be made aware of, and adhere closely to the requirements of the minimum dataset.
May 2008 Br J Cardiol 2008;15:156–7
Patient-focused outcomes following open-access echocardiography for suspected chronic heart failure
Stephen J Leslie, Victoria M Snowball, Andrea Ness, Janet Reid, Martin A Denvir

In a retrospective longitudinal cohort study of 111 consecutive patients with suspected left ventricular systolic dysfunction (LVSD) referred for open-access echocardiography, patient’s views at one-year follow-up in terms of satisfaction with the service, ongoing symptoms and personal health beliefs were assessed. Eighty-five (76%) patients completed a one-year follow-up questionnaire. LVSD was identified in only 18 (16%) patients. While 93% of all patients found the echocardiogram useful, 27% of patients could not recall being informed of the result. Many patients remained undiagnosed and symptomatic at one year. The detection rate for LVSD by open-access echocardiography remains low despite the use of a structured referral letter and screening electrocardiogram and chest X-ray.
May 2008 Br J Cardiol 2008;15:158–60
Managing patients with ‘statin intolerance’: a retrospective study
Rajesh K Nair, Rangaprasad L Karadi, Eric S Kilpatrick

The incidence of statin intolerance due to non-severe side effects is estimated to be 5–10%. As an increasing number of patients become eligible for lipid-lowering treatment, this is becoming a more prevalent issue. Very limited, if any, data exist so far in the management of this subgroup of patients. Clinic letters from 1,100 patients who attended the Lipid Clinic at Hull Royal Infirmary from January 2000 until December 2004 were searched for ‘statin intolerance’. Forty patients (19 male, 21 female, median age 62 years) were identified with intolerance to at least one statin drug but with an absolute indication to be on treatment. Out of the 40 patients, 26 (65%, 11 male, 15 female) were eventually able to tolerate a statin for at least six months without their initial side effect, the most commonly successful statins being rosuvastatin (n=9) and pravastatin (n=8). Overall, this required a median of two switches (range one to four) in statin treatment. Fourteen (35%) were unable to continue treatment after a median of 1.5 switches (range one to three), either because of continued intolerance or a decision not to proceed with more alternatives. In conclusion, nearly two thirds of patients with initial problems with a particular statin are able to take an alternative statin without side effects. This supports the trial of different statins in intolerant patients.
May 2008 Br J Cardiol 2008;15:161–65
The relationship between BNP and risk assessment in cardiac rehabilitation patients
Hugh J N Bethell, Jason D Glover, Julia A Evans, Sally C Turner, Raj L Mehta, Mark A Mullee

Risk stratification is important in the assessment of cardiac patients enrolled in physical training programmes but is often based on inadequate information. Measuring blood B-type natriuretic peptide (BNP) level, a marker of left ventricular dysfunction, might improve risk assessment. In an observational study blood BNP levels were measured in 100 consecutive patients joining a cardiac rehabilitation programme following acute myocardial infarction. The results were compared with the clinical risk assessment – high, moderate or low. There was a significant correlation between risk category (high, moderate or low) and BNP level (r=0.41, p=0.001). A BNP level of 100 pg/L or more gave a sensitivity of 89% (95% confidence interval [CI] 0.69, 0.97) and a specificity of 61% (95% CI 0.57, 0.63) for predicting high-risk patients with a positive predictive value of 33% (95% CI 0.26, 0.36) and a negative predictive value of 96% (95% CI 0.89, 0.99). A BNP level of less than 100 pg/ml gave a sensitivity of 78% (95% CI 0.55, 0.91) and a specificity of 54% (95% CI 0.43, 0.64) for predicting low-risk patients with a positive predictive value of 27% (95% CI 0.17, 0.40) and a negative predictive value of 92% (95% CI 0.80, 0.97). In conclusion, BNP levels provide information that may improve the accuracy of risk assessment of cardiac rehabilitation patients particularly when other information is limited.
May 2008 Br J Cardiol 2008;15:166–7
Thyroxine replacement therapy and risk of myocardial infarction: a cautionary tale!
Gurjinder Dahel, Shelley Raveendran, Kausik K Ray

Correction of thyroid hormone levels using thyroxine can have important cardiac implications. We report a case of myocardial infarction following rapid up-titration of thyroxine.
March 2008 Br J Cardiol 2008;15:79–81
Familial hypercholesterolaemia: recognising the unrecognised
Jonathan Morrell

Familial hypercholesterolaemia is a common genetic disorder that remains under-recognised. At present a simple genetic test is not available, although targeted genetic screening is being piloted in the UK. Recognition and treatment of this condition could help prevent many incidences of coronary heart disease. This article provides an overview of the pathophysiology, epidemiology, diagnosis and treatment of familial hypercholestrolaemia.
March 2008 Br J Cardiol 2008;15:83-85
Low-density lipoprotein-apheresis: an update
Stefanos Archontakis, Alison Pottle, Mahmoud Barbir

Low-density lipoprotein (LDL)-apheresis is the treatment of choice in homozygous familial hypercholesterolaemia as well as various other severe dyslipidaemic conditions. However, it appears to be under utilised in the UK. This article reviews the recent advances in (LDL)-apheresis techniques, as well as the beneficial effects and clinical outcomes of this therapeutic modality.
March 2008 Br J Cardiol 2008;15:87-94
New anticoagulant strategies in ST-elevation myocardial infarction treated with fibrinolytic therapy
Ian B A Menown

Anticoagulant therapy plays a key role in pharmacological reperfusion therapy for acute ST segment elevation myocardial infarction (STEMI). Until recently, the established role of unfractionated heparin (UFH) was unquestioned, but large trials with new agents including factor Xa inhibitors, direct thrombin inhibitors, and in particular, low molecular weight heparins (LMWHs), have shown potential advantages compared with UFH. This paper reviews the evidence base for the newer anticoagulants, with a focus on LMWH including the Enoxaparin and Thrombolysis Reperfusion for Acute Myocardial Infarction Treatment – Thrombolysis in Myocardial Infarction (ExTRACT TIMI)-25 study, which found that enoxaparin when appropriately adjusted for weight, age and renal function, provided superior net clinical benefit (balancing efficacy and safety) compared with UFH. In addition, new data from higher risk subgroups (the elderly, those with renal dysfunction or undergoing early coronary intervention) and the efficacy and safety of using concurrent clopidogrel are discussed to illustrate how these data may be integrated into contemporary practice.
March 2008 Br J Cardiol 2008;15:95-100
A UK survey of rosuvastatin in general practice: reaching cholesterol targets
George Kassianos, John Reckless, Cathy Emmas, Marc Evans, Andrea Tree, Andrew Vance

Data from 101 practices that had completed a survey of cholesterol target achievement using rosuvastatin in routine general practice were pooled to assess effectiveness at a national level. A total of 10,396 patients, who had total cholesterol (TC) measured prior to, and on, rosuvastatin 10 mg daily, were included in the analysis. Of these, 6,375 patients had not received a statin prior to rosuvastatin. The remainder had been switched from another statin. Significant reductions were observed in TC (28%) and low-density lipoprotein cholesterol (40%) when comparing prior to and on rosuvastatin 10 mg (p<0.001). A significantly greater proportion of patients achieved the General Medical Services (GMS) Quality and Outcomes Framework (QOF) target of TC ≤5 mmol/L with rosuvastatin 10 mg compared with prior to rosuvastatin (81% vs. 19%; p<0.0001). Of the 580 patients who had failed to reach target on atorvastatin 10 mg daily, 70% reached target on rosuvastatin 10 mg. Similarly, 68% of 246 patients who had failed to reach target on simvastatin 40 mg daily reached target on rosuvastatin 10 mg. General practitioners across the UK also substantially achieved other national and international cholesterol targets in patients treated with rosuvastatin 10 mg, including second line to simvastatin 40 mg and where higher doses of other statins had failed to reach target.
March 2008 Br J Cardiol 2008;15:101-5
A budget impact model for a drug in heart failure: eplerenone
Martin Duerden, Maggie Tabberer

The Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study (EPHESUS) showed that addition of eplerenone to optimal medical therapy reduced morbidity and mortality in patients with acute myocardial infarction complicated by left ventricular dysfunction and heart failure. This international study also showed that the addition of eplerenone reduced the number and duration of rehospitalisations for heart failure. A budget impact model has been developed to estimate the effect of adding eplerenone to standard care in the UK. The model is based on the results of the EPHESUS study, UK epidemiological data, UK drug acquisition costs and National Health Service (NHS) hospital in-patient costs and average length of stay for England. All costs are expressed in pounds sterling. It estimates the incremental costs and benefits of adding eplerenone to standard care in heart failure resulting from myocardial infarction, from the perspective of NHS healthcare decision makers over a three-year period. The model shows that if all eligible patients are treated with eplerenone the estimated cost per life year saved is £6,730 in year three. In a primary care trust with a population of 250,000, this level of treatment results in a reduction of 46 bed days for rehospitalisations due to heart failure, at a cost per bed day avoided of £1,469. With hospital in-patient care the biggest single healthcare cost in heart failure, reduction in hospitalisation is a key priority within the NHS in the UK. Models such as the one described here enable the budgetary consequences of using a new drug to be identified and clarify the role of drug treatment in delivering NHS priorities.
March 2008 Br J Cardiol 2008;15:106-9
Effect of ivabradine, a novel anti-anginal agent, on heart rate and symptom control: a first experience in a clinical ‘real-world’ setting
Tanuj S Lad, Glenda Osuoha, Shamara Fonseka, Julia S Hadley, Sandeep Gupta

Achieving a lower heart rate is important in treating angina. Established approaches include the use of beta blockers and certain calcium channel blockers. However, the use of these drugs may be limited by side effects or contraindications. Ivabradine (Procoralan®) is a novel agent that lowers heart rate through selective I(f) channel inhibition, acting specifically on the sinus node. We present a consecutive series of 30 patients initiated on ivabradine, within a district general hospital (DGH) setting. The aim of this study was to identify the heart rate-lowering and symptom-control properties of ivabradine, while monitoring adverse effects. Heart rate was measured on a baseline electrocardiogram (ECG) prior to starting ivabradine, and then within a 12-month follow-up period. The results identified a mean (standard deviation) 10 (14) beats per minute (bpm) decrease achieved on ivabradine (p<0.001), with greatest reduction in heart rate in those with a resting heart rate over 80 bpm prior to starting treatment (p<0.05), and in patients on a 5 mg twice-daily dosing regimen at follow-up (p<0.05). In parallel, the majority of patients reported favourable symptom benefit (21/30), and low rate of adverse events with discontinuation rate of only 2/30 felt directly related to the drug itself. We believe this to be the first report of using this novel drug in a ‘real-world’ DGH setting. The findings add confidence in using this anti-anginal agent in appropriate patients, and furthermore support conducting studies involving multiple centres, to further define and assess ivabradine in the clinical setting of angina.
March 2008 Br J Cardiol 2008;15:110
Surgery for palpitations?
Peadar F McKeown, Ian B A Menown, Paul F Rice

A 63-year-old gentleman presented with palpitations and a sensation of chest fullness. He had previously undergone laparoscopic oesophageal fundoplication.
March 2008 Br J Cardiol 2008;15:111–2
Percutaneous coronary intervention in dextrocardia
Tushar Raina, Ever D Grech, David Cumberland

Dextrocardia is a rare anomaly with an estimated prevalence of about one in 10,000. The incidence of coronary artery disease is the same as in the general population. We report two cases of successful percutaneous treatment of coronary stenoses and aim to highlight some of the additional technical challenges that such patients present to the Interventional Cardiologist.
January 2008 Br J Cardiol 2008;15:21
Subacute stent thrombosis within a paclitaxel-eluting stent
Andrew J Turley, James A Hall, Robert A Wright

A 60-year-old male was admitted acutely unwell with prolonged ischaemic chest pain. Seven weeks earlier he had undergone percutaneous coronary intervention (PCI) following admission with an acute coronary syndrome (ACS). Two paclitaxel-eluting stents to his left anterior descending (LAD) artery (2.75 x 32 mm, 2.75 x 16 mm), a 3 x 12 mm Tecnic stent to his obtuse marginal artery and 3.5 x 9 mm Tecnic stent to his proximal circumflex artery were inserted. The patient received intravenous heparin plus abciximab and an excellent angiographic result was achieved (figure 1A). He was discharged home on six months’ dual antiplatelet therapy.
January 2008 Br J Cardiol 2008;15:23-8
Implantable cardiac devices – past, present and future
Telal O Mudawi, Gerald C Kaye

Although cardiac electrostimulation was recognised centuries ago, the technology of implantable heart rhythm monitoring and therapeutic devices has only been established in the last few decades. Recent advances in such technology have led to simpler implantation techniques, greater patient convenience with smaller device sizes, extended battery longevity, increased device safety and reliability, and improved clinical outcomes.
January 2008 Br J Cardiol 2008;15:31-4
Controlling blood pressure over 24 hours: a review of the evidence
Mike Mead, Jennifer Adgey, Kathryn E Griffith, George Kassianos, Emran Khan, Philip Lewis, Jiten Vora

Despite huge advances in hypertension care in recent times, some important aspects of treatment are not routinely considered in practice, in particular the need for good 24-hour blood pressure (BP) control. Insufficient access to ambulatory blood pressure monitors (ABPM) in primary care and a lack of clear guidance limits routine use in BP management. ABPM, which measures BP over a full 24-hour period and captures BP fluctuations, may provide a more accurate reflection of patients’ ‘true’ BP than traditional office readings. Since uncontrolled 24-hour BP is linked to increased incidence of cardiovascular (CV) events and target organ damage, the panel believed the use of ABPM is beneficial to both patient and doctor. ABPM can aid compliance and guide treatment choices, given that there are marked differences in the duration of action of many commonly used BP treatments. A treatment with a long duration of action may be important in managing BP over 24 hours.
January 2008 Br J Cardiol 2008;15:35-9
Evaluation of an open-access heart failure service spanning primary and secondary care
Kiran CR Patel, Jennifer Prince, Seema Mirza, Lucy Edmonds, Rachel Duncan, Joanna Parry, Sally Jerome, John Wozniak, Nic Anfilogoff, Michael Frenneaux, Michael K Davies

Heart failure (HF) is common and the current gold-standard diagnostic modality for left ventricular systolic dysfunction (LVSD) is transthoracic echocardiography (TTE). To comply with the National Service Framework (NSF) for Coronary Heart Disease, an open access TTE service was established and this paper reports on the diagnostic yield of LVSD and valvopathy of TTE services in that service. Diagnostic services were made available to patients from both primary and secondary care. As part of the assessment, all patients were evaluated by TTE to assess left ventricular function and any valvular pathology. Overall, 61% of patients had normal left ventricular ejection fraction, 16% mild LVSD, 9% moderate LVSD and 14% severe LVSD. Forty-three per cent of patients had no evidence of valvopathy, 31% had mild, 19% moderate and 7% severe valvopathy. Valvopathy was the primary pathology in 15.8% of patients and 13.5% had LVSD as their primary pathology: 30.4% had no valvopathy or LVSD. In the remainder, it was not possible to determine the dominant pathology causing HF due to concomitant LVSD and valvopathy. TTE has a very high diagnostic yield in both primary and secondary care. Significant levels of valvopathy and LVSD are found in populations from both primary and secondary care.
January 2008 Br J Cardiol 2008;15:40-5
Chronic transfusion, iron overload and cardiac dysfunction: a multi-dimensional perspective
Hussain Isma’eel, Maria D Cappellini, Ali Taher

Cardiac dysfunction is common in patients with thalassaemia and is the leading cause of mortality in adult patients. Transfusional iron overload can affect heart function by directly damaging tissue through iron deposition or via iron-mediated effects at other sites. The main cardiac abnormalities reported in patients with thalassaemia and iron overload are left ventricular systolic and diastolic dysfunction, pulmonary hypertension, valvulopathies, arrhythmias and pericarditis. Prevalence varies according to the type of thalassaemia. However, even though patients with thalassaemia intermedia require fewer transfusions than those with thalassaemia major, they are still at high risk for cardiac complications. With the introduction of new technologies such as cardiac magnetic resonance T2*, the early detection of cardiac iron overload and associated cardiac dysfunction is now possible, allowing time for reversal through iron chelation therapy. Although chelation therapy can reverse iron-mediated cardiac disease by removing iron from iron-loaded cardiomyocytes and by alleviating the systemic iron overload contributing to heart failure, the challenges of deferoxamine infusions can significantly impact on compliance and, therefore, prognosis. The introduction of new oral iron chelators, together with improved understanding of the mechanisms and consequences of transfusional iron overload, should allow the continued improvement in cardiac outcomes for patients with thalassaemia and other transfusion-dependent anaemias.
January 2008 Br J Cardiol 2008;15:46-7
Pacemaker syndrome – a forgotten diagnosis?
Andrew Wiper, Nick P Jenkins, David H Roberts

An 86-year-old woman presented with a six-month history of severe peripheral oedema and limiting breathlessness. A dual chamber pacemaker had been implanted 12 years earlier for complete heart block, and she had recently been prescribed amiodarone for paroxysmal atrial fibrillation. Previous echocardiography had demonstrated a small hypertrophied left ventricle with an end-diastolic diameter of 3.9 cm and good systolic function.
January 2008 Br J Cardiol 2008;15:48-50
Pharmacological secondary prevention in people with peripheral arterial disease compared to thosewith coronary artery disease: a missed opportunity
Simon EJ Janes, Joe West, Brian R Hopkinson, John T Walsh

People with peripheral arterial disease (PAD) have a high prevalence of modifiable risk factors for coronary artery disease (CAD). Whether these risk factors are adequately treated remains unknown. We investigated people admitted to hospital with PAD and CAD. We compared use of antiplatelet agents, statins and angiotensin-converting enzyme (ACE) inhibitors before and during admission. Multivariate analysis showed that before admission, compared to patients with CAD, patients with PAD had decreased use of antiplatelet agents (odds ratio [OR] 2.7, 95% confidence interval [CI] 1.2–6.1), statins (OR 3.8, 95% CI 1.5–9.3) and ACE inhibitors (OR = 5.8, 95% CI 2.3–14.3). During admission, treatment was significantly less likely to be initiated in patients with PAD. This shows how secondary prevention can be neglected in patients with PAD. This is an important missed treatment opportunity, with substantial public health implications.
January 2008 Br J Cardiol 2008;15:51-4
Ultrasound-guided central venous access
Christopher P Gale, Andrew R Bodenham

Ultrasound guidance is a useful technique to aid central venous access. Alignment of the ultrasound probe and visualisation of the needle is a skill that takes some practice. This article describes how to perform ultrasound guidance to gain central venous access via the internal jugular, femoral and axillary/subclavian veins.
January 2008 Br J Cardiol 2008;15:55–6
Percutaneous retrieval of migrated femoral vein stent from the right heart
Sasalu M Deepak, Dharmendra Sookur, Richard D Levy

This case describes the discovery and subsequent attempts at removal of a migrated venous stent.
November 2007 Br J Cardiol 2007;14:255-9
Scientific Sessions 2007 of the American Heart Association
BJCardio editorial team

Major new trials reported at the American Heart Association 2007 Scientific Sessions, held in Orlando, Florida, US, on November 3rd–7th, showed mixed results for the new antiplatelet agent, prasugrel, and gave renewed hope for the high-density lipoprotein raising field. But there was disappointment regarding the use of statins in heart failure and beta blockers in general surgery.
November 2007 Br J Cardiol 2007;14:265
Aneurysm of the sinus of Valsalva
Jonathan M Behar, Thomas R Burchell, Ben Adeyemi, Fiona Myint

A 78-year-old woman presented to the vascular surgeons for a routine varicose vein procedure. She was fit and well with no significant medical history and had no cardiovascular risk factors. Clinically she was asymptomatic with a good excercise tolerance and no signs of heart failure. During the pre-operative assessment, a loud systolic murmur was heard all over the precordium with greatest intensity at the upper left sternal edge. Her electrocardiogram was unremarkable. A subsequent two-dimensional echocardiogram revealed a dilated aortic root and a large, 6.6cm aneurysm of the right coronary sinus of valsalva (see figure 1), which extended into the right ventricular outflow tract causing obstruction with an associated gradient of 44 mmHg. Her right ventricle was hypertrophied and there was mild tricuspid regurgitation. Her left ventricular function was normal and there was evidence of mild aortic regurgitation. A cardiothoracic opinion was sought but the operative risks were deemed unacceptable to both the surgeon and patient.
November 2007 Br J Cardiol 2007;14:267-71
The JBS 2 guidelines for the prevention of cardiovascular disease in people with diabetes: an approach to implementation
James D Lee, Sakera Shaikh, John R Morrissey, Vinod Patel

Patients with diabetes are at particularly high risk for cardiovascular disease. Indeed diabetes has been appropriately described as ‘a state of premature cardiovascular death associated with chronic hyperglycaemia’.1 Recently, the European Society of Cardiology (ESC) and the European Association for the Study of Diabetes (EASD) have published joint guidelines on diabetes, pre-diabetes, and cardiovascular diseases.2 Broadly, they reflect the rigorous approach of the 2005 revised Joint British Societies’ guidelines on the Prevention of Cardiovascular Disease in Clinical Practice (JBS 2).3 In this article, we will revisit the main JBS 2 guidelines for individuals with diabetes and compare them with the recommendations from the ESC/EASD.
November 2007 Br J Cardiol 2007;14:275-79
Improving access to financial support for heart failure patients: understanding the claims process and the doctors’ role
Christopher Ward

Many heart failure patients are eligible to receive financial support (Disability Living Allowance or Attendance Allowance) because of their impaired mobility. Those with a very limited prognosis can gain rapid access to these benefits by claiming under "special rules" with the support of a report (DS 1500) from their doctor.
November 2007 Br J Cardiol 2007;14:280-5
Switching statins: the impact on patient outcomes
Berkeley Phillips, Fayaz Aziz, Christopher P O"Regan, Craig Roberts, Amy E Rudolph, Steve Morant

Little is currently known of the effect of switching statin therapy on cardiovascular outcomes. Using The Health Improvement Network database, patients who had received atorvastatin for ≥ six months were identified. They were classified as ‘switch’ if they were subsequently switched to simvastatin, and were matched to up to four 'control' patients who remained on atorastatin. Time to death or first major cardiovascular event was compared, controlling for the matching co-variates, prior statin exposure and baseline cholesterol concentration.
November 2007 Br J Cardiol 2007;14:286-8
The 2007 Curriculum in Cardiology: an overview for trainees and trainers
Chris Gale, Helen Simpson, Saul Myerson, Nick Curzen, Theresa McDonagh, Ian Wilson, Peter Mills, James Hall, Stuart Cobbe

Implementation of a new specialty training Curriculum in Cardiology from August 2007 will bring significant changes to specialist training in cardiology. The format, delivery and evaluation will differ, and these changes are relevant to both existing and newly appointed trainees. This article aims to summarise the changes and incorporates presentations by the Cardiology Specialist Advisory Committee at the British Cardiovascular Society conference in June 2007.
November 2007 Br J Cardiol 2007;14:289-92
Radiation during cardiovascular imaging
Ariel Roguin, Prashant Nair

Several imaging modalities are available for the optimal management of patients with cardiovascular disease. When assessing any imaging technique, the radiation dose must be considered along with the value of the imaging technique. In this article, we summarise the radiation doses associated with cardiovascular imaging techniques, such as heart catheterisation, nuclear medicine and multi-slice computed tomography. The effective dose of the dual isotope scan, an image modality frequently used in cardiac patients, is higher (~25 mSv) than cardiac computed tomography (~10 mSv) or diagnostic heart catheterisation (~5 mSv). The physician should weigh carefully which test to recommend in each patient.
November 2007 Br J Cardiol 2007;14:296
Pericardial tamponade due to ruptured pyogenic hepatic abscess
Sushma Rekhraj, Trevor Wistow

This case describes the unfortunate consequence of hepatic abscess, initially discovered following abnormal liver function tests.
September 2007 Br J Cardiol 2007;14:207–12
Health-related quality of life from the perspective of patients with chronic heart failure
Karen Dunderdale, Gill Furze, David R Thompson, Stephen F Beer, Jeremy NV Miles

The aims of treatment in chronic heart failure are to reduce symptoms, improve function and prolong life. Currently there is no patient-centred health-related quality of life measure in chronic heart failure. The aim of this study was to explore health-related quality of life from the perspective of patients with chronic heart failure and to identify themes for inclusion in a patient-generated instrument.
Semi-structured interviewing of patients with an objective diagnosis of chronic heart failure was undertaken. Analysis of the transcripts identified seven themes on health-related quality of life. These were: changes in physical ability, emotional state, self-awareness and self-perception, changes in relationships, symptoms, maintaining social/lifestyle status and cognitive aspects.
Findings from this study will contribute to the development of a patient-led health-related quality of life measure for use in everyday practical care in a chronic heart failure population.
September 2007 Br J Cardiol 2007;14:215-218
One-year data from the UK arm of the REACH Registry
Jonathan M Morrell, George C Kassianos

Atherothrombosis is a leading cause of global mortality. It represents a significant public health issue in the UK and, as such, the UK Government has made it a healthcare priority. The global REduction of Atherothrombosis for Continued Health (REACH) Registry aims to evaluate the long-term risk of atherothrombotic events in an at-risk population, to assess the importance of cross-risk and to define predictors of atherothrombotic events. REACH has recruited over 68,000 people in over 5,000 centres in 44 countries, of which 618 were from the UK.
September 2007 Br J Cardiol 2007;14:221-28
Chronic kidney disease in primary care
Juliet Usher-Smith, Andy Young, Simon Chatfield, Mike Kirby

Chronic kidney disease (CKD) is an independent risk factor for cardiovascular disease and in February 2006 was added to the Quality and Outcomes Framework (QOF) for primary care in the UK. The QOF indicators apply to all patients with stage 3–5 CKD and include the production of a register of such patients, appropriate monitoring and treatment of hypertension and the prescription of angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs).
September 2007 Br J Cardiol 2007;14:229-33
Generic or intensive statin therapy: saving money or saving lives?
Rob Butler

Over the last few years, there has been a gradual increase in the use of intensive statin therapy, ostensibly atorvastatin 80 mg for high-risk individuals, such as those who suffered a myocardial infarction or underwent revascularisation. First-World economies, such as the UK, with a significant state contribution healthcare funding, had mounting anxiety because of the expanding indications and therefore cost of intensive statin therapy. The perceived relative expense of this strategy provoked a swift, often unilateral, withdrawal of such regimens by commissioners.
September 2007 Br J Cardiol 2007;14:234-6
Stent thrombosis and antiplatelet therapy: a review of 3,004 consecutive patients in a single centre
Nick Curzen, Geraint Morton, Alex Hobson, Iain Simpson, Alison Calver, Huon Gray, Keith D Dawkins

Stent thrombosis (ST) is an uncommon but serious complication of percutaneous coronary intervention (PCI), and is associated with the discontinuation of antiplatlet therapy. In a retrospective study of ST cases during a two-year period of the Wessex Regional Cardiac Unit, 3,004 (1,661 emergency and 1,343 elective) patients underwent PCI between November 2003 and October 2005. There were 25 episodes of ST occurring in 22 patients (overall incidence of ST is 0.83%). There were two (8%) cases of acute ST, eight (32%) of sub-acute ST and 15 (60%) of late or very late ST (five cases between six and 12 months and one case more than one year post-procedure). In the late and very late ST group only one patient was taking dual antiplatelet therapy.
September 2007 Br J Cardiol 2007;14:237-41
Non-invasive cardiac imaging: current and emerging roles for multi-detector row computed tomography. Part 2
Edward D Nicol, Simon PG Padley

The demand for non-invasive diagnostic imaging in cardiology increases with the advancing age of the population. Whilst exercise testing and myocardial perfusion scintigraphy have provided non-invasive functional assessment of coronary artery disease there has been little alternative to invasive coronary angiography for anatomical assessment of the coronary tree.
September 2007 Br J Cardiol 2007;14:242-44
Rhabdomyolysis and acute renal failure due to simvastatin and amiodarone
Haroon Siddique, Maria Mushkbar, Adrian Walker, John Scarpello

Rhabdomyolysis is an uncommon but potentially serious adverse reaction associated with the use of statins. Simvastatin is metabolised by cytochrome P450 CYP3A4 and amiodarone is an inhibitor of this enzyme. Concomitant use of these drugs, especially with high doses of simvastatinm may result in myopathy. Acute renal failure as a result of rhabdomyolysis due to this aetiology is rare with only a few cases reported previously. Here, we report a case of rhabdomyolysis and acute renal failure secondary to concomitant use of simvastatin and amiodarone.
September 2007 Br J Cardiol 2007;14:293-95
The VentureTM wire control catheter
Peter O’Kane, Lucy Blows, Simon Redwood

The presence of severe vessel tortuosity, extreme angulation of side-branch ostia, stent jail, or lack of control at the interface of chronic total occlusions can result in percutaneous coronary intervention failure or complications. The Venture™ wire control catheter is a new catheter system designed to facilitate tip direction of a standard 0.014” guidewire. The properties of this system are discussed in this article along with an example of its use in practice.
May 2007 Br J Cardiol 2007;14:143-50
Non-invasive cardiac imaging – current and emerging roles for multi-detector row computed tomography. Part 1
Edward D Nicol, Simon PG Padley

The demand for non-invasive diagnostic imaging in cardiology increases with the advancing age of the population. Whilst exercise testing and myocardial perfusion scintigraphy have provided non-invasive functional assessment of coronary artery disease there has been little alternative to invasive coronary angiography for anatomical assessment of the coronary tree. In recent years technological advances have enabled improvements in both temporal and spatial resolution such that multi-detector computed tomography (MDCT) is now able to reproducibly evaluate cardiac disease. The combination of this improved resolution with more advanced post-processing techniques now means that MDCT has the ability to perform both anatomical and functional assessment from a single study. This technique, therefore, not only provides a non-invasive alternative to conventional angiography but the same dataset allows concurrent assessment of cardiac function, assessment of aberrant vessels, graft patency studies and assessment of the coronary artery wall. Cardiac CT has the potential to provide a much more complete assessment than conventional coronary angiography. It is likely to become the non-invasive imaging modality of choice to exclude significant coronary artery disease in those with intermediate risk of coronary artery disease. This first part of a two-part article considers ECG-gated image reconstruction, image resolution, radiation dose, and post-processing protocols and limitations. The second part considers clinical applications and future developments.
May 2007 Br J Cardiol 2007;14:153-59
Baseline data from the UK arm of the REACH Registry
Jonathan M Morrell, George C Kassianos For The Reach Registry Investigators

Atherothrombosis is a leading cause of death worldwide. The REduction of Atherothrombosis for Continued Health (REACH) Registry aims to evaluate the long-term risk of atherothrombotic events in a global at-risk population, to assess the importance of cross-risk and to define predictors of atherothrombotic events. Over 69,000 people in 44 countries were recruited, of which 618 were in the UK. The majority (91%) of patients recruited in the UK had symptomatic disease (coronary artery disease, cerebrovascular disease or peripheral arterial disease) of which 14% had disease in more than one vascular bed. Classic cardiovascular risk factors were seen to be active and their management was found to be inadequate, albeit better in those with symptomatic disease than in those with risk factors only. UK data were in general typical of those found in the whole of the Western European sample.
May 2007 Br J Cardiol 2007;14:161-63
The European Working Time Directive: potential impact on cardiology specialist registrar training
Chris P Gale, Richard P Gale, Phil D Batin, John Wilson

The European Working Time Directive (EWTD) ensures doctors do not work excessive hours. On 1st August 2004, junior doctors were no longer excluded from the EWTD and their working hours were limited by law to 58 hours per week. By 2009, this will be reduced to 48 hours. Although benefits include improved patient care,1 the EWTD has implications for service provision and specialist registrar (SpR) training.
May 2007 Br J Cardiol 2007;14:165-68
How safe is femoral access? Insights from an audit of contemporary practice
Helen C Routledge, Peter F Ludman, Sagar N Doshi, John N Townend, Nigel P Buller

Complications of arterial access are an important cause of morbidity following percutaneous coronary intervention. Recently published data suggest a rate of around 3.5% of major vascular complications. We present an audit of vascular access site complications in a single centre over a 12-month period. Overall complication rates were low (1.2%) in a centre whose default strategy following femoral artery access is arterial closure using the Perclose™ device. Specific problems using the Starclose™ device in patients treated with abciximab are described. Infected femoral artery haematoma resulted in the most severe complications.
May 2007 Br J Cardiol 2007;14:169-70
Costs of aspirin should include treatment costs for dyspepsia
Yohan P Samarasinghe, Ian Purcell, Helen Rivas-Toro, Michael D Feher

This short report describes a questionnaire study undertaken in two London teaching hospitals, addressing the true pharmacokinetic implications of aspirin use. It suggests that the real costs of aspirin treatment should include the cost of the therapies used for treatment of associated dyspepsia.
May 2007 Br J Cardiol 2007;14:171-73
Asymptomatic myocardial involvement in acute dengue virus infection in a cohort of adult Sri Lankans admitted to a tertiary referral centre
Ravindra L Satarasinghe, Kanagasinham Arultnithy, Neomali L Amerasena, Uditha Bulugahapitiya, Deshu V Sahayam

Viral myocarditis is a well-recognised complication of many viruses leading to subsequent cardiomyopathies (dilated type). There are limited data available with respect to dengue virus involvement, an infection which can be asymptomatic and can lead to undifferentiated viral fever syndrome, dengue fever, dengue haemorrhagic syndrome or dengue shock syndrome. Dengue has probably been endemic in Sri Lanka for a long time although no cases of dengue haemorrhagic fever was reported until 1965. Now, several hundred cases a year have been reported annually from 1991. The only two published articles from Sri Lanka on myocardial involvement described cardiac sequelae, diagnosed quite late, retrospectively, in the non-active phase of the illness. Recent epidemics of the disease in Sri Lanka led us to design a study to look at myocardial involvement in clinically and serologically confirmed cases of dengue infection.
May 2007 Br J Cardiol 2007;14:175-78
Clinical trials versus the real world: the example of cardiac rehabilitation
Rod S Taylor, Hugh JN Bethell, David A Brodie

Clinical practice should follow evidence-based medicine, which is derived from clinical trials. The outcomes of clinical practice, however, may not equal that of trials if there are differences in the patients or the quality of treatment they receive. We report the example of cardiac rehabilitation to illustrate this point, comparing the characteristics of patients and treatments offered in randomised controlled trials (RCTs) in this area with those included in two large surveys of cardiac rehabilitation in the UK. We found that cardiac rehabilitation as currently practised in the UK is unlikely to be as effective as clinical trials may suggest.
March 2007 Br J Cardiol 2007;14:83-89
Peri-operative transoesophageal echocardiography
Susan Wright

Peri-operative transoesophageal echocardiography (TOE) has become part of the routine management of patients undergoing cardiac surgery. Its use in guiding not only surgery, but also the haemodynamic management of the patient, has made TOE an indispensable tool in the cardiac operating theatre. Practical aspects of intra-operative TOE are outlined and its application in differing clinical situations is reviewed.
March 2007 Br J Cardiol 2007;14:90-7
Stress echocardiography – current status
Roxy Senior, John Chambers

Stress echocardiography has a high diagnostic accuracy for the detection of coronary disease. It is as effective as myocardial perfusion imaging for the stratification of risk in patients with coronary disease and can detect myocardial hibernation after myocardial infarction or in heart failure.
March 2007 Br J Cardiol 2007;14:99-101
Echocardiography within the British Isles: executive summary of a British Society of Echocardiography survey
John Chambers, Kevin Fox, Roxy Senior, Petros Nihoyannopoulos

This paper is an executive summary of a recent postal survey carried out by the British Society of Echocardiography to guide future planning.
March 2007 Br J Cardiol 2007;14:102-104
Diabetes information in cardiovascular trials published in general medical journals
David P Macfarlane, Ken R Paterson, Miles Fisher

Individuals with diabetes have an increased risk of developing coronary artery disease and a poorer prognosis once coronary artery disease has developed, compared to patients without diabetes. To avoid confounding, most cardiovascular trials display profiles of traditional risk factors but additional factors are also important in patients with diabetes. We examined the information provided on patients with diabetes included in cardiovascular trials published in general medical journals.
March 2007 Br J Cardiol 2007;14:106-108
Hospital anxiety and depression in myocardial infarction patients
Joy McCulloch

The National Service Framework for Coronary Heart Disease recommends that psychological support should be offered to those patients who require it. A six-month study carried out at Darlington Memorial Hospital looked at psychological support needed by patients following myocardial infarction (MI). The psychological status of MI patients was formally assessed using the Hospital Anxiety and Depression (HAD) scale and appropriate referrals were made to psychological support services to improve patient management. The study also measured the impact that formal assessment of the psychological status of MI patients would have on service providers. Some 80 MI patients from the Darlington primary care trust (PCT) were eligible for inclusion in the study. Psychological assessment was undertaken at four stages during cardiac rehabilitation and 25 patients were eligible for referral for psychological support as a result of high HAD scores measured during the study period. Ten patients accepted referral, a higher number than during the previous six-month period when HAD scales had not been used. Eight patients were referred to occupational therapy services for help with anxiety issues, one patient was referred to the psychology service and one to liaison psychiatry. Both of these patients required help with depression. The study also found a high degree of patient satisfaction. The support received may also be required by many other groups of patients.
March 2007 Br J Cardiol 2007;14:109
Infective endocarditis with secondary lesions in the pinna
Akeel Jubber, Hon Shing Ong, Yoganathan Suthahar, Ravinder Randhawa

This case describes, for the first time, the appearance of possible cutaneous embolic lesions in the pinna of the ear secondary to infective endocarditis
March 2007 Br J Cardiol 2007;14:111-115
Use of a defibrillation coil in the coronary sinus to reduce ventricular defibrillation threshold
Sujatha Kesavan, Michael A James

Although the majority of implantable cardioverter defibrillator (ICD) implants occur without complication, high defibrillation threshold (DFT) can occasionally be a problem. The usual resolution to this problem is to include a subcutaneous electrode in the defibrillation circuit. Use of the subcutaneous array, however, is unpopular as extensive subcutaneous dissection is time-consuming, uncomfortable for the patient and provides another focus for infection. We report the use of the coronary sinus for the placement of a second defibrillation shock coil in a patient with an unacceptably high DFT, which was successfully reduced.
March 2007 Br J Cardiol 2007;14:117-119
Audit of the new GMS contract Quality and Outcomes Framework: raising standards in CHD
Janet McCarlie, Elisabet Reid, Adrian JB Brady

This paper briefly reviews an analysis carried out in the West of Scotland of the Quality and Outcomes Framework data gathered for coronary heart disease under the new General Medical Services contract for general practitioners. It shows encouraging progress in achieving clinical outcome predictors.
March 2007 Br J Cardiol 2007;14:119-120
Quality, evidence-based medicine and pay for performance: the primary care experience
Rubin Minhas

The report from McCarlie and colleagues in this issue (pages 117–19) on the success of Scottish general practice in achieving cardiovascular disease (CVD) targets for clinical indicators within the Quality and Outcomes Framework (QOF) mirrors similar progress across England and Wales.
January 2007 Br J Cardiol 2007;14:19-22
Outcome of atrial repair procedures in patients with transposition of the great arteries followed up in a district general hospital
Sushma Rekhraj, Leisa J Freeman

Patients with transposition of the great arteries (TGA) are now living longer due to improved medical and surgical care. Most of the current patients with TGA followed up at our district general hospital (DGH) grown-up congenital heart (GUCH) clinic have undergone a Mustard or a Senning atrial repair procedure between the early 1960s to mid 1980s. Complications found to be associated with the atrial repair procedure include arrhythmias, right ventricular impairment, tricuspid valve dysfunction, baffle-related problems and sudden death. This article reviews the outcome of patients with TGA in this DGH population and also addresses the issue of pregnancy and insurance.
January 2007 Br J Cardiol 2007;14:23-8
Management of atrial fibrillation: an overview of the NICE guidance on AF management
Timothy Watson, Eduard Shanstila, Gregory Yh Lip

This article aims to provide an overview of the management of atrial fibrillation (AF), with reference to the recently published National Institute for Health and Clinical Excellence (NICE) guidelines on AF management (http://www.nice. org.uk/CG36/guidance/pdf/english). This article is not meant to cover the whole guideline nor be a systematic review, as the full guideline contains all the search strategies and appraised evidence tables, and represents a comprehensive assessment of the evidence behind the recommendations in the NICE guideline (also available at http://rcplondon.ac.uk/pubs/books/af/index.asp).
January 2007 Br J Cardiol 2007;14:23-30
The NICE guidelines on atrial fibrillation: a personal view
David Fitzmaurice

The guidelines on atrial fibrillation (AF) produced by the National Institute for Health and Clinical Excellence (NICE) and published by the Royal College of Physicians are impressive in their scope and details. They are overtly evidence based and whilst there is some debate over some issues within the guidelines, there is no doubt that they represent much hard work from the Guidelines Development Group.
January 2007 Br J Cardiol 2007;14:31-6
The emerging role of intracardiac echocardiography – into the ICE age
Andrew RJ Mitchell, Prasanna Puwanarajah, Jonathan Timperley, Harald Becher, Neil Wilson, Oliver J Ormerod

Intracardiac echocardiography (ICE) is an imaging technique that is becoming increasingly available as an alternative to transoesophageal echocardiography to guide percutaneous interventional procedures. The probe can be inserted under local anaesthesia and is principally used during closure of atrial septal abnormalities. The main advantages of ICE over transoesophageal echocardiography include the elimination of the need for general anaesthesia, clearer imaging, shorter procedure times and reduced radiation doses to the patient. Within this article we review some of the current applications of ICE and how to image from within the heart.
January 2007 Br J Cardiol 2007;14:37-40
Coronary artery calcification is associated with alcohol intake but not oxidative stress or inflammation
Natalie C Ward, Kevin D Croft, Henrietta Headlam, Trevor A Mori, Keith Woollard, Ian B Puddey

Coronary artery calcification (CAC) is a component of the development of atherosclerosis. Coronary computed tomography scanning (CCT) can detect calcification and may be useful in individuals considered asymptomatic. Oxidative stress and inflammation are linked through common pathways and both are thought to be involved in the pathogenesis of atherosclerosis. To investigate if CAC was associated with increased oxidative stress (plasma F2-isoprostanes) and inflammation (high sensitivity C-reactive protein [hs-CRP]), we invited 102 self-selected individuals (mean age 52+/-7 years) who were undergoing CCT to take part in a study. Height, weight and clinic blood pressure was measured, a blood sample taken and a health and lifestyle questionnaire completed.
CAC was found to be positively correlated with age (p<0.01) and alcohol intake (p<0.001). There was a trend for higher CAC in men compared to women (p=0.08). CAC was higher in ex- and current smokers versus non-smokers (115+/-45 vs. 28+/-12 Agatston score, p=0.05), and lower in non-drinkers versus drinkers (18+/-17 vs. 90+/-29 Agatston score, p=0.03). There were no univariate correlations between CAC and plasma F2-isoprostanes (p=0.25) or HS-CRP (p=0.36). In multivariate analysis, age, male gender and alcohol intake remained independent predictors of CAC. We concluded that CAC was not associated with inflammation or oxidative stress, but was related to lifestyle factors including; age, gender and alcohol consumption.
January 2007 Br J Cardiol 2007;14:41-44
Uses of the multi-functional probing catheter in the recannalisation of chronic total occlusions
Lucy JH Blows, S Divaka Perera, Simon R Redwood

This paper discusses the uses of the Multi-functional probing catheter™ (Boston Scientific, Scimed) in the arena of percutaneous coronary intervention with specific reference to treating chronic total occlusions. This catheter is essentially a speedy monorail balloon without the balloon mounted on the end. Thus, it has a short monorail/rapid exchange port which exits at the distal tip of the catheter, and an over-the-wire port which exits proximally at the side of the catheter. Tackling chronic total occlusions often results in the creation of a false passage intramurally rendering it difficult to redirect the guide-wire into the true lumen. The Multi-functional probing catheter™ allows introduction of a second wire in a different direction from this lumen via the over-the-wire port. The benefits of this equipment for guide-wire support and wire exchange are examined. In addition, this support catheter allows distal vessel visualisation, confirming intraluminal wire position. A further use of this catheter is for intracoronary drug delivery especially in the context of vascular spasm, no reflow or thrombotic occlusion. The use of the Multi-functional probing catheter™ in two chronic total occlusion interventions cases is discussed in detail.
January 2007 Br J Cardiol 2007;14:45-48
A comparison of once- versus twice-weekly supervised phase III cardiac rehabilitation
Helen J Arnold, Louise Sewell, Sally J Singh

Optimum delivery of cardiac rehabilitation is not well defined. A retrospective analysis was conducted to determine the short-term effectiveness of once-weekly compared to twice-weekly supervised cardiac rehabilitation. The analysis included 206 post-myocardial infarction patients who participated in either once- or twice-weekly supervised exercise sessions for six weeks. The primary outcome measure was the incremental shuttle walking test (ISWT). Secondary measures of health-related quality of life were also completed. Once-weekly supervised rehabilitation was completed by 85 patients (65 men), mean (SD) age 61.89 (10.27) years, and twice-weekly supervised rehabilitation was completed by 121 (94 men) mean (SD) age of 59.24 (10.03) years. Both groups demonstrated a statistically significant increase in ISWT distance post-rehabilitation, with mean increases of 100.71 metres (p<0.001) and 88.44 metres (p<0.001) for the once- and twice-weekly groups respectively. A reduction in hospital anxiety and depression scores and improvements in the MacNew quality of life questionnaire was also found. On comparing the magnitude of these changes, there was no significant difference between the two groups. There is no evidence of additional short-term benefit, in terms of cardiovascular fitness and improvement in health-related quality of life measures, for patients attending twice-weekly supervised cardiac rehabilitation compared to once-weekly.
January 2007 Br J Cardiol 2007;14:49-50
A case of lipomatous hypertrophy of the interatrial septum and coronary artery disease
Momin Salahuddin, E Jane Flint

The condition of a large deposit of adipose tissue in the atrial septum or lipomatous hypertrophy of interatrial septum (LHIS) was first described in 1964. It has been reported that LHIS is associated with atrial arrhythmias but its clinical presentation as angina is uncommon. We report such a case here and a short literature review.
January 2007 Br J Cardiol 2007;14:51-55
A pilot study on computer-based opportunistic screening for coronary heart disease: universal assessment and education in primary care
Peter F Tyerman, Gill V Tyerman, Ruth Bacigalupo

Cardiovascular disease prevention is one of the major challenges of medicine in the UK and the developed world. Progress in the primary prevention of these diseases has been slow and patchy due to the difficulties and costs with the methods currently used. We set out to see in an observational study, if computer-based opportunistic screening could be a practical and cost-effective method of cardiovascular disease prevention in a high-risk primary care practice population in Barnsley, South Yorkshire. We found that over five years, 86% of the practice population was screened and educated for their personal risk of cardiovascular disease. This was carried out at a low cost in terms of both professional and administrative time. Using this computer-based opportunistic screening enables a profile of risk factors for both individuals and the practice to be de-veloped making the targetting of resources for prevention easy and effective. It is also possible that this programme could prove to be a cheap and targetted method of screening for coronary heart disease, diabetes and familial hyperlipidaemia. We conclude that computer-based opportunistic screening in general practice is an effective method of reaching a whole population and can enable large-scale interventions at low cost.
January 2007 Br J Cardiol 2007;14:57-60
‘Tidal wave’ of obesity and type 2 diabetes predicted to dominate CVD practice
Jo Waters

The management of the ‘tidal wave’ of obesity and type 2 diabetes that is expected to hit the UK over the next 10 years was one of the major themes to emerge from the Primary Care Cardiovascular Society Annual Meeting and AGM, held in Gateshead, October 5th – 7th 2006. Medical journalist Jo Waters reports.
November 2006 Br J Cardiol 2006;13:367-9
The impact of the new GP contract on measurement of lipids and use of statins in the over 80s with coronary heart disease
Samira Siddiqui, Chris Isles, Ewan Bell, Alan Begg

The benefits of statins for both primary and secondary prevention of coronary heart disease (CHD) are limited mainly to patients under 80. We examined the impact of the new General Medical Services (GMS) contract on measurement of lipids and prescribing of statins in patients over 80 years of age with CHD. We found that there has been a significant increase in both, with little evidence supporting this and substantial financial implications. National guidance on the assessment and management of lipids in the over 80s in the new GMS contract is urgently required.
November 2006 Br J Cardiol 2006;13:371-2
Revised GMS2: a target too far?
Mike Mead

If you speak to any general practitioner (GP) in the next few months, there are three letters that will be occupying his or her mind: QOF. Rather than an exotic hairdo, this stands for ‘Quality and Outcomes Framework’ and determines a considerable proportion of our income.
November 2006 Br J Cardiol 2006;13:399-404
Maternal cardiovascular medicine: towards better care for pregnant women with heart disease
Diane Barker, Nigel Lewis, Gerald Mason, Lip-Bun Tan

Cardiac disease has emerged as the leading cause of maternal death during pregnancy in the UK. Its incidence has been rising in the past two decades, largely due to increasing mortality from acquired heart disease, which currently exceeds mortality from congenital heart disease. According to the Confidential Enquiry, better care could have altered the course of 40% of the deaths from cardiac causes. Management of these patients is critical, because any maternal complication has major impacts on surviving children. Improvements in maternal cardiovascular medicine require concerted efforts through interdisciplinary collaboration of all specialties caring for pregnant cardiac patients. One important area for improvement is on how to identify and evaluate those at highest risks of pregnancy-related cardiac complications. Most assessments and clinical guidelines for the management of pregnant women with heart disease have been based on retrospective lesion-specific information. Direct evaluation of cardiac function during pregnancy may add further information, improving the cardiac care we can provide to individual pregnant cardiac patients. More research in this area is urgently needed. We also propose that improvement in training, research and exposure to the subspecialty of maternal cardiovascular medicine is needed to continue to raise standards of care for this patient population.
November 2006 Br J Cardiol 2006;13:405-10
Recent developments in smoking cessation
Serena Tonstad

Smoking cessation substantially reduces the risk of cardiovascular disease in the prevention of primary and secondary cardiovascular events. Current first-line therapies include nicotine replacement therapy and bupropion, that approximately double a smoker’s chances of long-term success. Both therapies are safe in patients with cardiovascular disease. Novel treatments include rimonabant, nicotine vaccines and varenicline. To date, varenicline, an a4a2 nicotinic acetylcholine receptor partial agonist has been approved for smoking cessation and has been shown to be efficacious and well tolerated in clinical studies conducted in healthy smokers.
November 2006 Br J Cardiol 2006;13:411-8
Cost-effectiveness of adding prolonged-release nicotinic acid in statin-treated patients who achieve LDL cholesterol goals but remain at risk due to low HDL cholesterol: a UK-based economic evaluation
BJCardio editorial team

Clinical guidelines focus on statins for dyslipidaemia management for prevention of cardiovascular disease. It is clear, however, that there remains an unacceptably high residual risk of further events among patients who achieve target low-density lipoprotein (LDL) cholesterol levels. Low high-density lipoprotein (HDL) cholesterol levels, an independent predictive factor, is likely to be an important contributor to this excess risk, and is also common among dyslipidaemic patients. The ARBITER 2 study (ARterial Biology for the Investigation of the Treatment Effects of Reducing cholesterol) showed that raising HDL cholesterol with prolonged-release (PR) nicotinic acid in addition to lowering LDL cholesterol with a statin slows progression of atherosclerosis, and would therefore be expected to improve cardiovascular risk reduction in this setting. This economic analysis evaluated the cost-effectiveness of this strategy using computer simulation economic modelling incorporating two decision analytic sub-models. In the first sub-model, a cohort of 2,000 patients was generated using baseline characteristics and statin effect from the Heart Protection Study. Treatment effects observed with PR nicotinic acid (1,000 mg/day) in the ARBITER 2 study were then applied. The second model evaluated long-term clinical and economic outcomes using Framingham risk estimates. Direct medical costs were accounted from a National Health Service (NHS) perspective and discounted by 3.5%. In the UK setting, the addition of PR nicotinic acid to statin therapy resulted in long-term reduction in CHD events and increased life expectancy in patients who had achieved target LDL cholesterol levels but had persistently low HDL cholesterol, and this was achieved at a cost well within the threshold (< £30,000 per life years gained) considered good value for money in the UK. This strategy was highly cost-effective in patients with diabetes. Thus, adding PR nicotinic acid to statin therapy in these patients is both clinically and cost-effective and could be recommended for routine use in this setting in the UK.
November 2006 Br J Cardiol 2006;13:419-24
Eisenmenger syndrome – conventional management and new therapeutic prospects
Anita Dumitrescu, Kevin P Walsh

Patients with Eisenmenger syndrome generally die prematurely from complications directly due to their pulmonary hypertension and cyanosis, or due to intercurrent events that are poorly tolerated because of the underlying inadequate cardiopulmonary reserve. To date, clinical management has aimed at avoiding situations that would destabilise their condition and treatment of its complications. However, therapeutic prospects are starting to look more encouraging. Results from a small study with the oral dual endothelin receptor antagonist, bosentan, have shown improved exercise capacity. Additionally, there appears to be a possible role for the phosphodiesterase-5-inhibitor, sildenafil, in the treatment of Eisenmenger pulmonary hypertension.
November 2006 Br J Cardiol 2006;13:425-9
Changes to the European Resuscitation Council cardiac arrest management guidelines – a commentary
Dilshan Arawwawala, Stephen Brett

The European Resuscitation Council guidelines for the management of cardiac arrest have been updated. The following commentary discusses the major changes, the evidence on which they are based and the practical issues of their introduction.
November 2006 Br J Cardiol 2006;13:430-1
Amiodarone, sunlight avoidance and vitamin D deficiency
Peter MF Campbell, Theresa J Allain

This short report looks at the incidence of vitamin D deficiency, which is an important problem in patients who take amiodarone and also in those who avoid sunlight exposure.
November 2006 Br J Cardiol 2006;13:432-3
An unusual presentation of malignant mesothelioma as constrictive pericarditis
Puneet Kakar, Vinay S Sreeguru, Somit Sarkar, Kate A Willmer, William T Berrill

This case report discusses a 54-year-old woman who presented to hospital with recurrent bilateral pleural effusions. She was eventually found to have constrictive pericarditis secondary to malignant mesothelioma. This disease presents a challenge to the physician with considerable difficulties in diagnosis, classification and treatment. This particular presentation of malignant mesothelioma is highlighted in the article.
November 2006 Br J Cardiol 2006;13:434-40
The effectiveness and tolerability of lercanidipine is independent of body mass index or body fat percent. The LERZAMIG study
Vivencio Barrios, Carlos Escobar, Alberto Calderón, Angel Navarro, Luis M Ruilope

This study set out to assess whether the effectiveness and tolerability of lercanidipine for the treatment of essential hypertension in daily clinical practice is affected by body mass index (BMI) or body fat percent (BFP). A total of 2,793 out-patients (mean age 59.8 years) with mild-to-moderate hypertension participated in a multi-centre, prospective, open-label study. All patients received oral treatment over 12 weeks with lercanidipine 10 mg, which was titrated to 20 mg if blood pressure (BP) control was not attained. They were visited at baseline and at four, eight and 12 weeks. BFP was measured by the bioelectrical impedance analysis using an Omron BF-302 body fat monitor. Patients who were overweight or obese were also prescribed a hypocaloric diet. Results showed that, at baseline, sytolic BP was 159.4+/-11.7 mmHg, diastolic BP was 94.5+/-7.5 mmHg, BMI was 30.9+/-8.4 kg/m2, and BFP 27.7+/-6.3%. At 12 weeks, BP was lowered to 138+/-10.1 mmHg (systolic) and 81+/-7.2 mmHg (diastolic) (p<0001). BMI and BFP significantly decreased to 29.3+8 kg/m2 and 27.3+4.1% (p<0.05), respectively, which was most likely to be diet-related. Antihypertensive effectiveness was independent of baseline BMI and BFP values. There was a low incidence of adverse effects (5.5%), with headache (3.4%) and pedal oedema (1.5%) being the most frequent. Some 93% of patients completed the 12-week treatment period. The study showed that lercanidipine is an effective and well tolerated antihypertensive drug in daily clinical practice and its antihypertensive properties are not influenced by BMI and BFP.
September 2006 Br J Cardiol 2006;13:332-37
Lifestyle management of blood pressure
BJCardio editorial team

Lifestyle modifications are an essential initial approach to the management of blood pressure. To review the current evidence in this area, The British Journal of Cardiology recently convened a round table meeting to look at the lifestyle management of raised blood pressure. It considered the role of dietary changes, exercise, alcohol and weight, and ways of changing patients’ behaviour, on blood pressure. The meeting, held at The Royal Society of Medicine, London, and supported by an unrestricted educational grant from Unilever, was attended by investigators involved in the EUROACTION study. EUROACTION is a European Society of Cardiology demonstration project in preventive cardiology which has just been completed in eight countries in both hospital and primary care. It is evaluating whether a nurse-led multidisciplinary team can help patients and families achieve recommended lifestyle and risk factor reduction targets for cardiovascular disease prevention.
September 2006 Br J Cardiol 2006;13:344-5
An unappreciated pioneer in cardiology: Ernest Starling
John Henderson

Most doctors have only heard of Ernest Starling through his law of the heart, although this was not a particularly important part of his research output. Shortly after qualifying in medicine at Guy’s Hospital, London, in 1888 (where he won the university gold medal in medicine), he began investigating the formation of lymph. To explain his findings, he proposed an inward osmotic force at the capillary: the only possible source of this force was the plasma proteins. At the capillary there was a balance between an inward (osmotic) force and an outward (hydrostatic) force. This became Starling’s ‘Filtration Principle’, which, in retrospect, was a paradigm shift in our understanding of the circulation.
September 2006 Br J Cardiol 2006;13:347-50
Should cardiologists be interested in albuminuria?
Clive Weston, Achanthodi Vasudev, Daniel Obaid, Saatehi Bandhopadhay, Jiten Vora

Excretion of excess urinary albumin is a marker of generalised endothelial dysfunction and both progressive renal disease and cardiovascular events in those with and without diabetes; its detection provides a simple way of identifying patients at particularly high risk. Effective management of cardiovascular risk factors and the use of angiotensin II receptor blockers (ARBs) and angiotensin-converting enzyme (ACE) inhibitors have been shown to retard or prevent progression of microalbuminuria to more profound albuminuria. Microalbuminuria can be reversed by such therapy and recently an ACE inhibitor has been shown to prevent the development of microalbuminuria in hypertensive patients with type 2 diabetes. Given the increasing prevalence of type 2 diabetes and the corresponding ascendancy of ensuing cardiovascular disease and renal failure, strict control of multiple risk factors, including microalbuminuria, is to be encouraged.
September 2006 Br J Cardiol 2006;13:353-9
Use of non-steroidal anti-inflammatory drugs does not modify the antihypertensive effect of lercanidipine in essential hypertension
Manuel Luque, Angel Navarro, Nieves Martell

The aim of this study was to assess whether the use of non-steroidal anti-inflammatory drugs (NSAIDs) affected blood pressure control in patients with essential hypertension who were being treated with lercanidipine, a vasoselective dihydropyridine calcium channel blocker. A total of 334 patients (mean [+ SD] age 61+10 years, 51% females) with mild-to-moderate essential hypertension and a history of osteoarthritis received lercanidipine (10 mg/day, up-titrated to 20 mg/day) for four to eight weeks until blood pressure control was achieved. At that point, treatment with NSAIDs (mostly diclofenac and naproxen) was started. Treatment with NSAIDs was maintained for four weeks. At baseline, mean systolic blood pressure (SBP) was 157=/-10 mmHg, diastolic blood pressure (DBP) 92=/-6 mmHg, and heart rate 75=/-9 beats per minute. The administration of lercanidipine was associated with a significant decrease of SBP (to 139=/-9 mmHg) and DBP (to 82=/-7 mmHg) (p<0.001), without changes of heart rate. SBP and DBP readings were not affected by the concomitant use of NSAIDs. Among 156 patients whose blood pressure was well controlled with lercanidipine, 128 (82%) continued to have well controlled SBP and DBP readings. The remaining 28 patients had SBP and DBP > 140 and/or 90 mmHg, but differences in blood pressure between the two groups were not significant. Eight patients (2.3%) had mild side effects and three were withdrawn due to ankle oedema. We conclude that the use of NSAIDs did not significantly modify the antihypertensive effect of lercanidipine in essential hypertension. Therefore, lercanidipine is a useful drug for hypertensive patients with osteoarthritis who require treatment with NSAIDs.
September 2006 Br J Cardiol 2006;13:361-2
Patient satisfaction of the Angina Plan in a rapid access chest pain clinic
Catherine Marie Sykes, Sara Nelson, Kathy Marshall

The aim of this study was to understand patients’ satisfaction with the Angina Plan (AP). Comments from the satisfaction questionnaire help us to understand why patients were satisfied with the AP.
July 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 39–AIC 45
Estimating the risk of percutaneous coronary intervention
Anjan Siotia, Paul Hancock, Julian Gunn

Percutaneous coronary intervention (PCI) is expanding in terms of both the numbers of patients treated and the scope and severity of coronary artery disease tackled. These developments have occurred in parallel with increased awareness of the importance of accountability and clinical governance. Whilst cardiac surgeons have durable risk scores such as Parsonnet and EuroSCORE to assist them and their patients with estimating procedure-related risks, interventionists lack such universally accepted tools. Or do they? In this paper, we review the available PCI risk scores and point out the pressing need for the systematic use of a robust, simple and widely acceptable risk score for routine clinical use.
July 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 46–AIC 47
Double-barrel lumen during recanalisation of a chronically occluded stent in a saphenous vein graft
Jun Tanigawa, Omer Goktekin, Carlo Di Mario

A 73-year-old man who had had a coronary bypass operation 15 years before presented with refractory angina despite full medication seven months after implantation of a 3.0 x 20mm non drugeluting stent in a saphenous vein graft (SVG) to the left circumflex artery.
July 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 48
‘Gatling gun’ stenting of left main stem trifurcation stenosis
Chris Newman, Julian Gunn

A 73-year-old man presented with post-infarct angina. Cardiac catheterisation revealed mildly impaired left ventricular function and high-grade stenoses of the right, left anterior descending, ramus intermedius and left main coronary arteries (RCA, LAD, ramus and LMS respectively).
July 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 49–AIC 56
Current status of non-invasive coronary angiography for the diagnosis of coronary artery stenosis
Kaeng W Lee, Jonathan Panting

Recently, several techniques for non-invasive imaging of the coronary artery have emerged as promising alternatives to conventional coronary angiography for the diagnosis of coronary artery stenosis. Such imaging modalities include magnetic resonance imaging, electron-beam computed tomography and multi-slice computed tomography. With these technologies, images can be acquired rapidly with high temporal and spatial resolution. In their current state of development, non-invasive techniques can reliably be used to visualise significant stenosis of the proximal and mid portions of the coronary tree. However, complete assessment can be hindered by calcification in the vessel wall and by motion artefact.
July 2006 Br J Cardiol 2006;13:257-66
Heart failure in older patients
Robin AP Weir, John JV Mcmurray, Jacqueline Taylor, Adrian JB Brady

As the population ages, so the prevalence of chronic heart failure (CHF) will rise. The majority of CHF patients in the future will be elderly, yet most of our current evidence for the management of this serious condition arises from trials that have largely excluded older patients. As a consequence, older patients who may derive the greatest benefit from treatments known to reduce morbidity and mortality in CHF, are often denied such treatments. The effects on quality of life of both the syndrome of CHF and its treatment in older CHF patients must be borne in mind, as must issues of compliance, prevalence of comorbidity, and requirement for physical and emotional support. We review the current epidemiology of CHF, and focus on the applicability and use of contemporary non-pharmacological and pharmacological therapy to older patients with CHF. The potential use of devices and surgery in older CHF patients is also discussed.
July 2006 Br J Cardiol 2006;13:267-72
Reducing fear and the risk of death in Marfan syndrome: a Chaucerian pilgrimage
Tal Golesworthy, Tom Treasure, Michael Lampérth, John Pepper

Chaucer's characters in The Canterbury Tales meet on their journey to the shrine of Thomas à Becket. They are on a pilgrimage, a special kind of journey that brings a diverse group of people together in a common purpose. As they converge on the place of pilgrimage, the tales they tell are informed by the varied experiences of their lives. The stories we tell here are of individuals brought together by a single objective: to find a solution better than total root replacement for people whose lives are threatened by aortic dilatation due to Marfan syndrome. Chaucer's pilgrims meet in the Tabard Inn in Southwark, where their journey to Canterbury is to begin. This modern journey began in St George's Hospital at the 2000 meeting of the Marfan Association, when the surgeon [TT] told his tale, an account of best current practice and its attendant risks.
July 2006 Br J Cardiol 2006;13:273-7
Safety and tolerability of prolonged-release nicotinic acid combined with a statin in NAUTILUS
Anja Vogt, Ursula Kassner, Ulrike Hostalek, Elisabeth Steinhagen-Thiessen, on behalf of the NAUTILUS Study Group

NAUTILUS (The multiceNtre, open, uncontrolled sAfety and tolerability stUdy of a modified-release nicoTinic acId formuLation in sUbjects with dySlipidaemia and low HDL cholesterol) was an open label, uncontrolled, phase IIIb study. The study population included a total of 566 patients with dyslipidaemia and low high-density lipoprotein (HDL) cholesterol (< 1.0 mmol/L [< 40 mg/dL] in men and < 1.2 mmol/L [< 46 mg/dL] in women) who were inadequately controlled by diet alone. Patients received once-daily treatment with prolonged release nicotinic acid (Niaspan®; target dose 2,000 mg/day), added to existing regimens for 15 weeks. At baseline, 40.5% of patients were receiving an HMG-CoA reductase inhibitor (statin), mostly simvastatin or atorvastatin. Patients taking and not taking concomitant statin therapy reported a similar incidence of all-cause adverse events (AE) of 64.6% vs. 57.9%, respectively, treatment- related AE (54.6% vs. 47.2%), all-cause serious AE (3.9% vs. 3.6%), treatment-related serious AE (0.9% vs. 0.3%), and withdrawals for AE (17.5% in each group). The incidence of flushing was similar in patients with and without statin treatment (45.0% vs. 40.1%), as was the proportion of patients withdrawing because of flushing (8.7% vs. 10.4%). Only about one quarter of patients flushed more than five times. There was no sign of serious hepatic or muscle toxicity. The addition of prolonged-release nicotinic acid markedly raised HDL cholesterol levels irrespective of statin treatment; it was well tolerated and effective when combined with a statin in patients with dyslipidaemia.
July 2006 Br J Cardiol 2006;13:278-82
Safety and tolerability of prolonged-release nicotinic acid in patients aged > 65 years enrolled in NAUTILUS
Anja Vogt, Ursula Kassner, Ulrike Hostalek, Elisabeth Steinhagen-Thiessen, on behalf of the NAUTILUS Study Group

Older patients are often at high risk for cardiovascular disease. Low high-density lipoprotein (HDL) cholesterol is an independent risk factor for cardiovascular disease. Prolonged-release nicotinic acid (Niaspan®) is a once-daily formulation of nicotinic acid with improved tolerability compared with the immediate-release formulation. It may be used to correct low levels of HDL cholesterol. NAUTILUS (the multiceNtre, open, uncontrolled sAfety and tolerability stUdy of a modified release nicoTinic acId formuLation in sUbjects with dySlipidaemia and low HDL cholesterol) evaluated prolonged-release nicotinic acid at doses of up to 2,000 mg/day once daily in 566 patients, of whom 33.6% were aged > 65 years. A similar incidence of adverse events (AE) was observed following 15 weeks of prolonged-release nicotinic acid treatment in older vs. younger patients for all-cause AE (55.3% vs. 63.3%) and for treatment-related AE (46.3% vs. 52.1%). Most AE were related to flushing, which also occurred at similar frequency in older and younger patients (39.5% vs. 43.4%). Gastrointestinal AE were the most common AE apart from flushing, and occurred in 12.1% of older patients and 14.4% of younger patients. Serious AE were uncommon. There was no hepatotoxicity or serious muscle toxicity. Marked improvements in indices of atherogenic dyslipidaemia were observed (increases from baseline in HDL cholesterol of 26% in older and 21% in younger patients and decreases in triglycerides of 16% and 9%, respectively). Prolonged-release nicotinic acid is well tolerated and effective in older patients, and is suitable for correction of low HDL cholesterol in this population.
July 2006 Br J Cardiol 2006;13:283
Palliative care in heart failure – a neglected area in specialist training?
Yasmin Ismail, Elizabeth McNeill, Mandie Townsend, Thomas MacConnell

Heart failure has a comparable prognosis to many cancers and accounts for approximately 4% of deaths in the UK. Despite its poor prognosis, few patients have access to specialist palliative care services. The National Institute for Health and Clinical Excellence (NICE) acknowledges that the palliative care needs of patients with heart failure and their informal carers are not currently being met. Its recently published guidance recommends the development of an effective multidisciplinary service model for such patients.
July 2006 Br J Cardiol 2006;13:284-86
Should acute MI patients receive dual antiplatelet therapy: a review of new data
Anthony Gershlick

Thrombolytic therapy in the management of acute myocardial infarction (MI) shows true evidence of benefit. Administration of a thrombolytic saves about 30 lives per 1,000 in those presenting within six hours of symptom onset but only 20 lives per 1,000 when patients receive treatment between six and 12 hours after symptom onset. After 12 hours there appears to be only a small and statistically uncertain benefit. The aim in thrombolysis should be to increase the number of patients who achieve TIMI grade 3 flow as soon as possible after the occlusive event. Additional benefit in improving thrombolysis, particularly in reducing 30-day mortality, has been shown by adding the antiplatelet agent, aspirin, to thrombolytic therapy. The addition of a second antiplatelet agent, such as clopidogrel, has been shown to be of benefit in other, less immediately severe atherothrombotic manifestations (unstable angina and non-ST-elevation MI) and looks to be a promising development in the management of acute ST-elevation MI. The potential advantages of dual antiplatelet therapy in this setting, investigated in the recently published CLARITY study, are discussed.
July 2006 Br J Cardiol 2006;13:289
So where is the heart?
Amit Kj Mandal, Elizabeth Mc Ashley, David Ward, Constantinos G Missouris

A 75-year-old gentleman presented to his general practitioner with palpitations and dizziness. A 24-hour Holter monitor confirmed the diagnosis of paroxysmal sustained atrial flutter and episodes of less organised rhythm, that were thought to be atrial fibrillation. His symptoms failed to improve on combination treatment with digoxin and bisoprolol. He was referred for flutter ablation. Our aim was to replace the above pharmacological agents with a class 1C drug. The patient was not taking warfarin. A transoesophageal echocardiogram (TOE) was therefore arranged to exclude left atrial thrombus, prior to performing the ablation.
July 2006 Br J Cardiol 2006;13:290-1
Spontaneous resolution of in-stent restenosis
Sayqa Arif, Jasper Trevelyan, Rajiv Gulati, Peter F Ludman

In 1993, a 61-year-old man underwent balloon angioplasty to the left anterior descending artery (LAD) after an anterior myocardial infarction. Repeat angiography in 1997 after a recurrence of symptoms revealed a severe proximal LAD stenosis, and this was again treated by balloon angioplasty. Two months later, the LAD had occluded and a 16 mm bare stainless steel stent (Nir®) was implanted with a 3 mm balloon (figure 1). Four months afterwards, angiography revealed severe in-stent restenosis (figure 2) and he was referred for coronary artery bypass grafting; the left internal mammary artery (LIMA) was grafted to the LAD. He remained symptom-free for six years until 2004, when his angina recurred. Repeat coronary angiography demonstrated spontaneous regression of the previously stenosed LAD stent, which was now widely patent (figure 3). The LIMA graft had involuted. A new stenosis in a large obtuse marginal branch was treated with a drug-eluting stent.
July 2006 Br J Cardiol 2006;13:293-6
Graduating to a higher level: national cardiology training for practitioners with a special interest
Catherine Burwell

This article describes the evaluation of a new postgraduate diploma in cardiology course run by the Bradford City Teaching Primary Care Trust.
July 2006 Br J Cardiol 2006;13:297-300
How well informed are general practitioners about management strategies to improve the prognosis of heart failure?
Archana Rao, John Walsh, David Gray

Heart failure is a common condition, characterised by poor prognosis. Despite evidence that effective treatment improves symptoms and prognosis, management remains sub-optimal. General practitioners (GPs) have a key role in the assessment and treatment of patients with heart failure. This study was designed to ascertain the knowledge and attitude of GPs towards the management of heart failure. Anonymised questionnaires were sent to 355 GPs in the Nottingham area in May 2003 and 227 (64%) responded. The mean (standard deviation) age of respondents was 45 (7) years and they had been in general practice for 15 (7.6) years. The questionnaires found that 223/227 (98%) of GPs were aware that angiotensin- converting enzyme (ACE) inhibitors have been shown in clinical trials to reduce mortality in heart failure; 155/224 (69%) were aware that beta blockers reduced mortality in heart failure; 53/225 (23.3%) believed diuretics improved prognosis. Almost 60% routinely initiated ACE inhibitors but 26% expressed concerns about their side effects and so were less likely to initiate this treatment. Most GPs seemed able to manage heart failure effectively and ACE inhibitor prescription for patients with chronic heart failure (CHF) is now well established within primary care. Knowledge and prescription rates for the remaining effective therapies remain low.
May 2006 Br J Cardiol 2006;13:185-90
Portable echocardiography: a review
Roxy Senior, John Chambers

Miniaturisation of machines has allowed echocardiography to be performed in the community as well as anywhere in the hospital. It has led to an expansion of the types of study performed: ultrasonic stethoscope, screening and focused studies, and standard echocardiograms. In expert hands, results compare favourably with standard studies on full systems. With focused studies, abnormalities may be missed in areas of the heart that are not imaged. For screening studies, the negative predictive accuracy is high while the positive predictive accuracy is lower. Portable echocardiography can save time and costs, but it is essential that studies are requested and performed within a tightly controlled clinical setting. Operators should be trained appropriately and be part of a broad echocardiography service that includes quality control, continuing education and expert supervision.
May 2006 Br J Cardiol 2006;13:191-4
Familial hypercholesterolaemia in children
D Paul Nicholls

Familial hypercholesterolaemia (FH) affects about one in 500 in the UK population. There are no symptoms or signs of raised cholesterol in children and so individuals can only be identified by screening, usually as a 'cascade' from known probands. Once identified, such children should be treated to prevent premature atherosclerosis.
May 2006 Br J Cardiol 2006;13:196-202
Cost-effectiveness of rosuvastatin, atorvastatin, simvastatin, pravastatin and fluvastatin for the primary prevention of CHD in the UK
Andrew Davies, John Hutton, John O'donnell, Sarah Kingslake

The effectiveness of rosuvastatin in improving lipid measurements and achieving guideline target levels in patients has been demonstrated in short-term randomised clinical trials. The Framingham Heart Study has provided some of the strongest evidence in establishing the relationship between risk factors such as smoking, hypertension and cholesterol and events from cardiovascular disease and subsequent mortality. Using Framingham risk equations for coronary heart disease, we used a Markov model to extrapolate beyond short-term trial evidence to calculate the cost-effectiveness of cholesterol-lowering therapy in 55-year-old men and women, with an initial total cholesterol: high-density lipoprotein cholesterol (TC:HDL) ratio of 5.5 and an untreated expected survival (under adjusted Framingham risk equations) of 17 years (men) and 19 years (women). After titration, cholesterol-lowering therapy reduced the weighted average TC:HDL ratio to 3.4 (rosuvastatin), 3.7 (atorvastatin), 3.9 (simvastatin), 4.1 (fluvastatin) and 4.2 (pravastatin). In comparison with no treatment, rosuvastatin produced the greatest health gain (0.71 quality-adjusted life-years [QALYS]) and pravastatin the smallest (0.42). In the base case analysis, rosuvastatin dominated atorvastatin and delivered additional benefits at the cost of £9,735 per QALY for men in comparison with generic simvastatin. Sensitivity analysis showed a high probability of rosuvastatin being cost-effective under conditions of uncertainty.
May 2006 Br J Cardiol 2006;13:205-208
Do fibrates offer special benefits in treating diabetic dyslipidaemia? Lessons from FIELD
Hugh F McIntyre

Although levels of total cholesterol are similar between populations with and without diabetes, there are important differences in lipid sub- fractions, with diabetic dyslipidaemia characterised by reduced levels of high-density lipoprotein (HDL) cholesterol and elevated triglycerides. In addition, small, dense, low-density lipoprotein (LDL) particles may increase atherogenicity. These differences may account for the increased vascular risk reported in diabetic populations. The benefit of HMG Co-A reductase inhibitors, primarily through LDL cholesterol reduction, has been demonstrated in populations with ischaemic heart disease. Fibrates are synthetic activators of the a subclass of the peroxisome proliferator-activated receptor (PPAR), and are reported to raise HDL cholesterol and lower triglyceride levels preferentially. The FIELD study was designed to assess whether the theoretical benefit offered by fibrates in diabetic dyslipidaemia was reflected in improved cardiovascular outcomes.
May 2006 Br J Cardiol 2006;13:209-11
The ‘wicked problem’ of the cardiology clinic
Usha Rao, Paul Hocking, Jonathan Goodfellow, Christopher Jh Jones

A major concern in cardiology in the UK has been the waiting times for patients referred from primary care to secondary care, which are often long. We have addressed this problem in our Trust. At various times the Trust had funded waiting list initiative clinics but, apart from small and transitory improvements, the situation continued to worsen. Various solutions to the out-patient services problems have been implemented. However, there is a lack of published information about system redesign. In this article we present some of the principles we are currently employing to redesign our out-patient service with a view to improve its efficiency. Our results are being published separately.
May 2006 Br J Cardiol 2006;13:213-5
Cardiac angiosarcoma presenting with death due to cardiac perforation
Ayyaz Sultan, Ahmed Amour, Sarfraz Khan

Cardiac angiosarcomas are malignant tumours that are rare, often with non-specific symptoms. They almost always have a rapid and fatal evolution, making diagnosis challenging. Therapeutic approaches include surgery, chemotherapy and radiotherapy alone, or in combination, but because the tumour is rare there are no randomised studies to guide treatment. Management is, therefore, usually individualised and often multidisciplinary.
May 2006 Br J Cardiol 2006;13:216-8
The accuracy of ECG screening by GPs and by machine interpretation in selecting suspected heart failure patients for echocardiography
Sanjay Jeyaseelan, Allan D Struthers, Barclay M Goudie, Stuart D Pringle, Frank M Sullivan, Peter T Donnan

National Institute for Health and Clinical Excellence (NICE) guidelines in the UK state that suspected heart failure patients should have an ECG in order to select patients for echocardiography. The research underpinning this recommendation comes from studies in which cardiologists interpreted the ECGs. In practice, however, it would be general practitioners (GPs) interpreting ECGs. The aims of this study were to assess both GPs and ECG machine interpretation in their ability to use ECGs to select suspected heart failure patients for echocardiography. Six GPs were asked to classify 90 ECGs taken from suspected heart failure patients either as normal or as having an abnormality present. The ECG machine report was also used to classify the ECG in the same way. These results were compared to a gold standard interpretation. The GPs and the ECG machine report would have not referred 17.8% and 8.3%, respectively, of the appropriate patients for echocardiography. In doing so, the GPs would have missed 5.6% of patients with left ventricular systolic dysfunction (LVSD) whereas the ECG machine report would have missed none. We conclude from our findings that there is heterogeneity between GPs in their interpretational skills. Some GPs could successfully use ECGs to select patients for echocardiography. The difference in cost between performing echocardiography on all patients and GPs screening with ECGs is £74 more per case. Screening with ECG machine interpretation costs virtually the same as performing echocardiography on all patients.
May 2006 Br J Cardiol 2006;13:220-4
Anxiety, depression and myocardial infarction: a survey of their impact on consultation rates before and after an acute primary episode
Everard W Thornton, Peter Bundred, Michelle Tytherleigh, Ann DM Davies

The study documents general practitioner (GP) consultations before and after a primary, acute myocardial infarction (MI) and examines how these relate to psychological distress. Data were derived from the numbers and category of consultations and their outcome, documented from medical records of 194 patients with a primary acute MI over a two-year period pre-MI and a six-month period post-MI. Objective measures of anxiety and depression were collated using the Hospital Anxiety and Depression Scale in four phased assessments over a six-month period following the MI. There was a high probability of consultation for cardiovascular and psychological symptoms before a MI. Post-MI, almost all patients receive an early consultation: high consultation rates continue for cardiovascular concerns but they are relatively low for psychological issues. However, questionnaire responses indicated a substantial minority of patients with clinical or borderline clinical levels of anxiety (30%) and depression (20%) post-MI. Patients are willing and able to make demands on their GPs post-MI, but not for psychological issues despite evidence of high levels of anxiety and depression; patients may be too accepting of distress. While GPs advise and are prepared to provide drug treatment for psychological concerns, they did not make referral for psychological support.
March 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 9–AIC 12
Percutaneous coronary intervention of the right ventricular artery: is it worth the effort?
David R Ramsdale, Robert Lowe

Loss of the right ventricular artery (RVA) is generally thought to be of little consequence. Nonetheless, reperfusion can enhance right ventricular recovery and improve the clinical condition. Five cases of percutaneous coronary intervention involving right ventricular branches are presented. We advocate a more positive approach to a significant stenosis in the RVA in patients who have stable or unstable angina or non-ST segment elevation myocardial infarction. Re-establishment of flow should limit ischaemia and infarction of the right ventricle and limit their adverse effects.
March 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 13
Bilateral coronary fistulae
Andrew J Turley, Ananthaiah Shyam-Sundar, Mark A de Belder

A 69-year-old woman was referred for cardiac catheterisation following a positive exercise tolerance test.
March 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 14–AIC 18
Percutaneous closure of coronary artery fistulae: is it time for a UK registry?
Alex Hobson, Nick Chalmers, Nick Curzen

Most coronary artery fistulae are asymptomatic but there may be complications such as rupture and myocardial infarction. Percutaneous intervention is an attractive alternative to open surgical repair that offers lower procedural risk. Increasing numbers of fistulae are being discovered incidentally during angiography. They present challenges in assessment and management. For example, there is poor correlation between symptoms and the size and flow rate of fistulae.
March 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 19–AIC 21
Near-patient testing for cardiac troponin I to reduce hospital stay in patients presenting with chest pain
Turab Ali, Jane Scrafton, Richard Andrews

Minimising the in-hospital stay of patients with chest pain, within safe limits, is crucial in reducing the cost of health care. The aim of this study was to determine whether the use of near-patient testing for cardiac troponin I could reduce the duration of in-hospital stay for patients presenting with chest pain who were considered to be at low risk of death or myocardial infarction. This prospective observational study of consecutive patients admitted with chest pain of possible cardiac origin was conducted in a medium-sized district general hospital. A near-patient system for troponin I analysis was compared to traditional laboratory-based troponin I analysis to assess any effect on duration of in-hospital stay in low-risk chest pain patients. Of the 295 patients enrolled in the study, 191 (68.7%) were troponin-negative and were classified as having chest pain of non-cardiac origin or cardiac pain at low risk of major adverse events. The introduction of near-patient testing for cardiac troponin I reduced the mean duration of hospital stay from 30.04 hours to 17.10 hours (p<0.001). At 30-day follow-up no deaths or myocardial infarctions had occurred.
March 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 22–AIC 25
Percutaneous cardiopulmonary support for circulatory assistance during angioplasty in a patient with Friedreich’s ataxia
Guido Materazzo, Davide Ghitti, Marco Rossi, Giuseppe Nasso, Paola Spatuzza, Carlo Maria De Filippo, Pietro Modugno, Amedeo Anselmi, Francesco Alessandrini

The case of a 70-year-old-woman affected by Friedrich's ataxia (FRDA), unstable angina and heart failure with left main 'equivalent' lesions is presented. As the patient was in need of revascularisation but would have been at high risk with coronary artery bypass grafting surgery, she underwent coronary angioplasty assisted with percutaneous cardiopulmonary support (PCPS). Despite the onset of temporary complications, the procedure was performed successfully. On the basis of this case and of a review of pertinent literature, the authors discuss the role of PCPS in high-risk patients, with respect to its indications and performance technique.
March 2006 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 26–AIC 28
Successful use of biventricular pacing to facilitate weaning from mechanical ventilation in a patient with severe left ventricular failure
Parind Patel, Jonathan Clague, Jeremy Cordingley

Biventricular pacing is increasingly used in the management of severe heart failure. We report the successful use of biventricular pacing to aid weaning from mechanical ventilation in a patient with severe left ventricular dysfunction.
March 2006 Br J Cardiol 2006;13:102-4
2005 BJCA survey of cardiology trainees
Saul Myerson

The second annual survey from the British Junior Cardiologists’ Association (BJCA) has new data on several areas, including the European Working Time Directive, modernising medical careers, and careers in academic cardiology. The surveys are becoming a strong and influential voice in cardiology. Last year’s survey was noted by many national bodies, including the British Cardiac Society (BCS) and the Royal College of Physicians. Over a third of BJCA members responded to this year’s survey and Dr Saul Myerson, BJCA President, highlights some of this year’s trends.
March 2006 Br J Cardiol 2006;13:113-20
A new therapeutic target: the CB1 receptors of the endocannabinoid system and visceral fat
Colin Waine

A constant abundance of food and a sedentary lifestyle has led to an increasing prevalence of obesity in the United Kingdom. This has resulted in a serious public health problem as obesity, in particular the presence of excess abdominal (visceral) fat, is associated with a high risk of cardiovascular disease, type 2 diabetes and the metabolic syndrome. Managing obesity by lifestyle changes alone has met with only limited success, so pharmacological intervention is often necessary to help patients reduce their cardiometabolic risk profile. The recent discovery of the role of the CB1 receptors of the endocannabinoid system, and how these receptors influence appetite and energy storage, has led to the development of promising new approaches to the management of obesity. This review charts the background to the development of novel antagonists (CB1 blockers) directed against the CB1 receptors and briefly summarises the available phase III data. The available phase III data suggest that CB1 blockers could have a major role to play in the management of multiple cardiovascular risk factors, by reducing visceral fat and directly improving lipid and glucose metabolism and insulin resistance.
March 2006 Br J Cardiol 2006;13:123-8
Minimally invasive cardiac surgery
Joanna Chikwe, James Donaldson, Alan J Wood

We summarise recent developments in minimally invasive cardiac surgery. We describe the modifications to anaesthetic technique, incisions, cardiopulmonary bypass and myocardial protection, and the endoscopic and robotic adjuncts that permit coronary artery surgery, valve repair and replacement, and repair of descending aortic aneurysms to be successfully carried out. The results for such surgery are summarised and compared to conventional open techniques as well as percutaneous procedures.
March 2006 Br J Cardiol 2006;13:131-6
The failure of LDL cholesterol reduction and the importance of reverse cholesterol transport. The role of nicotinic acid
H Robert Superko

Low-density lipoprotein cholesterol (LDL-C) reduction alone has consistently achieved a statistically significant 25–30% reduction in clinical events in multiple clinical trials. This degree of clinical benefit is inadequate, however, to stem the tide of coronary artery disease. A focus on low-density lipoprotein (LDL) reduction alone reduces the rate of coronary atherosclerosis progression but leaves a large number of patients experiencing clinical events despite adequate LDL-C control. One major contributor to coronary atherosclerosis that is not improved with LDL reduction is high-density lipoprotein (HDL) and reverse cholesterol transport. Clinical trials funded by the US National Institutes of Health (NIH) have demonstrated that a combination of LDL reduction and HDL increase can achieve better clinical and arteriographic outcomes compared to LDL reduction alone. HDL heterogeneity helps to explain differences in the efficiency of reverse cholesterol transport. This process can be enhanced through appropriate diet, loss of excess body fat and physical activity. Nicotinic acid and fibric acid derivatives can enhance reverse cholesterol transport and have been used in multiple clinical trials. The combination of nicotinic acid and a statin drug are particularly beneficial in NIH-sponsored clinical trials. The HDL increase induced by nicotinic acid is primarily HDL2. By combining a two-staged LDL-C reduction and HDL-C raising strategy, improved clinical outcomes can be achieved for patients with coronary artery disease.
March 2006 Br J Cardiol 2006;13:138-40
Perceptions of healthcare staff in relation to referral for cardiac rehabilitation
Ali Yalfani, Abebaw M Yohannes, Patrick Doherty, Jean Brett, Christine Bundy

Referral to cardiac rehabilitation (CR) is often incomplete. Those most likely to benefit are less likely to be offered the service and there has been little systematic exploration of the reasons for this situation in the UK. The purpose of this study was to investigate CR staff perceptions in relation to aspects of referral to CR programmes. In a prospective cross-sectional study, a 24-item questionnaire regarding perceptions of referrals was mailed to 115 referring staff of 23 CR out-patient programmes in the North West of England. The response rate was 85 (74%). The most common factors cited for low referrals were: funding limitation 57 (67%), limited facilities 56 (66%), shortage of trained staff 51 (60%) and patients" poor physical ability 50 (59%). Fifty-three (62%) respondents suggested participation would increase if CR were offered by a medical practitioner. Sixty-one (72%) respondents felt they provided CR according to recommended guidelines. Seventy-nine (93%) of the respondents agreed CR was necessary or appropriate for most cardiac patients and 76 (89%) reported CR offered more to patients than secondary prevention. The study concludes that CR programmes should be audited better and physicians need to be more actively involved in recruiting patients to programmes. Better funding is required to increase facilities and staff training to improve referral of patients.
March 2006 Br J Cardiol 2006;13:141-3
Does site matter?
Aravind Rengarajan, Krishna Adluri, Graham Perks, Inderpaul Birdi

Cardiac catheterisation access site complications are common. Their incidence depends on various risk factors such as female gender, nadir platelet count, diagnostic versus therapeutic intervention, excessive anticoagulation and so on. Thrombotic complications are common at the brachial site and haemorrhagic complications are more common at the femoral site. In spite of new devices for securing haemostasis, the incidence of these complications has not decreased. We report the case of a 71-year-old, obese woman who died secondary to femoral access site haemorrhage despite all surgical attempts. This case emphasises the need for a tailor-made approach for deciding the site of access.
March 2006 Br J Cardiol 2006;13:145-52
The ‘rule of halves’ still applies to the management of cholesterol in cardiovascular disease: 2002–2005
Simon de Lusignan, Nigel Hague, Jonathan Belsey, Neil Dhoul, Jeremy van Vlymen

The current national target in the UK for total cholesterol is 5 mmol/L. The Primary Care Data Quality (PCDQ) programme reported in 2002 that only 50% of patients with coronary heart disease (CHD) achieved the 5 mmol/L target and we report on progress since then. Routinely collected general practice computer data were extracted in two successive data collections in 2003 and 2004/05 and analysed. The standardised prevalence of CHD recorded in GP computer systems rose from 3.8% to 4.0% from 2002 to 2004/5. In patients with CHD, cholesterol recording rose from 47.6% to 89.0%, the percentage of patients receiving a statin rose from 49.4% to 71.5% and mean cholesterol levels fell from 5.18 to 4.67 mmol/L. The proportion of CHD patients with a cholesterol recording achieving the 5 mmol/L target increased from 44.7% to 67.7%. Overall, 53.1% of patients with cardiovascular disease had total chol-esterol below 5 mmol/L. Patients with CHD achieved better cholesterol control than those with stroke (4.87 mmol/L) or peripheral vascular disease (PVD) (4.79 mmol/L) and a higher percentage of patients achieved the 5 mmol/L target (60.1% versus 43.3% and 49.9% respectively). There remains scope for improved management of cholesterol in primary care and greater efforts are needed to see that more patients with cardiovascular disease benefit from best practice.
March 2006 Br J Cardiol 2006;13:154-6
Evaluation of post-MI patient diaries show concerns
Shirley Russell, Michael Kirby

The British Heart Foundation (BHF) diary has been designed to be a personal record for patients post-myocardial infarction (MI) to record their progress, keep a record of their condition, provide guidance on services and basic information on medication and risk factors, and to provide pages that the patient can use to manage their condition.
January 2006 Br J Cardiol 2006;13:27-35
Pure heart rate reduction: the If channels from discovery to therapeutic target
Michael Shattock, A John Camm

Studies indicate that increased heart rate is a risk factor for ischaematic cardiac events; accordingly heart rate reduction may improve outcome. Beta blockers and some calcium channel blockers reduce heart rate but their use may be limited by negative inotropic effects and several contraindications. Ivabradine, a selective sinus node If channel inhibitor, represents a therapeutic innovation in the treatment of ischaemia. Preclinical and early clinical studies show that ivabradine can reduce heart rate without affecting cardiac systolic function, suggesting that If inhibition may be an effective approach to minimise both angina and the underlying ischaemia. In clinical studies ivabradine has anti-anginal and anti-ischaemic effects in patients with stable angina and has comparable efficacy to atenolol and amlodipine. This anti-ischaemic effect is also observed in elderly patients in whom there is a greater incidence of stable angina. Furthermore, the absence of additional cardiac effects associated with If inhibition suggest that this approach may be effective in other patient groups, such as those at risk of acute coronary events or compromised left ventricular function. Further clinical trials with ivabradine to evaluate fully the therapeutic potential of If inhibition are ongoing.
January 2006 Br J Cardiol 2006;13:36-41
Meeting the NSF targets for door-to-needle time in acute myocardial infarction – the role of a bolus thrombolytic
Velmurugan C Kuppuswamy, Daniela Webbe, Sandeep Gupta

Coronary heart disease (CHD) remains the leading cause of premature death in the United Kingdom. The mortality from myocardial infarction (MI) can be reduced by reperfusion of the infarct-related artery with thrombolytic agents.2,3 The best results for survival are achieved in those patients who are thrombolysed early.4,5 We set out to investigate whether the time between arrival to hospital of a patient with acute MI and administration of thrombolytic therapy (door-to-needle time) could be improved by the introduction of a bolus thrombolytic in the accident and emergency (A&E) department in a busy inner city hospital. This study of 13 months’ duration compared the door-to-needle times and the proportion of patients thrombolysed within 30 minutes before and after the introduction of a bolus thrombolytic agent – reteplase. The findings demonstrated a 37% reduction in door-to-needle time (from 27 minutes to 16 minutes) and a 22% improvement in the proportion of patients thrombolysed within 30 minutes (from 68% to 86%) with reteplase. Our findings suggest that bolus thrombolytic agents such as reteplase can be used in a strategy to meet the National Service Framework (NSF) targets for door-to-needle time.
January 2006 Br J Cardiol 2006;13:44-6
New perspectives for cardiology from chaos theory
David Kernick

Converging from a number of disciplines, non-linear systems theory and, in particular, chaos theory, offers new descriptive and prescriptive insights into physiological systems that may more accurately reflect underlying mechanisms. This paper describes the implications of these new perspectives and briefly outlines how they might be applied to the study of cardiology.
January 2006 Br J Cardiol 2006;13:47-50
Application of the Duke’s treadmill score to a rapid access chest pain clinic
Oliver Gosling, Cyrus Daneshvar, Nicholas Bellenger, Matthew Dawes

In an observational study, we sought to determine the effect of applying the Duke’s treadmill score on patient assessment and prioritisation to coronary angiography waiting lists within a rapid access chest pain clinic in a UK district general hospital. After attending the rapid access chest pain clinic, patients requiring subsequent coronary angiography were placed on either an urgent or a routine waiting list. We determined the number of patients subsequently shown to have severe coronary artery disease (left main stem or three-vessel disease) in both waiting lists. We then assessed the effect of applying the Duke’s treadmill score retrospectively on these patients to produce regraded waiting lists (urgent and routine); these were compared with the actual lists generated clinically. The actual urgent list had 43/111 (39%) patients with severe disease; the actual routine list had 28/98 (29%) patients with severe disease (p=NS). Application of the Duke’s treadmill score to produce re-graded lists reduced the total number of patients on the urgent list from 111 to 68. Thirty-three of 68 (49%) patients on the Duke’s treadmill score urgent list had severe disease compared to 43/111 (39%) on the actual urgent waiting list. Specificity for allocating patients with severe disease to the urgent waiting list improved from 50% to 75% by application of the Duke’s treadmill score compared with the clinically generated list. Thus, the Duke’s treadmill score could be used in a rapid access chest pain clinic to prioritise patients objectively for cardiac catheterisation in a resource-limited system.
January 2006 Br J Cardiol 2006;13:53-5
National survey of the level of nursing involvement and perceived skills and attributes required in cardiac rehabilitation delivery
Morag K Thow, Danny Rafferty, Janet Mckay

The Scottish Intercollegiate Guidelines Network (SIGN) 2002 acknowledge the multiprofessional membership of cardiac rehabilitation (CR) teams required to deliver comprehensive CR. The clinical groups chiefly involved in delivering CR in the UK are nurses followed by physiotherapists. The participation, skills and attributes of physiotherapists in the UK have already been identified. This paper reports on the findings of a similar survey for nurses. The survey was piloted and then sent to all registered centres on the British Association for Cardiac Rehabilitation (BACR) and the Scottish CR Interest Group databases (CRIGS).
January 2006 Br J Cardiol 2006;13:56-7
Getting a sense of listening: an anthropological perspective on auscultation
Tom Rice, John Coltart

In his contribution to The auditory culture reader, Murray Schafer introduces the notion of clairaudience. Clairaudience refers, most fundamentally, to an ability to hear and, more specifically, to a capacity to hear ‘through’ or ‘beyond’ the sensory horizons which normally present themselves. This is a very suitable concept through which to consider the ear of an experienced auscultator. Not only is he or she able to hear through the layers of tissue which constitute the body and which usually contain sound, rendering it inaudible, but the auscultator is also able to infer what certain sounds might mean and what significance they might hold for a patient’s well-being in the present and future. The auscultator is able to deduce the relevance of sounds which are ‘unheard’ to the patients, and which remain incomprehensible to those not trained in medicine. An experienced auscultator holds a very particular sensory power.
January 2006 Br J Cardiol 2006;13:58-61
Alcohol septal ablation for hypertrophic obstructive cardiomyopathy: how and when?
Elliot J Smith, Ajay K Jain, Charles J Knight

Alcohol septal ablation is a percutaneous alternative to surgical myotomy-myomectomy for symptomatic patients who have hypertrophic cardiomyopathy (HCM) and left ventricular outflow tract (LVOT) obstruction. In the 11 years since its inception, the procedure has been proven safe and effective. While septal ablation may be more acceptable to patients than surgery, it lacks the long-term safety record of myotomy-myectomy. Here we discuss the mechanics of the procedure itself and examine its place in clinical practice, highlighting the importance of appropriate patient selection.
January 2006 Br J Cardiol 2006;13:62-4
Alcohol septal ablation: the first patient in 1994
Joshua A Vecht, Rekha Dave, Romeo J Vecht

Pathological findings compatible with hypertrophic obstructive cardiomyopathy (HOCM) were first described in the nineteenth century by the French pathologists, Hallopeau and Liouiville. However, it was not until 1958 that Teare recognised the condition as a separate entity; Goodwin named it HOCM in 1960.
January 2006 Br J Cardiol 2006;13:66-70
Heart disease prevention – what place for the glitazones?
Michael Kirby

This paper considers the role for glitazones in the treatment of type 2 diabetes following publication of the PROactive study, the first major outcome study with this class of agents. The macrovascular benefits of glitazones are discussed. Recent guidance for glitazone prescribing from the Association of British Clinical Diabetologists is also given.
January 2006 Br J Cardiol 2006;13:72-6
Achieving lipid goals in real life: the DISCOVERY-UK study
Alan Middleton, Ahmet Fuat

DISCOVERY-UK (the DIrect Statin COmparison of LDL-C Values: an Evaluation of Rosuvastatin therapY) was an open-label, parallel-group, multicentre study designed to compare the efficacy of recommended start doses of rosuvastatin with atorvastatin and simvastatin for reduction of low-density lipoprotein cholesterol (LDL-C) and goal attainment.
Patients with type IIa or type IIb hypercholesterolaemia and a 10-year coronary heart disease (CHD) risk > 20% or a history of CHD or other established atherosclerotic disease were randomised to receive rosuvastatin 10 mg, atorvastatin 10 mg or simvastatin 20 mg for 12 weeks.
Significantly greater LDL-C reductions were observed with rosuvastatin 10 mg compared with atorvastatin 10 mg and simvastatin 20 mg (50% versus 42% and 40%, both p<0.0001). The 1998 European goal (LDL-C < 3.0 mmol/L) was achieved by 89% of patients receiving rosuvastatin 10 mg, which was significantly more than patients receiving atorvastatin 10 mg (78%) and simvastatin 20 mg (72%) (both p<0.0001). Similar results were observed for the National Cholesterol Education Program Adult Treatment Panel III goal (LDL-C < 2.6 mmol/L) and 2003 European goals (LDL-C < 3.0 or < 2.5 mmol/L, depending on risk category).
In conclusion, rosuvastatin is more effective than atorvastatin or simvastatin for lowering LDL-C and enabling patients to achieve lipid goals at recommended start doses.
November 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 92–AIC 97
The ‘no-reflow’ phenomenon
Lucy Blows, Divaka Perera, Simon Redwood

Microvascular perfusion is considered a key factor with respect to preservation of left ventricular function and prognosis. No-reflow is recognised in the context of acute coronary syndromes and percutaneous intervention: myocardial blood flow at a tissue level remains impaired following restoration of epicardial flow. Once no-reflow is established, treatment is often ineffective and this phenomenon is associated with poor short- and long-term outcomes. A number of different pharmacological agents are used to prevent and treat this condition although data to support their use are limited. This article examines the pathophysiological aspects of this condition, its clinical correlates and proposed management strategies.
November 2005 Br J Cardiol 2005;12:471-6
Hypertension – its detection, prevalence, control and treatment in a quality driven British general practice
Peter Standing, Helen Deakin, Paul Norman, Ruth Standing

This study evaluated primary care hypertension management against UK quality targets and prescribing guidelines through a survey of 738 hypertensives in an urban three-partner personal list practice in April 2005. It looked at screening rates, prevalence, blood pressures of under 150/90 mmHg, measurement bias, ABCD prescribing and cost. The survey found that 94% of adults aged 25–79 years had been screened. With 738 confirmed cases, prevalence was 11.7% for all ages; 14.4% for those aged more than 16 years; and 46% in those over 65 years of age. Some 442 patients had ‘potential’ hypertension with their last blood pressure measurement being greater than 140/90 mmHg but inadequate follow-up. Blood pressure control of less than 150/90 mmHg was achieved in 83% of hypertensives with a six-fold terminal zero measurement bias. Looking at ABCD agents, 1,186 had been prescribed (1.84 per patient) costing £129,100 per annum. We believe that QOF hypertension prevalence in the practice (11.7%) and England (11.3%) is less than half the rate reported from community surveys. The practice demonstrated that QOF outcome targets are achievable by improving blood pressure targets to under 150/90 mmHg from 52% of patients in 2002 to 83% of patients by April 2005. Practice organisation, personal patient lists and quality targets were important factors in delivering successful care. Automated blood pressure measurement could eliminate observer bias. Restructuring therapy repeat instructions to include ABCD data encourages logical prescribing.
November 2005 Br J Cardiol 2005;12:468-70
How well do primary care teams identify patients with CHD and diabetes?
Debbie A Lawlor, Rita Patel, Shah Ebrahim

How well do primary care teams identify patients with CHD and diabetes? The British Women’s Heart and Health Study, a prospective cohort study, suggests that as many as half the women identified as having CHD on practice registers (and almost one third of diabetics) appear not to have the condition after a detailed manual review of records. The importance of auditing practice registers is highlighted.
November 2005 Br J Cardiol 2005;12:465-7
Myocardial calcification following post-operative septicaemia
Jeban Ganesalingam, Sanjay Prasad, Paul J Oldershaw

Myocardial calcification is a rare finding usually detected by computerised tomographic (CT) scanning. It is often missed and, when found, is often misdiagnosed. The addition of magnetic resonance imaging (MRI) to our investigative armamentarium enables correct diagnosis and appropriate management(October 2002). She underwent coronary angiography, which showed normal coronary arteries but significant left ventricular impairment. She continued to be managed medically for ventricular dysfunction.
November 2005 Br J Cardiol 2005;12:459-64
Gender difference in health-related needs and quality of life in patients with acute chest pain
Mohsen Asadi-Lari, Chris Packham, David Gray

Inequalities in health care between men and women have been described extensively with regard to access to diagnostic and therapeutic procedures. These inequalities affect coronary heart disease care. Although survival rates differ for men and women following a myocardial infarction, this alone does not fully explain inequity in access to health services, especially diagnostic and treatment procedures, for infarct survivors. A comprehensive self-administered health needs assessment (HNA) questionnaire was developed for concomitant use with generic (Short Form-12 and EuroQOL) and specific (Seattle Angina Questionnaire) health-related quality of life (HRQL) instruments on 242 patients (41% female) admitted to the Acute Cardiac Unit, Nottingham. Women expressed more dissatisfaction than men overall (p<0.05) and appeared to have more physical needs. Women were more likely to complain about transport, which influenced their access to healthcare facilities (p<0.001), to be concerned about getting help with cleaning (p<0.01), and to request information about rehabilitation services, potential limitations on their daily activities, and nutrition and diet (p<0.05). Women had lower health-related quality of life scores in all the HRQL variables, which was significant in EQ-5D (usual activities, and pain/discomfort), Seattle angina questionnaire (angina stability), and both components of the Short Form-12. This survey was the first attempt to apply a needs assessment tool combined with quality of life assessment for cardiac patients to identify potential gender disparities. Women reported greater health needs and greater dissatisfaction with current health services and had worse HRQL. Recognition of gender disparities in health needs and HRQL would clarify areas for improvement in healthcare services, and these might allow a better quality of life for infarct survivors.
November 2005 Br J Cardiol 2005;12:456-8
How would British stroke physicians diagnose and treat hypoxia in patients with acute stroke?
Christine Roffe, Amit Arora, Peter Crome, Richard Gray

There is no evidence from randomised controlled trials to guide oxygen treatment after stroke. This survey aims to establish a snapshot of views of clinicians on best current practice relating to the management of hypoxia early after acute stroke. A postal questionnaire was sent to all 231 members of the British Association of Stroke Physicians (BASP). For 88% of the 130 respondents the decision to give oxygen was guided by the oxygen saturation, and for 67% it was guided by clinical criteria. The mean cut-off for oxygen supplementation suggested was ? 93% SD 2 (range 85–98%). Sixty-seven respondents would give oxygen by nasal cannulae and 74 via face mask. The oxygen concentration selected was 24% (n=17), 28% (n=31), 35% (n=15), 40% (n=3) and 100% (n=3). This shows there is wide variation amongst stroke physicians about when to start oxygen, how much to give and by which route. There is a need for a randomised clinical trial to guide oxygen therapy after acute stroke.
November 2005 Br J Cardiol 2005;12:448-55
Possible clinical implications of the Cardiac Insufficiency Bisoprolol (CIBIS) III trial
Ronnie Willenheimer, Bernard Silke

The mainstay of heart failure management is angiotensin-converting enzyme inhibitor therapy initially as a vasodilator, followed by beta blockade at a varying time interval, based on clinical judgement. Early beta blockade has theoretical advantages in terms of possible protection against dysrhythmia or disease progression, although there may be short-term concerns regarding a possible deterioration in cardiac function and aggravation of heart failure. The Cardiac Insufficiency Bisoprolol (CIBIS) III trial examined the optimum paradigm of initiating treatment for chronic heart failure (CHF). A large cohort of 1,010 systolic CHF patients, at least 65 years of age, with stable, mild-to-moderate symptomatic disease, were followed-up for a mean of 1.25 years. Patients were randomly allocated to initial monotherapy with bisoprolol for six months, followed by the addition of enalapril, or the opposite sequence. Efficacy and safety of the bisoprolol-first strategy versus the enalapril-first strategy was similar in terms of the combined primary end point of mortality or all-cause hospitalisation (hazard ratio 0.94, 95% confidence interval 0.77–1.16, non-inferiority p=0.02). The two approaches also showed similar safety. The bisoprolol-first strategy showed a 28% mortality reduction after the monotherapy phase (p=0.24) and a 31% borderline-significant mortality reduction during the first year (p=0.06), but was associated with a 25% increase in worsening of CHF events (p=0.23). This paper highlights important features of the study design and patient population. Both the clinical perspective and possible clinical implications of CIBIS III are discussed.
November 2005 Br J Cardiol 2005;12:443-6
Aldosterone blockade in heart failure
Iain Squire

In spite of treatment with inhibitors of the renin-angiotensin system, plasma levels of aldosterone increase progressively in heart failure. This phenomenon of aldosterone escape is associated with adverse outcome. The aldosterone receptor antagonists spironolactone and eplerenone can improve prognosis for patients with heart failure. The commonest, and often problematic unwanted effect of these agents, hyperkalaemia, may limit their usefulness and brings with it the need for careful clinical and biochemical monitoring. Recent trials, however, have shown clear benefits for large groups of patients for spironolactone (in severe chronic heart failure) and eplerenone (heart failure soon after acute myocardial infarction). Due consideration should be given to the addition of the appropriate aldosterone antagonist in suitable patients.
November 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 74–AIC 79
The coronary pressure wire for decision- making in the real world
Williams Omorogiuwa, Michael Fisher

Coronary angiography is an imperfect tool for assessing the functional significance of lesions: while this may be determined non-invasively using myocardial perfusion scintigraphy or stress echocardiography, it is often not done. In these circumstances the coronary pressure-derived fractional flow reserve (FFR) serves as an alternative, lesion-specific means of assessing physiological importance. FFR is an invaluable tool not only in determining whether a lesion is functionally significant and should be tackled, but it also ensures that the appropriate physiological outcome is obtained from coronary intervention.
November 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 81–AIC 82
Percutaneous coronary interventions in West Yorkshire for the year 2002: an audit
Khaled Alfakih, Elizabeth Rennie, Stacey Hunter, James Mclenachan

Early invasive management in patients with unstable angina and non-ST elevation myocardial infarct (NSTEMI) is now well established. However, patients can wait for weeks at district general hospitals (DGHs) for in-patient transfer to the cardiac centre for percutaneous coronary intervention (PCI), which results in inefficient bed utilisation. At the Yorkshire Heart Centre (YHC), the referral process for unstable angina/NSTEMI was streamlined to minimise the delay between time of referral and PCI. We audited the waiting time from referral to the PCI procedure as well as the six- and 12-month outcomes for both acute and elective PCI and compared our outcome data to the published trials. A total of 1,757 patients underwent PCI at YHC in 2002; of these 47% were acute cases. 72% of patients were treated within two days of referral and 97% within three days. The mean waiting time for patients referred from within the YHC was 1.9 days and for those referred from the DGHs was 2.2 days. The six-month mortality rate for the acute PCI group was 2.5%.
November 2005 Br J Cardiol (Acute Interv Cardiol) 2005:12:AIC 83–AIC 91
Modelling the cost-effectiveness of cardiac interventions: the case of sirolimus-eluting stents
Neil Hawkins, Mark Sculpher, Martin Rothman

This article aims to provide a primer on decision modelling to assess the cost-effectiveness of interventions in cardiology. The paper uses a cost-effectiveness model developed to compare alternative coronary stents. This decision analytic model assesses costs to the UK health service and health benefits in terms of quality-adjusted life-years (QALYs). Data were taken from a range of sources, including 12-month follow-up data from three important double-blind randomised controlled trials: RAVEL, SIRIUS and E-SIRIUS. Methods are employed to show the uncertainty in cost-effectiveness. Sirolimus-eluting stents were compared to ‘bare metal’ stents in constructing this decision model. The patients included were those individuals with stable coronary disease randomised to the three trials. The main outcome measures were: mean QALYs, mean health service costs, incremental cost per additional QALY, and the probability that sirolimus- eluting stents are more cost-effective than bare metal stents. Mean QALY gains per patient from the sirolimus-eluting stent range from 0.011 to 0.017 over 12 months. Although the list price of the sirolimus- eluting stent is £617 more than the bare metal stent, its additional total mean cost per patient, including ‘cost offsets’ from a lower rate of subsequent events, ranges from £53 to £166. The incremental cost of the sirolimus-eluting stent per additional QALY ranges from £3,181 to £15,198. The probability that the sirolimus-eluting stent is less costly than the bare metal stent ranges from 0.13 to 0.34. If the health service is willing to pay up to £40,000 per additional QALY, the probability of the newer stent being the more cost-effective ranges between 0.8 and 1.0. These results are sensitive to assumptions about the price differential between the two forms of stent. Cost-effectiveness analyses based on models are used increasingly as a basis for decision making. It is essential that these models are developed with clinical input regarding appropriate assumptions and interpretation of evidence.
November 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 98–AIC 100
An unusual pulmonary embolus
Umeer Waheed, Phang Boon Lim, Jeremy Cordingley, Mike Mullen

Due to advances in paediatric congenital heart surgery in recent years, the number of patients who survive into adulthood with complex congenital heart disease has increased remarkably. When these patients present to non-specialist hospitals with apparently specific symptoms, the diagnosis may not be as straightforward as initially thought. Here we highlight a case which demonstrates this.
September 2005 Br J Cardiol 2005;12:401-3
Peripheral arterial disease – CVD by any other name?
Sarah Jarvis

The National Service Framework for Coronary Heart Disease (CHD) stated that individuals at greatest risk of CHD should be identified. This category included those with diagnosed peripheral vascular disease. Despite this, the condition was not included in the Quality and Outcomes Framework of the new General Medical Services contract. This article looks at the strong evidence to include peripheral arterial disease in the next update of the GMS contract, which is expected in April 2006. It also looks at what is being done to identify such patients, and their relative risk compared to other subpopulations at risk of atherothrombosis. The setting up of an international register – the REACH registry is also discussed.
September 2005 Br J Cardiol 2005;12:397-400
Statin prescribing: is the reality meeting the expectations of primary care?
Adrian JB Brady, John Norrie, Ian Ford

Two surveys were carried out to look at statin prescribing in UK general practice. The first was a study of the Mediplus prescribing database in relation to coronary heart disease (CHD) patients prescribed a statin. The second was a postal survey of the attitudes and beliefs about statin prescribing among general practitioners (GPs) who had contributed to this database. Results showed that despite 80% of GPs believing they had achieved target cholesterol levels (< 5 mmol/L) in 80% of their CHD patients, this was initially only achieved in 65% of patients, rising to 78% after titrations and switching. Only 46% of patients achieved a chol-esterol reduction of 25%, which increased to 56% after titrations and switching.
September 2005 Br J Cardiol 2005;12:394-5
Meig’s syndrome with massive pericardial effusion, bilateral pleural effusion and ascites
Mohammed N Al-Khafaji, Salim Ahmed

Meig’s syndrome is a condition in which an ovarian tumour (usually a fibroma) is associated with ascites and pleural effusion. It resolves after resection of the tumour. We report here what we believe to be the first case of a patient with pericardial effusion complicating Meig’s syndrome.
September 2005 Br J Cardiol 2005;12:392-3
COX-2 inhibitors: managing comorbidities in primary care
Rubin Minhas

The recent withdrawal of rofecoxib, a COX-2 inhibitor, has focussed attention on the use of COX-2 inhibitors and other non-steroidal anti-inflammatory drugs (NSAIDs) in patients with cardiovascular disease.
September 2005 Br J Cardiol 2005;12:387-91
COX-2 inhibitors and the cardiovascular system: is there a class effect?
Mohamed Bakr, Derek G Waller

Selective inhibition of COX-2 preferentially inhibits the production of prostaglandins responsible for vasodilation and inhibition of platelet aggregation. This potentially creates a pro-thrombotic state. This review examines the evidence that selective COX-2 inhibitors have adverse effects on the heart and circulation. The risk of myocardial infarction and other vascular ischaemic events, the effects on blood pressure and decompensation of treated heart failure are discussed. Conclusions are drawn about the relative risk with the different members of the drug class, and recommendations for clinical practice presented.
September 2005 Br J Cardiol 2005;12:379-86
New approaches to the management of dyslipidaemia
Lena M Izzat, Philip Avery

Multiple randomised controlled trials have unequivocally shown that lowering low-density lipoprotein cholesterol (LDL-C) results in a predictable reduction of coronary events and it appears that there is no threshold beyond which lowering LDL-C does not result in further benefit. Although statins are the mainstay of treating hyperlipidaemia, they cannot always succeed in achieving more stringent lipid targets in some patients as they inhibit only one element of cholesterol homeostasis: the endogenous pathway. Ezetimibe is a novel agent which inhibits the exogenous cholesterol pathway, with resultant complementary benefits with statins. Ezetimibe co-administered with a statin may provide an additional 16–18% reduction in LDL-C, compared to only a 6% further reduction in LDL-C with each doubling of a statin dose. This concept of combination therapy, tackling different homeostatic pathways, may be akin to strategies used in management of hypertension, where a combination of antihypertensive agents from different pharmacological classes is the norm.
September 2005 Br J Cardiol 2005;12:372-8
Problems of cardiac rehabilitation coordinators in the UK: are perceptions justified by facts?
Hugh JN Bethell, Julia Evans, Sheila Malone, Sally C Turner

The National Service Framework for Coronary Heart Disease recommended in 2000 that cardiac rehabilitation (CR) should be offered to 85% of patients recovering from myocardial infarction or revascularisation. This target is a long way from being met. Provision of CR might be improved by addressing the problems met by CR coordinators. This study, through a questionnaire and more detailed surveys of CR coordinator experiences, set out to identify these problems. CR coordinators' problems were canvassed in the 2001/2 Annual Survey of CR programmes in the UK and their responses were compared with figures from the same survey and from surveys from the North West and the South East Regions of England. We found their main problems included lack of money (87%), lack of staff (90%), lack of space (74%), lack of sessions (74%), failure of referral of heart failure patients (66%), attendance problems (71%) and waiting lists (55%). All of these perceived problems were confirmed by the figures from at least one of the surveys – and, in most cases, by two or three of the surveys. These findings point to measures for improving CR provision. These include proper funding on a cost per patient basis, the provision of adequate space and the better use of information technology.
September 2005 Br J Cardiol 2005;12:361-6
Cardiac rehabilitation: results of a national survey
Allison Thorpe, Sian Griffiths, Charles F George

The provision of cardiac rehabilitation (CR) services in the UK was surveyed in March 2003. Three hundred questionnaires were sent to Directors of Public Health based in Primary Care Trusts. One hundred and eighty-five replies were received, a 61.7% response rate. In 72.8% of cases CR services were provided in both the acute and community sectors, but in 22.8% services were only available in the acute sector. CR services were patchy, lacked integration and in only 31.3% of Primary Care Trusts (PCTs) were they described as adequately funded.
Many patients are not receiving this important treatment modality after either myocardial infarction or cardiac surgery.
July 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 45–AIC 48
Drug-eluting stents: NICE guidelines and the reality
Tim Wells, Keith Dawkins

The National Institute for Clinical Excellence (NICE) stent appraisal (2003) defined criteria for the use of drug-eluting stents (DES) on the basis of lesion length, vessel diameter and the absence of recent myocardial infarction or intra-luminal thrombus. The appraisal suggested that as many as one third of all stents may need to be DES. In order to determine the requirement for DES and adherence to these guidelines, we assessed 1,673 consecutive patients undergoing coronary intervention over a 17-month period. A total of 2,513 stents were implanted, of which 50.1% were DES. In all, 77.4% of patients fulfilled NICE criteria for at least one DES. A further 7.3% of patients were excluded because of either a recent (< 24 hours) myocardial infarct or visible intra-luminal thrombus. A total of 33.4% of patients who did fulfil NICE criteria for DES deployment inappropriately received a bare-metal stent (BMS) whilst 5.7% patients inappropriately received a DES. These results would suggest that NICE have grossly underestimated the need for DES in ‘real world’ practice. Despite our centre using a high volume of DES, significant numbers of patients were inappropriately treated with BMS, with a smaller number inappropriately treated with DES, according to NICE criteria.
July 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 49–AIC 53
Diabetic revascularisation by coronary angioplasty: is one stent better than another?
Jeremy N Butts, Kenneth P Morgan, Kevin J Beatt

As confidence in the use of drug-eluting stents (DES) increases, they are being used in patients with progressively more complex disease. Diabetes is still an independent risk factor for restenosis along with lesion length and reference vessel diameter. This article gives an overview of recent stenting trials, including those with more complex disease such as DIABETES, PORTO 1 and TAXUS V. It also looks at head-to-head randomised controlled trials of sirolimus-eluting stents against paclitaxel-eluting stents: ISAR-DESIRE, SIRTAX, ISAR-DIABETES and REALITY. These give a better indicator of comparative efficacy than meta-analyses which include differing patient populations and trial designs. Finally, studies comparing angioplasty with surgery are considered.
July 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 56–AIC 59
Introduction of primary percutaneous coronary intervention for ST elevation myocardial infarction in a district general hospital
Sohail Qaisar, Melanie Fellows, Hannah Whitlam, Rumi Jaumdally, James M Beattie, Patricia J Lowry, Nadia El-Gaylani, Robert G Murray, Jerome Ment, Michael Pitt

The objective of this study was to assess the feasibility and impact of providing a primary percutaneous coronary intervention (PCI) programme for ST elevation myocardial infarction (STEMI) in a district general hospital (DGH) in the UK. A retrospective review of cardiac catheter laboratory PCI database records and hospital notes was carried out in a 950-bed teaching DGH in the West Midlands, serving a catchment population of 500,000. The patients consisted of 108 men and women aged 28–86 years presenting with thrombolysis-eligible STEMI, treated by primary PCI between November 2002 and August 2004. The main outcome measures used in this study were time from hospital presentation to PCI (‘door to coronary device’ time), mortality and hospital length of stay. The median door to device time was 86 minutes (range 25 to 286). Some 78% and 52% of patients had door to device times of less than 120 and 90 minutes, respectively. Median length of hospital stay was five days (range 3–30), compared to eight days in patients treated with thrombolysis in the years 2000–2004. In-hospital mortality was seven patients (6.5%). We conclude that, in the contemporary era of interventional cardiology, it is feasible to introduce a primary PCI service for STEMI in a DGH setting with acceptable ‘door to coronary device’ times and mortality.
July 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 61
Sub-intimal dissection guided by retrograde angiography to recanalise a chronic coronary artery occlusion
Amal Louis, Julian Gunn

A 62-year-old man presented with chronic stable angina, how coronary angiography revealed a chronic proximal occlusion of the right coronary artery (RCA) with retrograde filling of the vessel from the septal branches of the left anterior descending (LAD) artery.
July 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 62–AIC 67
Oral treatments for pulmonary arterial hypertension
Matt J Wright, J Simon R Gibbs

The management of pulmonary arterial hypertension (PAH) has changed dramatically over the last decade. Where once the physician had only limited tools to combat this devastating condition, recent randomised controlled trials have shown that there are now treatments that both prolong the rate of progression and improve survival. The ‘gold standard’ of treatment, due to its beneficial effect on survival, is epoprostenol, a prostacyclin analogue. However, there are a number of problems with the prostacyclin analogues, mainly centred on their administration and cost, which led to their use only in severely ill patients. A better understanding of the pathophysiology of PAH has led to a number of other pharmacological targets, namely antagonism of endothelin (ET) receptors and increasing local levels of nitric oxide (NO) via inhibition of phosphodiesterase 5. The successful treatment of PAH means that there is now a growing population of patients on disease-modifying agents, so it is essential that physicians are aware of their use, benefits and side effects.
July 2005 Br J Cardiol 2005;12:329-30
Setting a pace in cardiac rehabilitation
Mandy Fitzgerald-Barron

Coronary heart disease (CHD) is the most common cause of death in the UK; one in four men and one in six women will die as a result of CHD.
July 2005 Br J Cardiol 2005;12:313-7
Additional benefits versus practicalities of beta-blocker use in CHF patients: the ‘some is better than none’ rule
Graham Archard

Treatments for heart failure include digoxin, angiotensin-converting enzyme inhibitors, angiotensin II receptor blockers, aldosterone antagonists and beta blockers. Beta blockers have been contra-indicated until fairly recently, with recognition of the role of the sympathetic nervous system in chronic progression of heart damage.
Benefits of beta blockade, proven in clinical trials, include reduction in all-cause mortality, sudden death, hospitalisation rates for heart failure, and reversal of some degree of heart damage. Carvedilol and bisoprolol are currently licensed in the UK for chronic heart failure. National Institute for Clinical Excellence (NICE) guidelines give recommendations for initiation of treatment, dose titration and management of adverse effects. Benefits are still apparent in patients who cannot tolerate target drug doses. Several studies show, however, that beta blockers are underprescribed in general practice.
July 2005 Br J Cardiol 2005;12:308-11
Atrial fibrillation: strategies in primary care
Michael Kirby

This article describes the diagnosis, classification and management of atrial fibrillation (AF) in primary care. It looks at its increasing incidence, its risk factors, and the identification and classification of this common arrhythmia. The routine investigations for AF and its treatment, including drug therapy and cardioversion, are also discussed. Finally, with AF being a major risk factor for stroke, strategies to prevent thromboembolism are considered.
July 2005 Br J Cardiol 2005;12:306-7
Tranexamic acid and acute myocardial infarction
Amit KJ Mandal, Constatinos G Missouris

The plasminogen activator inhibitors have an important therapeutic role in controlling bleeding in patients with congenital and acquired coagulation disorders. They are being increasingly used in patients with blood loss and to prevent bleeding. However, these antifibrinolytic agents can also facilitate the development of thrombosis. We report a patient with severe gastrointestinal bleeding who developed acute myocardial infarction following the administration of the antifibrinolytic agent, tranexamic acid.
July 2005 Br J Cardiol 2005;12:302-5
Profile of documented medical history of chest pain: a multicentre audit of 1,226 consecutive patients with validated acute MI
Niamh Kilcullen, Rajiv Das, Peter Mackley, Christiana A Hall, Christine Morrell, Beryl M Jackson, Micha F Dorsch, Robert J Sapsford, Mike B Robinson, Alistair S Hall for the EMMACE-1 Study Group

This study set out to evaluate the completeness of medical records of chest pain. A planned, multicentre, structured abstraction of data from case-notes was made at 20 adjacent acute hospitals in Yorkshire on 1,226 consecutive patients presenting with chest pain and validated myocardial infarction (MI). The hospital records included those collected by ambulance crews, accident and emergency staff, and admitting medical teams. The main outcome measure was completeness of medical records with regard to 10 commonly advocated descriptors of chest pain. A mean number of 5.62 chest pain descriptors was recorded. This value differed with hospital (range 4.81 to 6.73 factors recorded; p<0.0001); place of admission (medical admissions unit = 6.10; coronary care unit 5.94; accident & emergency department = 5.62; general ward = 5.08; p<0.0001); gender (male = 5.74; female = 5.39; p=0.004) and age (< 68.4 years = 5.83; > 68.4 years = 5.43; p<0.0001). Mean chest pain scores were also significantly different for District General Hospitals (DGHs) without angiography facilities as compared to DGHs with angiogram facilities and tertiary centres (respectively 5.46 vs. 5.81 vs. 5.81 p<0.007). Contrary to standard medical texts and teaching, we observed that documentation of chest pain histories was abbreviated in many cases.
July 2005 Br J Cardiol 2005;12:298-01
Cardiac patients’ concerns and desire for information: a case for unmet needs
Mohsen Asadi-Lari, Chris Packham, David Gray

Tailoring healthcare provision to fulfil patients" needs is a principal objective of health services. Data on needs are sparse, especially in patients with coronary heart disease, who tend to have a high mortality rate, who often require admission to hospital and have an impaired health-related quality of life. A novel questionnaire was administered concomitantly with generic and specific quality of life tools in a cross-sectional study of a random sample of patients (n=242) aged 31–93 years (median 71 years) admitted with suspected acute coronary syndromes. Patients with confirmed infarction had fewer healthcare needs and reported less need for information on heart disease compared to those with other manifestations of coronary disease (p<0.01). Those recently seen by a general practitioner were better informed about their current treatment (p<0.01). Coronary disease patients with low quality of life scores were more likely to be anxious about cardiac problems (p<0.001). They were more likely to spend more time thinking about these concerns (p<0.001) and to seek help from, and to have increased expectations of, the family doctor or cardiologist (p<0.001), particularly in seeking greater commitment to their care. Reported deficiencies in service included difficulty accessing healthcare services, especially for men < 65 years (p=0.01) and availability of repeat prescriptions for the over 75-year-olds (p<0.05). Patients with coronary disease had unmet healthcare needs and worse health-related quality of life. Further investigation of healthcare needs among patients with coronary disease could lead to simply improved services and major health improvement. Assessment of quality of life appeared to be a surrogate for formal healthcare needs assessment.
July 2005 Br J Cardiol 2005;12:291-7
Comparison of two- and three-drug combination therapy with candesartan in patients with severe hypertension
Heinrich Holzgreve, Reinhard Gotzen, Gerhard Kiel

The efficacy and tolerability of two candesartan treatment regimens were evaluated in 578 severely hypertensive patients already receiving a diuretic plus an angiotensin-converting enzyme (ACE) inhibitor, a calcium channel blocker (CCB) or a beta blocker. Existing treatments were standardised during a two-week run-in period. Patients with uncontrolled blood pressure (diastolic blood pressure [DBP] > 90 mmHg) were randomly switched to a regimen comprising candesartan 16 mg plus hydrochlorothiazide (HCT) 12.5 mg once daily for four weeks (switch regimen, n=291), or had candesartan 8 mg once daily added to their existing treatment (add-on regimen, n=287). After four weeks’ treatment, mean sitting DBP was reduced from baseline by 11.2 mmHg (SD 11.2) and 13.9 mmHg (SD 11.5) in the switch and add-on treatment groups, respectively. Mean sitting SBP was decreased by 15.3 mmHg (SD 18.7) and 20.7 mmHg (SD 20.3), respectively. During an additional four weeks’ treatment, ‘switch’ non-responders had their doses of study medications doubled, resulting in a further reduction of 5.4 mmHg (SD 9.8) DBP and 5.9 mmHg (SD 14.9) SBP. Both treatment regimens were well tolerated. Thus, in patients with severe hypertension, adding candesartan to a standard-dose two-drug combination, or switching from a pre-existing two-drug, standard-dose combination to high-dose candesartan plus HCT enables enhanced BP control, with superiority of the three- over the two-drug combination.
July 2005 Br J Cardiol 2005;12:283-90
Milk, heart disease and obesity: an examination of the evidence
Amit KJ Mandal, Constatinos G Missouris

The plasminogen activator inhibitors have an important therapeutic role in controlling bleeding in patients with congenital and acquired coagulation disorders. They are being increasingly used in patients with blood loss and to prevent bleeding. However, these antifibrinolytic agents can also facilitate the development of thrombosis. We report a patient with severe gastrointestinal bleeding who developed acute myocardial infarction following the administration of the antifibrinolytic agent, tranexamic acid.
July 2005 Br J Cardiol 2005;12:275-82
Should all diabetic patients receive aspirin? Results from recent trials
Nick Barwell, Gillian Marshall, Claire McDougall, Adrian JB Brady, Miles Fisher

Atherosclerotic cardiovascular disease (CVD) is common in patients with diabetes, and antiplatelet therapy has been the cornerstone of preventative therapy for many years. The majority of the evidence for the use of aspirin in patients with diabetes comes from subgroup analysis of major secondary prevention trials. Secondary prevention data from the Antiplatelet Trialist’s Collaboration meta-analysis suggests that the benefit derived from aspirin is similar in diabetic and non-diabetic populations. In the general population, data from primary prevention studies have shown the benefit of aspirin in terms of cardiovascular mortality, but there is little evidence to suggest that aspirin is beneficial in terms of total or cardiovascular mortality for primary prevention in a diabetic population. Clopidogrel may have advantages over aspirin and combined therapy may be superior for certain types of coronary artery disease and stroke, although this is offset by an increased risk of haemorrhage in the latter setting. The use of aspirin in the prevention of CVD in patients with diabetes should therefore be focused on those with a history of vascular events or aggressively treated hypertension.
May 2005 Br J Cardiol 2005;12:243-4
Heart failure management – a secondary care perspective
Martin Cowie

In the previous article, Dr Sarah Jarvis provides a useful perspective on the management of heart failure in primary care. Recent reports from the Department of Health and the Healthcare Commission have highlighted the lack of progress in implementing evidence-based practice in heart failure. It is essential that primary and secondary care work together to improve the situation.
May 2005 Br J Cardiol 2005;12:240-3
Heart failure management in primary care – the story so far
Sarah Jarvis

Increasing rates of coronary heart disease and the increasing longevity of the UK population mean that the number of cases of heart failure seen in general practice is rising rapidly. Simultaneously, this disease area has been recognised by the National Institute for Clinical Excellence, which has published guidelines for its management, and it has been made a target for remuneration under the new General Medical Services contract. This, together with the latest clinical trial evidence, has dramatically changed how heart failure is managed in primary care. Considering these recommendations and the latest clinical trial evidence, a logical management plan for heart failure is suggested.
May 2005 Br J Cardiol 2005;12:233-8
The diagnosis and management of heart failure across primary-secondary care: a qualitative study
Ahmet Fuat, Pali Hungin, Jeremy James Murphy

The management of heart failure has altered greatly and good outcomes are dependent on an accurate, specific diagnosis and modern therapy. In 50% of cases, heart failure is diagnosed in hospital, with high readmission rates. There is evidence of variations in the diagnosis and management practices between specialists and hospitals, compromising uniformly high standards. In turn, this is likely to affect the quality of ongoing management in primary care. This qualitative study explores specialists’ attitudes and practices in the diagnosis and management of heart failure with a view to identifying barriers to provision of uniformly high standards of care.
May 2005 Br J Cardiol 2005;12:230-31
Coronary spasm as a cause of sudden death induced by malignant ventricular arrhythmia
Joseph John, Gerry C Kaye

Coronary artery spasm is an uncommon presentation of angina and may be associated with other vasospastic diseases such as Raynaud’s disease. It is widely accepted that local imbalance of production and removal of nitric oxide (NO) and other endothelium-derived factors is generally responsible for the arterial spasm in variant angina. Very rarely, diffuse spasm can herald ventricular arrhythmias due to sudden reduction in perfusion.
May 2005 Br J Cardiol 2005;12:224-9
Can we treat heart failure effectively and maintain potassium homeostasis? A clinician’s perspective
Iain Squire

Hypokalaemia and hyperkalaemia are common complications of heart failure and its treatment: either may increase markedly the risk of arrhythmias and sudden cardiac death. Hypokalaemia predominates in the early stages of heart failure. The risk of hyperkalaemia increases as renal function declines, usually in the context of advancing heart failure. For patients with heart failure, serum potassium levels of between 4.5–5.5 mmol/L are recommended. Monitoring of serum potassium is essential, with more frequent monitoring in patients with moderate renal failure, relatively high serum potassium, or in those at high risk of renal impairment, e.g. elderly or diabetic patients. Hypokalaemia can be ameliorated by a potassium-sparing diuretic or an aldosterone receptor antagonist; increasing dietary potassium intake or taking potassium supplements is less effective. Doses of loop or thiazide diuretics should be optimised. Hyperkalaemia is more often seen in advanced heart failure. Restriction of dietary potassium and withdrawal of potassium supplements are standard. Temporary discontinuation of angiotensin-converting enzyme inhibitor and/or aldosterone receptor antagonist therapy may be appropriate but attempts should be made to reintroduce these. Excessive diuretic therapy should be avoided. With routine potassium monitoring and pre-emptive intervention included in heart failure protocols, the risks to patients can be minimised.
May 2005 Br J Cardiol 2005;12:219-23
Sleep-disordered breathing and heart failure: an opportunity missed?
Ali Vazir, Mary J Morrell, Anita K Simonds, Hugh F Mcintyre

Sleep-disordered breathing (SDB) is common in patients with congestive heart failure (CHF). SDB appears to be associated with accelerated progression of heart failure. However, it is seldom recognised in cardiology clinics, especially as CHF patients with SDB rarely report symptoms specific to SDB, such as excessive day-time sleepiness. The term SDB incorporates both central sleep apnoea (CSA) and obstructive sleep apnoea (OSA). CSA is thought to be a consequence of heart failure, whereas OSA is thought to be associated with hypertension and excessive sympathetic nerve activation, which may exacerbate failure of the heart through haemodynamic and mechanical mechanisms. The treatment of SDB is likely to be an important complementary step in the management of heart failure, particularly OSA, where treatment with continuous positive airway pressure is well established and significant improvements in left ventricular ejection fraction plus quality of life have been reported. The treatment of CSA remains unclear and requires further research. This review will examine the prevalence, diagnosis, pathophysiology, clinical features and treatment of SDB in patients with CHF.
May 2005 Br J Cardiol 2005;12:211-8
Aldosterone: an important mediator of cardiac remodelling in heart failure
Allan D Struthers

Aldosterone is intimately linked to the pathophysiology of heart failure, and high levels of aldosterone are associated with worse prognosis. Many non-renal effects of aldosterone contribute to the congestive heart failure syndrome, including endothelial dysfunction, reactive myocardial fibrosis and cardiac remodelling. The precise mechanism by which aldosterone stimulates myocardial collagen accumulation and fibrosis is not yet fully understood. It may largely occur secondary to aldosterone-related endothelial dysfunction and inflammation, since endothelial dysfunction can lead to micro-thrombus formation and tissue micro-infarction, which repairs itself by fibrosis. Other contributory effects may include a direct impact of aldosterone on the collagen synthesis pathway. In the RALES study, spironolactone in conjunction with an angiotensin-converting enzyme (ACE) inhibitor was found to reduce mortality in chronic moderate-to-severe heart failure; the EPHESUS study more recently reported significant reductions in death and hospitalisation when eplerenone was added to ACE inhibitor and beta blocker therapy in patients with clinical evidence of heart failure following acute myocardial infarction. Clinicians should now consider routinely adding an aldosterone receptor antagonist to standard therapy of patients with left ventricular dysfunction and heart failure in order to reduce cardiac morbidity and mortality.
May 2005 Br J Cardiol 2005;12:205-8
Heart failure after myocardial infarction: a neglected problem?
Martin R Cowie, Larry Lacey, Maggie Tabberer

Improvements in the management of acute myocardial infarction together with population ageing have contributed to a growing burden of heart failure. Around half of new cases of heart failure in patients aged less than 75 years are due to coronary artery disease; many of these patients develop heart failure in the context of acute myocardial infarction. Left ventricular systolic dysfunction is the single most common cause of heart failure after myocardial infarction. Of the estimated 65,000 new cases of heart failure in the UK each year, it is likely that around 15,000 occur in the context of acute myocardial infarction. Ventricular remodelling generally occurs in the early period after myocardial infarction, and early identification offers the potential to modify this process and reduce the risk of heart failure. Clear guidelines should be built into the myocardial infarction care pathway to ensure an integrated approach from hospital and community services.
March 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 9–AIC 14
Elevation of troponin I in acutely ill medical patients: a pilot study and literature review
Jonathan Watt, Andrew P Davie, Anne Cruickshank

Previous studies have identified a significant incidence of clinically unrecognised myocardial ischaemia in intensive care unit (ICU) patients, as determined by elevation of serum troponin. This pilot study demonstrates a similar high frequency of such a phenomenon in patients who are acutely ill, but without clinical evidence of myocardial ischaemia, on the general medical wards of a large city hospital. Elevation of serum troponin in these patients is associated with higher hospital mortality and increased lengths of hospital stay. Recognition that slight elevation of troponin levels may occur in the context of significant medical illness in acute general medical ward patients is important as it may avoid erroneous diagnosis of myocardial infarction and subsequent unnecessary investigations. A literature review of the various causes of an elevated troponin result is then presented.
March 2005 Br J Cardiol (Acute Interv Cardiol) 2006;13:AIC 14–AIC 18
Risk of death, MI and patterns of care delivered in non-ST elevation ACS patients with intermediate elevations in cardiac troponin T: a UK DGH experience
Kausik Ray, James Bolton, Alice Veitch, Paul Sheridan, Michael Gillett, Ahmed Al Rifai, Ramasamy ManivArmane, Alan Brennan, Gillian Payne, Wazir Baig

Abstract Prior studies have suggested a gradation in clinical risk with increasing elevations of cardiac troponins in patients with non-ST elevation acute coronary syndromes (ACS). We hypothesised that patients with cardiac troponin-T (cTnT) between 0.01-0.1 μg/L might be perceived as a low-risk group and consequently receive less active medical treatment.
March 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 27–AIC 30
Delivering a modern PCI service: can we change with the times?
Michael S Norell, Saib S Khogali, James M Cotton, Michael R Cusack

The volume and complexity of patients undergoing percutaneous coronary intervention (PCI) is growing steadily. This, and the increasing tendency for these procedures to be unplanned, requires us to rethink the way we deliver care in this setting. This article addresses the processes involved, which include pooling of PCI lists, multidisciplinary team meetings and integrated care pathways for both elective and unplanned cases. The value of pre-assessment clinics, specific cardiac triage teams and “generic” catheter lab workers is also discussed. More traditional elements of the service such as on-call rotas are reappraised. Newer concepts, like dedicated PCI meetings to plan strategy and review previous problem cases for educational purposes, are also introduced.
March 2005 Br J Cardiol (Acute Interv Cardiol) 2005;12:AIC 31–AIC 32
Complex cardiac myxoma
David J Fox, Geir J Grötte, Lawrence Cotter

Cardiac myxomas are the most common benign intracardiac tumour, and are more common in women. Since many patients suffer from cerebral or systemic embolism, early diagnosis is vital to plan for surgical intervention. Surgical excision is advocated as soon as possible, particularly in left atrial myxoma, because of the high risk of valvular obstruction and systemic embolisation. Patients with a family history of the disorder are at greater risk of tumour recurrence.
March 2005 Br J Cardiol 2005;12:156-60
The definition of maximally tolerated blood pressure treatment
Terry McCormack, Mark Davis

The new General Medical Services contract has introduced the term ‘maximally tolerated blood pressure treatment’, which it defines as a cut-off point at which a doctor might advise the patient to accept the current blood pressure level. Whilst this is a sensible idea, the contract does not give any guidance as to how the doctor should decide when that point has been reached. In this article the Primary Care Cardiovascular Society considers the issue, looking at available evidence, and publishes a consensus statement on the definition for maximally tolerated blood pressure treatment.
March 2005 Br J Cardiol 2005;12:146-8
Aneurysms of the sinus of Valsalva following infective endocarditis
Analie Grimshaw, Eu Krishna Adluri, Chris J Smallpeicegénie Di Stefano, Stephen Saltissi

Aneurysms of the sinus of Valsalva associated with infective endocarditis are rare. They can present during an episode of acute endocarditis or as late sequelae, with or without rupture. Their management involves repair of the annulus and closure of the aneurysm with a Dacron patch.
March 2005 Br J Cardiol 2005;12:149-54
Organising primary prevention: an approach by multifactorial risk score profile
John M Waddell, Caron Neal

Interventions on individual risk factors are most effective when directed at those with highest absolute risk. Joint British Society Guidelines and National Service Frameworks (NSF) indicate that these individuals should be identified. There is a need to continuously categorise the population by risk to identify those for primary prevention. This article describes a project that was set up to use clinical information technology in an innovative way. It was introduced as an administrative routine for the whole population of a large district (Blyth Valley, Northumberland) through the general practices to which the patients belong.
March 2005 Br J Cardiol 2005;12:145
Angiotensin-converting enzyme polymorphism in Turkish male athletes: relationship to left ventricular mass and function
Dursun Dursunoglu, Halil Tanriverdi, Harun Evrengul, Günfer Turgut, Sebahat Turgut, Osman Genç, H Asuman Kaftan, Mustafa KIlIç

Angiotensin-converting enzyme (ACE) is a key enzyme in the production of angiotensin II. The cloning of the ACE gene has made it possible to identify a deletion (D)-insertion (I) polymorphism that appears to affect the level of serum ACE activity. The aim of our study was to analyse the ACE gene I/D polymorphism in Turkish male athletes and to evaluate its relationship to left ventricular mass and function. Forty male athletes (mean age 23.4+1.8 years) were included in this study, and they underwent both complete echocardiographic assessment and analysis of ACE I and D allele frequencies in peripheral blood by polymerase chain reaction. They were separated into three subgroups according to their ACE DD (n=13), DI (n=16) and II (n=11) genotypes. Thickness of the interventricular septum (IVS), the left ventricular posterior wall (LVPW) and left ventricular mass (LVM) and LVM index (LVMI) were measured by the M-mode. Left ventricular ejection fraction was calculated using Simpson’s method, and so was the myocardial performance index. There was no statistically significant differences between the ACE DD, DI and II genotypes at the p>0.05 level by age, body mass index, heart rate, systolic and diastolic blood pressures. The thickness of the IVS (12 mm) and LVPW (10.7 mm), and LVM (302.8 g) and LVMI (157.3 g/m2) in ACE DD genotypes were higher than for both ACE DI (10.8 mm; 9.7 mm; 231.9 g; 125.3 g/m2) and II genotypes (9.0 mm; 8.6 mm; 185.0 g; 107.5 g/m2) in athletes. Left ventricular systolic and global functions among the three ACE genotypes were not different statistically. Our findings suggest that left ventricular hypertrophy is partially determined by genetic disposition and DD genotype of ACE is a potential genetic marker associated with an elevated risk of left ventricular hypertrophy.
March 2005 Br J Cardiol 2005;12:136-8
A randomised controlled study of ramipril dose-escalation packs in clinical practice
Stephen J Leslie, Sharon A Faulds, Andrea Rankin, Allister D Hargreaves

The benefits of angiotensin-converting enzyme (ACE) inhibitors occur early in the treatment period and may be dose-dependent. The utilisation of ACE inhibitors in cardiovascular patients is often suboptimal. This current study evaluates the clinical use of a specific ACE inhibitor dose-escalation pack. Fifty hospital in-patients with a definite indication for ACE inhibitor therapy were randomised to receive either a dose-escalation pack or 'usual' initiation and escalation of ramipril. Patients and general practitioners received an information sheet outlining the benefits and risks of ACE inhibitors and the need for monitoring of serum urea and electrolytes. The groups were matched for age, gender, deprivation score and blood pressure. One patient died in each group and one patient withdrew from the control group. More patients in the dose-escalation group reached target dose by six weeks (72% vs. 33%; p< 0.01) and three months (67% vs. 35%; p<0.05). At three months, there were no differences in serum creatinine, urea or potassium (all p>0.05). Cough was the most commonly reported side effect although there was no difference in its incidence between the dose-escalation and control groups (8% vs. 6%, p>0.05). This study demonstrates that the use of a specific dose-escalation pack for the ACE inhibitor ramipril is a simple, reliable and safe mechanism for reaching a target dose. This approach could find utility with other drug therapies.
March 2005 Br J Cardiol 2005;12:125-9
A review of olmesartan medoxomil – a new angiotensin II receptor blocker
Andrew Whittaker

Blockade of the renin-angiotensin system by angiotensin-converting enzyme (ACE) inhibitors or angiotensin II receptor blockers (ARBs) has been shown to be effective in treating hypertension and heart failure. There are currently seven ARBs in clinical practice, of which olmesartan medoxomil (Olmetec®) is the newest agent in the class. This article reviews the pharmacokinetics, pharmacodynamics, safety, efficacy, clinical use, dosing and cost of olmesartan medoxomil. This information is based on published data from human efficacy, safety and drug comparison studies. Olmesartan medoxomil (10–40 mg) has been shown consistently to achieve significant reductions in both systolic and diastolic blood pressures in human studies, which persist over the course of one year. There are limited, mainly experimental, data on its use in heart failure and atherosclerosis. It is an effective and well-tolerated agent with a long duration of action, allowing once-daily dosage in the treatment of hypertension.
March 2005 Br J Cardiol 2005;12:125-9
Should all diabetic patients receive an ACE inhibitor? Results from recent trials
Claire McDougall, Gillian Marshall, Adrian JB Brady, Miles Fisher

Diabetes is associated with both premature cardiovascular disease and renal disease. The presence of microalbuminuria is itself an independent risk factor for the development of cardiovascular disease. Angiotensin-converting enzyme (ACE) inhibitors were initially shown to slow the progression of established renal disease in patients with type 1 diabetes. Subsequent trials have demonstrated a similar benefit in patients with type 2 diabetes and with the use of angiotensin II receptor blockers (ARBs). The use of ACE inhibitors to prevent cardiovascular events in patients with established cardiovascular disease but not left ventricular dysfunction was established in two large randomised trials – HOPE and EUROPA. These benefits were maintained within the diabetic subgroups of these trials and appear to be independent of blood pressure lowering. The LIFE trial also provides evidence of the benefits of ARBs in reducing cardiovascular events in a high-risk population of diabetic patients with hypertension and left ventricular hypertrophy. Ideally, therefore, all diabetic patients with renal or cardiovascular disease should be treated with ACE inhibitors or ARBs.
March 2005 Br J Cardiol 2005;12:107-16
The management of hypertension in patients with benign prostatic hyperplasia and erectile dysfunction
Michael Kirby, Roger Kirby

Lowering elevated blood pressure reduces mortality and the risk of stroke, coronary heart disease and heart failure. The presence of benign prostatic hyperplasia (BPH) is a compelling indication for the use of an alpha blocker in the treatment of hypertension. Alpha blockers are first-line therapy for men with lower urinary tract symptoms (LUTS) and prostatic hyperplasia. In men with prostates larger than 30 cm3 or prostate-specific antigen > 1.4 ng/ml, 5-alpha reductase inhibitors may also be added. Typically, alpha blockers improve LUTS by 30–40% and maximum urinary flow rates by 16–25%, with clinical improvement within two weeks. The 5-alpha antagonists are only effective in men with a large prostate and may take up to six months to achieve their full effect. The Medical Treatment of Prostatic Symptoms (MTOPS) study assessed the long-term effects of doxazosin, finasteride and combination treatment on symptom scores, the clinical progression of BPH and the long-term risk of complications. Combination treatment reduced the risk of clinical progression by 66%, a significantly greater reduction than that induced by either agent alone. The improvement in the symptom score was also significantly greater in the combination treatment group. Erectile dysfunction (ED) may be a marker for other diseases, such as hypertension. ED is both more prevalent and more severe among patients with hypertension than among the general population. The link may be related to nitric oxide/cyclic GMP pathways and endothelial function. Many prescription drugs are associated with ED, including antihypertensive agents. The alpha blockers and angiotensin receptor blockers are the drugs least likely to cause ED, and may even improve the situation. All currently licensed ED treatments are suitable for managing ED in the cardiovascular patient, when used according to the manufacturer’s instructions. PDE5 inhibitors and alpha blockers should be temporally separated, or selective alpha blockers may be preferable, in order to avoid postural hypotension.
March 2005 Br J Cardiol 2005;12:118-22
Dyslipidaemia in ethnic populations: special considerations
Anthony H Barnett

There is extensive evidence of an increased risk of coronary heart disease (CHD) amongst South Asians (Indo-Asians) compared with Caucasians. This increased risk is not explained by conventional risk factors for CHD, such as smoking, hypertension and elevated total cholesterol levels. Studies have consistently demonstrated an increased prevalence of metabolic abnormalities including insulin resistance, diabetes, impaired glucose tolerance and dyslipidaemia, characterised by low plasma levels of high-density lipoprotein cholesterol (HDL-C) and high levels of triglycerides and lipoprotein a (Lp[a]), amongst South Asians. Together these factors predispose to accelerated atherosclerosis, and this is accentuated by adoption of a Western lifestyle. Nicotinic acid is the most potent lipid-modifying therapy for increasing HDL-C (by up to 30%), and is also effective in reducing triglycerides and Lp(a). Clinical studies in Caucasian patients have shown that nicotinic acid can also be safely used in patients with controlled type 2 diabetes. Long-term intervention studies have demonstrated the clinical benefits of nicotinic acid treatment, reducing cardiovascular morbidity and mortality in Caucasian patients with CHD. Nicotinic acid could potentially offer important therapeutic benefits in South Asians. Further clinical studies in this patient group are needed to substantiate this potentially useful treatment strategy and identify specific groups that would derive most benefit.
January 2005 Br J Cardiol 2005;12:71-3
Developing an evaluated patient-mediated intervention for monitoring amiodarone therapy
Jill Murie

Amiodarone is used to prevent atrial and ventricular arrhythmias in high-risk patients, such as after a myocardial infarction (MI) and in congestive cardiac failure. Its use has increased since the mid-1990s and, in 2001, around one million prescriptions were dispensed in primary care in England.
January 2005 Br J Cardiol 2005;12:65-70
Evidence-based treatment of hypertension: what’s the role of angiotensin II receptor blockers?
FD Richard Hobbs, Peter Irwin, Janet Rubner

Many large studies have confirmed the importance of controlling hypertension in reducing cardiovascular morbidity and mortality. Prescribers are now faced with a wide choice of antihypertensives and a growing body of evidence about their effects. This article reviews recent evidence about angiotensin II receptor blockers (ARBs). It concludes that they are effective in reducing blood pressure and cardiovascular disease. ARBs also have a renoprotective effect in diabetes. They are generally better tolerated than ACE inhibitors or beta blockers. Newer members of the class may be more effective than older ones at controlling hypertension, and combinations of ARBs with ACE inhibitors may be more effective than either drug alone. Many patients will require combinations of different classes of antihypertensive agents, and ARBs have an important place in providing therapy tailored to the needs of the individual patient.
January 2005 Br J Cardiol 2005;12:61-3
Early amiodarone pulmonary toxicity simulating heart failure
Manoj Bhandari, Trevor W Maskell, Ian D Pavord, Peter J Hubner

We report a case of very early onset of amiodarone-induced pulmonary toxicity, which appeared 12 days after starting treatment.
January 2005 Br J Cardiol 2005;12:57-60
Antiplatelet therapy for stroke prevention
Lian Zhao, Stan Heptinstall, Philip Mw Bath

Antiplatelet therapy plays a major role in the secondary prevention of ischaemic stroke. The antiplatelet agents that are most used in the clinic include aspirin, dipyridamole and clopidogrel. These agents inhibit platelet activation through different mechanisms of action. Aspirin is the first-line drug in the secondary prevention of stroke; a combination of aspirin with dipyridamole produces a synergistic antithrombotic effect. Clopidogrel is slightly more effective than aspirin at reducing the risk of ischaemic events. Trials comparing the combination of aspirin and clopidogrel versus aspirin are underway. Intravenous antiplatelet therapy with glycoprotein IIb/IIIa receptor inhibitors for acute stroke and as an adjunct to carotid artery stenting appears promising. However, oral GPIIb/IIIa receptor inhibitors appear hazardous.
January 2005 Br J Cardiol 2005;12:53-6
Holes and strokes
Mushtaq Wani, Ranjini Navaratnasingam

Five case histories are described to illustrate the importance of patent foramen ovale and atrial septal aneurysm as risk factors in stroke aetiology. Diagnostic methods, and the current and future management of these atrial septal defects, are briefly discussed.
January 2005 Br J Cardiol 2005;12:50-2
Audit of cardiac rehabilitation in light of the National Service Framework for coronary heart disease
Fiona Taylor, Andrew Beswick, Jackie Victory, Karen Rees, Ingolf Griebsch, Robert West, Rod Taylor, Jackie Brown, Margaret Burke, Shah Ebrahim

January 2005 Br J Cardiol 2005;12:47-9
Using the Framingham coronary risk appraisal functions to derive the expected annual number of UK coronary artery disease events
Arran Shearer, Paul Scuffham, David E Newby

The Framingham Heart Study investigators have recently developed new coronary risk appraisal functions which relate risk factors to the short-term probability of experiencing cardiovascular disease events. We populated the risk appraisal functions with UK data and estimated that approximately 256,000 new coronary artery disease (CAD) events occur annually in the UK. Approximately half of the estimated CAD events were acute myocardial infarctions (AMI) and almost three quarters occurred in men. Our estimates fit well with hospital in-patient data but less well with British Heart Foundation estimates of AMI and angina. Differences between US and UK relative risks, clinical practice and populations may account for these discrepancies. Our estimates may be considered as a lower limit of the annual number of UK CAD events.
January 2005 Br J Cardiol 2005;12:37-44
Current insights and new opportunities for smoking cessation
Hayden McRobbie

Assisting smokers to stop smoking is often seen as a difficult task but is crucial for health improvement, especially for those with established cardiovascular disease. Healthcare professionals are now, more than ever, in a position to help smokers who want to stop. For the greatest chance of success smokers should be referred to stop smoking services that provide multi-session treatment combining intensive behavioural support with nicotine replacement therapy or bupropion. Promising new medications are being developed that will add to the current treatment strategies and may give smokers a greater chance of stopping for good.
January 2005 Br J Cardiol 2005;12:31-6
The role of candesartan in the treatment of chronic heart failure
Hugh F McIntyre

The renin-angiotensin system (RAS) plays a fundamental role in cardiovascular pathophysiology. In particular, angiotensin II (AII) has been identified as a culprit in endothelial and vascular damage, elevated blood pressure, and cardiac failure. Pharmacological inhibition of this system is available through two mechanisms; the reduction of AII formation by inhibition of angiotensin-converting enzyme (ACE), and by direct blockade of the type 1 angiotensin II receptor by angiotensin II receptor blockers (ARBs). Angiotensin-converting enzyme (ACE) inhibitors have a proven role in the management of elevated blood pressure and diabetes and may confer specific vascular benefit. In patients with chronic heart failure (CHF) secondary to left ventricular systolic dysfunction (LVSD), there is extensive evidence that, when compared to placebo, ACE inhibitors reduce morbidity and mortality. Randomised placebo controlled trials have also shown ACE inhibitors reduce all-cause mortality and major cardiovascular events after myocardial infarction. Given the unequivocal benefit of ACE inhibitors, initial studies with ARBs in patients with LV dysfunction (in CHF and following myocardial infarction) have focused on two areas: the role of ARBs when compared with ACE inhibitors, and when combined with ACE inhibitors. Only recently, with the results of the CHARM study, have the role of ARBs when compared to placebo in a population with CHF been clarified. This study also addressed the benefit of ARBs in patients with heart failure and preserved LV systolic function.
November 2004 Br J Cardiol 2004;11:495-6
Education – the dawning of a new era?
Sally Smith

The Calman Review of 1998 recognised that continuing medical education through the postgraduate education allowance scheme (PGEA) had failed to deliver improvements in patient care. Instead, continuing professional development (CPD) has been put forward, which is intended to identify and fulfil learning needs. The primary care team itself is recognised to be a valuable learning resource.
November 2004 Br J Cardiol 2004;11:492-4
Palpitations and syncope in primary care
Amit KJ Mandal, George G Kassianos

Palpitations are a common complaint. It is useful for the GP to determine which are benign and which are potentially life-threatening and require urgent referral. Two cases are presented here in which the GP used 24-hour electrocardiogram (ECG) monitoring to detect a prolonged daytime sinus pause. Both patients were referred, as a consequence, for permanent pacemaker insertion. A 24-hour ambulatory ECG monitoring machine allows the GP to reassure patients whose palpitations have a benign origin, to reduce inappropriate referrals to secondary care, and to produce a more informative referral letter.
November 2004 Br J Cardiol 2004;11:487-91
Statins in primary care: bridging the treatment gap
Rubin Minhas

Audits of cholesterol management in patients with coronary heart disease (CHD) demonstrate that many patients do not achieve targets set out in national guidelines. Under-treatment is a component of the treatment gap and many patients are prescribed low-dose statins. The delivery of systematic care and adoption of more efficacious initial doses will increase the number of patients who achieve recommended low-density lipoprotein cholesterol (LDL-C) levels and maintain their LDL-C goals. Current studies indicate that rosuvastatin, atorvastatin and simvastatin are the most efficacious agents for lowering LDL-C and triglycerides. Compliance and persistence with statin treatment are poor and represent significant barriers to delivering mortality reductions in clinical practice. Efforts to improve concordance are necessary to ensure that treatment benefits are realised in clinical practice.
November 2004 Br J Cardiol 2004;11:483-5
Chest pain induced by 5-fluorouracil
David JB Thomas, Anita Sarker, Robert Glynne-Jones

Five-fluorouracil (5-FU) is commonly used to treat solid tumours, and in palliative and adjuvant chemotherapy. The agent 5-FU is being used in ever-increasing dosage, and this results in more side effects.
November 2004 Br J Cardiol 2004;11:479-82
Carotid artery disease: stenting, endarterectomy or medical therapy?
Mitchell M Lindsay, Keith G Oldroyd

Carotid artery disease is a major cause of stroke. Carotid endarterectomy when performed with a low complication rate in patients with severe lesions has been shown to reduce the subsequent risk of stroke in a series of randomised controlled trials in both symptomatic and asymptomatic populations. The CAVATAS trial demonstrated that simple balloon angioplasty of carotid stenoses was as good as endarterectomy in terms of stroke prevention and was associated with a lower complication rate. Carotid stenting performed with the use of distal protection devices has been shown to be superior to endarterectomy in patients considered to be at increased perioperative risk as assessed by a variety of clinical and angiographic parameters. Comparisons of carotid stenting and endarterectomy in patients considered to be of normal perioperative risk are ongoing. Optimal medical therapy is mandatory for all patients with carotid artery disease.
November 2004 Br J Cardiol 2004;11:478
Cerebral and pulmonary embolic disease in association with an atrial septal aneurysm
Paresh A Mehta, Simon W Dubrey, Richard Grocott-Maso

This image shows a non-communicative atrial septal aneurysm (ASA), as seen on trans-oesophageal echocardiography, in a 57-year-old man with multiple cerebral and pulmonary emboli. He was a non-smoker, with no risk factors for cardiovascular disease.
November 2004 Br J Cardiol 2004;11:474-7
Adherence to anticoagulation guidelines for atrial fibrillation: a district general hospital survey
Paresh A Mehta, Richard Grocott-Mason, Simon W Dubrey

Atrial fibrillation (AF) is the commonest sustained cardiac arrhythmia and a significant cause of hospital admission, morbidity and mortality. AF significantly increases the risk of embolic stroke, and anticoagulation with warfarin can reduce this risk by up to 61%. International guidelines recommend the use of warfarin for atrial fibrillation in patients considered at higher risk for stroke. This prospective observational study evaluates current adherence to anticoagulation guidelines for patients with atrial fibrillation. It was carried out in a district general hospital in London on 93 patients with atrial fibrillation admitted via the emergency department over a four-month period. Patients’ mean age was 77 years and the mean age of onset of AF was 75 years. Eighty-eight per cent of patients were > 75 years and/or had another risk factor for embolic stroke requiring warfarin therapy. Anticoagulation treatment did not adhere to guidelines in 56% of patients at the time of hospital admission. This proportion fell slightly to 52% at the time of hospital discharge. A total of 20% of patients were discharged on no anticoagulation at all. The adherence to anticoagulation guidelines for patients with atrial fibrillation, who are at risk of embolic stroke, appears inadequate. Despite the evidence supporting oral anticoagulation, clinical practice seems resistant to change. The future may include patient self-monitoring and the use of oral direct thrombin inhibitors to improve stroke prophylaxis.
November 2004 Br J Cardiol 2004;11:468-73
Maximising the benefit from pre-operative cardiac evaluation for elective, non-cardiac surgery
Jonathan MT Pierce, Oliver Allenby-Smith, Jonathan Goddard

The objective of this study was to examine the association of delusional and real memories for events with both the pre-operative and early post-operative clinical condition and to examine interventional, supportive and therapeutic factors. Its design was retrospective, using a questionnaire and review of clinical records. The study was carried out in a university teaching hospital cardiothoracic intensive care unit (ICU) on 161 patients without professional experience of intensive care, who had received four days or more in intensive care after cardiac surgery. Its main outcome measures were the prevalence of delusional memory persisting after recovery and the recall of real events whilst in intensive care. Seventy-eight (48%) patients recalled events apparently occurring whilst in intensive care, which were delusional or hallucination-like (‘dreamers’). This group recalled a mean of 2.6 of a possible 10 normal intensive care events compared with 1.0 of 10 for those who were not able to recall delusions or hallucinations (‘non-dreamers’). Dreamers were younger at the time of surgery (mean age 63.6 vs. 68.9 years, p=0.003). Dreaming was more common in patients who received intravenous glucose (to treat hypoglycaemia), midazolam, steroids and in those with episode(s) of sepsis. We concluded vivid memory of unreal events is common after discharge from intensive care. The aetiology is probably multifactorial. The retrospective nature and the inexact methods preclude confirming that midazolam is a direct, much less a causal, risk factor. However, the association is strong enough to warrant prospective studies.
November 2004 Br J Cardiol 2004;11:462-66
Delusional memories following cardiac surgery and prolonged intensive care: a retrospective survey and case note review
Jonathan MT Pierce, Oliver Allenby-Smith, Jonathan Goddard

The objective of this study was to examine the association of delusional and real memories for events with both the pre-operative and early post-operative clinical condition and to examine interventional, supportive and therapeutic factors. Its design was retrospective, using a questionnaire and review of clinical records. The study was carried out in a university teaching hospital cardiothoracic intensive care unit (ICU) on 161 patients without professional experience of intensive care, who had received four days or more in intensive care after cardiac surgery.
Its main outcome measures were the prevalence of delusional memory persisting after recovery and the recall of real events whilst in intensive care. Seventy-eight (48%) patients recalled events apparently occurring whilst in intensive care, which were delusional or hallucination-like (‘dreamers’). This group recalled a mean of 2.6 of a possible 10 normal intensive care events compared with 1.0 of 10 for those who were not able to recall delusions or hallucinations (‘non-dreamers’). Dreamers were younger at the time of surgery (mean age 63.6 vs. 68.9 years, p=0.003). Dreaming was more common in patients who received intravenous glucose (to treat hypoglycaemia), midazolam, steroids and in those with episode(s) of sepsis.
We concluded vivid memory of unreal events is common after discharge from intensive care. The aetiology is probably multifactorial. The retrospective nature and the inexact methods preclude confirming that midazolam is a direct, much less a causal, risk factor. However, the association is strong enough to warrant prospective studies.
November 2004 Br J Cardiol 2004;11:455-60
Should all diabetic patients receive a statin? Results from recent trials
Gillian Marshall, Claire McDougall, Adrian JB Brady, Miles Fisher

Diabetes is associated with the development of premature cardiovascular disease. In the three early trials of statin therapy for patients with established coronary heart disease there were many patients with diabetes; subgroup analysis has confirmed the benefits of cholesterol lowering with statin therapy in these patients. In the two early primary prevention trials, however, there were few patients with diabetes and so, initially, there was little evidence supporting the use of statins in diabetic patients without cardiovascular disease. The Heart Protection Study (HPS) and Collaborative AtoRvastatin Diabetes Study (CARDS) have now provided this evidence and firmly established that cholesterol lowering is of benefit in reducing cardiovascular events in patients with type 2 diabetes, regardless of the level of baseline cholesterol, or the presence or absence of cardiovascular disease. A few recent studies have failed to find benefit in diabetic patients but there are explanations for these negative findings. Ideally all patients with diabetes, especially the middle-aged and elderly, should be treated with statins but it remains uncertain at what age therapy should start and how low to reduce the cholesterol for maximum benefit.
November 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 80–AIC 84
Future devices: bioabsorbable stents
Huw Griffiths, patrick Peeters, Jan Verbist, Marc Bosiers, Koen Deloose, Bernhard Heublein, Roland Rohde, Viktor Kasese, Charles Ilsley, Carlo Di Mario

There are many advantages to bioabsorbable stents, including the potential to inhibit intimal hyperplasia by avoiding prolonged foreign body reaction and/or releasing antiproliferative drugs during degradation. The bioabsorbable polymer poly-l-lactic acid (PLLA) is used as a biodegradable coating of permanent metallic stents but can also be used to manufacture complete stents, at the expense of a greater recoil. Clinical, angiographic and intravascular ultrasound results at four years with the first stent tested (Igaki Tamai, Igaki, Japan) show patency rates similar to the rates expected with stainless steel stents and full reabsorption. Magnesium stents are another, perhaps more encouraging, development because they retain mechanical properties similar to conventional metallic stents. Full degradation of the magnesium alloy used to manufacture the Biotronik Lekton Magic stent requires 6–8 weeks. In man, initial clinical experience with this stent has been gained in patients with critical lower limb ischaemia. An ongoing study is testing its safety and efficacy in human coronary arteries.
November 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 85–AIC 88
Bivalirudin in percutaneous coronary intervention
Daniel J Blackman, Adrian P Banning

Bivalirudin is a direct thrombin inhibitor that will be available in the UK in November 2004 as adjunctive anticoagulant therapy during percutaneous coronary intervention (PCI). Its mechanism of action offers potential advantages over heparin in terms of both efficacy and bleeding. Bivalirudin is convenient – ACT monitoring is unnecessary, infusion is only for the duration of the procedure, and half-life is short so that early sheath removal and ambulation are possible. Finally, bivalirudin may offer major cost savings over glycoprotein (GP) IIb/IIIa inhibitors. The REPLACE-2 trial demonstrated equivalent efficacy and reduced bleeding with bivalirudin alone versus heparin-plus-GP IIb/IIIa inhibition in 6,010 patients undergoing elective or urgent PCI (30-day MACE 7.6% vs. 7.1%, major bleeding 2.4% vs. 4.1%). Further trials are underway to evaluate the efficacy of bivalirudin during PCI for high-risk acute coronary syndromes (ACS) and acute myocardial infarction (AMI). This paper considers when bivalirudin should be used in contemporary PCI. The ISAR-REACT study provides firm evidence that heparin alone is safe and effective for elective PCI in low-to-moderate risk patients (30 day MACE 4% heparin-alone vs. 4% abciximab). Patients with AMI or unstable ACS were not included in the REPLACE-2 trial and should continue to receive GP IIb/IIIa inhibitors until further data are available. Bivalirudin could be considered in patients at intermediate risk in whom GP IIb/IIIa inhibitors are currently widely used, including during complex elective PCI, elective PCI in diabetics, and in patients with stabilised or low-risk ACS. Bivalirudin will also have a specific role in patients at increased risk of bleeding and with heparin-induced thrombocytopaenia. Further data are required before more widespread adoption of bivalirudin can be recommended.
November 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 89–AIC 92
An investigation into the prognostic value of the cardiac marker troponin T in patients with suspected acute coronary syndrome without ST segment elevation
Aidan Kirkpatrick, Michael Martin, Philip Lewis, Simon Capewell, Gary Cook, Georgios Lyratzopoulos

This study was set up to investigate the prognostic significance of different bands of troponin T in the diagnosis and management of patients presenting with suspected acute coronary syndrome without ST segment elevation. The study was a cohort study, set in a District General Hospital in the north west of England. The participants were 421 patients admitted with suspected acute coronary syndrome without ST segment elevation over a three-month period. Analysis was carried out depending on whether the level of troponin elevation was in a negative (< 0.03 µg/L), intermediate (0.03–0.1 µg/L) or positive (> 0.1 µg/L) band. The outcome was a composite of all-cause mortality or hospital admission due to non-fatal myocardial infarction at 30 days and 12 months. Both intermediate and positive levels of elevated troponin increased the risk of all-cause mortality and non-fatal myocardial infarction at least two-fold, both at 30 days and 12 months (p<0.01). People over 50 were found to have a worse prognosis than younger patients at 12 months (p<0.05) but gender had no significant effect. Patients with suspected acute coronary syndromes without ST segment elevation who have either intermediate or positive levels of troponin T show a substantial increase in adverse outcomes during short- and long-term follow-up. Further research is required on these bandings as new generations of troponin assays are developed with improved levels of precision.
November 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 93–AIC 94
Treatment of unprotected left main stem stenosis in an 81-year-old using a rapamycin-coated stent
Sagar N Doshi, Karim Ratib, John Townend

We report a case of unprotected, ostial left main coronary artery disease successfully treated with a rapamycin-coated ‘Cypher’ stent in an 81-year-old woman who was declined for coronary artery bypass surgery because of significant co-morbidity.
September 2004 Br J Cardiol 2004;11:408-12
Beta blocker therapy for patients with heart failure in primary care
David Wald, Sarah Milne, Richard Chinn, Margaret Martin, Ranjit More

Beta blockers are under-used in heart failure, despite their evident benefits. Here an educational and clinical support link between secondary and primary care was set up to mentor a nurse practitioner in heart failure management. A nurse-led heart failure clinic was established in a Hampshire general practice that enabled beta blocker therapy to be started safely and up-titrated successfully, without hospital referral.
September 2004 Br J Cardiol 2004;11:405-7
Echocardiography in the community
Ed Southall

In the second commentary on echocardiography in the community, general practitioner Ed Southall writes about the new British Society of Echocardiography accreditation process and his own experiences in running a community echocardiography service in South Devon.
September 2004 Br J Cardiol 2004;11:393-6
The treatment of peripartum cardiomyopathy
Stephen J Leslie, Yaso Emmanuel, C Mark Francis, Andrew D Flapan

Peripartum cardiomyopathy (PPCM) is characterised by the development of left ventricular (LV) dilatation and dysfunction during the last month of pregnancy, or the first five months of the post-partum period, in the absence of any pre-existing cardiac disease. PPCM is a rare but serious complication of pregnancy, with a variable outcome. Symptoms such as breathlessness and peripheral oedema are common in normal pregnancy and it is easy to misdiagnose PPCM in its early stages. The aetiology of the condition is uncertain.
Treatment options are similar to those for other forms of dilated cardiomyopathy. However, there are important considerations when treating women with PPCM as they may be pregnant or breast feeding. Close communication is required between cardiologists, obstetricians and neonatologists, not only for the treatment of the PPCM patient but also for protection of the baby. Women who decide to continue with further pregnancies should be carefully monitored.
September 2004 Br J Cardiol 2004;11:388-92
Lowering blood pressure for the secondary prevention of stroke
Joanna K Lovett

Hypertension is the most important modifiable risk factor for stroke. The risk of stroke increases directly in proportion to systolic and diastolic blood pressure, and lowering blood pressure can reduce the risk of a first stroke by up to 40%. Current evidence suggests that it is safe and effective to lower blood pressure with an ACE inhibitor and a thiazide diuretic in patients with established cerebrovascular disease. The reduction in subsequent stroke is present both in hypertensive and non-hypertensive patients and is most likely to be related directly to the blood pressure- lowering effect. Ongoing studies will help to determine whether other classes of drugs, such as the angiotensin receptor blockers, are also safe and effective in the secondary prevention of stroke, and whether blood pressure should be lowered in the first few days after a major stroke.
July 2004 Br J Cardiol 2004;11:307-9
Is provision and funding of cardiac rehabilitation services sufficient for the achievement of the National Service Framework goals?
Ingolf Griebsch, Jackie Brown, Andrew D Beswick, Karen Rees, Robert West, Fiona Taylor, Rod Taylor, Jackie Victory, Margaret Burke, Sally Turner, Hugh Bethell, Shah Ebrahim

The objectives of this analysis were to ascertain the population need for out-patient cardiac rehabilitation in England, to estimate the current level of provision and associated costs, to identify economies of scale in service provision and to investigate budgetary implications of extending provision. Discharge statistics from the Hospital Episode Statistics database (HES) in England in the year 2000, and data from centres contributing to the British Association for Cardiac Rehabilitation (BACR) survey were analysed. A short follow-up questionnaire was sent to respondents of the BACR survey. The main outcome measures were: the number of patients eligible for cardiac rehabilitation; the percentage referred, joining and completing programmes; health service costs associated with current levels of provision; elasticity of costs; and costs associated with expanding services. Using an inclusive definition of need, about 267,000 people required cardiac rehabilitation in England in the year 2000. This figure fell to 100,000 if services were restricted to those aged below 75 years with acute myocardial infarction, unstable angina or following revascularisation. Health service costs per patient completing a programme were £354 (staff) and £486 (total). Out-patient cardiac rehabilitation represented a NHS cost of approximately £12.5–19.0 million per annum. A 1% increase in patients completing a programme is estimated to lead to a 0.25% fall in the staff cost per patient. A budget increase of 630% would be necessary to treat all eligible patients using moderate staffing configurations, which would fall to 170% if only those aged below 75 years with restricted diagnoses were to be treated. We conclude that a substantial proportion of the population need for cardiac rehabilitation goes unmet and that achievement of current targets for provision is likely to require considerable additional resources. Reconfiguration of service provision towards less complex services would enable more patients to be treated. Current information systems in cardiac rehabilitation services are inadequate to provide indicators of performance and monitoring.
July 2004 Br J Cardiol 2004;11:329-32
Integrated Care Pathways – what can we do to make them happen?
Mark Davis

Integrated Care Pathways (ICPs) are one way of implementing protocol-based care. Healthcare professionals need to draft and implement ICPs in order to meet clinical governance targets. In a two-day workshop ‘Integrated healthcare delivery – let’s get practical’, 27 multidisciplinary delegates from four NHS Modernisation Teams progressed ICPs in the areas of stroke, post-myocardial infarction and heart failure. Good ICPs should include a clear assessment procedure for the clinical condition, consultation with all care providers, guidelines or best available clinical evidence, patient education and an audit tool.
July 2004 Br J Cardiol 2004;11:326-8
The new NHS: changing the face of British cardiology
Ola Soyinka

The titles of the lectures at a recent Primary Care Cardiovascular Society (PCCS) meeting show the face of British cardiology is indeed changing. Control of NHS budgets and of patient care is shifting; guidelines for prevention of disease continue to change in line with new evidence; new ways of learning are being developed and yet more new laboratory tests are being pressed into service. As usual the PCCS speakers articulately covered the topics – they also had to be succinct as, after just 90 minutes, the session was over and it was ‘all change’ for the audience. Medical writer Ola Soyinka reports from the PCCS plenary session at the British Cardiac Society Annual Conference in Manchester on 25th May 2004.
July 2004 Br J Cardiol 2004;11:323-5
An evidence-based audit of coronary heart disease clinics
Patrick McElduff, Richard Edwards, Andreas P Arvanitis, Janis Holloway,

The National Service Framework (NSF) for Coronary Heart Disease (CHD) requires practices to establish registers of patients with CHD and to implement audits of care for these patients. Little is known about the potential health impact of registers and audits. We therefore looked at the impact of establishing such systems on patients with CHD at Cleveleys Group Practice. All patients with CHD are recorded on a computerised register that is used to recall patients for an annual review to nurse-led clinics. Data from annual audits are used to estimate the number of adverse events prevented in the practice by the use of effective medications. We found that the use of effective treatments was estimated to save approximately 27 lives and prevent 30 non-fatal myocardial infarctions each year. The increased use of effective treatments after the introduction of the register coincided with a reduction in average levels of systolic blood pressure and total cholesterol, preventing two deaths and three non-fatal myocardial infarctions each year. Based on the best available evidence from randomised controlled trials, the benefit of this care to a practice population is substantial.
July 2004 Br J Cardiol 2004;11:315-20
Angiotensin II receptor blockers: a new lease of LIFE?
Michael Kirby, Rubin Minhas

The National Service Framework (NSF) for Coronary Heart Disease (CHD) requires practices to establish registers of patients with CHD and to implement audits of care for these patients. Little is known about the potential health impact of registers and audits. We therefore looked at the impact of establishing such systems on patients with CHD at Cleveleys Group Practice. All patients with CHD are recorded on a computerised register that is used to recall patients for an annual review to nurse-led clinics. Data from annual audits are used to estimate the number of adverse events prevented in the practice by the use of effective medications. We found that the use of effective treatments was estimated to save approximately 27 lives and prevent 30 non-fatal myocardial infarctions each year. The increased use of effective treatments after the introduction of the register coincided with a reduction in average levels of systolic blood pressure and total cholesterol, preventing two deaths and three non-fatal myocardial infarctions each year. Based on the best available evidence from randomised controlled trials, the benefit of this care to a practice population is substantial.
July 2004 Br J Cardiol 2004;11:312-4
A case of spontaneous tension pneumopericardium
Simon Stacey, Alex W Green, Richard A Best

Pneumopericardium is a rare condition, seen most commonly in the context of chest trauma in adults, and in mechanical ventilation in neonatal practice. Mortality is high, more so if pericardial gas is accompanied by pus and, ultimately, tamponade.1 Here we present a case of tension pyopneumopericardium leading to cardiac tamponade which had a favourable outcome. The aetiology remains uncertain in this instance, although an oesophagopericardial fistula cannot be discounted. In addition, we review the causes and clinical features of this condition as reported in the literature.
July 2004 Br J Cardiol 2004;11:310-11
Phase 4 cardiac rehabilitation: a comparison of exercise intensity levels and ratings of perceived exertion between cardiac and non-cardiac participants
Lynn H Angus, Heather G Gray

Meta-analyses of exercise-based cardiac rehabilitation (CR) trials have shown improved survival1,2 and significant improvements in cardio-respiratory fitness for individuals who have sustained a myocardial infarction (MI).3 According to the British Association of Cardiac Rehabilitation (BACR) Exercise Prescription Guidelines, phase 4 cardiac participants should exercise at a similar intensity level to that recommended for healthy adults to gain maximum benefits.4 To date, however, there has been a paucity of research to support or question these guidelines. This led to this pilot study, which aimed to compare the exercise intensity levels and ratings of perceived exertion of cardiac and non-cardiac participants during a phase 4 CR exercise class.
July 2004 Br J Cardiol 2004;11:302-5
Provision of rehabilitation services to patients with implanted cardioverter defibrillators: a survey of UK implantation centres
Dorothy J Frizelle, Robert JP Lewin, Gerry C Kaye

This study investigated the current level of provision of cardiac rehabilitation (CR) for automatic implanted cardioverter defibrillator (ICD) patients in the UK, the clinical and technical staff views on the need for such a service, and the current level of provision and the most commonly reported barriers to meeting these needs. The study was carried out via a postal questionnaire survey of all NHS implantation centres for ICD patients. The majority of respondents (99%) believed they should provide rehabilitation for their patients, but only 14 (36%) centres had a programme for rehabilitation that ICD patients could access and only four (10%) of these were specifically designed for ICD patients. The majority of respondents (74%) believed they were not meeting their patients’ needs for rehabilitation. The most commonly endorsed barriers to providing and developing CR services were limited multidisciplinary staff, a wide geographical catchment area, and administrative and organisation difficulties. There was wide support for the potential of using a home-based, remotely monitored, rehabilitation package. This shows that the vast majority of staff in implantation centres agree with the recent NICE recommendations that there is an unmet need to provide CR for ICD patients.
July 2004 Br J Cardiol 2004;11:300-1
Development of the BACR/BHF minimum dataset for cardiac rehabilitation
Robert JP Lewin, David R Thompson, Alun Roebuck

This article describes the process used to arrive at the set of assessment measures and minimum dataset for cardiac rehabilitation (CR) that has been endorsed by the British Association for Cardiac Rehabilitation (BACR) and the British Heart Foundation (BHF) for the national audit of CR.
July 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 45–AIC 52
Role of LMWH in ACS, with or without PCI and GP IIb/IIIa blockade
Diana A Gorog, Alamgir MN Kabir, Michael S Marber

Low molecular weight heparin (LMWH) and unfractionated heparin (UFH) are used to prevent rethrombosis and distal platelet embolisation in acute coronary syndromes. LMWH have a more predictable anticoagulant response and are less likely to result in bleeding. For the moment UFH should be used in primary percutaneous coronary intervention (PCI). It may also be preferable to use UFH in the setting of rescue PCI following tenecteplase (TNK) treatment. In those over 75 years of age, the combination of TNK with enoxaparin has been shown to be superior to TNK with UFH in reducing ischaemic end points without increasing the risk of haemorrhage. Results from TIMI IIB indicate that enoxaparin is superior to UFH for the acute management of non-ST elevation ACS (in patients managed conservatively). Enoxaparin and UFH appear to have similar efficacy and safety profiles when used in conjunction with glycoprotein IIb/IIIa blockade during PCI.
July 2004 Br J Cardiol 2004;11:292-9
Hypercholesterolaemia and its potential role in the presentation and exacerbation of hypertension
Andrei C Sposito, Jose Augusto S Barreto-Filho

Hypertension is a major cardiovascular risk factor and its pathogenesis remains elusive. For a long time, hypertension and dyslipidaemia have been viewed as independent but synergistic cardiovascular risk factors increasing the risk of premature atherosclerosis. Recently, a growing body of evidence has indicated that hypercholesterolaemia promotes impairment in several mechanisms implicated in blood pressure control such as nitric oxide bioavailability, renin-angiotensin activity, the sympathetic nervous system, sodium and fluid homeostasis and ion transport/signal transduction. Moreover, recent clinical studies have pointed out a beneficial effect of cholesterol-lowering treatment in reducing blood pressure to a small but significant degree. Our assumption is that depending on the complex inter-relationships between genetic background and life style, hypercholesterolaemia may be a trigger to blood pressure elevation. An integrated approach to the treatment of hypertension and dyslipidaemia can, therefore, maximise both blood pressure control and prevention of cardiovascular disease. In this review, we discuss recent important data from our and other groups, demonstrating the clinical evidence of the hypertensinogenic effects of hypercholesterolaemia, and the biological mechanisms which underlie them.
July 2004 Br J Cardiol 2004;11:287-90
Diurnal rhythms, the renin-angiotensin system and antihypertensive therapy
Michael Schachter

The circadian rhythms of the cardiovascular system are related to the risk of events such as myocardial infarction and stroke. The so-called ‘morning surge’ in heart rate and blood pressure at around the time of waking is a particularly hazardous period. The sympathetic nervous system and the renin-angiotensin system are thought to be the main regulators of these rhythms and a potential target of antihypertensive medication is the blunting of the morning surge through action on these systems. This article reviews some of the mechanisms involved and recent therapeutic approaches to this problem.
July 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 53–AIC 61
Contrast-induced nephropathy
Tadhg G Gleeson, John O’Dwyer, SuDi Bulugahapitiya, David P Foley

The use of coronary angiography as a diagnostic tool in modern hospital medicine continues to rise. With the increasing use of therapeutic coronary interventions, and the increases in procedure times and volumes of contrast media, incidence rates of contrast-induced nephropathy (CIN) have also been seen to climb over recent years. CIN has subsequently been shown to be a significant contributor to morbidity and mortality during hospitalisation. In this current clinical setting, it is incumbent on the modern cardiologist to be aware of this potentially serious complication of angiography, to be familiar with its presentation and treatment, and to be able to recognise at-risk groups and institute prophylactic measures where appropriate.
July 2004 Br J Cardiol 2004;11:282-6
The National Cholesterol Education Program III scoring system for CHD risk estimation cannot be used with European recommendations
Navneet Singh, See Kwok, C Jeffrey Seneviratne, Michael France, Paul Durrington

To target statin therapy effectively in primary coronary heart disease (CHD) prevention, recommendations increasingly advocate the assessment of absolute CHD risk. Using methods from two recent sets of national recommendations, we estimated absolute CHD risk in 412 men and women whose general practitioners requested it on clinical grounds. Substantially fewer men and women had CHD risk exceeding 15%, 20% and 30% over 10 years with the National Cholesterol Education Program III (NCEP III) scoring system than with the Joint British charts. The latter agreed closely with the 1990 version of the Framingham risk equations.
July 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 62–AIC 67
The pulmonary artery catheter – a personal view
Adrian Steele

The pulmonary artery catheter (PAC) was introduced into critical care medicine without objective evidence of its efficacy. The direct risks from the PAC are around 1.5% for a serious complication and 0.2% for death. The Connors study on 5,735 intensive care patients used case-matching techniques, and demonstrated a worse outcome in the PAC cohort. However, in this study the need for inotropes and the response to treatment were excluded from the regression analysis. Three further studies have failed to show an association between PAC placement and outcome after case-mix adjustment. It has proved extremely difficult to recruit enough intensive care patients to exclude a clinically important mortality benefit of the PAC. New techniques such as the oesophageal Doppler, pulse contour continuous cardiac output and lithium dilution cardiac output machines offer simpler, and perhaps better, alternatives to the PAC. Nonetheless, even if future trials are negative, the PAC should remain available for treatment of patients with unusual conditions or combinations of conditions.
July 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 68–AIC 69
Isolated ventricular non-compaction presenting as acute myocardial infarction
Divaka Perera, Dudley J Pennell, Barry J Kneale

Isolated ventricular non-compaction is a rare cardiomyopathy, which is probably underdiagnosed. We describe a case manifested by chest pain, indistinguishable from acute myocardial infarction.
July 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 70–AIC 72
Emergency non-surgical epicardial catheter ablation of incessant ventricular tachycardia in a man with dilated cardiomyopathy
Mark J Earley, Michael AJ Park, Richard J Schilling

Ventricular tachycardia (VT) and sudden cardiac death are feared complications of severe heart failure, whatever the aetiology. VT has the propensity to become incessant, and this carries an adverse prognosis. In some cases incessant VT is refractory to a combination of electrical cardioversion and pharmacological therapy such that emergency catheter ablation is required. Even when the conventional endocardial approach fails, ablation can be performed safely and effectively via the epicardial route.
May 2004
British Hypertension Society Guidelines 2004 – BHS IV. Ten key comments for primary care
Mike Mead

The latest British Hypertension Society guidelines, BHS IV, have particular implications for primary care. This article discusses 10 key areas on which general practitioners should focus as a result of the new guidance, with a comment about the significance of each in a primary care setting.
May 2004 Br J Cardiol 2004;11:243-45
Angiotensin-converting enzyme inhibitor prescription for heart failure in general practice, and the impact of a Rapid Access Heart Failure Clinic in Cardiff
Pitt O Lim, Gary Lane, Jayne Morris-Thurgood, Michael P Frenneaux

We assessed whether the presence of a Rapid Access Heart Failure Clinic (RAHFC) had an impact on the angiotensin-converting enzyme (ACE) inhibitor prescribing habits of primary care physicians. We selected 10 general practices (GP) that referred and 10 practices that did not refer patients to the RAHFC. The study covered a period of two years immediately preceding the commencement of the RAHFC and about 1.5 years afterwards. A total of 309 patients, divided into two groups, were studied. Cohort 1 consisted of 198 patients (103 from referring and 95 from non-referring GP) with a new diagnosis of chronic heart failure (CHF) made by the GP pre-RAHFC. Cohort 2 consisted of 111 patients (48 from referring and 63 from non-referring GP) diagnosed as having CHF post-RAHFC. In cohort 1, 27.1% of patients in the referring practices were on ACE inhibitor versus 40.0% in the non-referring practices (p=0.056). ACE inhibitor prescription was reassessed 1.5 years post-RAHFC: it had significantly increased to 51.4% (p<0.001) in the referring practices, but not in the non-referring practices (43.1%, p=0.659). Interestingly, the increase in ACE inhibitor prescription among referring practices was predominantly due to initiation by the primary care physicians themselves (76% of cases) rather than by the RAHFC. The baseline trend of lower ACE inhibitor prescription rate in cohort 1 in the referring practices compared to non-referring practices was not seen in cohort 2 (54.1% vs. 50.7%, p=0.844). Using ACE inhibitor prescription status as an indicator of diagnostic certainty of CHF by primary care physicians, it has sensitivity, specificity, positive and negative predictive values of 45.5%, 52.9%, 38.5% and 60.0%, respectively, for the presence of CHF as confirmed by the RAHFC. In conclusion, RAHFC facilitated increased ACE inhibitor prescription by primary care physicians. However, CHF was commonly misdiagnosed in the community and this might lead to inappropriate ACE inhibitor prescription.
May 2004 Br J Cardiol 2004;11:239-41
Paradoxical embolism causing cerebral infarction in a young man with hereditary haemorrhagic telangiectasia
Vijaya Lakshmi, Chinmoy K Maity

Paradoxical embolism is a relatively uncommon clinical condition. Only a few hundred cases have been reported in the literature.1 Despite sophisticated technological advances, it remains an under-diagnosed clinical entity.2 Blood clots formed either in the right side of the heart or in the venous circulation escape via an intra- or extra-cardiac right-to-left shunt into the systemic circulation. This results in an arterial embolism, hence the term paradoxical embolism. The condition can cause significant morbidity and mortality. We report a case of cerebral infarction secondary to paradoxical embolism. This is the first case to be reported in the literature with the unique and rare association of patent foramen ovale and pulmonary arteriovenous malformation with hereditary haemorrhagic telangiectasia.
May 2004 Br J Cardiol 2004;11:235-8
Driving and the doctor: awareness of current driving regulations for cardiovascular conditions amongst doctors and nurses
Joseph de Bono, Lucy Hudsmith, Grant Heatlie

Many common cardiovascular conditions preclude patients from driving for a period of time. These regulations often affect previously fit people and may have far-reaching consequences for an individual. The doctors caring for these patients are responsible for informing them of any relevant driving restrictions. We present a survey of general physicians’ and cardiac specialist nurses’ understanding of the current Driver and Vehicle Licensing Authority (DVLA) regulations. Overall, there is a limited knowledge of driving regulations among physicians as a group (36% correct responses). In contrast to their poor knowledge with respect to cardiovascular conditions (30% correct), a far higher proportion of physicians knew when a patient could return to driving following an epileptic seizure (76%, p<0.001). Consultants fared better than their junior colleagues, with 41% of questions answered correctly; specialist cardiac nurses had a correct response rate of 57% for cardiac events. Most of the wrong responses overestimated the duration of the restrictions, suggesting a conservative attitude to advice offered.
May 2004 Br J Cardiol 2004;11:229-34
Ximelagatran: the future in anticoagulation practice?
Ali Hamaad, Muzahir H Tayebjee, Gregory YH Lip

Recent years have shown a diverse array of new antithrombotic drugs in development or appearing in clinical practice. Until now, warfarin has remained the anticoagulant drug of choice despite the numerous disadvantages associated with its use. Ximelagatran, an oral direct thrombin inhibitor (DTI), has now emerged as a serious contender to replace warfarin as standard anticoagulation. Its use in prophylaxis and treatment of venous thromboembolic disease is already well established and recent data also suggest the benefits of ximelagatran over warfarin in non-valvular atrial fibrillation, both in terms of safety and efficacy. This review will examine ximelagatran as a novel anticoagulant with its application in numerous clinical settings, such as venous thromboembolism and non-valvular atrial fibrillation, and how it may one day replace warfarin as the anticoagulant of choice.
May 2004 Br J Cardiol 2004;11:224-8
Bradycardia and tachycardia occurring in older people: investigations and management
Colin Berry, Andrew C Rankin, Adrian JB Brady

In the elderly, the investigation of symptoms potentially due to an arrhythmic cause is similar to that for a younger person. In many cases, however, a history obtained from a friend or relative can be valuable. Routine investigations should include tests of thyroid function, an electrocardiogram (ECG), and ambulatory ECG recording. In patients without cerebrovascular disease, carotid sinus massage with continuous ECG monitoring should be performed. The role of device therapy in the management of arrhythmias in patients of all ages is increasing. Permanent pacing can improve symptoms and prognosis in patients with certain bradycardia, and the indications for pacing are available in contemporary international guidelines. Recent developments in device therapy include multisite pacing and implantable cardioverter defibrillators. Emerging data suggest that these devices can be used to good effect in selected elderly patients.
May 2004 Br J Cardiol 2004;11:218-23
The cost of coronary artery disease in the UK
Arran Shearer, Paul Scuffham, Patrick Mollon

In the elderly, the investigation of symptoms potentially due to an arrhythmic cause is similar to that for a younger person. In many cases, however, a history obtained from a friend or relative can be valuable. Routine investigations should include tests of thyroid function, an electrocardiogram (ECG), and ambulatory ECG recording. In patients without cerebrovascular disease, carotid sinus massage with continuous ECG monitoring should be performed. The role of device therapy in the management of arrhythmias in patients of all ages is increasing. Permanent pacing can improve symptoms and prognosis in patients with certain bradycardia, and the indications for pacing are available in contemporary international guidelines. Recent developments in device therapy include multisite pacing and implantable cardioverter defibrillators. Emerging data suggest that these devices can be used to good effect in selected elderly patients.
May 2004 Br J Cardiol 2004;11:205-10
Outcomes guarantee for lipid-lowering drugs: results from a novel approach to risk sharing in primary care
Stephen Chapman, Elly Reeve, David Price, Giri Rajaratnam, Richard Neary

Current guidelines emphasise the importance of lipid management in secondary prevention of coronary heart disease (CHD). This audit of lipid levels and lipid-modifying therapy was undertaken in 1,736 patients, 919 men and 817 women, who were either attending a lipid clinic in inner-city Britain (n=1,035, 60%) or a general practice surgery covering 9,500 patients (n=701, 40%). Patient data were obtained from review of case notes and latest results for serum total, low-density lipoprotein (LDL-C) and high-density lipoprotein cholesterol (HDL-C) were categorised in accordance with UK guideline targets (total cholesterol < 5 mmol/L, LDL-C < 3 mmol/L and HDL-C > 1 mmol/L). Overall, 48% of men and 61% of women had raised total cholesterol levels above target and 23% of men and 8% of women had low levels of HDL-C; these proportions were generally consistent for individual centre data. Amongst patients with established CHD who were receiving statin therapy, 31% of men and 47% of women had raised total cholesterol levels above target and 24% of men and 8% of women had low HDL-C levels. This suggests that a substantial proportion of patients at risk of developing or with established CHD, either attending general practice or a specialist lipid clinic, fail to meet recommended lipid targets. Redress of this failure requires more aggressive management, possibly with multidrug lipid-modifying therapy.
May 2004 Br J Cardiol 2004;11:195-04
Management of coronary artery disease: implications of the EUROPA trial
Kim M Fox

The recent EUropean trial on Reduction Of cardiac events with Perindopril in stable coronary Artery disease (EUROPA) examined the effect of treatment with the angiotensin-converting enzyme (ACE) inhibitor perindopril in 12,218 patients with stable coronary artery disease (CAD). After 4.2 years, treatment with perindopril 8 mg once daily resulted in a 20% relative risk reduction in the primary end point, a composite of cardiovascular death, non-fatal myocardial infarction, and cardiac arrest (p=0.0003). Risk reductions were also observed for secondary end points, including fatal and non-fatal myocardial infarction (24% reduction, p<0.001) and hospitalisation for heart failure (39% reduction, p=0.002). These benefits were observed on top of standard recommended preventive therapies such as antiplatelet agents, beta blockers and lipid-lowering drugs. Benefits were consistent for all patients with CAD, irrespective of the presence or absence of risk factors such as age, diabetes, hypertension, previous myocardial infarction, or previous revascularisation. Perindopril, a lipophilic tissue ACE inhibitor which binds strongly to ACE, has several anti-atherogenic actions and vascular properties which may contribute to its protective effect. EUROPA is the first trial to show the benefit of ACE inhibition in a broad population often seen in daily clinical practice. The results suggest that perindopril should be added to other recommended preventive treatments in all patients with CAD.
March 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 14–AIC 16
Debulking of malignant cardiac tumour discovered at operation for presumed right atrial thrombus obstructing the tricuspid valve
Mohamad N Bittar, Shukri Mushahwar, John A Carey

Primary cardiac lymphomas (PCL) are rare neoplasms. They occur at any age and are rare in immunocompetent patients, accounting for 1.3% of all cardiac tumours and 0.5% of all extranodal lymphomas. PCL have been increasingly found in patients with acquired immune deficiency syndrome (AIDS).1 PCL are difficult to diagnose, especially during the early stages of the disease when their manifestations are non-specific.2 Discovery of a malignant cardiac tumour at operation would usually be managed by biopsy and closure without resection, and inevitably would result in early mortality. We report a patient who is alive 12 months after resection of a primary cardiac non-Hodgkin’s B cell lymphoma.
March 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 17–AIC 23
Advanced pacing techniques in congestive heart failure
John R Paisey, John M Morgan

Heart failure is an increasingly common condition for which device therapy, including the advanced pacing technique cardiac resynchronisation therapy, is becoming an accepted treatment. In this review we discuss the rationale, evidence base, indications, limitations and implant technique of this maturing treatment modality and speculate on expansion of its role in the near future.
March 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 24–AIC 32
Management of heart failure and the role of the new inotrope levosimendan
Nicholas Ioannou, Duncan LA Wyncoll

Despite the availability of an array of medical therapies for the treatment of heart failure, quality of life is often poor for the majority of patients, and the mortality remains high. In addition, treatment is regularly not well tolerated and this results in frequent hospital admissions for some patients. This article reviews the management and medical treatment of acute heart failure, focusing on the emerging role of levosimendan. Levosimendan is currently licensed in 10 European countries (Simdax, Orion Pharma, Finland) for the treatment of acute heart failure. It is a new inotropic drug with a dual mechanism of action: sensitisation of the cardiac myofilament to calcium, thus enhancing cardiac contractility, and vasodilation of vascular smooth muscle. The published clinical studies so far have utilised intravenous levosimendan. However, the agent is also well absorbed orally, and phase two trials of its use in stable patients with less severe heart failure are underway.1
March 2004 Br J Cardiol 2004;11:162-8
Cardiac rehabilitation in the UK 2000 – can the National Service Framework milestones be attained?
Hugh JN Bethell, Sally C Turner, Julia A Evans

Cardiac rehabilitation offers physical, psychological and survival benefits for patients recovering from cardiac illness. This questionnaire survey of all known cardiac rehabilitation units in the UK provides data on how well the National Service Framework targets for cardiac rehabilitation are being met.
March 2004 Br J Cardiol 2004;11:158-60
Antiplatelet therapy – the education gap
Jonathan Morrell

There is a widespread lack of awareness amongst the British public of the link between myocardial infarction and stroke, and about secondary prevention.
March 2004 Br J Cardiol 2004;11:156-7
Neurogenic atrial fibrillation
Anjan Siotia, Rangasamy Muthusamy

Atrial fibrillation (AF) is the commonest sustained arrhythmia encountered in clinical practice. Depending upon its time course, AF can be classified into three categories: paroxysmal, persistent and permanent.
March 2004 Br J Cardiol 2004;11:148-55
Efficacy and safety of fluvastatin ER 80 mg compared with fluvastatin IR 40 mg in the treatment of primary hypercholesterolaemia
William Insull Jr, Adrian D Marais, Ronnie Aronson, Sheryl Manfreda, and the Fluvastatin Study Group

The efficacy and safety of once- or twice-daily immediate-release (IR) fluvastatin 40 mg were compared with those of the extended-release (XL) formulation of fluvastatin 80 mg every night (qpm), which facilitates sustained drug delivery. Patients (n=442) with primary hypercholesterolaemia (Fredrickson types IIa and IIb) were randomised to the three treatment groups in the ratio 1:1:1. Active treatment was administered for 24 weeks, following a four-week placebo/dietary lead-in period. At week 24, the mean reduction in low density lipoprotein cholesterol levels in patients treated with fluvastatin XL 80 mg every night (qpm) (-33.5%) was significantly greater than in the fluvastatin IR 40 mg every night (qpm) group (-23.2%; p<0.001), and similar to the reduction for patients treated with fluvastatin IR 40 mg twice-daily (bid) (-31.4%). Significant and dose-related alterations in other lipid variables were also apparent, particularly for high density lipoprotein cholesterol (10.2% increase) and apolipoprotein A1 and B levels (+11.5% and -24.2%, respectively) in the fluvastatin XL 80 mg qpm group compared with the fluvastatin IR 40 mg qpm group (all p<0.001). Mean triglyceride levels decreased by 14.6% in the fluvastatin XL 80 mg qpm group. Adverse events were generally mild, with no differences in frequency across the groups. Fluvastatin XL 80 mg qpm is a safe and effective lipid-lowering treatment for patients with type II hypercholesterolaemia.
March 2004 Br J Cardiol 2004;11:144-7
Thermography of the human arterial system
Christodoulos Stefanadis

One of the main targets of current research in cardiology is a diagnostic modality able not only to identify vulnerable atherosclerotic lesions but also to monitor the effects of therapeutic interventions on plaque composition. Most of the currently available techniques identify luminal diameter or stenosis, wall thickness or plaque volume, but are not capable of recognising vulnerable plaques that are prone to rupture. Thermography is a new technique which provides insight into the local inflammatory process within the atherosclerotic plaque. In this review we will present in detail the developments and the clinical implications of thermography in the human arterial system.
March 2004 Br J Cardiol 2004;11:138-43
Will prevention of type 2 diabetes reduce the future burden of cardiovascular disease? The evidence base today
ohn HB Scarpello

The prevalence of type 2 diabetes is set to double over the next 25 years, leading to substantial morbidity and mortality, particularly from macrovascular diabetic complications. Pre-diabetic dysglycaemia, characterised by impaired glucose tolerance (IGT) and/or impaired fasting glucose (IFG), is associated with an increased risk of developing both type 2 diabetes and cardiovascular disease. IGT and IFG appear well before type 2 diabetes is diagnosed, thereby presenting an opportunity for intervention to reduce the future burden of diabetes and cardiovascular disease. Intensive lifestyle interventions are effective in preventing or delaying diabetes but are difficult to sustain long term. Intervention trials with pharmacological agents, e.g. the Diabetes Prevention Program (DPP) with metformin, and the STOP-NIDDM study with acarbose, have demonstrated significant decreases in the risk of progression to type 2 diabetes in populations with IGT. Moreover, preliminary evidence with these agents supports a possible beneficial effect on cardiovascular outcomes.
March 2004 Br J Cardiol 2004;11:129-36
Evolution of the HMG CoA reductase inhibitors (statins) in cardiovascular medicine
Christopher J Packard

Recent trials have broadened the evidence base for statin use. It has now been documented that these drugs are effective agents not only in the general at-risk population, but also in the primary and secondary prevention of coronary heart disease in type 2 diabetics and in the elderly. The Heart Protection Study demonstrated the benefits of statin therapy in diabetics free of vascular disease, regardless of initial low-density lipoprotein (LDL) cholesterol level. Age is no longer a barrier to treatment, as revealed in the Prospective Study of Pravastatin in the Elderly at Risk, a trial which found that even a relatively brief period of statin therapy in elderly patients can result in a 19% reduction in the risk of a coronary event. Statins have the ability to lower the plasma concentration of all apoB-containing lipoproteins. This may help explain their clinical efficacy in diabetics who generally have unremarkable LDL-cholesterol levels. Most currently available statins are also able to induce a modest (5% to 10%) rise in high-density lipoprotein cholesterol, an effect that appears distinct from LDL lowering. This broadens their use to subjects with a variety of problems such as the metabolic syndrome and insulin resistance. The success of large-scale trials in coronary heart disease contrasts with the abundant evidence of under-treatment, even in high-risk groups. Thus the greatest need, at present, is to close the gap between the principles and practice of coronary disease prevention.
March 2004 Br J Cardiol 2004;11:123-27
Inhibition of the renin-angiotensin system in diabetic patients – beyond HOPE
Anthony H Barnett

Treatment to reduce blood pressure is effective in preventing and slowing the progression of the vascular complications of diabetes. Recent studies have suggested that use of antihypertensives that inhibit the renin-angiotensin system may have particular benefit in patients with type 2 diabetes in terms of cardiovascular and renal protection. Present practice is to use angiotensin-converting enzyme (ACE) inhibitors as first-line agents, with angiotensin II receptor antagonists (AIIAs) as back-up drugs in the event of side effects or intolerance. The findings of recent trials with AIIAs, however, suggest that they are an equivalent class of drugs to the ACE inhibitors from the point of view of renal profile and that their better side-effect profile could also make them suitable first-line drugs for patients with microalbuminuria and overt nephropathy.
March 2004 Br J Cardiol 2004;11:112-7
What’s new in the new British Hypertension Society guidelines for the management of hypertension – BHS IV
Bryan Williams, Neil Poulter

The British Hypertension Society (BHS) has recently published its latest guidance for the management of hypertension, BHS-IV.1,2 This article summarises these recommendations and discusses the main features of the new guidance.
March 2004 Br J Cardiol (Acute Interv Cardiol) 2004;11:AIC 9–AIC 13
Treatment of bifurcation coronary lesions in the era of drug-eluting stents. The ‘crush’, ‘reversed crush’ and ‘skirt’ techniques
Ghada W Mikhail, Flavio Airoldi, Antonio Colombo

Percutaneous treatment of bifurcation coronary lesions is less successful than treatment of non-bifurcation lesions, with a higher incidence of side branch occlusion and restenosis. The ‘crush technique’ was developed to ensure complete coverage of the ostium of the side branch, where restenosis frequently occurs. Drug-eluting stents are deployed in both side and main branches. The main branch stent crushes the side branch stent against the wall of the main vessel. The ‘reversed crush’ is used when the side branch result is unsatisfactory following stenting of the main branch, or when a 6F guiding catheter is needed. The ‘skirt technique’ was designed to treat pseudobifurcation lesions (lesions in the main branch which are immediately proximal to a bifurcation). It involves sandwiching two balloons in one stent. Preliminary results using the crush technique in 35 patients show angiographic success in all lesions.
January 2004 Br J Cardiol 2004;11:75-9
A community-based service for patients with congestive cardiac failure: impact on quality of life scores
Huw Williams, Elizabeth Morrison, Debra Elliott

Echocardiography remains the ‘gold standard’ for the objective assessment of left ventricular systolic function. Even with the high prevalence of left ventricular systolic dysfunction, echocardiography is not universally available within UK primary care, despite the fact that the condition is predominantly managed within this arena. We describe a service within one Primary Care Trust, where general practitioners and nurses refer patients who are suspected of having, or who are at high risk of developing heart failure, for a clinical assessment and an echocardiogram. Following this, a treatment plan is formulated and those with systolic dysfunction are followed up by a heart failure nurse. She ensures that the treatment regimen is adhered to and that the correct physiological and biochemical monitoring takes place. In our study we found that of those referred, only 33% had evidence of left ventricular systolic dysfunction, with 62% showing normal function. Of those patients with left ventricular systolic dysfunction, 86% required a significant change in their medication. Three months after the assessment, using the ‘Minnesota Living with Heart Failure Questionnaire’, considerable improvement was noted in the quality of life of patients with left ventricular systolic dysfunction. This paper suggests that there is considerable scope for improvement in the management of chronic heart failure.
January 2004 Br J Cardiol 2004;11:71-4
NSF lipid targets in patients with CHD: are they achievable in a real-life primary care setting?
Philip H Evans, Manjo Luthra, Christine Pike, Alison Round, Maurice Salzmann

The secondary prevention of coronary heart disease (CHD) is a recognised priority for primary care and is a fundamental part of the published National Service Framework (NSF). The majority of patients receive statins to reduce their total cholesterol (TC) and low-density lipoprotein chol-esterol (LDL-C) levels. The NSF set out targets for both TC and LDL-C. This study was designed to investigate the applicability of these targets in a real-life setting. One hundred and ten patients aged under 75 with established CHD were screened and their lipids measured. Eighty (73%) were on a statin. Mean TC was 6.3 mmol/L before treatment and 4.8 mmol/L after. Of these 80 patients, 46 (58%) had a TC below 5.0 mmol/L. Only 39% of patients met the stricter criterion of less than 5.0 mmol/L and a 25% fall in TC. No patient whose pre-treatment TC was below 5.0 mmol/L had reached a 25% reduction as well. The use of a threshold and a percentage may be potentially confusing to GPs and reduce the implementation of these targets.
January 2004 Br J Cardiol 2004;11:69-70
Left recurrent laryngeal nerve palsy secondary to an aortic aneurysm (Ortner’s syndrome)
F Runa Ali, Andrew J Hails, Bernard Yung

In patients presenting with persistent hoarseness due to left recurrent laryngeal nerve (LRLN) palsy and an abnormal left hilum on chest radiographs, a major cause is bronchogenic carcinoma. We describe two cases presenting with such a combination of symptoms and signs in whom a diagnosis of bronchogenic carcinoma was suspected. In each case, the LRLN palsy was in fact due to direct compression of the nerve by an aortic aneurysm.
January 2004 Br J Cardiol 2004;11:65-8
The ACTION, EUROPA and IONA trials: similarities, differences, outcomes and expected outcome
Johannes A Kragten, Gilbert Wagener

The ACTION (A Coronary disease Trial Investigating Outcome with Nifedipine GITS) study is the largest ever performed randomised trial of an anti-anginal drug in patients with chronic stable angina. Its aim is to assess the effect of nifedipine GITS 60 mg versus placebo on standard therapy for coronary artery disease on event-free survival; its composite end point includes death from any cause, acute myocardial infarction, hospitalisation for overt heart failure, emergency coronary angiography, disabling stroke and procedures for peripheral revascularisation. ACTION is one in a series of trials assessing drug effects in chronic stable coronary artery disease. The IONA (Impact Of Nicorandil in Angina) and EUROPA (EURopean trial On reduction of cardiac events with Perindopril in stable coronary artery disease) studies demonstrated that the K-ATP channel activator nicorandil and the angiotensin-converting enzyme inhibitor perindopril reduced the primary composite end point for cardiac events by 17% and 20%, respectively. Nifedipine GITS is an effective antihypertensive and anti-anginal drug. In the INSIGHT trial, nifedipine GITS 30/60 mg demonstrated comparable outcomes to a diuretic combination therapy with significant effects on intermediate end points. ENCORE I (Evaluation of Nifedipine and Cerivastatin on Recovery of coronary Endothelial function) demonstrated that nifedipine GITS 30/60 mg positively affected the pathophysiology of coronary artery disease. We therefore anticipate that nifedipine will affect blood pressure, anginal symptoms and resulting complications, and the coronary atherosclerotic process in those patients randomised to receive this agent in the ACTION study.
January 2004 Br J Cardiol 2004;11:61-4
Bradycardia and tachycardia occurring in older people: an introduction
Colin Berry, Andrew C Rankin, Adrian JB Brady

Arrhythmias are more common in the elderly and in many situations are of prognostic importance. The incidence of arrhythmias in the elderly is increasing, most likely due to enhanced longevity. Alterations in heart rate and rhythm may occur because of age-related change within the heart. Elderly people are more likely to experience co-morbid health problems, intercurrent illness and adverse drug reactions, all of which may result in arrhythmias. Falls are a common problem in elderly people; an arrhythmic cause should always be considered.
January 2004 Br J Cardiol 2004;11:56-60
The present and future role of aldosterone blockade
Allan D Struthers

Angiotensin-converting enzyme (ACE) inhibitor therapy only partially suppresses aldosterone production and ‘aldosterone escape’ occurs in up to 40% of patients with congestive heart failure (CHF). The RALES and EPHESUS studies show clearly that even in the presence of ACE inhibitor therapy, aldosterone contributes to mortality in CHF. There are many mechanisms for this. Firstly, aldosterone contributes to endothelial dysfunction and attenuates endothelium-dependent vasodilatation, at least partly by reducing nitric oxide bioavailability. Aldosterone also promotes myocardial fibrosis and cardiac remodelling by enhancing collagen synthesis, resulting in increased myocardial stiffness and increased left ventricular mass. These mechanisms mediated by aldosterone contribute to increased risk of ventricular arrhythmias and sudden cardiac death. Inhibition of aldosterone’s effect on mineralocorticoid receptors should now be considered standard therapy in populations of CHF patients. Aldosterone blockers also reduce the blood pressure in all types of hypertensive patients and may have an additional role as add-on therapy in hypertension, especially to lessen target organ damage.
January 2004
The prevalence of low levels of high-density lipoprotein cholesterol among patients treated with lipid-lowering drugs
Dirk Devroey, Brigitte Velkeniers, Willem Betz, Jan Kartounian

Some patients with initial normal levels of high-density lipoprotein cholesterol (HDL-C) have lower HDL-C levels during lipid-lowering treatment. The aim of this study was to estimate the prevalence of low HDL-C (< 1.0 mmol/L; < 40 mg/dL) before and during lipid-lowering treatment. Additionally, the prevalence of low HDL-C during fibrate and statin treatment was compared. All patients attending two Health Insurance Associations during February and March 2002 for continuing reimbursement of their lipid-lowering drug were included in this study. Date of birth, sex and the actual lipid-lowering drug were recorded. The most recent lipoprotein levels and those after a three-month diet before the start of the treatment were recorded. In total, 2,259 patients (56% women) were included; 69% were treated with statins and 31% with fibrates. Low HDL-C levels were found before the initiation of the treatment in 7% of the statin patients and in 11% of the fibrate patients. During treatment, 10% of the statin patients and 13% of the fibrate patients had low HDL-C levels. The proportion of patients whose HDL-C decreased below 1.0 mmol/L (40 mg/dL) during treatment was 6% for statins and 4% for fibrates. Although lipid-lowering drugs are known to increase HDL-C levels slightly, not all patients benefit from this effect.
January 2004 Br J Cardiol 2004;11:42-9
The surgical management of mitral valve disease
Joanna Chikwe, Axel Walther, John Pepper

We summarise the natural history and pathophysiology of mitral valve stenosis and regurgitation. The indications for surgery, and the various surgical options including mitral valvotomy, mitral valve repair and mitral valve replacement with bioprosthetic and mechanical valves are discussed. The results of surgery for mitral valve disease in the UK are summarised.
January 2004 Br J Cardiol 2004;11:34-8
How do we define myocardial infarction? A survey of the views of consultant physicians and cardiologists
Julia Helen Baron, Alice Joy, Michael Millar-Craig

In 2000, the European Society of Cardiology and American College of Cardiology issued a consensus document concerning the redefinition of myocardial infarction (MI). They proposed that the diagnosis of acute MI should be based on the rise and fall of specific markers combined with at least one of the following: ischaemic symptoms, ECG changes consistent with ischaemia or infarction, or coronary intervention. The implications of this redefinition are widespread, and it has been met with mixed opinions from physicians. Here we present the results of a survey, sent to 1,000 consultants in cardiology and general medicine, concerning the availability and their use of cardiac markers and their current working diagnosis of MI. Four case studies were included in the survey. Some 361 responses were analysed. Creatine kinase (CK) remains the most frequently used marker for the diagnosis of MI, but 23% of consultants had moved to a definition based on troponins. Fourteen per cent of consultants no longer used CK in their practice. Ninety-two per cent of consultants had access to troponin assays. Definitions varied widely between consultants, even within individual hospitals, as did the responses to the case studies.
January 2004 Br J Cardiol 2004;11:39-41
Redefining acute MI: the potential impact on rehabilitation services
Mark Snowden

We summarise the natural history and pathophysiology of mitral valve stenosis and regurgitation. The indications for surgery, and the various surgical options including mitral valvotomy, mitral valve repair and mitral valve replacement with bioprosthetic and mechanical valves are discussed. The results of surgery for mitral valve disease in the UK are summarised.
January 2004 Br J Cardiol 2004;11:27-32
Heart failure and venous thromboembolism: a major hidden risk
Julia Helen Baron, Alice Joy, Michael Millar-Craig

In 2000, the European Society of Cardiology and American College of Cardiology issued a consensus document concerning the redefinition of myocardial infarction (MI). They proposed that the diagnosis of acute MI should be based on the rise and fall of specific markers combined with at least one of the following: ischaemic symptoms, ECG changes consistent with ischaemia or infarction, or coronary intervention. The implications of this redefinition are widespread, and it has been met with mixed opinions from physicians. Here we present the results of a survey, sent to 1,000 consultants in cardiology and general medicine, concerning the availability and their use of cardiac markers and their current working diagnosis of MI. Four case studies were included in the survey. Some 361 responses were analysed. Creatine kinase (CK) remains the most frequently used marker for the diagnosis of MI, but 23% of consultants had moved to a definition based on troponins. Fourteen per cent of consultants no longer used CK in their practice. Ninety-two per cent of consultants had access to troponin assays. Definitions varied widely between consultants, even within individual hospitals, as did the responses to the case studies.
November 2003 Br J Cardiol 2003;10:484-88
What’s new in cardiovascular disease: report from the PCCS Annual Meeting and AGM
Dr Ola Soyinka

‘New’ was the operative word at this year’s Primary Care Cardiovascular Society annual meeting, held in Dublin from 3rd–4th October 2003. Delegates heard about the ‘new’ GP contract, the ‘new’ science of pharmacogenetics, the ‘new’ breed of healthcare professionals (with special interests) and a ‘new’ diploma in cardiovascular disease.
November 2003 Br J Cardiol 2003;10:478-81
Diabetes and coronary heart disease: combining the National Service Frameworks
Mike Mead

The two National Service Frameworks for coronary heart disease, and for diabetes, share some common themes. This article discusses where they overlap with each other and with national targets for stroke outlined in the National Service Framework for Older People. It then details a simple 10-point plan on how Primary Care Trusts can develop strategies to implement NSF targets so they achieve national standards.
November 2003 Br J Cardiol 2003;10:472-7
Computer-enhanced assessment of cardiovascular risk
Peter Tyerman, Gill V Tyerman, Trefor Roscoe, Mike Campbell, Jenny Freemen

This study investigated the impact of the use of a computer programme to collect data on cardiovascular risk factors, which could also provide patient education. A retrospective analysis was carried out of data recorded over three years in a general practice in Barnsley, an area with the second highest prevalence of ischaemic heart disease in England. The study found that use of a simple computer-based system by the primary care team led to 55% of the population being assessed within three years. Consequent patient education and lifestyle changes led to a reduction of risk factors in those at high risk who were re-screened. A possible reduction on admissions to hospital for cardiovascular disease was also noted.
November 2003 Br J Cardiol 2003;10:470-1
Acute, reversible type II (Wenkebach) heart block due to combined chloroquine and diltiazem treatment
Neil Swanson, Nilesh J Samani

International travel to malarial areas is increasingly common. Chemoprophylaxis using chloroquine is common, but can cause cardiac problems. We describe a new problem, of reversible heart block, in a patient on both chloroquine and the frequently-used calcium channel blocker, diltiazem.
November 2003 Br J Cardiol 2003;10:462-8
Modified-release nicotinic acid for dyslipidaemia: novel formulation improves tolerability and optimises efficacy
Michael Schachter

Data from epidemiological and intervention studies have conclusively shown that a low level of high-density lipoprotein cholesterol (HDL-C) is an important risk factor for cardiovascular disease. Increasing low HDL-C levels produces risk reduction comparable with that observed with decreasing low-density lipoprotein cholesterol (LDL-C) in the major statin trials. The latter have shown that, even with effective statin therapy, there is still an unacceptably high residual risk of major coronary events. A substantial proportion of patients with coronary heart disease (CHD) with acceptable levels of LDL-C will have low levels of HDL-C and increased serum triglycerides. Of the available lipid-modifying treatments, nicotinic acid is the most potent agent for increasing HDL-C (by about 30% from baseline). In addition, it effectively decreases triglycerides and has a relatively modest effect in decreasing LDL-C. Modified-release nicotinic acid has been developed to overcome the poor tolerability associated with earlier formulations while maintaining the efficacy of immediate-release nicotinic acid. Modified-release nicotinic acid is effective and safe for the treatment of dyslipidaemia, including the atherogenic dyslipidaemia associated with type 2 diabetes and the metabolic syndrome. Combination therapy with modified-release nicotinic acid and a statin offers complementary therapeutic benefits, as well as reducing the progression of, or even regressing, atherosclerosis. This strategy can represent an important advance for clinical management of at-risk patients with dyslipidaemia.
November 2003 Br J Cardiol 2003;10:453-61
The surgical management of aortic valve disease
Joanna Chikwe, Axel Walther, John Pepper

We summarise the natural history and pathophysiology of aortic stenosis and regurgitation, the indications for surgery, the advantages and disadvantages of tissue, mechanical, homograft and autograft aortic valve replacement, and the prediction of operative mortality for individual patients.
September 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10:AIC 75–AIC 77
The use of glycoprotein IIb/IIIa antagonists in acute coronary syndromes: are we following the NICE guidelines?
Julia Baron, Alice V Joy, Sarah Armstrong, Michael Millar-Craig

Recent developments in the management of non-ST elevation acute coronary syndromes (ACS) have included the introduction of glycoprotein (GP) IIb/IIIa inhibitors. The National Institute for Clinical Excellence (NICE) has published guidelines on their use, which state that these agents should be given to all high-risk patients. Here, we present the results of a national survey of 1,000 consultant cardiologists and general physicians. A total of 361 replies were analysed: 98% of respondents treated patients with ACS and 92% of respondents had access to troponin assays. Overall, 241 (67%) of respondents prescribed GP IIb/IIIa inhibitors for ACS. There was a significant difference between cardiologists and generalists, with 194 (77%) cardiologists and 46 (42%) general physicians prescribing GP IIb/IIIa inhibitors in ACS (p=0.0013). Despite the presence of government guidelines regarding the administration of GP IIb/IIIa antagonists in ACS, we calculate that only 32% of respondents are prescribing IIb/IIIa inhibitors as recommended by NICE
September 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10:AIC 78–AIC 81
Implantable left ventricular assist devices
Mario Petrou

End-stage heart failure represents a major public health challenge and carries a poor prognosis. After a 30-year gestation period, mechanical assist devices are now poised to make a significant impact in the treatment of heart failure patients. This review gives a general overview of the subject and describes some of the devices currently available in greater detail.
September 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10:AIC 82–AIC 88
Atrial fibrillation after coronary bypass surgery – pathophysiology, resource utilisation and management strategies
Joseph Alex, Gurpreet S Bhamra, Alex RJ Cale, Steven C Griffin, Michael E Cowen, Levent Guvendik

Background: With an incidence rate of 30–50%, atrial fibrillation (AF) after bypass surgery continues to be one of the most common complications. The possibilities of haemodynamic instability and thromboembolism necessitate the initiation of antiarrhythmic and anticoagulant therapy. Despite early initiation of therapy, AF can increase post-bypass morbidity and mortality. It can also prolong intensive care unit and hospital stay and further increase resource utilisation. In this article we review the pathophysiology, risk factors, effect on resource utilisation, current prophylactic and therapeutic strategies, and risk-benefit assessment of anticoagulant therapy in post-bypass AF. Methods: This is a review of the medical literature on post-bypass AF from January 1980 to March 2003. Relevant older references were also reviewed. Clinical and research studies on the mechanisms, pathophysiology, risk factors, complications, resource utilisation, prophylaxis and management were collected from the Medline, Embase, Cinhal and Sigle databases and reviewed. Conclusion: AF significantly increases complications and resource utilisation after bypass surgery. Prophylactic therapy could significantly reduce the incidence of AF. In AF lasting more than 48 hours, anticoagulant or antiplatelet therapy based on individual risk assessment is recommended.
September 2003 Br J Cardiol 2003;10:395-8
Thrombolysis in the pre-hospital setting
Paul Kelly

Pre-hospital thrombolysis has proven clinical benefits in the management of acute myocardial infarction (MI). If the targets for administering thrombolysis, in particular call-to-needle time, are to be met, then it seems likely that its use will be more widespread. With appropriate training and support, paramedics can competently perform 12-lead electrocardiograms (ECGs) and administer thrombolysis. Cardiologists should be prepared to undertake paramedic training and play a central role in the development of protocols and pathways for the administration of pre-hospital thrombolytic therapy.
September 2003 Br J Cardiol 2003;10:392-4
A case of acute aortic valve endocarditis due to Erysipelothrix rhusiopathiae acquired from fish
Muhammad Arif

A case of acute aortic valve endocarditis due to Erysipelothrix rhusiopathiae acquired from fish.
September 2003 Br J Cardiol 2003;10:386-91
The Clinical Standards Board for Scotland’s quality assurance system in secondary prevention following acute myocardial infarction
Marion Barlow, Rona Smith, Sarah Wedgwood

The Clinical Standards Board for Scotland (CSBS) was established in 1999 to develop a national system of quality assurance and accreditation of clinical services with the aim of promoting public confidence in the NHS in Scotland (NHSS). The coronary heart disease pathfinder project assessed services to patients following myocardial infarction. The quality assurance system involves comparison of performance against written standards developed by a multidisciplinary project group which included lay members. Six nationally applicable standards were the subject of comprehensive open consultation with both the public and the professions. All acute trusts in Scotland were issued with a self-assessment tool followed by a visit from a multidisciplinary external review team comprising of lay representatives and health service professionals who produced a verbal and written report. There was a pool of over 100 reviewers and each team numbered on average eight reviewers, two of whom were lay members. A national report of Scotland’s performance was published by CSBS in October 2001. The main areas of concern in Scotland’s national performance were that few sites were able to meet the standard relating to thrombolysis times and there was an overall lack of robust audit material. It was noted, however, that the major strength of Scotland’s delivery of healthcare lay with the staff providing services. The process of accreditation in Scotland differs from that of other countries and one of its strengths lies in the involvement of the public, patients and health professionals as peers in all stages. The process itself encouraged dissemination of good practice and highlighted areas of concern.
September 2003 Br J Cardiol 2003;10:379-84
Recent advances in insulin therapy
Caroline Day, Helen Archer, Clifford J Bailey

Increased attention to good glycaemic control in diabetic patients has encouraged more intensive use of insulin. To help achieve a steady ‘basal’ insulin supply, a new long-acting insulin analogue glargine (Lantus®) has been introduced. This provides a flatter ‘peakless’ circulating concentration of insulin than protamine (isophane) and lente insulins, facilitating dose escalation with reduced risk of hypoglycaemia. Another long-acting insulin analogue detemir (Levemir®) is advanced in development. Intensive insulin therapy requires ‘top-ups’ to coincide with mealtimes. The recently introduced rapid-acting monomeric analogues, lispro and aspart, are particularly useful in this respect. The monomeric analogues are quickly absorbed and short acting: hence they reduce post-prandial glucose excursions (which have been ascribed especial cardiovascular risk) with less risk of hypoglycaemia than conventional short-acting insulin. Premixed rapid-intermediate acting mixtures of monomeric analogues with protamine are also available. Continuous subcutaneous insulin infusion is receiving increased use as the pump technology advances, mainly incorporating the monomeric insulin analogues. Inhaled insulins continue in development, and various oral insulin formulations have entered clinical trials.
September 2003 Br J Cardiol 2003;10:373-8
Atrial fibrillation in the elderly
Colin Berry, Alan Rae, Jaqueline Taylor, Adrian J Brady

Atrial fibrillation (AF) is the commonest sustained arrhythmia affecting elderly people. It will become increasingly prevalent in Western societies, given the growing proportion of elderly people in these populations.>br> AF may lead to a variety of embolic phenomena, notably stroke. Furthermore, AF may complicate other conditions, such as hypertension and heart failure. AF is associated with an increased risk of death. The management of AF can be a difficult problem, particularly in symptomatic, elderly patients. Results from recent large, multicentre clinical trials in sustained AF have demonstrated that a rate control strategy with conventional drugs, is at least as effective, and possibly superior, to rhythm control by chemical or electrical cardioversion over a three-year period. Whether these results can be extrapolated to longer time periods than the trials’ durations (approximately 3.5 years) is not known. Results from clinical trials of a new oral anticoagulant, ximelagatran, indicate that this agent is as good an anticoagulant as warfarin in sustained AF. Other results are awaited from on-going trials on the tolerability and side-effect profile of this drug. The possibility of an alternative anticoagulant which does not share warfarin’s need for routine monitoring of its anticoagulant effect, nor share warfarin’s potential for adverse interactions with other drugs, is very attractive, particularly in elderly patients. In the longer term, radiofrequency ablation techniques might provide a more widely available, curative therapy, for elderly patients with AF.
September 2003 Br J Cardiol 2003;10:370-2
How to evaluate the performance of oral anticoagulation clinics
David A Fitzmaurice, Patrick Kesteven

Increasing numbers of patients are receiving warfarin therapy, with atrial fibrillation being the main indication. If warfarin therapy is to be effective, however, good therapeutic control is important. Recent advances in models of management, including primary care clinics and patient self-management, has meant that patients have an increasing choice as to how and where they have their warfarin monitored. Comparison of performance between these different models of care has been historically difficult due to the use of different reporting techniques. This paper highlights the different methods of reporting therapeutic control, including adverse event reporting, and recommends that at least two measures from a set of recognised parameters should be used. This makes comparison of control between centres possible.
September 2003 Br J Cardiol 2003;10:367-0
The introduction of a new service for direct current cardioversion (DCCV) for atrial fibrillation in a district general hospital
Jennie Walsh, David A Sandler, Charlie Elliot, Andy Challands

The timing and effectiveness of a new protocol for organising direct current cardioversion (DCCV) for patients with atrial fibrillation (AF) was compared with the existing system in a medium-sized district general hospital in the United Kingdom. The new protocol comprised a monthly dedicated DCCV list in the operating theatres, with an anaesthetist and an Operating Department Assistant providing anaesthesia, and cardiology medical staff performing the cardioversion. The last 35 consecutive patients undergoing DCCV for AF before the new protocol was introduced were compared with the first 35 patients having DCCV under the new protocol. The time to perform 35 consecutive cardioversions was reduced from 32 months to 10 months. The new system resulted in no cancellations for administrative reasons and only one patient for a clinical reason. Sinus rhythm (SR) was restored in 60% cases under the new protocol (double the success rate before the new protocol) and 76% patients discharged in SR under the new protocol, remained in SR at clinic follow-up. A simple change in the method of delivering a clinical service has resulted in an improvement in both the administration and clinical outcome for patients. Such changes, requiring co-operation between anaesthetic and cardiology departments, could be implemented widely for the benefit of many patients.
September 2003 Br J Cardiol 2003;10:358-65
Stroke prevention in atrial fibrillation
FD Richard Hobbs

This article explores the strengths and weaknesses of current treatment pathways of atrial fibrillation as discussed at a multidisciplinary meeting of healthcare professionals organised by the Thrombosis Quorum. By discussing case studies using a Socratic method of dialogue to elicit better questioning of management practices, the meeting reached a consensus on various issues in the care of the patient with atrial fibrillation.
September 2003 Br J Cardiol 2003;10:351-7
Drug therapy for the management of atrial fibrillation: an update
Andrew RJ Mitchell

With an ageing population in the United Kingdom, atrial fibrillation has become an increasing cause of morbidity and mortality, and a burden on health resources. Drug therapies for the management of atrial fibrillation have a number of roles, including the restoration and maintenance of sinus rhythm and the prevention of thrombo-embolic complications. New anti-arrhythmic drugs are under development and alternatives to warfarin are being investigated. This article examines the current knowledge on the effectiveness of drug therapy in atrial fibrillation and discusses some aspects of the future of drug therapy for atrial fibrillation.
September 2003 Br J Cardiol 2003;10:329-31
Cardiology and the new GMS contract for GPs
Mike Mead

With an ageing population in the United Kingdom, atrial fibrillation has become an increasing cause of morbidity and mortality, and a burden on health resources. Drug therapies for the management of atrial fibrillation have a number of roles, including the restoration and maintenance of sinus rhythm and the prevention of thrombo-embolic complications. New anti-arrhythmic drugs are under development and alternatives to warfarin are being investigated. This article examines the current knowledge on the effectiveness of drug therapy in atrial fibrillation and discusses some aspects of the future of drug therapy for atrial fibrillation.
July 2003 Br J Cardiol 2003;10:315-7
Screening for asymptomatic peripheral vascular disease in primary care
Kamlesh Khunti

In addition to identifying those patients with coronary heart disease, the National Service Frame-work also requires general practitioners to identify all people with a diagnosis of occlusive arterial disease, including stroke and peripheral vascular disease, and offer appropriate interventions. Asymptomatic peripheral vascular disease is common; it is estimated almost one in five patients between the ages of 55 and 74 would be identified as at risk. Patients with asymptomatic disease have the same increased risk of cardiovascular events and death as in patients with symptomatic disease. The author discusses how to diagnose asymptomatic disease, the merits of a screening programme in primary care, and which patients general practitioners should target.
July 2003 Br J Cardiol 2003;10:310-4
The need for 24-hour blood pressure control
Mike Mead

The current focus of our efforts in treating hypertension is to ‘treat to target’ using combination therapy. However, 24-hour control of blood pressure (BP) is of crucial importance in reducing cardiovascular risk. There is a circadian rhythm for such risk, with morning peaks in sudden cardiac death, myocardial infarction, unstable angina and ischaemic stroke. There is also a natural circadian rhythm in BP. Lack of a significant nocturnal dip worsens prognosis: patients tend to have increased left ventricular hypertrophy, cardiovascular mortality and cerebrovascular disease. Risk is related to the patient’s total BP load. The implications are that truly long-acting once-daily antihypertensives are needed, with a trough/peak ratio > 50%. Patient compliance is very important. Ambulatory BP monitoring should be used in selected patients. Patients should be advised to take their antihypertensive medication on waking rather than waiting until after breakfast.
July 2003 Br J Cardiol 2003;10:308-9
Digoxin toxicity: an unusual presentation of infective endocarditis
Handrean Soran, Louise Murray, Naveed Younis, Steve PY Wong, Peter Currie, Ian R Jones

We describe a case of infective endocarditis, which presented with digoxin toxicity. This case is of interest since the patient only became pyrexial six days after admission when blood cultures grew Streptococcus viridans. We believe this is the first case of infective endocarditis presenting with digoxin toxicity.
July 2003 Br J Cardiol 2003;10:305-07
Management of erectile dysfunction in men with cardiovascular conditions
Michael Kirby

Erectile dysfunction (ED) is reported to coexist with cardiovascular disease. It may be the first clinical manifestation of cardiovascular disease making it a helpful, early marker. Psychogenic causes are also an important component of ED. Around half of all men over the age of 40 years are affected by ED but treatment is often not requested by the patient. ED can be successfully treated pharmacologically. PDE-5 inhibitors are currently the treatment of choice. Physicians should initiate discussion about sexual health and ED in the diagnosed cardiovascular patient.
July 2003 Br J Cardiol 2003;10:297-304
Clinical usefulness of HDL cholesterol as a target to lower risk of coronary heart disease – Summary of evidence and recommendations of an expert group*
Frank M Sacks

Multiple lines of evidence show that high-density lipoproteins (HDL) protect against coronary heart disease (CHD), and that low blood levels of HDL cholesterol (HDLc) indicate high risk of a coronary event. Major epidemiological studies show that a low HDLc is a strong predictor of CHD, and this relationship occurs at any level of low-density lipoprotein cholesterol (LDLc) or triglycerides, demonstrating independence. When the HDLc level is raised by drug therapy, coronary atherosclerosis is decreased and CHD events are lessened. Increases in HDLc are in fact independently correlated with coronary angiographic and clinical benefit. HDL stimulates the removal of cholesterol from cells in the vascular wall. The cholesterol is taken up by HDL and shuttled in part to the liver for excretion in the bile. Experiments in transgenic mice provide proof that increased HDL secretion protects against atherosclerosis caused by an atherogenic diet or genetic hyperlipidaemia. In humans, HDL has direct beneficial effects on coronary arterial vasodilation. This compelling scientific evidence thus justifies HDLc as a target to reduce risk of CHD. An international group of experts in epidemiology, clinical and basic science formed a consensus that an HDLc concentration of 1.0 mmol/L (40 mg/dL) is a realistic clinical guideline for patients at high risk of a coronary event. Specific diet and drug therapies were recommended.
July 2003 Br J Cardiol 2003;10:293-6
Percutaneous coronary intervention in the elderly
Paul Neary, Jacqueline Taylor, Adrian Brady

Older patients represent the majority of those considered for coronary intervention but they are under-represented in most clinical trials in this area. Reviewing registry data and pooled data from clinical trials, this article discusses the effect of age on procedural mortality and morbidity. It also reviews the effect of age on interventional procedures in unstable patients, and on pharmacological intervention. Despite the higher initial risks in older patients, the authors argue that several risk factors are responsible for predicting poor outcome following interventional procedures. Percutaneous coronary intervention can be very successful in the elderly and its risks must be balanced against the many important benefits older patients stand to gain from the procedure.
July 2003 Br J Cardiol 2003;10:288-92
COX-2 inhibitors and cardiovascular risk
COX-2 inhibitors and cardiovascular risk Mike Schachter

Non-steroidal anti-inflammatory drugs (NSAIDs) have potentially dangerous side effects, which has led to intense interest in the development of the cyclo-oxygenase (COX) inhibitors. This article reviews the science, safety and clinical evidence to date with these drugs. They appear to have fewer gastrointestinal and equivalent renal risks to NSAIDs. Reviewing the clinical evidence, particularly the complex cardiovascular effects of the COX inhibitors, the article discusses the clinical relevance of their thrombogenic and anti-atherosclerotic potential. Since many of the studies are retrospective analyses, randomised clinical trials are needed to ascertain whether these cardiovascular effects constitute a problem or an unexpected benefit, and whether there are differences between the different COX-2 inhibitors.
July 2003 Br J Cardiol 2003;10:281-6
Is there any evidence that tea drinking impacts on cardiovascular health in the UK?
Jenny Poulter, Caroline Bolton-Smith, Anton Rietveld

Epidemiological studies in the Netherlands first demonstrated an inverse relationship between ordinary (technically known as black) tea drinking and cardiovascular disease (CVD) mortality. Subsequent population-based studies have variously agreed with, been opposite to (notably in the UK) or produced null results. Currently, UK epidemiological studies look out of step with the rest of the world. This review highlights that, in the UK, tea drinking is more pronounced in the lower socio-economic (SE) groups, whilst tea drinking is associated with higher SE groups in the other countries that have linked tea to CVD. It is this key difference that may account for the apparent positive relationship between tea drinking and CVD mortality in the UK; low SE status (and high tea drinking) is also strongly associated with a high prevalence of the major CVD risk factors. Any positive benefits from tea drinking are likely to be due to a high content of antioxidant flavonoids, particularly the catechins. In vitro and intervention studies support mechanisms, such as improved endothelial function, whereby tea flavonoids may be cardioprotective. Whilst there is no evidence from population studies of positive cardiovascular benefit from tea drinking in the UK, tea is still contributing flavonoids to individual diets and these may well be beneficial. Tea drinking can safely be encouraged as part of a healthy diet. Further studies are required to clarify the situation.
July 2003 Br J Cardiol 2003;10:273-80
EBCT coronary calcium imaging for the early detection of coronary artery disease in asymptomatic individuals
D Vijay Anand, Avijit Lahiri, David Lipkin

Coronary heart disease (CHD) is the leading cause of death in the UK. Approximately 50% of myocardial infarctions occur in patients with no prior history of CHD or cardiovascular risk factors while sudden death is often the first manifestation of CHD in as many as 35% of patients. The realisation that standard risk factors incompletely predict incident CHD events has led to the development of several non-invasive imaging techniques to accurately assess the risk of CHD over the last decade. Several epidemiological studies have established that the total coronary atherosclerotic plaque burden is a powerful predictor of future hard coronary events (myocardial infarction and death). This article reviews the role of electron beam computed tomography (EBCT) in the early detection of subclinical coronary artery disease, the identification of ‘high-risk’ asymptomatic patients for intensive medical intervention, and its role in evaluating the progression of coronary artery disease and in monitoring the efficacy of medical therapies.
May 2003 Br J Cardiol 2003;10:223-28
Cholesterol management in patients with IHD: an audit-based appraisal of progress towards clinical targets in primary care
Simon de Lusignan, Billy Dzregah, Nigel Hague, Tom Chan

Anonymised data collected from 24 participating localities in England have been aggregated for this report. The data are taken from general practice computer records using a validated extraction tool Morbidity Information Query and Export SynTax (MIQUEST). The number of patients with heart disease, a cholesterol measure, whether they had been prescribed a statin, their quality of control, and its implications are reported. In the population studied of 2.4 million, 89,422 patients had a diagnosis of ischaemic heart disease; a prevalence rate of 3.7%. Cholesterol measurement was available for half (48.3%) of these patients, of whom half (55.2%) were taking a statin. As a result of this treatment gap, 118 excess myocardial infarctions annually are predicted, equivalent to around 7,150 events nationally. Compared to previous audits carried out in UK general practice, considerable progress has been made towards the achievement of treatment goals. The treatment gap is represented by a combination of lack of measurement and recording of data as well as poor quality of control.
May 2003 Br J Cardiol 2003;10:220-21
Percutaneous drainage and successful treatment of pericardial tamponade due to Dressler syndrome
Mehmet Kabukçu, Fatih Demircioglu, Fatma Topuzoglu, Oktay Sancaktar, Filiz Ersel-Tüzüner

Patients with Dressler syndrome generally present with malaise, fever, chest pain, leukocytosis, an elevated erythrocyte sedimentation rate and pericardial effusion.1 To the best of our knowledge, presentation of Dressler syndrome with pericardial tamponade is very rare. An investigation on Medline revealed that no cases had been reported in the last 10 years. We reported this case because of its rare presentation pattern and its successful treatment with percutaneous catheter drainage.
May 2003 Br J Cardiol 2003;10:218-9
Prevalence and risks of undertreatment with statins
Adrian J Brady, D John Betteridge

Statins are prescribed worldwide for patients with coronary heart disease (CHD) and also for those at risk of developing atherosclerotic vascular disease. This article looks at the prescribing of statins in the UK demonstrating how they are underprescribed in this country, how ineffective doses of statins are used due to many doctors not understanding how to implement guidelines, and how the greatest reductions in CHD risk are achieved by the greatest reductions in cholesterol.
May 2003 Br J Cardiol 2003;10:217
Left ventricular hypertrophy and aortic stenosis: a commentary
Kim Rajappan, Jamil Mayet

Routledge et al. have addressed an increasingly topical issue. They demonstrate in a small cohort of patients with aortic stenosis (AS) that the use of angiotensin- converting enzyme (ACE) inhibitors may be safe, particularly with some degree of systemic hypertension.1 This adds to the evidence that the use of ACE inhibitors in this patient population should not be strictly contraindicated. However, the more searching question of whether they should be used remains unanswered.
May 2003 Br J Cardiol 2003;10:214-16
Left ventricular hypertrophy and aortic stenosis: a possible role for ACE inhibition?
Helen C Routledge, Kairen R Ong, Jonathon N Townend

Aortic valve stenosis is a common cause of left ventricular hypertrophy (LVH). Severe LVH in association with aortic stenosis does not always regress following valve replacement surgery and is associated with a poor prognosis. The importance of angiotensin II in the hypertrophic process is increasingly recognised and the benefits of angiotensin-converting enzyme (ACE) inhibition in reducing LVH associated with hypertension are well established. Although ACE inhibitors are currently contraindicated in aortic stenosis (AS) on theoretical grounds there are very few data to support this. We have audited the current use of ACE inhibitors in a group of patients with AS and found that 27% of this group are currently taking an ACE inhibitor with no documented adverse effects. Trials to investigate the therapeutic benefit of ACE inhibition in preventing adverse left ventricular remodelling are merited but must be preceded by safety and tolerability studies.
May 2003 Br J Cardiol 2003;10:212-3
Use of nicotine replacement therapy early in recovery post-acute myocardial infarction to aid smoking cessation
Katherine A Willmer, Valerie Bell

Patients admitted to hospital with a diagnosis of acute myocardial infarction (AMI) have high motivation to stop smoking. Nicotine replacement therapy (NRT) is known to be valuable in helping smokers quit although it is not commonly prescribed in patients in the acute phase following AMI. Results from a full in-patient smoking cessation service were retrospectively analysed after the first 12 months, with particular reference to safety and efficacy in patients with AMI. Of 42 patients admitted with AMI who smoked and who were referred to the service, 32 (76%) received NRT with counselling as an in-patient, one as an out-patient and nine received counselling only. Assessment at four weeks showed 11 (26%) were still smoking, one (2%) had been lost to follow-up and 30 (71%) had successfully quit. Of these, six (20%) had not required NRT, one (3%) had received out-patient NRT and 23 (77%) had received in-patient NRT. There were no adverse outcomes in any patients. This suggests an in-patient smoking cessation programme, including prescription of NRT in the first five days following presentation with AMI, is a safe and effective means of helping vulnerable people to give up smoking.
May 2003 Br J Cardiol 2003;10:207-10
Persistent left superior vena cava – an anomaly to remember
Krishna Adluri, Jitendra M Parmar

Persistent left superior vena cava (PLSVC) is the most common anomaly involving central venous return in thorax. Anatomically it is a mirror image of the right superior vena cava and is usually asymptomatic but can cause difficulties during Swan-Ganz catheterisation and insertion of pacing systems. This article presents a comprehensive review of this anomaly and clinical scenarios in which it can prove problematic, illustrated by an example.
May 2003 Br J Cardiol 2003;10:197-205
Thrombolytic therapy for acute ischaemic stroke
Matthew Walters, Jacqueline Taylor, Adrian Brady

Thrombolytic therapy for acute ischaemic stroke improves outcome in a highly selected group of patients. It will shortly be licensed in the UK for this indication. Implementation of this treatment will be difficult as current stroke services are ill-equipped to meet the challenges associated with aggressive management of hyperacute stroke.
This article evaluates the published literature concerning thrombolytic therapy in the context of ischaemic stroke and briefly discuss the obstacles which prevent more widespread use of this treatment in the UK. It also considers the effect of age on efficacy and tolerability of thrombolytic therapy.
May 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10(1):AIC 45–AIC 48
The frequency of acute coronary syndromes and the cost of glycoprotein IIb/IIIa inhibitor treatment
Gary Cook, Philip Lewis, Michael Martin, Kathleen Carolan, Ian Short, Georgios Lyratzopoulos, Daniel Havely

The objective of this survey was to estimate the proportion of episodes of acute coronary syndromes (ACS) without ST segment elevation in relation to the total number of acute chest pain presentations. We attempted to estimate costs associated with glycoprotein (GP) IIb/IIIa inhibitor treatment in patients with high-risk features. This was a prospective survey set in a typical British district general hospital, serving a population of about 300,000. It took place over a 14-week period. The participants were all patients presenting with chest pain of possible cardiac origin, identified by intensive surveillance of all emergency medical admissions (EMAs) in patients over 16 years of age and all adult and elderly medicine in-patients. At the time of the study, the upper limit of normal for troponin T (TnT) used in this hospital was 0.05 µg/L. The main outcome measures were: the proportion of EMAs due to chest pain of likely cardiac origin; the number of episodes of ACS without ST elevation as a proportion of all EMAs; and the projected prescribing costs of GPIIb/IIIa inhibitor treatment for high-risk cases. We found that 22% (CI 20.07–23.5%) of all EMAs were due to chest pain likely to be of cardiac origin. One event of ACS without ST elevation was generated for every 25.6 (CI 23.8–28.6) EMAs. Using a TnT value of > 0.1 µg/L to define high risk and suitability for GPIIb/IIIa inhibitor treatment, a minimum of 66% of patients with ACS without ST elevation would be eligible for treatment. In the study hospital, this translates to an annual cost of £131,000 (equivalent to £43,600 per 100,000 catchment population) or £11.45 per all-cause hospital EMA. In conclusion, about two thirds of patients with ACS without ST elevation have high-risk features and would potentially benefit from treatment with GPIIb/IIIa inhibitors. The costs of drug treatment are appreciable, but financial planning can be assisted by the data presented here.
May 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10:AIC 49–AIC 51
Pre-operative strategies on clopidogrel use in coronary artery bypass grafting
Andreas Hoschtitzky, Adrian Marchbank

There is a lack of standards pertaining to stopping antiplatelet agents in patients with acute coronary syndromes prior to coronary surgery. We conducted a national survey of all centres performing cardiac surgery in the UK and Ireland into practices and standards in relation to clopidogrel and aspirin before coronary artery surgery (n=36). The response rate was 89%. The majority of centres used combination antiplatelet therapy in either some or all pre-operative acute coronary syndrome patients (79%). Aspirin alone is given in 19% of this surgical subpopulation. Aspirin is stopped 4.9 + 0.5 days (mean + SEM) and clopidogrel 6.5 + 0.5 days prior to surgery. There are no clear departmental policies in most cases (21 of 32 units) regarding cessation of clopidogrel. A subjective increase in bleeding was reported in 69% of centres; in 15 centres (47%) patients had returned to theatre for bleeding. Many units in the UK still do not have a policy regarding antiplatelet therapy in those patients with acute coronary syndromes who are awaiting coronary bypass surgery. A randomised controlled trial is probably the correct way of evaluating the best strategy on use and omission of aspirin and clopidogrel in this setting.
May 2003 Br J Cardiol 2003;10:169-71
Interventions to aid smoking cessation post-myocardial infarction
Celine Adams

Interventions to aid smoking cessation post-myocardial infarction Celine Adams Smoking kills. Almost a fifth (19%) of all coronary heart disease deaths in the UK are attributable to smoking.1 Many of these could be prevented. Smoking cessation significantly decreases mortality and – in the setting of myocardial infarction – this reduction is estimated at 35%.2 Smoking cessation is also cost effective with interventions in the UK ranging from £212 to £873 per life year gained.3 But in the setting of unstable cardiovascular disease, safe and efficacious methods of helping patients to stop smoking are yet to be demonstrated.
May 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10:AIC 52–AIC 55
Robotic coronary artery surgery
Douglas West, Anthony C de Souza, John Pepper

Cardiopulmonary bypass and the median sternotomy incision have revolutionised cardiac surgery, helping coronary artery bypass to become a routine procedure. Cardiopulmonary bypass was originally developed to allow open-heart surgery, but was adopted for coronary surgery because it provided a still operating field. However, the cost of good surgical access has been a large scar, with slow recovery and occasional serious wound complications. Adaptation of robotic technology from production engineering provides a new way of performing coronary artery bypass grafting (CABG) without large incisions, and often without cardiopulmonary bypass. Although the first endoscopic robotic cases were reported several years ago, widespread adoption of the new technique is still some way off. We review the progress of robotic CABG to date, and discuss current research fields.
May 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10:AIC 56–AIC 58
Outcome of percutaneous coronary intervention in acute coronary syndromes: from clinical trials to clinical practice
Khaled Alfakih, Mike Robinson, Alistair Hall, James Mclenachan

Early angiography and revascularisation are beneficial for patients with non-ST segment elevation myocardial infarction (NSTEMI). However, the Prospective Registry of Acute Ischaemic Syndromes in the UK (PRAIS-UK) demonstrated low levels of revascularisation in the UK in patients at high cardiovascular risk. In the study described here, the authors attempted to streamline their referral process for acute revascularisation and conducted an audit to quantify the delay and to monitor outcomes. There were 1,640 percutaneous coronary interventions (PCIs) in West Yorkshire during the year 2000; of these 45% were acute interventions. The catheter laboratory database identified 212 acute PCI patients with a Leeds city postcode. Average times from admission to angiogram, angiogram to intervention, and intervention to discharge are described, as are patient characteristics. Acute and six-month outcome data are given for the whole cohort and for a high-risk subgroup. The six-month composite rate of death and myocardial infarction was lower than that observed in PRAIS-UK. The data show that the time delay between admission and intervention can be kept to a reasonable level.
May 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10:AIC 59–AIC 60
Amnesia: a matter of the heart
Divaka Perera, Neeraj Bhasin, Simon R Redwood

Infective endocarditis can be difficult to diagnose, especially in the absence of typical clinical features or Duke criteria. Seeding of emboli to the cerebral cortex can give rise to neurological symptoms. In the case presented here amnesia was, unusually, the most prominent feature.
May 2003 Br J Cardiol 2003;10:235-40
Hand-held echocardiography for primary care
Han B Xiao

Echocardiography is a commonly used diagnostic tool in assessing cardiac disease. The advent of hand-held ultrasound devices means useful information on cardiac cavity size, ventricular wall thickness and function, or apparent valvular pathology can now be obtained by general practitioners after adequate training. This will be particularly useful in the care of patients with suspected heart failure, left ventricular hypertrophy, a cardiac murmur or atrial fibrillation. It will reduce the number of patients needing referrals and the waiting times for hospital echocardiography services. It is limited by the technical specifications of the equipment and operators expertise.
May 2003 Br J Cardiol 2003;10:230-4
A survey among UK general practitioners on attitudes to cardiovascular postgraduate education
Terry McCormack

A survey on cardiovascular education was sent out to over 1,800 general practitioners by the Primary Care Cardiovascular Society. This generated 304 replies. Of those responding, the majority indicated they would be interested in post-graduate education in cardiovascular medicine. Most would prefer a simple distance-learning course covering the 30 compulsory hours of postgraduate education required every year. Some would be interested in a more demanding course to achieve GPSI status. The majority did not like the current option of clinical assistant work in a hospital out-patients’ department but would attend such a department for education. There were differing views on who should pay for the course.
May 2003 Br J Cardiol 2003;10:229
Cholesterol management and IHD: a comment
John Pittard

A systematic approach to the identification and treatment of high-risk coronary heart disease (CHD) patients has been adopted in the UK health care system.
March 2003 Br J Cardiol (Heart Brain) 2003;10:HB 4–HB 7
Treating the symptoms of vascular dementia
Clive G Ballard

Historically, the approach towards dementia associated with vascular disease has been to manage risk factors. Recent findings also suggest that symptomatic treatment is a realistic option, and cardiologists should be aware of treatments that are, or may soon be, available for their patients. Here, agents that have been evaluated for the symptomatic treatment of vascular dementia (VaD) are reviewed. In particular, the role of cholinesterase inhibitors is discussed. These agents are commonly used worldwide to treat the symptoms of Alzheimer’s disease (AD). Since most patients with VaD have concomitant AD, cholinesterase inhibitors may provide some benefits in these patients. In addition, these agents have demonstrated some efficacy in patients with possible or probable VaD.
March 2003 Br J Cardiol (Heart Brain) 2003;10:HB 8–HB 14
Vascular dementia
Lawrence J Whalley, Alison D Murray

Vascular disease is the most common treatable cause of dementia. Contemporary epidemiological models suggest that in developed Western societies, vascular disease alone accounts for about 15% of all dementia. In association with Alzheimer’s disease, however, it is suspected to be involved in at least 50% of all dementia. Recent research points to shared risk factors in vascular dementia and Alzheimer’s disease, and common pathogenetic processes are likely. The exact criteria required for a diagnosis of vascular dementia remain imprecise and poorly developed. Advances in brain structural and functional imaging provide the best prospects for improvement in vascular dementia diagnosis. Here we set out the major processes that impinge upon the health of neurones and may contribute to vascular dementia. Clinical trials of interventions that might slow progression of cognitive impairment to vascular dementia are fully justified and are likely to improve the care of many old people at particular risk of dementia.
March 2003 Br J Cardiol (Heart Brain) 2003;10:HB 15–HB 19
Antihypertensive treatment and the prevention of stroke and dementia in elderly patients
Arduino A Mangoni, Stephen HD Jackson

Stroke, cognitive impairment and dementia are well-established complications of long-standing hypertension. There is a considerable time lag, usually several decades, between the onset of hypertension and the occurrence of these complications. Although antihypertensive treatment has been shown to decrease the risk of a first stroke, little evidence is available on the effects of antihypertensive treatment on the incidence of recurrent cerebrovascular events, cognitive impairment and dementia. The results of recent studies addressing this issue are discussed, along with directions for future research.
March 2003 Br J Cardiol (Heart Brain) 2003;10:HB 20–HB
Vascular dementia – a suitable case for treatment
Roger Bullock

Vascular dementia (VaD) and Alzheimer"s disease (AD) are often described as distinct entities. Recent literature suggests that they may be part of a continuum, where pure VaD is quite rare, Alzheimer"s disease is only 40% of the total and AD with cerebrovascular disease makes up the majority of cases that present to memory clinics. This relationship between VaD and AD is highlighted by their common risk factors – especially cardiovascular. Pure VaD is a heterogeneous entity, now separated clinically and radiologically into cortical, subcortical and strategic infarct subtypes. The treatment of VaD includes the primary and secondary prevention of cardiovascular and cerebrovascular disease; and early signs of a dementia may not always involve memory loss. This can lead to late presentations of patients when the more obvious signs and symptoms occur. Consequently, dementia services should work more closely with cardiology and stroke services in order to detect early cases of VaD. This will be increasingly important as new treatments become available.
March 2003 Br J Cardiol 2003;10:128-36
Antidiabetic drugs
Clifford J Bailey, Caroline Day

Achieving good glycaemic control is an important part of the treatment strategy to minimise vascular complications in diabetes. An expanding range of differently acting oral antidiabetic agents provides new choices for type 2 patients. This review considers the attributes and limitations of these agents, and their positioning in the treatment process.
March 2003
My approach to assessing CHD risk
Rubin Minhas

My approach to assessing CHD risk
March 2003 Br J Cardiol 2003;10:155-58
Drawbacks and benefits of cardiovascular risk tools

There are now well-recognised guidelines which state that when reducing someone’s risk of cardiovascular disease the decision to start medication depends on the patient’s absolute risk of coronary heart disease, as opposed to their relative risk, which should be determined using multiple risk factors. More than 29 cardiovascular risk tools are available to calculate a patient’s absolute risk of cardiovascular disease. Choosing which risk tool to use can be difficult. This article gives a description of the differences between cardiovascular risk tools. It also discusses some of the problems and benefits of risk tools in general and examines the differences between absolute and relative risk.
March 2003 Br J Cardiol 2003;10:145-52
A four-year audit of secondary prevention in a single general practice
George Savage, Peter Ewing, Helen Kirkwood, Katrina Cowie

Scotland has one of the highest mortality rates for ischaemic heart disease (IHD) in the world, accounting for one quarter of all deaths. Much evidence demonstrates aggressive management of risk factors can make a significant difference to this high morbidity and mortality. Current evidence suggests that secondary prevention of IHD is currently not carried out well in primary care in the UK. Our practice set out to see if this could be improved by using computer records. Over the course of four years more than 80% of IHD patients are now on aspirin, almost 90% have blood pressure recorded annually (average 130/74 mmHg), 82% are non-smokers, 84% have an annual cholesterol check, 65% have a cholesterol < 5 mmol/L, 56% are on a cholesterol-lowering drug (average cholesterol is 4.76 mmol/L), 61% are on cardioprotective drugs, and there was one acute infarct. We suggest that secondary prevention can be improved at a practice level with a good recording system, and a motivated primary care team.
March 2003 Br J Cardiol 2003;10:143-4
Syncope and chest pain at rest in aortic stenosis
Simon G Williams, Steven J Lindsay

Angina pectoris occurs in 30–40% of patients with aortic stenosis, despite a normal coronary circulation. This along with syncope, classically occurs during exercise. There are a number of suggested pathophysiological mechanisms for these symptoms, all of which lead to an imbalance between myocardial oxygen supply and demand. We report an 81-year-old patient who had several episodes of chest pain occurring at rest, leading to syncope resulting in electro-mechanical disassociation (EMD) cardiac arrest. The electrocardiogram (ECG) during these episodes showed profound ST depression, leading to the hypothesis that the underlying pathophysiology was due to myocardial ischaemia caused by the aortic stenosis alone.
March 2003 Br J Cardiol 2003;10:137-40
Sibutramine: a safety profile
Omar Ali

Sibutramine is one of two anti-obesity agents approved by the National Institute of Clinical Excellence. It inhibits the re-uptake of noradrenaline and serotonin in the brain. By enhancing the sensation of satiety after a meal and reducing the fall in basal metabolic rate which usually occurs during weight loss, sibutramine is a useful aid to achieving weight loss and weight maintenance. Randomised controlled trials have shown that sibutramine 10 mg/day, in combination with diet and exercise, produces and maintains a dose-related weight loss of 5–10% in the majority of obese patients studied. This is accompanied by a range of important health benefits, including improvements in cholesterol and triglyceride levels. Adverse publicity led to the European Commission's Committee for Proprietary Medicinal Products recently carrying out an in-depth investigation into the use of sibutramine in over 12,000 patients across Europe. Its findings support the use of sibutramine in obesity management, with no causal link found between the use of the drug and mortality. No change has been made to the Summary Product of Characteristics regarding the cardiovascular safety of sibutramine and the drug has been re-instated for use in Italy. Prescribers should be aware of the cautions surrounding sibutramine use. While it is not advisable for those with a history of coronary heart disease or cardiac arrhythmias, published data reveal that most patients on sibutramine experience a drop in blood pressure and it may be used safely in patients with controlled hypertension. A small number of patients treated may show increases in blood pressure, particularly those who appear to be non-responders. Regular blood pressure monitoring is therefore advised.
March 2003 Br J Cardiol 2003;10:123-7
Heart disease in older patients: myocardial infarction
Lewis E Vickers, Jacqueline Taylor, Adrian JB Brady

Almost a half of all myocardial infarctions occur in those over 70 years of age and this is projected to rise further as the number of older patients in the total population increases. Following myocardial infarction, complications are more common in the older patient and the mortality outlook is much worse in those aged over 75 years. Guidelines generally favour the administration of thrombolysis post-myocardial infarction to older patients, although there is a lack of randomised clinical trials with thrombolysis in this group. Observational data, however, suggest that there is a significantly increased risk of mortality in patients aged over 75 years and this means the elderly are less likely to receive thrombolytic therapy, even when no contraindications are present. Randomised trials have shown that percutaneous coronary intervention is associated with a better outcome in the older patient. With the advances in antiplatelet therapy and the advent of intracoronary stents, this outcome is expected to improve further. The article also discusses therapeutic options in secondary prevention.
March 2003 Br J Cardiol 2003;10:118-22
The role of homocysteine in the clinical assessment of cardiovascular risk
Jennifer Bexley

Clinical and epidemiological studies suggest elevated levels of total plasma homocysteine (> 15 µmol/L) are associated with an increased risk of cardiovascular disease, independent of other known risk factors. This review outlines the causes of hyperhomocysteinaemia, current evidence of a positive association with cardiovascular disease, and how such findings may have important implications for future assessments of risk and nutritional recommendations, particularly for those with a previous or family history of cardiovascular disease.
March 2003 Br J Cardiol 2003;10:115-7
Homocysteine and cardiovascular disease: time to routinely screen and treat?
Patrick O’Callaghan, Deirdre Ward, Ian Graham

Modest elevations in plasma homocysteine from either genetic or acquired causes appear to relate to cardiovascular disease on the basis of strong epidemiological evidence. We know that homocysteine can be lowered with varying doses of folic acid, with or without vitamins B6 and B12, although we do not yet know the potential cardiovascular benefit of vitamin supplementation in these subjects. Several multicentre interventional trials are underway to address this question and, until these are complete, we recommend a healthy diet high in folate replete foodstuffs. We also recommend oral folic acid supplements in some subjects with cardiovascular disease and high homocysteine, mindful that definitive evidence of benefit is lacking.
March 2003 Br J Cardiol 2003;10:110-2
Ambulatory blood pressure measurement is indispensable to good clinical practice: a comment
Eoin O’Brien

The evidence for ambulatory blood pressure measurement (ABPM) as an indispensable investigation in clinical practice is now overwhelming. For years the argument against ABPM has been based on a lack of evidence showing the technique was superior to conventional measurement in predicting outcome. There is now ample evidence from longitudinal studies that ABPM is a much stronger predictor of cardiovascular morbidity and mortality than conventional measurement.1 Moreover, though the relevance of nocturnal hypertension has been a controversial topic, recent evidence has shown that a non-dipping nocturnal pattern is a strong independent risk for cardiovascular mortality.
March 2003 Br J Cardiol 2003;10:105-9
How can ambulatory blood pressure monitoring help in the management of patients with uncontrolled or variable hypertension?
Wasim Ahmed, Maurice A Jackson, Jonathan Odum, Johann CB Nicholas, Paul B Rylance

The study aim was to compare clinic and 24-hour ambulatory blood pressure monitoring, and to determine the influence of the latter on the management of a group of patients with variable or uncontrolled blood pressure. A retrospective data analysis was carried out on patients selected from out-patient clinics at New Cross Hospital. One hundred and seventy-one patients with uncontrolled or variable blood pressure underwent 24-hour ambulatory blood pressure monitoring and 153 results were analysed. Following ambulatory blood pressure monitoring, 56% of the patients had their treatment regimens either decreased, unaltered or did not require antihypertensive therapy. The study found 24-hour ambulatory blood pressure monitoring helps in the assessment of overall 24-hour blood pressure control of patients and may also help in the better management of difficult groups of patients.
February 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10(1):AIC 17–AIC 20
The role of glucose-insulin-potassium therapy in the current management of acute myocardial infarction
Narbeh Melikian, Farzin Fath-Ordoubadi

Glucose-insulin-potassium (GIK) therapy addresses the metabolic changes of ischaemia secondary to acute myocardial infarction. These changes include elevated plasma free fatty acid concentration and glucose intolerance. A meta-analysis of trials from the pre-thrombolysis era showed a significant reduction in the number of deaths in the GIK group in comparison to placebo (16.1% vs. 21% respectively, p=0.004). High-dose GIK therapy was found to be of particular benefit. Three randomised trials in the post-thrombolysis era have been published, with variable results. The DIGAMI study (in diabetics) and the ECLA pilot trial had positive results: in the latter there was a 60% reduction in in-hospital mortality in patients who received GIK therapy plus reperfusion. By contrast, the Pol-GIK trial was negative. Outstanding questions include the usefulness of GIK therapy and beta blockade in the presence of thrombolysis or primary angioplasty. GIK therapy and beta blockade might act in complementary fashion to antagonise the metabolic changes of ischaemia while thrombolysis or angioplasty improve early reperfusion and limit infarct size. Patients with acute coronary syndrome might benefit more from GIK therapy since they have some coronary flow.
February 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10(1):AIC 22–AIC 27
Percutaneous intervention in unprotected left main coronary disease
Kanarath P Balachandran, Keith G Oldroyd

A significant left main coronary artery (LMCA) stenosis is an important predictor of survival in patients with coronary artery disease. In the past, percutaneous coronary intervention (PCI) was generally restricted to patients with protected left main disease; and >50% stenosis of the LMCA was a contraindication to balloon angioplasty. In the pre-stent era, results of left main balloon angioplasty were poor. For example, in one series, in-hospital mortality was 9.1% in the elective group and 50% in the acute group. The development of coronary stenting and effective antiplatelet therapy in the 1990s stimulated renewed interest in PCI for LMCA disease. A number of studies reported good outcomes for protected LMCA lesions, though results in haemodynamically unstable patients remained poor. The figures for a number of studies of elective PCI for unprotected left main stenosis are also described. The best documented outcomes so far are one-year actuarial survival of 89% in high-risk patients and 98% in low-risk patients. If severe calcification is obvious on angiography or ultrasound then debulking seems sensible. The data suggest that directional coronary atherectomy alone or with stenting may be associated with reduced restenosis rates. The use of glycoprotein IIb/IIIa inhibitors and drug-eluting stents may further improve the outlook for patients with LMCA stenosis.
February 2003 Br J Cardiol (Acute Interv Cardiol) 2003;10(1):AIC 28–AIC 32
‘Real world’ small vessel coronary artery stenting: an analysis
Allison Morton, Thomas Papadopoulos, Clare Wales, Robert Bowes, Stephen Campbell, David Oakley, Nigel Wheeldon, Christopher Newman, David Crossman, David Cumberland, Julian Gunn

The objective of this study was to describe the context, procedural outcome and long-term results of contemporary small vessel (SV) coronary artery stenting. It was set in a tertiary cardiology centre. The study was designed as a retrospective analysis of the procedural and long-term results in a consecutive series of patients undergoing implantation of an SV stent (defined as < 2.5 mm) in 1999–2000. Of the 1,130 percutaneous coronary interventions (PCIs) in the study period, 138 (12%) involved placement of SV stents. Of these interventions 58% consisted of SV stents as sole treatment. Some 69% of patients were male and their mean age was 58 years; 46% were hypertensive, 13% diabetic, 84% hypercholesterolaemic and 18% were smokers. Of these patients 54% were in anginal classes III and IV. Of the SV stents fitted, 94% were 2.5 mm and 6% were 2.0 mm. 75% of SV stents were implanted in main epicardial vessels. The mean follow-up for these patients was 17 months. Long-term symptomatic benefit was achieved in 76%. The major adverse cardiac events (MACE) rate was 15%, comprising 1% acute myocardial infarction (AMI) and 14% re-PCI. There were no deaths. In conclusion, SV stenting in the modern era, in an unselected series of patients, is performed in 12% of PCI procedures. It comprises the sole treatment in 58% of these interventions. The majority of SV stents are 2.5 mm and are placed in main coronary arteries. Procedural and long-term results are excellent. These data may inform the choice of treatment for patients with SV disease and may be useful in planning studies in stenting SVs.
January 2003 Br J Cardiol 2003;10:74-6
Analgesia alert
John K Inman

The mode of action of non-steroidal anti-inflammatory drugs and the role of the cyclo-oxygenase enzymes COX1 and COX2 and their inhibitors is described. These can have potentially serious effects on the cardiovascular and renal system which are discussed. The alternative, widely-prescribed analgesic, paracetamol, is also discussed, as are two theories ‘confounded by indication’ and ‘protopathic bias’ to help explain why paracetamol is sometimes described as being linked to asthma and upper gastro-intestinal damage, both effects not expected from a knowledge of its mode of action.
January 2003 Br J Cardiol 2003;10:70-2
Amiodarone monitoring: involving patients in risk management
Jill Murie

Amiodarone is a potentially hazardous drug indicated for atrial and ventricular arrhythmias. The purpose of the audit was to assess the risk associated with amiodarone therapy and identify measures to improve patient safety. The setting was a rural practice with 13,000 patients in Lanark, Scotland. A computer search identified 16 patients (11 male, five female) receiving amiodarone. The mean age was 74 years (range 61–89 years). Action taken was raising doctor awareness and systematic biochemical and clinical review. Results showed that, in spite of substantial mortality and morbidity prior to the audit, there was no effective practice monitoring system for amiodarone therapy. The prevalence of clinical hypothyroidism and hyperthyroidism (29%) and ‘silent’ biochemical thyroid dysfunction (14%) exceeded published estimates (14–18% and 10% respectively). Although standards improved for biochemical monitoring, increasing awareness of the need for close surveillance did not appear to change the practice of some of the general practitioners (GPs), notably the clinical examination of pulse and blood pressure. The audit demonstrates a need for a more systematic approach to amiodarone monitoring. Recommenda-tions include enhancements to the patient information leaflet, the development of local protocols and patient involvement in quality improvements including improved communication, patient-held record cards, better quality follow-up information, and more effective reporting systems.
January 2003 Br J Cardiol 2003;10:59-68
Current progress in lipid therapy
Rubin Minhas

There is strong evidence to support a causal relationship between the level of circulating plasma cholesterol and the risk of clinically overt coronary heart disease (CHD) events. Current UK guidelines recommend reductions of total cholesterol levels to below 5.0 mmol/L. Statins remain the drugs of first choice for reducing low-density lipoproteins (LDL). Rosuvastatin has already been approved in the Netherlands and is likely to become more widely available in the next year. It has a potent effect in lowering LDL and it also appears to raise high-density lipoproteins (HDL). It has a similar safety profile compared with other statins. Cholesterol absorption inhibitors are a new treatment option for the management of hypercholesterolaemia. Ezetimibe, the first drug in this class, has recently been approved for use in the US and Germany. It selectively inhibits the uptake of dietary and biliary cholesterol at the level of the enterocyte. The site of action of ezetimibe may be the ‘sterol permease’ transport protein. As monotherapy, the role of ezetimibe appears limited at present. However, in combination with a low-dose statin, significant reductions in plasma LDL levels are seen. It may also be a useful agent for patients with homozygous familial hypercholesterolaemia.
January 2003 Br J Cardiol 2003;10:56-7
Pregnancy following heart transplantation: a case report
Thomas A Barker, Lawrence Cotter

The success of developments in heart transplantation has given women recipients the opportunity to have children. The first successful pregnancy in a patient who had received a heart transplant was reported by Lowenstein et al. in 1988.1 The cardiovascular effects of pregnancy demonstrate the durability of transplanted hearts. We report a successful pregnancy in a 20-year-old patient who had previously had a heart transplant; we also discuss the management of such patients.
January 2003 Br J Cardiol 2003;10:50-4
National survey of emergency department management of patients with acute undifferentiated chest pain
Steve Goodacre, Jon Nicholl, Jo Beahan, Deborah Quinney, Simon Capewell

Acute, undifferentiated chest pain (chest pain ?cause) presents a frequent and difficult challenge to clinicians working in the emergency setting. We aimed to survey current management of this problem in UK accident and emergency departments by sending a postal questionnaire to the lead clinician or first named consultant in every major A&E department in the UK.
Responses were received from 177/238 departments (74%). Although 74 departments (42%) had formal guidelines, many referred only to diagnosed coronary syndromes. Guidelines for undifferentiated chest pain usually recommended observation for six to 12 hours followed by troponin testing. Short-stay facilities were available in 38 departments (21%) and were planned for 55 departments (31%). Provocative cardiac testing could be accessed by 38 departments (21%). Patients were admitted by general physicians in 152 hospitals (86%) and cardiologists in 18 (10%). The estimated proportion of patients admitted was extremely variable. Although 45 departments (25%) employed specialist nurses, only in 20 did they manage patients with undifferentiated chest pain.
Reported management of acute, undifferentiated chest pain in the UK shows wide variation. Innovative technologies and diverse methods of service delivery are being adopted in a number of departments. These innovations require thorough evaluation.
January 2003 Br J Cardiol 2003;10:45-48
The future of cardiology – heart disease in older patients
Andrew Docherty, Jacqueline Taylor, Adrian JB Brady

Cardiovascular death is steadily decreasing but still accounts for 40% of deaths (235,000) in this country per year. More than 85% occur in older patients over the age of 65 years. The future of cardiology lies in the delivery of care to this rapidly expanding population of older people, whose growing numbers will account for an increasing trend upwards in the prevalence of cardiovascular morbidity in the UK. There will be increasing numbers of heart failure, hypertension, myocardial infarction, angina, atrial fibrillation, pacemaker implants and heart valve implantation in older patients. Randomised clinical trials often exclude the treatment of these conditions in patients over 75 years and results cannot always be easily extrapolated. Older patients often seem to be disadvantaged when compared with younger patients with cardiovascular disease. This article is the first in a series examining the treatment of older patients with cardiovascular disease.
January 2003 Br J Cardiol 2003;10:36-43
Prescribing of ACE inhibitors and statins after bypass surgery: a missed opportunity for secondary prevention?
R Andrew Archbold, Azfar G Zaman, Nicholas P Curzen, Peter G Mills

Angiotensin-converting enzyme (ACE) inhibitors and statins improve prognosis in patients with coronary artery disease. Effective secondary prevention strategies, however, are frequently under-utilised. We sought to determine prescribing habits for ACE inhibitors and statins in 324 patients undergoing coronary artery bypass graft surgery (CABG) at two regional cardiac centres in the United Kingdom. We prospectively recorded ACE inhibitor and statin use on admission and discharge, ACE inhibitor and statin initiation and withdrawal during the hospital stay, and sought associations with treatment withdrawal. 82 (25.3%) patients were taking an ACE inhibitor on admission compared with 37 (11.4%) at discharge (p<0.0005). An ACE inhibitor was initiated during the hospital stay in five (1.5%) patients and was withdrawn in 50 (15.4%). On admission, 157 (48.5%) patients were receiving statin therapy compared with 154 (47.5%) at discharge (p=ns). Statin treatment was initiated in 23 (7.1%) patients, but was withdrawn in 20 (6.2%) others. Thus, only a minority of patients were receiving ACE inhibitors and statins on admission for isolated elective CABG. ACE inhibitor treatment was discontinued during the hospital stay in over 60% of these patients. Furthermore, statin therapy was no more common at discharge than on admission. This study highlights a missed opportunity for effective secondary prevention in a high risk population.
January 2003 Br J Cardiol 2003;10:29-34
The SIGN guideline on cardiac rehabilitation
Chris Isles

The SIGN guideline on cardiac rehabilitation was published in January 2002 and endorsed by the British Association of Cardiac Rehabilitation. This paper summarises the recommendations, which cover all four phases of recovery and the three main cardiac rehabilitation interventions.
November 2002 Br J Cardiol 2002;9:624-7
Early thrombolysis for the treatment of acute myocardial infarction. Who will provide this treatment in the UK? Part II.
Terry McCormack

This article describes the successful provision of a thrombolysis service by general practitioners in the isolated rural area of Whitby, North Yorkshire, and also in rural areas of Sweden. It discusses the difficulties in providing such a service, particularly the rural/urban paradox whereby specialist pre-hospital thrombolysis services can be much more easily provided in urban areas than rural areas where the need is normally much greater. The results of a small straw poll on thrombolysis amongst Primary Care Cardiovascular Society members show that rural general practitioners are much more interested in providing a pre-hospital thrombolysis service than their urban colleagues; paying a fee for such a service should be considered in future planning. The article also reviews the various thrombolytic agents favouring the use of fibrin-specific thrombolytic agents by bolus for pre-hospital thrombolysis.
November 2002 Br J Cardiol 2002;9:640-4
Hypertension trials – the current evidence base and forthcoming trials
Peter Sever, Neil Poulter

Recently reported and ongoing morbidity and mortality trials in hypertensive patients are addressing important unanswered questions in hypertension management. What is the optimal first-line treatment for hypertension, what is the ideal combination of antihypertensive drugs, how are these influenced in particular patient subgroups, and what are the treatment thresholds and blood pressure goals of treatment for optimal prevention of cardiovascular disease? Limitations of some recent trials are highlighted and emphasise the need for further prospective meta-analyses of studies to provide adequate power to address some of these important questions. Current ongoing large scale studies, including ALLHAT and ASCOT, will shortly be reporting results to the scientific community and are likely to influence management decisions across a wide range of patient subgroups.
November 2002 Br J Cardiol 2002;9:634-8
The HEARTS collaboration – delivering improved secondary prevention of CHD for patients with heart disease
Frank Sullivan, Stuart D Pringle, Hamish Dougall, Neill McEwan, Gavin Murphy, Douglas Boyle, Andrew D Morris

Full implementation of the available evidence on secondary prevention should ensure that all patients after myocardial infarction should be offered both effective treatment and be maintained on treatment. This article describes the Heart disease Evidence-based Audit and Research in Tayside Scotland (HEARTS) collaboration which has been set up to try and achieve this. HEARTS can collect electronic data from many sources; prioritise data from multiple sources, such as hospital and general practice; process and link patient records; and, allow manual validation of electronic data. It can also facilitate clinical governance issues in general practice and hospital plus disseminate information to patients. It is hoped that, in addition to secondary prevention, it will be able to extend its focus to other aspects of cardiovascular disease in the future as well as being used for epidemiological and qualitative projects. The system maintains the security and rights of patients at all times.
November 2002 Br J Cardiol 2002;9:630-33
The electronic health record and the management of cardiovascular disease
Alan G Begg, John M Griffith

A dvanced web-based clinical care applications as part of an electronic health record can assist clinicians to meet Government targets for the management of cardiovascular disease. A clinical module of the Tayside electronic health record collects electronic data automatically from a variety of sources and holds this data in a central regional repository. It identifies those patients with existing cardiovascular disease and also those high priority patients at risk of developing clinical atherosclerosis. It allows the clinician to effectively manage these patients in line with national evidence-based guidelines. Real time audit of patient management is instantly available at the point of direct patient contact, as well as benchmarking to agreed performance criteria. Demonstrating improvement in clinical outcomes remains the eventual goal.
November 2002 Br J Cardiol 2002;9:615-6
An unusual case of pericardial constriction
Michael Pitt, Stephen Rooney, R Gordon Murray

An unusual case of pericardial constriction Michael Pitt, Stephen Rooney, R Gordon Murray Pericardial constriction remains a rare condition. The precise aetiology is undefined in up to 50% of cases. We describe a case of rapidly progressive pericardial constriction and highlight how post-mortem examination remains useful in establishing unexpected diagnoses.
November 2002 Br J Cardiol 2002;9:611-3
In-patient transfer for coronary angiography: a substitute for clinical evaluation?
Emma Helm, Elizabeth Hamlyn, John Chambers

Waiting for in-patient transfer for the investigation of chest pain is a significant cause of ‘bed-blocking’. We performed an audit of 58 consecutive in-patient transfers. The mean delay between referral and transfer was 10 days (range one to 28 days). At the time of transfer the mean number of pain-free days was five (range one to 21 days). Of the 37 patients with a working diagnosis of unstable angina, only 19 (51%) underwent some sort of non-invasive risk stratification prior to referral, nine patients (24%) were walking around the hospital or had taken weekend leave and 13 (35%) had normal anatomy or subcritical disease. Of 21 with post-infarct angina, seven (33%) underwent exercise stress testing, five (24%) were mobilising around the hospital and 18 (86%) underwent some sort of intervention. In conclusion, waiting times for in-patient angiography were long and utilisation of non-invasive investigation was low.
November 2002 Br J Cardiol 2002;9:609-10
Fish oils and cardioprotection – mechanisms explored
Derek M Yellon, Derek Hausenloy

Interest in the cardioprotective properties of marine omega-3 polyunsaturated fatty acids (n-3 PUFAs) has been renewed following the publication of three large trials earlier this year demonstrating a reduction in sudden cardiac deaths from the ingestion of marine n-3 PUFAs, along with the recent availability in the UK of its pharmacological equivalent, Omacor™. Secondary prevention trials, such as the Diet and Reinfarction Trial (DART) and the more recent analysis of the GISSI-Prevenzione data, found a reduction in sudden deaths associated with supplementation of n-3 PUFAs in post-myocardial infarction patients.1,2
November 2002 Br J Cardiol 2002;9:600-9
What is the current role of omega-3 polyunsaturated fatty acids in post-myocardial infarction management?
Lena Marie Izzat, Philip Avery

The low incidence of ischaemic heart disease amongst Greenlandic Eskimos has intrigued researchers for many years. The answer was found in their marine-based diet, very rich in omega-3 polyunsaturated fatty acids (n-3 PUFAs). These have shown anti-arrhythmic, endothelial protective, anti-atherogenic, antithrombotic and antiplatelet effects in many observational studies, which have paved the way for the potential role in secondary prevention post-myocardial infarction. Many trials have emphasised the importance of oily fish in the secondary prevention of coronary heart disease. Oily fish consumption, however, is poor in the UK. It has the disadvantages of possible toxic chemical contaminants, a large calorific content and some people simply do not like it. The GISSI-Prevenzione trial studied the effect of a highly purified n-3 PUFA supplement and found it conferred a 20% relative risk reduction in mortality and a 45% reduction in the risk of sudden cardiac death. This early protection supports the anti-arrhythmic potential of n-3 PUFAs. A supplement containing 90% concentrate of the n-3 PUFAs, eicosapentaenoic acid and docosahexanoic acid, known as Omacor™, is now licensed in the UK as adjuvant treatment in secondary prevention post-myocardial infarction, in addition to standard medical treatment including statins. The prescription of n-3 PUFA supplements are best initiated in secondary care. The index admission is generally the best time to initiate secondary prevention when patients tend to be most receptive.
November 2002 Br J Cardiol 2002;9:593-9
The cardiological complications associated with HIV infection and acquired immune deficiency syndrome (AIDS)
Timothy C Hardman, Scott D Purdon

Our increased understanding of the human immunodeficiency virus (HIV), including elucidation of the processes of transmission and replication, has led to the development of relatively effective therapies to minimise and manage the clinical consequences of HIV infection. These therapeutic developments have undoubtedly improved rates of morbidity and mortality in infected patients. The improvements in quality of life and life expectancy have been accompanied by an increase in the number of patients demonstrating cardiac complications, occurring either as a result of the infection itself or the drugs used to control the virus. Cardiac involvement occurs frequently in HIV/AIDS patients and it seems likely that the myocardium, pericardium and/or endocardium are involved. Myocarditis, one of the most common types of cardiac involvement observed in HIV patients, the cause of which can be difficult to identify, may be responsible for myocardial dysfunction. Opportunistic infections, including HIV itself, have been suggested as the cause of myocarditis. Dilated cardiomyopathy is usually found in the late stage of HIV infection and myocarditis may be the triggering causative factor. The mechanism behind pericardial effusion remains unclear but it too may be related to infections or neoplasms. Non-bacterial thrombotic endocarditis and infective endocarditis have been described in AIDS patients, both of which cause significant morbidity. Human immunodeficiency virus-related pulmonary hypertension is a diagnosis of exclusion, and symptoms and signs may mimic other pulmonary conditions in AIDS patients. Cardiac Kaposi’s sarcoma and cardiac lymphoma are the frequently encountered malignant neoplasms in AIDS patients – the prognosis is grave in patients with these conditions.
November 2002 Br J Cardiol 2002;9:567-69
Improving care for patients with heart disease: implications of the Fifth report on the provision of services for patients with heart disease
Paul Kalra, Roger Hall, John Camm

Details of the ‘Fifth report on the provision of services for patients with heart disease’, compiled jointly by the British Cardiac Society and the Royal College of Physicians, were published recently. We recommend that all health workers concerned with the care and management of patients with cardiovascular disorders should be aware of the report and contribute to its implementation.
October 2002 Br J Cardiol 2002;9:554-9
Implementation of the National Service Framework for Coronary Heart Disease in primary care
Caroline Levie, Stewart Findlay

The innovation of specialist nurses in coronary heart disease prevention across 12 practices in a rural County Durham Primary Care Trust (PCT) with a high rate of premature death from heart disease helped the Trust achieve the National Service Frame-work (NSF) for Coronary Heart Disease (CHD) targets and milestones. The introduction of nurse-led CHD clinics at each practice provided a structured follow-up for all patients with CHD to locally agreed guidelines. Audit data collected showed that after 12 months, the service showed an improved management of secondary prevention: more patients had had their cholesterol measured, more had received lipid-lowering medication and more had achieved target cholesterol levels of < 5.0 mmol/L than at baseline. Aspirin prescribing also increased. The PCT has also recently introduced a specialist heart failure nurse to carry out a similar programme and, in addition, has addressed cardiac rehabilitation to provide a home-based service for some patients.
October 2002 Br J Cardiol 2002;9:549-52
Early thrombolysis for the treatment of acute myocardial infarction. Who will provide this treatment in the UK? Part 1
Terry McCormack

This article looks at the results of four studies which examined the delivery of early thrombolysis by general practitioners and ambulance paramedics to patients suffering an acute myocardial infarction. The studies found that they could provide early thrombolysis safely. One study in an isolated rural area in Scotland found general practitioners would have very limited experience of thrombolysis – one case per general practitioner per year – and that use of thrombolysis by local general practitioners fell off sharply after the study. A second study carried out in 15 European countries and Canada, found that there was no significant improvement in mortality and morbidity in the pre-hospital group given thrombolysis at home. This was also found by a Dutch study. An American study using computer-assisted diagnostic ECGs relayed to a physician at the base hospital, found little difference in the pre-hospital and hospital treatment arms but a dramatic improvement in the speed of treatment of both groups. Pre-hospital thrombolysis was also reduced. Two studies found ambulances became ‘tied up’ when thrombolysis was delivered at home. These studies were used as part of a submission on behalf of the Primary Care Cardiovascular Society to the National Institute for Clinical Excellence. The rest of the submission is discussed in part two of this article next month.
October 2002 Br J Cardiol 2002;9:546-7
Atrial fibrillation in a patient with Wolff-Parkinson-White syndrome
Tariq Azeem, Seong Som Chuah, Philip S Lewis

The authors describe a case of a Wolff-Parkinson-White syndrome patient experiencing atrial fibrillation, which was difficult to distinguish from ventricular tachycardia.
October 2002 Br J Cardiol 2002;9:539-45
Revascularisation and beyond
Wiek H van Gilst, Freek WA Verheugt, Felix Zijlstra, William E Boden

Thrombolytic therapy has revolutionised the management of acute myocardial infarction (MI) and saved many thousands of lives. Since these agents first became available nearly 20 years ago, many new pharmacological therapies have been developed to try and improve both short-term and long-term outcome following MI. Surgical interventions too are being considered as a serious option during the immediate post-MI period to avoid the adverse effects of thrombolysis and improve long-term outcome. At the same time, research is focusing on what therapy should follow acute MI treatment to improve the long-term outlook for patients. Both old and new therapeutic options need to be considered to offer patients the best chance of a full recovery and long-term survival after MI.
October 2002 Br J Cardiol 2002;9:538
Intracavity gradients during stress echocardiography
David Platts, Mark Monaghan

These images are from a 65-year-old woman referred for stress echocardiography following a history of exercise-induced dizziness and shortness of breath. A dobutamine stress echocardiogram was performed. The resting heart rate was 90 beats per minute and resting blood pressure was 210/90 mmHg. The resting images showed severe concentric left ventricular hypertrophy with normal systolic function.
October 2002 Br J Cardiol 2002;9:533-7
Aldosterone antagonism: new ideas, new drugs
Mike Schachter

In the last few years our ideas about the physiological and pathological roles of aldosterone have changed enormously. It is now widely recognised that this hormone not only plays a crucial role in normal salt and water regulation, and its abnormalities in congestive heart failure and some types of hypertension, but also has other effects. These may include the promotion of cardiac and vascular inflammation and fibrosis and increased likelihood of arrhythmias. These perspectives coincide with a revived interest in aldosterone antagonists, particularly since the RALES trial showing the benefits of spironolactone in patients with congestive heart failure. This long-established drug does unfortunately have serious adverse effects, notably gynaecomastia and menstrual abnormalities. New drugs, such as eplerenone, are being developed which are more selective for the aldosterone receptor and have less interaction with receptors for other steroid hormones. Early studies indicate that this drug may have comparable efficacy to spironolactone in patients with hypertension and heart failure, while adverse effects appear to be less frequent and severe. The development of such compounds will encourage greater emphasis on aldosterone antagonism in cardiovascular drug therapy.
October 2002 Br J Cardiol 2002;9:530-2
Workload implications of hypertension guidelines: a general practice view
Kathryn E Griffith

The major objective for the diagnosis and treatment of hypertension should be the detection of those at increased risk of coronary heart disease (CHD) and stroke, and the reduction of this risk.
October 2002 Br J Cardiol 2002;9:524-30
Workload implications of implementing national guidelines for hypertension
Karen Rowland Yeo, Wilfred W Yeo

We examined the workload implications of the National Service Framework for Coronary Heart Disease and the 1999 British Hypertension Society guidelines for the management of hypertension in clinical practice. The 1998 Health Survey for England was used to estimate the proportion of the English population aged 35 to 74 years that may require antihypertensive therapy. Of 8,154 subjects with blood pressure measurements, 400 (4.9%; 95% CI 4.4 to 5.4%) with cardiovascular disease were taking antihypertensive drugs and a further 100 (1.2%; 1.0 to 1.5%) were at treatment thresholds for secondary prevention of cardiovascular disease. There were 848 (10.4%; 9.7 to 11.1%) subjects free of cardiovascular disease on antihypertensive therapy and an additional 1,083 (13.3%; 12.5 to 14.0%) were identified for treatment. We estimate that 29.8% (28.8 to 30.8%) of the English population aged 35 to 74 years were candidates for antihypertensive therapy, of which 15.3% (14.5 to 16.1%) were already being treated but only 5.4% (4.9 to 5.9%) had their blood pressure controlled. An additional 14.5% of the English population will need antihypertensive therapy and an extra 9.9 % will need to have their treatment intensified to attain the blood pressure targets set by the British Hypertension Society guidelines.
October 2002 Br J Cardiol 2002;9:519-23
The current status of combined heart and kidney transplantation
Jo Chikwe, John Pepper

Heart transplantation is an accepted therapeutic option in selected patients with end-stage heart failure. Up to 10% of patients develop renal failure while on the waiting list for heart transplantation. Renal dysfunction is a relative contraindication to heart transplantation. In order to establish current practice in UK heart transplant centres and overall surgical outcomes for combined heart and kidney transplantation, we surveyed the eight units currently responsible for heart transplantation, all but one of which had carried out at least one combined heart and kidney transplant. We obtained outcome data from the United Kingdom Transplant organisation. We found a wide variability in the level of renal function considered a contraindication to heart transplantation, and no consensus on the criteria for combined heart and kidney transplantation. The 30-day mortality was 14% (4/28) and survival at one, three, five and 10 years was 66.5 (95% confidence interval 57.3–75.7), 50.2 (40.3–60.1), 45.6 (35.6–55.7), and 30.8 (19.2–42.4) respectively, with significant variability between centres. A prospective, controlled trial is needed to address these issues, but such a study remains extremely unlikely in the context of the increasing scarcity of organ donors.
September 2002 Br J Cardiol 2002;9:488-90
Secondary prevention in patients awaiting CABG in the North West of England

This study looks at how well cardiovascular risk factors were being controlled in a high-risk group of patients awaiting coronary artery bypass surgery. It shows significant short falls in the implementation of currently advocated strategies.
September 2002 Br J Cardiol 2002;9:481-7
GP use of beta blockers in heart failure
Mike Mead

This article explains how general practitioners can diagnose and treat heart failure in primary care. Diagnosis is difficult and four diagnostic tests – the electrocardiogram, chest x-ray, blood test for natriuretic peptides and echocardiography – are recommended as being of particular value in confirming the diagnosis in primary care.
A six-step treatment strategy is then given advising i) confirming the diagnosis, ii) excluding other treatable causes of heart failure, iii) giving general advice to the patient, iv) starting treatment with a diuretic, v) then adding an angiotensin-converting enzyme inhibitor, and, vi) finally adding a beta blocker. A 10-point plan explaining in detail how to start beta blockers in primary care concludes the article.
September 2002 Br J Cardiol 2002;9:478-80
Pleuritic chest pain and hypoxia – a diagnostic dilemma
Sanjiv Mahadeva, Pulak Sahay, Richard V Lewis

Pleuritic chest pain and hypoxia – a diagnostic dilemma Sanjiv Mahadeva, Pulak Sahay, Richard V Lewis Pulmonary thromboembolism (PE) is notoriously difficult to diagnose since it commonly presents in a non-specific manner. Only 15–30% of the patients identified at post-mortem as having a massive PE have been diagnosed correctly prior to death.1,2 However, large studies have shown that certain clinical symptoms and features such as dyspnoea, tachypnoea, pleuritic chest pain with a normal chest radiograph and a low PaO2 are present in more than 90% of patients with PE.2 Clinicians in a district hospital setting have to rely on these features, especially when facilities for detailed imaging such as computerised tomography (CT) or pulmonary angiography are not available. Occasionally, certain other diseases can mimic the clinical picture of PE and lead to delay in instituting appropriate treatment. We present two patients with symptoms and clinical investigations which were highly suggestive of acute PE but who turned out to have very different diagnoses in the end.
September 2002 Br J Cardiol 2002;9:476-7
Rapid appraisal of clinicians’ reactions to guidance from the National Institute of Clinical Excellence on use of glycoprotein IIb/IIIa antagonists for acute coronary syndromes
Khaled Alfakih, Alistair Hall, Mike Robinson

Rapid appraisal of clinicians’ reactions to guidance from the National Institute of Clinical Excellence on use of glycoprotein IIb/IIIa antagonists for acute coronary syndromes Khaled Alfakih, Alistair Hall, Mike Robinson We conducted a postal survey of UK consultant cardiologists to assess reaction to the guidance issued by the National Institute of Clinical Excellence (NICE) on the use of glycoprotein IIb/IIIa antagonists (GPAs) for acute coronary syndromes.
September 2002 Br J Cardiol 2002;9:469-75
Extended-release fluvastatin 80 mg shows greater efficacy, with comparable tolerability, versus immediate-release fluvastatin 40 mg for once daily treatment of primary hypercholesterolaemia
Donald B Hunninghake, Michael Davidson, Howard R Knapp, Helmut G Schrott, Sheryl Manfreda, and the Fluvastatin Study Group

A new extended-release (XL) formulation of fluvastatin has been developed for once daily treatment of primary hypercholesterolaemia. This study was designed to determine the safety and effect of fluvastatin XL 80 mg on a range of lipid parameters compared with the immediate-release (IR) formulation of fluvastatin 40 mg. In a multicentre, double-blind study, 555 patients with primary hypercholesterolaemia (Fredrickson types IIa or IIb) were randomised to 24 weeks treatment with fluvastatin XL 80 mg or IR 40 mg, each given once daily at bedtime. The study found the least square mean reduction in LDL-C after 24 weeks treatment was 32.6% in the fluvastatin XL 80 mg group (n=312) and 23.9% in the fluvastatin IR 40 mg group (n=165), an 8.7% between-treatment difference (95% confidence interval: 6.5%, 10.9%) in favour of the XL formulation (p<0.001). A higher proportion of patients in the fluvastatin XL 80 mg group achieved ≥ 35% reductions in low-density lipoprotein cholesterol (42.3% vs. 13.3%). High-density lipoprotein cholesterol levels were increased by 9.1% and 7.0%, respectively in the XL and IR groups; median triglyceride levels fell by 19% and 13%, respectively. Tolerability was comparable in the two groups, and there were no laboratory safety concerns. The study concluded that fluvastatin XL 80 mg once daily is safe as a starting dose and effectively lowers low-density lipoprotein cholesterol and triglyceride levels in patients with primary hypercholesterolaemia.
September 2002 Br J Cardiol 2002;9:460-8
The role of orlistat in the treatment of obese patients with mild to moderate hypercholesterolaemia: consequences for coronary risk
Iain Broom, Elixabeth Hughes, Paul Dodson, John Reckless, on behalf of the Orlistat UK Study Group

This study investigated the effect of orlistat on weight loss and serum lipid parameters in obese patients with hypercholesterolaemia. A total of 215 adult obese patients (body mass index ≥30 kg/m2) with hypercholesterolaemia (total plasma cholesterol ≥6.5 mmol/L or plasma low density lipoprotein cholesterol ≥4.2 mmol/L) were recruited for screening at 12 out-patient clinics in the UK. Of these, 142 patients were randomised to receive double-blind treatment for 24 weeks with orlistat 120 mg (n=71) or placebo (n=71) three times daily in combination with a mildly hypocaloric diet. Patients completing the double-blind phase (orlistat n=42, placebo n=55) were eligible to enter a further 28-week open-label phase and received orlistat 120 mg three times daily in combination with the hypocaloric diet. Mean weight loss after 24 weeks was 4.4 kg (4.4%) in the orlistat group vs. 2.6 kg (2.5%) with placebo (p<0.01). At the end of the double-blind phase, 44.0% of orlistat-treated patients vs. 18.0% of placebo recipients had lost ≥5% of their initial body weight (p<0.001), and 7.6% vs. 4.2% had lost ≥10% (p=NS). Patients who continued on orlistat during the open-label phase had a mean weight loss of 4.97 kg (4.86%) after 52 weeks. Patients who switched to orlistat had a mean weight loss of 4.28 kg (4.23%). Orlistat was associated with significantly greater reductions than placebo in plasma total cholesterol (-10.88 + 1.36% vs. -3.25 + 1.33%; p<0.001) and LDL-cholesterol (-14.14 + 2.68% vs. -3.68 + 3.61%; p<0.05) during the double-blind phase. Despite similar weight loss at the end of the 52-week period, patients who remained on orlistat throughout the study had greater improvements in plasma lipid concentrations than patients who switched to orlistat after 24 weeks. Orlistat, in combination with a mildly hypocaloric diet, promotes clinically meaningful weight loss and improvements in lipid concentrations in obese patients with hypercholesterolaemia.
September 2002 Br J Cardiol 2002;9:449-59
Hypertrophic cardiomyopathy: from gene to bedside
Sami Firoozi, Julia Rahman, William J McKenna

Hypertrophic cardiomyopathy (HCM) is the commonest inherited cardiovascular disorder with a prevalence of one in 500 in the general population. It is believed to be a disease of the cardiac sarcomere and is caused by a variety of mutations in genes responsible for sarcomeric contractile proteins. It is characterised macroscopically by myocardial hypertrophy and microscopically by myocyte fibrosis and disarray. Most patients tend to present with functional limitation and symptoms such as palpitation, chest pain or syncope. The underlying mechanisms involved are complex, multiple and not yet fully understood. Further clarification of these mechanisms may enable improvements in current symptom control or the development of new avenues of therapy. A small but significant proportion of patients suffer sudden cardiac death and this can be the initial presentation of the condition. In fact, HCM is the commonest cause of sudden death among individuals below the age of 30 years. The identification of this high-risk cohort remains the most important aspect of HCM management, particularly in light of growing evidence of the effectiveness of prophylactic strategies.

September 2002 Br J Cardiol (Acute Interv Cardiol) 2002;9(1):AIC 5–AIC 10
League tables, risk assessment and an opportunity to improve standards
Stephen Westaby

The implications of the Secretary of State’s approval of the introduction of league tables for cardiac surgeons are discussed. Surgeons are to be ranked according to mortality rates for first-time coronary artery bypass graft operations. It is questionable whether anybody will gain from this information: the focus of surgeons’ attention is transferred from patient care to self-preservation. The introduction of league tables in New York State has resulted in surgeons being reluctant to operate on higher risk patients and in secondary referrals of patients out of the State. League tables also encourage the manipulation of risk factor status. Many factors other than the individual surgeon’s skill influence the quality of care and patient outcomes. These factors include the patient’s status, the timing of surgery, the surgical team, equipment in the operating room and post-operative care. An alternative to the punitive process of public reporting is the application of continuous quality improvement to healthcare. This starts from the position that most negative outcomes are due not to individual failures but to failures of process and systems.
September 2002 Br J Cardiol (Acute Interv Cardiol) 2002;9(1):AIC 13–AIC 17
Are waiting times for coronary artery bypass graft surgery longer than they should be? Implications of the NICE guidelines for coronary artery stents
Marios Tryfonidis, Brian Prendergast, Nicholas Curzen

The objective of this study was to test the hypothesis that some patients on the routine waiting list for coronary artery bypass (CABG) surgery are suitable for percutaneous coronary intervention (PCI), as suggested in the NICE appraisal of coronary artery stents. A retrospective analysis was performed of 100 consecutive patients who had recently undergone CABG surgery from the routine waiting list in a tertiary cardiothoracic centre. The coronary angiograms of these patients were reviewed by an interventional cardiologist and a cardiac surgeon to assess patients’ potential suitability for PCI. The mean total waiting time from being listed for angiography to having CABG surgery was 18.7 months. The mean delay from angiography to CABG surgery was 13.5 months. Of the 100-patient cohort, 70 were referred by a non-interventional cardiologist and 30 by an interventionalist (ratio 2.3:1). Fifteen patients were deemed potentially suitable for PCI after angiographic review. Of these, 13 (87%) were referred by a non-interventional cardiologist without angiographic review by an interventional specialist. The majority (86%) of the 15 patients deemed potentially suitable for PCI had single or double vessel coronary artery disease, in contrast to the population as a whole (38%). These data suggest (a) that current CABG waiting lists could be reduced by up to 15% if coronary angiograms were reviewed by an interventional cardiologist in addition to a consultant cardiothoracic surgeon and (b) that referral arrangements should be adopted to facilitate such a review. The clinical implications of these data could be fully assessed by rolling out prospectively to other groups in the Coronary Heart Disease Collaborative.
September 2002 Br J Cardiol (Acute Interv Cardiol) 2002;9(1):AIC 20–AIC 25
Volumetric haemodynamic monitoring and continuous pulse contour analysis – an untapped resource for coronary and high dependency care units?
Tushar V Saluhke, Duncan LA Wyncoll

Critically ill patients in the coronary care or high dependency units (CCU, HDU) need accurate assessment of their haemodynamic status to guide fluid or vasoactive drug therapy. Both central venous pressure and pulmonary artery occlusion pressure are poor guides to cardiac filling and pulmonary oedema, and using a pulmonary artery catheter often fails to improve clinical outcome. The PiCCO system is a relatively new and less invasive approach to cardiac monitoring. It has been used extensively in intensive care and is reviewed in this article. This approach uses thermo-dilution techniques to reliably calculate volumetric measurements of cardiac preload and cardiac output, and can provide continuous real-time cardiac output and stroke volume variation measurements through pulse contour analysis. The reliability and accuracy of this method has drastically refined fluid and vasopressor management of the hypotensive patient and the management and prevention of pulmonary oedema. This method of measuring cardiac output correlates well with gold standard methods of cardiac output calculation and has been validated in adults and children. The PiCCO system can be an invaluable tool in the optimisation of the circulation in cardiac, medical and surgical patients commonly seen in the CCU and HDU.
September 2002 Br J Cardiol (Acute Interv Cardiol) 2002;9(1):AIC 26–AIC 31
The evolving role of the cardiac inotrope, enoximone, in heart failure
Liam J Cormican, A Craig Davidson

Chronic heart failure is a progressive syndrome which continues to have high rates of morbidity and mortality. Heart failure rates are increasing in parallel with the ageing population, as are rates of hospitalisation for acute episodes of decompensated failure. Little progress has been made in the medical management of such episodes. Positive inotropes, including selective phosphodiesterase III inhibitors, are associated with increased mortality when administered over the long term. Now newer approaches, using selective agents such as enoximone orally at lower doses alone or in combination with carefully titrated beta1-selective adrenergic blockade, may provide a more favourable outcome in terms of symptom management, functional status and improved survival. Trials are underway to determine whether this is the case. Published trials with enoximone and protocols for forthcoming trials are reviewed.
August 2002 Br J Cardiol 2002;9:
The cholesterol management debates
BJCardio editorial team

THE CHOLESTEROL MANAGEMENT DEBATES ESC debate Motion 1: "This house believes that lowering current cholesterol targets will have additional benefits to CV risk management" Motion 2: "This house believes that the benefits of raising HDL warrant its introduction as another lipid variable to target." The lower the better. The real benefits of lowering cholesterol even further The Atlantic divide in coronary prevention PCCS debate Motion 1: "This house believes that current government policy is leading to the erosion of clinical judgement, exemplified by the CHD National Service Framework." Motion 2: "This house believes that optimal management of cholesterol is a relief, not a burden." The National Service Framework for CHD – Big Brother or helpful guide? A stitch in time – counting the cost of optimal CHD prevention
July 2002 Br J Cardiol 2002;9:422-4
Hypertension in the elderly – the primary care perspective
Sarah Jarvis

The proportion of the elderly population is rapidly growing, increasing the numbers of hypertensive patients and the workload in primary care. The average GP will currently have around 100 hypertensive patients over the age of 75 years in their care; this number is likely to be much higher in popular retirement areas. Clinical trials have shown the benefits of vigorous blood pressure control in the elderly; current recommendations are to reduce blood pressure to under 140/85 mmHg in at-risk groups and to under 130/80 mmHg in diabetics. Hypertension treatment continues to be difficult, however, due to poor compliance. This is for a number of reasons, including the fact that it is often a symptomless condition, the side effects of antihypertensive medication and the number of concomitant medical conditions making drug regimes complicated in the elderly. Newer classes of antihypertensive agents, such as beta blockers, angiotensin-converting enzyme inhibitors and angiotensin II receptor antagonists, are proving to reduce other risks as well as reducing blood pressure. Angiotensin II receptor antagonists appear to be better tolerated than other antihypertensive drugs; clinical trial results are awaited to assess their protective effects as well as their effect on quality of life, health economics and cost-effectiveness.
July 2002 Br J Cardiol 2002;9:411-3
Coronary artery ectasia identified on chest X-ray
Duncan Hogg, Stephen Yule, Kevin Jennings

We describe an asymptomatic 51-year-old man in whom severe coronary artery ectasia was evident on a plain AP chest X-ray (CXR).
July 2002 Br J Cardiol 2002;9:406-10
Brugada syndrome: a review
Badri Chandrasekaran, Arvinder S Kurbaan

Brugada syndrome was described 10 years ago. It is a syndrome of sudden cardiac death associated with partial right bundle branch block and ST segment elevation in the right precordial leads V1-V3 on the resting ECG. Those affected have structurally normal hearts (as demonstrated by standard techniques) but they have a mortality rate of 10% a year, whether they are symptomatic or asymptomatic. It is thought to be primarily a disease of cardiac conduction and has been linked to abnormalities in the sodium channel (SCN5A). Differential diagnoses include arrhythmogenic right ventricular dysplasia, idiopathic ventricular fibrillation and polymorphic ventricular tachycardia. Brugada et al. suggest that the Brugada shift pattern on 12-lead ECG is a specific marker for those at risk of sudden death. They recommend that symptomatic individuals be protected with an implantable cardiac defibrillator. Asymptomatic individuals remain a diagnostic dilemma.
July 2002 Br J Cardiol 2002;9:401-5
he effect of nifedipine GITS on outcomes in patients with previous myocardial infarction: a subgroup analysis of the INSIGHT study
Giuseppe Mancia, Luis M Ruilope, Moris J Brown, Christopher R Palmer, Talma Rosenthal, Alain Castaigne, Peter W de Leuw, Gilbert Wagener

Post-myocardial infarction (MI) patients have a higher risk for subsequent cardiovascular and cerebrovascular events than the average population. This study was to test the effects on outcomes of nifedipine GITS compared to the diuretic combination co-amilozide in hypertensive patients with a history of MI on outcomes (subset of the INSIGHT study). The multinational, randomised, double-blind International Nifedipine GITS Study: Intervention as a Goal in Hypertension Treatment (INSIGHT) study compared the treatment effects of nifedipine GITS 30 mg and co-amilozide (hydrochlorothiazide 25 mg plus amiloride 2.5 mg) in hypertensive patients aged 55–80 years with a blood pressure of 150/95 mmHg (or 160 mmHg systolic). This pre-specified subanalysis was performed in patients with a history of MI. The primary outcome was a composite of cardiovascular death, non-fatal stroke, MI, and heart failure. Of 6,321 randomised patients, 383 (6.1%) had a previous MI. The percentage of primary outcomes in post-MI patients did not differ between the two treatment groups (14.9%). The number of post-MI patients with composite secondary outcomes was 53 (27.2%) in the nifedipine GITS group and 60 (31.9%) in the co-amilozide group. The incidence rates of primary and secondary outcomes were higher in patients with a previous MI than in patients without a history of MI. For the randomised use of nifedipine GITS and co-amilozide in hypertensive patients with a previous MI, the choice seemed unimportant for outcomes and blood pressure lowering. The results of this subgroup analysis are consistent with INSIGHT's overall findings of no significant differences in efficacy, suggesting that post-MI hypertensive patients are no more likely to suffer further events when treated with long-acting nifedipine than on co-amilozide.
July 2002 Br J Cardiol 2002;9:394-400
Atherosclerosis imaging and coronary calcification
Matthew J Budoff

Recently published data have greatly expanded the applicability of electron beam tomography and electron beam angiography. Guidelines and policy towards these modalities have shifted, with increased recognition of their importance among experts in cardiology, lipidology and preventive medicine. Given the high sensitivity of coronary calcification for the presence of obstructive coronary artery disease (CAD) (95–99%), exclusion of coronary calcium may be useful as a filter prior to invasive diagnostic procedures or hospital admission.
June 2002 Br J Cardiol 2002;9:362-8
A case study from a Sussex Primary Care Group: improving secondary prevention in coronary heart disease using an educational intervention prevention guidance
Simon de Lusignan, N Hague, Claire Yates, M Harvey

An educational intervention was developed to try to raise both data quality standards and those of clinical care in the secondary prevention of coronary heart disease. The intervention was used within primary care organisations utilising their own clinical data and with primary care professionals learning from each other. A special tool (MIQUEST) was used to extract the clinical data. Anony-mised data were then shared with the whole primary care organisation at six-monthly data quality workshops. Patients needing interventions were identified in individual practices and these practice visits were also used as learning opportunities. At the end of the study there was an increase in the recording of the diagnosis of ischaemc heart disease (IHD).
June 2002 Br J Cardiol 2002;9:359-60
The NHS Plan: general practitioners with special interests
David Colin-Thome

Many general practitioners (GPs) already have a special clinical interest. This role is now being developed and formalised by the Department of Health and by 2004, 1,000 posts of general practitioners with special interests (GPwSI) will have been created. Alongside their normal general practice work, these GPs will also offer a particular specialist service under contract to a Primary Care or Acute Trust taking referrals from fellow GPs. A National Develop-ment Group is currently consulting relevant bodies to publish advice on the commissioning and appointment of such GPs. It is hoped these appointments will help integrate primary care and hospital services under the new NHS Plan, leading to enhanced patient care and the delivery of the National Service Frameworks. It will also give continuing job satisfaction to GPs wanting to extend their role.
June 2002 Br J Cardiol 2002;9:356-7
Serious interaction between digoxin and warfarin
Arpandev Bhattacharyya, Manju Bhavnani, David James Tymms

Drug interaction with warfarin is a common cause of loss of anticoagulant control. An interaction between warfarin and digoxin has not previously been documented in the British National Formulary or datasheet. We report a case of digoxin toxicity responsible for prolongation of the INR to more than 10.
June 2002 Br J Cardiol 2002;9:355
On-call seen as a pathophysiologic state
Johan EP Waktare, Alex Stewart, John P Lyons

On-call seen as a pathophysiologic state Johan EP Waktare, Alex Stewart, John P Lyons Recently, one of us (AS) underwent 24-hour Holter (ambulatory ECG) monitoring for investigation of minor cardiac symptoms. The recording was performed during a night as medical registrar on-call. We feel the result provides some interesting insights into the pathophysiology of life as a modern junior doctor.
June 2002 Br J Cardiol 2002;9:351-4
Patients of Southern Asian descent treated with valsartan (POSATIV) study
Jatin KV Patel and Richard Leaback, on behalf of the POSATIV investigators

Southern Asians in the UK have a substantially increased (50%) risk of coronary heart disease compared with the general population, in part due to a high prevalence of hypertension and diabetes. This patient group has not been specifically studied in a clinical trial using modern antihypertensive therapy such as the angiotensin II receptor antagonists (AIIRAs). A multi-centre, double-blind, randomised, parallel-group study compared the effects of treatment with valsartan 80 mg once daily (o.d.) with control therapy (bendrofluazide 2.5 mg o.d.) in 116 patients with mild hypertension (diastolic blood pressure [DBP] ≥ 90 mmHg and ≤ 105 mmHg) after a four-week run-in period. Sitting blood pressure was measured at baseline (end of run-in) and after four and eight weeks of treatment using the OMRON automatic oscillometric blood pressure monitor. The study medication dosage was doubled if patients had < 4 mmHg decrease in DBP after four weeks. Compared with the control group (n=62), the addition of valsartan 80/160 mg o.d. (n=51) resulted in a significantly greater reduction in blood pressure at eight weeks (mean change in blood pressure -15.6 mmHg [95% CI -19.9 to -11.2 mmHg] for systolic blood pressure [SBP] and -9.3 mmHg [95% CI -11.8 to -6.8 mmHg] for DBP; p<0.001). Both treatments were well tolerated. Valsartan is effective and well tolerated, and would be an appropriate treatment option in Southern Asian hypertensive patients.
June 2002 Br J Cardiol 2002;9:343-50
Efficacy of micronised fenofibrate in patients with primary hyperlipidaemia: a comparison with pravastatin
Jean Ducobu, Luc Van Haelst, Herva Salomon

This randomised, double-blind, six-month trial assessed the efficacy and tolerability of micronised fenofibrate and pravastatin in 265 patients (18–75 years of age) with primary hyperlipidaemia (pure hypercholesterolaemia, type IIa; and mixed dyslipidaemia, type IIb) recruited from 28 European centres. After a first three-month phase in which patients received once daily either micronised fenofibrate 200 mg or pravastatin 20 mg, type IIa patients attaining low density lipoprotein cholesterol (LDL) < 4.14 mmol/L and type IIb patients attaining LDL < 4.14 mmol/L and triglycerides < 2.26 mmol/L continued with the same dose in a three-month extension phase. Patients not meeting these criteria received a double dose of drug in this extension phase.
June 2002 Br J Cardiol 2002;9:339-42
Complications associated with 64 temporary pacing wires implanted at a district general hospital – should this procedure be reserved for specialist centres?
Adam Brown, Barnaby Thwaites

This study assessed complication rates in 64 emergency temporary pacing procedures, of which atrioventricular block formed the largest group (72%). Of the in-hospital deaths, most (76%) were due to myocardial infarction, and none due to the procedure. Immediate complications occurred in 22%: arrhythmia or arterial puncture, and one hemiparesis. Late complications occurred in 34%: loss of capture, infection including one instance of staphylococcal septicaemia. No complications occurred in 59%. Involvement of a consultant in the procedure did not reduce complication rates. In such potentially unstable patients, the risks of not pacing or delaying pacing probably far outweigh those of immediate intervention.
June 2002 Br J Cardiol 2002;9:337-8
Primary pulmonary hypertension: a GP comment
Ross Price

General practitioners (GPs) are subject to bombardments of medical information from many sources – local pharmaceutical formularies, local and national guidelines, national service frameworks, medical newspapers, peer-reviewed national journals and special interest publications.
June 2002 Br J Cardiol 2002;9:330-6
Management of primary pulmonary hypertension
Ghada W Mikhail, J Simon R Gibbs, Magdi H Yacoub

The onset of symptoms in primary pulmonary hypertension (PPH) is usually insidious with several years elapsing before the diagnosis is actually made. It is important that general physicians should be made aware of this fact and that they should have a high rate of suspicion of the subtle nature of the clinical presentation in this group of patients. Patients with a suspected diagnosis of PPH should be referred to specialised centres where early diagnosis and treatment can be initiated. We review the salient features of PPH and provide an insight into the various therapeutic options that are now available for this disease.
May 2002 Br J Cardiol 2002;9:303-4
NICE announce audit of secondary prevention guidance
Tom Quinn

NICE announce audit of secondary prevention guidance Tom Quinn The National Institute for Clinical Excellence (NICE) has ann-ounced plans to commission the development of an audit tool to support the primary care management of patients who have survived myocardial infarction (MI). The audit will focus on aspects of treatment and support highlighted in the National Service Framework (NSF) for Coronary Heart Disease1 and NICE’s own guideline Prophylaxis for patients who have experienced a myocardial infarction,2 inherited from the Department of Health in 1998 and published in early 2001.
May 2002 Br J Cardiol 2002;9:297-02
Optimising management of patients with hypertension and diabetes
George Kassianos

Optimal management of hypertension and diabetes is essential if the cardiovascular and renal mortality and morbidity associated with this condition is to be reduced. Recent guidelines from the National Service Framework for Diabetes and the Scottish Intercollegiate Guidelines Network are discussed. Recent studies (UKPDS, RENAAL and PRIME) looking at the contribution tight blood pressure control and angiotensin II receptor antagonists can make to the management of this hypertension in diabetics are also covered. Finally, the author advises how primary care can implement guidelines in practice to give the best possible care to patients with diabetes.
May 2002 Br J Cardiol 2002;9:294-6
Extensive multiple coronary artery to left ventricular fistulas – a 10-year case history
Matthew J Banks, Jane Flint, Peter R Forsey, George D Kitas

Extensive multiple coronary artery to left ventricular fistulas – a 10-year case history We report the 10-year case history of a 50-year-old woman who presented with angina due to extensive, bilateral, multiple coronary artery to left ventricular fistulas (MCALVF). 201Thallium myocardial scintigraphy revealed reversible ischaemia due to coronary ‘steal’. Cardiac catheterisation showed left ventricular dilatation due to high cardiac output from significant coronary to left ventricular shunt.
May 2002 Br J Cardiol 2002;9:291-3
Coarctation of the aorta: a life-long disease of the entire vascular system
Mark Turner, Dirk Wilson, Andrew J Marshall

Coarctation of the aorta is an important differential diagnosis in adults with hypertension. Unfortunately, simply removing the obstruction does not restore cardiovascular normality. Patients may continue to be hypertensive, demonstrate abnormalities of endothelial function and remain at risk of premature coronary artery disease and other vascular disease. Therapy therefore requires both relief of the mechanical obstruction and long-term follow-up to deliver optimal antihypertensive therapy, vascular risk factor modification and detection and management of complications (such as bicuspid aortic valve and cerebral aneurysms). This paper discusses the management of three cases of this condition.
May 2002 Br J Cardiol 2002;9:287-90
The use of echocardiography for stroke and peripheral embolus: is it time for British/European guidelines?
Oliver R Segal, J Rex Dawson, Sandeep Gupta

The American College of Cardiology and the American Heart Association recommend echocardiography in patients with stroke or peripheral embolus who are less than 45 years of age or in those without evidence of cerebrovascular disease or other obvious cause.1 There are no equivalent guidelines from British or European Cardiac Societies. The prevalence of stroke and peripheral embolus has made it a common indication for the use of echocardiography. Despite this, to our knowledge there has been no previously published evaluation of the use of echocardiography in such patients in the UK. We undertook a retrospective review of transthoracic (TTE) and transoesophageal echocardiogram (TOE) reports (n=7,870) over 37 months at St. Bartholomew’s Hospital department of cardiology. This identified 153 (1.9%) patients investigated for stroke/transient ischaemic attack (TIA) or peripheral embolus. Of these, six patients had two or more examinations producing a total of 160 reports; five reports were unrecorded and, therefore, 155 reports were analysed. A total of 12 reports (7.7%) identified possible cardiac sources of emboli with a further n=3 reporting spontaneous contrast in the left atrium. The potential embolic sources included patent foramen ovale (PFO)(n=3), aortic atheroma (n=3), aneurysmal atrial septum (n=2), mobile lesions on the mitral valve (n=3) and thrombus in the left atrial appendage (LAA)(n=1).
These results have led to the development of standardised criteria with the design of a template on the performing and reporting of echocardiograms in this type of patient.
May 2002 Br J Cardiol 2002;9:280-6
Angiotensin II receptor antagonists in the treatment of heart failure: background to and design of the CHARM study
Simon W Dubrey

While angiotensin-converting enzyme (ACE) inhibitors are established agents for the treatment of hypertension and heart failure, in contrast the angiotensin II receptor antagonists (AIIRAs) have failed to demonstrate more than equivalence in randomised clinical trials. Trials such as ELITE II are criticised on the grounds that the dose used of losartan (50 mg) may have been sub-optimal. In ValHeFT, valsartan was shown to be superior to placebo only in patients who did not also receive a beta blocker. The ambiguity of response of AIIRAs in such trials will hopefully be clarified in CHARM, a large, placebo-controlled study which will assess the effects of candesartan in heart failure patients with either reduced ejection fractions in addition to an ACE inhibitor, and in those intolerant to an ACE inhibitor, as well as in patients with preserved ventricular function (diastolic heart failure) not on an ACE inhibitor. The design of the study is discussed.
May 2002 Br J Cardiol 2002;9:273-9
Therapeutic potential of the natriuretic peptide system
Paul R Kalra, Andrew JS Coats

Neurohormonal activation has a central role in the pathophysiology of various cardiovascular disorders. Despite recent therapeutic advances, potential exists to further manipulate these activated systems. The natriuretic peptide family consists of at least four structurally related peptides, with varying degrees of biological similarity. In the context of cardiovascular disease, the vast majority of data relates to atrial natriuretic peptide (ANP) and brain natriuretic peptide (BNP).
May 2002 Br J Cardiol 2002;9:265-72
The pathophysiology of primary pulmonary hypertension
Ghada W Mikhail, J Simon R Gibbs, Magdi H Yacoub

Primary pulmonary hypertension (PPH) is a progressive disease with a poor prognosis. It is characterised by an elevated pulmonary artery pressure and pulmonary vascular resistance that ultimately lead to right ventricular failure and death. PPH is a relatively rare and neglected disease which, until recently, had been poorly understood and had no effective form of therapy. This, however, is changing with the rapid accumulation of knowledge relating to the disease and its management. In this article, we review the possible mechanisms that may have a pivotal role in the development of the disease.
April 2002 Br J Cardiol 2002;9:
The specialist nurse in coronary heart disease prevention:evidence for effectiveness
Lucy Wright

Nurse-led interventions may improve the delivery of preventive care briefly discuss insights from parallel qualitative research; to present the preliminary results of the Bromley Changes care for coronary heart disease. In the SHIP trial, three cardiac liaison nurses co-ordinated care at the hospital-general practice interface. In the ASSIST trial, three different strategies of implementing secondary prevention were used. Although various measures improved, there was no difference in clinical outcome. Qualitative research indicates that specialist education for nurses is vital. The preliminary results of the Bromley Changes for Life Programme are described: this programme achieved significant risk factor and therapeutic targets. The way forward may lie with the cardiac specialist nurse.
April 2002 Br J Cardiol 2002;9:
The evidence for guideline implementation strategies
Irwin Nazareth

There is an enormous gap between the publication of new evidence and its clinical implementations. Research on interventions that are designed to change professionals’ clinical behaviour is detailed here: specific generic interventions, interventions specific to cardiovascular medicine, and continuing medical education. Barriers to change include information problems, stress and inertia. Further research and evaluation are required.
April 2002 Br J Cardiol 2002;9:
Secondary prevention of coronary heart disease in primary care:the evidence
Jonathan Mant

The National Service Framework for Coronary Heart Disease emphasises the role of primary care in secondary prevention. More than 20% of men and 12% of women aged 65 years and over suffer from ischaemic heart disease. Lifestyle changes and drug treatment may effectively reduce risk but uptake of the evidence base is patchy. There are a number of possible approaches to enhance the uptake. Nurse-led clinics and health promotion clinics can lead to improvement in reported lifestyle and self-reported health status. Audit and feedback may lead to more use of appropriate drugs. Systematic recall will lead to better documentation that care conforms to standard practice, and nurses are at least as effective as doctors in achieving this. The first step is to set up accurate morbidity registers.
April 2002 Br J Cardiol 2002;9:
The evidence for secondary prevention and cardiac rehabilitation in hospitals
Jane Flint

An integrated effort is needed to provide seamless care for patients between hospital and general practice. The use of protocols that are common to both sectors will lead to the best possible outcomes. It seems that secondary prevention may reduce sudden death and the 28-day mortality rate. The evidence base for the drugs used in secondary prevention is derived mostly from hospital trials. The relevant findings for aspirin, beta blockade, statins, ACE inhibitors and oral anticoagulants are discussed. After coronary revascularisation, special care is required if patients are to have a smooth path: both exercise and comprehensive cardiac rehabilitation are valuable.
April 2002 Br J Cardiol 2002;9:241-4
Can we do more to get patients to cholesterol targets?
Richard Hobbs

The role of cholesterol lowering in reducing cardiovascular risk is well established but a large proportion of qualifying patients at the highest risk are still not getting treatment with statins. Of those that do, most are not achieving recommended cholesterol targets. The cost of this, in terms of death and work days lost, is enormous. Patients should not be discharged after an acute event until secondary prevention has been initiated. Individual patient response to therapy should be subsequently monitored and adjusted as appropriate; patients should be reassured on statin safety.
April 2002 Br J Cardiol 2002;9:230-2
Can left bundle branch block cause chest pain?
Mammen Ninan, Jonathan W Swan

Can left bundle branch block cause chest pain? Mammen Ninan, Jonathan W Swan Exercise-induced left bundle branch block usually indicates underlying coronary artery disease or myocardial disease. Association of left bundle branch block (LBBB) with chest pain in the absence of coronary artery disease is rare. We describe the case history of a patient with chest pain associated with left bundle branch block with normal coronary arteries and review the literature on left bundle branch block associated with chest pain.
April 2002 Br J Cardiol 2002;9:226-9
Five thousand echocardiograms: what have we done?
David J Bell, David A Sandler

This article describes the use of transthoracic echocardiography (TTE) in a series of 5,000 consecutive echocardiograms in a mid-sized UK district general hospital. The report highlights the basic demographics, reasons for the requests, yield of abnormal results and sources of the requests. The authors comment on the percentage of abnormal results for the different request categories and on how TTE can be best utilised as a cardiac investigation.
April 2002 Br J Cardiol 2002;9:223-5
Patent foramen ovale, a normal variant or a congenital abnormality requiring treatment?
Mark S Turner, Anthony P Salmon, Gareth Thomas, Andrew J Marshall

It has now become possible to close a patent foramen ovale (PFO) using a percutaneous device. In addition, it has become increasingly clear that right-to-left shunting through a PFO can cause both stroke and decompression illness, due to paradoxical embolism of blood clots or gas bubbles. For these reasons, diagnosis of large PFO with significant right-to-left shunts has become important. The diagnosis can be made by transthoracic echocardiography with injection of bubble contrast, combined with multiple sustained Valsalva manoeuvres. Whilst transoesophageal echocardiography provides detailed anatomical information, functional information (with regard to right-to-left shunting) is better provided by transthoracic studies where a Valsalva can be properly performed. Device closure can prevent right-to-left shunting and can be achieved using a number of different devices. However, device closure has yet to be proven beneficial in a randomised trial. In light of the clear evidence implicating PFO, we undertake closure procedures in selected patients.
April 2002 Br J Cardiol 2002;9:221-2
Cardiac troponins and the risk stratification of chest pain
Archana Rao, Mandie Evans

We present three cases of patients who had chest pain with abnormal but non-diagnostic ECGs and negative troponin I, carried out in the appropriate time frame. All three went on to have extensive coronary artery disease demonstrated on coronary angiogram. These cases illustrate that use of troponin I alone as a marker for risk stratification of cardiac chest pain is not adequate: above all, a high index of clinical suspicion is of paramount importance.
April 2002 Br J Cardiol 2002;9:215-20
Future perspectives in stroke management
Philip MW Bath

Clinical research relating to stroke management is at something of a watershed. On the one hand, some therapies are well proven and established, and on the other some approaches have repeatedly failed. Examples of successes include antithrombotic (aspirin, dipyridamole, clopidogrel, warfarin) and antihypertensive therapies (diuretic, angiotensin-converting enzyme inhibitors), carotid endarterectomy for secondary prevention,1-4 and aspirin in acute ischaemic stroke.5 In contrast, several strategies have repeatedly failed, especially the use of anticoagulation and neuroprotection in acute ischaemic stroke. This review gazes into the crystal ball to see what we might be doing when managing patients with stroke in 10 years time.
April 2002 Br J Cardiol 2002;9:209-14
Acute effects of low-dose statins on serum cholesterol and creatinine kinase activity
Yohan P Samarasinghe, Graham Ball, Michael D Feher

One of the potential side effects of the HMG CoA reductase inhibitors (statins) is a rise in creatinine kinase (CK) activity. This is sometimes accompanied by myalgia and rarely by rhabdomyolysis. Statins are increasingly being started earlier in the presentation of acute coronary syndromes but the rise in CK activity that they may cause could be a potential confounding factor in the diagnosis of myocardial infarction (MI) in this population. In this open-labelled, prospective study, 12 hypercholesterolaemic, Caucasian subjects, with a significant cardiovascular risk, were commenced on low-dose statin therapy. Blood samples were taken prior to commencing the statin then on day three and seven for lipid profile and CK activity. Patients maintained their normal lifestyles and usual medication. Interviews were conducted at each visit. A consistent fall in total and low density lipoprotein (LDL) cholesterol levels was shown over the study period of one week. Apart from one participant, who had a CK rise on day three with accompanying myalgia, there was no consistent change in CK activity within the group. High density lipoprotein (HDL) cholesterol levels also did not show any significant change over the week. We conclude that the rapid and consistent fall in both total and LDL cholesterol levels with low-dose statin was not paralleled by any consistent change in CK activity. The lack of change in CK activity over one week, following acute initiation of statin therapy, is unlikely to cause difficulty in the diagnosis of MI. If the beneficial effects of statin therapy are due to cholesterol reduction, then acute initiation in coronary syndromes would be favourable.
April 2002 Br J Cardiol 2002;9:193-4
Statins: myalgia and myositis
Anthony S Wierzbicki

Statins: myalgia and myositis Anthony S Wierzbicki The topic of side effects of statin therapy has become more prominent since the precautionary withdrawal of cerivastatin following reports of death and rhabdomyolysis with this particular statin, especially when given in simultaneous combination therapy with gemfibrozil. In addition, many patients complain of myalgia with statins; this side effect has an incidence of up to 5%. There is a tendency for earlier use of statins in coronary care units because of improved compliance and the possibility of a reduction in peri-infarction events in registry studies, although the MIRACL trial of atorvastatin in acute coronary syndromes did not show any significant differences in hard end points at 16 weeks
April 2002 Br J Cardiol 2002;9:
The National Service Framework for Coronary Heart Disease
Richard Hobbs

Cardiovascular disease is the most important cause of illness in Britain. The focus of the National Service Framework for Coronary Heart Disease (NSF for CHD) is appropriate since the burden of CHD is high in the UK. Interventions for primary and secondary prevention include advice on reducing modifiable risk factors, smoking, maintaining blood pressure < 140/85 mmHg and using statins and dietary advice to lower serum cholesterol. Identification of those at greatest risk will require practice-based registers. Audits will be needed to ensure that the stipulated interventions are offered to those on the disease registers. The biggest implication for primary prevention will be selection of patients at increased risk of CHD. Implementation of the NSF will increase GPs’ workload.
April 2002 Br J Cardiol 2002;9:
Lipid control:the interface between specialist clinics and general practice
Mary Seed

The lipid-lowering trials have shown positive results in terms of reducing cardiovascular events. It is mandatory to measure lipid levels in patients with other cardiovascular risk factors, such as diabetes and hypertension. Explaining cardiovascular risk and lifestyle changes takes longer than the standard 7–9 minute consultation and might be more appropriate in a nurse-led clinic. Good communication between GPs and specialists can still be difficult to achieve: face-to-face meetings are helpful and email should be playing a major role. The National Service Framework for CHD prevention puts a great deal of pressure on GPs. Secondary prevention is non-controversial although ideal levels of LDL are not being reached.
April 2002 Br J Cardiol 2002;9:
Cardiovascular disease in diabetes care: a preventative strategy
Vinod Patel

An effective strategy for the prevention of cardiovascular disease in patients with diabetes is needed with the epidemic of diabetes mellitus around the world. The aims are to cut morbidity and mortality from coronary heart disease by risk factor reduction and to reduce the diabetic complications of retinopathy, renal disease and peripheral vascular disease. Findings of the United Kingdom Prospective Diabetes Study (UKPDS) imply that all diabetics should be subject to intensive glycaemia control and tight blood pressure control. GISSI-3 and the DIGAMI studies showed the benefits of lisinopril and an insulin/glucose infusion, respectively, post-MI. The HOPE study set out to examine whether ramipril reduced cardiovascular events in patients at high risk: the results were highly significant. The statin studies 4S, CARE and WOSCOPS showed the value of statins in primary and secondary prevention of cardiovascular events in patients with diabetes. Low-dose aspirin therapy should be used in patients with diabetes who are at high risk of cardiovascular events.
March 2002 Br J Cardiol 2002;9:
Day-case transradial coronary intervention – the future face of PCI in the UK
Somnath Kumar, David H Roberts

Percutaneous coronary intervention (PCI) is one of the mainstays in the treatment of coronary artery disease. Although the recent BCIS audit data indicate an improvement in the rate of PCI in the UK, it lags well behind the intervention rate in other European countries. The National Service Framework (NSF) for Coronary Heart Disease recommends an increase in the PCI rates to more than 750 per million population in order to achieve a target waiting time of three months. 1 To achieve this goal a major change in infrastructure is needed, with the opening of more interventional centres and the training and appointment of more interventional cardiologists. Within the current infrastructure and in a shorter time scale the targets may be met by performing more PCI through day-case work. The cardiologists directly control the day-case beds without any interference from the other medical specialities. Following the availability of modern low-profile stent technology and safer pre-treatment with oral antiplatelet agents, day-case intervention is a feasible option. 2 The RADICAL study A well-staffed day-case unit with an experienced senior sister and a pre-admission clinic has shown promising results in our unit at Blackpool for the management of day-case PCI through the radial route (Radial Approach for Day-case Intervention in Coronary Artery Lesions, the RADICAL study). Stable patients on the waiting list for PCI Table 1. The current status and future directions of day-case radial PCI PCI through the radial route is known to be safe, effective, economical and patient-friendly. In a pilot study we are evaluating its safety and efficacy in the day-case setting in selected patients with stable angina We believe that more day-case PCI will be the only way forward to achieve the NSF target rates for coronary revascularisation discharge of the patient. Following the procedure we take the sheath out immediately and apply a RADI Stop in the catheter lab.
March 2002 Br J Cardiol 2002;9:
Downsizing – using 5 French catheters via the radial artery
James M Cotton

Rapid technological advances in interventional cardiology have led to a marked change in practice over the past 20 years. Improvements in balloon dilation and stent catheter design, coupled with advances in guide catheter technology, have allowed routine percutaneous coronary interventions (PCI) to be performed through smaller guides. Initially there was a change from 10 to 9 French (F) catheters, and more recently from 8 to 6 F. These developments have not only led to a reduction in arterial complications, but also to changes in arterial access sites. The radial route has become increasingly popular, virtually eliminating access site complications. Moreover, this route has been shown to be preferred by many patients, the prime advantages being patient comfort, early mobilisation and reduced bleeding complications.
March 2002 Br J Cardiol 2002;9:
Complications of transradial procedures
Alun Harcombe

This short article aims to discuss the potential complications of transradial procedures and to set out approaches to minimising or avoiding them. Complications may relate to the operator, the patient, the equipment used or the nature of the procedure. Complications can simply be defined as minor (non-life-threatening, reversible, unlikely to extend hospital stay) or major (life-threatening, likely to cause permanent damage or to extend hospital stay). The complications of transradial procedures are rarely major and very rarely life-threatening – a major benefit of the radial approach. The potential complications can be divided into: neuro-vascular complications, spasm, vasovagal reactions and reflex ST segment changes. artery have been reported following transradial procedures. These include dissection, haematoma, perforation, bleeding, pseudo-aneurysm formation, arteriovenous fistula and even ischaemic con-tracture involving the hand. Most of these complications are minor, but they can result in access or procedural failure. Major vascular complications are very rare, occurring in only 0.06% of a recent series of 5,354 consecutive transradial procedures. Localised radial occlu-sion, which causes no untoward ischaemia, occurs in up to 5% of patients, but half of these occlusions recanalise within weeks. Spasm This is the most common complication of transradial procedures, and can vary from a minor event to a major painful stimulus ending the procedure.
March 2002 Br J Cardiol 2002;9:
Quality of life and economic issues
Peter F Ludman

The transradial approach for coronary angiography and angioplasty offers potential advantages over the femoral approach that include early patient ambulation, a reduced length of stay and reduced procedural cost. While many patients enjoy the freedom of early mobility, a proportion will experience forearm discomfort, either when catheters are manipulated during the procedure, or at the end of the procedure when the radial arterial sheath is withdrawn. This discomfort is caused by radial artery spasm. Spasm is induced both by mechanical stimulation of the arterial wall by the catheter shaft and arterial sheath, and by high levels of circulating catecholamines, which are raised by anxiety and pain. This review will examine data that address the pros and cons of a radial approach, particularly with respect to how well patients tolerate the procedure, the causes of radial artery spasm, and questions relating to potential benefits in terms of procedural cost. sheaths were used discomfort was usually experienced only at the end of the procedure, during sheath removal. Six years ago, a group from Argentina 2 reported some provisional data comparing femoral, percutaneous brachial and radial routes. They found significantly more pain with the radial procedures than with either the femoral or percutaneous brachial. Nevertheless, there were much earlier times to walking and to discharge in both the radi-al and percutaneous brachial groups. Later, Cooper 3 also compared femoral versus radial diagnostic angiography in 200 patients. Quality of life was assessed by the Medical Outcomes Study Short Form 36-item health status question-naire (SF-36). Procedure-specific questions were assessed using 0–10 visual analogue scales. Pain at the access site and preference for catheterisation method were also assessed with a visual analogue scale. In contrast to previous studies, they found that the radial route was better tolerated on SF-36 questionnaires and visual analogue scales at one week. When all patients were asked which route they preferred, most strongly preferred the radial route and when the 44 to a cocktail of verapamil and nitroglycerine was compared with the response to papaverine. 5 Verapamil plus nitroglycerine led to a much more rapid onset of vasodilatation, with a more pro-longed duration of action.
March 2002 Br J Cardiol 2002;9:
PCI via the radial artery: what is the learning curve?
Michael S Norell, Angela Hoye

PCI via the radial artery: what is the learning curve? Michael S Norell, Angela Hoye Introduction A ssessing the process by which a new approach is adopted requires an appreciation of the climate into which that change is introduced. We are an average UK interventional centre in terms of volume (650 cases per year), under pressure to increase throughput in the face of competing demands for the time of both consultant and specialist registrar (SpR) trainee operators. We were attracted to the notion of the radial approach because we thought that it might enhance day-case activity when the number of beds available for elective cases was declining. Although femoral arterial closure devices might also address this, our experience has indicated that their impact is less predictable. Some patients may still have to stay in hospital overnight because of a groin problem, even though the interventional procedure itself was uneventful. All our consultant operators are well trained in the Sones technique, but this procedure is itself not without diagnostic and interventional activity, provides a refreshing change. There is a clear advantage to the patient, catheter lab and ward staff, and the ever-more-senior operator will be reassured to know that he is still capable of taking on change.
March 2002 Br J Cardiol 2002;9:
Transradial coronary angioplasty
Simon S Eccleshall

Transradial coronary angioplasty Simon S Eccleshall Introduction T he most commonly used access sites for interventional cardiology are the femoral, brachial and radial arteries. The selection of arterial approach significantly influences the cost of the procedure and the patient’s quality of life as well as vascular access site complication rates, affecting procedural morbidity and mortality figures. 1 The exponential rise in stent deployment combined with more aggressive antiplatelet and anticoagulant therapy has exacerbated femoral vascular complications, with major bleeding rates of 23% following rescue angioplasty with concurrent use of glycoprotein (GP) IIb/IIIa inhibitors. 2 A safer route of arterial access would therefore be highly desirable. whom preceding diagnostic films were performed by the femoral route. 4 The transradial technique therefore fulfils the requirements for a safer access site for interventional procedures, with the added advantages of cost savings and improved quality of life. This approach can be used in combination with the femoral artery for intra-aortic balloon pump insertion and in combination with per-cutaneous puncture of a vein for right heart catheterisation and temporary pacing, whilst still conferring the benefits of safer arte-rial access. Technique catheter is vitally important when using the transradial technique: it must provide support from the aortic wall whilst being co-axial with the coronary ostium.
March 2002 Br J Cardiol 2002;9:
Transradial coronary angiography
David Hildick-Smith

Transradial coronary angiography DAVID HILDICK-SMITH T he transradial approach to coronary angiography was first considered to be a serious possibility in 1989. Gradual miniaturisation of equipment, coupled with the continuing desire to reduce patient discomfort and procedural risks, allowed the introduction of 6 French (6F) catheters. At 2 mm diameter, these fit without difficulty into most radial arteries. After Campeau experimented with this approach, others saw the potential, both for angiography and for angioplasty. From the diagnostic point of view, a simple transfemoral catheterisation is quick, uncomplicated, requires limited bed rest afterwards and can be accomplished with ease on a day-case basis in most patients. An arm approach is required in some patients because of difficulties with peripheral vascular disease, haemostasis or an inability to lie flat. These patients have formed the focus of our transradial diagnostic programme at Papworth Hospital. the transfemoral and transradial routes for diagnostic coronary angiography. 1 This study gave clear results: even allowing for the learning curve, the transradial route took longer, was more com-plicated, and resulted in a greater degree of pain in a significant proportion of patients. We therefore decided that the radial route should be reserved for patients in whom there is a relative con-traindication to the femoral approach, and we have continued with this policy ever since, though other authors have suggested that the transradial route is preferred by patients for diagnostic as well as interventional work. 2 We then compared the transradial route with the brachial cut-down procedure in a randomised study of 100 patients with con-traindications to the femoral approach. (~5%) and therapeutic anticoagulation (~10%). Diagnostic coronary angiography from the radial artery begins with a modi-fied Allen test to assess dual palmar arch circulation.
March 2002 Br J Cardiol 2002;9:
Starting a transradial programme
Jim Nolan

F doctors, catheter lab and nursing staff find the procedures difficult, technically demanding and time- consuming. Laboratory throughput is reduced, and some patients experience considerable discomfort or unpleasant vasovagal reactions. There is a high rate of puncture and procedure failure in the early stages, but these procedures can be easily completed from another access site if necessary. It is important that all the staff are clear about the reasons for starting a transradial programme (reduced vascular access site complication rate, easy and reliable haemostasis even when aggressive antithrombotic therapy is used, immediate patient mobilisation) and that there exists an important learning curve. Starting a transradial programme Jim Nolan The radial sheath should be removed at the end of the procedure, before the patient leaves the catheterisation laboratory. 2 In the rare situation of early re-intervention, an alternative access site can be used. When removing long sheaths, exert steady constant pressure
March 2002 Br J Cardiol 2002;9:182-4
Continuity and quality of care in people with coronary heart disease in general practice
Kamlesh Khunti, Kate C Windridge

Continuity of care is much valued by patients and doctors. It is seen as a core feature of the discipline in general practice, although there is little supporting evidence that it leads to improvement in the care given during the management of patients with chronic disorders. This study shows that increased continuity is not associated with improved clinical care in the secondary prevention of coronary heart disease. The study also shows that it is possible to maintain high continuity for a chronic condition in a group practice with flexible working arrangements. This has implications for recruitment of future general practitioners.
March 2002 Br J Cardiol 2002;9:171-81
Delivering evidence-based care to patients with heart failure: results of a structured programme
Martin R Cowie, Hugh McIntyre, Zoya Panahloo ON BEHALF OF THE OMADA INVESTIGATORS

The Omada programme, a nurse-delivered model of care, has achieved improved levels of evidence-based intervention for patients with chronic heart failure in nine secondary care centres in the UK. It may provide an appropriate model for audit and delivery of care, in line with the requirements of the National Service Framework for Coronary Heart Disease.
March 2002 Br J Cardiol 2002;9:168-70
Recurrent syncope in a patient with Andersen’s syndrome
Wayne R Arthur, Gerry C Kaye, Robert F Mueller

Recurrent syncope in a patient with Andersen’s syndrome Wayne R Arthur, Gerry C Kaye, Robert F Mueller Most common inherited diseases with cardiac involvement are associated with structural abnormalities of the heart and/or great vessels. Discussions of inherited cardiac electrophysiological abnormalities were once limited to Jervell and Lange-Nielsen syndrome and Romano-Ward syndrome. Subsequently, other genetically distinct arrhythmogenic cardiovascular disorders have been discovered.1 These result from mutations in the fundamental cardiac ion channels that orchestrate the action potential of the human heart. Most of these genetic channelopathies are depicted by marked QT prolongation on the electrocardiogram.
March 2002 Br J Cardiol 2002;9:163-7
Stroke in the patient with coronary heart disease
Diana R Holdright

Coronary heart disease (CHD) and stroke frequently coexist, partly because they share many risk factors. After myocardial infarction (MI), there is a significant risk of mural thrombus formation, left ventricular aneurysm, impaired left ventricular function and atrial fibrillation; all these increase the risk of stroke. The risk of neurological deficit after cardiac surgery is higher in those patients who have already had a stroke. Cognitive decline after cardiac surgery is common: it may follow a pattern of early improvement but later decline. Lipid-lowering therapy has been shown to reduce non-fatal stroke in patients at risk of developing or with coronary artery disease. Clopidogrel with aspirin may be of benefit in patients with unstable angina and non-ST elevation MI. Antihypertensive treatment and stopping smoking are helpful. The HOPE trial results showed a powerful and preventative role for ACE inhibitors.
March 2002 Br J Cardiol 2002;9:158-62
The clinical application of ACE inhibitors in coronary artery disease
Abba Gomma, John Henderson, Henry Purcell, Kim Fox

The renin-angiotensin-aldosterone system (RAAS) plays a key role in the pathogenesis of cardiovascular disease. Blockade of this system results in a number of biologically important beneficial effects, including inhibition of the breakdown of bradykinin, reduction in blood pressure and inhibition of neuroendocrine activity, as well as reversal of endothelial dysfunction. Angiotensin-converting enzyme (ACE) inhibitors have an established role in the management of hypertension and heart failure. More recently, for instance in the HOPE trial, they have been investigated in patients with a history of coronary artery disease, stroke, peripheral vascular disease, or diabetes plus at least one other cardiovascular risk factor, but with preserved left ventricular function. Treatment with ramipril was shown to reduce cardiovascular events significantly, especially in patients who had diabetes. Two further ongoing trials – EUROPA (with perindopril) and PEACE (with trandolapril) – are described, which have important differences in trial design and which will further assess the protective effects of ACE inhibition in patients with stable coronary artery disease.
March 2002 Br J Cardiol 2002;9:153-7
A survey of control of major risk factors following coronary artery bypass graft surgery
Mohd R Abdul-Rahman, Saveena S Ghaie, Justo R Sadaba, Levent T Guvendik, Alexander R Cale, Michael E Cowen, Steven C Griffin

The aim of this survey was to review the awareness and efficacy amongst patients and general practitioners (GPs) in controlling coronary risk factors following coronary artery bypass graft surgery (CABG). It was a prospective cohort study based on an inclusive registry at our department 230 patients who underwent CABG between April 1999–July 2000 and who had a history of hypertension and hypercholesterolaemia were selected. Frequency of blood pressure (BP) and cholesterol monitoring, blood glucose control, current smoking status, weight and medications were established via telephone interview of patients. BP and cholesterol levels were confirmed by written questionnaires to GPs. BP and cholesterol were considered to be controlled if they were ≤ 140/85 mmHg and ≤ 5.0 mmol/L respectively. Of the 230 patients, 213 were successfully contacted. After surgery, 181 (85%) patients had BP checks at least six-monthly by their GPs, 13 (6.1%) less frequently and 19 (8.9%) not at all. Cholesterol levels were checked at least six-monthly in 128 (60.1%), less frequently in 47 (22.1%) and not at all in 38 (17.8%). Thirteen of the 20 patients who were smoking at the time of surgery continued to smoke. BP and cholesterol readings were obtained for 169 of the 213 patients. Of these, BP was well controlled in 92 (54.4%), uncontrolled in 61 (36.1%) and not checked in 16 (9.5%). Cholesterol was well controlled in 106 (62.7%), uncontrolled in 35 (20.7%) and not checked in 28 (16.6%) patients. Although patients and GPs are generally aware of the importance of controlling coronary disease risk factors, more effort is required if we are to meet the Joint British recommendations on prevention of coronary heart disease.
March 2002 Br J Cardiol 2002;9:147-52
Intracoronary brachytherapy
Dougal R McClean, Martyn R Thomas

Restenosis following PTCA or intracoronary stent insertion remains the greatest challenge to interventional cardiology. Intracoronary brachytherapy may use either beta- or gamma- radiation. The target cells are most likely in the adventitial layer of the vessel wall. The principle of using brachytherapy post-angioplasty to reduce restenosis has been proven in animal models. Multiple randomised trials have shown brachytherapy to be the current optimal therapy to treat in-stent restenosis. The data for the use of intracoronary radiation for treatment of de novo coronary lesions are less strong. Potential complications of brachytherapy include ‘edge effect’ and ‘late late stent thrombosis’. These problems are being minimised with the use of long sources and prolonged antiplatelet therapy. Drug delivery stents may challenge the role of brachytherapy in preventing and treating restenosis in the near future.
March 2002 Br J Cardiol 2002;9:131-4
PROGRESS in the secondary prevention of stroke
Scott W Muir, Kennedy R Lees

PROGRESS in the secondary prevention of stroke Scott W Muir, Kennedy R Lees Over the last 10 years there has been considerable progress in the development of secondary prevention strategies for ischaemic stroke. No longer is aspirin the cornerstone of stroke secondary prevention. Trials like ESPS-21 and CAPRIE,2 have established the place of antiplatelet agents in secondary prevention. The 4S3 and CARE4 studies, among others, and the recently presented Heart Protection Study5 have alluded to the benefits of statins, not only in the setting of ischaemic heart disease, but now also in the setting of cerebrovascular disease. Until the publication of the PROGRESS study6 in September of last year, the question of blood pressure reduction in the setting of secondary prevention was unanswered and contentious.
March 2002 Br J Cardiol 2002;9:122-24
Caffeine-containing drinks – a cause of arrhythmias?
Saul G Myerson, Yohan Samarasinghe, Chris Taylor, Michael D Feher

Caffeine-containing drinks are increasingly available but excessive consumption can give rise to health hazards. A case is described here of a 31 year old man with no history of cardiovascular disease but a very high caffeine intake; he developed atrial fibrillation, which required treatment with flecainide. He has reduced his caffeine intake and remains well to date.
February 2002 Br J Cardiol 2002;9:120-21
Myocardial infarction in a patient with hypertrophic cardiomyopathy
Suneel Talwar, Khalid Khan

Myocardial infarction in a patient with hypertrophic cardiomyopathy Hypertrophic cardiomyopathy (HC) is a disease characterised by marked heterogeneity in its morphology and natural history. The prevalence of significant coronary artery disease in this population has been estimated to be just over 10%.1 On the other hand, the prevalence of transmural myocardial infarction in the absence of significant coronary atherosclerosis is about 15% in a population of patients who have died from HC.2 Although electrocardiographic criteria for diagnosis of acute myocardial infarction (AMI) in adults are well known and accepted, no general criteria exist for diagnosis of AMI in patients with HC. Further, there are no clear-cut guidelines for the management of patients with HC who present with a suspected AMI.
February 2002 Br J Cardiol 2002;9:115-19
United Kingdom Prospective Diabetes Study: implications for metformin
Clifford J Bailey, Ian W Campbell

One of the purposes of the United Kingdom Prospective Diabetes Study (UKPDS) was to compare the efficacy of different antidiabetic drugs in the long-term treatment of type 2 diabetes. In overweight type 2 patients, use of metformin as the initial antidiabetic drug therapy reduced overall mortality and reduced various long-term complications to a greater extent than other first-line treatments tested (sulphonylureas and insulin) whilst controlling hyperglycaemia to a similar extent. The benefit of early intervention with metformin may be due, at least in part, to its actions against insulin resistance and associated cardiovascular risk factors. Thus the UKPDS has provided evidence that early intensive glucose control with metformin in overweight type 2 diabetic patients is a particularly effective approach to reduce vascular complications and improve survival.
February 2002 Br J Cardiol 2002;9:109-14
The cost-effectiveness of amlodipine treatment in patients with coronary artery disease
Roman Casciano, John J Doyle, Alistair McGuire, Raúl Arocho, Steve Arikian, JuliaN Casciano, Heather Kugel, Nick Marchant, Renee Kim

The objective of this paper was to quantify the impact on overall cardiovascular disease treatment costs resulting from the use of amlodipine in the coronary artery disease (CAD) population in the UK. A Markov cohort simulation model was developed to estimate the overall average healthcare costs of patients with CAD in the UK and to determine the cost-effectiveness of the use of amlodipine as part of their treatment regimen. Outcome probabilities used in the model were based on patient-level data from the Prospective Evaluation of the Vascular Effects of Norvasc Trial (PREVENT). Cost estimates for in-patient and out-patient care associated with each outcome were applied to quantify the overall average healthcare cost for each arm of the study. The hospitalisation rate per patient in the placebo cohort was 61.8% while that in the amlodipine cohort was 44.3%. This corresponds to an average cost per patient for cardiovascular disease (CVD) treatment of £1,858.64 for amlodipine patients and £1,800.49 for placebo patients over three years of follow-up. Calculations yield a cost per hospitalisation avoided of £331.67. In conclusion, the inclusion of amlodipine in the treatment regimen for patients with CAD is expected to result in improved clinical outcomes through a marginal investment in cost.
February 2002 Br J Cardiol 2002;9:106-8
Does the routine use of lead increase prognostic yield in exercise electrocardiography?
Khalid Mahmood, Daniel Higham

We studied the potential benefits of using lead V4R during routine exercise treadmill testing for patients undergoing district general hospital investigation for suspected coronary artery disease. Some 298 patients with known or suspected coronary artery disease, referred for exercise testing, had an electrocardiogram recorded with standard leads and had lead V4R placed in the V4R position. The exercise tests were interpreted using standard criteria and were reported as being negative, inconclusive, positive or adversely positive. The mean age of the patients was 57 years. Some 86 (29%) of the tests were positive: 12 of the 86 positive tests showed significant changes in lead V4R (14%). Of the 86 positive tests, 25 were adversely positive (29%) and, of these, nine had a positive V4R test (36%). Patients with V4R positive tests compared to those with V4R negative tests had significantly decreased exercise duration leads with ST changes and reduced workload. The finding of a positive V4R test indicated a significantly greater chance of an adversely positive exercise test result (p<0.001), with nine of the 12 positive V4R results (75%) being associated with adversely positive tests. There were no isolated positive V4R tests.
February 2002 Br J Cardiol 2002;9:103-5
Prognosis, outcome and recurrence of stroke
Graham Venables

Defining prognosis may be helpful in planning acute treatment of stroke, setting rehabilitation goals and setting resource priorities. Case fatality is 12% within the first seven days of a first-ever stroke. Late deaths are usually due to the consequences of immobilisation and stroke recurrence. Long-term outcome is difficult to predict but older age, significant pre-stroke co-morbidity and severe stroke are generally associated with poor physical recovery. Stroke patients have a risk of recurrence 15 times that of an age- and sex-matched population. Stroke type may influence recurrence. Early stroke recurrence may be prevented by antiplatelet drugs. Patients in atrial fibrillation and with recently symptomatic high-grade carotid stenosis are at particular risk of stroke.
February 2002 Br J Cardiol 2002;9:99-102
Atrial septal defects – a differential diagnosis for breathlessness in adults and the elderly
Mark S Turner, Anthony P Salmon, Andrew J Marshall

Atrial septal defects are a common form of congenital heart disease that can present at any age, even in the elderly. As symptoms may be non-specific (breathlessness, palpitations), a high index of suspicion should be maintained. The ECG may be normal in the absence of significant pulmonary hypertension although a chest radiograph should be helpful. The diagnosis is usually confirmed by transthoracic echocardiography, although some types of atrial septal defects may be missed in adults who are poor echo subjects. Transoesophageal echo provides definitive diagnostic information and should be undertaken in any patient with right heart dilatation of unknown cause. Whilst closure of atrial septal defects may not prevent atrial arrhythmia, it can reduce the haemodynamic consequences if episodes occur. Many atrial septal defects can now be closed with percutaneous devices, avoiding the need for sternotomy.
February 2002 Br J Cardiol 2002;9:92-8
Grown-up congenital heart disease – experience in a district general hospital
Leisa J Freeman, Sheila Wood, Toni Hardiman, Antony JF Page

Some 340 adult patients (186 male, 154 female; average age 36 years) with congenital heart disease are now seen in a dedicated clinic at a district general hospital. Septal defects and aortic pathology account for 48% of cases seen and 21% have complex congenital heart disease. A first operation has been performed in 55%, a second operation in 13.3% and a third operation in 3.2%. Pulmonary hypertension is present in 7%. Eighty two of the 154 women have had 123 pregnancies. Care issues relating to the pregnant grown-up congenital heart disease (GUCH) patient are discussed. The growth of this population is highlighted, as is the requirement for more structured care. Issues relating to the establishment of a dedicated GUCH clinic are discussed, including training of cardiologists in this sub-speciality.
February 2002 Br J Cardiol 2002;9:68-71
Whatever happened to silent ischaemia?
Prithwish Banerjee

Myocardial ischaemia is a reliable predictor of significant coronary artery disease (CAD). During an episode of myocardial ischaemia, anginal pain may appear late or not at all, even in the presence of ischaemic changes on the electrocardiogram (ECG). This phenomenon of silent ischaemia was first described by Stern and Tzivoni in 1974.1 As many as 70% of daily ischaemic episodes in stable CAD and 90% of episodes in unstable angina are silent.
February 2002 Br J Cardiol 2002;9:65-67
Adult congenital heart disease: time for a national framework
Michael A Gatzoulis

Adult congenital heart disease: time for a national framework Michael A Gatzoulis Congenital heart disease (CHD) is one of the most common inborn defects, occurring in approximately 0.8% of newborn infants. Adults with congenital heart disease are the beneficiaries of successful paediatric cardiac surgery and cardiology programmes across the United Kingdom. Had it not been for surgical intervention in infancy and childhood, 50% or more of these patients would have died before reaching adulthood.
February 2002 Br J Cardiol 2002;9:
Angiotensin II: the greatest serial killer of all time?
Mike Holland

This supplement has been sponsored by Merck Sharp & Dohme Limited. It features highlights from a meeting "Changing the course of cardiovascular disease", which was held in March 2001 in Istanbul and sponsored by Merck Sharp & Dohme Limited.
January 2002 Br J Cardiol 2002;9:7–9
Britain: still the sick man of Europe?
Adrian JB Brady

The publication of the Healthwise Database in the British Medical Journal in June 2001 has shown again that in Britain we are poor at implementing well-established strategies which we know reduce the risk of coronary events in patients with ischaemic heart disease. The Healthwise study, which was carried out over 18 months between 1997 and 1998, examined the records of 548 general practitioners (GPs) throughout mainland Britain. The records of 989 161 patients were examined and 24 431 patients with established coronary heart disease (CHD) were identified. The mean age of men was 67 years and women 72 years, and two thirds of the patients were over 70. The middle-aged man with angina has generally been regarded as the typical coronary disease patient. This is not true: it is my view that in the future we will be devoting much of our energies to heart disease in the elderly. The prevalence of CHD was 2.5% in this survey but it is known that the true prevalence is greater than this. There must be, then, a proportion of patients who are not considered by their general practitioner to have established coronary disease. The Healthwise study addressed one main area: the measures that were being adopted by general practitioners to address risk factors and drug therapy for patients with established coronary heart disease.
January 2002 Br J Cardiol 2002;9:54-6
A secondary prevention tool for use by primary care organisations
Chris Harris

Though the evidence for secondary prevention of cardiovascular disease is strong, the substantial benefits in terms of outcomes are often lost at practice level with competing clinical priorities and, at primary care group/trust level, with competing commissioning priorities. Our primary care trust has developed a secondary prevention tool that gives a clear picture of the benefits achievable with effective secondary prevention.
January 2002 Br J Cardiol 2002;9:23-30
Stroke rehabilitation
Marion Walker

The devastating consequences of stroke make rehabilitation a substantial challenge. The benefits of stroke units are well established; the collaborative work of the multidisciplinary team may be one of the most important factors. The evidence for the efficacy of occupational therapy is conflicting and a meta-analysis of community occupational therapy trials is under way. Greater physiotherapy input is associated with a reduction in death and deterioration. One third of all surviving stroke patients require speech and language therapy but most receive less than 45 minutes per week. More rehabilitation research needs to be conducted. In the absence of scientific evidence, expert opinion still has an important part to play in the rehabilitation process.
January 2002 Br J Cardiol 2002;9:38-41
Biphasic positive pressure ventilation in acute cardiogenic pulmonary oedema
Nicola Cooper, Badie Jacob

Non-invasive positive pressure ventilation (NIPPV) may be used in the treatment of acute cardiogenic pulmonary oedema. It has been shown to reduce the need for intubation and to improve left ventricular function. Patients do not need to be admitted to intensive care but can be managed in a coronary care unit. Two cases are described in this article. The indications, contraindications and complications of NIPPV are described and a practical guide to its use is given.
January 2002 Br J Cardiol 2002;9:47-48
Obesity management in cardiovascular disease – a view from primary care
Michael Schachter, Henry Purcell, Caroline Daly, Mary Sheppard

Overweight and obesity affect around half of the UK population, and are a serious public health problem. Obesity is associated with hypertension, dyslipidaemia, type 2 diabetes and a sedentary lifestyle, and has been shown to be an independent risk factor for development of cardiovascular disease. There are characteristic structural changes of the heart and vasculature in obesity. There is strong evidence that even modest weight reduction lowers cardiovascular risk. Dietary intervention, lifestyle advice and increased exercise are the initial strategy, but selected patients will require adjunctive treatment with anti-obesity drugs. In the absence of contraindications, orlistat is appropriate to use in obese patients with established cardiovascular disease, though sibutramine use is contraindicated in this population. Surgical intervention, such as gastric restrictive procedures, may be needed in severe obesity but there is a high complication rate among the morbidly obese and particularly in those who are also diabetic.
January 2002 Br J Cardiol 2002;9:49
Fax stretch
Andrew RJ Mitchell, Alistair KB Slade

Fax machines are essential tools in modern medicine. With increasing pressure to reduce ‘door to needle’ times in acute myocardial infarction, appropriate interpretation of electrocardiograms (ECGs) by cardiologists is desirable and the use of fax machines to transmit recordings is advised.1-4 Fax technology is not infallible, however.
January 2002 Br J Cardiol 2002;9:50-2
Successful pregnancy following a peripartum cardiomyopathy
Oliver R Segal, Kevin Fox

Successful pregnancy following a peripartum cardiomyopathy Peripartum cardiomyopathy is a rare complication of pregnancy, characterised by the development of heart failure secondary to a dilated cardiomyopathy in the peripartum period. Peripartum cardiomyopathy (PPCM) carries a significant morbidity and mortality and there is a risk of recurrence in subsequent pregnancies. Many issues relating to this condition are unresolved, including its exact aetiology, optimal treatment and assessment of the risk of recurrence.
January 2002 Br J Cardiol 2002;9:54-6
A secondary prevention tool for use by primary care organisations
Chris Harris

Though the evidence for secondary prevention of cardiovascular disease is strong, the substantial benefits in terms of outcomes are often lost at practice level with competing clinical priorities and, at primary care group/trust level, with competing commissioning priorities. Our primary care trust has developed a secondary prevention tool that gives a clear picture of the benefits achievable with effective secondary prevention.
